Clinical Coding for non coders A brief overview

Clinical Coding for non coders A brief overview of clinical coding and the role of the Clinical Classifications Service
How to view this presentation Clicking in the top right of each slide will navigate through the notes. Only once all the notes have been viewed the ‘next page’ icon will appear. Use and to navigate backwards and forwards through the slides. For optimum viewing avoid the keyboard controls and use the mouse only.

The background to Clinical Coding The history of diagnostic and interventional classifications

What is Clinical Coding? The translation of medical terminology, as written by the clinician to describe a patient’s complaint, problem, diagnosis, treatment or reason for seeking medical attention, into a coded format which is nationally and internationally recognised. Clinical Coders are highly trained specialists who develop the skills throughout their career to accurately record a patient’s healthcare problems and interventions using a classification system of diseases (ICD-10) and procedures (OPCS-4). Medical terminology ICD-10 codes

John Graunt - Weekly Bills of Mortality LONDON week ending 31 st January 1634 The Disease and Casualties this week Abortive 2 Aged 36 Bedridden 1 Bloody flux 1 Bruised 1 Consumption: later became Cancer 1 known as tuberculosis Chilbed 3 Chrisoms 19 Consumption 77 Convulsions 44 Cough 2 Dropsie 1 Christened Males Female In all This, as you can see, is very basic information. The terminology has advanced a lot since then. 107 109 216 John Graunt, a physician, was the first to start collecting data on the number of patients dying and what they were dying from. That was in the seventeenth century, and the information he collected became known as the ‘Weekly Bills of Mortality’. Executed 33 Feaver 10 Flox and smallpox 5 Found dead in the street (an infant) 1 Teeth: Extremely poor dental French pox 1 Grippinghygiene as was prevalent in in the guts 13 Jaundices 1 those times often led to death Infants as bacterial infection from the 18 Killed with a fall 3 teeth and gums can spread to Murthered other parts of the body, 1 particularly the heart. Overlaid 2 Quinsie 1 Rickets 8 Rising of the lights 8 Scowering 1 Overlaid: In olden times, several Scurvy 2 children used to share the same Stillborn 9 Rising of the lights: In the bed. This term would suggest that Stone 1 past lights was a term for one person turning over may have Stopping of the lungs, so rising of the stomachcaused suffocation in another. 3 lights suggests choking or Suddenly 6 breathlessness. Messages Teeth 16 from someone who has Windie 3 original accounts suggest Worms 1 that rising of the lights nearly Plague always occurred in women who had recently given birth. Deceased in the burials this week - 63 So it could mean either Parishes clear of the plague - 130 Parishes infected - 20 Gripping in the guts / Stopping of • Post partum depression or the stomach: Probably referred to hysteria types of bowel / digestive obstruction. • Pulmonary embolus. Buried Males Female In all 213 196 409 0

Florence Nightingale – Notes on Hospitals “I am fain to sum up with an urgent appeal for adopting … some uniform system of publishing the statistical records of hospitals. There is a growing conviction that in all hospitals, even in those which are best conducted, there is a great and unnecessary waste of life … In attempting to arrive at the truth, I have applied everywhere for information, but in scarcely an instance have I been able to obtain hospital records fit for any purposes of comparison … If wisely used, these improved statistics would tell us more of the relative value of particular operations and modes of treatment than we have means of ascertaining at present. ” Florence Nightingale attempted to collect information about the outcome of care. In the beginning she developed her During the Crimean War, diseases such as typhus, typhoid, cholera, and dysentery were rife in the army hospitals. own method of recording outcomes using the three distinct groups. They are all pretty self explanatory: Many more soldiers were dying from diseases than from wounds. Nightingale played an active role during the War and Notes on Hospitals, London: Longman, Green, Roberts, Longman and Green, 1. Relieved = the patient was discharged having been cured of the medical condition they had been suffering from worked towards improvements in sanitation, nutrition, and activity for the patients of the hospitals. Death rates were 1863. 2. Not relieved = the patient had been discharged but had not been relieved of the medical condition they were reduced dramatically with the introduction of such measures. Later, Nightingale kept meticulous records of the number of deaths, and the causes of deaths, so that on her return to Great Britain she could justify the need for improving suffering from conditions in hospitals. In 1858 Florence Nightingale became the first female member of the Royal Statistical Society. 3. Died = speaks for itself!
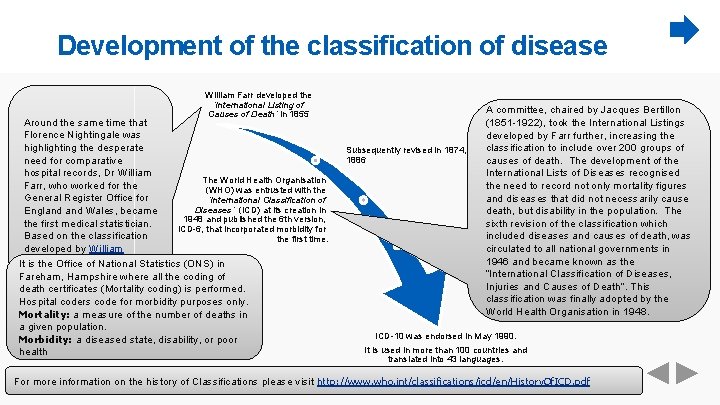
Development of the classification of disease William Farr developed the ‘International Listing of Causes of Death’ in 1855 Around the same time that Florence Nightingale was highlighting the desperate need for comparative hospital records, Dr William The World Health Organisation Farr, who worked for the (WHO) was entrusted with the General Register Office for ‘International Classification of Diseases’ (ICD) at its creation in England Wales, became 1948 and published the 6 th version, the first medical statistician. ICD-6, that incorporated morbidity for Based on the classification the first time. developed by William Cullen, Farr was appointed It is the Office of National Statistics (ONS) in to develop an internationally Fareham, Hampshire where all the coding of applicable and uniform death certificates (Mortality coding) is performed. classification for the Hospital coders code for morbidity purposes only. recording of causes of death. Mortality: a measure of the number of deaths in a given population. Morbidity: a diseased state, disability, or poor health A committee, chaired by Jacques Bertillon (1851 -1922), took the International Listings developed by Farr further, increasing the classification to include over 200 groups of Subsequently revised in 1874, 1880 and 1886 causes of death. The development of the International Lists of Diseases recognised the need to record not only mortality figures and diseases that did not necessarily cause death, but disability in the population. The sixth revision of the classification which ICD was consequently included diseases and causes of death, was revised every 10 years until the ninth revision in circulated to all national governments in 1975 1946 and became known as the “International Classification of Diseases, Injuries and Causes of Death”. This classification was finally adopted by the World Health Organisation in 1948. ICD-10 was endorsed in May 1990. It is used in more than 100 countries and translated into 43 languages. For more information on the history of Classifications please visit http: //www. who. int/classifications/icd/en/History. Of. ICD. pdf
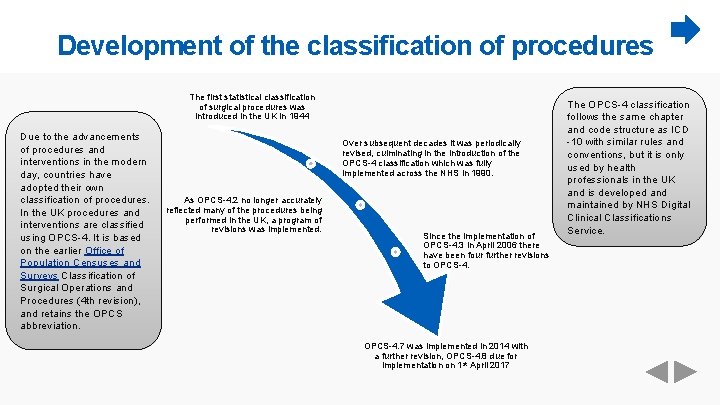
Development of the classification of procedures The first statistical classification of surgical procedures was introduced in the UK in 1944 Due to the advancements of procedures and interventions in the modern day, countries have adopted their own classification of procedures. In the UK procedures and interventions are classified using OPCS-4. It is based on the earlier Office of Population Censuses and Surveys Classification of Surgical Operations and Procedures (4 th revision), and retains the OPCS abbreviation. Over subsequent decades it was periodically revised, culminating in the introduction of the OPCS-4 classification which was fully implemented across the NHS in 1990. As OPCS-4. 2 no longer accurately reflected many of the procedures being performed in the UK, a program of revisions was implemented. Since the implementation of OPCS-4. 3 in April 2006 there have been four further revisions to OPCS-4. 7 was implemented in 2014 with a further revision, OPCS-4. 8 due for implementation on 1 st April 2017 The OPCS-4 classification follows the same chapter and code structure as ICD -10 with similar rules and conventions, but it is only used by health professionals in the UK and is developed and maintained by NHS Digital Clinical Classifications Service.

The importance of coded data The coding process and how data is used

Current Classifications – ICD-10 & OPCS-4 The classifications we use in clinical ‘A classification is a systematic arrangement of like entities coding are the ‘International based on differing characteristics’ Classification of Diseases and • Groups ‘like’ entities together in a standardised medical language • Provides a structured framework for statistical information • Governed by rules and conventions • Nationally and internationally recognised Related Health Problems – Tenth Revision’ (ICD-10) and ‘Office of Population Censuses and Surveys Classification of Interventions and Procedures – Fourth Revision’ Classifications provide us (OPCS-4). with a tool to interpret large amounts of information in a format which can be easily tabulated, aggregated, interpreted analysed. The format ensures the information is comparable, consistent and easily manipulated. For more information on ICD-10 and to view the ICD-10 browser please click on the image
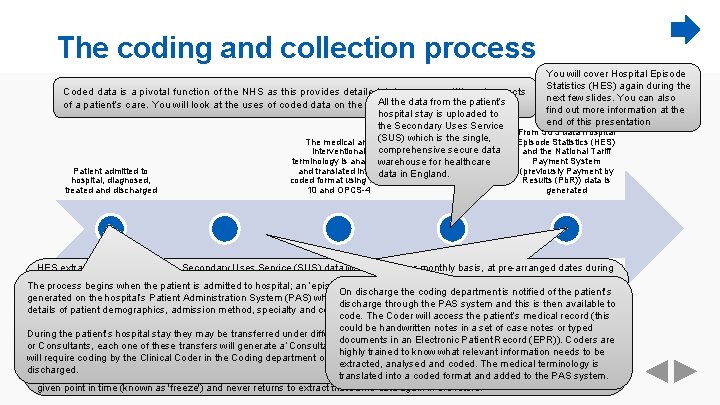
The coding and collection process You will cover Hospital Episode Statistics (HES) again during the next few slides. You can also find out more information at the end of this presentation Coded data is a pivotal function of the NHS as this provides detailed data on many different aspects All the data from the patient’s of a patient’s care. You will look at the uses of coded data on the next slides. hospital stay is uploaded to the Secondary Uses Service From SUS data Hospital Episode Statistics (HES) The medical and (SUS) which is the single, and the National Tariff interventional comprehensive secure data Payment System terminology is analysed warehouse for healthcare (previously Payment by Patient admitted to and translated into a data in England. hospital, diagnosed, treated and discharged coded format using ICD 10 and OPCS-4 Results (Pb. R)) data is generated The medical record is After the information is HES extracts are taken from the Secondary Uses Service (SUS) data warehouse on a monthly basis, at pre-arranged dates during accessed by the Clinical coded onto the year. Each extract is cumulative and contains data submitted for the financial year so far, i. e. month 1 will only contain the data Coder and the relevant The process begins when the patient is admitted to hospital; an ‘episode of care’ is hospital’s information On discharge the coding department is notified of the patient’s information for the patient’s submitted with an activity date in April, but month 6 will contain data submitted with an activity date from April to September. system the data is generated on the hospital’s Patient Administration System (PAS) which contains hospital stay is extracted discharge through the PAS system and this is then available to uploaded to the data including: details of patient demographics, admission method, specialty and consultant. code. The Coder will access the patient’s medical record (this HES represents a series of fixed positions aligned to extracted data, while SUS is continuously updated whenever data is submitted. warehouse known as Main condition treated or Secondary Uses Service could be handwritten notes in a set of case notes or typed This is why there can be differences between SUS and HES even when looking at the same time period. investigated During the patient’s hospital stay they may be transferred under different specialities (SUS) documents in an Electronic Patient Record (EPR)). Coders are Secondary diagnoses or Consultants, each one of these transfers will generate a ‘Consultant Episode’ and highly trained to know what relevant information needs to be National Tariff data is sourced from SUS data which is the same source as used for HES data. There a number of differences Any relevant procedures or will require coding by the Clinical Coder in the Coding department once the patient is interventions extracted, analysed and coded. The medical terminology is between National Tariff data and HES data. The first difference relates to the cumulative nature of the HES extract with the year to discharged. translated into a coded format and added to the PAS system. date being extracted each time whereas National Tariff data is not cumulative and simply takes a single monthly snapshot at a given point in time (known as 'freeze') and never returns to extract that same data again in the future.
The uses of coded data - Statistical Coded information can be used in a statistical manner to provide accurate and uniform data which can be utilised in many areas of healthcare. National tariff payment system and Allows each Resource HRG 4+ individual Trust to Indirect care of management & plan and allocate the patient is casemix planning resources supported by a according to the casemix of their Classification patients. The aim of the National Tariff Payment Allows health care specialists to analyse Clinical indicators System is to provide a transparent, frequency of occurrence of diseases and Epidemiological / rules-based system for paying Trusts. identify at risk populations based on aetiological studies It rewards efficiency, supports patient demographic and geographical coded choice and diversity and encourages data. For example, epidemiologists can (Indirect activity for sustainable waiting time use coded data to analyse where lung reductions. Payment are linked to cancers most commonly occur in the UK, Care) activity and adjusted for casemix. and then assess why this may be. Importantly, this system ensures a fair Coded data provides an income Provides information with which and consistent basis for hospital for the Trusts by securing funding to monitor Trust performance funding rather than being reliant from the Treasury. Inaccurate against other Trusts, thus principally on historic budgets and the coded data may result in a failure ensuring equality for patients, negotiating skills of individual to secure the funds necessary to implementation of best practice managers. HRG v 4+ codes signify provide services which meet the and addressing bad practice. clinically similar treatments that use needs of the population. Examples of clinical indicators common levels of healthcare resource include patients re-admitted to (iso-resource). An information hospital following discharge management tool, their development Health trends Commissioning after stroke or myocardial is to support the National Tariff infarction. Payment System. Statistical
The uses of coded data - Clinical Coded information can also be used for clinical purposes. Clinical use of clinical coded data is direct care of the patient and is most significantly supported by a Terminology, you will look at the difference between a classification and a terminology later in this presentation. Provides coded information for comparisons of patient care and measurement of outcomes within specialties. Clinical Audit Treatment effectiveness Cost analysis, treatment effectiveness and outcome measurements all provide additional clinical information to improve patient care on both a local and national level. Clinical governance Clinical (Direct Care) Outcome measurement Direct care of the patient is most significantly supported by a Terminology (SNOMED CT) Cost analysis Clinical Decision Support Trusts can use coded information to analyse internal performance, to assist best practice and to address problem areas in the treatment of patients. SNOMED CT (a terminology) provides clinicians with the knowledge and person-specific information they need to care for their patients.

Hospital Episode Statistics (HES) HES is a data warehouse containing details of all admissions, outpatient appointments and Accident and Emergency (A&E) attendances at NHS hospitals in England. This data is collected during a patient's time at hospital and is submitted to allow hospitals to be paid for the care they deliver. HES data is designed to enable secondary use, that is used for non-clinical purposes, of this administrative data. The benefits of HES: • monitor trends and patterns in NHS hospital activity • assess effective delivery of care • support local service planning • provide the basis for national indicators of clinical quality • reveal health trends over time • inform patient choice • determine fair access to health care • develop, monitor and evaluate government policy • support NHS and parliamentary accountability
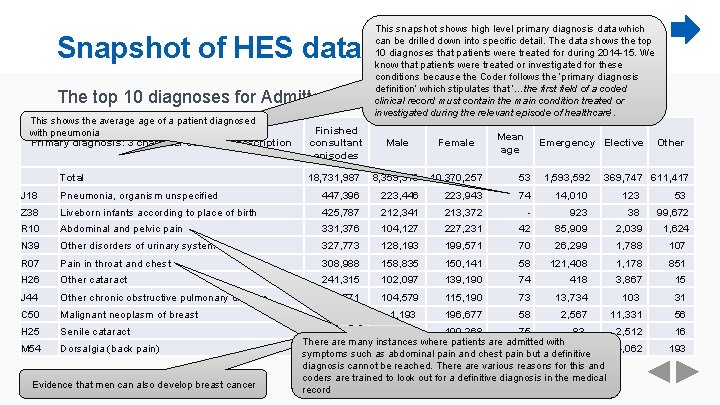
Snapshot of HES data This snapshot shows high level primary diagnosis data which can be drilled down into specific detail. The data shows the top 10 diagnoses that patients were treated for during 2014 -15. We know that patients were treated or investigated for these conditions because the Coder follows the ‘primary diagnosis definition’ which stipulates that ‘…the first field of a coded clinical record must contain the main condition treated or investigated during the relevant episode of healthcare’. The top 10 diagnoses for Admitted Patient Care in England, 2014 -15 This shows the average of a patient diagnosed with pneumonia Primary diagnosis: 3 character code and description Finished consultant episodes Male Female Mean age Emergency Elective Other Total 18, 731, 987 8, 359, 373 10, 370, 257 53 1, 593, 592 369, 747 611, 417 J 18 Pneumonia, organism unspecified 447, 396 223, 446 223, 943 74 14, 010 123 53 Z 38 Liveborn infants according to place of birth 425, 787 212, 341 213, 372 - 923 38 99, 672 R 10 Abdominal and pelvic pain 331, 376 104, 127 227, 231 42 85, 909 2, 039 1, 624 N 39 Other disorders of urinary system 327, 773 128, 193 199, 571 70 26, 299 1, 788 107 R 07 Pain in throat and chest 308, 988 158, 835 150, 141 58 121, 408 1, 178 851 H 26 Other cataract 241, 315 102, 097 139, 190 74 418 3, 867 15 J 44 Other chronic obstructive pulmonary disease 219, 771 104, 579 115, 190 73 13, 734 103 31 C 50 Malignant neoplasm of breast 197, 877 1, 193 196, 677 58 2, 567 11, 331 56 H 25 Senile cataract 172, 287 72, 014 100, 268 75 83 2, 512 16 M 54 Dorsalgia (back pain) Evidence that men can also develop breast cancer There are many instances where patients are admitted with 167, 268 62, 309 104, 942 57 19, 517 4, 062 193 symptoms such as abdominal pain and chest pain but a definitive diagnosis cannot be reached. There are various reasons for this and coders are trained to look out for a definitive diagnosis in the medical record

The future of Clinical Coding ICD-11 and SNOMED CT

ICD-11 development ICD-11 is currently in development; the testing phase is a thorough process to ensure the classification is fit for purpose and that it is an improvement on ICD-10. The World Health Organization (WHO) is currently developing the 11 th revision of ICD. WHO will brief the World Health Assembly in May 2018 and if ICD-11 is accepted countries can choose to adopt the new classification. The purpose of ICD-11 is to better reflect progress in health sciences and medical practice which are continuously evolving and will evolve at the same rate going forward. It is designed to be used in electronic health information systems and aligns with other classifications and terminologies such as ICD-O (International Classification of Disease for Oncology) and SNOMED-CT. To view the ICD 11 browser please click on the image

SNOMED CT is a clinical terminology Clinical Coders are not directly involved with SNOMED CT. However, the Government’s latest white paper Personalised Health and Care 2020 endorses the move to adopt a single clinical terminology – SNOMED CT – to support direct management of care into the entire health system by 2020. A structured list of terms for use in clinical practice. These terms describe the care and treatment of patients and cover areas like diseases, operations, treatments, drugs and healthcare administration. This allows for detailed recording of treatment. Clinical Terminologies are designed for use with an electronic system and are used to support direct management of care i. e. clinical use. Think back to the earlier slides that highlighted the Cross-maps are already provided from SNOMED CT concepts to ICD-10 and difference between OPCS-4. If the decision is taken to implement ICD-11, cross-maps will also be statistical and provided to ICD-11. clinical use of data To aid Clinical Coders the Clinical Classifications Service produce a product known as the cross-maps. This provides For more information on SNOMED CT please visit the SNOMED CT webpage probable classification codes for a ‘clinical meaning’ but still relies on the classification expertise of the coder to select the most appropriate codes based on the full information in the patient record to support statistical data.

SNOMED CT and clinical classifications are complementary and serve different purposes. SNOMED CT is the vocabulary for use by clinicians in an Electronic Patient Record (EPR). It is recorded at the point of care and is focussed on what a clinician wants to record about the patient. ICD-10 and OPCS-4 are recorded after the event and focusses on what we need to count for statistical and epidemiological analyses. Neither a clinical terminology nor a clinical classification can, by itself, serve all the purposes for which health information is currently used or will be used in the future. SNOMED CT is dynamic and updated twice a year to keep up with the latest developments in healthcare. ICD-10 and OPCS-4 are only updated every three years. This ensures stability for consistent and comparable analyses of population health across time. Remember: So the products are complimentary…not competing. Clinical use of data is supported by a terminology (SNOMED CT) Statistical use of data is supported by classifications (ICD-10/ICD-11 and OPCS-4)

The Clinical Classifications Service Our key responsibilities, product development and support

Our Role The team at the Clinical Classifications Service is made up of Classifications Specialists who hold a vast amount of expert knowledge in all aspects of Clinical Coding. All specialists are Accredited Clinical Coders by background and some are also approved Clinical Coding Auditors and/or Trainers. • Develop and maintain standards • Centre of expertise and point of contact • Product support helpdesk • ICD-10 and OPCS-4 • SNOMED CT cross maps • Clinical coding audit methodology • Training and accreditation • World Health Organisation Collaborating Centre Develop, issue and maintain the standards relating to all clinical classification data in use in the NHS (ICD-10 and OPCS-4) promoting the Provide the centre of expertise and a consistency of classification as a key point of contact for national and part of delivering a patient-centred international coding classifications work Deliver Classifications and Coding health service. Standards Support giving official resolutions to all clinical coding queries Develop and maintain an extensive portfolio of associated products (including cross maps from SNOMED CT concepts to ICD-10 and OPCS-4) Drive data quality by developing and delivering top notch clinical coding audit Provide an education, training and methodology accreditation programme for clinical coders to support an individual coder's Conduct comprehensive quality continuous professional development to assurance exercises on the developing become a trainer or auditor or manager ICD-11

Product Support and Development • • Classifications and Coding Standards Support and the national clinical coding query mechanism ICD-10 and OPCS-4 files and supporting tools such as metadata files National standard clinical coding reference materials UK Coding Review Panel providing guidance and developing national clinical coding standards National Clinical Coding Qualification (UK) and associated materials Clinical coding audit methodology, Code of Practice and workshops Clinical classifications training service – a portfolio of courses and training materials to support coders and trainers ICD-11 Working Group The Clinical Classifications Service is responsible for a whole host of products, some of which are shown here.

Further information If you are interested in finding out more information about anything covered in this presentation please visit the sites below: ICD-10 SNOMED CT OPCS-4 NHS Digital Terminology and Classifications HES WHO SUS

www. digital. nhs. uk @nhsdigital enquiries@nhsdigital. nhs. uk 0300 303 5678
- Slides: 24