Clinical Cancer Genetics in Breast and Ovarian Cancers


Clinical Cancer Genetics in Breast and Ovarian Cancers The Role of Cancer Genetics in Precision Medicine April 17, 2018 & May 1, 2018 Kamel Abou Hussein, MD Assistant Professor of Medicine Division of Hematology and Oncology Preeti Sudheendra, MD Assistant Professor of Medicine Division of Hematology and Oncology
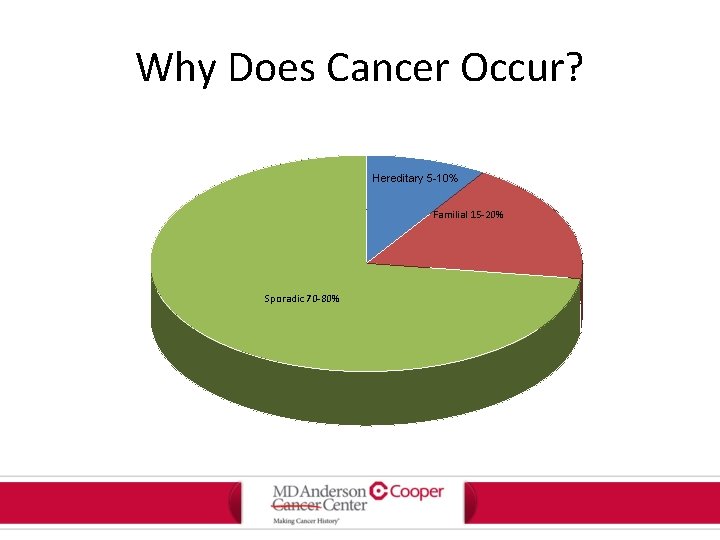
Why Does Cancer Occur? Hereditary 5 -10% Familial 15 -20% Sporadic 70 -80%

When to Suspect Hereditary Cancer • Breast cancer diagnosed ≤ 50 years • Ashkenazi Jewish ancestry and breast/ovarian (or pancreatic) cancer • Triple negative breast cancer ≤ 60 • Multiple primary cancers • Breast cancer in a male • Ovarian cancer at any age • Family history and/or known familial mutation NCCN version 1. 2018 “Genetic/Familial High Risk Assessment: Breast and Ovarian”; www. nccn. org
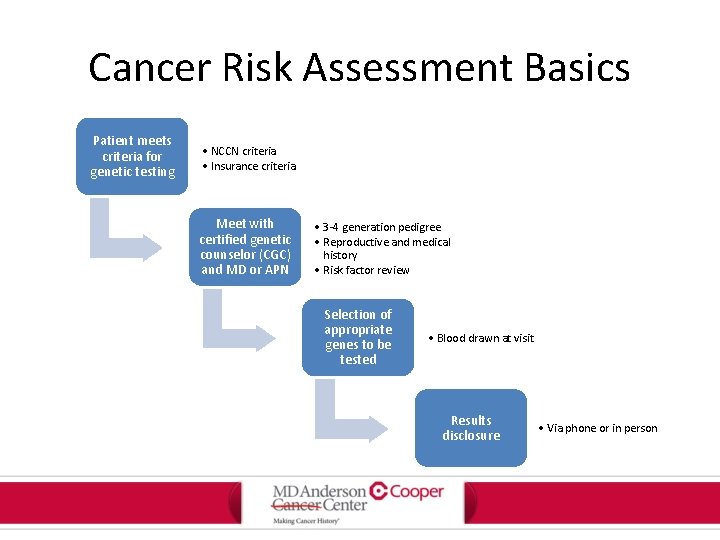
Cancer Risk Assessment Basics Patient meets criteria for genetic testing • NCCN criteria • Insurance criteria Meet with certified genetic counselor (CGC) and MD or APN • 3 -4 generation pedigree • Reproductive and medical history • Risk factor review Selection of appropriate genes to be tested • Blood drawn at visit Results disclosure • Via phone or in person

Benefits of Genetic Testing • For those with cancer: – Implications for medical management – A possible answer to “Why? ” • For those without cancer: – Implications for risk reduction and increased surveillance • For all: – Impact on risk of family members

Limitations and Risk of Testing • Negative result – Still doesn’t answer the “why? ” – Doesn’t mean a person without cancer will never get cancer – Cancer risk may still be elevated • Variant of uncertain significance – Doesn’t clarify risk – Can cause anxiety • Positive result – Can cause anxiety especially in family members – Genetics is a “family affair” – Concerns about genetic discrimination
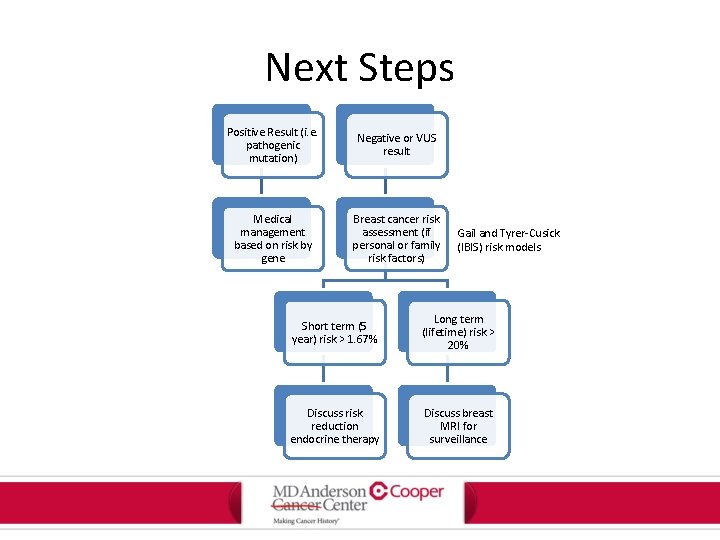
Next Steps Positive Result (i. e. pathogenic mutation) Negative or VUS result Medical management based on risk by gene Breast cancer risk assessment (if personal or family risk factors) Gail and Tyrer-Cusick (IBIS) risk models Short term (5 year) risk > 1. 67% Long term (lifetime) risk > 20% Discuss risk reduction endocrine therapy Discuss breast MRI for surveillance

Managing High Breast Cancer Risk due to Personal and Family History

Principles of Chemoprevention • If 5 year risk > 1. 67% consider endocrine therapy for risk reduction (i. e. chemoprevention) • Duration of therapy 5 years • Choice of agents: – Tamoxifen – Raloxifene – Aromatase inhibitors – not currently approved

Principles of Increased Surveillance • If lifetime risk > 20% consider use of breast MRI • MRI used in conjunction with mammogram • Optimal schedule unknown – Commonly staggered every 6 months • Particularly useful for patients with dense breasts

Managing Hereditary Breast and Ovarian Cancer (HBOC) Risk
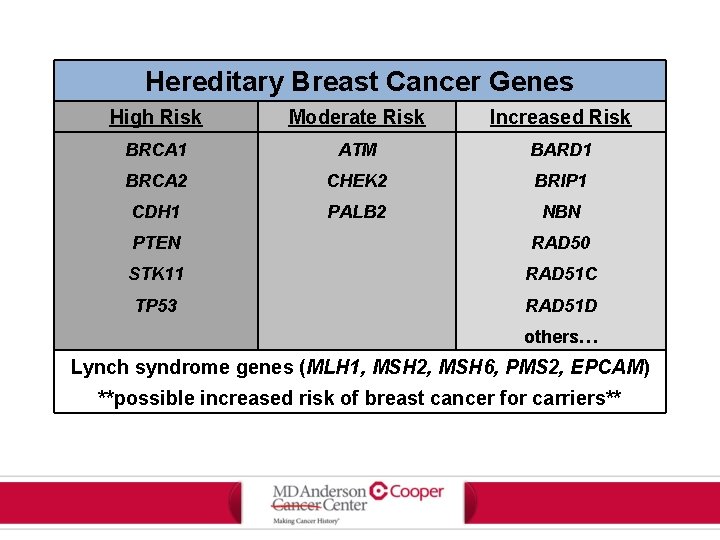
Hereditary Breast Cancer Genes High Risk Moderate Risk Increased Risk BRCA 1 ATM BARD 1 BRCA 2 CHEK 2 BRIP 1 CDH 1 PALB 2 NBN PTEN RAD 50 STK 11 RAD 51 C TP 53 RAD 51 D others… Lynch syndrome genes (MLH 1, MSH 2, MSH 6, PMS 2, EPCAM) **possible increased risk of breast cancer for carriers**
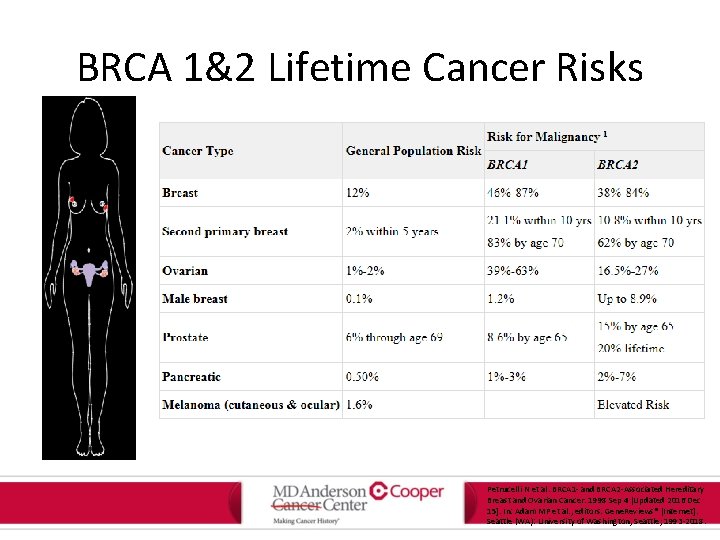
BRCA 1&2 Lifetime Cancer Risks Petrucelli N et al. BRCA 1 - and BRCA 2 -Associated Hereditary Breast and Ovarian Cancer. 1998 Sep 4 [Updated 2016 Dec 15]. In: Adam MP et al. , editors. Gene. Reviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993 -2018.

Prophylactic Mastectomy 639 FHx + s/p B/L prophylactic mastectomy 214 “high risk” ~14 year follow up Expected 156 Actual 3 425 “moderate risk” Expected 37. 4 Actual 4
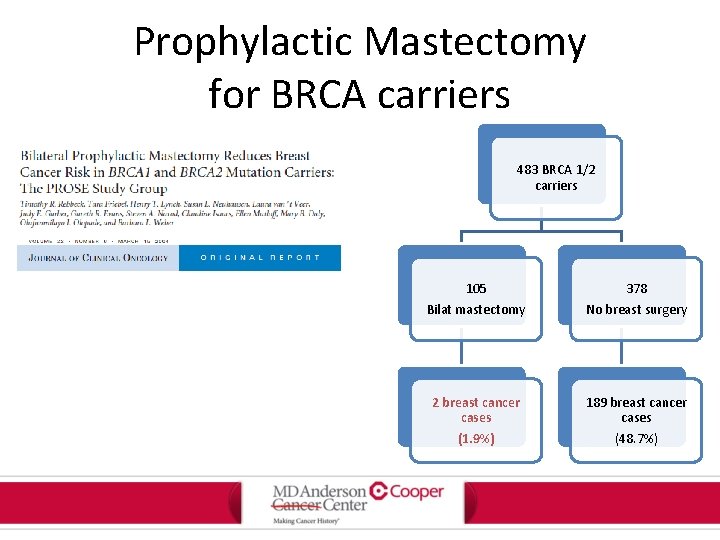
Prophylactic Mastectomy for BRCA carriers 483 BRCA 1/2 carriers 105 Bilat mastectomy 378 No breast surgery 2 breast cancer cases 189 breast cancer cases (1. 9%) (48. 7%)
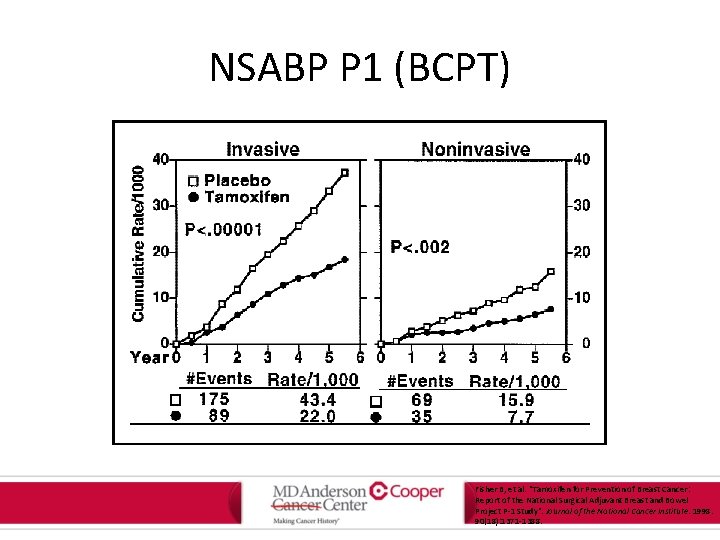
NSABP P 1 (BCPT) Fisher B, et al. "Tamoxifen for Prevention of Breast Cancer: Report of the National Surgical Adjuvant Breast and Bowel Project P-1 Study". Journal of the National Cancer Institute. 1998. 90(18): 1371 -1388.

Tamoxifen in BRCA Carriers • BRCA 1 – tend to be ER negative cancers – No risk reduction benefit of Tamoxifen (NSABP-P 1) • BRCA 2 – tend to be ER positive cancers – 62% risk reduction with tamoxifen (NSABP P 1) King M et al. Tamoxifen and Breast Cancer Incidence Among Women With Inherited Mutations in BRCA 1 and BRCA 2 National Surgical Adjuvant Breast and Bowel Project (NSABPP 1) Breast Cancer Prevention Trial. JAMA. 2001; 286(18): 2251– 2256

Risk Reducing Salpingo-Oophorectomy (RRSO) for BRCA carriers • 80% risk reduction in tumor of ovary or fallopian tube • Decreased mortality esp in BRCA 1 carriers • 4% incidence of finding occult malignancy • Reduction in breast cancer risk – Greatest benefit in BRCA 1 carriers who had RRSO ≤ age 40 Rebbeck TR et al. Meta-analysis of risk reduction estimates associated with risk-reducing salpingooopherectomy in BRCA 1 or 2 mutation carriers. J Natl Cancer Inst. 2009; 101: 80 -87. Sherman ME et al. Pathologic findings at risk-reducing salpingooopherectomy. J Clin Oncol. 2014; 32: 3275 -3283. Eisen A et al. Breast cancer risk following bilateral oophorectomy in BRCA 1 and 2 mutation carriers. J Clin Oncol 2005; 23: 74917496.
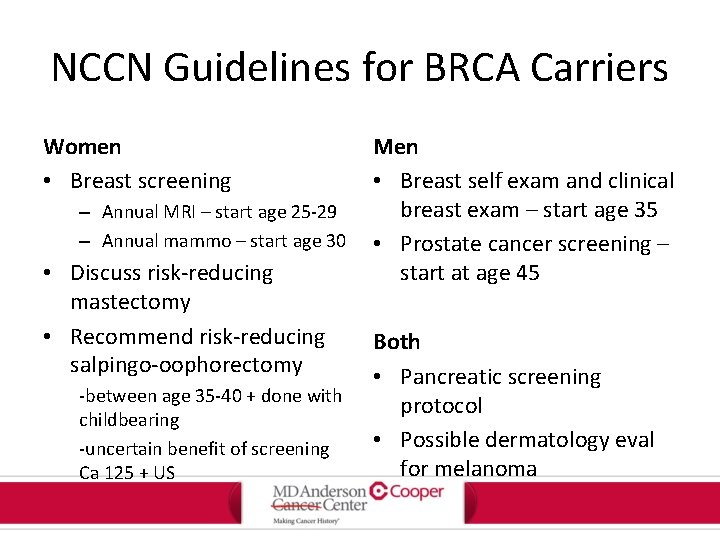

NCCN Guidelines for BRCA Carriers Women • Breast screening – Annual MRI – start age 25 -29 – Annual mammo – start age 30 • Discuss risk-reducing mastectomy • Recommend risk-reducing salpingo-oophorectomy -between age 35 -40 + done with childbearing -uncertain benefit of screening Ca 125 + US Men • Breast self exam and clinical breast exam – start age 35 • Prostate cancer screening – start at age 45 Both • Pancreatic screening protocol • Possible dermatology eval for melanoma

Cancer Genetics Program Practice Locations 2 Cooper Plaza, Camden 900 Centennial Blvd, Voorhees 100 Salem Drive, Willingboro Locations for Inspira patients: Vineland, Mickleton, Mullica Hill

Cancer Genetics Program Team Oncologists Generosa Grana, MD (Program Director) Christina Brus, MD Alexandre Hageboutros, MD A. Kamel Abou Hussein, MD Pallav Mehta, MD Jamin Morrison, MD Kumar Rajagopalan, MD Kanu Sharan, MD Robert Somer, MD Christian Squillante, MD Preeti Sudheendra, MD Advanced Practice Nurses (APNs) Jennifer Bonafiglia, APN-C Phyllis Duda, APN-C Kristi Kennedy, APN-C Helen Nichter, APN-C Evelyn Robles-Rodriguez, APN-C Genetic Counselors Brooke Levin, MS, LCGC Vanessa Manso, MS, LCGC Kristin Mattie, MS, LCGC Matthew Share, MS, LCGC Jennie Stone, MS, LCGC Program Staff Manager Evelyn Robles-Rodriguez, RN, MSN, APN, AOCN Administrative Coordinator Brandi Ford, CCMA, AAS (Camden) Medical Assistant Myra Salcedo, RMA (Camden)

- Slides: 23