Clinical and radiological presentation and diagnosis David W


























- Slides: 73

Clinical and radiological presentation and diagnosis David W. Denning National Aspergillosis Centre University Hospital South Manchester [Wythenshawe Hospital] University of Manchester

The National Aspergillosis Centre 225 -250 new patients with aspergillosis referred annually

CLASSIFICATION OF ASPERGILLOSIS Airways/nasal exposure to airborne Aspergillus Persistence without disease - colonisation of the airways or nose/sinuses Invasive aspergillosis • Acute (<1 month course) • Subacute/chronic necrotising (1 -3 months) Chronic aspergillosis (>3 months) • Chronic cavitary pulmonary • Aspergilloma of lung • Chronic fibrosing pulmonary • Chronic invasive sinusitis • Maxillary (sinus) aspergilloma Allergic • Allergic bronchopulmonary (ABPA) • Extrinsic allergic (broncho)alveolitis (EAA) • Asthma with fungal sensitisation • Allergic Aspergillus sinusitis (eosinophilic fungal rhinosinusitis)

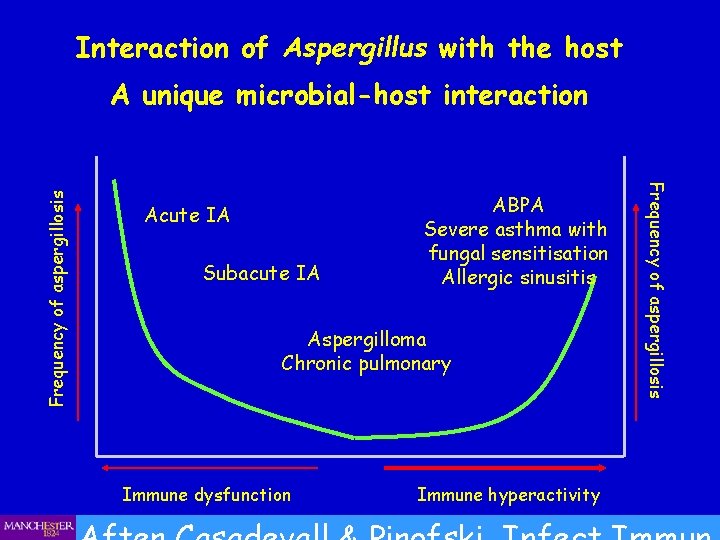
Interaction of Aspergillus with the host Acute IA Subacute IA ABPA Severe asthma with fungal sensitisation Allergic sinusitis Aspergilloma Chronic pulmonary Immune dysfunction Immune hyperactivity . Frequency of aspergillosis A unique microbial-host interaction

Size of Aspergillus disease problem globally 1. 2. 3. 4. Over 200, 000 patients develop IA annually. Key groups include ~10% of acute leukaemia (30, 000) and stem cell and other transplants (7, 500) and 1. 3% of COPD patients admitted to hospital (60, 000 IA cases). Chronic pulmonary aspergillosis after TB – 1. 1 M cases prevalence Chronic pulmonary aspergillosis total - ~3 M Asthma 197 M in adults, of which ~10 -20% severe, UK and USA have very high prevalence rates

How common is ABPA in asthma? 10/1390 (0. 72%) 9/255 (3. 5%) 6/264 (2. 3%) Donnelly, Irish J Med Sci 1991; 160: 288; Eaton, Chest 2000; 118: 66; Al-Mobeireek, Resp Med 2001; 98: 341

Size of Aspergillus disease problem globally 1. 2. 3. 4. 5. 6. Over 200, 000 patients develop IA annually. Key groups include ~10% of acute leukaemia (30, 000) and stem cell and other transplants (7, 500) and 1. 3% of COPD patients admitted to hospital (60, 000 IA cases). Chronic pulmonary aspergillosis after TB – 1. 1 M cases prevalence Chronic pulmonary aspergillosis total - ~3 M Asthma 197 M in adults, of which ~10 -20% severe, UK and USA have very high prevalence rates Allergic bronchopulmonary aspergillosis in asthma - ~4 M worldwide (2. 1% of adults referred with asthma) Severe asthma with fungal sensitisation - ~6 M worldwide (33% of 10% (severe only))

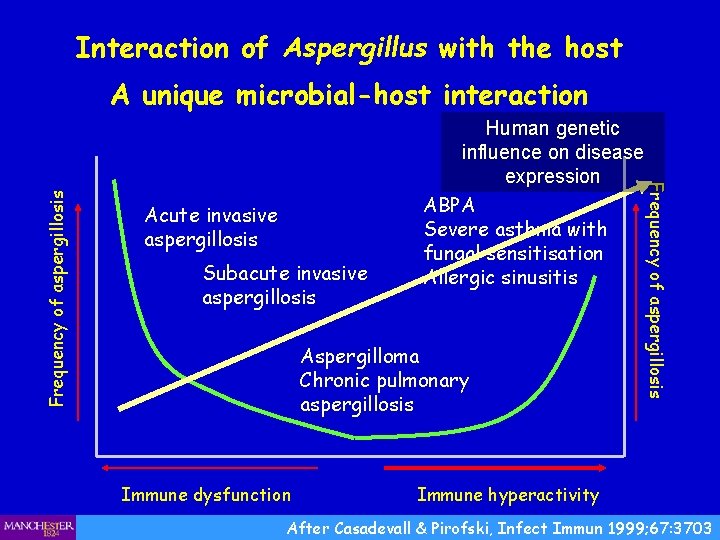
Interaction of Aspergillus with the host Acute invasive aspergillosis Subacute invasive aspergillosis Human genetic influence on disease expression ABPA Severe asthma with fungal sensitisation Allergic sinusitis Aspergilloma Chronic pulmonary aspergillosis Immune dysfunction Frequency of aspergillosis A unique microbial-host interaction Immune hyperactivity . After Casadevall & Pirofski, Infect Immun 1999; 67: 3703

Chronic Pulmonary Aspergillosis

Common symptoms • Cough, usually productive • Shortness of breath • Weight loss • Tiredness • Coughing up blood • Chest ache / discomfort Occasionally • Fever • Severe chest pain from rib fracture • Additional chest infections • Angina and heart attacks (chronic inflammation)

Underlying diseases 9 patients with chronic cavitary pulmonary aspergillosis 15 with chronic necrotising pulmonary aspergillosis Camuset et al, Chest 2007: 131: 1435

Underlying diseases - CPA • Classical tuberculosis * • Atypical tuberculosis * • Allergic bronchopulmonary aspergillosis * • Lung cancer survivor * • Pneumothorax * • COPD/emphysema * • Sarcoidosis (stage II/III) * • Rheumatoid arthritis • Thoracic surgery • Asthma • Chest radiotherapy • None * Common Smith, ISHAM 2009

Chronic pulmonary aspergillosis – -existing disease pre Prior pulmonary disease esp: Atypical mycobacteria pulmonary infection Sarcoidosis Tuberculosis Recurrent pneumothorax Prior pulmonary surgery ABPA Denning DW et al, Clin Infect Dis 2003; 37: S 265

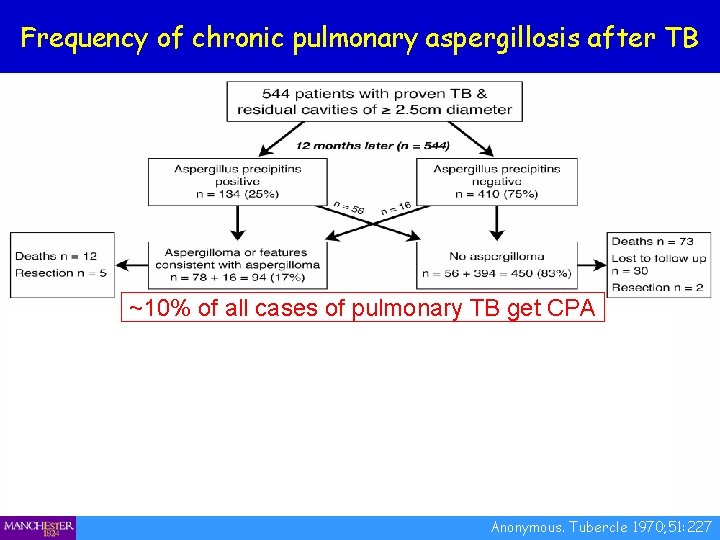
Frequency of chronic pulmonary aspergillosis after TB ~10% of all cases of pulmonary TB get CPA Anonymous. Tubercle 1970; 51: 227

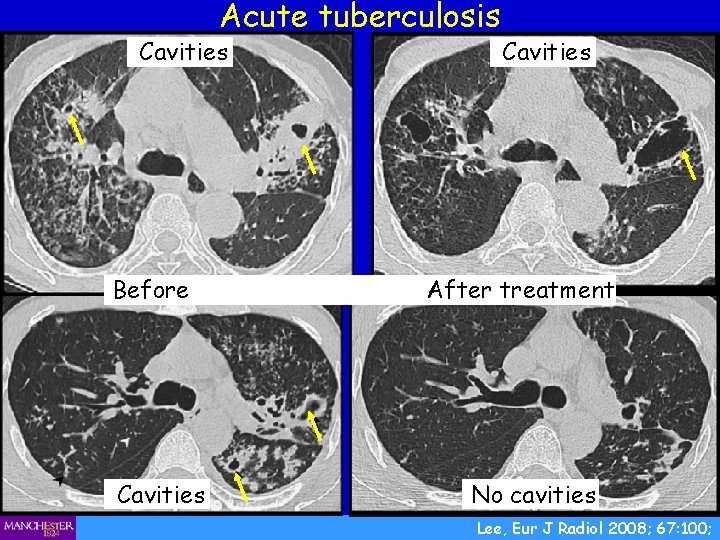
Acute tuberculosis Cavities Before Cavities After treatment No cavities Lee, Eur J Radiol 2008; 67: 100;

Chronic pulmonary aspergillosis Infection of the lung by Aspergillus Single fungal ball or aspergilloma in a preexisting cavity

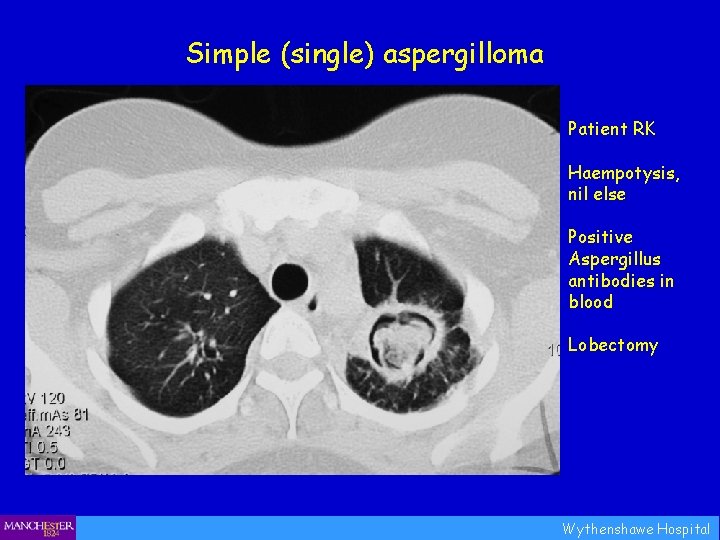
Simple (single) aspergilloma Patient RK Haempotysis, nil else Positive Aspergillus antibodies in blood Lobectomy Wythenshawe Hospital

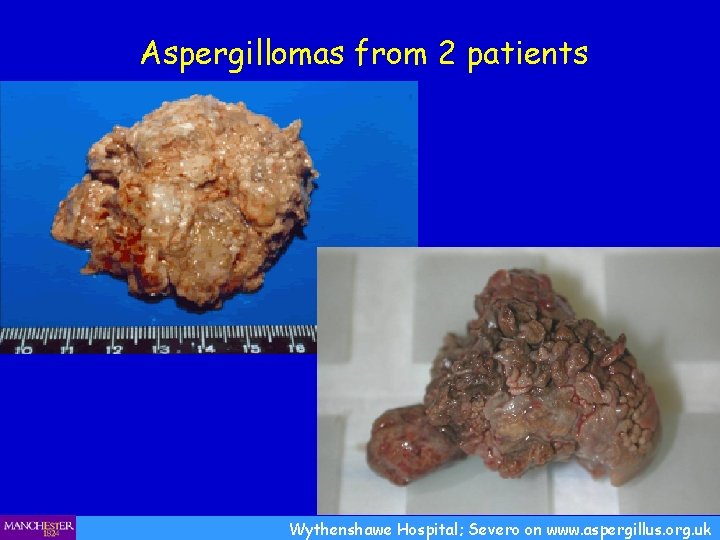
Aspergillomas from 2 patients Wythenshawe Hospital; Severo on www. aspergillus. org. uk

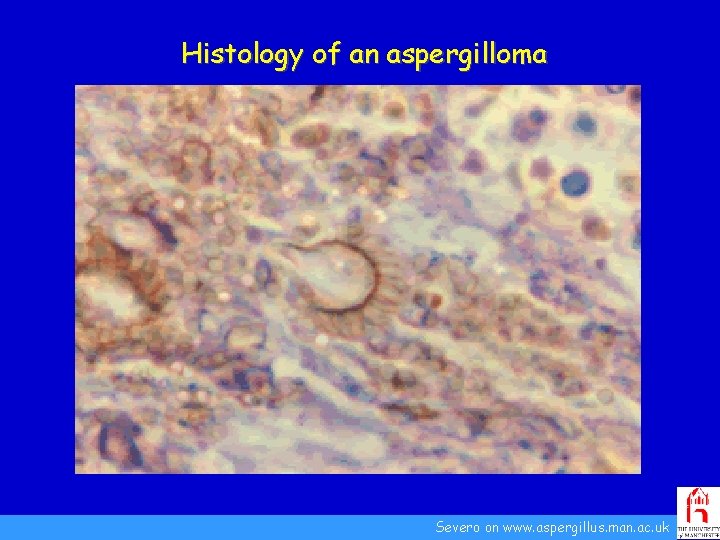
Histology of an aspergilloma Severo on www. aspergillus. man. ac. uk

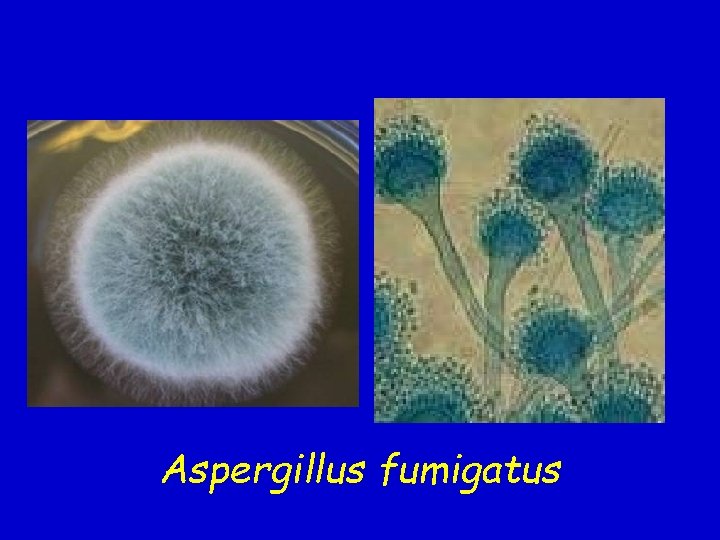
Aspergillus fumigatus

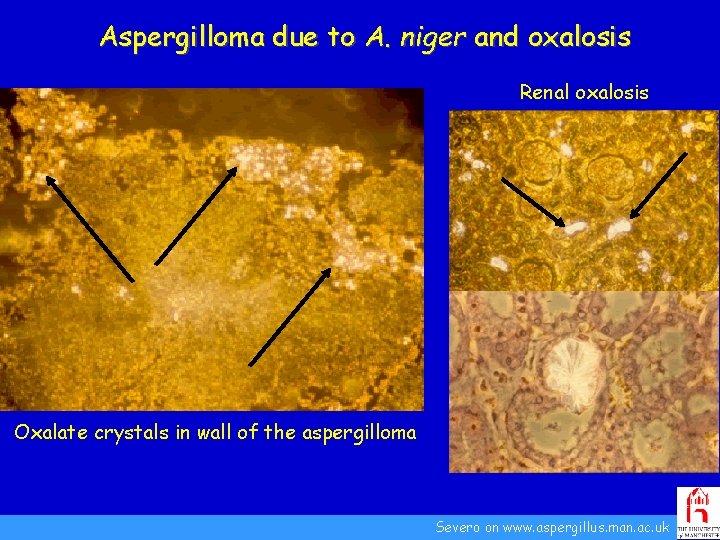
Aspergilloma due to A. niger and oxalosis Renal oxalosis Oxalate crystals in wall of the aspergilloma Severo on www. aspergillus. man. ac. uk

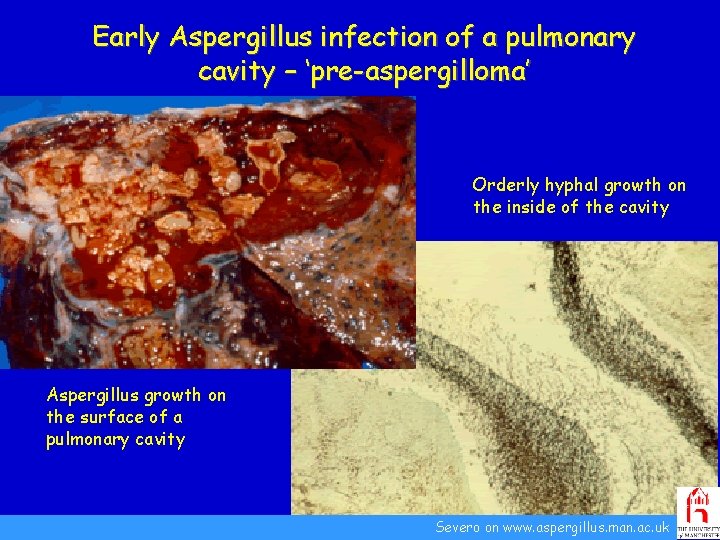
Early Aspergillus infection of a pulmonary cavity – ‘pre-aspergilloma’ Orderly hyphal growth on the inside of the cavity Aspergillus growth on the surface of a pulmonary cavity Severo on www. aspergillus. man. ac. uk

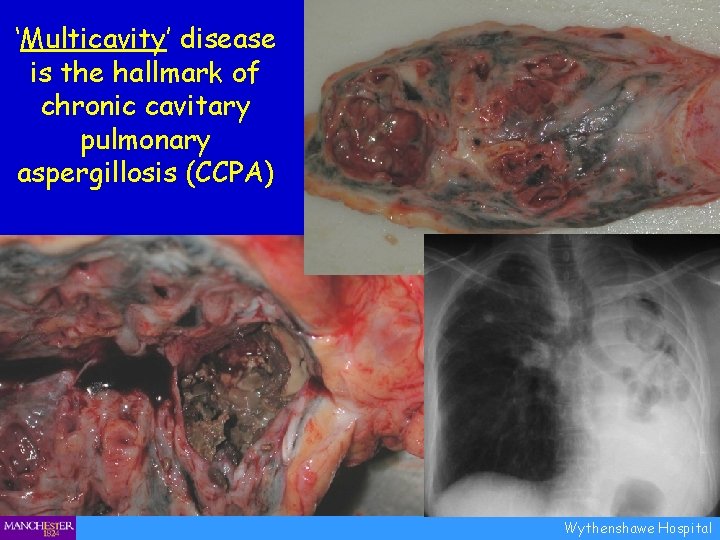
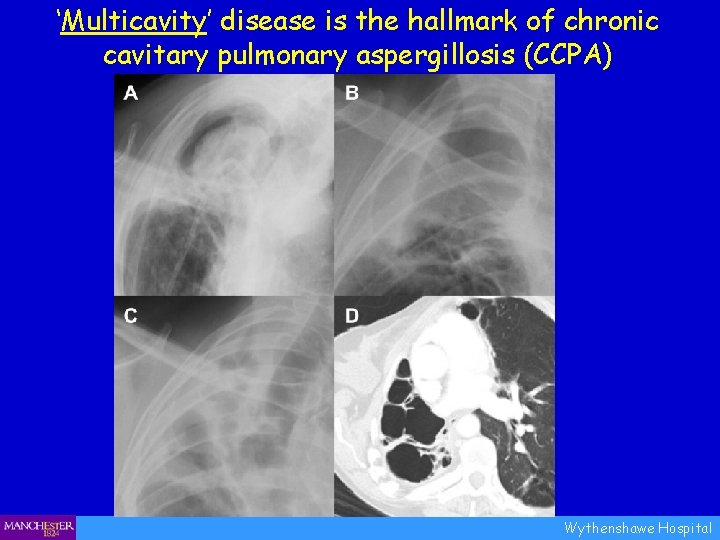
‘Multicavity’ disease is the hallmark of chronic cavitary pulmonary aspergillosis (CCPA) Wythenshawe Hospital

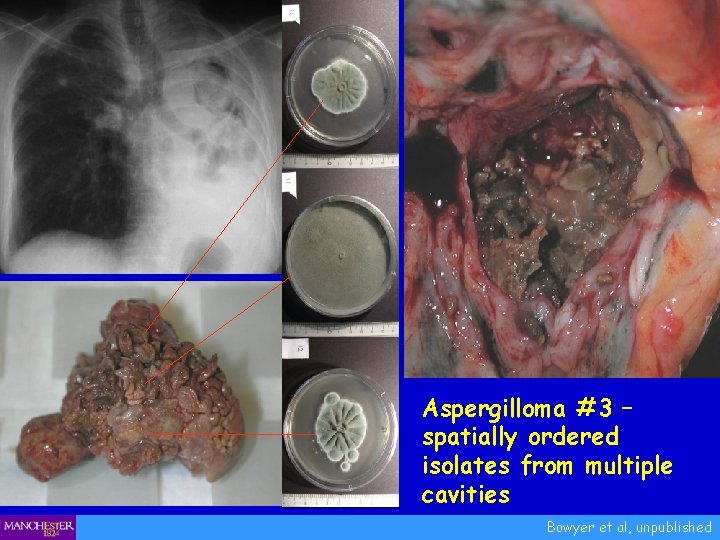
Aspergilloma #3 – spatially ordered isolates from multiple cavities Bowyer et al, unpublished

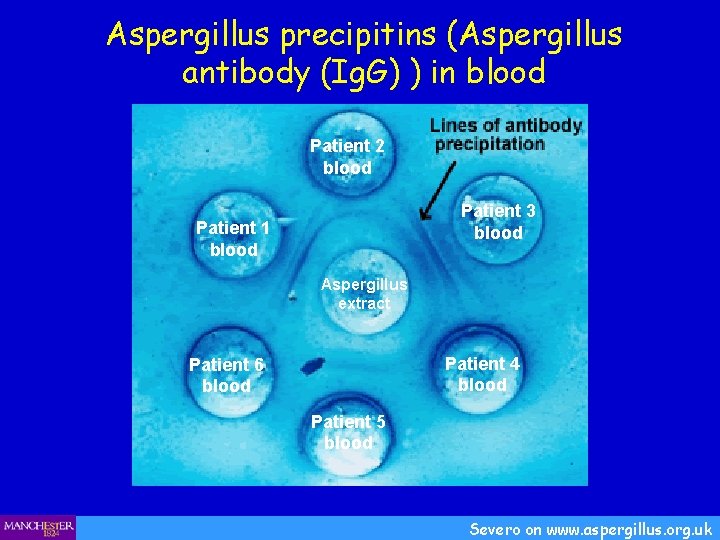
Aspergillus precipitins (Aspergillus antibody (Ig. G) ) in blood Patient 2 blood Patient 3 blood Patient 1 blood Aspergillus extract Patient 4 blood Patient 6 blood Patient 5 blood Severo on www. aspergillus. org. uk

Aspergillus Ig. G serology Baxter, AAA 2010; Abstr 51

Chronic pulmonary aspergillosis serology All 18 patients had positive Aspergillus precipitins (1+-4+) All 18 patients had elevated inflammatory markers, CRP, PV and / or ESR May have elevated total Ig. E and Aspergillus specific Ig. E (RAST) Only 40% have a positive sputum culture Denning DW et al, Clin Infect Dis 2003; 37: S 265

Chronic pulmonary aspergillosis Infection of the lung by Aspergillus Single fungal ball or aspergilloma in a preexisting cavity Chronic cavitary pulmonary aspergillosis +/- fungal ball

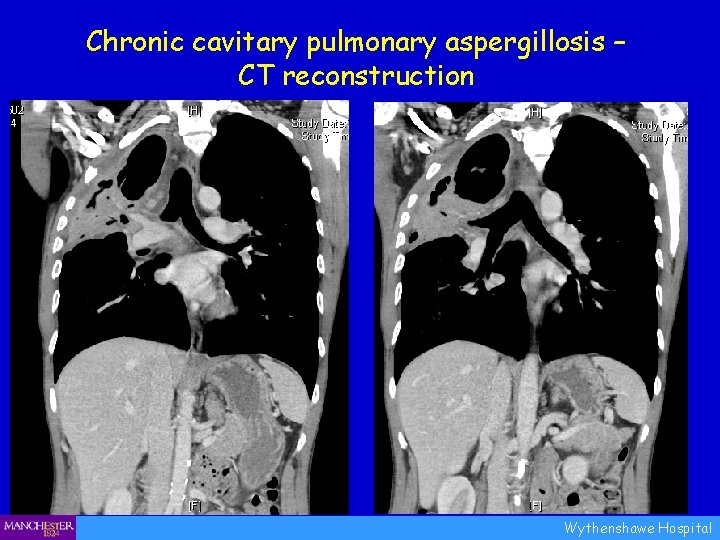
Chronic cavitary pulmonary aspergillosis – CT reconstruction Wythenshawe Hospital

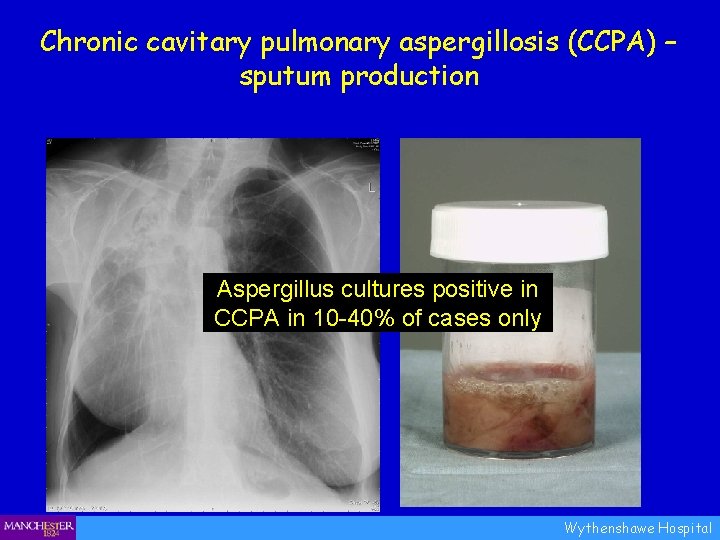
Chronic cavitary pulmonary aspergillosis (CCPA) – sputum production Aspergillus cultures positive in CCPA in 10 -40% of cases only Wythenshawe Hospital

‘Multicavity’ disease is the hallmark of chronic cavitary pulmonary aspergillosis (CCPA) Wythenshawe Hospital

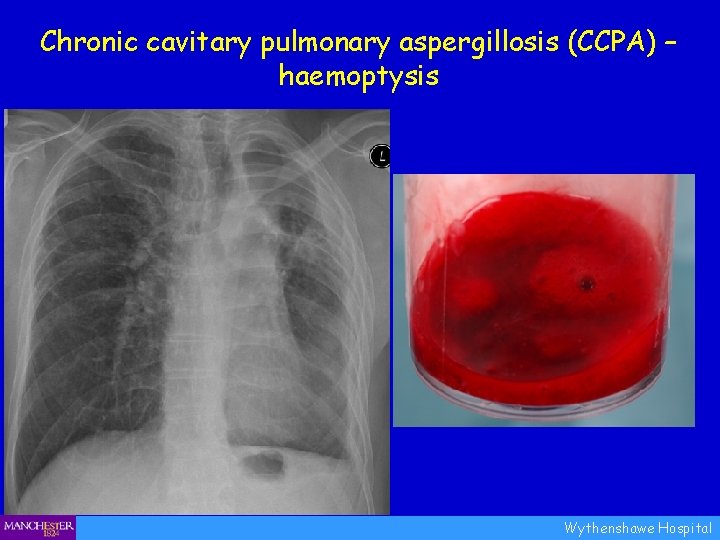
Chronic cavitary pulmonary aspergillosis (CCPA) – haemoptysis Wythenshawe Hospital

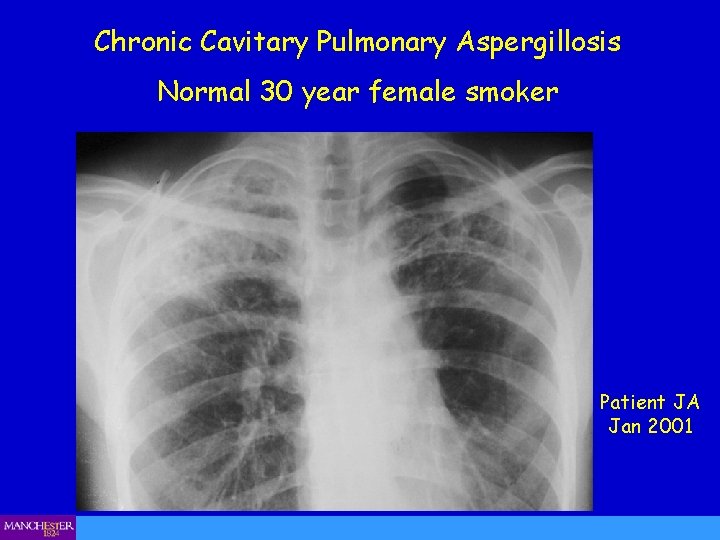
Chronic Cavitary Pulmonary Aspergillosis Normal 30 year female smoker Patient JA Jan 2001

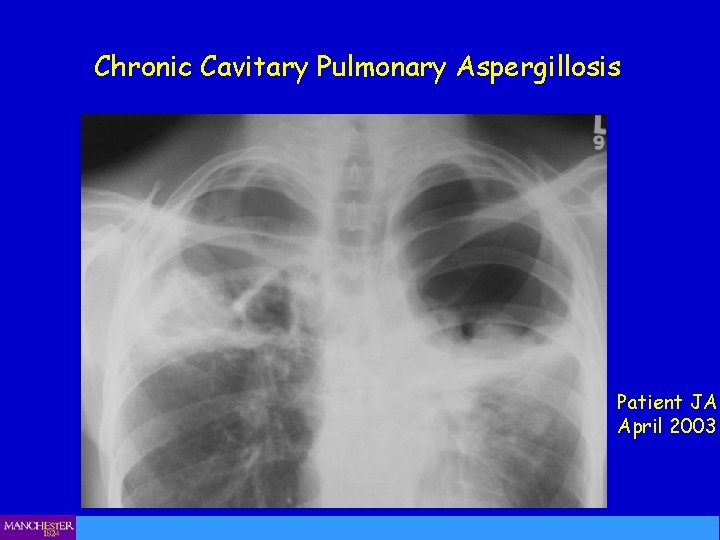
Chronic Cavitary Pulmonary Aspergillosis Patient JA April 2003

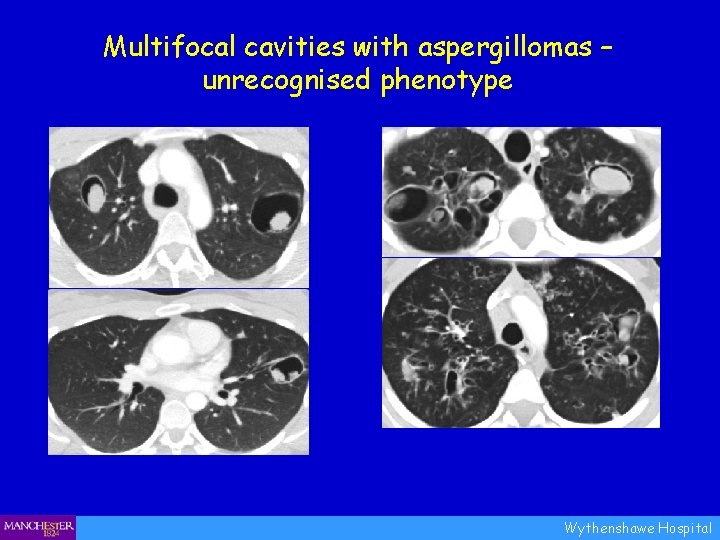
Multifocal cavities with aspergillomas – unrecognised phenotype Wythenshawe Hospital

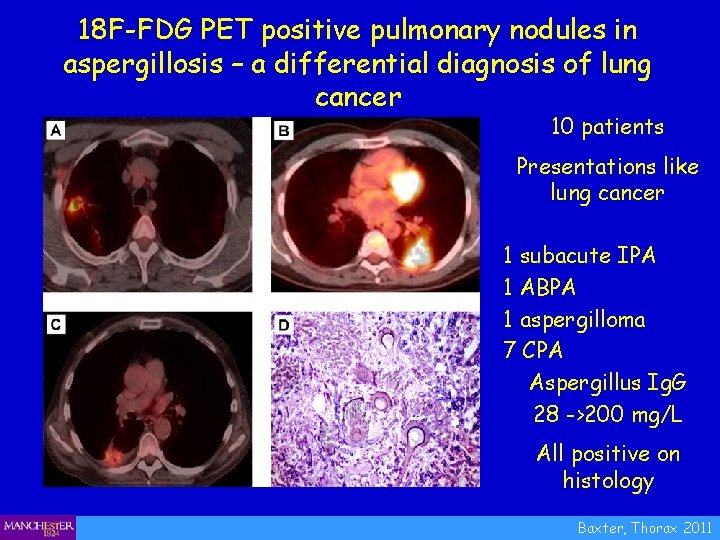
18 F-FDG PET positive pulmonary nodules in aspergillosis – a differential diagnosis of lung cancer 10 patients Presentations like lung cancer 1 subacute IPA 1 ABPA 1 aspergilloma 7 CPA Aspergillus Ig. G 28 ->200 mg/L All positive on histology Baxter, Thorax 2011

CLASSIFICATION OF ASPERGILLOSIS Airways/nasal exposure to airborne Aspergillus Persistence without disease - colonisation of the airways or nose/sinuses Invasive aspergillosis • Acute (<1 month course) • Subacute/chronic necrotising (1 -3 months) Chronic aspergillosis (>3 months) • Chronic cavitary pulmonary • Aspergilloma of lung • Chronic fibrosing pulmonary • Chronic invasive sinusitis • Maxillary (sinus) aspergilloma Allergic • Allergic bronchopulmonary (ABPA) • Extrinsic allergic (broncho)alveolitis (EAA) • Asthma with fungal sensitisation • Allergic Aspergillus sinusitis (eosinophilic fungal rhinosinusitis)

Allergic Bronchopulmonary Aspergillosis

ABPA – Diagnostic clues • Asthma/CF not well controlled • History of ‘pneumonia’ • History of coughing up plugs, or paroxysms of coughing that clear when chest clears • Central bronchiectasis on CT scan, or mucoid impaction • Eosinophilia Rare cases in non-asthmatics, non-CF patients

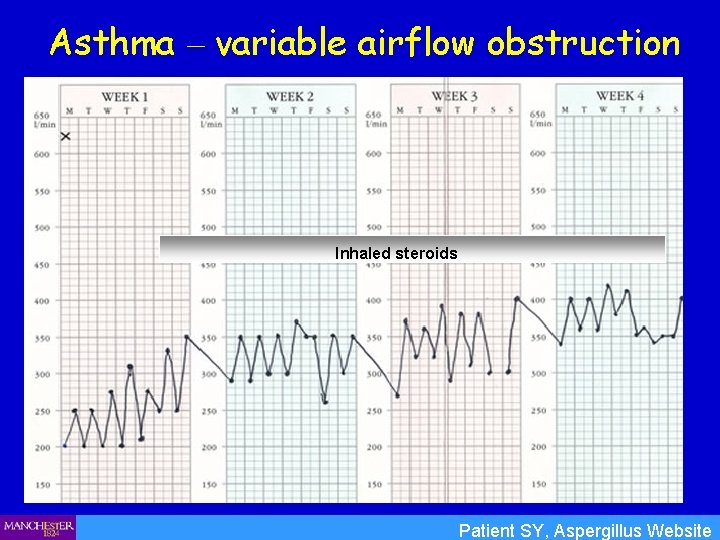
Asthma – variable airflow obstruction Inhaled steroids Patient SY, Aspergillus Website

Proposed new criteria for ABPA 1. 2. 3. Serum Ig. E >1000 IU/m. L Asthma OR CF Airway obstruction (ie CT scan/bronchoscopy) by or production of mucus plugs containing hyphae Which fungus? 1. Fungal sensitisation (Ig. E or SPT) and/or fungus detected in respiratory secretions Knutsen et al, AAAAI Task Force on Fungus and Asthma

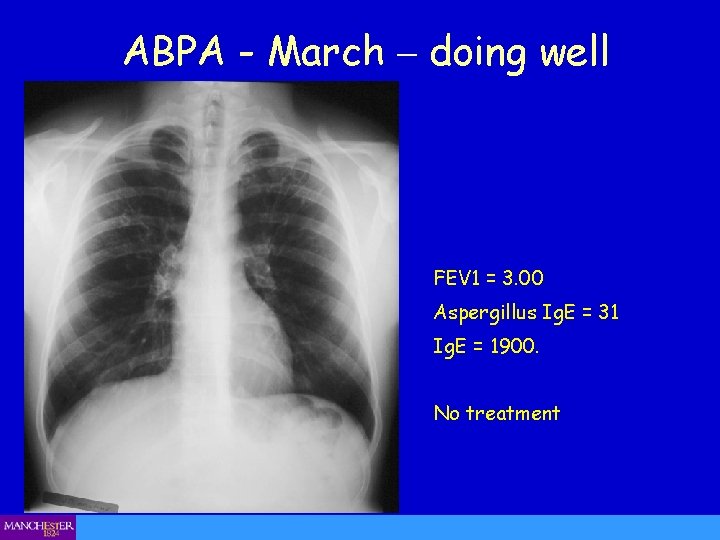
ABPA - March – doing well FEV 1 = 3. 00 Aspergillus Ig. E = 31 Ig. E = 1900. No treatment

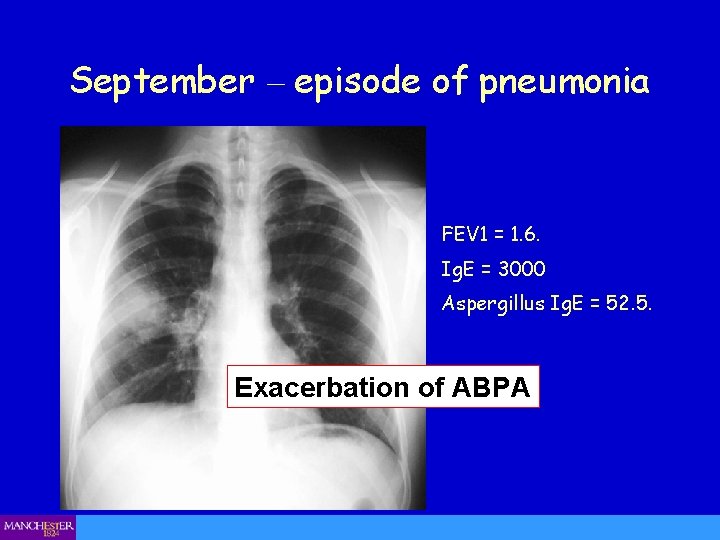
September – episode of pneumonia FEV 1 = 1. 6. Ig. E = 3000 Aspergillus Ig. E = 52. 5. Exacerbation of ABPA

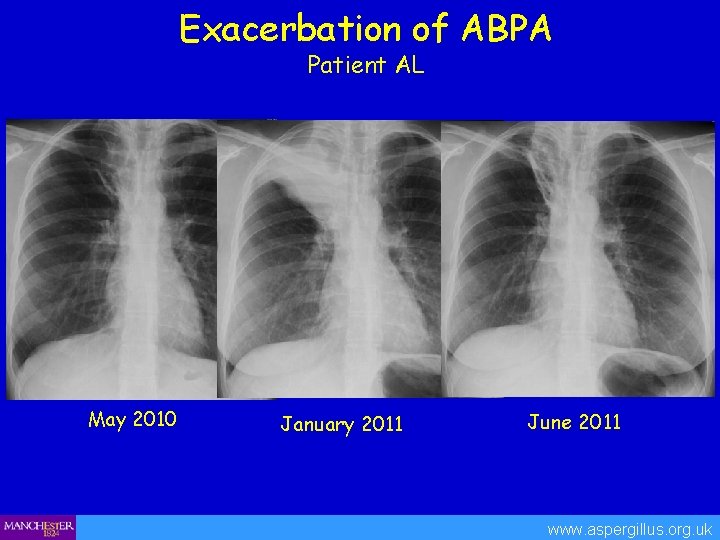
Exacerbation of ABPA Patient AL May 2010 January 2011 June 2011 www. aspergillus. org. uk

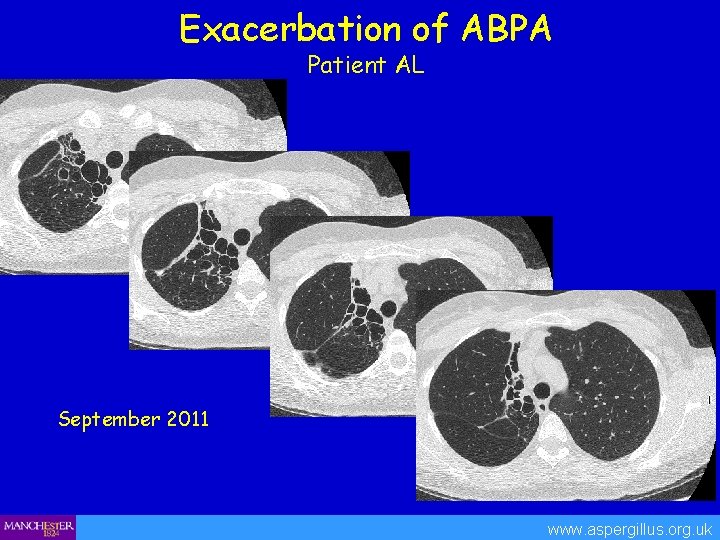
Exacerbation of ABPA Patient AL September 2011 www. aspergillus. org. uk

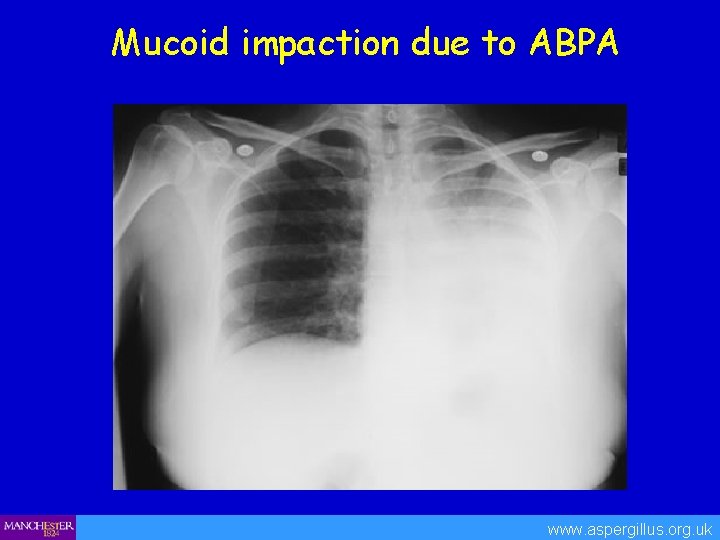
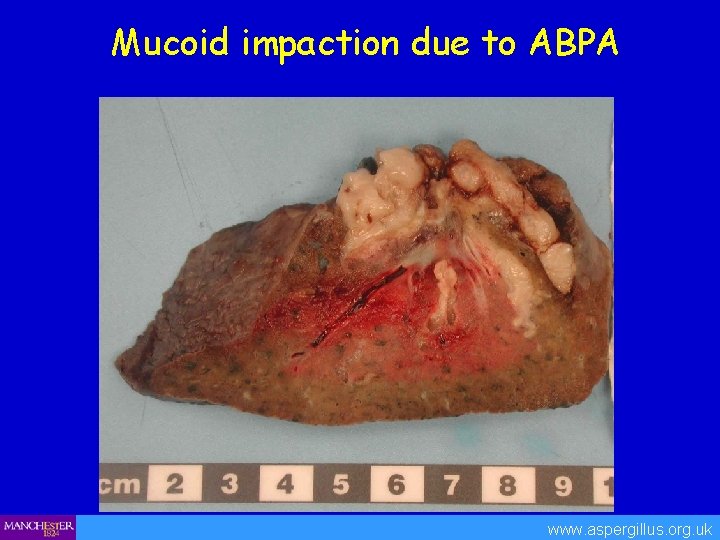
Mucoid impaction due to ABPA www. aspergillus. org. uk

Mucoid impaction due to ABPA www. aspergillus. org. uk

Sputum in ABPA www. aspergillus. org. uk

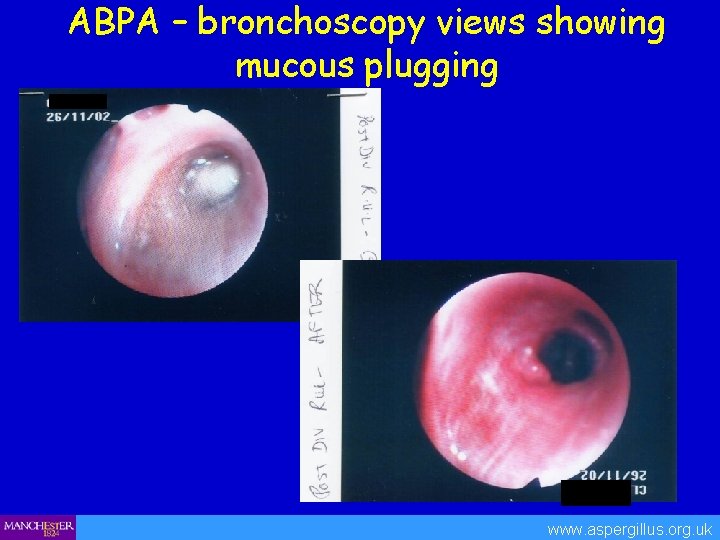
ABPA – bronchoscopy views showing mucous plugging www. aspergillus. org. uk

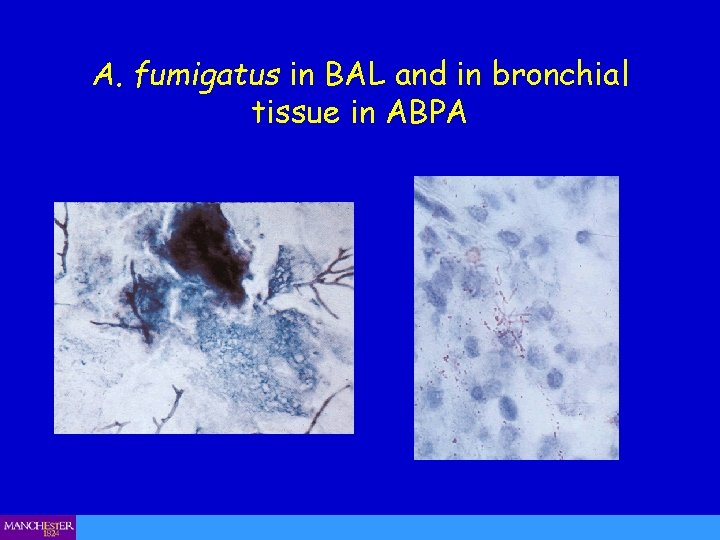
A. fumigatus in BAL and in bronchial tissue in ABPA

Severe Asthma and Fungal Sensitisation www. emphysema-copd. co. uk

Fungal exposure in asthmatics is related to: • Life-threatening asthmatic attacks (ie thunderstorm asthma) • Severe asthma and hospital admission • Increased wheezing and symptoms • Loss of medication control • Allergic bronchopulmonary mycosis • Eosinophilic fungal rhinosinusitis O'Hollaren, N Engl J Med 1991; 324: 359; and many others

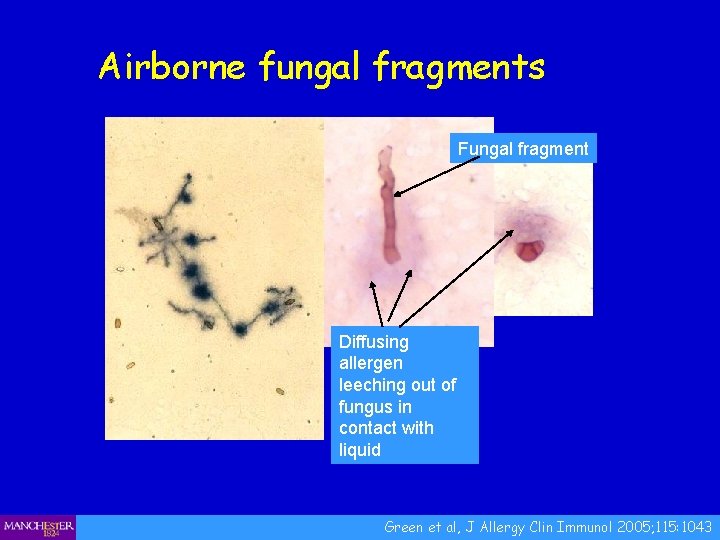
Airborne fungal fragments Fungal fragment Diffusing allergen leeching out of fungus in contact with liquid Green et al, J Allergy Clin Immunol 2005; 115: 1043

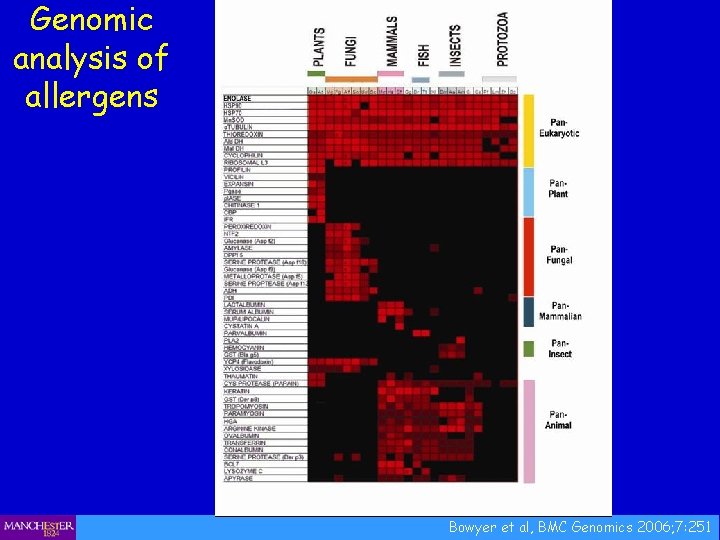
Genomic analysis of allergens Bowyer et al, BMC Genomics 2006; 7: 251

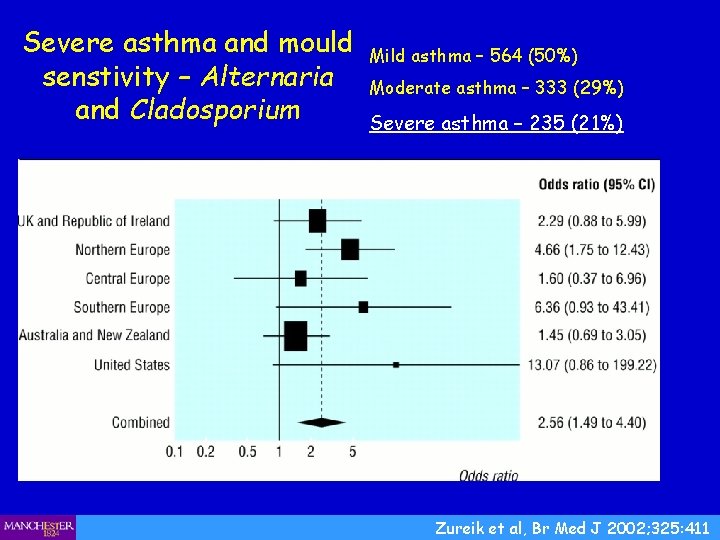
Severe asthma and mould senstivity – Alternaria and Cladosporium Mild asthma – 564 (50%) Moderate asthma – 333 (29%) Severe asthma – 235 (21%) Zureik et al, Br Med J 2002; 325: 411

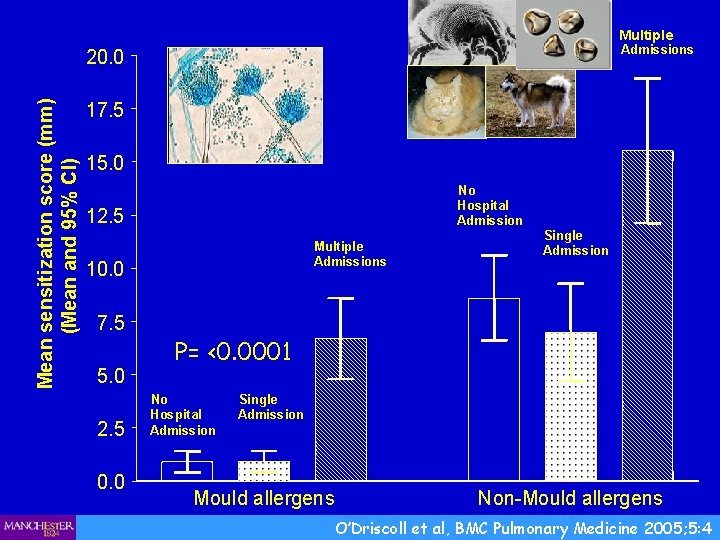
Multiple Admissions Mean sensitization score (mm) (Mean and 95% CI) 20. 0 17. 5 15. 0 No Hospital Admission 12. 5 Multiple Admissions 10. 0 7. 5 5. 0 2. 5 0. 0 Single Admission P= <0. 0001 No Hospital Admission Single Admission Mould allergens Non-Mould allergens O’Driscoll et al, BMC Pulmonary Medicine 2005; 5: 4

Colonisation in ‘normal’ lungs 22 of 30 (73%) grew a fungus in both lung samples taken 10/30 (33%) grew >1 species Lass-Florl et al, Br J Haematol 1999; 104: 745

Asthma and Aspergillus 79 adult asthmatics and 14 controls Patients sensitised to A. fumigatus compared with nonsensitised asthmatics had: lower lung function (% pred. FEV 1 68% vs 88% p < 0. 05), more bronchiectasis (68% versus 35% p < 0. 05) and more sputum neutrophils (80. 9% vs 49. 5% p < 0. 01). Fairs et al, Am J Respir Crit Care Med 2010; July 16

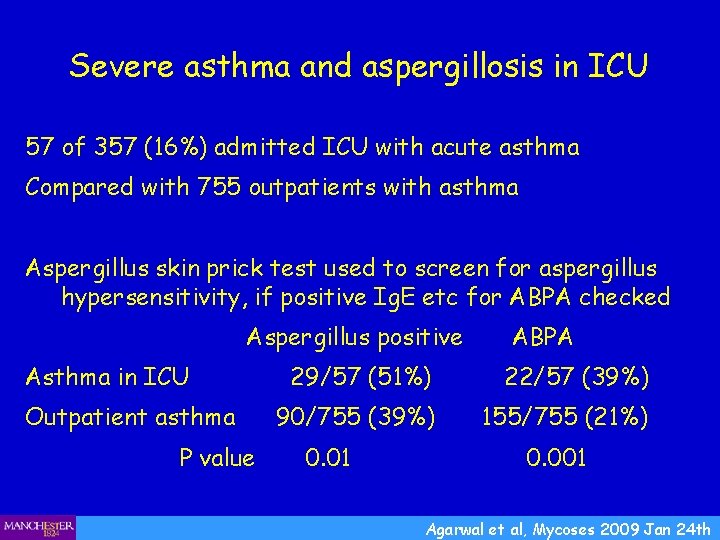
Severe asthma and aspergillosis in ICU 57 of 357 (16%) admitted ICU with acute asthma Compared with 755 outpatients with asthma Aspergillus skin prick test used to screen for aspergillus hypersensitivity, if positive Ig. E etc for ABPA checked Aspergillus positive Asthma in ICU Outpatient asthma P value ABPA 29/57 (51%) 22/57 (39%) 90/755 (39%) 155/755 (21%) 0. 01 0. 001 Agarwal et al, Mycoses 2009 Jan 24 th

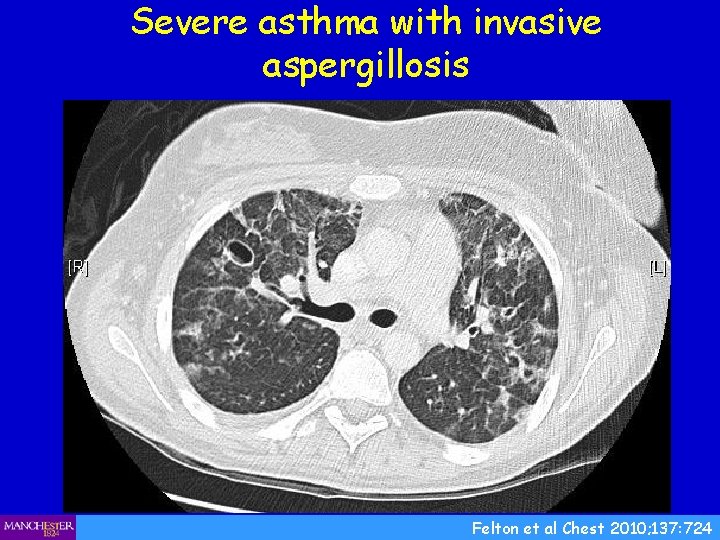
Severe asthma with invasive aspergillosis Felton et al Chest 2010; 137: 724

Severe asthma with fungal sensitisation (SAFS) Criteria for diagnosis • Severe asthma (BTS step 4 or 5) AND • RAST (Ig. E) positive for any fungus OR • Skin prick test positive for any fungus AND • Exclude ABPA (ie total Ig. E <1, 000 iu/m. L) Denning et al, Eur Resp J 2006; 27: 615

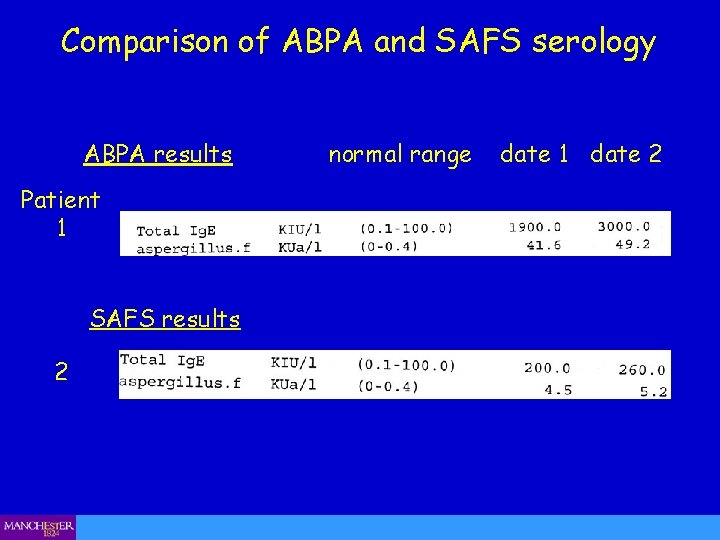
Comparison of ABPA and SAFS serology ABPA results Patient 1 SAFS results 2 normal range date 1 date 2

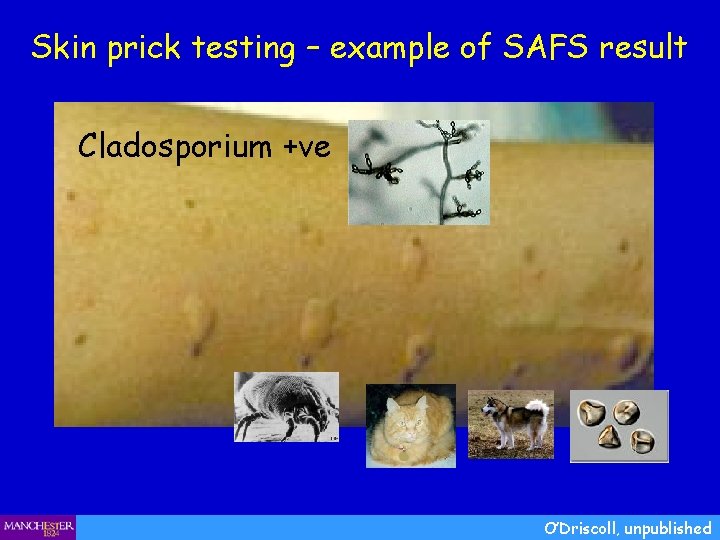
Skin prick testing – example of SAFS result Cladosporium +ve O’Driscoll, unpublished

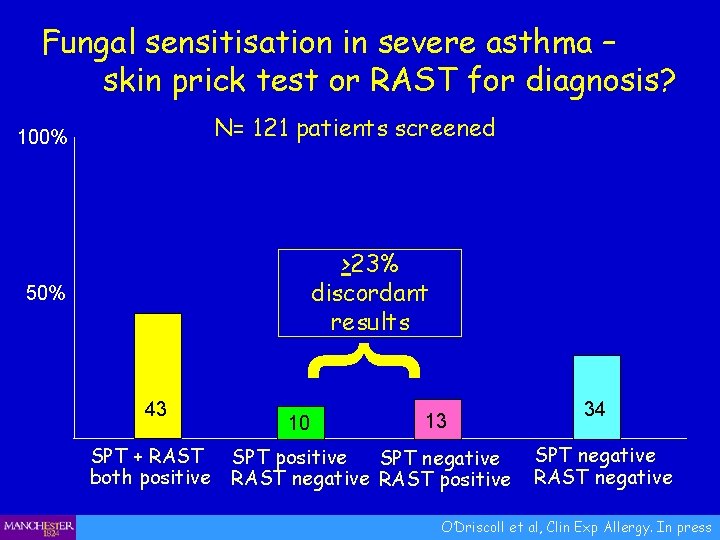
Fungal sensitisation in severe asthma – skin prick test or RAST for diagnosis? N= 121 patients screened 100% >23% discordant results } 50% 43 SPT + RAST both positive 10 13 SPT positive SPT negative RAST positive 34 SPT negative RAST negative O’Driscoll et al, Clin Exp Allergy. In press

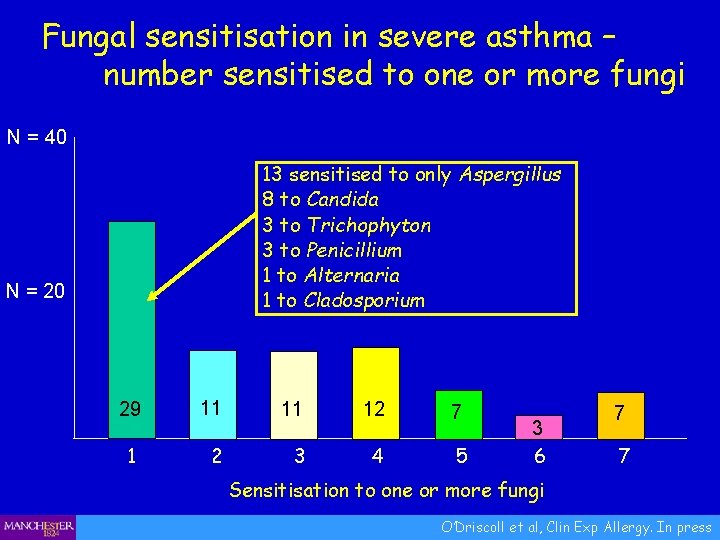
Fungal sensitisation in severe asthma – number sensitised to one or more fungi N = 40 13 sensitised to only Aspergillus 8 to Candida 3 to Trichophyton 3 to Penicillium 1 to Alternaria 1 to Cladosporium N = 20 29 11 11 12 7 1 2 3 4 5 3 6 7 7 Sensitisation to one or more fungi O’Driscoll et al, Clin Exp Allergy. In press

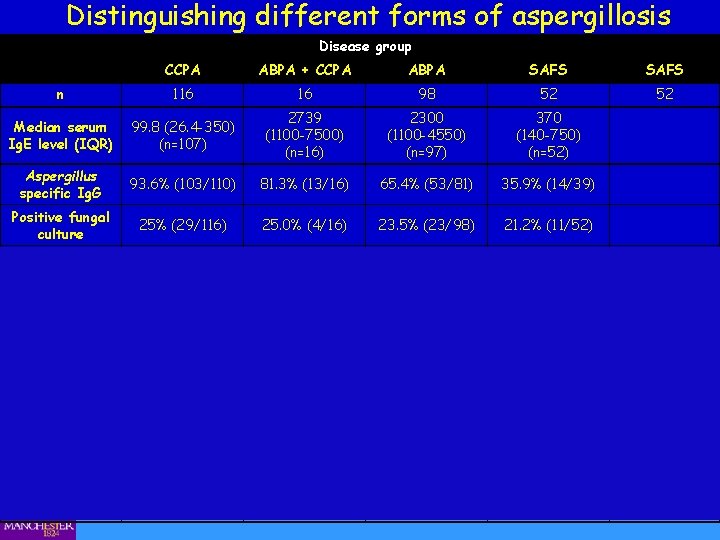
Distinguishing different forms of aspergillosis Disease group CCPA ABPA + CCPA ABPA SAFS n 116 16 98 52 52 Median serum Ig. E level (IQR) 99. 8 (26. 4 -350) (n=107) 2739 (1100 -7500) (n=16) 2300 (1100 -4550) (n=97) 370 (140 -750) (n=52) Aspergillus specific Ig. G 93. 6% (103/110) 81. 3% (13/16) 65. 4% (53/81) 35. 9% (14/39) Positive fungal culture 25% (29/116) 25. 0% (4/16) 23. 5% (23/98) 21. 2% (11/52) Positive specific Ig. E Positive SPT Mixed mould N/T 88. 9% (8/9) 90. 9% (20/30) 100% (2/2) A. fumigatus 37. 7% (40/106) 93. 8% (15/16) 96. 9% (94/97) 78. 8% (41/52) 90. 9% (20/30) Alternaria alternata 10. 0% (1/10) 100% (10/10) 77. 5% (55/71) 32. 5% (13/40) 47. 4% (9/19) C. albicans 33. 3% (3/9) 90. 0% (9/10) 81. 4% (57/70) 37. 5% (15/25) 52. 6% (10/19) Cladosporium herbarum 20. 0% (2/10) 80. 0% (8/10) 70. 4% (50/71) 24. 4% (10/41) 35. 5% (6/17) Penicillium chrysogenum 27. 3% (3/11) 100% (10/10) 85. 3% (58/68) 30. 0% (12/40) 43. 8% (7/16) Trichophyton mentagrophyte 33. 3% (2/6) 100% (3/3) 65. 2% (30/46) 25. 0% (9/36) 23. 1% (3/13)

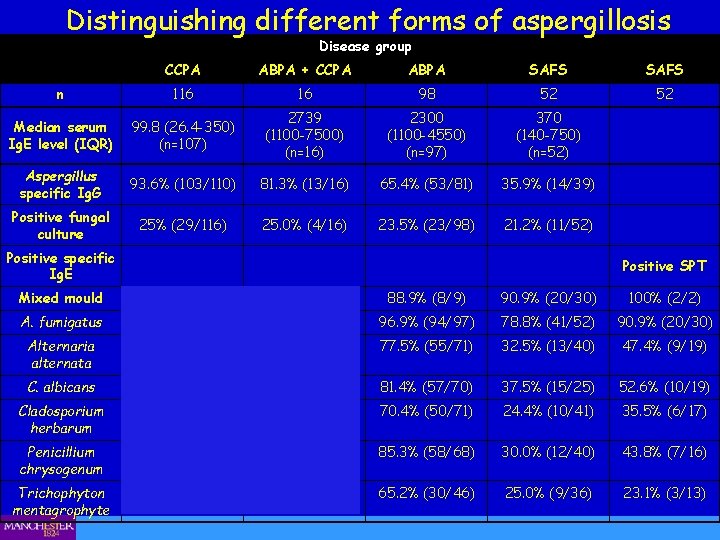
Distinguishing different forms of aspergillosis Disease group CCPA ABPA + CCPA ABPA SAFS n 116 16 98 52 52 Median serum Ig. E level (IQR) 99. 8 (26. 4 -350) (n=107) 2739 (1100 -7500) (n=16) 2300 (1100 -4550) (n=97) 370 (140 -750) (n=52) Aspergillus specific Ig. G 93. 6% (103/110) 81. 3% (13/16) 65. 4% (53/81) 35. 9% (14/39) Positive fungal culture 25% (29/116) 25. 0% (4/16) 23. 5% (23/98) 21. 2% (11/52) Positive specific Ig. E Positive SPT Mixed mould N/T 88. 9% (8/9) 90. 9% (20/30) 100% (2/2) A. fumigatus 37. 7% (40/106) 93. 8% (15/16) 96. 9% (94/97) 78. 8% (41/52) 90. 9% (20/30) Alternaria alternata 10. 0% (1/10) 100% (10/10) 77. 5% (55/71) 32. 5% (13/40) 47. 4% (9/19) C. albicans 33. 3% (3/9) 90. 0% (9/10) 81. 4% (57/70) 37. 5% (15/25) 52. 6% (10/19) Cladosporium herbarum 20. 0% (2/10) 80. 0% (8/10) 70. 4% (50/71) 24. 4% (10/41) 35. 5% (6/17) Penicillium chrysogenum 27. 3% (3/11) 100% (10/10) 85. 3% (58/68) 30. 0% (12/40) 43. 8% (7/16) Trichophyton mentagrophyte 33. 3% (2/6) 100% (3/3) 65. 2% (30/46) 25. 0% (9/36) 23. 1% (3/13)

Conceptual framework for CPA and IA Normal Chronic inflammation and fibrosis Granulomas, acute inflammation, central necrosis Vascular invasion, necrosis, dissemination Hyphal load in tissue Immune function Massive Aspergilloma - CCPA - CNPA/subacute IPA - acute IPA www. aspergillus. org. uk

Alternative Aspergillus diagnoses • • • Aspergillus bronchitis Obstructing bronchial aspergillosis Invasive Aspergillus tracheobronchitis Community acquired Aspergillus pneumonia Sub-acute invasive pulmonary aspergillosis (often called chronic necrotising pulmonary aspergillosis or CNPA) • Extrinsic allergic (bronchiol)alveolitis (EAA) • Aspergillus empyema

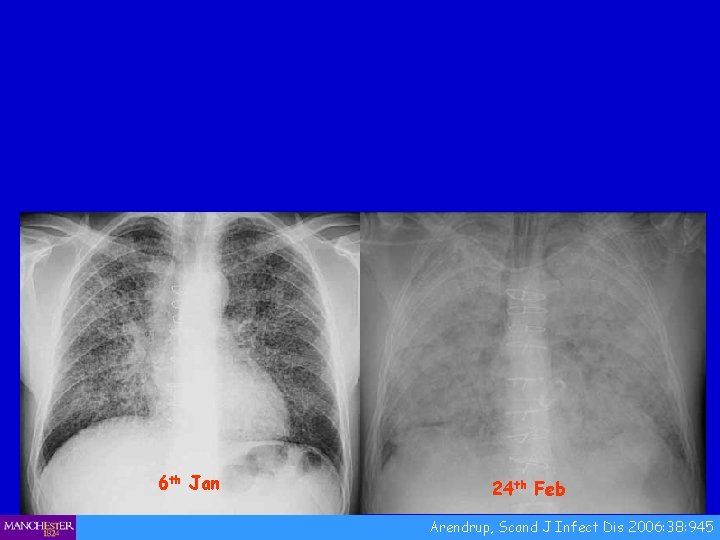
6 th Jan 24 th Feb Arendrup, Scand J Infect Dis 2006: 38: 945

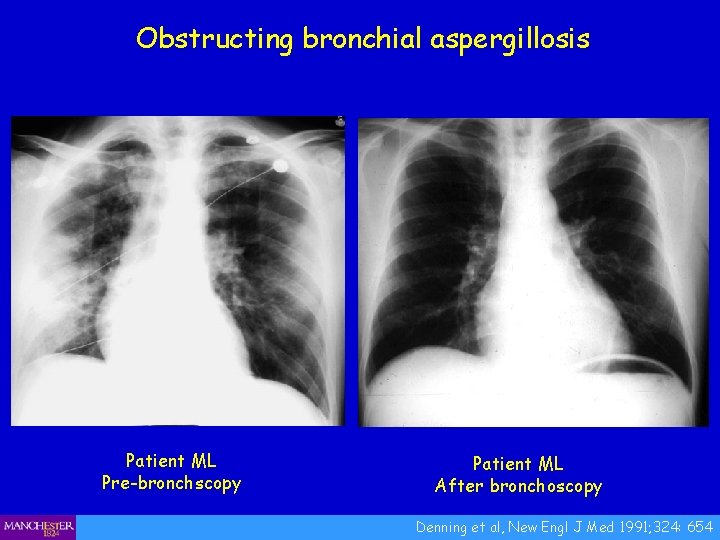
Obstructing bronchial aspergillosis Patient ML Pre-bronchscopy Patient ML After bronchoscopy Denning et al, New Engl J Med 1991; 324: 654

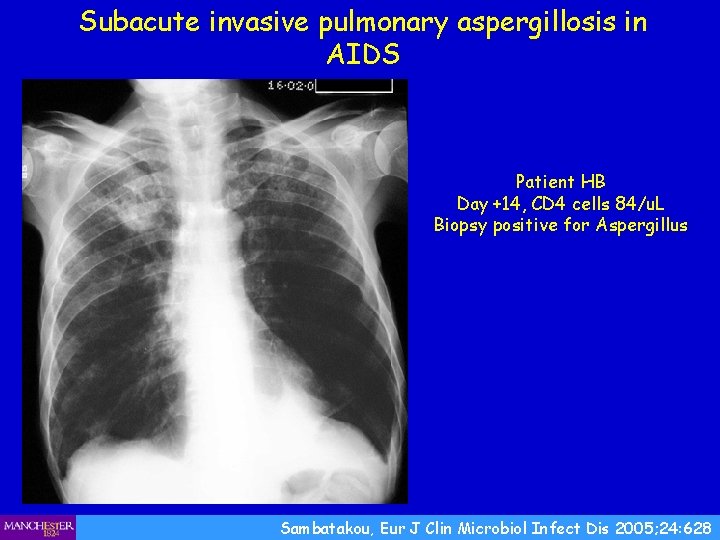
Subacute invasive pulmonary aspergillosis in AIDS Patient HB Day +14, CD 4 cells 84/u. L Biopsy positive for Aspergillus Sambatakou, Eur J Clin Microbiol Infect Dis 2005; 24: 628

Conclusions • CPA = 3 months of pulmonary cavitation or nodule +/aspergilloma, with symptoms + Aspergillus Ig. G or precipitins positive • CPA patients almost all have an underlying diagnosis • ABPA = asthma (any severity) or cystic fibrosis + total Ig. E >1, 000 + SPT or Aspergillus Ig. E positive. • SAFS = severe asthma + fungal SPT or Ig. E positive + total Ig. E <1, 000 • Some patients have overlap syndromes and more than 1 Aspergillus diagnosis