CMS Certified Community Behavioral Health Clinic Cost Report

CMS Certified Community Behavioral Health Clinic Cost Report Part I – 1/12/16 2: 30 - 4 ET Part II – 1/14/16 1: 30 - 3 ET

Webinar Agenda I. Welcome II. Goals III. Introduction to Cost Report IV. Review of Cost Report Tabs V. CMS Tools for States VI. Schedule of PPS TA webinar sessions VII. Questions 2

Goals of this PPS Technical Assistance Webinar • Review the CMS CCBHC cost report • Introduce crosswalk tool for use when a state submits own cost report 3

Introduction to the CMS CCBHC Cost Report • A state may elect to require clinics to use the CMS CCBHC cost report or a state-developed template that adheres to Section 4 of the PPS Guidance: Cost Reporting and Documentation Requirements • The state must receive approval of its alternative cost report and demonstrate that it is as comprehensive as the CMS model by completing the cost report crosswalk presented with this webinar. 4

Who completes the CMS CCBHC Cost Report? • A CCBHC employee or consultant with: – Knowledge of accrual-based accounting – An understanding of Medicaid and Medicare cost principles – An understanding of how to enumerate visits for the selected PPS methodology • The CCBHC CEO, CFO, Director, or a direct delegate who certifies the cost report 5

Cost Report Updates • Cost Report was made available for public comment on September 14, 2015 in the Federal Register • Changes incorporated into the final version: – Added cost-to-charge ratio approach to allocate costs between population groups – Included anticipated visits and charges for CCBHC services not provided prior to DY 1 – Clarified that reported clinic hours exclude the hours of the mobile crisis team – Removed names of supervisory personnel and their hours – Clarified that NPIs should be reported only for practitioners with numbers available 6

Required Cost Report Data • Costs, visits and charges associated with demonstration services provided to all clinic users, not just Medicaid beneficiaries • Data to support cost allocation methods • For PPS-2, data about special populations 7
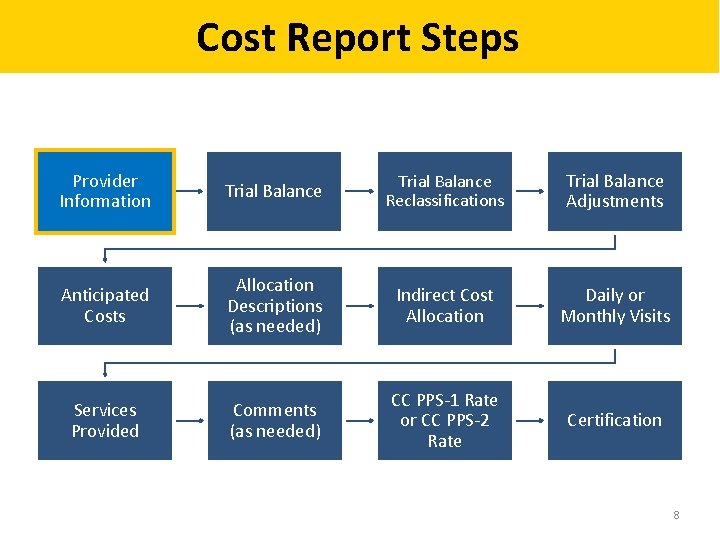
Cost Report Steps Provider Information Trial Balance Reclassifications Trial Balance Adjustments Anticipated Costs Allocation Descriptions (as needed) Indirect Cost Allocation Daily or Monthly Visits Services Provided Comments (as needed) CC PPS-1 Rate or CC PPS-2 Rate Certification 8

Provider Information Tab • Used to gather basic information about the CCBHC: – The provider number, clinic hours, clinic type, etc. Ensures all satellite sites are established prior to April 1, 2013 and reported on tab if filing consolidated report. • Part I is for single sites or central office information; Part II is if the entity is filing a consolidated report and should be completed for every additional site. – 9
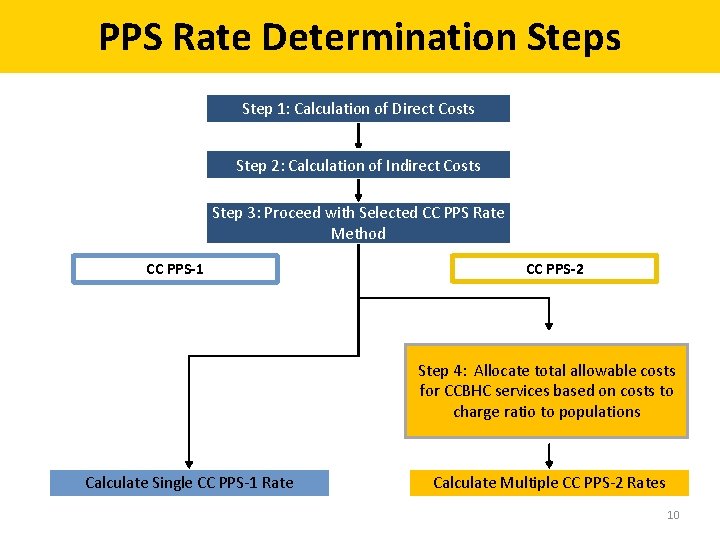
PPS Rate Determination Steps Step 1: Calculation of Direct Costs Step 2: Calculation of Indirect Costs Step 3: Proceed with Selected CC PPS Rate Method CC PPS-1 CC PPS-2 Step 4: Allocate total allowable costs for CCBHC services based on costs to charge ratio to populations Calculate Single CC PPS-1 Rate Calculate Multiple CC PPS-2 Rates 10
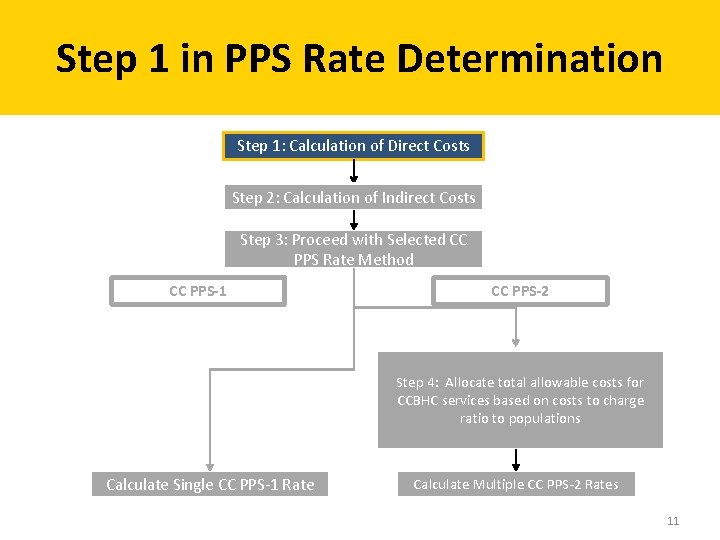
Step 1 in PPS Rate Determination Step 1: Calculation of Direct Costs Step 2: Calculation of Indirect Costs Step 3: Proceed with Selected CC PPS Rate Method CC PPS-1 CC PPS-2 Step 4: Allocate total allowable costs for CCBHC services based on costs to charge ratio to populations Calculate Single CC PPS-1 Rate Calculate Multiple CC PPS-2 Rates 11
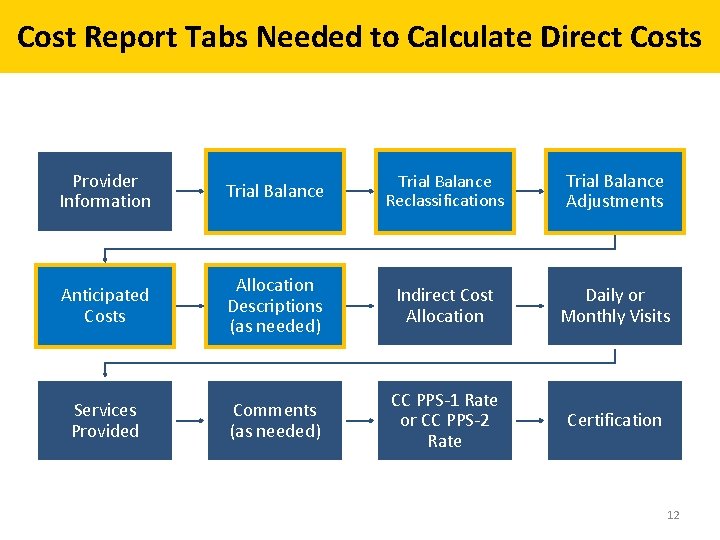
Cost Report Tabs Needed to Calculate Direct Costs Provider Information Trial Balance Reclassifications Trial Balance Adjustments Anticipated Costs Allocation Descriptions (as needed) Indirect Cost Allocation Daily or Monthly Visits Services Provided Comments (as needed) CC PPS-1 Rate or CC PPS-2 Rate Certification 12

Step 1: Calculation of Direct Costs Trial Balance tab Compensation & Other + Trial Balance Reclassification tab Trial Balance Adjustments tab Reclassifications + Adjustments + Anticipated Costs tab Anticipated Costs = Allocation Descriptions tab for any allocations of direct costs Direct Costs (DC) 13

Allowable Cost - Considerations • Allowable cost is identified using requirements in 45 CFR § 75 Uniform Administrative Requirements, Cost Principles, and Audit Requirements for HHS Awards and 42 CFR § 413 Principles of Reasonable Cost Reimbursement • Costs may be adjusted or reclassified between direct CCBHC, direct non-CCBHC, and indirect costs (overhead) • Indirect costs are allocated to direct costs using the Indirect Cost Allocation tab • When allocations are used, they should be described in the Allocation Descriptions tab 14

Trial Balance Tab • Used to gather allowable cost information and classify it as direct CCBHC, direct non-CCBHC, or indirect cost • The tab: – Captures total costs – Shows reclassifications – Shows adjustments – Shows anticipated costs by cost center and cost type – Should be reconcilable to the trial balance for the financial statements 15

Trial Balance Reclassifications Tab • Use to reclassify the expenses listed on the Trial Balance tab • Reclassify costs where expenses are applicable to more than one expense category • Allocate direct costs using this tab, but provide a narrative explaining the method used to allocate direct costs in the Direct Cost Allocation tab 16

Trial Balance Adjustments Tab • Use to adjust the expenses listed on Trial Balance tab • Types of items to be entered on this table include those items: – Which constitute recovery of expenses through grants, sales, charges, fees, etc. – Needed to adjust expenses in accordance with cost principles described in 45 CFR § 75 • An example of other costs not allowed are certain costs associated with related parties, such as rent expense. Rent expense from a related party must be adjusted to the depreciable amount for the building, as per 45 CFR 75. 465. 17

Anticipated Costs Tab • Use to add or change the expenses listed on Trial Balance tab to allow for services not previously offered but required as a CCBHC • Estimate changes in cost and FTEs providing CCBHC services 18

Allocation Descriptions Tab • The purpose of this tab is to expedite cost report review and avoid last minute questioning of costs. • This tab allows the clinic to describe in detail the calculations and methods to support the allocation of direct and indirect costs • Data reported in this tab should support allocations in the Trial Balance, Reclassifications, Adjustments, and CC PPS-2 tabs 19
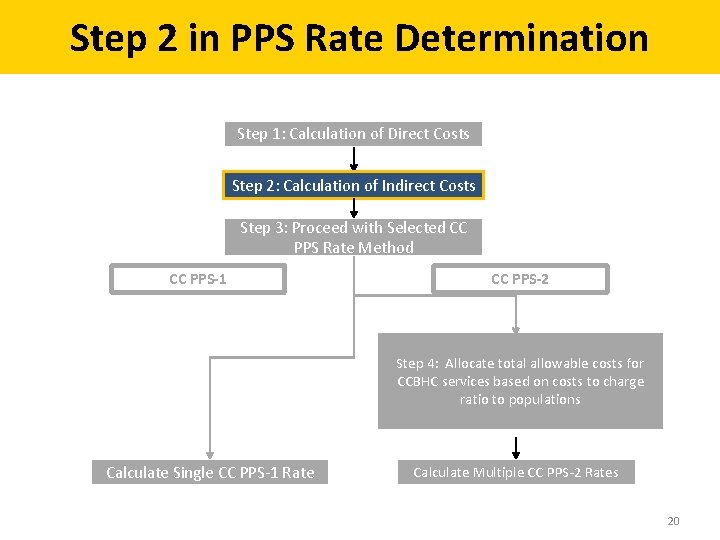
Step 2 in PPS Rate Determination Step 1: Calculation of Direct Costs Step 2: Calculation of Indirect Costs Step 3: Proceed with Selected CC PPS Rate Method CC PPS-1 CC PPS-2 Step 4: Allocate total allowable costs for CCBHC services based on costs to charge ratio to populations Calculate Single CC PPS-1 Rate Calculate Multiple CC PPS-2 Rates 20
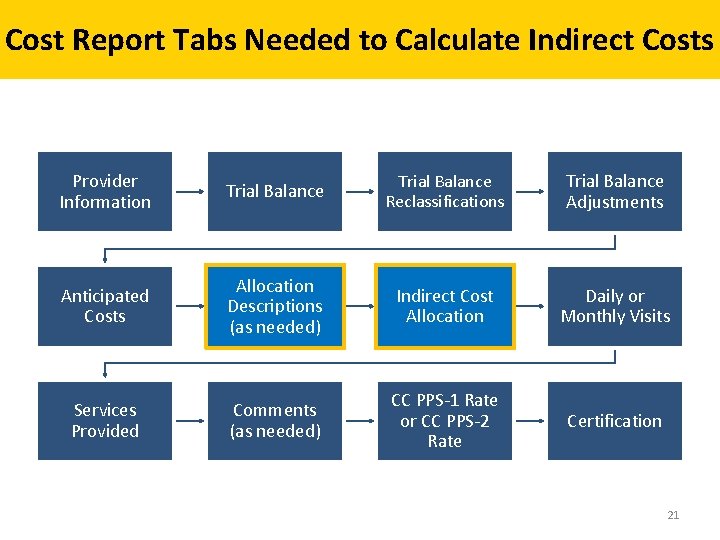
Cost Report Tabs Needed to Calculate Indirect Costs Provider Information Trial Balance Reclassifications Trial Balance Adjustments Anticipated Costs Allocation Descriptions (as needed) Indirect Cost Allocation Daily or Monthly Visits Services Provided Comments (as needed) CC PPS-1 Rate or CC PPS-2 Rate Certification 21

Step 2: Calculation of Indirect Costs Indirect Cost Allocation tab Federally Approved Rate OR 10 % Federal Minimum Rate OR Proportionate Allocation by % of DC OR Custom Allocation Method = Allocation Descriptions for any allocations of IDC Indirect Costs (IDC) (Allocated to CCBHC Services) 22
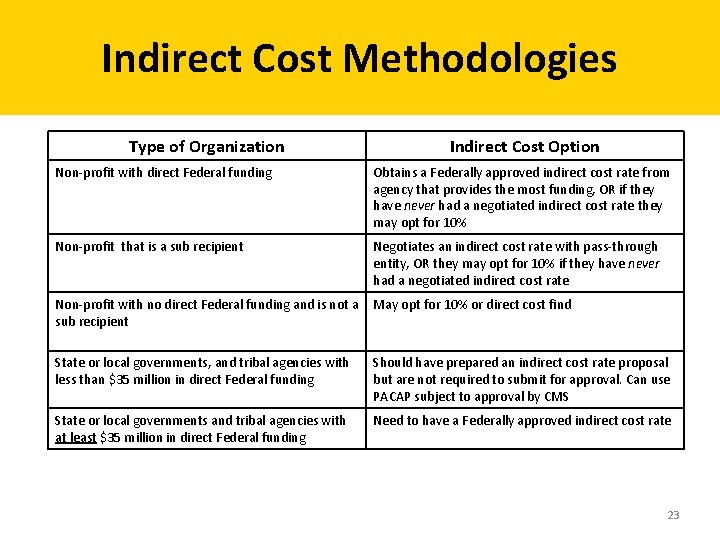
Indirect Cost Methodologies Type of Organization Indirect Cost Option Non-profit with direct Federal funding Obtains a Federally approved indirect cost rate from agency that provides the most funding, OR if they have never had a negotiated indirect cost rate they may opt for 10% Non-profit that is a sub recipient Negotiates an indirect cost rate with pass-through entity, OR they may opt for 10% if they have never had a negotiated indirect cost rate Non-profit with no direct Federal funding and is not a sub recipient May opt for 10% or direct cost find State or local governments, and tribal agencies with less than $35 million in direct Federal funding Should have prepared an indirect cost rate proposal but are not required to submit for approval. Can use PACAP subject to approval by CMS State or local governments and tribal agencies with at least $35 million in direct Federal funding Need to have a Federally approved indirect cost rate 23

Indirect Cost Allocation Tab • Use to identify the method used for calculating allocable indirect costs to CCBHC services • The worksheet can be used for the following methods of allocation: – Federally approved indirect cost rate by a cognizant agency – Minimum rate for qualifying entities (10%) – Proportionate allocation by percentage of direct costs – Other, where the entity must provide a description and justification of the allocation method 24
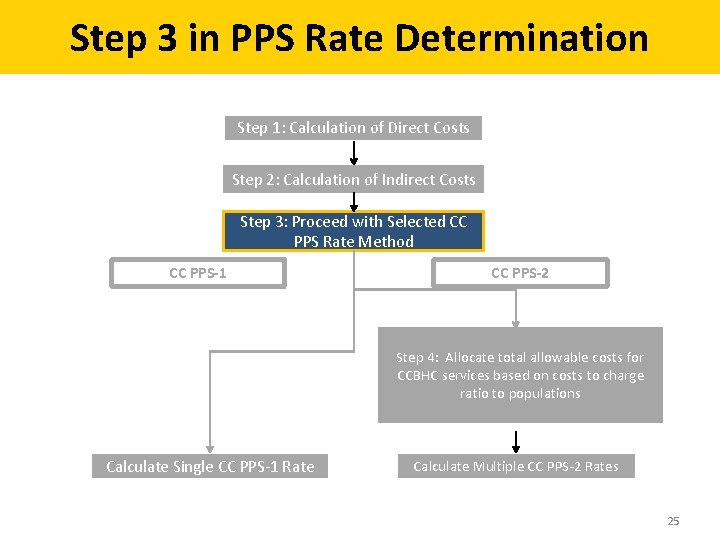
Step 3 in PPS Rate Determination Step 1: Calculation of Direct Costs Step 2: Calculation of Indirect Costs Step 3: Proceed with Selected CC PPS Rate Method CC PPS-1 CC PPS-2 Step 4: Allocate total allowable costs for CCBHC services based on costs to charge ratio to populations Calculate Single CC PPS-1 Rate Calculate Multiple CC PPS-2 Rates 25
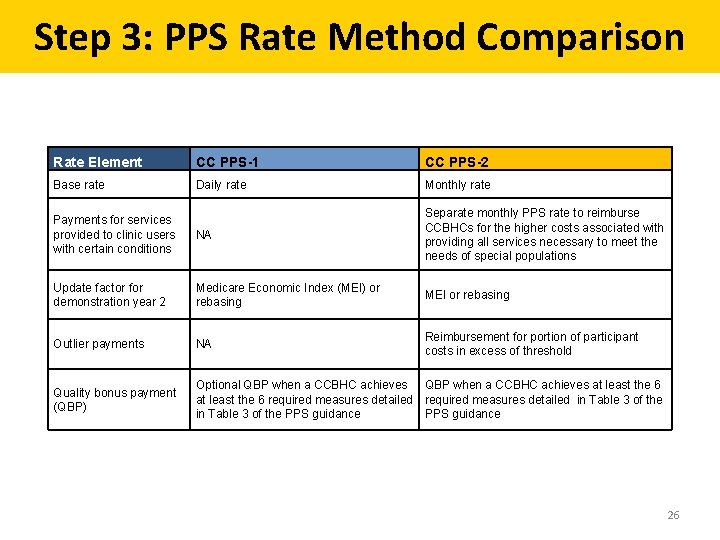
Step 3: PPS Rate Method Comparison Rate Element CC PPS-1 CC PPS-2 Base rate Daily rate Monthly rate Payments for services provided to clinic users with certain conditions NA Separate monthly PPS rate to reimburse CCBHCs for the higher costs associated with providing all services necessary to meet the needs of special populations Update factor for demonstration year 2 Medicare Economic Index (MEI) or rebasing MEI or rebasing Outlier payments NA Reimbursement for portion of participant costs in excess of threshold Quality bonus payment (QBP) Optional QBP when a CCBHC achieves at least the 6 required measures detailed in Table 3 of the PPS guidance 26
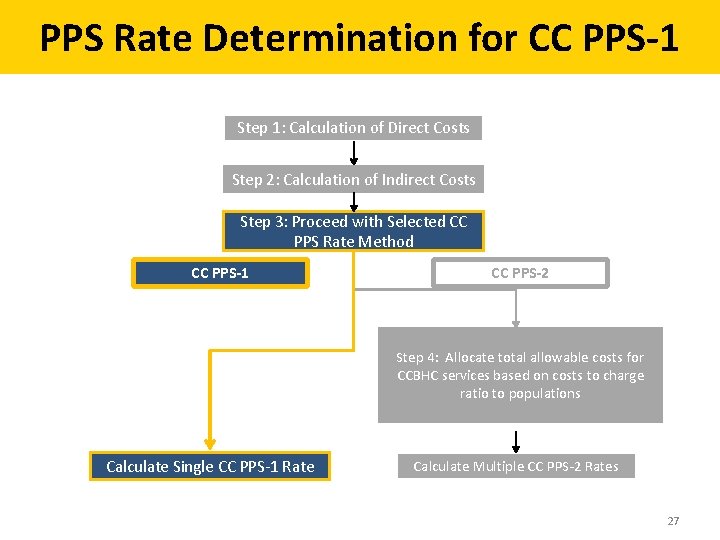
PPS Rate Determination for CC PPS-1 Step 1: Calculation of Direct Costs Step 2: Calculation of Indirect Costs Step 3: Proceed with Selected CC PPS Rate Method CC PPS-1 CC PPS-2 Step 4: Allocate total allowable costs for CCBHC services based on costs to charge ratio to populations Calculate Single CC PPS-1 Rate Calculate Multiple CC PPS-2 Rates 27
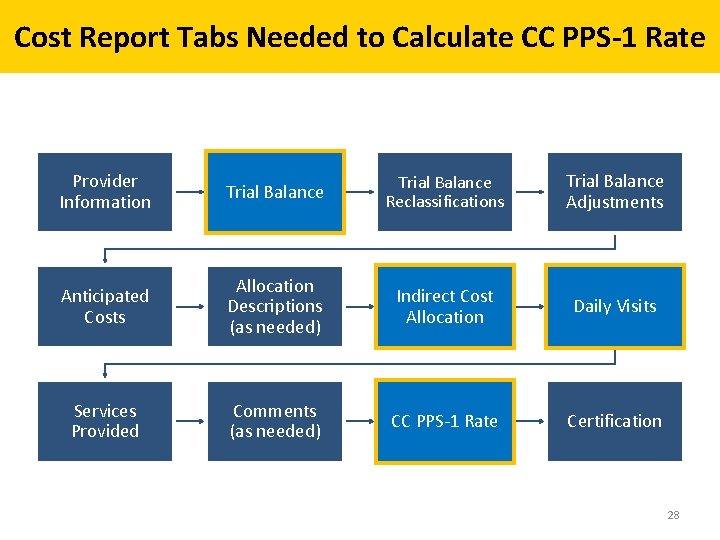
Cost Report Tabs Needed to Calculate CC PPS-1 Rate Provider Information Trial Balance Reclassifications Trial Balance Adjustments Anticipated Costs Allocation Descriptions (as needed) Indirect Cost Allocation Daily Visits Services Provided Comments (as needed) CC PPS-1 Rate Certification 28

CC PPS-1 Rate Tab • Use to determine the all-inclusive CCBHC payment rate per daily visit for the reporting period for states selecting the CC PPS-1 rate method. • Contains two parts: ‒ Part I – Determination of Total Allowable Cost Applicable to CCBHC ‒ Part II – Determination of CC PPS-1 Rate • Requires input of MEI to trend data – Market basket data: https: //www. cms. gov/Research-Statistics. Data-and-Systems/Statistics-Trends-and. Reports/Medicare. Program. Rates. Stats/Market. Basket. Data. html 29

Daily Visits Tab for CC-PPS 1 • Use this tab to report the total annual number of daily CCBHC visits delivered to all clinic users that receive demonstration services; includes daily visits of DCOs* and services delivered to non Medicaid beneficiaries. * A DCO is an entity that is not under the direct supervision of the CCBHC but is engaged in a formal relationship with the CCBHC and delivers services under the same requirements as the CCBHC. 30
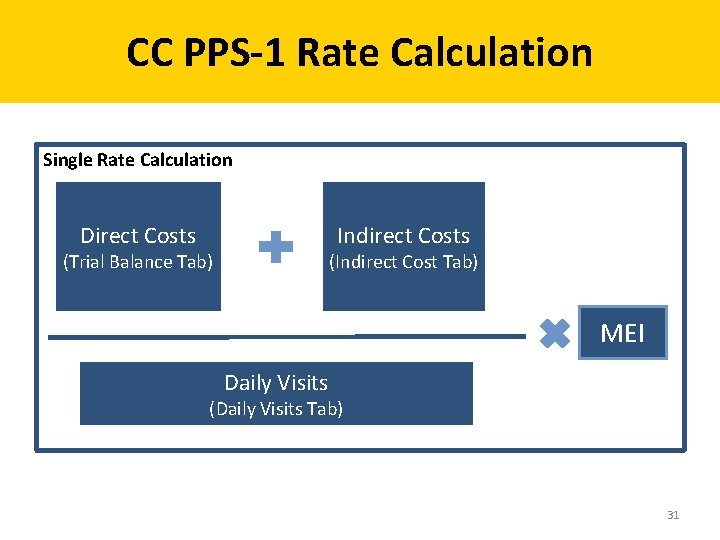
CC PPS-1 Rate Calculation Single Rate Calculation Indirect Costs Direct Costs (Indirect Cost Tab) (Trial Balance Tab) MEI Daily Visits (Daily Visits Tab) 31
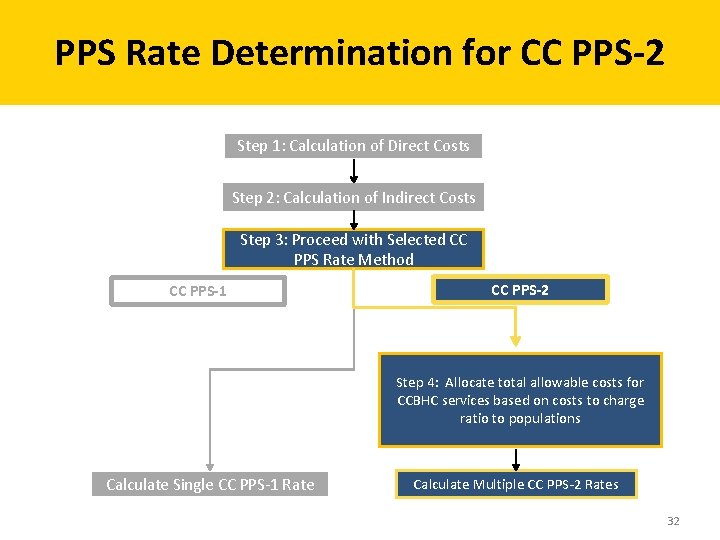
PPS Rate Determination for CC PPS-2 Step 1: Calculation of Direct Costs Step 2: Calculation of Indirect Costs Step 3: Proceed with Selected CC PPS Rate Method CC PPS-1 CC PPS-2 Step 4: Allocate total allowable costs for CCBHC services based on costs to charge ratio to populations Calculate Single CC PPS-1 Rate Calculate Multiple CC PPS-2 Rates 32

Cost Report Tabs Needed to Calculate CC PPS-2 Rate Provider Information Trial Balance Reclassifications Trial Balance Adjustments Anticipated Costs Allocation Descriptions (as needed) Indirect Cost Allocation Monthly Visits Services Provided Comments (as needed) CC PPS-2 Rate Certification 33

CC PPS-2 Rate Tab • Requires costs to be allocated by population group • Costs must be allocated to the categories identified in the Monthly Visits tab • Requires input of the MEI to trend cost data 34
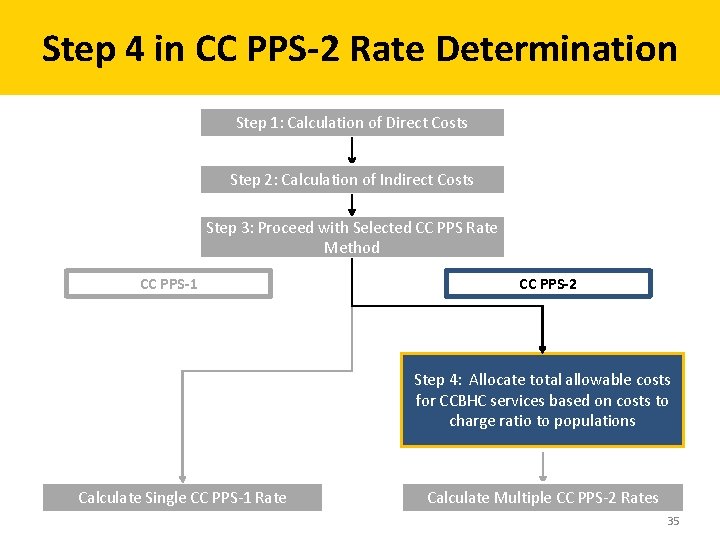
Step 4 in CC PPS-2 Rate Determination Step 1: Calculation of Direct Costs Step 2: Calculation of Indirect Costs Step 3: Proceed with Selected CC PPS Rate Method CC PPS-1 CC PPS-2 Step 4: Allocate total allowable costs for CCBHC services based on costs to charge ratio to populations Calculate Single CC PPS-1 Rate Calculate Multiple CC PPS-2 Rates 35
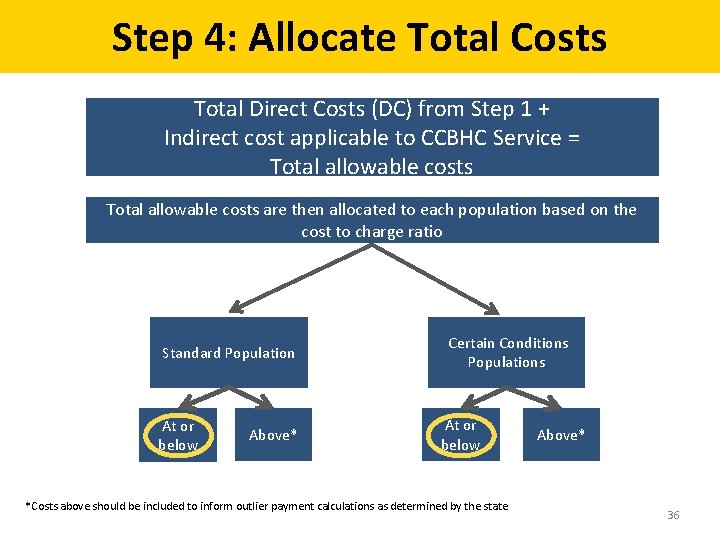
Step 4: Allocate Total Costs Total Direct Costs (DC) from Step 1 + Indirect cost applicable to CCBHC Service = Total allowable costs are then allocated to each population based on the cost to charge ratio Standard Population At or below Above* Certain Conditions Populations At or below *Costs above should be included to inform outlier payment calculations as determined by the state Above* 36

Monthly Visits Tab CC PPS-2 • Use this tab to report the total annual number of monthly CCBHC visits delivered to all clinic users that receive demonstration services; includes monthly visits of DCOs and services delivered to non Medicaid beneficiaries. • A clinic user’s monthly visit may not be counted in multiple population categories. • The count of monthly visits must include all clinic users who received demonstration services, not just Medicaid beneficiaries. 37
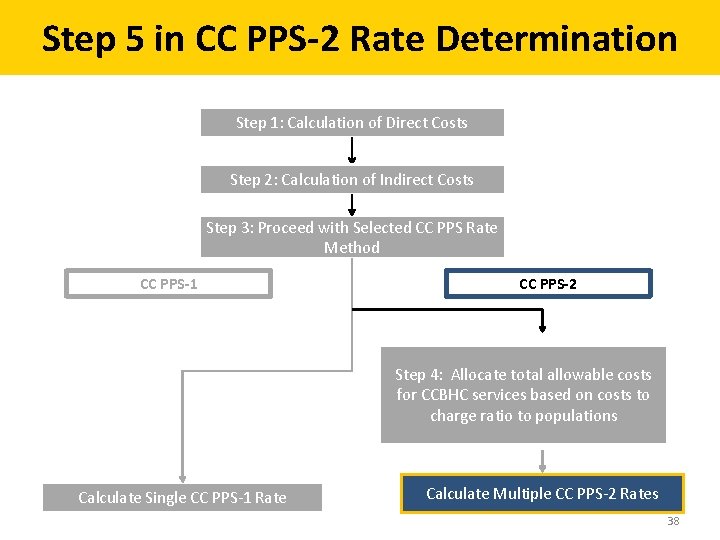
Step 5 in CC PPS-2 Rate Determination Step 1: Calculation of Direct Costs Step 2: Calculation of Indirect Costs Step 3: Proceed with Selected CC PPS Rate Method CC PPS-1 CC PPS-2 Step 4: Allocate total allowable costs for CCBHC services based on costs to charge ratio to populations Calculate Single CC PPS-1 Rate Calculate Multiple CC PPS-2 Rates 38
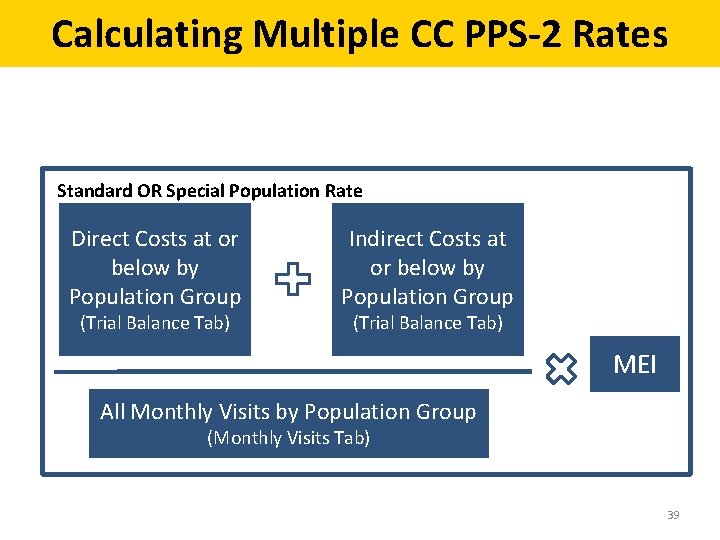
Calculating Multiple CC PPS-2 Rates Standard OR Special Population Rate Direct Costs at or below by Population Group (Trial Balance Tab) Indirect Costs at or below by Population Group (Trial Balance Tab) MEI All Monthly Visits by Population Group (Monthly Visits Tab) 39
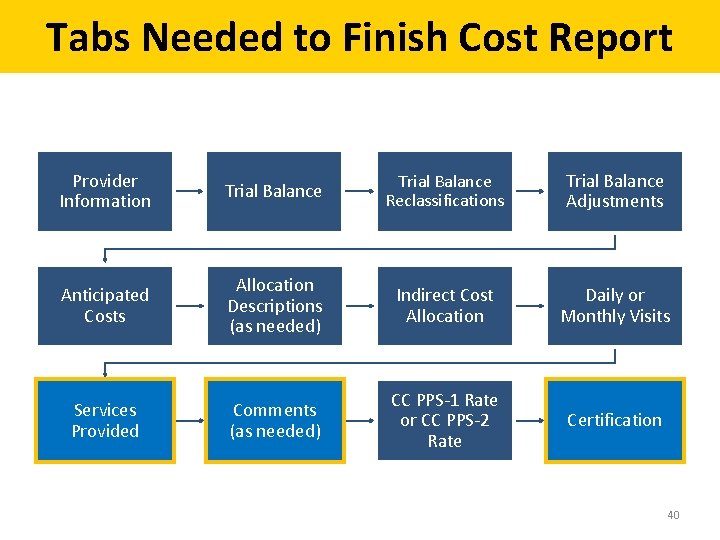
Tabs Needed to Finish Cost Report Provider Information Trial Balance Reclassifications Trial Balance Adjustments Anticipated Costs Allocation Descriptions (as needed) Indirect Cost Allocation Daily or Monthly Visits Services Provided Comments (as needed) CC PPS-1 Rate or CC PPS-2 Rate Certification 40

Services Provided, Comments, and Certification Tabs • Use the Services Provided tab to report the number of FTEs and the number of services provided for CCBHC services for each type of practitioner • Use the Comments tab to explain any cost anomalies, entries in “Other (specify)” lines in Trial Balance, Trial Balance Adjustments, Services Provided, and CC PPS-2 Rate tabs, or any other considerations the state should make regarding the expenses used to determine the payment rate • Cost reports must include certification from the CEO, CFO or an authorized delegate 41

Collaboration Tools • Mailboxes – CMS mailbox for PPS guidance-related questions: CCBHCDemonstration@cms. hhs. gov – CMS mailbox for Quality Based Payment-related questions: MACQuality. TA@cms. hhs. gov • 223 PPS TA Share. Point Site Link – Crosswalk template for State developed cost reports • Q&As posted at the 223 Landing Page on Medicaid. gov 42
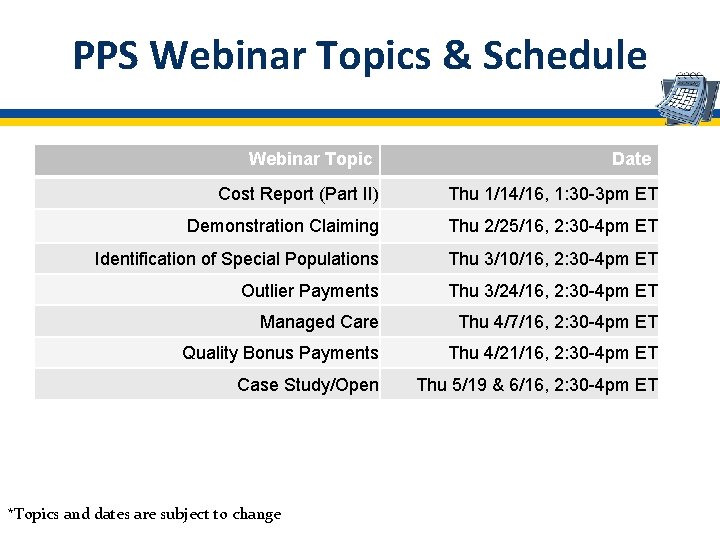

PPS Webinar Topics & Schedule Webinar Topic Date Cost Report (Part II) Thu 1/14/16, 1: 30 -3 pm ET Demonstration Claiming Thu 2/25/16, 2: 30 -4 pm ET Identification of Special Populations Thu 3/10/16, 2: 30 -4 pm ET Outlier Payments Thu 3/24/16, 2: 30 -4 pm ET Managed Care Thu 4/7/16, 2: 30 -4 pm ET Quality Bonus Payments Thu 4/21/16, 2: 30 -4 pm ET Case Study/Open Thu 5/19 & 6/16, 2: 30 -4 pm ET *Topics and dates are subject to change

Questions 44
- Slides: 44