Coagulation Cascade Ahmad Shihada Silmi Msc FIBMS IUG

Coagulation Cascade Ahmad Shihada Silmi Msc, FIBMS IUG Faculty of Science Medical Technology Dept

Coagulation o o o A set of reactions in which blood is transformed from a liquid to a gel Coagulation follows intrinsic and extrinsic pathways The final three steps of this series of reactions are: n n n Prothrombin activator is formed Prothrombin is converted into thrombin Thrombin catalyzes the joining of fibrinogen into a fibrin mesh
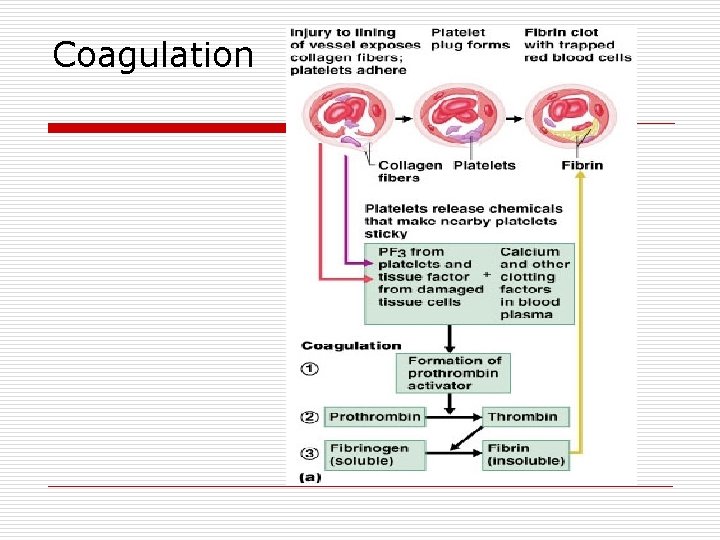
Coagulation
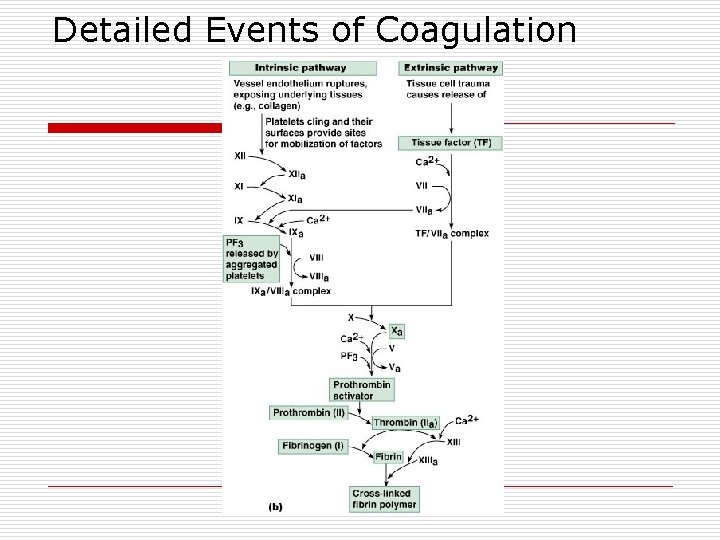
Detailed Events of Coagulation

Coagulation Phase 1: Two Pathways to Prothrombin Activator o o May be initiated by either the intrinsic or extrinsic pathway n Triggered by tissue-damaging events n Involves a series of procoagulants n Each pathway cascades toward factor X Once factor X has been activated, it complexes with calcium ions, PF 3, and factor V to form prothrombin activator

Coagulation Phase 2: Pathway to Thrombin o Prothrombin activator catalyzes the transformation of prothrombin to the active enzyme thrombin

Coagulation Phase 3: Common Pathways to the Fibrin Mesh o o Thrombin catalyzes the polymerization of fibrinogen into fibrin Insoluble fibrin strands form the structural basis of a clot Fibrin causes plasma to become a gel-like trap Fibrin in the presence of calcium ions activates factor XIII that: n Cross-links fibrin n Strengthens and stabilizes the clot

Fibrinogen Fibrin

Fibrinogen Thrombin Fibrin
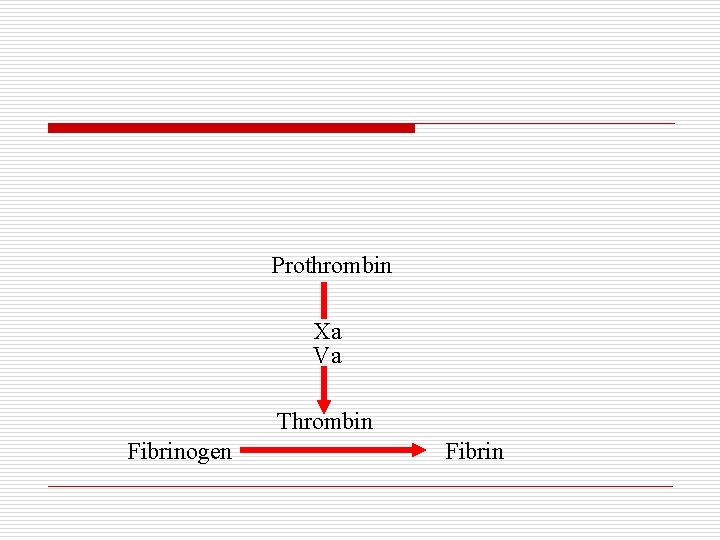
Prothrombin Xa Va Thrombin Fibrinogen Fibrin
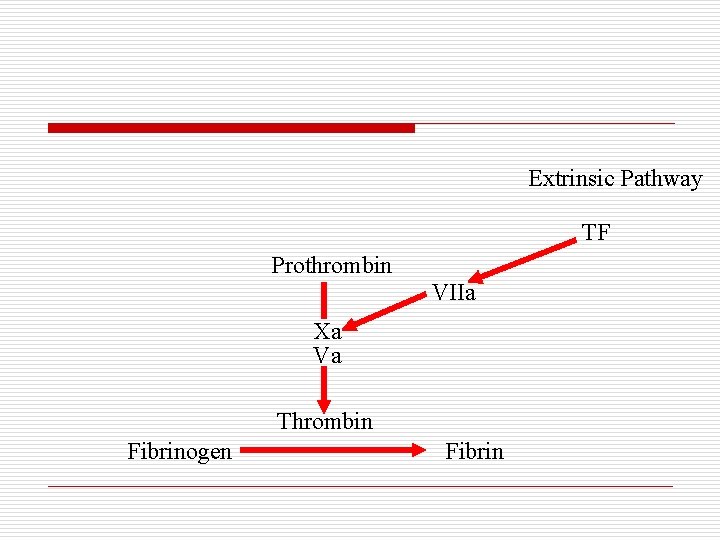
Extrinsic Pathway TF Prothrombin VIIa Xa Va Thrombin Fibrinogen Fibrin
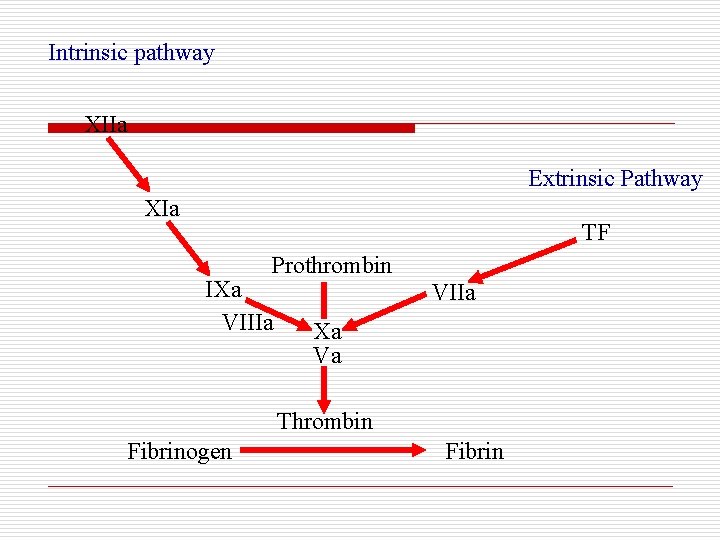
Intrinsic pathway XIIa Extrinsic Pathway XIa TF Prothrombin IXa VIIIa VIIa Xa Va Thrombin Fibrinogen Fibrin
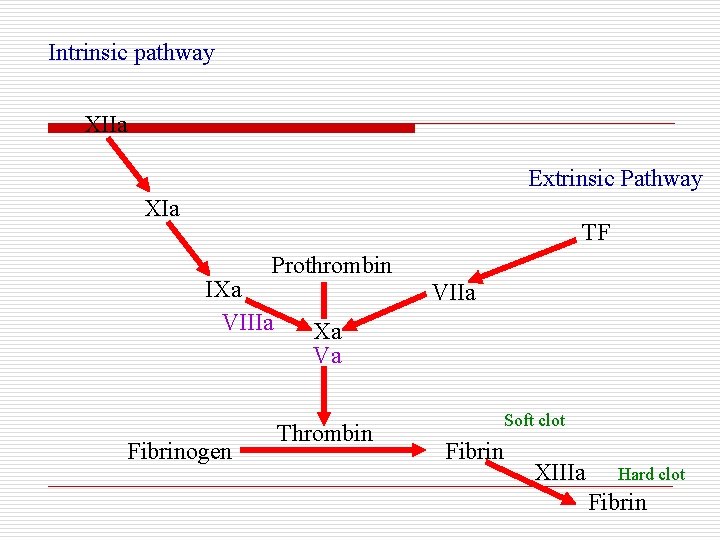
Intrinsic pathway XIIa Extrinsic Pathway XIa TF Prothrombin IXa VIIIa Fibrinogen VIIa Xa Va Thrombin Soft clot Fibrin XIIIa Hard clot Fibrin
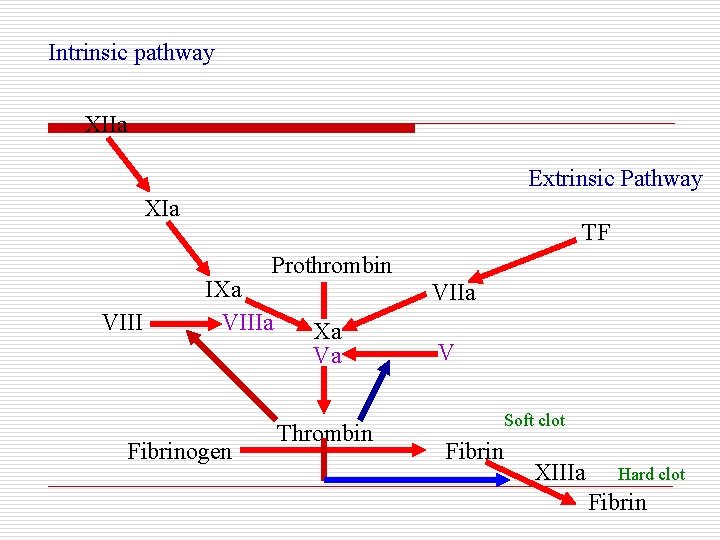
Intrinsic pathway XIIa Extrinsic Pathway XIa TF Prothrombin VIII IXa VIIIa Fibrinogen VIIa Xa Va Thrombin V Soft clot Fibrin XIIIa Hard clot Fibrin

The intrinsic pathway begins with the contact factors, factor XII, HMWK, and prekallikrein, which activates factor XI. Activated factor XI can then activate factor IX, which then acts with its cofactor, factor VIII, to form tenase complex on a phospholipid surface to activate factor X. Activated factor X then combines with its cofactor, factor V, to form the prothrombinase complex on a phospholipid surface, converting prothrombin to thrombin.
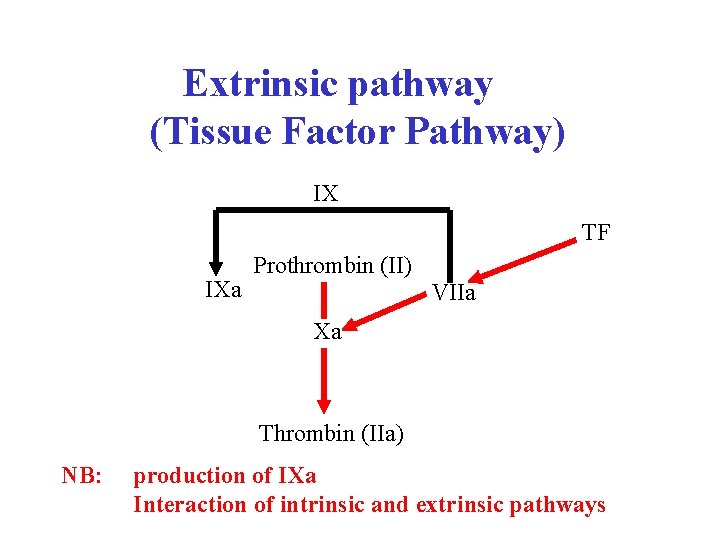
Extrinsic pathway (Tissue Factor Pathway) IX TF IXa Prothrombin (II) VIIa Xa Thrombin (IIa) NB: production of IXa Interaction of intrinsic and extrinsic pathways
Tissue Factor Pathway Inhibitor • • Kunitz-type protease inhibitor (kringles) 34 and 41 k. D forms in plasma (C-term truncation) Directly inhibits Xa Inhibits VIIa-TF complex in a [Xa]-dependent manner • Bound to LDL, HDL and Lp (a) • ~10% present in platelets (endothelium also)
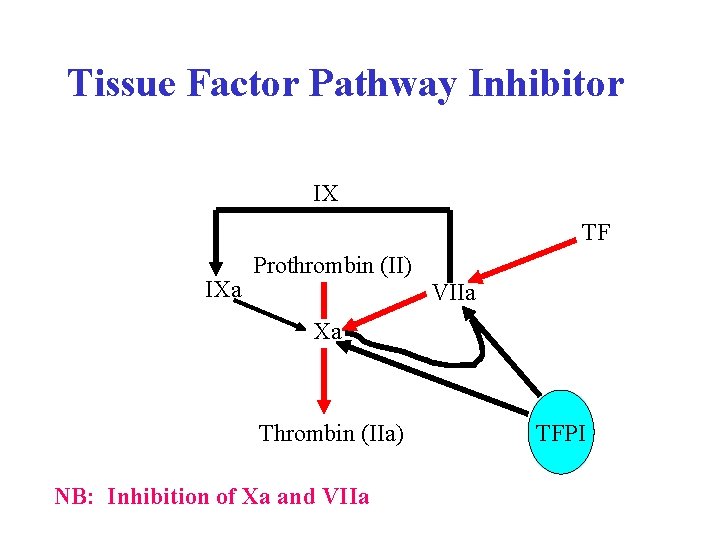
Tissue Factor Pathway Inhibitor IX TF IXa Prothrombin (II) VIIa Xa Thrombin (IIa) NB: Inhibition of Xa and VIIa TFI TFPI

Tissue Factor Pathway Net result: Production of IXa Production of small amounts of thrombin (IIa) NB: no/little fibrin formed!

Tissue Factor Pathway • VIIa forms as usual via binding of VII to TF • VIIa activates some X Xa • Xa converts a small amt of prothrombin to thrombin; this thrombin is used to produce small amts of VIIIa and Va • As the conc of TF-VIIa-Xa-thrombin increases, Tissue Factor Pathway Inhibitor inactivates this complex stopping further production of thrombin. • New: VIIa also activates IX IXa (Key to new scheme) • IXa, with VIIIa (produced as above), produces Xa; this Xa with Va (produced as above) produces new thrombin; this thrombin produces more VIIIa and Va and now we get lots of thrombin and fibrin!
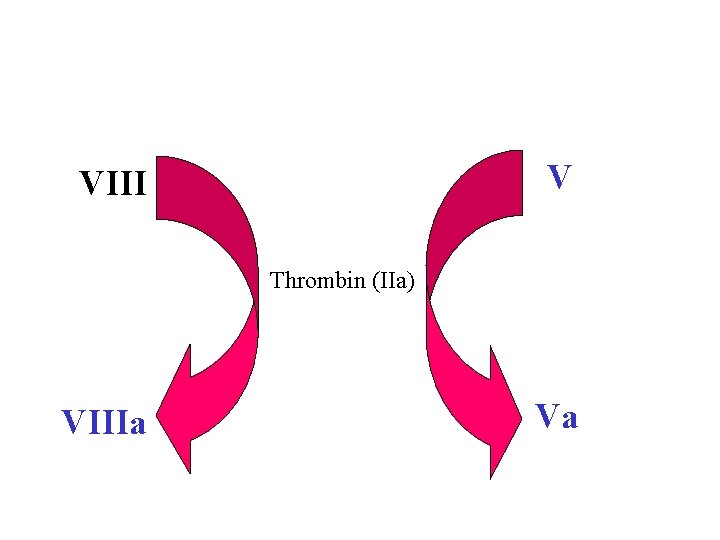
V VIII Thrombin (IIa) VIIIa Va
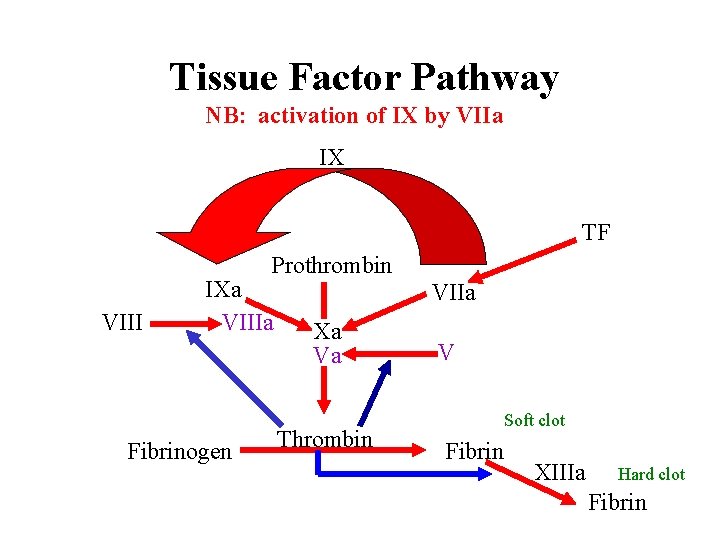
Tissue Factor Pathway NB: activation of IX by VIIa IX TF Prothrombin VIII IXa VIIIa Fibrinogen VIIa Xa Va Thrombin V Soft clot Fibrin XIIIa Hard clot Fibrin

However, The coagulation “cascade” doesn’t explain how blood clots in vivo. Several evidence support that coagulation cascade goes in different way § Cerebal matter injection led to large clot in the heart (Dupuy experement). § Deficiency of factor X, HMWK, PK are without haemorrhagic symptoms. § Prothrombin time reagent, this brought into question that patient lacking factor VIII & IX showed normal clotting time. § All these have led to

Current Concept of coagulation

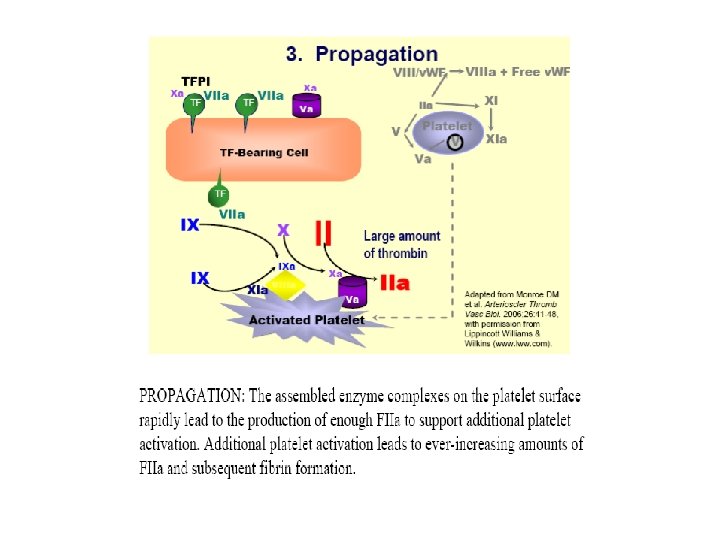
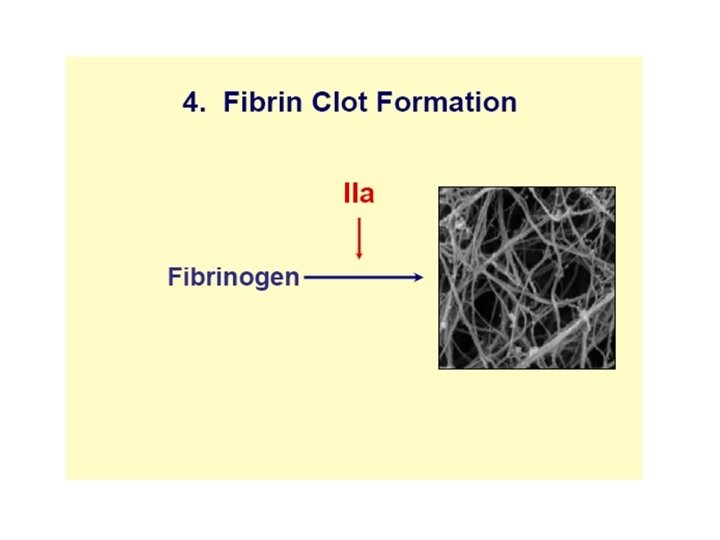

Summary

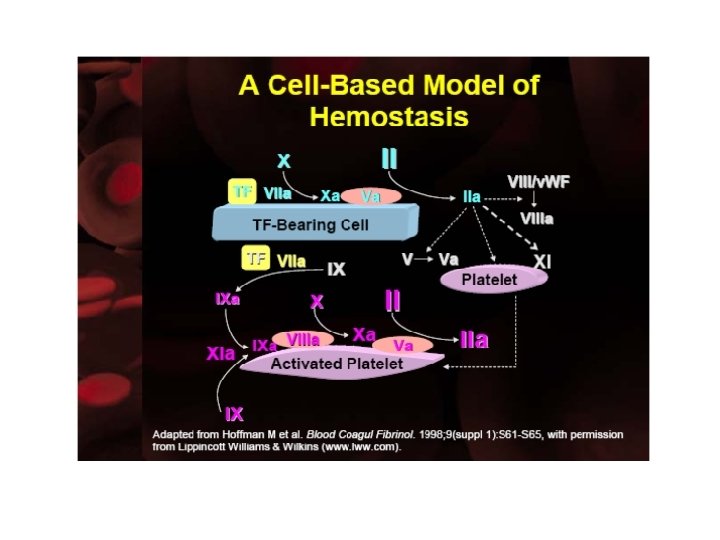

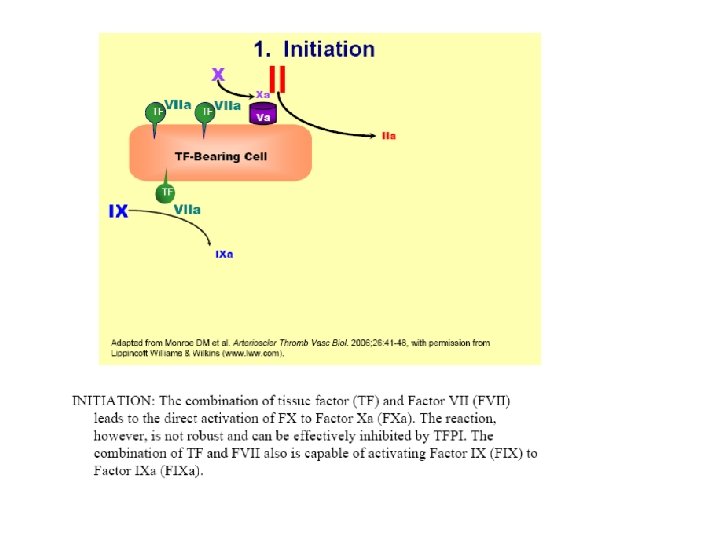
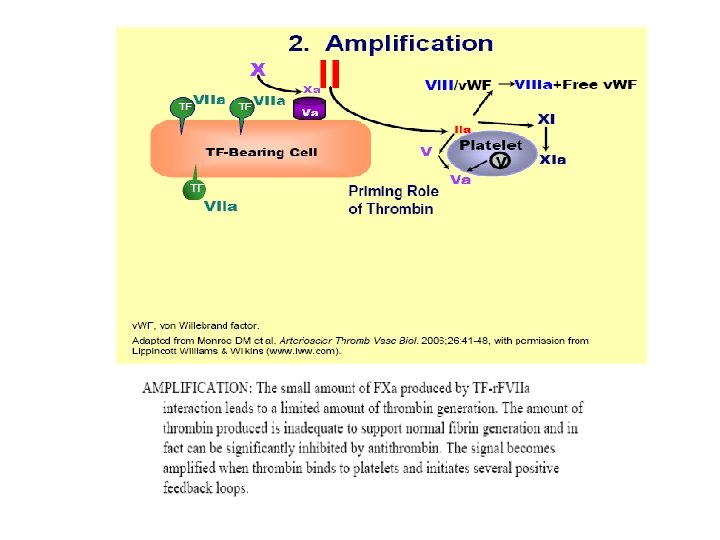
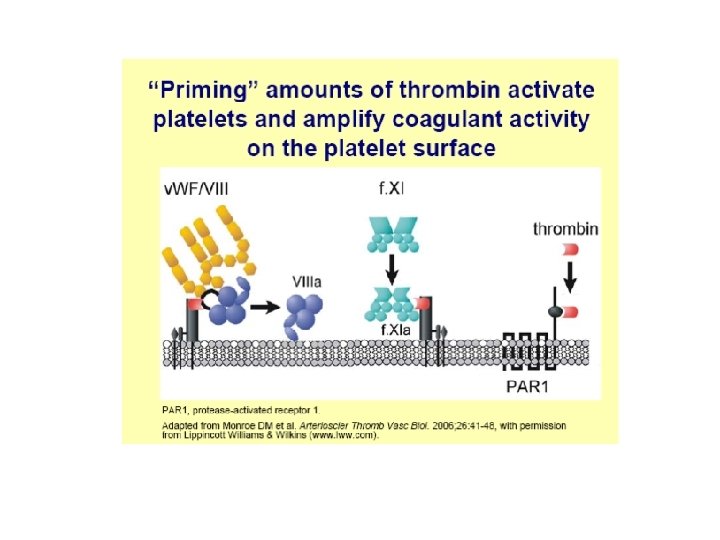
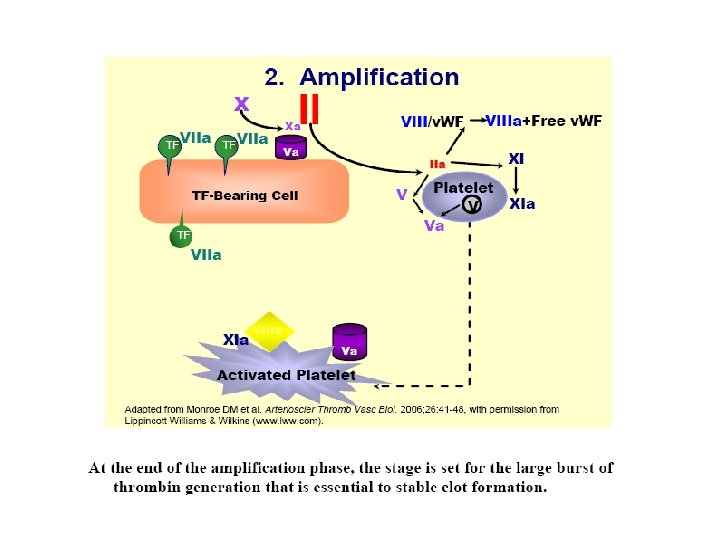
This coagulation cascade suggests that there are “intrinsic” and “extrinsic” pathways in the coagulation process, but we must modify our definition of these pathways a little. The “extrinsic” or tissue factor pathway consists of the FVIIa/TF complex and the FXa/Va complex. It operates on the TF-bearing cell to initiate the coagulation process. Its components are shown in aqua in the slide. The “intrinsic” pathway does not include FXII or its cofactors PK and HMWK, which do not appear to be necessary for hemostasis. Thus, we can consider the “intrinsic” pathway to consist of FXI(a), the FIXa/VIIIa complex, and the FXa/Va complex. It operates on the platelet surface during the propagation phase to generate a burst of thrombin. Its components are shown in hot pink in the slide. Thus, both of these pathways are needed for hemostasis, because they operate on different surfaces and play distinct roles.

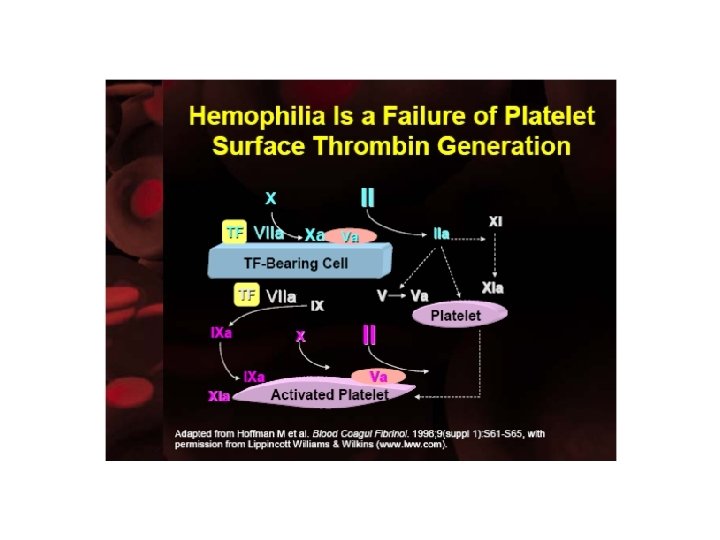

This described above makes it clear what goes wrong in Hemophilia: Platelet adhesion at a site of injury occurs normally in hemophilia, as does production of FXa and small amounts of thrombin on TF-bearing cells during the initiation stage of coagulation. However, platelet surface FX activation by FIXa/FVIIIa is abolished and, therefore, platelet surface thrombin generation fails. The FVIIa/TF complex cannot effectively substitute for the FIXa/VIIIa complex, because it produces FXa on the “wrong” surface.


Naturally Occurring Inhibitors Ahmad Sh. Silmi Msc, FIBMS IUG Faculty of Science Medical Technology Dept

Coagulation Inhibitors The activity of coagulation system must be attenuated. – Numerous inhibitors are found in blood. Coagulation is controlled by three types of actions. – Inhibition of converting enzymes (e. g. , AT III, C 1 esterase inhibitor, a 2 macroglobulin, a 2 -antiplasmin, a 1 -antitrypsin, HC-II). • Act on one or more of the converting enzymes (activated factors). • AT III-heparin pathway: major system - 80% of the thrombin inhibitory action in plasma. – Destruction of protein cofactors (e. g. , TM-PC-PS system). • TM-PC-PS system degrades cofactors V & VIII: C, inhibiting prothrombinase and tenase complexes, respectively. – Blocking receptor availability needed for complex formation (e. g. , Tissue factor pathway inhibitor (TFPI) and annexin V).

Antithrombin III (AT III) • naturally-occuring anticoagulant • binds to factors IXa, XIa, XIIa (slow) • accelerated by heparin manyfold Implication: Heparin has almost NO anticoagulant action without AT III
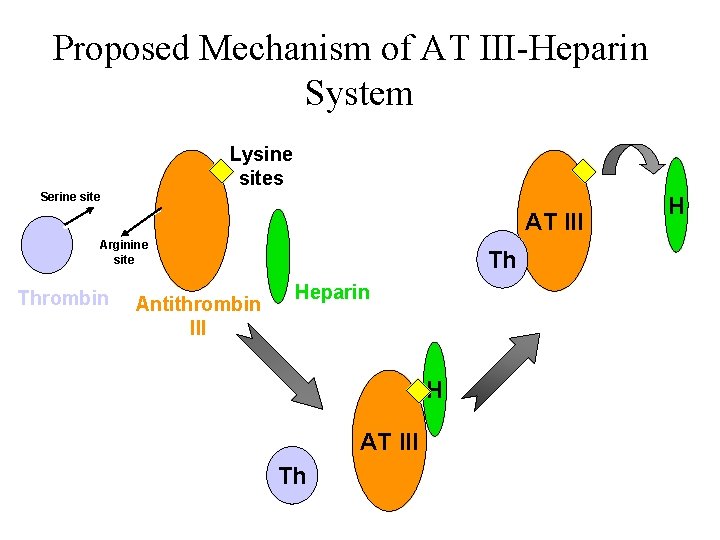
Proposed Mechanism of AT III-Heparin System Lysine sites Serine site AT III Arginine site Thrombin Antithrombin III Th Heparin H AT III Th H
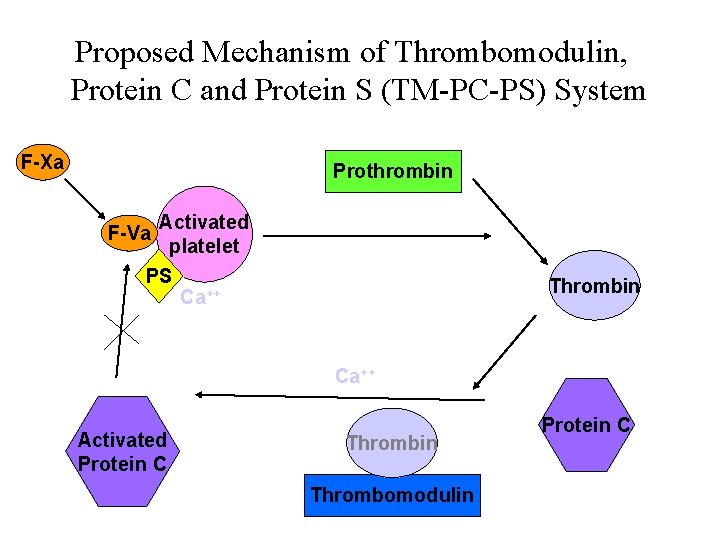
Proposed Mechanism of Thrombomodulin, Protein C and Protein S (TM-PC-PS) System F-Xa Prothrombin F-Va Activated platelet Thrombin Ca++ x PS Ca++ Activated Protein C Thrombin Thrombomodulin Protein C
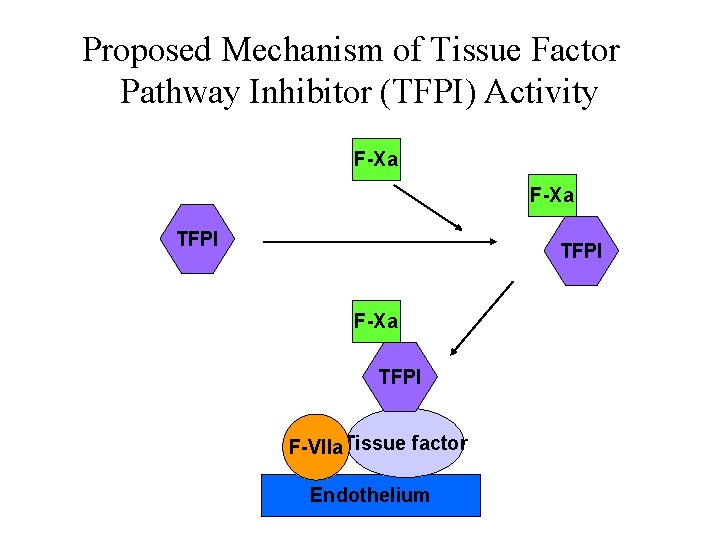
Proposed Mechanism of Tissue Factor Pathway Inhibitor (TFPI) Activity F-Xa TFPI F-VIIa. Tissue factor Endothelium
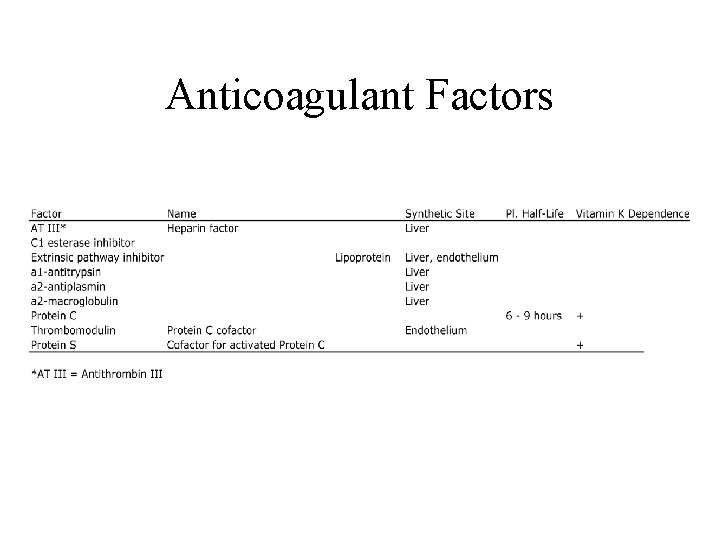
Anticoagulant Factors
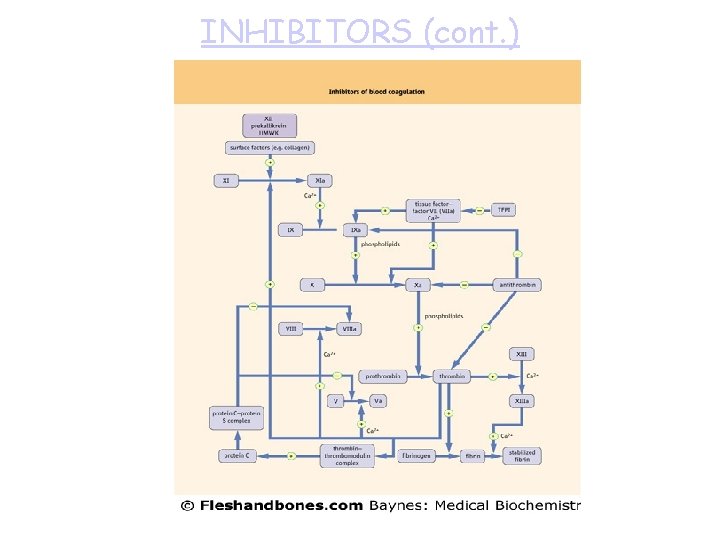
INHIBITORS (cont. )
- Slides: 47