Clinical Practice Guidelines Decompensated cirrhosis Presented by Hend

Clinical Practice Guidelines Decompensated cirrhosis Presented by : Hend naguib Ass. lecturer of Hepatology Internal Medicine

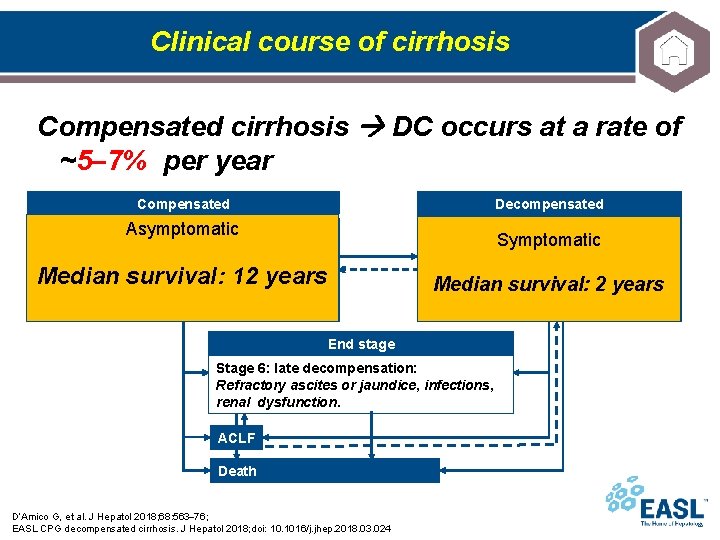
Clinical course of cirrhosis Compensated cirrhosis DC occurs at a rate of ~5– 7% per year Decompensated Compensated Stage 0: no varices, mild PH Asymptomatic LSM >15 and <20 or HVPG >5 and <10 mm. Hg Stage 3: Bleeding Symptomatic Stage 1: no varices, CSPH LSM ≥ 20 or HVPG ≥ 10 mm. Hg Median survival: 12 years Stage 2: varices (=CSPH) Stage 4: First non-bleeding decompensation Median survival: 2 years Stage 5: Second decompensating event End stage Stage 6: late decompensation: Refractory ascites or jaundice, infections, renal dysfunction. ACLF Death D’Amico G, et al. J Hepatol 2018; 68: 563 76; EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Overall management of DC AIM prevent progression NOT treat complications Two alternative approaches can be taken: • Suppress aetiological factor(s) • Target key factors in the pathogenesis

Suppression of aetiological factor(s) Recommendation In patients with DC the aetiological factor should be removed, particularly alcohol consumption and hepatitis B or C virus infection, as this strategy is associated with decreased risk of decompensation and increased survival. (II-2, 1). EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Treatment of key pathogenic factors • Several strategies have been evaluated: – Targeting microbiome abnormalities and bacterial translocation to improve the gut–liver axis (i. e. Rifaximin). – Treating the inflammatory state (i. e. Statins). – Targeting portal hypertension (i. e. β-blockers). – Enoxaparin appeared to delay the occurrence of hepatic decompensation. – Pentoxifylline treatment significantly reduced the risk of liver-related complications (HE, renal impairment , bacterial infection). Further clinical research is needed EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
Ascites

Ascites Most common complication ( 5– 10% )of patients • What is the impact ? ? – Impairs patient working and social life. – Frequently leads to hospitalization. – Poor prognosis (5 -year survival, 80% 30%). EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
prognosis • Development of ascites in patients with cirrhosis is associated with a poor prognosis – 1 -year mortality: 40% – 2 -year mortality: 50% Recommendation Since the development of grade 2 or 3 ascites in patients with cirrhosis is associated with reduced survival, LT should be considered as a potential treatment option II-2 EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Evaluation and Diagnosis – – History Physical examination Abdominal ultrasound Laboratory assessment : analysis of ascitic fluid • Cirrhosis is responsible for 80% of cases of ascites Grading of ascites* Grade 1 Mild ascites: only detectable by ultrasound examination Grade 2 Moderate ascites: manifest by moderate symmetrical distension of abdomen Grade 3 Large or gross ascites: provokes marked abdominal distension *Ascites recurring on ≥ 3 occasions within a 12 -month period despite dietary sodium restriction and adequate diuretic dosage are considered recurrent EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

When to do Diagnostic paracentesis ? ? -All patients with new-onset grade 2 or 3 ascites. -Patients hospitalized for worsening ascites or any complication of cirrhosis.

Evaluation and diagnosis Recommendation Neutrophil count >250 cells/µl denotes SBP (II-2; 1) Ascitic total protein <1. 5 g/dl higher risk of developing SBP (II-2; 1). SAAG should be calculated when the cause of ascites is not immediately evident. (II-2; 1). Cytology should be performed to differentiate malignancy-related from non-malignant ascites. (II-2; 1) Bedside inoculation blood culture bottles with 10 ml fluid each; SAAG ≥ 1. 1 g/dl indicates that portal hypertension is involved in ascites formation with an accuracy of about 97%

Management • Moderate ascites – Hospitalization not required – Correct sodium imbalance: sodium imbalance • Dietary salt restriction and increased renal excretion with diuretics. Recommendation Moderate restriction of sodium intake (80– 120 mmol/day, corresponding to 4. 6– 6. 9 g of salt) is recommendeds (I; 1) Extreme sodium restriction (<40 mmol/day) should be avoided ( development of diuretic-induced hyponatraemia and renal failure) (II-2; 1). Prolonged bed rest not recommendeds (III; 1) EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

secondary hyperaldosteronism • Which type of diuretic? ? ?

Diuretics • Mainstay of medical treatment are anti-mineralocorticoid drugs. Recommendation First episode of grade 2 ascites • Anti-mineralocorticoid drug alone 100 mg/day with stepwise increase every 72 hours to a maximum of 400 mg/day if no response to lower doses) (I; 1) patients who do not respond to anti-mineralocorticoids or develop hyperkalaemia, furosemide (from 40 mg/day with 40 stepwise increases to 160 mg/day) (I; 1) Long-standing or recurrent ascites • Combination of an anti-mineralocorticoid drug and furosemide(I; 1). Torasemide can be given for a weak response to furosemide(I; 2) Maximum weight loss: 0. 5 kg/day in patients without oedema, 1 kg/day in patients with oedema (II-2; 1) EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

First weeks of treatment patients should undergo frequent clinical and biochemical monitoring (I; 1)

considerations prior to initiating diuretics Diuretic therapy is generally not recommended in patients with persistent overt hepatic encephalopathy (III; 1)

Monitoring of patients receiving diuretics • Loop diuretics can lead to hyponatraemia , hypokalemia and hypomagnesemia. Muscle cramps Recommendation Discontinue severe hyponatraemia, AKI, worsening hepatic encephalopathy, or incapacitating muscle cramps(III; 1) Discontinue furosemide for severe hypokalaemia (<3 mmol/L ) Discontinue anti-mineralocorticoids for hyperkalaemia (>6 mmol/L) (III; 1) Albumin infusion are recommended in patients with muscle cramps(I; 1) * EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Management of Grade 3 ascites • Grade 3 or large ascites – LVP, is the treatment of choice. (I; 1) - Plasma volume expansion should be performed by albumin. infusion (8 g/L ascites). (I; 1) - After LVP, patients should receive the minimum dose of diuretics necessary to prevent re-accumulation of ascites. (I; 1) *Grade of evidence I, grade of recommendation 1 EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Contraindicated drugs Increase risk of renal impairment. Recommendation NSAIDs should not be used (II-2; 1) Angiotensin-converting enyzme inhibitors, angiotensin II antagonists(II-2; 1) Aminoglycosides are discouraged (increased risk of AKI). (II-2; 1) EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Refractory ascites: definition – “Ascites that cannot be mobilized or the early recurrence , (after LVP)which cannot be prevented by medical therapy” Refractory ascites Diuretic resistant lack of response to sodium restriction and diuretic treatment Diuretic intractable Development of diuretic-induced complications that preclude the use of an effective diuretic dosage Refractory ascites is associated with a poor prognosis Median survival around 6 months EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Refractory ascites: diagnostic criteria Diagnostic criteria Treatment Intensive diuretic therapy for at least 1 week duration and on a salt-restriction. Early Reappearance of grade 2 or 3 ascites within 4 ascites weeks of initial mobilization recurrence • HE: • Renal impairment: increase of serum creatinine to a value >2 mg/dl. Diuretic • Hyponatraemia: a decrease of serum sodium induced <125 mmol/L complicati • Hypo- or hyperkalaemia: a change in serum ons potassium to <3 mmol/L or >6 mmol/L despite appropriate measures • Incapacitating muscle cramps

Refractory ascites: management Recommendation Repeated LVP plus albumin (8 g/L of ascites removed) are recommended as first-line treatment for refractory ascites(I; 1). • High doses of NSBB should be avoided (i. e. propranolol >80 mg/day) (II-2; 1) • Carvedilol can not be recommended at present(I; 2) • Addition of midodrine to diuretic treatment cannot be recommended (III; 1) *See also section on gastrointestinal bleeding EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
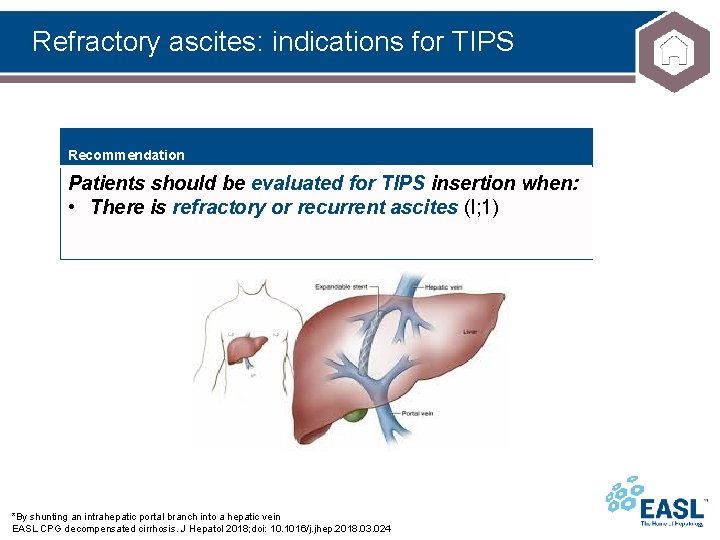
Refractory ascites: indications for TIPS Recommendation Patients should be evaluated for TIPS insertion when: • There is refractory or recurrent ascites (I; 1) *By shunting an intrahepatic portal branch into a hepatic vein EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
• Alfapump implantation in patients with refractory ascites not amenable to TIPS insertion is suggested in experienced centres. However, close patient monitoring is warranted because of the high risk of adverse events including renal dysfunction and technical difficulties (I; 2)
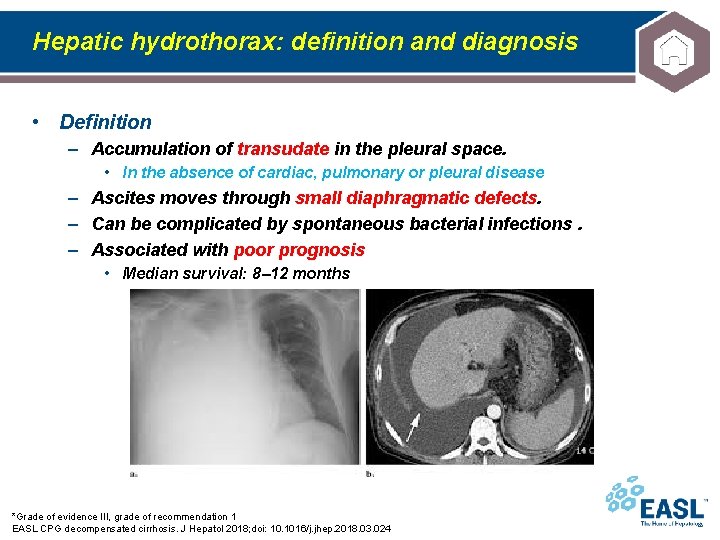
Hepatic hydrothorax: definition and diagnosis • Definition – Accumulation of transudate in the pleural space. • In the absence of cardiac, pulmonary or pleural disease – Ascites moves through small diaphragmatic defects. – Can be complicated by spontaneous bacterial infections. – Associated with poor prognosis • Median survival: 8 12 months *Grade of evidence III, grade of recommendation 1 EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Hepatic hydrothorax: treatment Treatment of ascites with diuretics and/or LVP. (III; 1) • Therapeutic thoracentesis is required to relieve dyspnoea. (III; 1) • What beyond diuretics and thoracentesis ? EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Hepatic hydrothorax Recommendation TIPS insertion for recurrent symptomatic hepatic hydrothorax is recommended(II-2; 1) Pleurodesis can be suggested to patients with refractory hepatic hydrothorax not amenable to LT or TIPS insertion (III; 1) Mesh repair of diaphragmatic defects(II-2; 2) EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Hyponatraemia Serum sodium concentration <130 mmol/L. • Hypo- and hypervolaemic hyponatraemia can occur. • Recommendation Patients with cirrhosis who develop hyponatraemia should be evaluated for LT(II-2, 1). Removal of the cause and administration of normal saline are recommended in the management of hypovolaemic hyponatraemia(III; 1) Fluid restriction to 1, 000 ml/day is recommended in the management of hypervolaemic hyponatraemia. (III; 1). EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

• Hypertonic saline should be limited to rare patients with life-threatening complications. It can be considered in patients with severe hyponatraemia who are expected to undergo LT within days. • Correction should be slow to avoid irreversible neurological sequelae. • Albumin can be administered but data are very limited. • vaptans should be limited to clinical trials.
Variceal haemorrhage

Variceal haemorrhage: pathophysiology and natural history • 70% of GI bleeding events result from VH Recommendation Patients with DC are at high risk and should have an Endoscopy to screen for varices. If OGD is performed, the presence, size and presence of red wale marks should be reported In patients without varices in whom aetiological factor persists and/or remain decompensated, screening OGD should be repeated yearly. EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Variceal haemorrhage: prevention and treatment Recommendation Primary prophylaxis for detection of high-risk varices. (small varices with red signs, small varices in Child C patients and medium or large varices irrespective of Child class) Patients with small varices with red wale marks or Child–Pugh C should be treated with NSBBs Patients with medium–large varices should be treated with either NSBBs or EBL • Choice of treatment can be based on local resources and expertise, patient preference, contraindications and AEs • NSBBs could be preferred for lowering portal pressure, they also exert other potential beneficial effects NSBBs equally effective EBL

NSBBS Ascites is not a contraindication for NSBBs. (propranolol and nadolol) • The use of carvedilol can not be recommended • Caution in cases of severe or refractory ascites • progressive hypotension<90 • bleeding, sepsis , • SBP , AKI, hyponatremia After recovery, reinstatement of NSBBs can be attempted

Is the concept of titration of NSBBs will be a target heart rate of 50– 55 bpm? ? ?

Prevention of variceal rebleeding(secondery prophylaxis) NSBBs and EBL in combination Monotherapy • Covered TIPS placement is recommended in patients who continue to be intolerant to NSBBs *Provided that there are no absolute contraindications EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
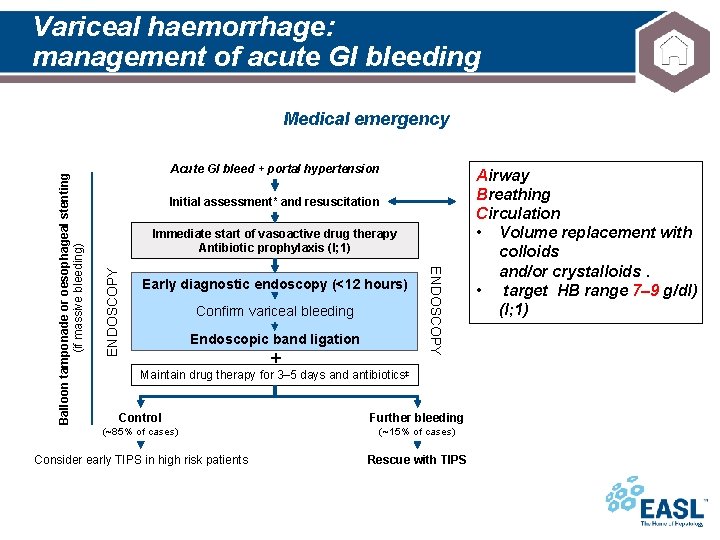
Variceal haemorrhage: management of acute GI bleeding Acute GI bleed + portal hypertension Initial assessment* and resuscitation ENDOSCOPY Immediate start of vasoactive drug therapy Antibiotic prophylaxis (I; 1) Early diagnostic endoscopy (<12 hours) Confirm variceal bleeding Endoscopic band ligation + ENDOSCOPY Balloon tamponade or oesophageal stenting (if massive bleeding) Medical emergency Maintain drug therapy for 3– 5 days and antibiotics‡ Control Further bleeding (~85% of cases) (~15% of cases) Consider early TIPS in high risk patients Rescue with TIPS Airway Breathing Circulation • Volume replacement with colloids and/or crystalloids. • target HB range 7– 9 g/dl) (I; 1)

Terlipressin is 2 mg/4 h during the first 48 h, followed by 1 mg/4 h thereafter. • Somatostatin is a continuous infusion of 250 µg/h (that can be increased up to 500 µg/h) with an initial bolus of 250 µg. • Octreotide is a continuous infusion of 50 µg/h with an initial bolus of 50 µg. • Ceftriaxone (1 g/24 h) for up to seven days

Acute variceal haemorrhage: treatment • Early covered TIPS (placed within 24– 72 hours) can be suggested for child–Pugh class C with score <14. • PPI after EBL may reduce the size of post-banding. β-blockers should be avoided during the acute bleeding episode EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

persistent bleeding!!!? ?

Management of persistent bleeding -TIPS should be used as the rescue therapy of choice in cases of persistent bleeding or early re-bleeding. -Balloon tamponade should be used in case of uncontrolled bleeding as a temporary ‘‘bridge” (max 24 hours) EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
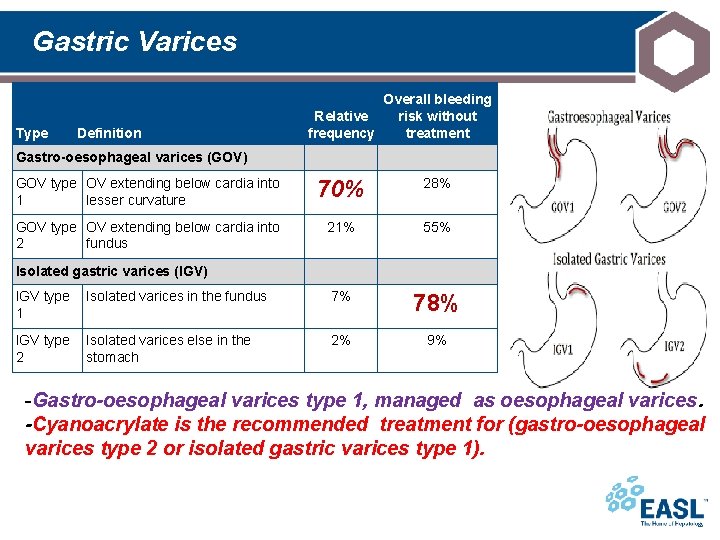
Gastric Varices Type Definition Overall bleeding risk without Relative frequency treatment Gastro-oesophageal varices (GOV) GOV type OV extending below cardia into 1 lesser curvature 70% 28% GOV type OV extending below cardia into 2 fundus 21% 55% Isolated gastric varices (IGV) IGV type 1 Isolated varices in the fundus 7% 78% IGV type 2 Isolated varices else in the stomach 2% 9% -Gastro-oesophageal varices type 1, managed as oesophageal varices. -Cyanoacrylate is the recommended treatment for (gastro-oesophageal varices type 2 or isolated gastric varices type 1).

Portal hypertension gastropathy Recommendation NSBB and iron supplementation and/or blood transfusion, are recommended as first-line therapy for chronic haemorrhage from PHG Acute PHG bleeding may be treated with somatostatin analogues or terlipressin. EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
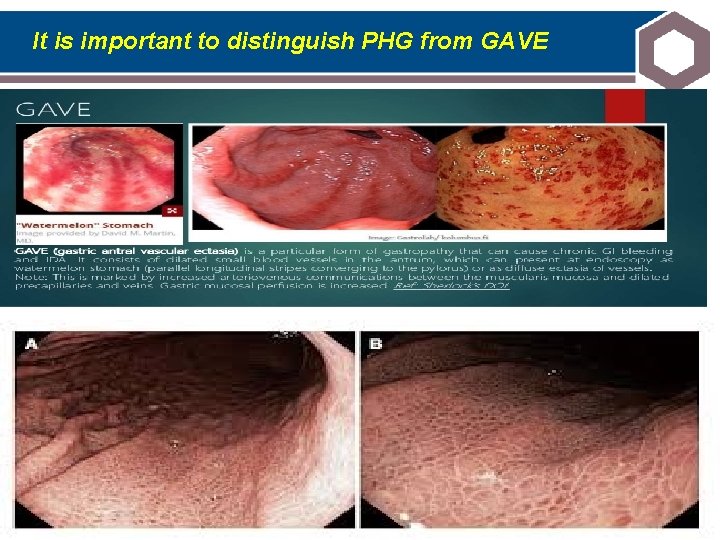
It is important to distinguish PHG from GAVE


Spontaneous bacterial peritonitis –DEFINITION Definition: bacterial infection of ascitic fluid without any intra-abdominal surgically treatable source of infection. –Prevalence : all patients with cirrhosis and ascites are at risk. –Prognosis : mortality exceeded 90% when first described. EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Diagnosis? ? – Signs/symptoms of peritonitis: abdominal pain, tenderness, vomiting or diarrhoea, ileus – Signs of systemic inflammation: hyper- or hypothermia, chills, altered WBC count – Worsening liver function, HE, shock, renal impairment, GI bleeding However: SPB may be asymptomatic, particularly in outpatients EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Spontaneous bacterial peritonitis: diagnosis Diagnosis is based on diagnostic paracentesis Recommendation SBP diagnosed by a neutrophil count in ascitic fluid >250/mm 3. Ascitic fluid culture positivity is not a prerequisite for SBP diagnosis. (negative 60%) is done to guide for antibiotic. EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Management of SBP • Empirical IV antibiotics should be started immediately following diagnosis Thirdgeneration cephalosporins 1 st line ( I, 1). Antibiotic resistance Piperacillin/tazobactam, Carbapenem • At least 5– 7 days • Check efficacy for second paracentesis after 48 hours at least 25%) reduction in leucocyte count.
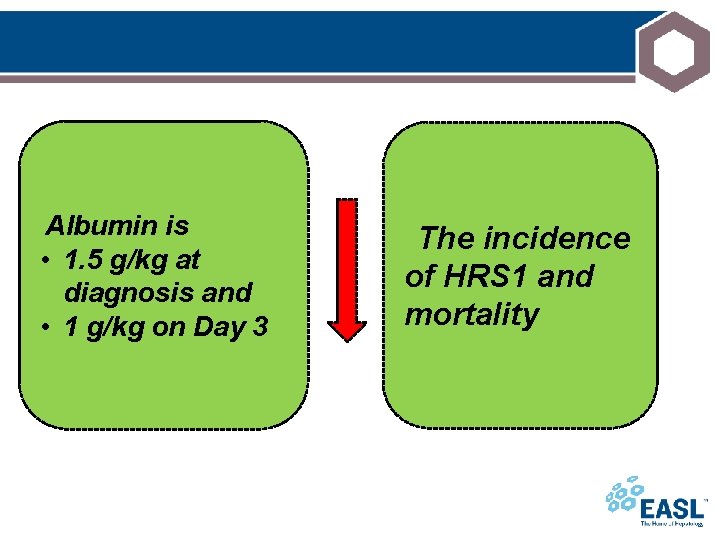
Albumin is • 1. 5 g/kg at diagnosis and • 1 g/kg on Day 3 The incidence of HRS 1 and mortality

Primary prophylaxis of SBP • Primary prophylaxsis with norfloxacin (400 mg/day) is recommended in patients with: • Child–Pugh score ≥ 9 and serum bilirubin level ≥ 3 mg/dl. • Ascitic fluid protein lower than 15 g/L 1. Wiest R, et al. Gut 2012; 61: 297– 310; EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Secondary prophylaxis In patients who survive an episode of SBP, the recurrence rate at 1 year is approximately 70% • Prophylactic norfloxacin (400 mg/day, orally) is recommended in patients who recover from an episode of SBP. • PPIs may increase the risk for the development of SBP, their use should be restricted to those with a clear indication. 1. Rimola A, et al. J Hepatol 2000; 32: 142– 53; EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Management of other infections • Non-SBP infections, as well as SBP, are known as common precipitating factors for ACLF. • C reactive protein and procalcitonin can be used for detecting infection • High bacterial resistance to antibiotics, carbapenem alone or in combination with other antibiotics should be preferred. • Routine use of albumin not infections other than SBP recommended in *Carbapenem alone or in combination with other antibiotics proved to be superior to third-generation cephalosporins in healthcare-associated infections other than SBP EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
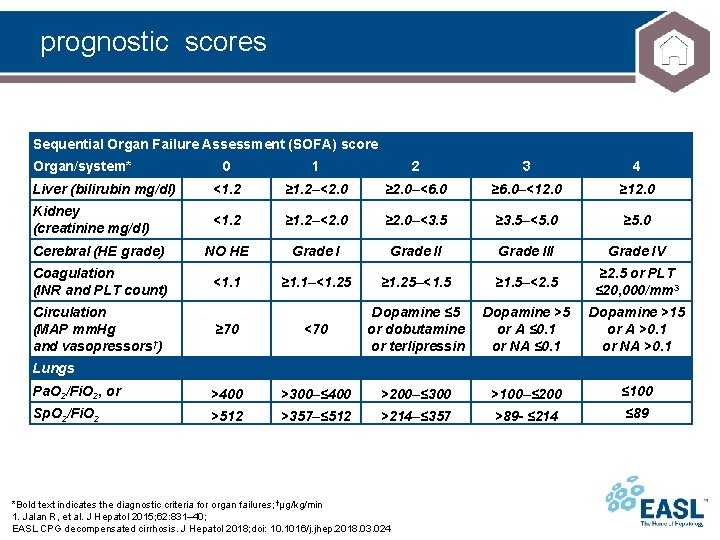
prognostic scores Sequential Organ Failure Assessment (SOFA) score Organ/system* 0 1 2 3 4 Liver (bilirubin mg/dl) <1. 2 ≥ 1. 2–<2. 0 ≥ 2. 0–<6. 0 ≥ 6. 0–<12. 0 ≥ 12. 0 Kidney (creatinine mg/dl) <1. 2 ≥ 1. 2–<2. 0 ≥ 2. 0–<3. 5 ≥ 3. 5–<5. 0 ≥ 5. 0 Cerebral (HE grade) NO HE Grade III Grade IV Coagulation (INR and PLT count) <1. 1 ≥ 1. 1–<1. 25 ≥ 1. 25–<1. 5 ≥ 1. 5–<2. 5 ≥ 2. 5 or PLT ≤ 20, 000/mm 3 ≥ 70 <70 Dopamine ≤ 5 or dobutamine or terlipressin Dopamine >5 or A ≤ 0. 1 or NA ≤ 0. 1 Dopamine >15 or A >0. 1 or NA >0. 1 Pa. O 2/Fi. O 2, or >400 >300–≤ 400 >200–≤ 300 >100–≤ 200 ≤ 100 Sp. O 2/Fi. O 2 >512 >357–≤ 512 >214–≤ 357 >89 - ≤ 214 ≤ 89 Circulation (MAP mm. Hg and vasopressors†) Lungs *Bold text indicates the diagnostic criteria for organ failures; †μg/kg/min 1. Jalan R, et al. J Hepatol 2015; 62: 831– 40; EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024
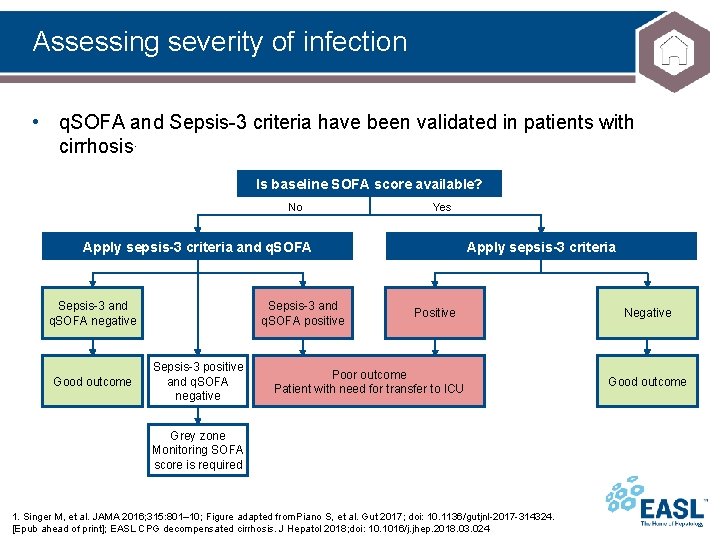
Assessing severity of infection • q. SOFA and Sepsis-3 criteria have been validated in patients with cirrhosis. Is baseline SOFA score available? No Yes Apply sepsis-3 criteria and q. SOFA Sepsis-3 and q. SOFA negative Good outcome Sepsis-3 and q. SOFA positive Sepsis-3 positive and q. SOFA negative Apply sepsis-3 criteria Positive Poor outcome Patient with need for transfer to ICU Grey zone Monitoring SOFA score is required 1. Singer M, et al. JAMA 2016; 315: 801– 10; Figure adapted from Piano S, et al. Gut 2017; doi: 10. 1136/gutjnl-2017 -314324. [Epub ahead of print]; EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024 Negative Good outcome
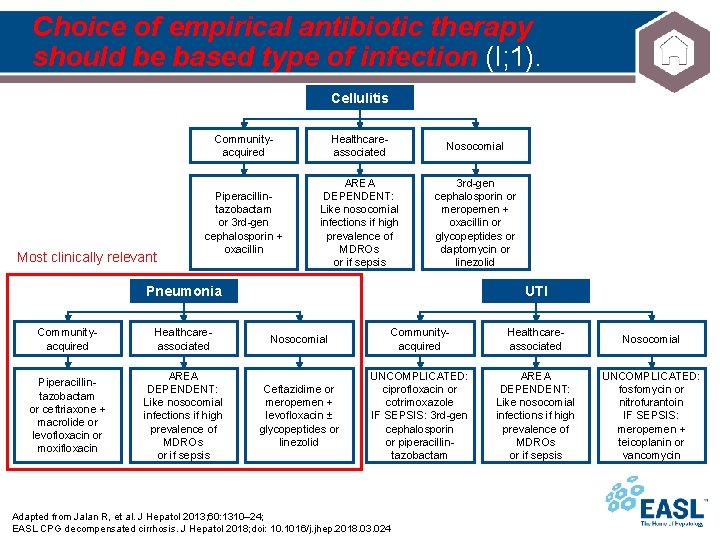
Choice of empirical antibiotic therapy should be based type of infection (I; 1). Cellulitis Most clinically relevant Communityacquired Healthcareassociated Nosocomial Piperacillintazobactam or 3 rd-gen cephalosporin + oxacillin AREA DEPENDENT: Like nosocomial infections if high prevalence of MDROs or if sepsis 3 rd-gen cephalosporin or meropemen + oxacillin or glycopeptides or daptomycin or linezolid Pneumonia Communityacquired Healthcareassociated Piperacillintazobactam or ceftriaxone + macrolide or levofloxacin or moxifloxacin AREA DEPENDENT: Like nosocomial infections if high prevalence of MDROs or if sepsis UTI Nosocomial Communityacquired Healthcareassociated Nosocomial Ceftazidime or meropemen + levofloxacin ± glycopeptides or linezolid UNCOMPLICATED: ciprofloxacin or cotrimoxazole IF SEPSIS: 3 rd-gen cephalosporin or piperacillintazobactam AREA DEPENDENT: Like nosocomial infections if high prevalence of MDROs or if sepsis UNCOMPLICATED: fosfomycin or nitrofurantoin IF SEPSIS: meropemen + teicoplanin or vancomycin Adapted from Jalan R, et al. J Hepatol 2013; 60: 1310– 24; EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Renal impairment

Renal impairment • In patients with liver diseases, even a mild increase in SCr should be considered since it may underlie a marked decrease of GFR (II, 1) • First step is to establish CKD, AKI. (II, 1) • Screening and treatment of infection are most important(II, 1) • Diuretics and/or β-blockers should be immediately stopped(II, 1) • In patients with AKI and tense ascites, therapeutic paracentesis ( with albumin infusion even with a low volume paracentesis) *Proteinuria/haeamaturia/ultrasonography abnormalities. †Stage 1 A (s. Cr <1. 5 mg/dl), Stage 1 B (s. Cr ≥ 1. 5 mg/dl) EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

Renal impairment: definitions of kidney disease • Kidney Disease: Improving Global Outcomes (KDIGO) group definitions: Definition Functional criteria Structural criteria AKI Increase in s. Cr ≥ 50% within 7 days, OR increase in s. Cr ≥ 0. 3 mg/dl within 2 days No criteria AKD decrease in GFR ≥ 35% for <3 months, OR increase in s. Cr ≥ 50 % for <3 months Kidney damage for <3 months CKD GFR <60 ml/min per 1. 73 m 2 for ≥ 3 months Kidney damage for ≥ 3 months SO… Baseline s. Cr • s. Cr obtained within 3 months prior to admission. *International Club of Ascites-recommended adaptation of KDIGO group criteria EASL CPG decompensated cirrhosis. J Hepatol 2018; doi: 10. 1016/j. jhep. 2018. 03. 024

ICA diagnostic criteria for HRS-AKI • Cirrhosis and ascites • No response after 2 consecutive days of diuretic withdrawal and plasma volume expansion with albumin 1 g per kg of body weight • Absence of shock • No use of nephrotoxic drugs (NSAIDs, aminoglycosides, iodinated contrast media) • No macroscopic signs of structural kidney injury: – Absence of proteinuria (>500 mg/day) – Absence of microhaematuria (>50 RBCs per high power field) – Normal ultrasonography
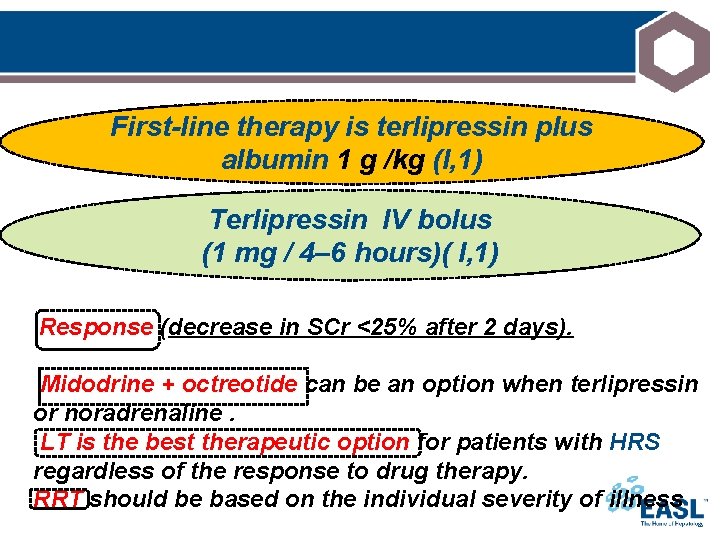
First-line therapy is terlipressin plus albumin 1 g /kg (I, 1) Terlipressin IV bolus (1 mg / 4– 6 hours)( I, 1) Response (decrease in SCr <25% after 2 days). Midodrine + octreotide can be an option when terlipressin or noradrenaline. LT is the best therapeutic option for patients with HRS regardless of the response to drug therapy. RRT should be based on the individual severity of illness

- Slides: 62