CLINICAL APPROACH TO REFRACTIVE ERRORS Ayesha Abdullah 27

CLINICAL APPROACH TO REFRACTIVE ERRORS Ayesha Abdullah 27. 11. 2017

Learning objectives By the end of this lecture the students would be able to • Correlate optics with the underlying problem in various types of refractive errors & their correction with lenses • Describe the clinical presentation of refractive errors • Outline the clinical protocol for the assessment of refractive errors 2

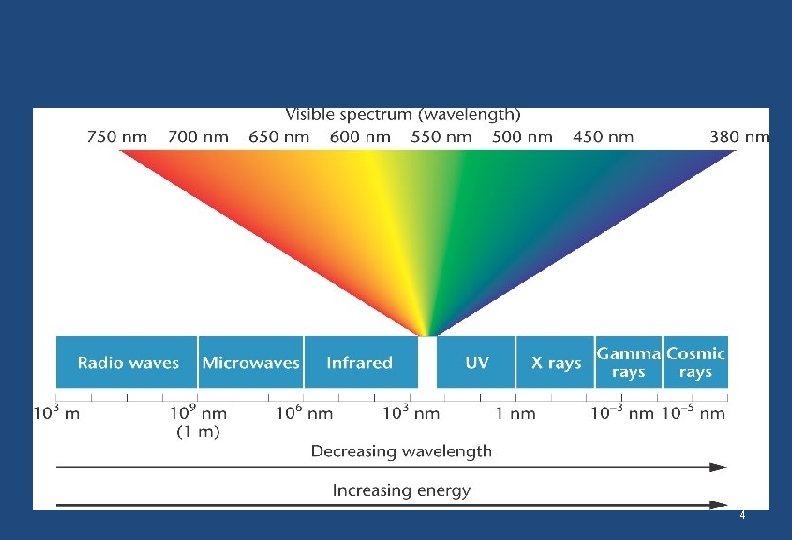
To begin with �Light ? �Refraction ? �Main refractive surface of the eye? �Why is it so? �How much is the refractive power of the cornea? �Refractive errors? �How much is the role of lens in refraction? �What is the role of accommodation in refraction? 3
4

What is Emmetropia & Ametropia? • The state of having no refractive error is emmetropia • A Balanced state of refractive power of the cornea, lens and the length of the eyeball • Parallel rays of light are brought to a focus on the fovea when the eye is not accommodating • The state of the eye when parallel rays of light are not focused on the fovea with the accommodation relaxed is called ametropia 5
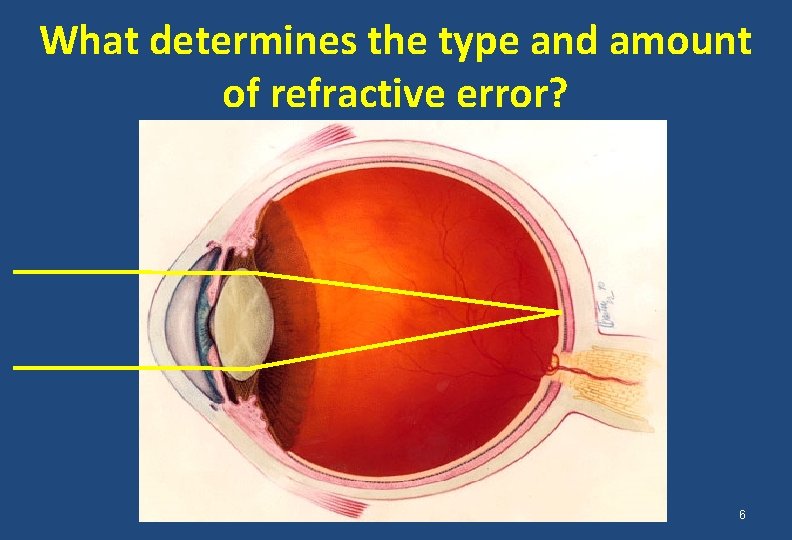
What determines the type and amount of refractive error? 6

What determines the type and amount of refractive error? An interplay among ücorneal power, CAAL ülens power, üanterior chamber depth, üaxial length Determines an individual’s refractive status 7
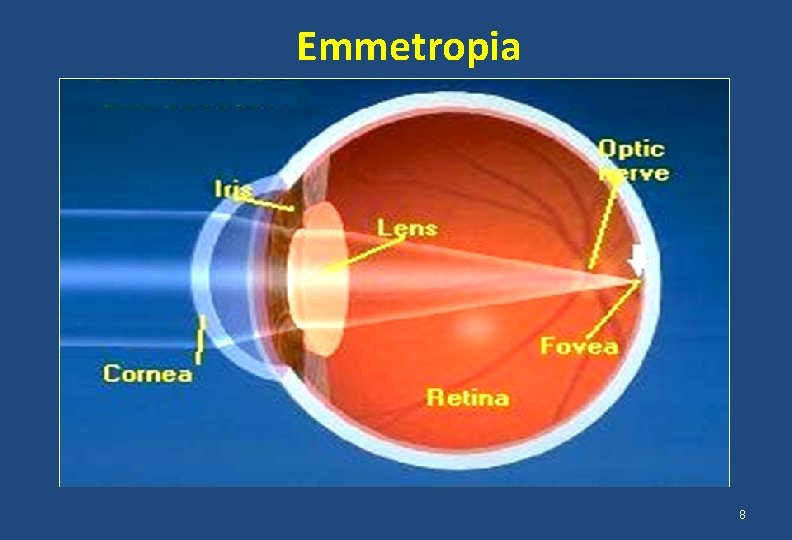
Emmetropia 8

What determines the type and amount of refractive error? • Refractive errors of up to 5 D are considered to be biological variation • Higher degrees of refractive errors can be associated with structural anomalies of the ocular structures e. g. the cornea, lens, choroid and the retina 9

Ametropia When parallel rays of light are NOT brought to a focus onto the retina Ametropia could be ü Axial ü Curvature ü Index CIA 10

Types of Ametropia • Myopia, common in young age group • Hyperopia, common in very young children & old age • Astigmatism; common in young age group but less common than myopia 11
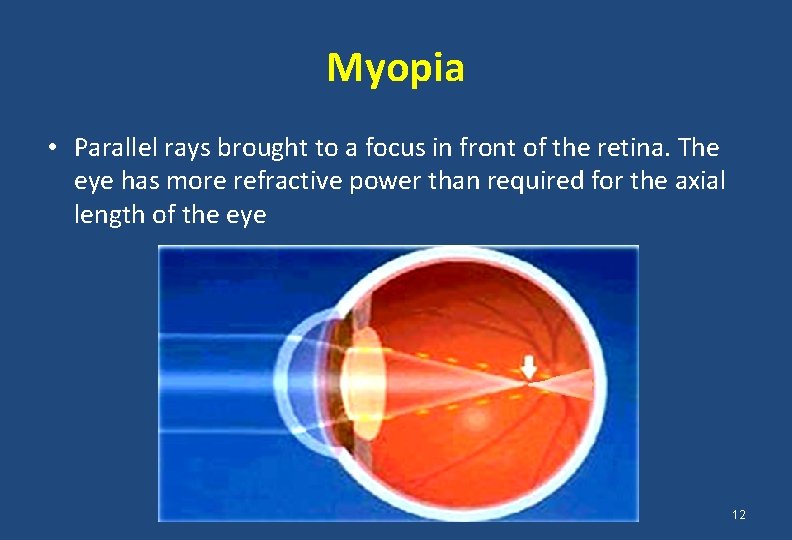
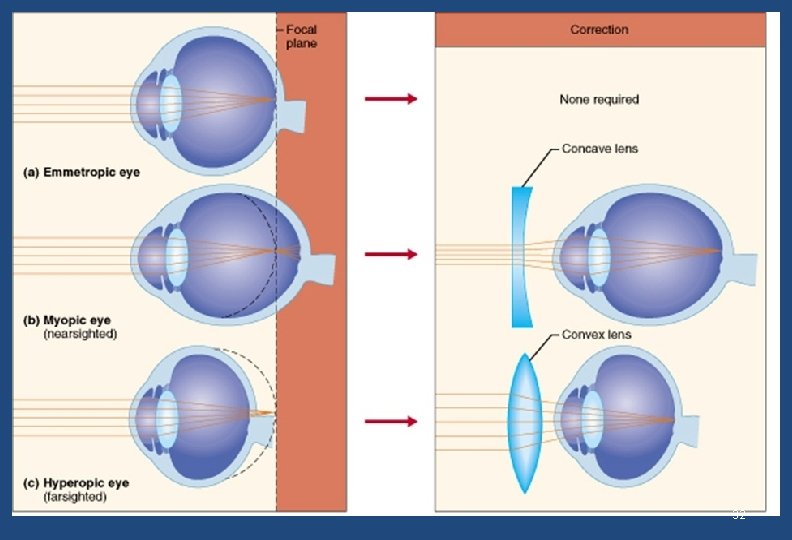
Myopia • Parallel rays brought to a focus in front of the retina. The eye has more refractive power than required for the axial length of the eye 12

Simple Myopia Usual onset by adolescence but may begin as late as 25 years of age. Gradually increases until the eye is fully grown Seldom exceeds -6 dioptres. 13

Pathological myopia • Commonly begins as physiological but rather than stabilizing when adult size of the eyeball is achieved, the eye continues to enlarge. • It is associated with pathological changes in the posterior segment that can be seen on Ophthalmoscopy • It can lead to complications like retinal breaks and detachment • Can go upto over -20 diopters 14
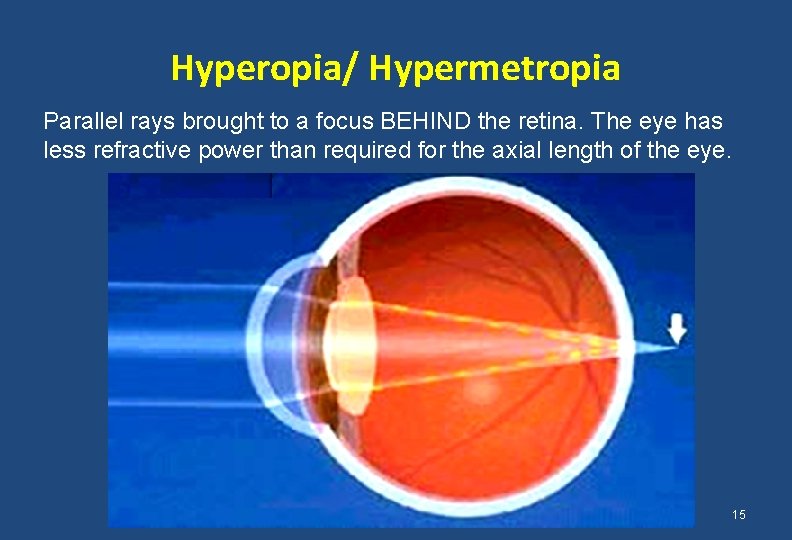
Hyperopia/ Hypermetropia Parallel rays brought to a focus BEHIND the retina. The eye has less refractive power than required for the axial length of the eye. 15

Hyperopia • Manifest • Latent or Hidden • At birth practically all eyes are hypermetropic to the extent of +2. 5 to +3. 0 diopters. • Emmetropisation occurs as the eye grows. • Emmetropia may not be reached and hypermetropia may persist. 16
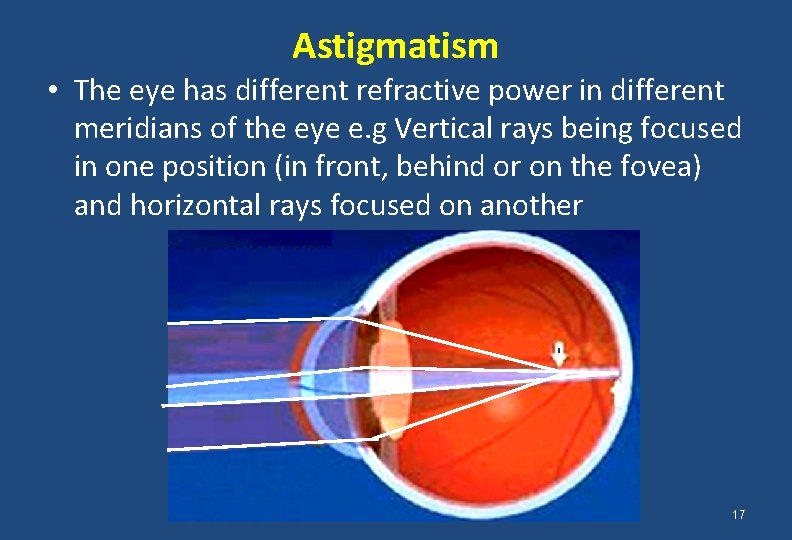
Astigmatism • The eye has different refractive power in different meridians of the eye e. g Vertical rays being focused in one position (in front, behind or on the fovea) and horizontal rays focused on another 17
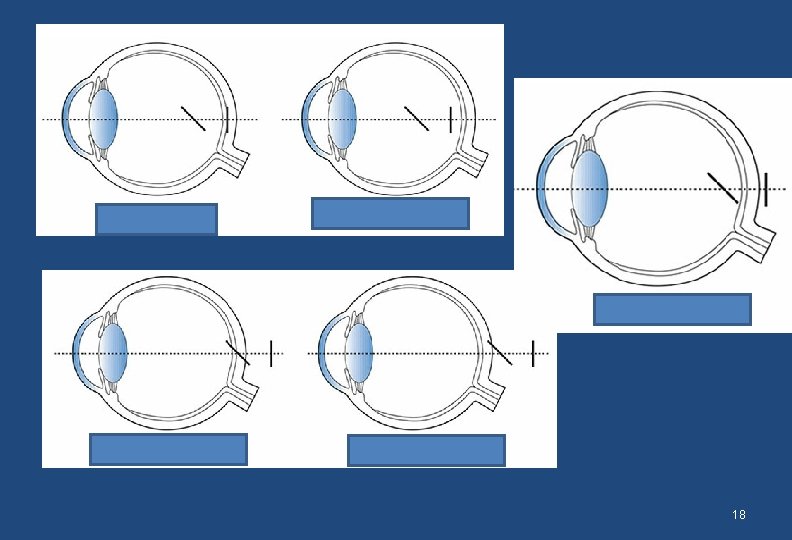
18

How do refractive errors present? • Asthenopia , eyestrain & visual fatigue • Blurring of vision • Ocular discomfort with itching, burning of the eyes and at times increased sensitivity to light etc • Headache presenting after visual work especially in those above 40 years could be because of RE, however a headache presenting early morning is extremely unlikely to be because of RE 19

http: //www. richmondeye. com/simulations-of-eye-disorders/ 20

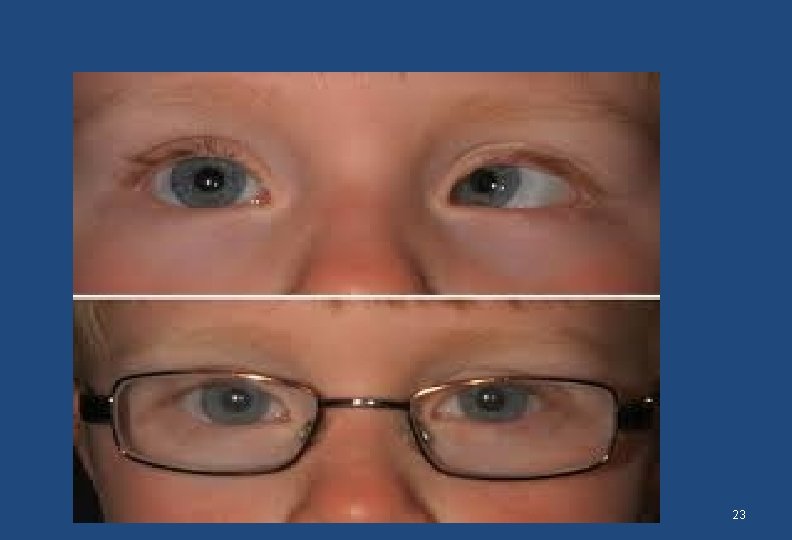
In Pre-school children • Can present in a variety of ways • In preverbal children it can present as delayed milestones of visual development; inability to focus at visually stimulating objects, follow light or bright object • Squint • Lazy eye or eyes 21

In school going children • Lack of interest in visual tasks, class work • Generally apathic or withdrawn behaviour • Difficulty in reading or seeing the black/ white board from distance • Squint • Lazy eye 22
23
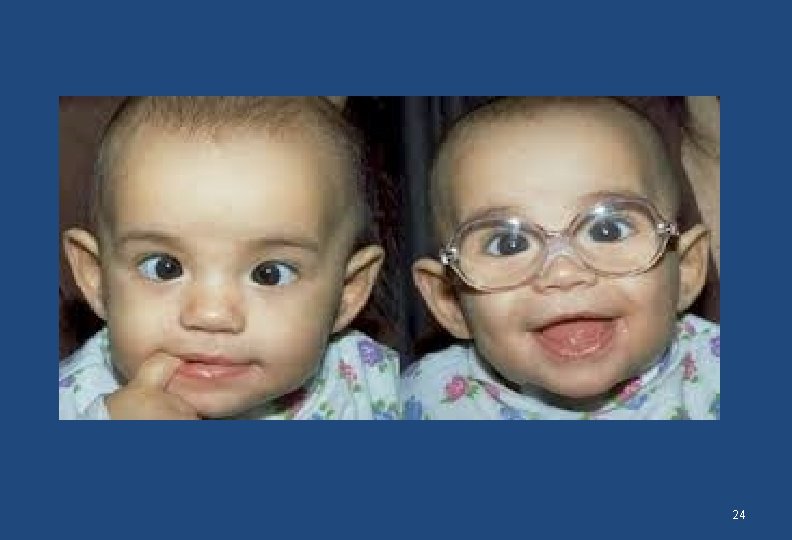
24

Signs • Decreased visual acuity that improves with pinhole • The eyeball may be obviously small (hyperopia) or large (myopia) • The cornea my be conical in shape (irregular astigmatism (keratoconus) • Pupils are normal • Posterior segment may show abnormalities 25
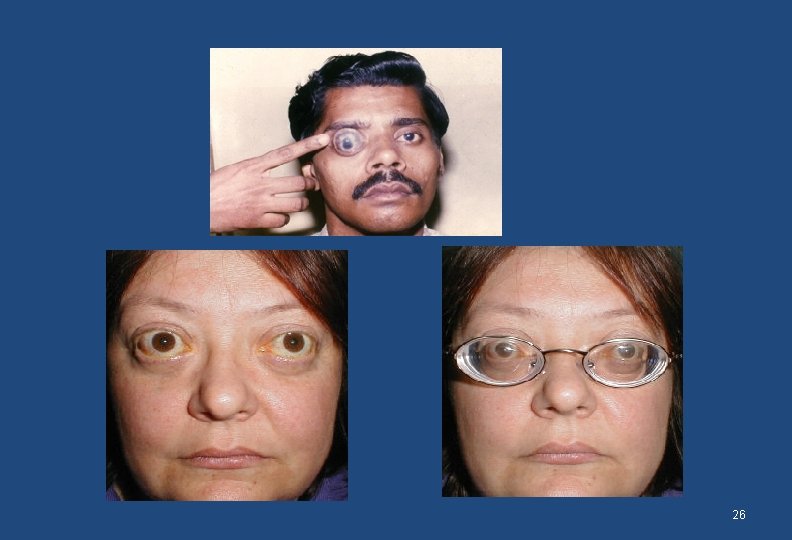
26
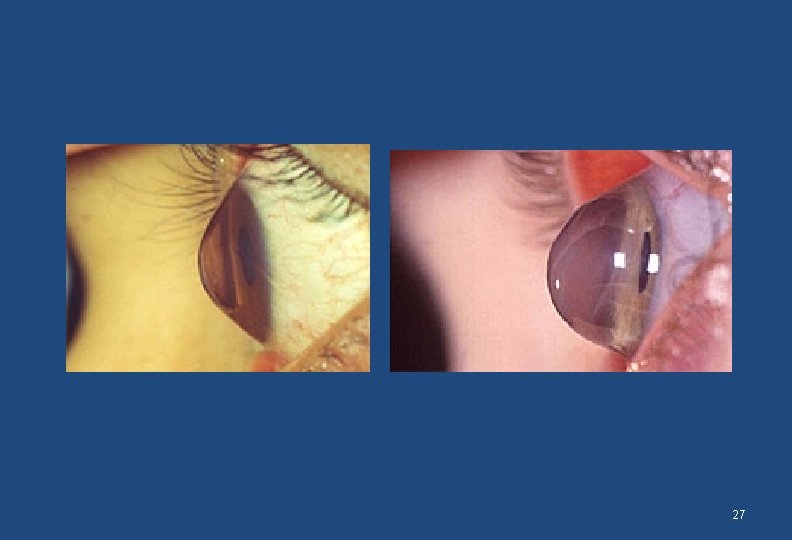
27
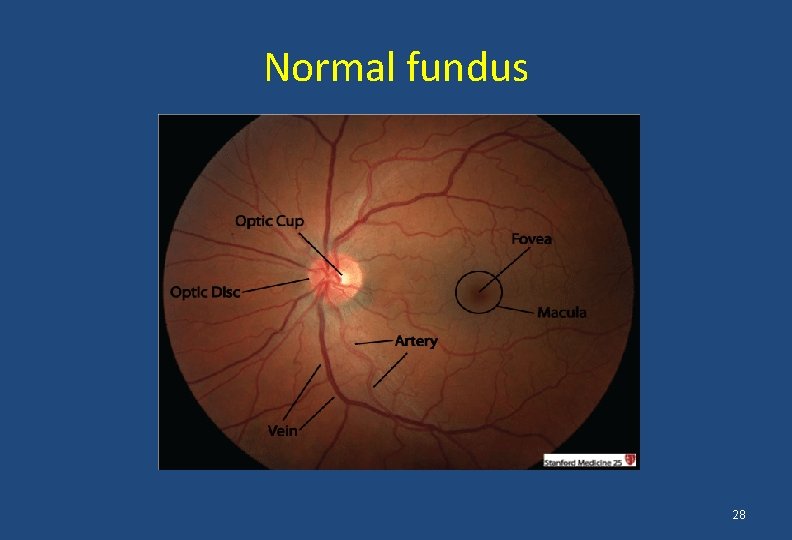
Normal fundus 28
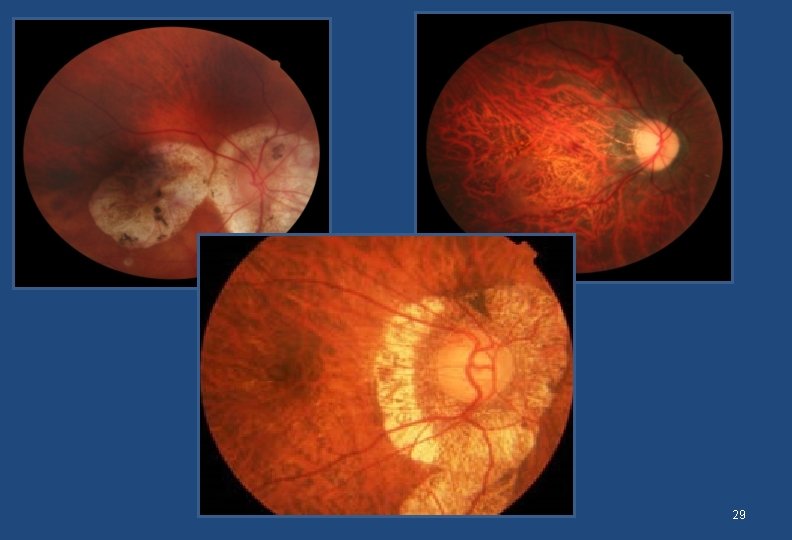
29
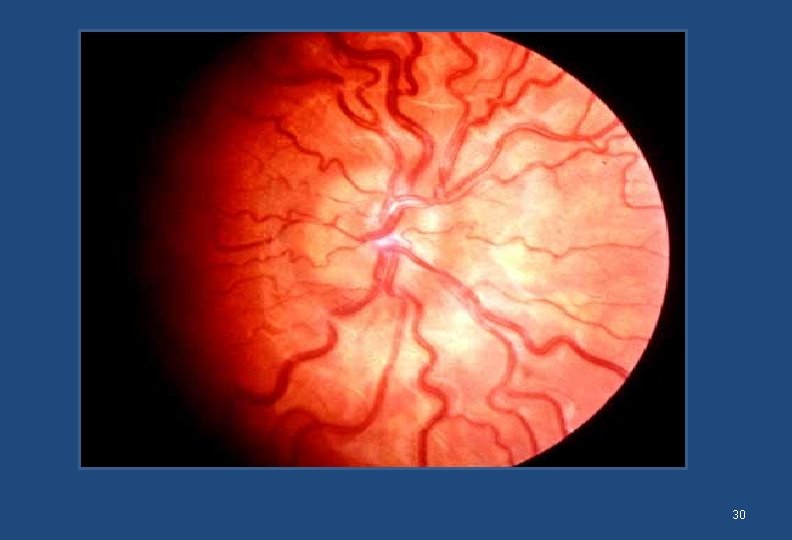
30

Treatment of RE • Spectacles • Contact lens • Refractive surgery 31
32
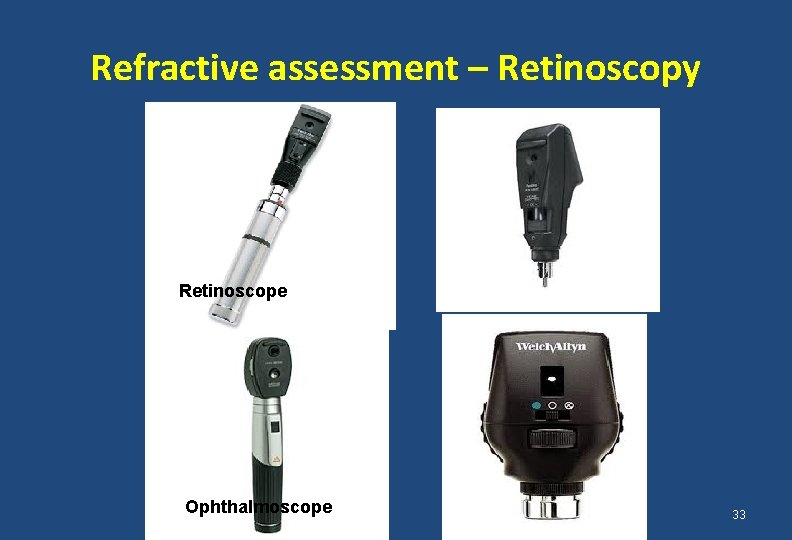
Refractive assessment – Retinoscopy Retinoscope Ophthalmoscope 33
Retinoscopy/ manual refraction 34

Autorefraction 35

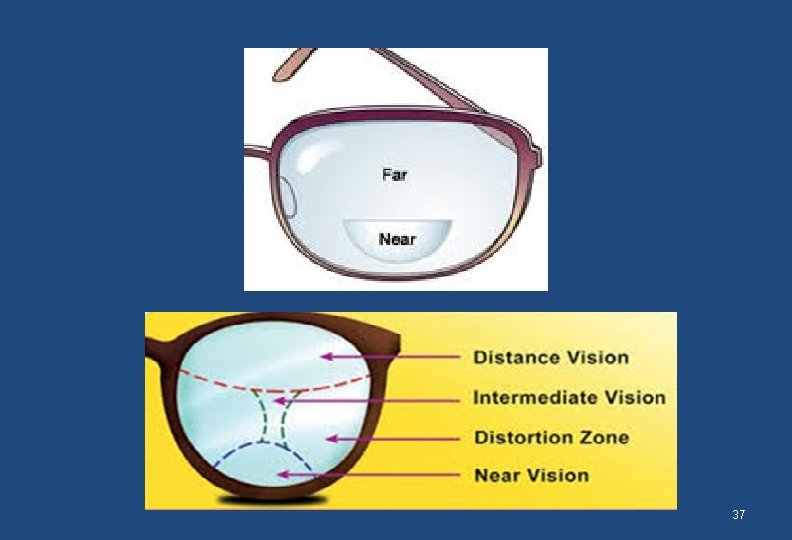
Presbyopia • What is Presbyopia? • Physiological failure of the lens to accommodation due to – hardening of lens with age – weakness of ciliary’s muscle and suspensory ligament • How is it corrected? • Suitable spherical lens for near work • A plus lens or a lesser minus lens 36
37

• Which of the following types of refractive error varies in different meridia A. B. C. D. Myopia Hyperopia Astigamtism Presbyopia 38

• Which of the following is the least invasive procedure for the correction or refractive errors A. B. C. D. E. Spectacles Contact lenses Laser refractive surgery Reractive surgery Clear lens extraction 39

• Which of the following is most useful in the diagnosis of refractive error A. B. C. D. E. Assessment of distance VA Assessment of Near VA Assessment of Pupils Assessment of pinhole VA Ophthalmoscopy 40
- Slides: 40