Clinical Foot and Ankle Biomechanics Overview of course

Clinical Foot and Ankle Biomechanics Overview of course By Paul Harradine (Podiatrist) Fiona Holdcroft May 2009

Session Overview • Functional anatomy: – Basic terminology – The ‘normal’ foot – The abnormal foot – Gait • Biomechanical foot and ankle assessment • Our role in treatment • Summary/conclusions

The ‘Normal’ Foot • The unified theory – 3 previous podiatric theories – All disagree in normal, abnormal and treatment methodology – All achieved clinical results – Unified theory combines the above

Basic Terminology • Pronation (Arch lowering) – Position of Eversion, Abduction & Dorsiflexion • Supination (Arch Rising) – Position of Inversion, Adduction & Plantarflexion • • Varus - Inversion Valgus - Eversion Forefoot - Structures distal to midtarsal joint 1 st Ray – 1 st metatarsal, medial cuneiform & navicular – NOT hallux
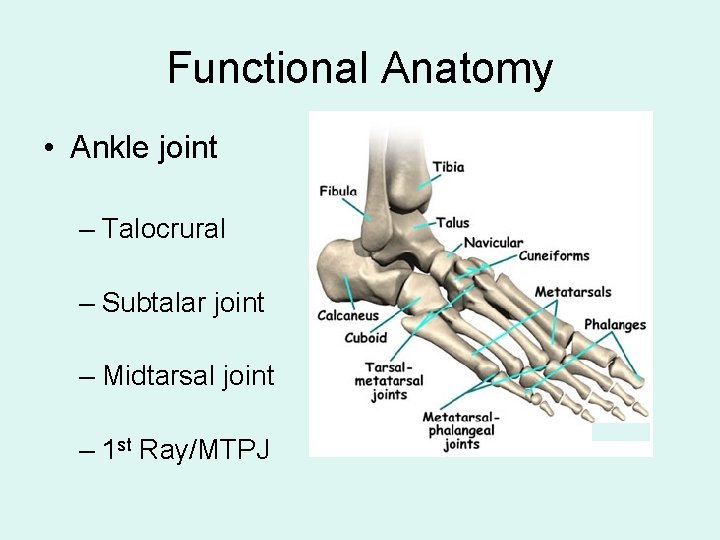
Functional Anatomy • Ankle joint – Talocrural – Subtalar joint – Midtarsal joint – 1 st Ray/MTPJ
Normal foot function
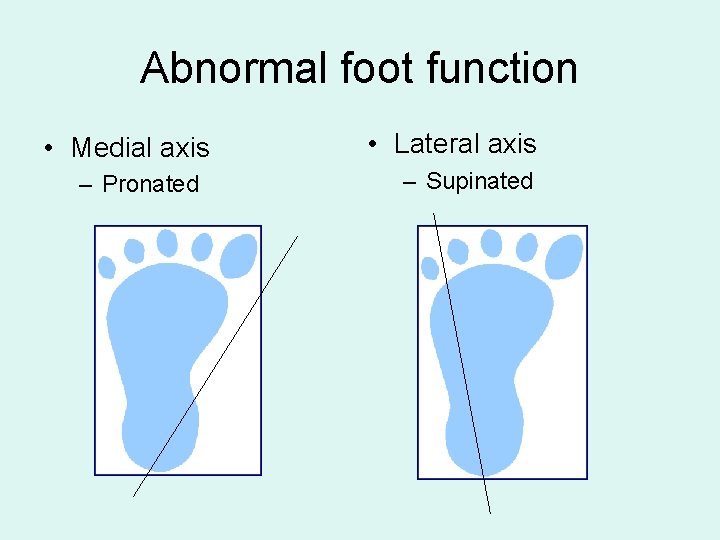
Abnormal foot function • Medial axis – Pronated • Lateral axis – Supinated
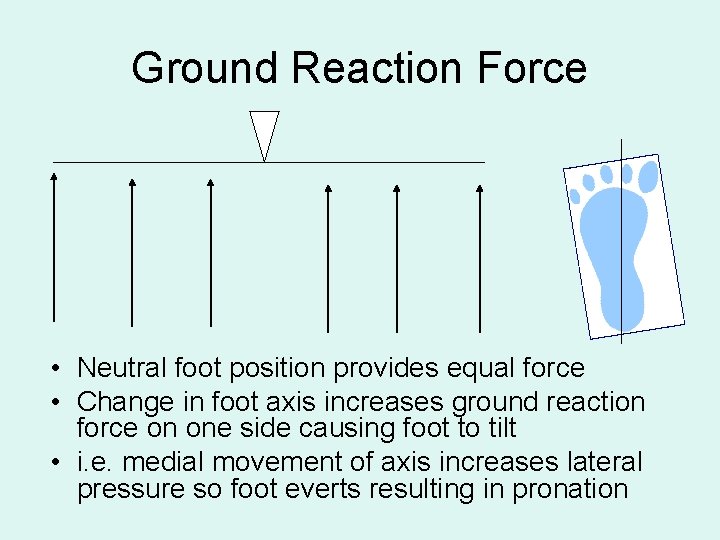
Ground Reaction Force • Neutral foot position provides equal force • Change in foot axis increases ground reaction force on one side causing foot to tilt • i. e. medial movement of axis increases lateral pressure so foot everts resulting in pronation

Interaction of 1 st ray and 1 st MTPJ • Try: – PF/DF 1 st ray – PF/DF hallux – DF 1 st ray then DF hallux • Normal interaction – ROM 1 st MTPJ is dependant on position of 1 st ray – 1 st ray has to PF (drop) to allow translation – Can get functional limitation of DF at hallux with lack of 1 st ray PF
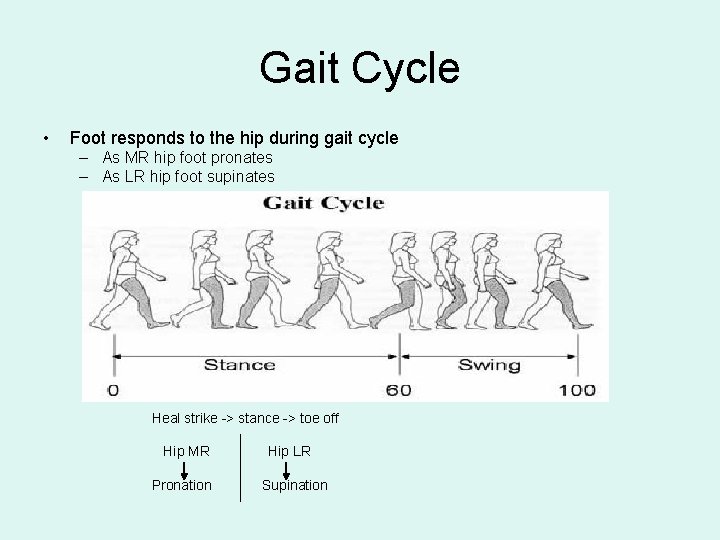
Gait Cycle • Foot responds to the hip during gait cycle – As MR hip foot pronates – As LR hip foot supinates Heal strike -> stance -> toe off Hip MR Pronation Hip LR Supination
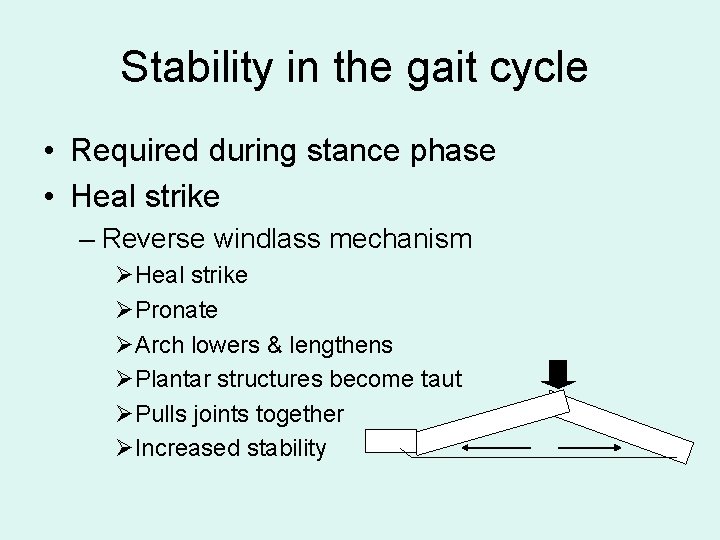
Stability in the gait cycle • Required during stance phase • Heal strike – Reverse windlass mechanism ØHeal strike ØPronate ØArch lowers & lengthens ØPlantar structures become taut ØPulls joints together ØIncreased stability
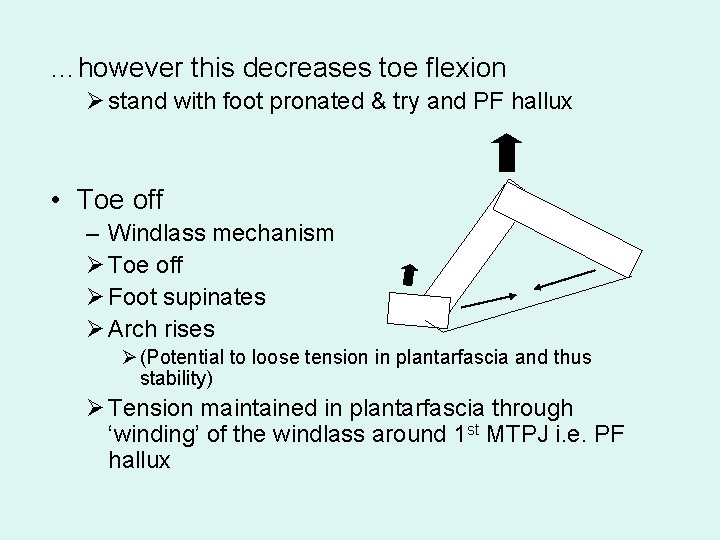
…however this decreases toe flexion Ø stand with foot pronated & try and PF hallux • Toe off – Windlass mechanism Ø Toe off Ø Foot supinates Ø Arch rises Ø (Potential to loose tension in plantarfascia and thus stability) Ø Tension maintained in plantarfascia through ‘winding’ of the windlass around 1 st MTPJ i. e. PF hallux
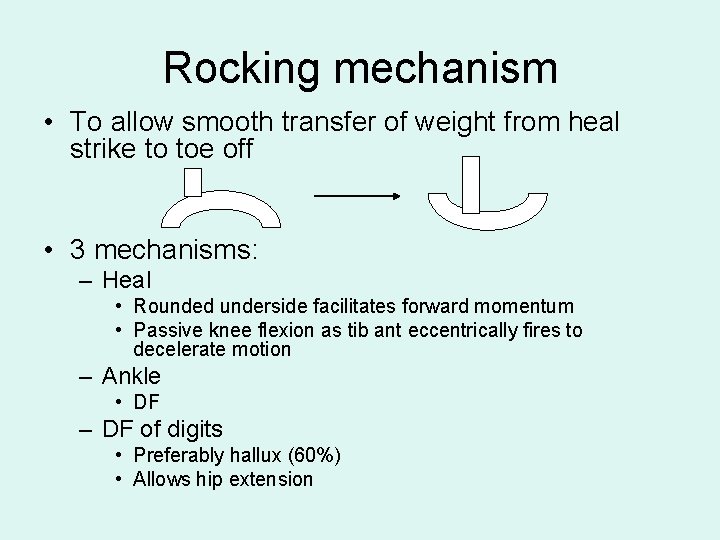
Rocking mechanism • To allow smooth transfer of weight from heal strike to toe off • 3 mechanisms: – Heal • Rounded underside facilitates forward momentum • Passive knee flexion as tib ant eccentrically fires to decelerate motion – Ankle • DF – DF of digits • Preferably hallux (60%) • Allows hip extension
Over pronation • To hard – Can not re-supinate or LR at hip – Gait compensation e. g. abductory twist, reduced hip rotation • To far – Lower limb functional malalignment • Increased MR hip ‘squinting patella’ – Increased plantarfascia stress – Gait compensation e. g. side sway, excessive pelvic rotation, decreased hip extension, trunk flexion, abductory twist, MTJ DF, 1 st IPJ DF, lateral column propulsion • Functional hallux limitus & reduced 3 rd rocker
What causes pronation? • Muscle activity e. g. weak gluts • Increased external pronatory forces – Obesity – Running • Ankle Equinus – Reduced DF ROM (<10 degrees with foot in subtalar neutral) – Reduced 2 nd rocker
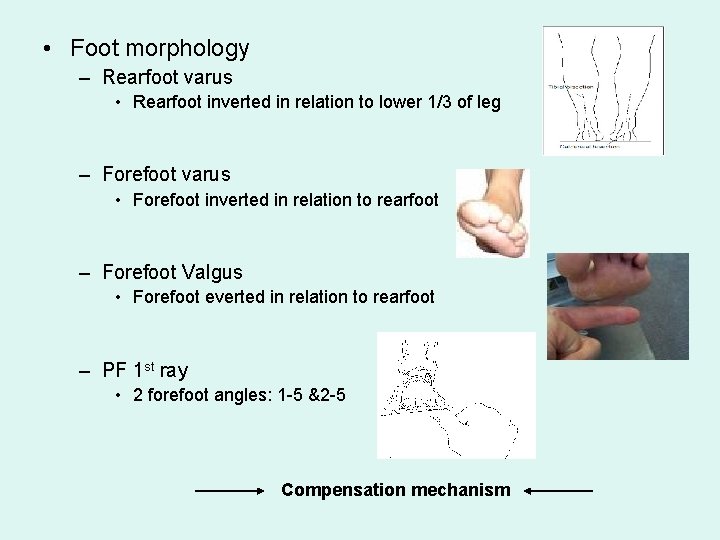
• Foot morphology – Rearfoot varus • Rearfoot inverted in relation to lower 1/3 of leg – Forefoot varus • Forefoot inverted in relation to rearfoot – Forefoot Valgus • Forefoot everted in relation to rearfoot – PF 1 st ray • 2 forefoot angles: 1 -5 &2 -5 Compensation mechanism

ARCH height means nothing - It is irrelevant Important thing is reserve of pronation

Foot assessment • LL assessment in supine • Subtalar neutral • Pronation tests – Supination Resistance Test – Maximum Pronation Test – Navicular Drop Test – Hubschers Test – STJ Axis Position • Gait analysis

LL assessment in supine • Leg length – Malleolus position pre and post ‘sit up’ • • MR/LR at hips Knee extension Position of tibial tuberosity vs patella Tibial torsion

Subtalar neutral • Patient prone • Feel talus position with ‘inside hand’ • Move foot to find neutral with ‘outside hand’ • In subtalar neutral assess for – ROM DF? – Rearfoot or forefoot varus/valgus? – Position of 1 st ray?

Pronation tests • Quick guide into relationship between patients foot function and symptoms • 5 tests • Help to answer the question – – – How hard is the patient pronating? How far is the patient pronating? Is there a functional hallux limitus? Does my patient need an onward podiatry referral? Does my patient need orthotics? • Possible false negative BUT not false positive due to static assessment of dynamic structure

Supination Resistance Test • Assesses force required to re-supinate STJ • With patient standing try and lift arch with moderate force i. e. supinate foot • Assess resistance – Easy: abnormally small pronatory forces ? supinator – Moderate: Normal – Hard: Abnormally large pronatory forces

Maximum Pronation Test • Assesses reserve of pronation, and thus if patient is maximally pronated irrespective of arch height • With patient standing ask them to roll down their arches. Assess for calcaneal eversion (from behind): – < 2 degrees rearfoot eversion -> no reserve of pronation, thus maximally pronated – >2 degrees rearfoot eversion ->reserve of pronation, thus not maximally pronated

Navicular Drop Test • Assesses amount of pronation relevant to STJ, not arch height • With patient standing record height of navicular tubercle with neutral axis (from behind). Repeat with patient relaxed • >10 mm drop indicates abnormally pronated foot position

The Hubscher Test • Assesses for functional hallux limitus • With patient standing attempt to passively DF hallux • Grade on scale 0 -3: – 0: Nil DF (abnormal - ? pronator) – 1: Slight DF (abnormal - ? pronator) – 2: DF with resistance. Slight arch raising with limited MR leg (normal) – 3: DF with limited resistance. Complete arch rising with obvious MR leg (abnormal - ? supinator)

STJ Axis Position • Allows estimation of joint axis position • With patient standing palpate talus head and estimate angle of axis by imagining perpendicular line to talus – Medial axis indicates ? pronation – Axis towards 2 nd toe indicates neutral foot position – Lateral axis indicates ? supination
Pronatory Gait Compensations • • • Abductory twist Reduced pelvic rotation Trunk flexion/forward lean Decreased arm swing Increased side sway Excessive pelvic rotation Decreased hip extension MTJ DF 1 st IPJ DF Lateral column propulsion

Our role in treatment • Exercises: aim to decreases pronatory forces – – LR hip strengthening Stretches for ankle equinus Intrinsic foot muscle strengthening Proprioception training • Mobilisations: aim to increase ROM to restore normal gait – TCJ – MTJ – 1 st MTPJ
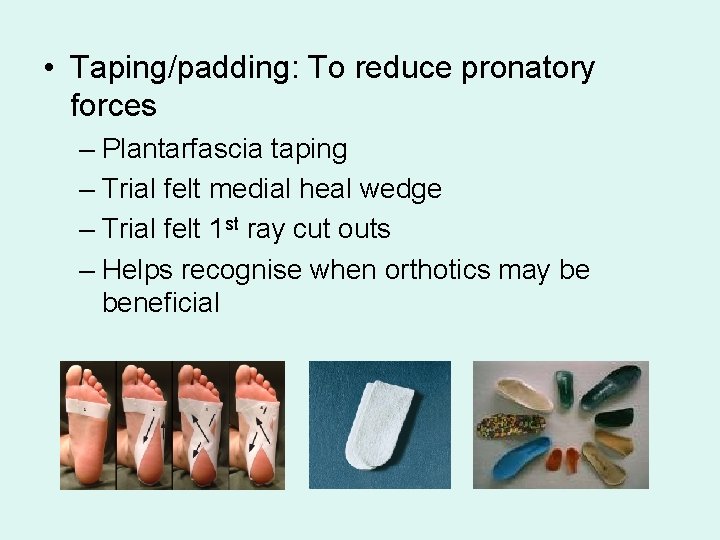
• Taping/padding: To reduce pronatory forces – Plantarfascia taping – Trial felt medial heal wedge – Trial felt 1 st ray cut outs – Helps recognise when orthotics may be beneficial

Orthotics • Aim to reduce pronatory forces and facilitate medial column propulsion – – Equalise ground reaction force Bring axis from medial position to 2 nd toe Level the see-saw Facilitate ‘normal’ gait • Use rearfoot posting with medial heal support +/1 st ray cut off NOT arch support • Need to recognise when to use custom or non custom orthotics

Custom vs non-custom orthotics Non-custom • Immediate provision • Inexpensive • Bulky • Limited modification to patient • Often 1 st ray impingement Custom • Modified for patient • Required for complex patients • Outcome reviewed • Less bulky • Wait to see podiatry • More expensive NB Poorly fitting orthotics can cause functional hallux limitus AND Never alter an orthotic, refer back to prescriber

The Runner • Running is not an accelerated form of walking: – Increased GRF (2. 5 -3 x body weight) – Increased frequency of heal strike – Increased limb varus • Therefore – Increased need to reduce pronatory forces e. g. with orthotics, strengthening – Need to check outcomes dynamically – Look at footwear

Trainers • Many varieties • 3 Classification – Neutral – Stability – Motion Control Mizuno Waverider 11 Weight Brooks GTS Adrenalin 8 Control Brooks Beast/Ariel

• Upper support – If push down on medial border of shoe it should provide support and not compress down • Flexion stability – If push up on distal end of shoe should flex at MTPJ NOT mid foot Good flexion stability Bad flexion stability Poor upper stability

Summary • Foot acts as a see-saw and responds to GRF • Normal foot function during gait: – – – – Heal strike and the 1 st rocker MR hip and foot pronation Reverse windlass mechanism 2 nd rocker to allow stance LR and foot supination 3 rd rocker for toe off Windlass Mechanism and medial column propulsion Hip and knee extension to progress to swing phase

• Screen for over pronation with 5 key tests • Recognise when – Foot position may be impacting on symptoms – Orthotics may be appropriate – Referral to podiatry is indicate
- Slides: 36