Code Blue Erin Stiefel Monique Sandoval Vivianne Sanada

Code Blue Erin Stiefel, Monique Sandoval & Vivianne Sanada GNRS 586: Leadership and Management Janet Wessels, MSN, RN, PHN July 15, 2015

Background ❖ 80 y. o. male ❖Hx: CAD, HTN & Schizophrenia ❖Admitting diagnosis: hallucinations & anxiety ❖Unit: inpatient psychiatric ❖Hospital day 2: sudden onset of confusion, bradycardia & hypotension ❖Pt lost consciousness & a “code blue” was called ❖Inpatient psych unit is adjacently located to a major academic medical center ❖Code team within the main hospital was activated ❖Part of code team had never been to psych unit ❖The two buildings connect on 4 th floor

Background ❖Senior resident & intern used the only route they knew of to get to the inpatient psych unit ❖Upon arrival, patient pulseless & apneic with O 2 mask on ❖Chest compressions / ventilatory support not yet initiated ❖Resident & intern began CPR with bag-valve-mask ❖Monitor leads incompatible with stickers placed on the patient ❖Patient remained pulseless with an uncertain rhythm & O 2 sats remained 80% ❖O 2 was connected, but never turned on by RN ❖Code status was revealed as DNR, without documentation ❖Resuscitation efforts were continued by some at this point ❖Son was called confirming DNR ❖Efforts were stopped & patient died moments later
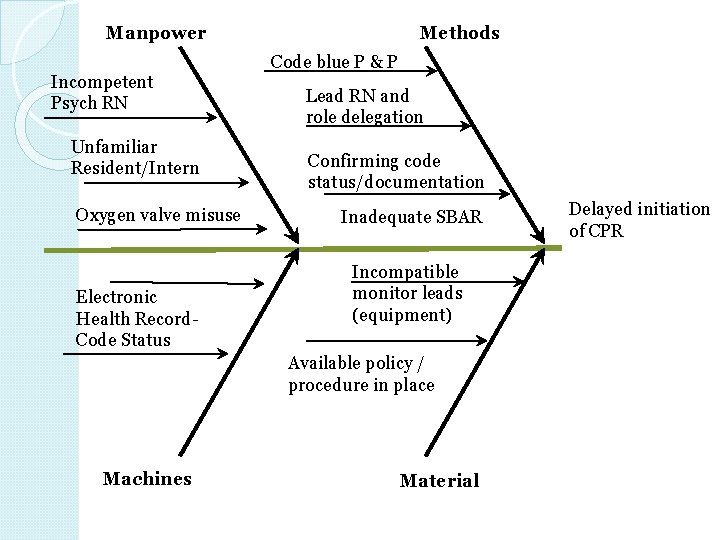
Manpower Incompetent Psych RN Unfamiliar Resident/Intern Oxygen valve misuse Electronic Health Record. Code Status Methods Code blue P & P Lead RN and role delegation Confirming code status/documentation Inadequate SBAR Incompatible monitor leads (equipment) Available policy / procedure in place Machines Material Delayed initiation of CPR
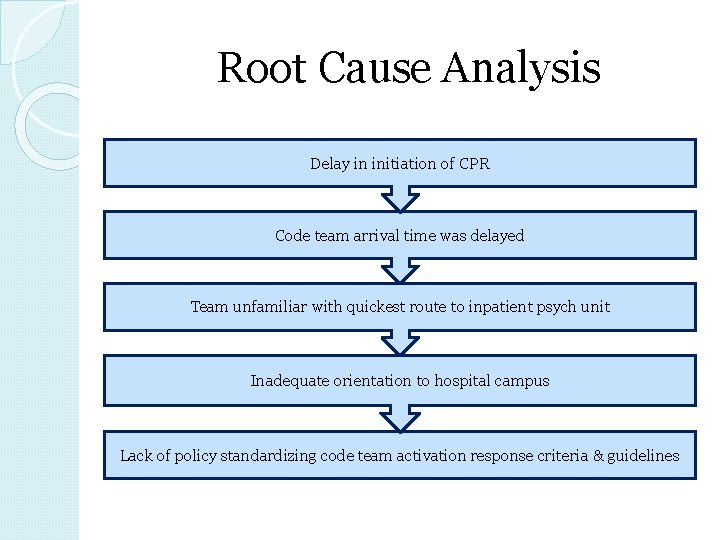
Root Cause Analysis Delay in initiation of CPR Code team arrival time was delayed Team unfamiliar with quickest route to inpatient psych unit Inadequate orientation to hospital campus Lack of policy standardizing code team activation response criteria & guidelines

Root Cause Analysis v. There was a significant delay in the patient receiving CPR due to a lack of protocol outlining training guidelines & standardization criteria for code team.
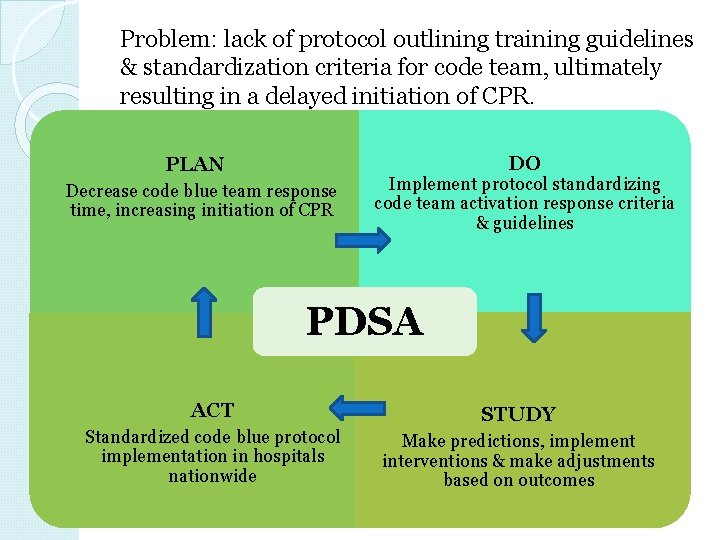
Problem: lack of protocol outlining training guidelines & standardization criteria for code team, ultimately resulting in a delayed initiation of CPR. DO PLAN Decrease code blue team response time, increasing initiation of CPR Implement protocol standardizing code team activation response criteria & guidelines PDSA ACT STUDY Standardized code blue protocol implementation in hospitals nationwide Make predictions, implement interventions & make adjustments based on outcomes

PDSA: Aim v Reduce designated hospital code blue team response time per call to under 3 minutes from time of overhead code call to unit arrival for 100% of code blue incidents within 6 months.
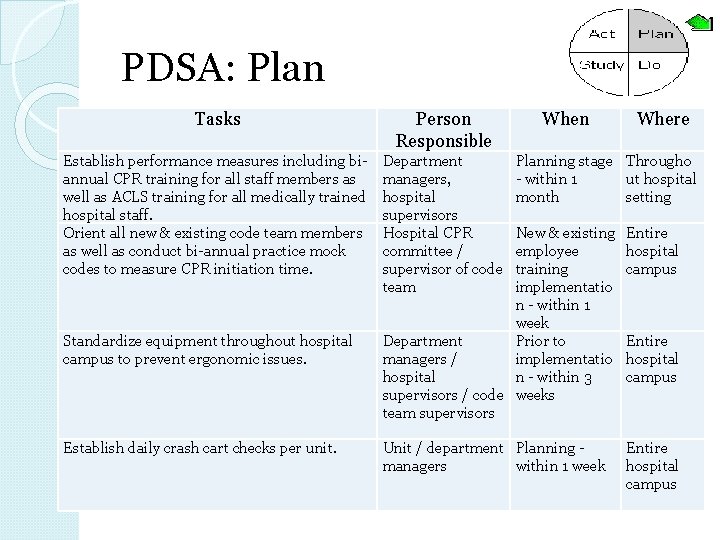
PDSA: Plan Tasks Person Responsible Establish performance measures including biannual CPR training for all staff members as well as ACLS training for all medically trained hospital staff. Orient all new & existing code team members as well as conduct bi-annual practice mock codes to measure CPR initiation time. Department managers, hospital supervisors Hospital CPR committee / supervisor of code team Standardize equipment throughout hospital campus to prevent ergonomic issues. Establish daily crash cart checks per unit. When Where Planning stage Througho - within 1 ut hospital month setting New & existing employee training implementatio n - within 1 week Department Prior to managers / implementatio hospital n - within 3 supervisors / code weeks team supervisors Entire hospital campus Unit / department Planning managers within 1 week Entire hospital campus
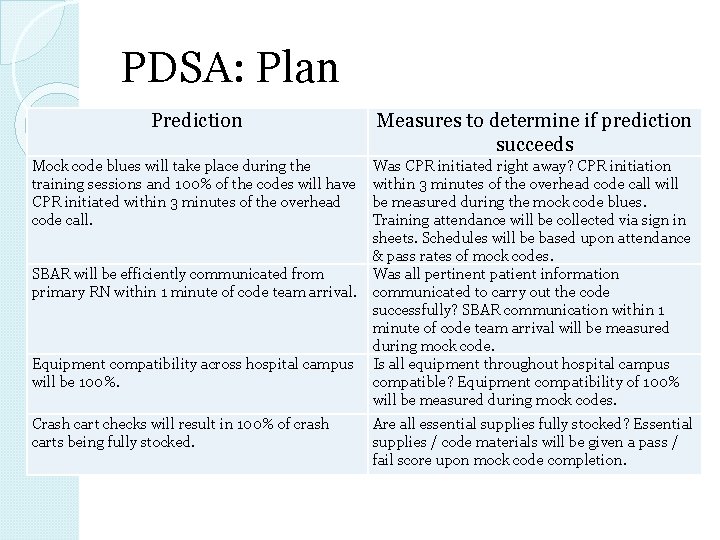

PDSA: Plan Prediction Measures to determine if prediction succeeds Mock code blues will take place during the training sessions and 100% of the codes will have CPR initiated within 3 minutes of the overhead code call. Was CPR initiated right away? CPR initiation within 3 minutes of the overhead code call will be measured during the mock code blues. Training attendance will be collected via sign in sheets. Schedules will be based upon attendance & pass rates of mock codes. Was all pertinent patient information communicated to carry out the code successfully? SBAR communication within 1 minute of code team arrival will be measured during mock code. Is all equipment throughout hospital campus compatible? Equipment compatibility of 100% will be measured during mock codes. SBAR will be efficiently communicated from primary RN within 1 minute of code team arrival. Equipment compatibility across hospital campus will be 100%. Crash cart checks will result in 100% of crash carts being fully stocked. Are all essential supplies fully stocked? Essential supplies / code materials will be given a pass / fail score upon mock code completion.

PDSA: DO Code Team: Protocol implementation ❖ Bi-annual skill competency testing ➢ New hire & existing code team orientation ➢ Mock codes / simulations ➢ Adherence to response time standards ➢ Map routes for entire hospital campus ➢ Equipment standardization / function tests ➢ Crash cart checks ➢ SBAR training ➢ Code status documentation checklist ➢ EHR training: code status ❖ Time frame: 6 months of orientation, training & mock codes in order for protocol to be implemented in daily practice

PDSA: Study Prediction Outcome CPR will be initiated within 3 minutes of overhead code call by arrival of code blue team in 100% of code blue incidents. Code team arrival averaged at 5 minutes, rather than 3. Upon code team arrival primary RN will delegate roles within 1 minute of arrival. Role delegation lasted 2 minutes on average. Bedside RN will deliver adequate SBAR while code team is beginning role tasks, within 1 minute of arrival. SBAR was clear, succinct, and beneficial to the code team. Code team will debrief & discuss problem Debrief sessions helped identify areas for areas to address for success of future improvement and allowed the code team codes. to focus on individual areas of weakness to make adequate policy improvements. 100% of hospital staff will pass BLS skills 100% of hospital staff passed the BLS checks, 100% of code team will pass mock skills check, 85% of code team passed code blue simulation checklist. mock code blue simulation due to arrival time.

PDSA: Study Problem Solution Code team arrival averaged at 5 minutes, rather than 3. Increase time frame to 9 months to allow staff to become accustomed to new protocol Role delegation to initiation of Code team will have role tasks took longer than the 1 minute delegation by manager at goal beginning of shift rather than during code Summary of findings: ● Implementing the new protocol has been successful at reducing the time it takes the code blue team to arrive to code calls ● Our aim of reducing code blue team response time per call to under 3 minutes for 100% of code blue incidents was not quite reached ● The 6 month time frame may not have been enough time to allow the staff to become accustomed to the new protocol

PDSA: Act ❖Standardized code blue protocol implementation in hospitals nationwide ❖Based on study outcomes reducing adverse code events ❖Code blue team protocol will include: ➢hospital campus orientation ➢emergency route tour of hospital campus ➢equipment standardization & checks ➢simulated mock code blues ➢decrease in time from overhead code call to CPR initiation ➢SBAR training ➢skill competency testing

Stakeholder Analysis v Internal (unit) stakeholders ü Management ü Nurse Managers ü Psych Nursing Staff ü The “Code Team” v Senior Medical Resident v Medical Intern v Anesthesia Resident v Anesthesia Attending v Critical Care Nurse v External stakeholders ü Patient ü Family / pts loved ones (son) ü Academic medical center ü Insurance companies ü Other hospitals
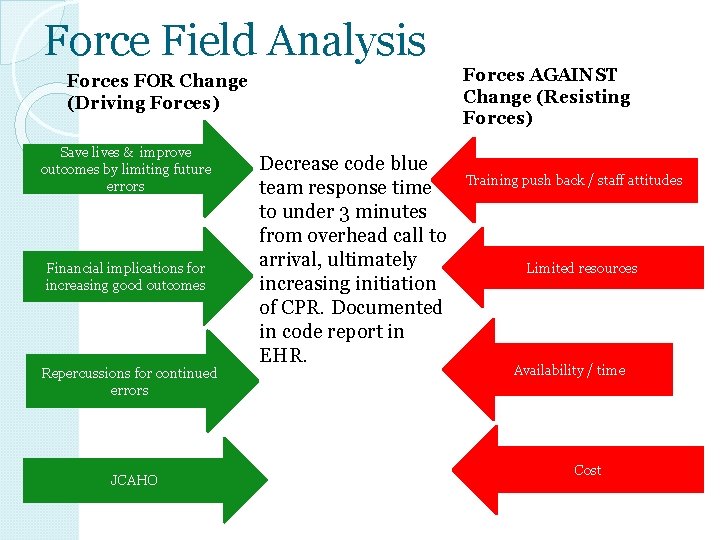
Force Field Analysis Forces AGAINST Change (Resisting Forces) Forces FOR Change (Driving Forces) Save lives & improve outcomes by limiting future errors Financial implications for increasing good outcomes Repercussions for continued errors JCAHO Decrease code blue team response time to under 3 minutes from overhead call to arrival, ultimately increasing initiation of CPR. Documented in code report in EHR. Training push back / staff attitudes Limited resources Availability / time Cost

References Adams, B. D. , Carr, B. , Raez, A. , & Hunter, C. J. (2009). Cardiopulmonary resuscitation in the combat hospital and forward operating base: use of automated external defibrillators. Military Medicine, 174(6), 584 -587. Guidelines 2000 for Cardiopulmonary Resuscitation and emergency cardiovascular care. Part 4: the automated external defibrillator: key link in the chain of survival. The American Heart Association in Collaboration with the International Liaison Committee on Resuscitation. (2000). Circulation, 102(8 Suppl), I 60 -I 76. , Lanfranchi. J. A. (2013). Instituting code blue drills in the OR. AORN Journal, 97(4), 428 -434. doi: 10. 1016/j. aorn. 2013. 017 Mullen, L. , & Byrd, D. (2013). Using simulation training to improve perioperative patient safety. AORN Journal, 97(4), 419 -427. doi: 10. 1016/j. aorn. 2013. 02. 001 Qureshi, S. A. , Ahern, T. , O'Shea, R. , Hatch, L. , & Henderson, S. O. (2012). A standardized code blue team eliminates variable survival from in-hospital cardiac arrest. The Journal Of Emergency Medicine, 42(1), 74 -78. doi: 10. 1016/j. jemermed. 2010. 023
- Slides: 17