Coagulation Defects In Obstetrics Normal coagulation 2 processes

Coagulation Defects In Obstetrics

Normal coagulation (2 processes) 1. Plug of platelets in response to disruption of vascular endothelium &exposure of collagen →platelet adhesion & clamping 2. Formation of fibrin cap (coagulation cascade)

Coagulation cascade (intrinsic &extrinsic pathways) • Intrinsic pathway: - Its components circulating in the blood stream - Its function measured by PTT and primarily affected by heparin therapy • The extrinisic pathway : - Initiated by tissue thromboplastin ( lll) + extrinsic coenzyme (Vll) activate factor x (common pathway ) - Measured by PT & inhibited by warfarin therapy

• Both pathways culminate in activation factor X which initiates the common pathway
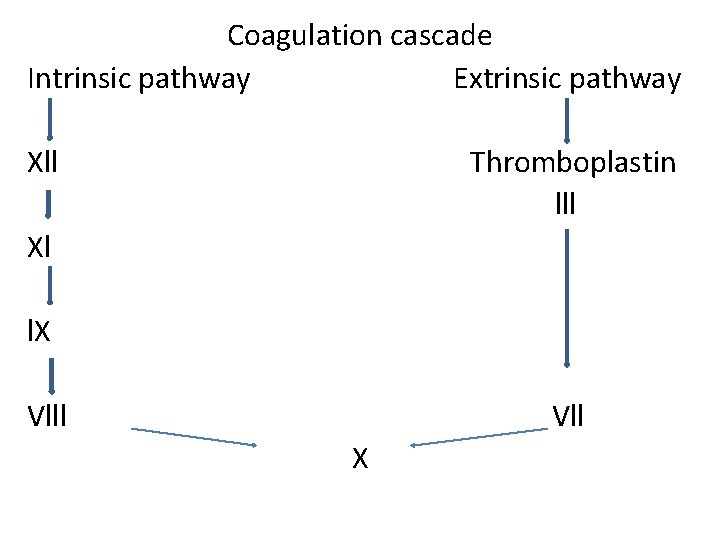
Coagulation cascade Intrinsic pathway Extrinsic pathway Xll Thromboplastin lll Xl l. X Vlll Vll X

X Common pathway Phosphplipids + Xa + Va + Ca + platelet surface factors Prothrombin(ll) Thrombin Fbrinogen(l) Fibrin degradation

Antagonism of coagulation cascade • Clot prevention : - Antithrombin lll , alpha two macroglobulin and alpha one antitrypsin inhibit factor - Protein c & ltscofactor s → inactivate factor V and Vlll • Clot dissolution : Plasminogen →plasmin Ẁ enhances fibrin degradation

Pathophysiology of DIC • Tissue destruction →releasa thrombo plastin (lll) into the circulation e. g abruption (extrinisic)→ the main cause of DIC - Endothelial injury → collagen & other tissue factors are realsed in the circulation → activate factor X e. g pre-eclampsia - Certain endotoxins and exotoins activate factor X - Proteases as present in mucin produced by neopasms →direct activation of factor X

Coagulation Defects In Obstetrics • Defiency of coagulation factors with tendency to bleeding results from disseminated intravascular coagulation ( DIC ) , dilutional coagulopathy and excessive infusion with Dextran solution.

Disseminated Intravascular Coagulation paradoxic situation in which both thrombotic & fibrinolytic mechanism are simultaneously activated →coagulation &haemorrhagic diseses are present at the same time

A) Disseminated Intravascular Coagulation 1. When DIC occurs there is consumption of blood platelets, fibrinogen and clotting factors 2. This is accompanied by increased activity of the fibrinolytic system to produce lysis of the fibrin thrombi to maintain patency of the microcirculation 3. This results in increased fibrin degradation products 4. Bleeding occurs when plasma fibrinogen reaches 100 mg% or less 5. During pregnancy the fibrinogen level is 400 -600 mg%

Aetiology The causes of DIC and hypofibrinogenaemiain obstetrics include: 1. Sever placental abruption. Commonest cause and responsible for 60 -70% of cases 2. Missed abortion. The degenerated placenta or dead fetus liberates thrombopastin which enters the maternal circulation causing intravascular 3. Intrauterine death (1∕ 3 cases > 5 wk ) 4. Septic abortion , puerperal sepsis, chorioamnionitis and pyelonephritis

The endotoxin of Gram-negative organisms as E coli leads to: (a)Damage of vascular endothelium (b) clump of platelets (c) activates factor 12 5. Amniotic fluid embolism , the amniotic fluid contains thromboplastin 6. Sever pre-eclampsia and eclampsia due to damage of capillary endothelial cells and release ofthromboplastin from degenerated placenta

7. Uterine rupture and any extensive tissue damage. (a) trauma may cause release of thromboplastin from damaged tissues in the circulation. (b) formation of a large haematoma may consume fibrinogen and other clotting factors (c) uterine rupture may allow amniotic fluid to enter maternal circlation 8. Incompatible blood transfusion red cell leads to release of thromboplastin 9. Acute fatty liver of pregnancy it may present like preeclampsia

• Diagnosis A. Failure of the blood to coagulate may give to petechiae epistaxis , haematuria , bleeding from needle puncture sites and postpartum hemorrhage B. The clot observation test ( weiner test). It is a rapid bedside test. 5 ml of venous blood are withdrawn in a test tube normally clot formed in 6 -12 min. Failure of any clot to from within 10 minutes indicates that fibrinogen is less than 100 mg %. If clot incubated at 37 c , dissolves after 30 minutes. It means excessive fibrinolytic activity

C. A coagulation profile is ordered which will show : 1. Plasma fibrinogen is reduced (N: 200 300 mg% in pregnacy 400 -600 mg% ) 2 - Bleeding time : N : 2 - 4 min , increase in DIC due to decrease platelt 3 – Clotting time : N: 6 – 12 min 4 - Platelet count is decreased ( ˂ 150, 000 per cu. mm)

5 - Prothrombin time (PT) is increased ( N: 10 -15 seconds 6. Thrombin time ( T T) is increased ( N : 25 -35 seconds 7. Partial thromboplastin time ( PT T) isincreased ( N: 25 -35 seconds) 8. Antithrombin III consumption is increased so its level or activity is decreased( N: 22 -39 mg /dl or activity 84 - 123% )

9. D-Dimers. These products rise when there is thrombosis and are morespecific than fibrin degradation products (above o. 5 ug is abnormal). D-dimers result from lysis of fibfin throbi by plasmin , so they only increase when there is clot formation

10 -Fibrin degradation (split ) products (N 10 ug%) are increased (more than 40 micrograms / ml) Eibrin degradation products may increase in absence of thrombosis as in liver disease as they are cleared by the liver

Treatment 1. Treatment of the cause , e. g, if DIC is due to infection , broad spectrum antibiotic are given 2. Fresh whole blood to replace the blood volume , red cells and clotting factors. If whole blood is not availabe , give packed red cells and fresh frozen plasma( FFP ) or cryo-precipitate 3. Plateles are transfused if platelet count is below 50, 000/cu. mm. 4. Administration of antithrombin III concentrate may improve the condition

5. Recombinant activated factor 7 ( rf FVIIa ) 6. Heparin. In case of a dead fetus and when laboratory tests indicate DIC but the patient is not bleeding. Heparin is given to raise the fibrinogen level to above 200 mg % 7. The coagulation defect corrects itself spontaneously within 24 hours after delivery or removal of the cause
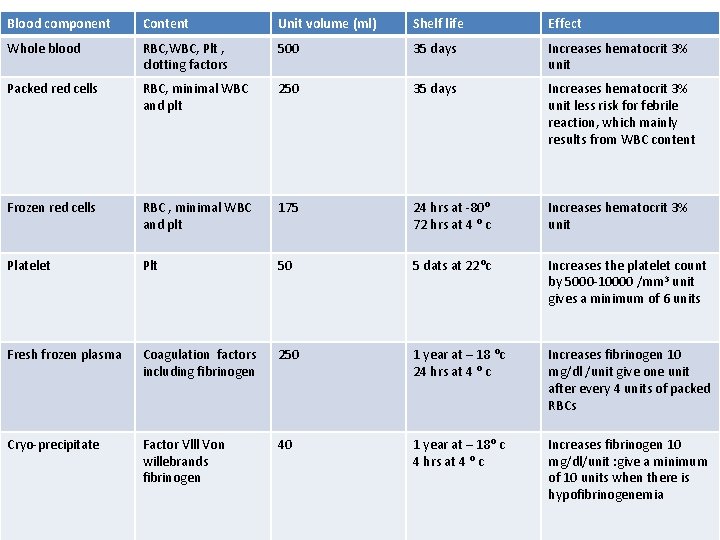
Blood component Content Unit volume (ml) Shelf life Effect Whole blood RBC, WBC, Plt , clotting factors 500 35 days Increases hematocrit 3% unit Packed red cells RBC, minimal WBC and plt 250 35 days Increases hematocrit 3% unit less risk for febrile reaction, which mainly results from WBC content Frozen red cells RBC , minimal WBC and plt 175 24 hrs at -80⁰ 72 hrs at 4 ⁰ c Increases hematocrit 3% unit Platelet Plt 50 5 dats at 22⁰c Increases the platelet count by 5000 -10000 /mm 3 unit gives a minimum of 6 units Fresh frozen plasma Coagulation factors including fibrinogen 250 1 year at – 18 ⁰c 24 hrs at 4 ⁰ c Increases fibrinogen 10 mg/dl /unit give one unit after every 4 units of packed RBCs Cryo-precipitate Factor Vlll Von willebrands fibrinogen 40 1 year at – 18⁰ c 4 hrs at 4 ⁰ c Increases fibrinogen 10 mg/dl/unit : give a minimum of 10 units when there is hypofibrinogenemia

B) Dilutional Coagulopathy This can result if large amounts of intravenous fluids or blood ( 5 units or more ) are given This leads to dilution of coagulation factors and tendency to bleeding So a unit of FFP should be given for every 5 units of transfused blood D) Dextran infusion Excessive infusion with dextran may cause coagulopathy Dextran forms a fibrinogen – dextran complex leading to Hypofibrinogenemia and prevents aggregation of platelets

Notes 1. Fibrin degration products prevent formation offibrin clots , inhibit myomt. Contraction, cause toxic myocarditis, so increase bleed. And shock 2. Cryoprecipitate. Obtained from fresh frozen plasma bywarming to 4 c. It supplies fibrinogen factor VIII, and von willebrand factor. Each unit of cryoprecipitate raises thefibrinogen level about 10 mg/ dl 3. One unit of platelets rasis the platelet count by 10, 000/mm 3 4. Causes of Hypofibrinogenemia include causes of DIC , dilutional coagulopathy and dextran infusion

5. Dextran innterferes with crossmatching 6. Platelet concentrate contains some red blood cells and so needsto be ABOand. Rhesus compatible 7. Measurement of antithrombin IIIis the most sensitive test to diagnose DIC

Amniotic fluid embolism (AFE) (Anaphylactoid syndrome of pregnancy) • INCIDENCE 1 in 8000 to 1 in 80, 000 deliveries. • AETIOLOGY 1. The exact cause is unknown 2. It may be due to sudden escape of a large volume of amniotic fluid into the maternal venous circulation after rupture of membranes during labour 3. The amniotic fluid emboli will block the pulmonary arterioles and capillaries leading to pulmonary hypertension and hypoxia

4. Hypoxia leads to left ventricular heart failure and death 5. The condition tends to occur in labours with strong uterine contractions and when the uterus is excessively stimulated by oxytocin infusion or prostaglandin. 6. It may also occur during (C. S) and after rupture of the uterus 7. It is suggested that AFE is an immune response caused by exposure of the mother to amniotic fluid leading to anaphylatic reaction and shock 8. It usually occurs at the time of delivery , but has been reporter after amniocentesis and therapeutic abortion 9. also uterine hyperstimulation is found in less than 10%of patients

• Clinical picture 1. The patient develops sudden severe dyspnea 2. Cyanosis and cough with frothy and Blood stained sputum 3. This is immediately followed by apnea and profound shock 4. Chest pain is unusual 5. Death occurs in 25% of cases within one hour and the majrity who survive will develop disseminated intravascular coagulation (DIC) with bleeding from the genital tract and from all sites of trauma 6. The amniotic fluid contains thromboplastin which leads to intravascular coagulation

Diagnosis -It is based on clinical picture and laboratory studies which include : -Complete blood count , Arterial blood gases , Coagulation profile and it often diagnosed by exclusion -Diagnosis in the past was confirmed by postmortem examination to detect the presence of amniotic fluid elements as – A- fetal squamous cells – B- lanugo hair – C- vernix caseosa – D- meconium in pulmonary arterioles and capillaries However only 50 -70% of patients dying from this syndrome have this finding Also amniotic fluid elements in the pulmonary circulation are detected in normal pregnancy

• Differntial diagnosis This includes 1. Pulmonary thromboembolism 2. Aspiration pneumonia 3. Myocardial infarction 4. Septic shock 5. Other causes of sudden postpartum collapse

• Treatment 1. Oxygen is supplied by an endotracheal tube and mechanical ventilation 2. Treatment of shock: a) Blood volume expansion by colloids , crystalloids, or blood b) Pressor agents such as dopamine or norepinephrine 3. Digitalis if there is left ventricular failure which is common 4. Treatment of pulmonary oedema which is common (70%) by diuretics as frusemide ( lasix)

5. Corticosteroids may help as the syndrome may be immune mediated ( hydrocortisone 500 mg IV every 6 hours until the patient recovers) 6. When DIC occurs it is treated properly 7. If maternal cardiac arrest occurs before delivery , the fetus is delivered immediately by forceps or by CS if conditions are not favourable for vaginal delivery. Prognosis 1. Maternal mortality is about 60% 2. Many of the women ( 75%) who survive will suffer neurlolgical damage secondary to hypoxia 3. Neonatal survival is about 75% with 50% of those surviving will suffer neurological problems

THANK YOU
- Slides: 33