CLINICAL CYTOLOGY IN GYNAECOLOGY Presenters Curthbert Goodluck Daudi

CLINICAL CYTOLOGY IN GYNAECOLOGY Presenters: Curthbert Goodluck Daudi Ntunaguzi Supervisor: Dr Mgaya

Outline �Introduction Ø Definitions and advantages Ø Methods of Obtaining Samples Ø Patient Preparation �Staining Techniques Ø Papanicolaou o Maturation Index Ø Liquid Based Cytology �Cytology Reporting Ø The Bethesda System �Features Reported by Cytology �References

Introduction CYTOLOGY A branch of Pathology dealing with -clusters of cells -Individual cells in smears CYTOLOGY IN GYNAECOLOGY deals with exfoliated cells from superficial squamous cells or forcibly scrapped cells from Cervix

Introduction… �The most successful application of clinical cytology is diagnosis of cervical abnormalities before they develop into invasive cervical carcinoma, screening and follow-up of cervical carcinoma, especially squamous carcinoma �Cytology smears are sensitive to abnormalities, although there is variable interpretation on any particular smear �The most important factor is to detect an abnormality and to start an appropriate management plan �Specimen should be obtained and prepared by trained individuals

Advantages �The advantages of diagnostic cytology are that Øsimple procedure, Øhelps in faster reporting, Øis relatively inexpensive, Øhas high population acceptance and facilitates cancer screening in the field. ØDoes not need anesthesia

Methods of obtaining cellular samples from the female genital tract 1. Cervical Smear ü The Cervex brush, Endo-cervical brush or wooden scraper is applied to entire portion of cervix & into external os to collect material from endocervical canal ü Material is quickly spread on slides fixation pap stain 2. Vaginal Smear ü Useful for assessment of hormonal status ü Material from lateral wall of upper 1/3; Handle as for cervical 3. smear Posterior Fornix Aspiration ü Useful in detecting endometrial Ca. It uses pipette with suction bulb 4. Endometrial Aspiration ü Sample directily from endometrium:
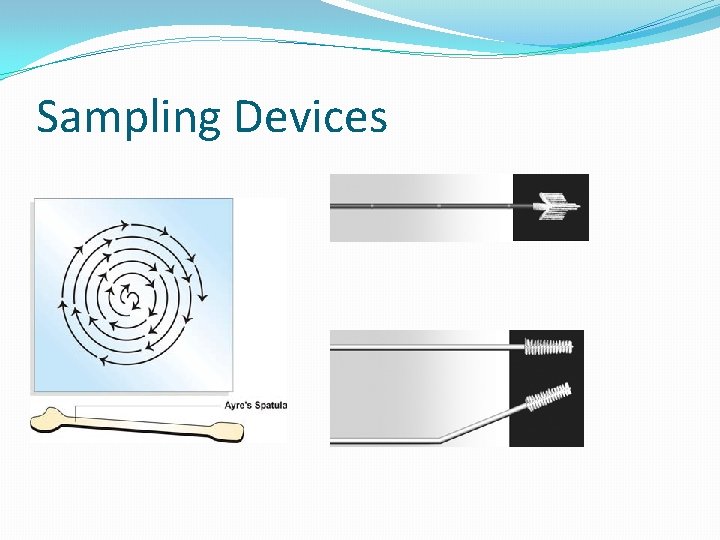
Sampling Devices

Patient Preparation �Patient should not douche the vagina for at least a day before the examination. � No intravaginal drugs at least one week before the examination. �Patient should abstain from coitus for one day before the examination. � Smear should not be taken during menstrual bleeding, because of contamination with blood, endometrial component , debris and histiocytes.

Staining Techniques �Papanicolaou (Pap) stain Multichromatic staining histological technique developed by George Papanicolaou �An alcohol dried preparation better nuclear detail than air fixation �Stains ribosomes blue green, particularly in parabasal cells, mesothelial cells and metaplastic squamous cells �Stains metabolically inactive cells pink, such as superficial cells �Stains keratinized cells or thick specimens orange (benign or malignant) �Must fix smear quickly and stain carefully

Procedure. �Manual staining with the Papanicolau method uses the following steps: 1. Remove smear from fixative. 2. Rinse smear in descending grade of alcohol (80%, 70% ethyl alcohol 3. Rinse in tap water: 2 gentle dips.

4. Stain in Harris hematoxylin for 3 minutes. 5. Rinse in running tap water for 15 seconds. 6. Differentiate in 1% acid in 70% ethyl alcohol: 2 dips 7. Rinse in running tap water. 8. Blue in running tape water for 5 minutes. 9. Rinse smear in ascending grades of alcohol (70%, 80% ethyl alcohol) 10 dips each

10. Rinse in 2 changes of 95% ethyl alcohol: 10 dips each. 11. Stain with Orange G-6 for 2 minutes. 12. Rinse in 2 changes of 95% ethyl alcohol: 4 dips each. 13. Stain in EA- 36 solution for 3 minutes 14. Rinse in 2 changes of 95% ethyl alcohol: 4 dips each 15. Complete dehydration in 2 changes of absolute ethyl alcohol: 10 dips each

16. Clear alcohol in Xylene 2 changes four dips each. 17. Mount the slide with DPX and cover slip. 18. Label specimen accordingly. (Numbered stickers). 19. Arrange the stained slides into Hard board serially. 20. Examine the stained slides under the microscope for staining quality. 21. Send to the Pathologist for Examination.

Maturation Index �Is a ratio obtained through performing a random count of three major cell types (parabasal, intermediate, and superficial cells) that are shed from the squamous epithelium �Based on assumption that the sex hormones estrogen, progesterone, androgen (testosterone) bring about maturation in squamous cell that can be detected by cytological examination �The higher the number of mature cell designated superficial and intermediate, the higher the maturation index or estrogen effect in the body

�There are only two absolutes when it comes to cellular patterns in maturation index �Predominance of parabasal cells indicates an absence of estrogen stimulation �Predominance of superficial cells indicates estrogen stimulation �Intermediate cells have little clinical usefulness �The maturation index provides practitioners with a sample that is easily analyzed to detect hormonal changes in the vagina that are age appropriate or an early sign of possible hormonal related disease process
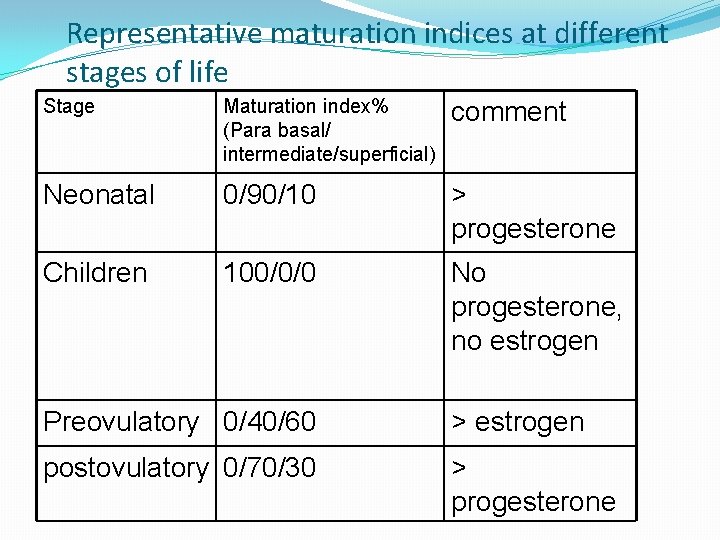
Representative maturation indices at different stages of life Stage Maturation index% (Para basal/ intermediate/superficial) comment Neonatal 0/90/10 ˃ progesterone Children 100/0/0 No progesterone, no estrogen Preovulatory 0/40/60 ˃ estrogen postovulatory 0/70/30 ˃ progesterone
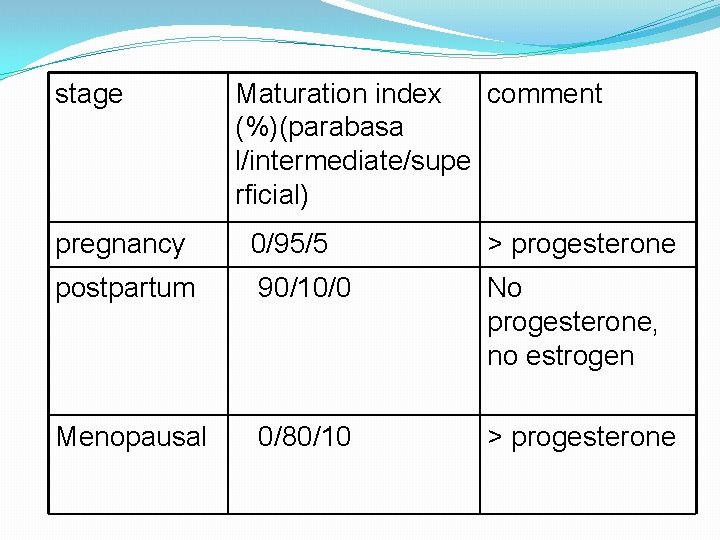
stage Maturation index comment (%)(parabasa l/intermediate/supe rficial) pregnancy 0/95/5 ˃ progesterone postpartum 90/10/0 No progesterone, no estrogen Menopausal 0/80/10 ˃ progesterone

�Liquid based cytology Technique �Head of spatula, where cells are lodged, is broken off into small glass vial containing preservative fluid, or rinsed directly into preservative fluid �Sample is sent to lab, then spun and treated to remove mucus, pus or other obscuring material �Random sample of remaining cells is taken and deposited onto a slide

Bethesda System for Cervicovaginal Cytology reporting �The Bethesda system (TBS) is a system for reporting cervical or vaginal cytological diagnoses, used for reporting Pap smear results. �It was introduced in 1988, and revised in 1991 and 2001. �The name comes from the location (Bethesda, Maryland) of the conference that established the system.

�Types of results 1. Squamous cell abnormalities �LSIL – Low-grade Squamous Intraepithelial Lesion �Indicates possible cervical dysplasia �LSIL usually indicates mild dysplasia (CIN 1), more than likely caused by a human papillomavirus infection. �CIN 1 is the most common and most benign form of cervical intraepithelial neoplasia and usually resolves spontaneously within two years.

�HSIL – High-grade Squamous Intraepithelial Lesion �Indicates moderate or severe cervical intraepithelial neoplasia or carcinoma in situ. �In some cases these lesions can lead to invasive cervical cancer, if not followed appropriately �Atypical squamous cells of undetermined significance (ASC-US) �Atypical squamous cells – cannot exclude HSIL (ASC-H) �Squamous cell carcinoma

2. Glandular cell abnormalities �Adenocarcinoma �can arise from the endocervix, endometrium and extrauterine sites. AGC �AGC, formerly AGUS, is an acronym for atypical glandular cells of undetermined significance. �The management of AGC is colposcopy with or without an endometrial biopsy

Features Reported by Gynecological Cytology �Benign Features �Inflammation/ Infection �Premalignant lesions �Squamous Cell Carcinoma �Adenocarcinoma �Endometrial carcinoma

Benign features: Cytology description �Evenly distributed heterochromatin and euchromatin �Chromatin granules are small and uniformly distributed (versus coarse and uniform in lymphocytes and ovarian granulosa cells) �Chromatin is sharp and crisp �No hyperchromasia (in contrast, lymphocytes are usually hyperchromatic) �Nuclear membranes are smooth �Chromatin rims have uniform thickness 24

�Nucleoli are conspicuous but not large and not prominent (but are more conspicuous if reactive or biosynthetic activity is present) �Honeycomb configuration when viewed en face �Transparent cytoplasm in squamous or transitional cells suggests benign and mature cells �Immature benign cells: ↑ N/C ratio, denser cytoplasm, vesicular nuclei Differential diagnosis Ø Reactive changes, due to any type of stimuli (p. H change, hormonal changes, inflammatory causes) may resemble dysplasia

Air drying artifact �Definition Ø Artifact due to delay in immersion in alcohol fixative Ø More common on conventional than liquid based smears Ø Specimen is unsatisfactory if more than 75% of cells show air drying; if less extensive, may be mentioned as a quality indicator Ø May cause discrepant diagnosis of LSIL or under diagnosis for HSIL Ø Associated with ASCUS in perimenopausal women
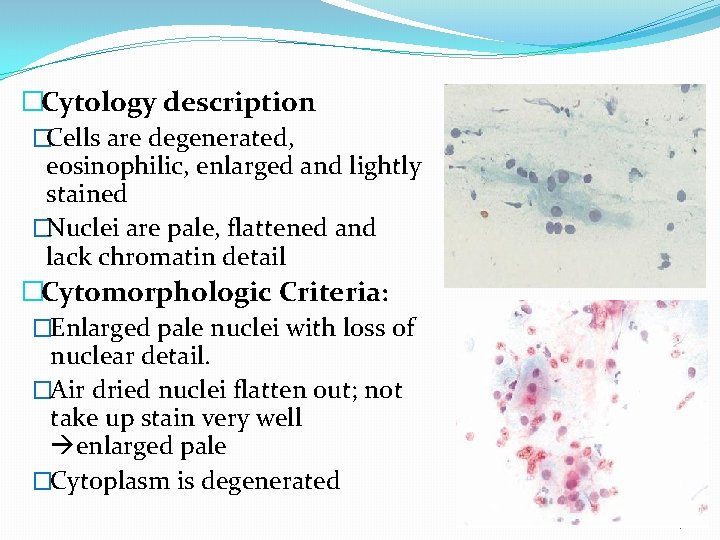
�Cytology description �Cells are degenerated, eosinophilic, enlarged and lightly stained �Nuclei are pale, flattened and lack chromatin detail �Cytomorphologic Criteria: �Enlarged pale nuclei with loss of nuclear detail. �Air dried nuclei flatten out; not take up stain very well enlarged pale �Cytoplasm is degenerated 27

Arias-Stella reaction �Definition Ø Pregnancy related changes that without a clinical history may appear worrisome, including cytomegaly, enlarged nuclei, smudgy chromatin, frequent nuclear inclusions, prominent nucleoli Ø Named for Peruvian pathologist �Clinical features Ø Often over diagnosed as SIL, but pregnant women with atypical glandular lesions (AGUS) may have SIL on subsequent biopsy Ø Arias-Stella changes disappear after pregnancy Ø Pathologists are often not told patient is pregnant or post-partum
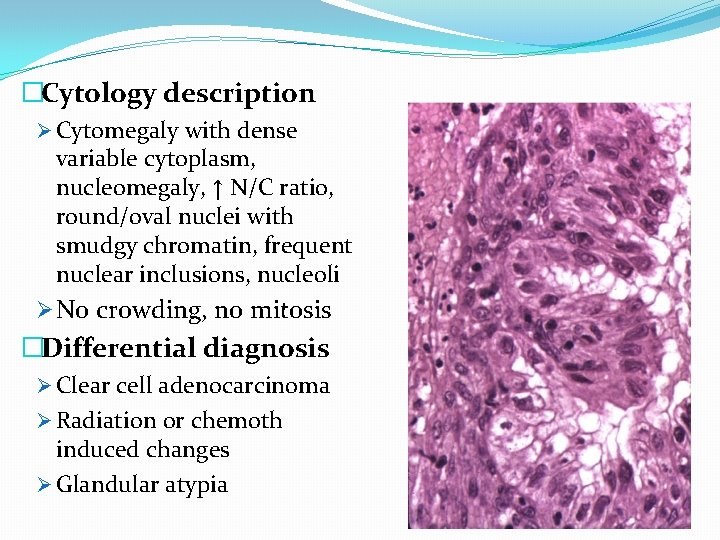
�Cytology description Ø Cytomegaly with dense variable cytoplasm, nucleomegaly, ↑ N/C ratio, round/oval nuclei with smudgy chromatin, frequent nuclear inclusions, nucleoli Ø No crowding, no mitosis �Differential diagnosis Ø Clear cell adenocarcinoma Ø Radiation or chemoth induced changes Ø Glandular atypia 29

Atrophy �Definition ØIncreased number of basal and parabasal cells, associated with Diagnosis of ASCUS �Clinical features �Assoc with scanty smears, ASCUS in post- menopausal women �Changes may disappear after topical estrogen �Prognostic features �New guidelines recommend HPV testing as initial triage management of postmenopausal women with cytological result of LSIL 01/01/2022 Cytology_ Gyn 30

Atrophy �Cytology description ØIncreased number of parabasal and basal cells, which form sheets and syncytial-like aggregates or hyperchromatic crowded groups ØNaked nuclei (small cells) may be seen; naked, uniform nuclei ØCells have high N/C ratio but uniform chromatin ØPseudokeratinized cells (pink to orangophilic cytoplasm) due to degeneration ØSevere atrophy can show dirty background with inflammation, debris, old blood, blue blobs and giant cells 31
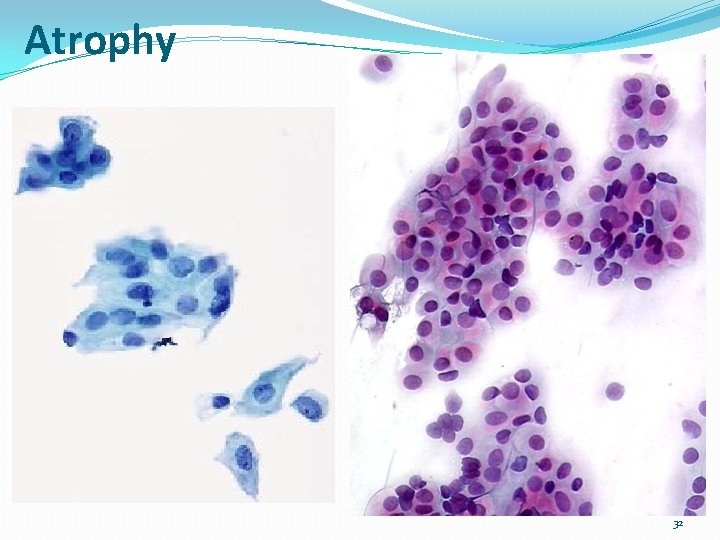
Atrophy 32
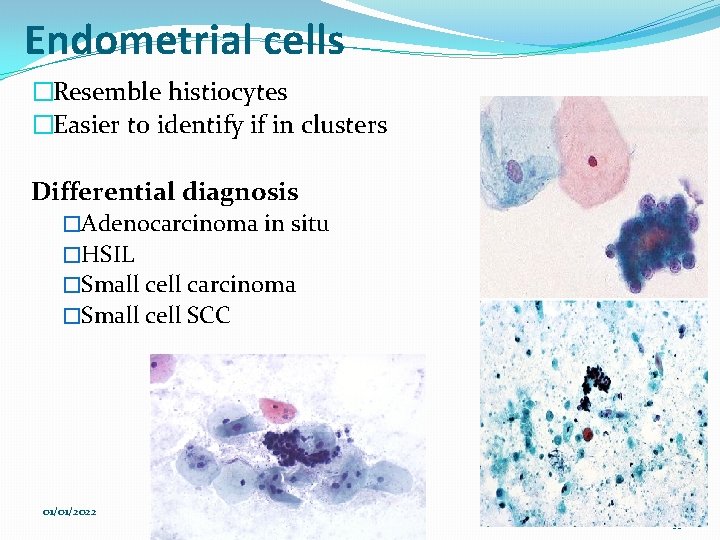
Endometrial cells �Resemble histiocytes �Easier to identify if in clusters Differential diagnosis �Adenocarcinoma in situ �HSIL �Small cell carcinoma �Small cell SCC 01/01/2022 Cytology_ Gyn 33
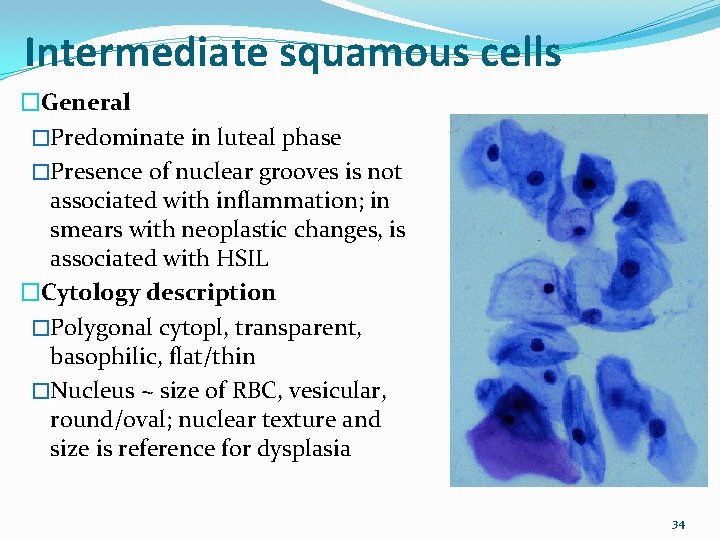
Intermediate squamous cells �General �Predominate in luteal phase �Presence of nuclear grooves is not associated with inflammation; in smears with neoplastic changes, is associated with HSIL �Cytology description �Polygonal cytopl, transparent, basophilic, flat/thin �Nucleus ~ size of RBC, vesicular, round/oval; nuclear texture and size is reference for dysplasia 34

Unsatisfactory specimen �Unsatisfactory if >75% of specimen is obscured by blood or inflammation �Also due to scant cellularity Ø An adequate conventional Pap test should have 8, 000 to 12, 000 squamous cells ØAn adequate liquid-based Preparation (LBP) should have at least 5, 000 squamous cells (review at least 10 microscopic fields at 40 x) 35

�Terminology �Examples of sample reports for unsatisfactory cases: Ø Unsatisfactory because of obscuring inflammation Ø Unsatisfactory because of insufficient squamous cellularity Ø Unsatisfactory because of obscuring blood 36

Inflammation/ Infection �Actinomycosis, bacterial vaginosis �Candida, chlamydia, chronic cervicitis �CMV, Enterobius, granuloma inguinale �Granulomas, herpes/HSV, Lactobacillus �Leptothrix, Schistosomiasis, syphilis �Trichomonas, tuberculosis, Wucheria
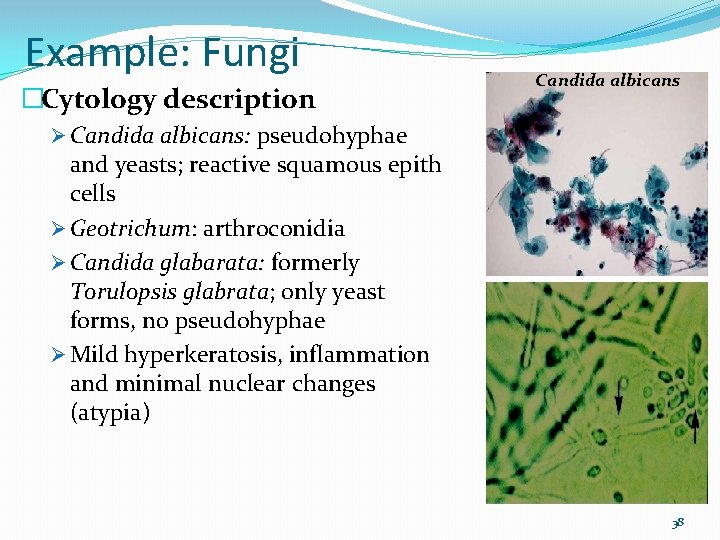
Example: Fungi �Cytology description Candida albicans Ø Candida albicans: pseudohyphae and yeasts; reactive squamous epith cells Ø Geotrichum: arthroconidia Ø Candida glabarata: formerly Torulopsis glabrata; only yeast forms, no pseudohyphae Ø Mild hyperkeratosis, inflammation and minimal nuclear changes (atypia) 38

Granuloma inguinale �Definition �Sexually transmitted disease caused by Calymmatobact granulomatis, a gram negative organism �Cytology description �Giant cells in Pap test or a collection of epithelioid MФ (granuloma) �Donovan bodies (intracytoplasmic coccobacilli in macrophages stained by Giemsa or Wright's stain) are seen, may have bipolar densities in smears taken from scrapings of edge of lesions, are pleomorphic, up to 2 microns 39
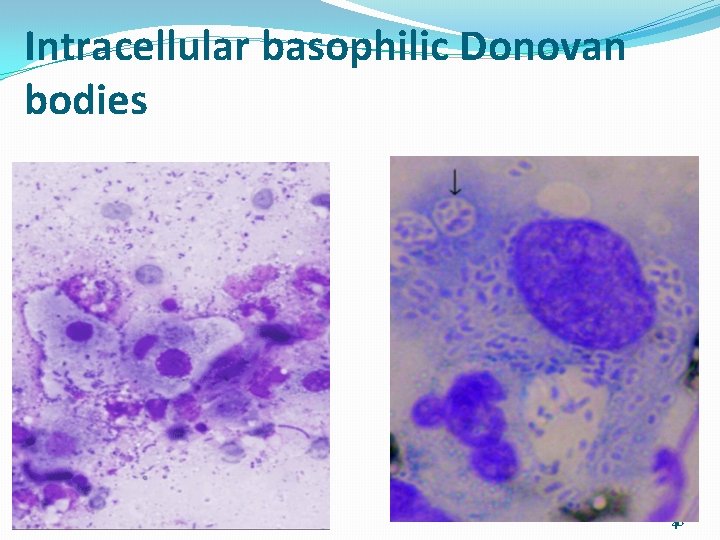
Intracellular basophilic Donovan bodies 01/01/2022 Cytology_ Gyn 40

Herpes simplex virus (HSV) �Common disease caused by herpes simplex 1 (HSV 1) or HSV 2 Cytology description �Early changes can include mononucleated cells �Multinucleated cells with dense, intranuclear Cowdry-type viral inclusions �Nuclei have ground glass appearance due to accumulation of viral particles, which causes peripheral margination of chromatin

Herpes simplex virus (HSV)… �Also nuclear molding �“ 3 M’s of herpes” - margination of nuclei, molding & multinucleation �Cowdry: intranuclear eosinophilic amorphous or droplet-like bodies surrounded by clear halo, with (type A, herpes) or w/o (type B, adenovir or poliovirus) margination of chromatin on the nuclear membrane
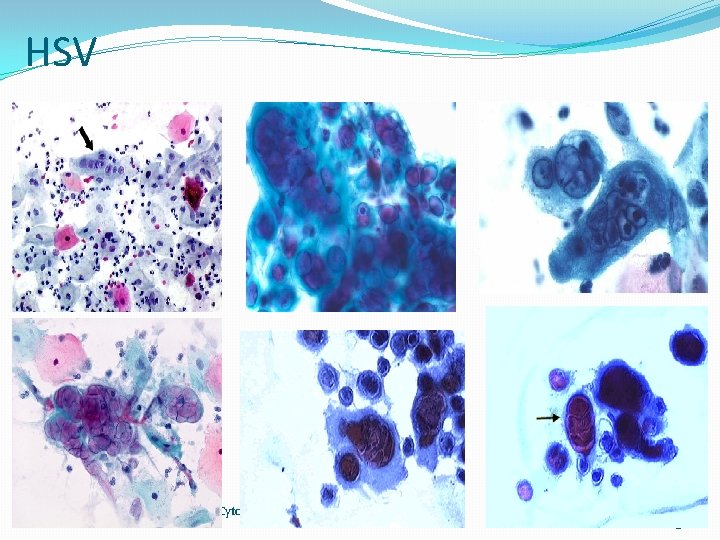
HSV 01/01/2022 Cytology_ Gyn 43

Trichomonas vaginalis �Definition �Facultative anaerobic protozoan parasite without mitochondria or peroxisomes �Morphologic identification with liquid based preparations is highly accurate and should not require confirmatory testing �In contrast, confirmatory tested is recommended for diagnosis based on conventional smears of women without symptoms

�Cytology description �Pear-shaped, oval to round or kite shaped, 15 -30 microns �Often has eosinophilic cytoplasmic granules �Pale, vesicular and centrally located nuclei �Adjacent squam cells have hyperchromatic nuclei and small, evenly circumscribed, perinuclear halos �Commonly assoc with acute inflam (polyballs), lymphs & mast cells �May coexist with SIL and even cancer

Atypia / Premalignant / preinvasive lesions �Adenocarcinoma in situ (AIS) �Atypical glandular cells (AGC) �Atypical repair, atypical reserve cell hyperplasia �Atypical squamous cells (ASC) �Chemotherapy effect, condyloma, HPV �HSIL/CIN II, HSIL/CINIII, LSIL/CIN I �Paget's disease, radiation atypia, SIL

LSIL / CIN I / low grade dysplasia �Terminology �Low grade squamous intraepithelial neoplasia (LSIL) encompasses HPV changes and cervical intraepithelial neoplasia I (CINI) �Previously called mild dysplasia �Cytology description �Enlarged nuclei at least 3 x size of nucleus of intermediate cell, but N/C ratio is less than 1: 3 �Hyperchromasia (nuclei darker than that of intermediate cell), cell may be enlarged (largest atypical cells in gynecologic cytology are LSIL), slight ↑ in N/C ratio �No nucleoli �Binucleation is more common than multinucleation

�±Koilocytes; nuclear pleomorphism, wrinkled nuclei, hyperchromasia, binucleation, perinuclear halos with distinct clear zone around nucleus and condensation of denser cytoplasm around the periphery �Immature LSIL may be interpreted as metaplasia, ASCUS or HSIL �Few/no mitotic figures, particularly in lower ½ of epithelium; no atypical mitotic figures �Differential Diagnosis �Reactive epithelial changes �Postmenopausal squamous atypia � HSIL

HSIL / CIN II / moderate dysplasia �Terminology �CIN II / moderate dysplasia is classified as HSIL �Cytology description �Cell size is same as squa metaplastic or parabasal cells; polygonal shape (like intermediate or superficial cell), denser cytoplasm �N/C ratio is 1: 3 to 1: 2 �Enlarged and hyperchromatic nucleus �Nuclear membranes may be irregular (crinkled paper) �No nucleoli �Check for variation in nuclear size at basal layer
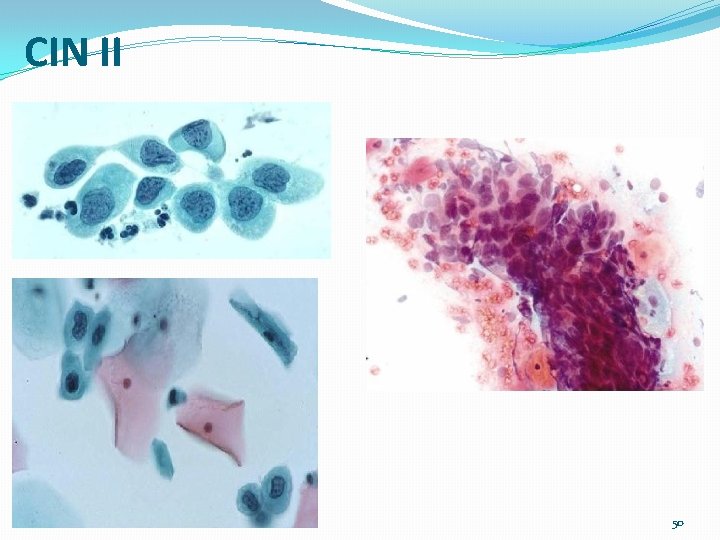
CIN II 01/01/2022 Cytology_ Gyn 50

HSIL / CIN III / severe dysplasia �Terminology �Also called carcinoma in situ �Cytology description �Usually single, small, round/oval cells with scant cytoplasm and increased N/C ratio (> 1: 2) �Nuclear membrane does not have sharp angles �Nuclei vary markedly in contour and have irregular coarsely clumped chromatin �No macronucleoli, no tumor diathesis
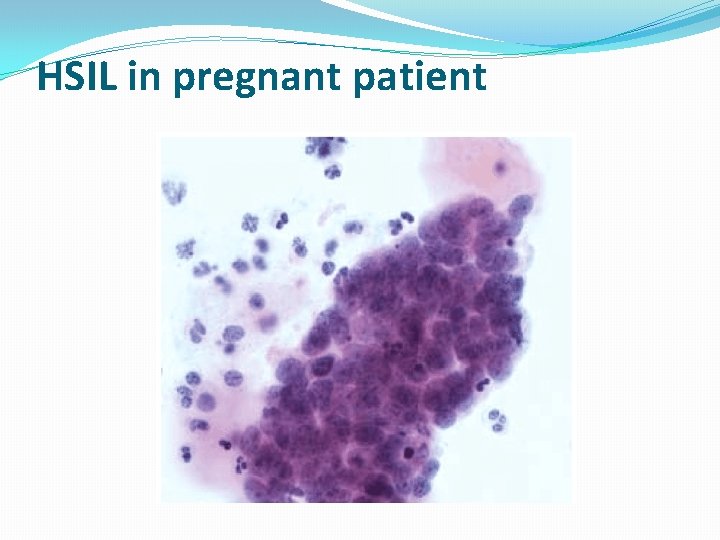
HSIL in pregnant patient

Squamous cell carcinoma of cervix �Definition �Malignant invasive tumor showing squamous cell differentiation �Diagnosis in conventional smears is more likely to be missed if few malignant cells and not keratinized; also if Trichomonas present

SCC: Cytology description �Highly irregular shaped cells (tadpole, caudate) �Keratinized cells are orange, often with squamous pearls �Nonkeratinized cells have dense, hard, basophilic cytoplasm �Also cannibalism (tumor cells surround other cells) �Prominent nucleoli may be seen �Compared to adenocarcinoma, have more irregular cellular and nuclear shapes, more cytoplasmic density, more chromatin granularity, more hyperchromasia

SCC: Cytology description, Cont’d �Tumor diathesis in background (necrosis, hemorrhage, inflammatory cells) is suggestive of malignancy �Tumor diathesis in liquid based cytology is more subtle than with conventional smears; consists of necrotic material at peripheral of cell groups (“clinging diathesis”) and not in the background �Other features in liquid based cytology are mild to moderate inflammation, coexistent dysplasia, keratinization, decreased cell coverage

SCC: Cytology description, Cont’d �Papillary squamo-transitional carcinoma of cervix: o Liquid based cytology specimens are moderately to highly cellular with three dimensional, arborizing, papillary clusters of basal or parabasal cells; o Occasional fibrovascular cores; o Cells vary from bland to SIL; o Frequent mitotic figures; o Occasional tumor diathesis and dyskeratotic cells; o No koilocytosis
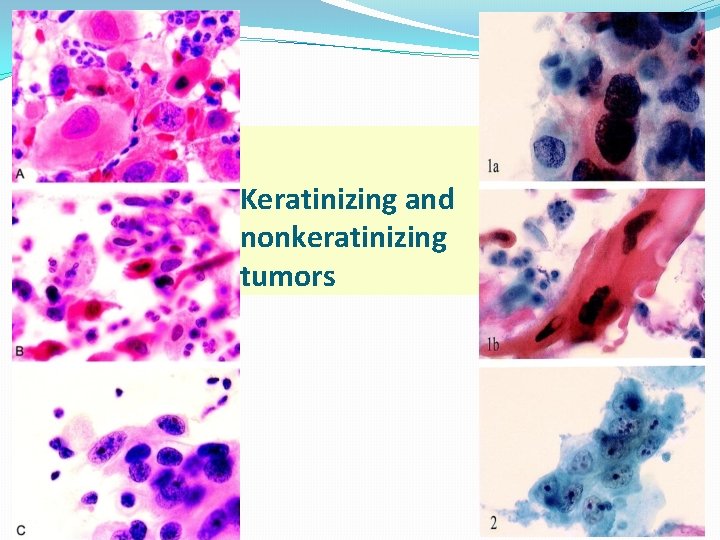
Keratinizing and nonkeratinizing tumors 01/01/2022 57
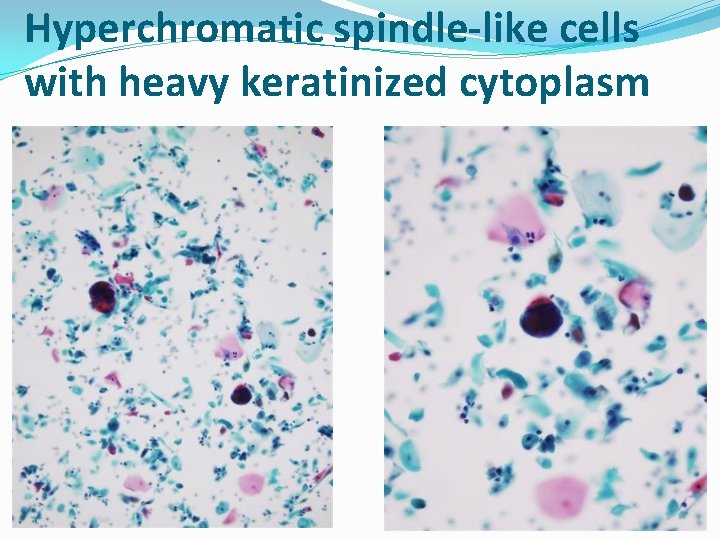
Hyperchromatic spindle-like cells with heavy keratinized cytoplasm 01/01/2022 Cytology_ Gyn 58

Adenocarcinoma of cervix �Definition �Endocervical glandular lesion characterized by high grade cytology, nuclear enlargement, mitosis and stromal invasion �Cytology description �Multilayering �May form glandular structures with central lumina or acinar formations with peripheral nuclei

�Cells are pleomorphic, large or small with fluffy cytoplasm, cytoplasmic vacuolization, loss of nuclear polarity, true nuclear crowding, nuclei with clumped chromatin, marked variation of nucleoli, occasional mitotic figures �Invasion: heavy blood with abundant glandular epithelium, even without tumor diathesis or fully malignant nuclear criteria �May see morules (also seen with mesothelial cells, benign and malignant lesions)

�Endocervical adenocarcinoma: usually columnar with granular cytoplasm, rosettes, sheets with holes vs. balls, round plump cells, molded groups �Conventional smears that are false negative often have fewer and smaller abnormal cells, small nuclei, less atypia and less hyperchromasia
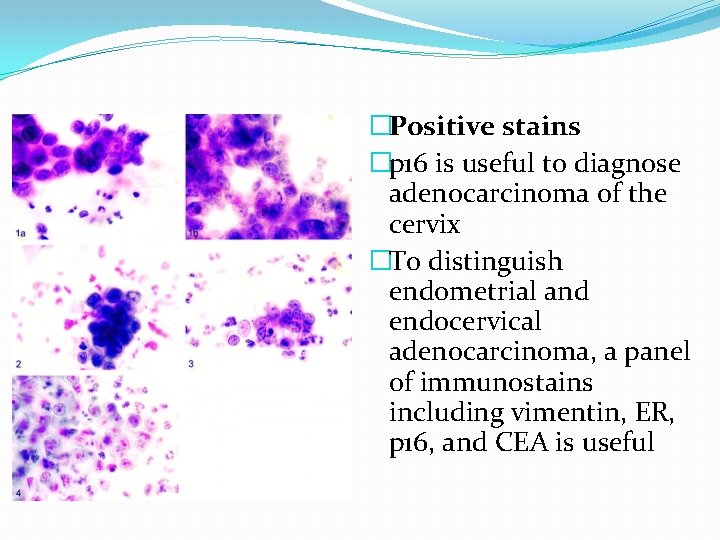
�Positive stains �p 16 is useful to diagnose adenocarcinoma of the cervix �To distinguish endometrial and endocervical adenocarcinoma, a panel of immunostains including vimentin, ER, p 16, and CEA is useful

Endometrial adenocarcinoma �Clinical features �Cervical smear is 45% sensitive in detecting endometrial adenocarcinoma �Cervical smear is useful to detect its involvement of endometrial carcinoma �Thin-Prep may be more sensitive than conventional smears �Low risk (<2%) of nodal spread if normal cervical smear �Cytology description �Glandular component present �Also scattered single cells with hyperchromatic nuclei, 1 -3 nucleoli, mitotic figures, apoptotic bodies, watery diathesis �Thin-Prep shows tumor diathesis (53%, usually high grade lesions
- Slides: 63