Clinical and lab aspect of anaerobic infection Ali

Clinical and lab aspect of anaerobic infection Ali Somily MD, FRCPC, ABMM

Classification 1. Anaerobic spore forming bacilli 2. 3. 4. 5. 6. (Clostridia) Gram negative bacilli non-sporing forming (Bacteroides) Anaerobic streptococci (Peptostreptococcus) Anaerobic staphylococcus (Peptococcus) Gram negative diplococci (Veillonella) Gram positive bacilli (Actinomyces)

Anaerobiosis • Lack cytochrome-cannot use oxygen as hydrogen • acceptor Most Lack – Catalase – Peroxidase • Contain flavoprotein so in the presence of oxygen • produce H 2 O 2 which is toxic Some lack enzyme superoxide dismutase so many killed , peroxide and toxic radicales enzyme like fumarate reductase must be in reduced form to work

HABITAT I : • These organism are normal flora in: • A. Oropharynx • eg. 1. Bacteroides melaninogenicus v. Now called provetella melaninogenicus – 2. Fusobacteria – 3. Veillonella

HABITAT II: • B. Gastrointestinal tract – – – Found mainly in the large colon in large numbers Total number of anaerobes = 10 11 While all aerobes (including E. coli) = 10 4 – examples are v (1) B acteroides fragilis v (2) Bifidobacterium species • C. Female genital tract (mainly in the vagina)

INFECTIONS CAUSED BY , NONSPORING ANAEROBES • A. The head, neck and respiratory tract • B. The lower abdomen and the pelvis

FEATURES OF ANAEROBIC INFECTIONS Characterized by • Infections are always near to the site of the body which are habitat. • Infection from animal bites. • Deep abscesses • The infections are also polymicrobial foul smell • Gas formation • Detection of "Sulphur granules"' due to actinomycosis • Failure to grow organism from pus if not culture anaerobically. • Failure to respond to usual antibiotics.

INFECTIONS BEGIN • DISRUPTION OF BARRIERS – TRAUMA – OPERATIONS – CANCEROUS INVASION OF TISSUES • DISRUPTION OF BLOOD SUPPLY – DROPS OXYGEN CONTENT OF TISSUE – DECREASE IN Eh POTENTIAL – TISSUE NECROSIS

WHAT ARE THE INFECTION CAUSED BY THESE ANAEROBIC ORGANISMS I 1. 2. 3. 4. 5. 6. Post operative wound infection Brain abscess Dental abscesses Lung abscess Intra abdominal abscess, appendicitis, diverculitis All these infection cause bacteriaemia

WHAT ARE THE INFECTION CAUSED BY THESE ANAEROBIC ORGANISMS II 1. 2. 3. 4. 5. 6. Infection of the female genital tract Septic abortion Puerperal infection or sepsis Endometritis Pelvic abscess 12. Other infections – – – a) Breast abscess in puerperal sepsis b) Infection of diabetic patients (diabetic foot infections). c) Infection of pilonidal sinus

ORAL & DENTAL • > 400 SPECIES OF ANO 2 IN MOUTH • MOST INFECTIONS = POLYMICROBIC – MIXED ORGANISMS – ENTER AS A GROUP • ANO 2 NOT INITIAL INVADER – USUALLY SECONDARY – 1 ST ORGANISM DECREASES [O 2] & Eh

ORAL & DENTAL • COMMONLY ASSOCIATED WITH 1. 2. 3. 4. 5. DENTAL ABSCESSES ROOT CANALS JUVENILE PERIODONTITIS ADULT PERIODONTITIS CLENCHED FIST INJURIES

ENT – HEAD & NECK 1. CHRONIC OTITIS MEDIA 2. CO-PATHOGENS WITH CHRONIC 3. STREP TONSILLITIS ACUTE SINUSITIS – POST-DENTAL EXTRACTIONS OR TRAUMA – 2 o INVADER

ENT – HEAD & NECK • VINCENT’S ANGINA – COMBINATION OF FUSOBACTERIUM & SPIROCHETE SPECIES OVERGROWTH – ANAEROBIC PHARYNGITIS – GRAY MEMBRANE – FOUL ODOR

Vincent’s disease • Trench mouth • Sudden onset of pain in the gingiva (mastication) • Necrosis of the gingiva – interdental papilla – a marginated, punched-out, and eroded appearance • • • A superficial grayish pseudomembrane altered taste sensation is present Fever, malaise, and regional lymphadenopathy

Ludwig’s Angina
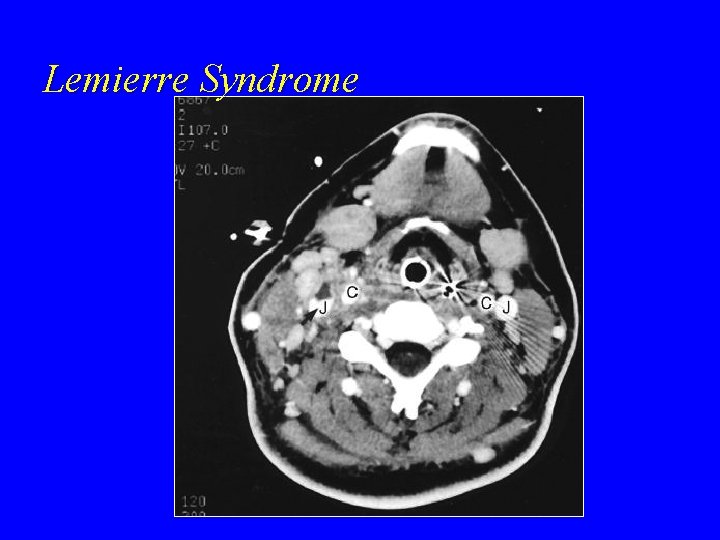
Lemierre Syndrome
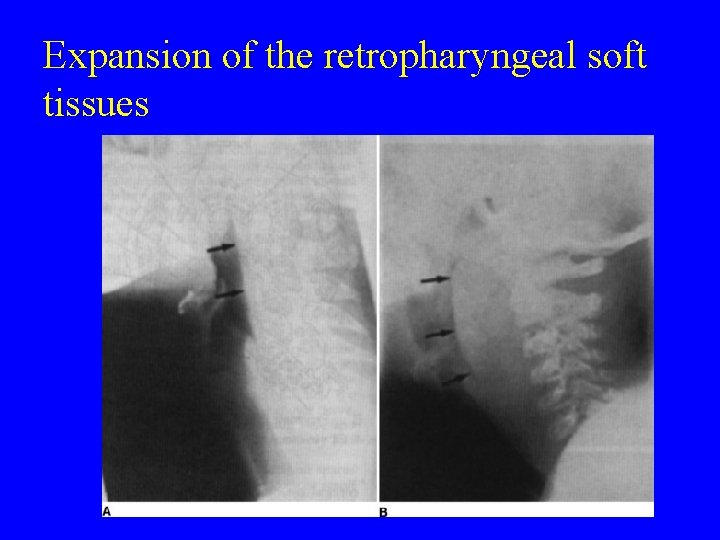
Expansion of the retropharyngeal soft tissues

PLELRO PULMONARY I FECTION • • • ASPIRATION LUNG ABSCESS ASPIRATION PNEUMONIA M ETASTATIC LUNG ABSCESS BRONCHIACTSIS ALL OF ABOVE CAN CAUSE EMPYEMA

LUNG & PLEURAL 1. 2. 3. 4. 5. ASPIRATION PNEUMONIA EMPHYSEMA LUNG ABSCESSES MALIGNANCIES LEUKOPENIA
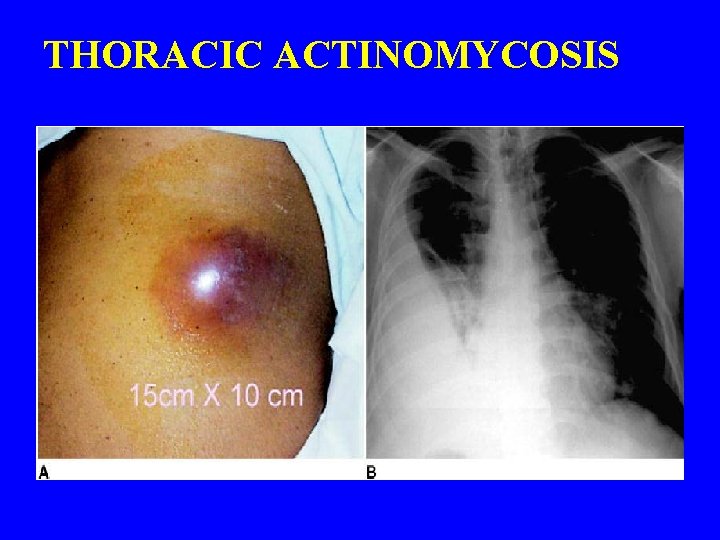
THORACIC ACTINOMYCOSIS
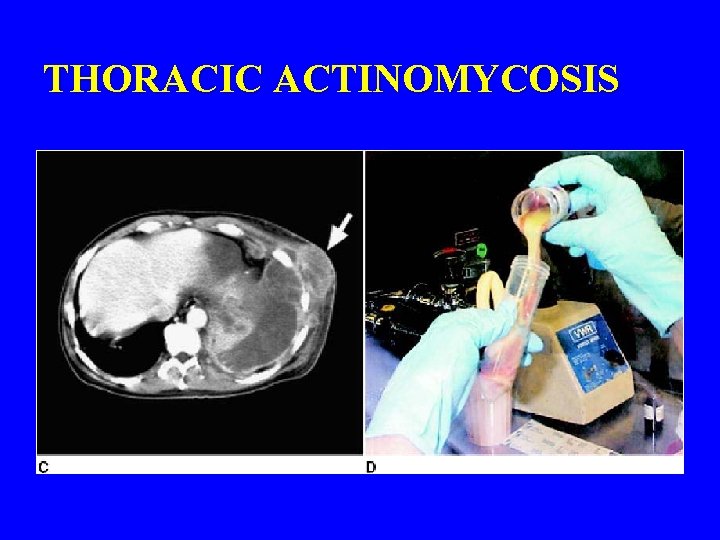
THORACIC ACTINOMYCOSIS
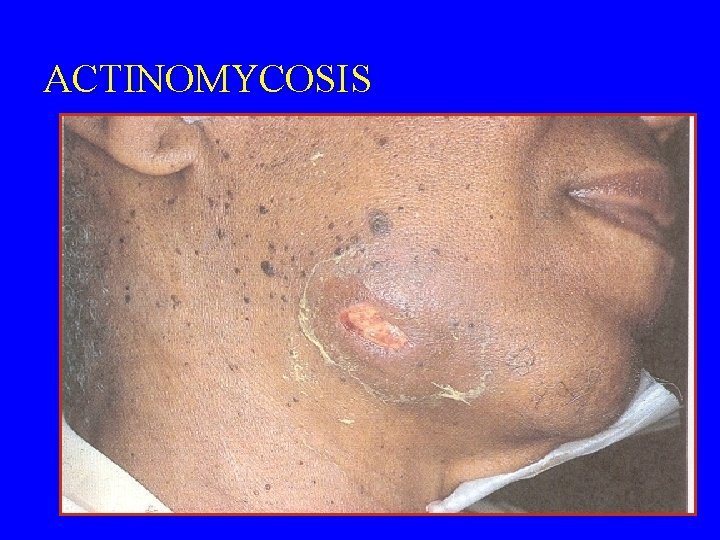
ACTINOMYCOSIS
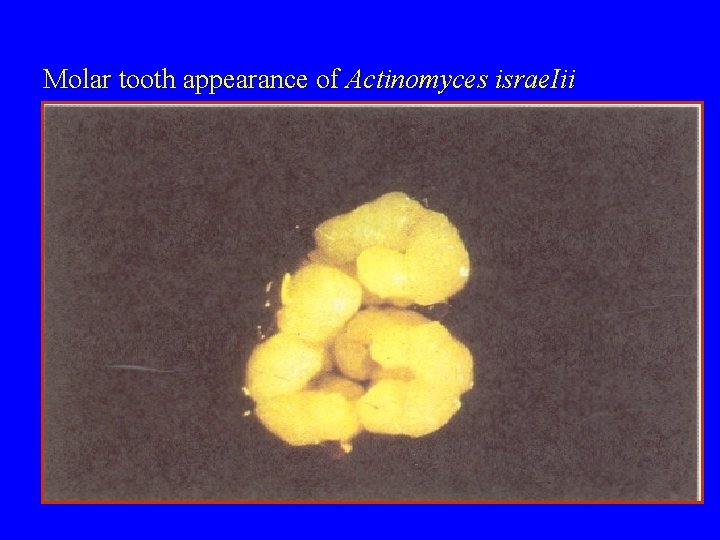
Molar tooth appearance of Actinomyces israe. Iii

Macroscopic colony (left) Gram stain (right) of Actinomyces

SKIN & SOFT TISSUE • TRAUMATIZED & DEVITALIZED TISSUE 1. TRAUMATIC WOUNDS 2. HUMAN/ANIMAL BITES 3. ISCHEMIA OF EXTREMITIES • DIABETES • ATHEROSCLEROSIS
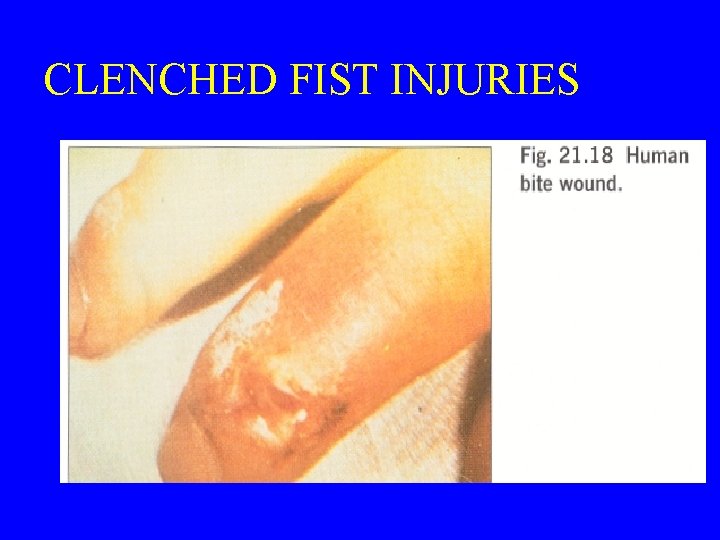
CLENCHED FIST INJURIES
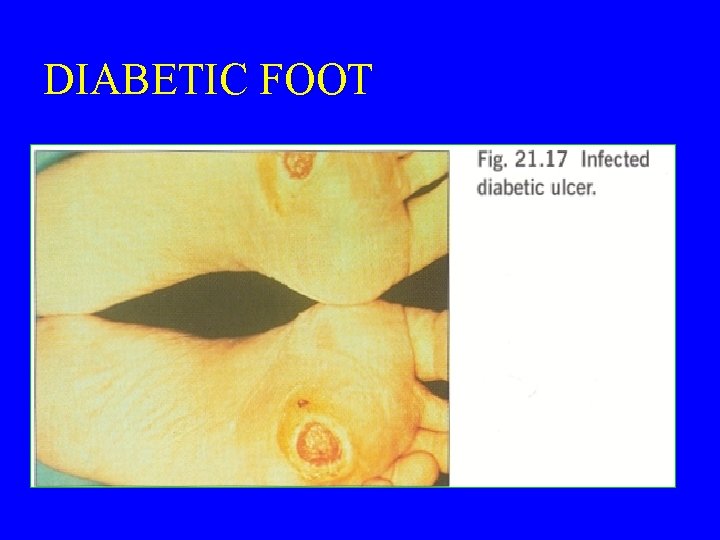
DIABETIC FOOT
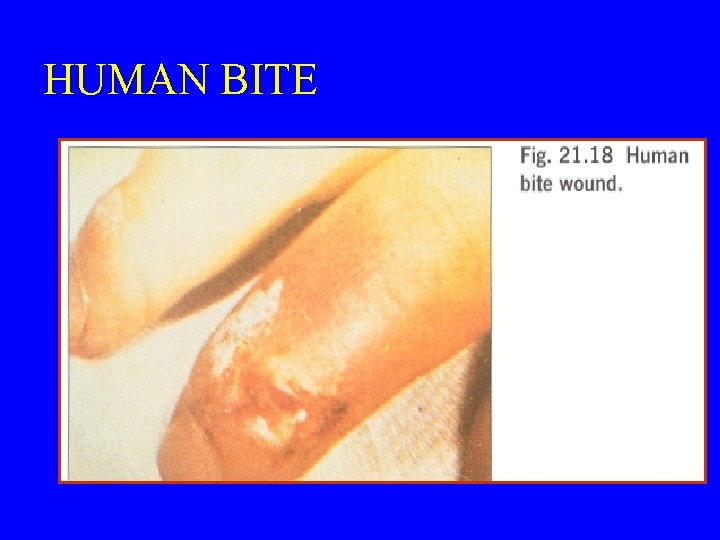
HUMAN BITE
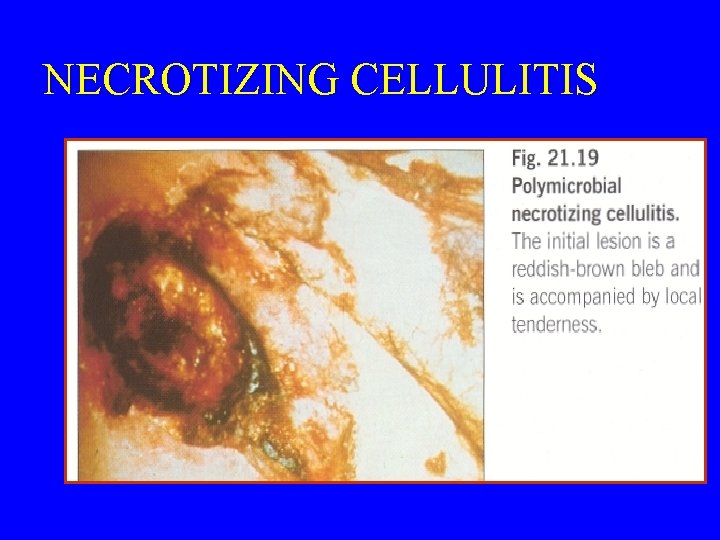
NECROTIZING CELLULITIS

PUERPERAL INFECTION SEPTIC ABORTION • PUERPERAL ABSCESS • SEPTIC ABORTION • BACTERAEMIA • • PELVIC ABSCESS ADENXAL ABSCESS PERITONITIS ENDOMETRITIS

ABDOMINAL INFECTIONS • MANIPULATION, INVASION OR TRAUMA TO GI TRACT 1. 2. 3. 4. TRAUMA SURGERY APPENDICITIS MALIGNANCIES • COLON CANCER

CNS 1. HEAD TRAUMA 2. HEMATOGENOUS SPREAD – FROM ANY INFECTED BODY SITE 3. GEOGRAPHIC SPREAD – SINUS INFECTIONS – DENTAL ABSCESSES

BONE & JOINT • • HEMATOGENOUS SPREAD TRAUMA PERIVASCULAR DISEASE JUVENILE PERIODONTITIS

OTHER INFECTIONS • • • GRAM NEGATIVE BACTREMIA BREAST ABSCESS AXILLARY ABSCESS INFECTION OF DIABETIS EG. DIABETIC ULCERS INFECTION OF PILONIDAL SINUS PARONYCHIA

LABORATORY DIAGNOSIS: • When anaerobic infection is suspected; – a) Specimens have to be collected from the site containing necrotic tissue. – b) Pus is better than swabs. – c) Specimens has to be send to the laboratory within 1/2 hour why? – d) Fluid media like cooked meat broth are the best culture media. – e) Specimens have to incubated anaerobically for 48 hours.

Anaerobic chamber

TREATMENT: • Bacteroides fragilis is always resistant to • • • penicillin. But penicillin can he used for other anaerobes Flagyl (metronidazole) is the drug of choice. Clindamycin can also be used.

CLASSIFICATION 1. Anaerobic spore forming bacilli 2. 3. 4. 5. 6. (Clostridia) Gram negative bacilli nonsporing (Bacteroides) Anaerobic streptococci (Peptostreptococcus) Anaerobic staphylococcus (Peptococcus) Gram negative diplococci (Veillonella) Gram positive bacilli (Actinomyces)

ORGANISM GROUPS • GRAM NEGATIVE RODS – BACTEROIDES – PREVOTELLA – PORPHYROMONAS – FUSOBACTERIUM – BUTYRIVIBRIO – SUCCINOMONAS

Bacteroides fragilis
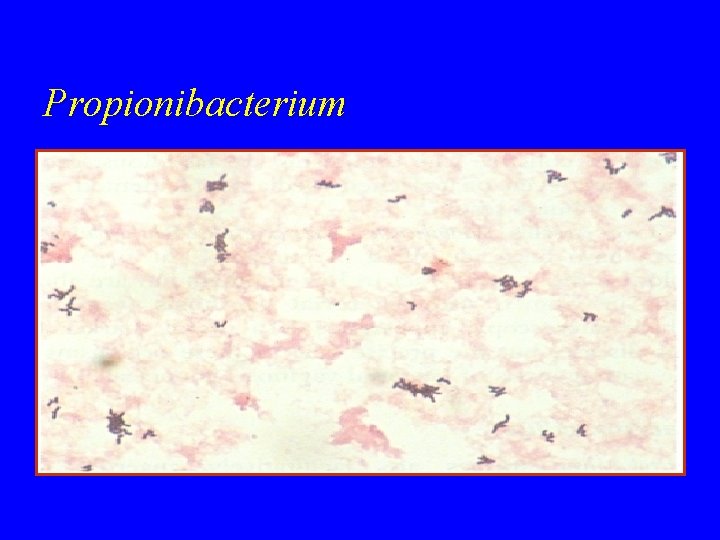
Propionibacterium
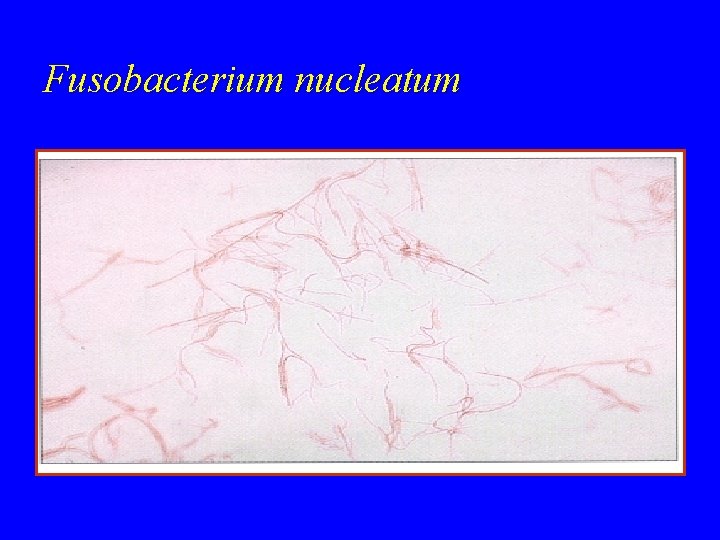
Fusobacterium nucleatum

BACTEROIDES • • STRICT ANAEROBE PLEOMORPHIC GRAM NEGATIVE BACILLI (COCCO BACILLI) NORMAL FLORA IN – OROPHARYNX – GASTROINTESTINAL TRACT – VAGINA

BACTEROIDES FRAGILIS GP • GROUP = B. FRAGILIS, B. VULGARIS, B. THETAIOTAMICRON, B. UNIFORMIS – ACCOUNT FOR 1/3 OF ALL ISOLATES – RESISTANT TO 20% BILE – RESISTANT TO MANY ANTIBIOTICS • PENICILLIN, KANAMYCIN, VANCOMYCIN, COLISTIN – AND MANY MORE

BACTEROIDES FRAGILIS GP • GLC = MAJOR ACETIC & SUCCINIC, • LACTIC & PROPIONIC ACIDS NO PIGMENTATION OF COLONIES OR FLUORESCENCE

BACTEROIDES OTHER SP • BACTEROIDES SPECIES OTHER THAN B. FRAGILIS GROUP – GLC = MAJOR ACETIC & SUCCINIC ONLY – BILE SENSITIVE – RESISTANT TO KANAMYCIN ONLY – SOME PIGMENTED

BACTEROIDES • B. FRAGILIS IN THE GUT AND VAGINA • B. MELANINOGESUS AND B. ORALIS IN • • • THE MOUTH AND OROPHARYNX B. FRAGILIS PENICILLIN RESISTANT, OTHER ARE SENSITIVE, IT IS THE COMMONEST ORGANISM IN THE GUT 10 12 ORGANISM /GRAM OF FAECES
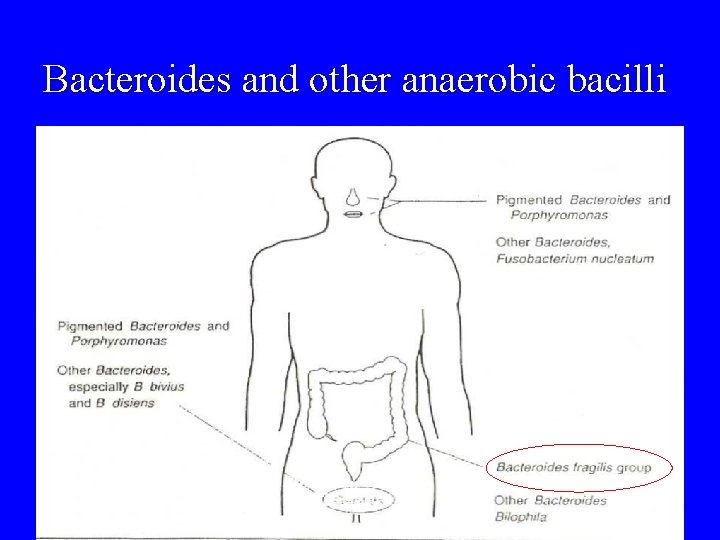
Bacteroides and other anaerobic bacilli
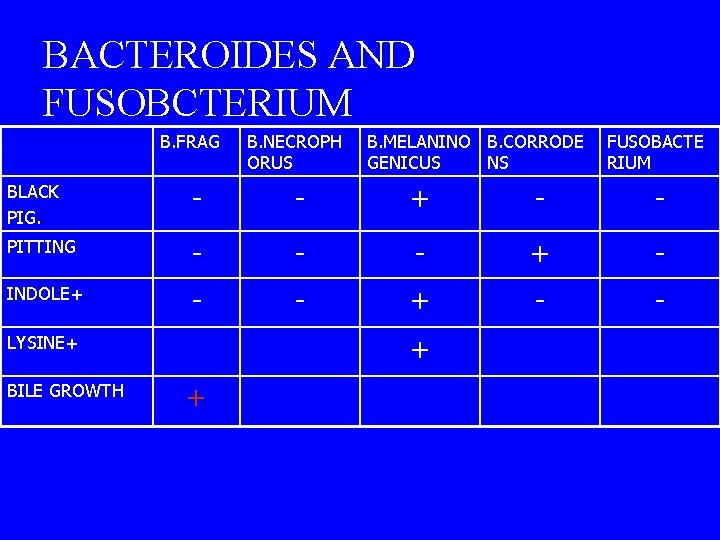
BACTEROIDES AND FUSOBCTERIUM B. FRAG B. NECROPH ORUS B. MELANINO B. CORRODE GENICUS NS FUSOBACTE RIUM BLACK PIG. - - + - - PITTING - - - + - INDOLE+ - - + LYSINE+ BILE GROWTH +

Growth of Bacteroides fragilis on Bacteroides bile-esculin agar

PEPTOCOCCUS NIGER • GRAM POSITIVE COCCI • GLC = ACETIC, BUTYRIC, ISOBUTYRIC, • ISOVALERIC, CAPROIC BLACK PIGMENT

PEPTOSTREPTOCOCCUS • • GRAM POSITIVE COCCI GLC = ACETIC, SOME BUTYRIC Ps. ASACCHAROLYTICUS INDOLE + Ps. ANAEROBIUS, Ps. MAGNUS, Ps. PREVOTI, Ps. INDOLECUS

STREP & STAPH • ANAEROBIC SPECIES OF STAPH AND • • STREPTOCOCCUS INTERMEDIUS STAPHYLOCOCCUS SACCHAROLYTICUS

VEILLONELLA PARVULA • • • GRAM NEGATIVE COCCI GLC = ACETIC & PROPIONIC NITRATE + HEAD AND NECK INFECTIONS DENTAL ABSCESSES

CLOSTRIDIUM SPECIES • LARGE GRAM POSITIVE RODS • SPORE FORMATION • SPECIFIC DISEASES – PSEUDOMEMBRANOUS COLITIS – TETANUS – BOTULISM – GANGRENE - MYONECROSIS

C. difficile

CLOSTRIDIA

CLOSTRIDIA • Causative Agents For – 1. Gas gangrene : Cl. perfringens and other e. g septicum – 2. Tetanus : Cl. tetani – 3. Botulism : Cl. botulinum – 4. Toxic enterocolitis : Cl. difficile (Pseudomembernous colitis)

Clostridium perfringens (CI. welchii) • • Morphology large rods gram +ve With bulging endospores Not motile Capsulated
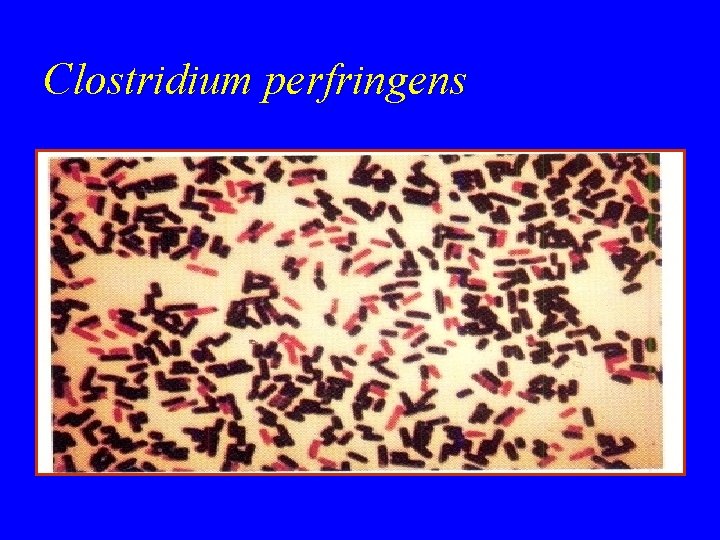
Clostridium perfringens
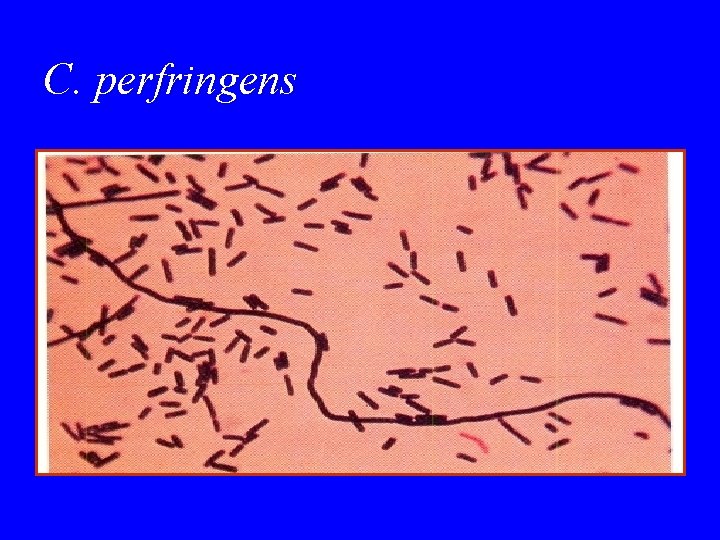
C. perfringens
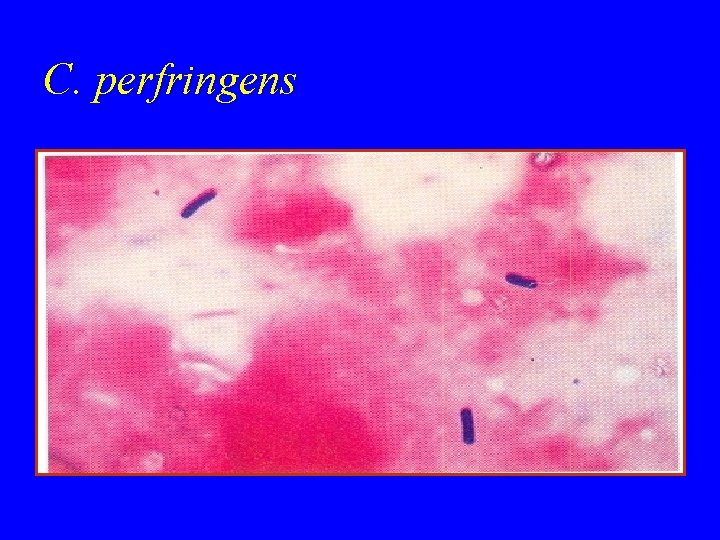
C. perfringens

Culture: • A) Blood agar with haemolytic colonies • (double zone of haemolysis B) Cooked meat medium • Gives the NAGLAR'S Reaction & toxin neutralization on Egg yolk medium & toxin is a phospholipase
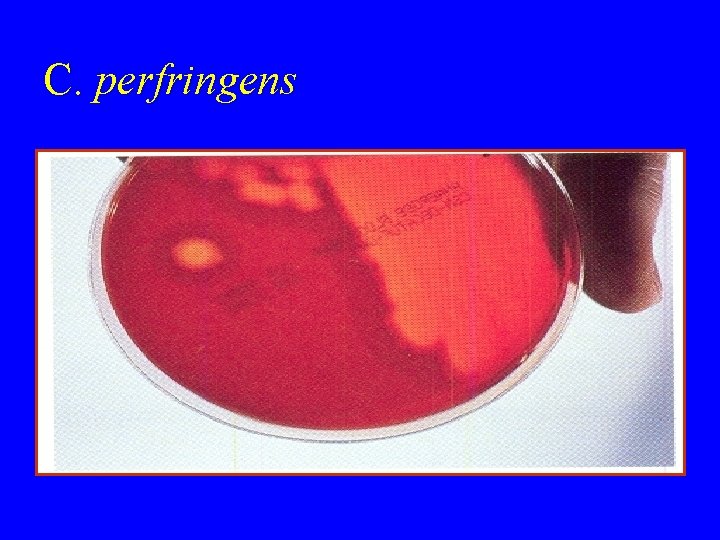
C. perfringens
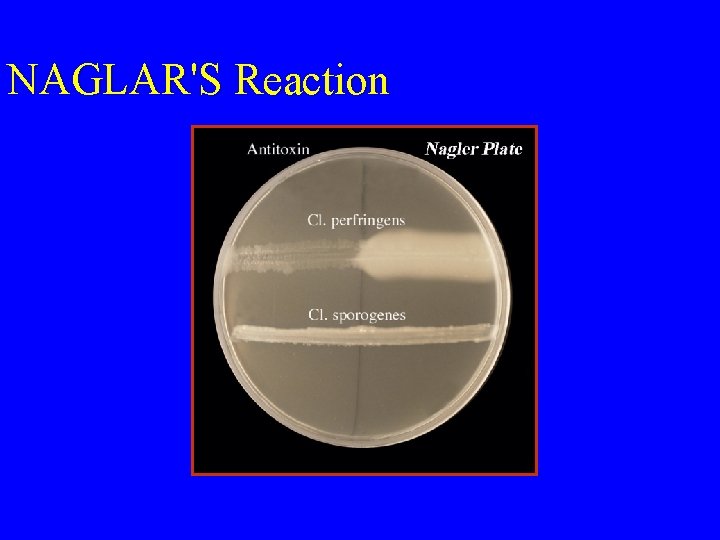
NAGLAR'S Reaction
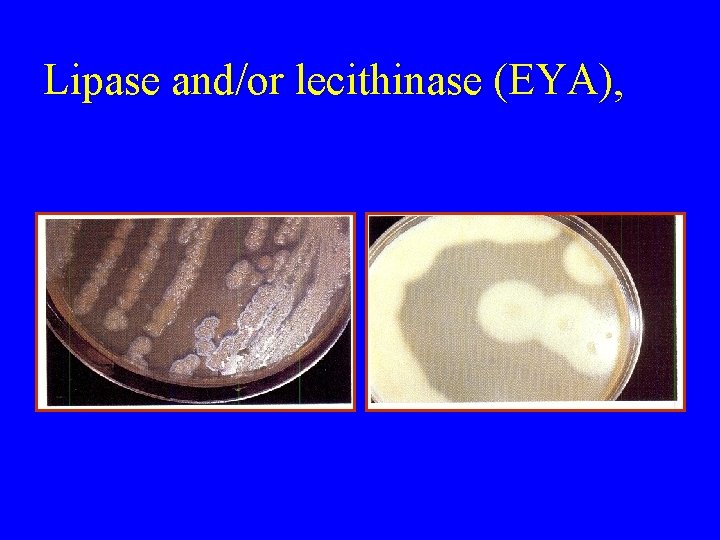
Lipase and/or lecithinase (EYA),

Diseases Caused by C. perfringens • • • 1) Wound Contamination 2) Wound infection 3) Gas Gangrene - most important disease 4) Gas Gangrene of the uterus in criminal abortion 5) Food Poisoning • Spores are swallowed Germinate in gut after 18 hours • Toxin • abdominal pain and diarrhoea

GAS GANGRENE • Causes mainly – – (Cl perfringens) (Cl. welchil) CI. novyl, CI. Septicum CI oedemaritians – – Traumatic open wounds Compound fractures Muscle damages Contamination with dirt etc, • Pathogenesis: • Mainly in war wounds, • Old age, – Low blood supply • Amputation of thigh – Prophylaxis with penicillin
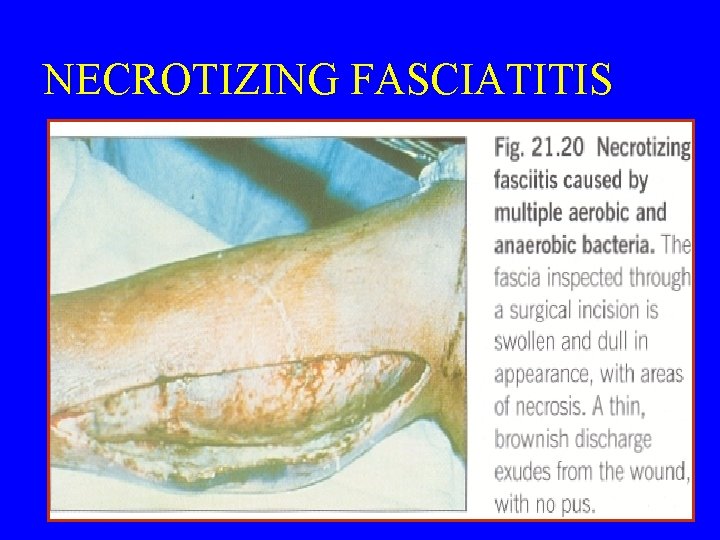
NECROTIZING FASCIATITIS
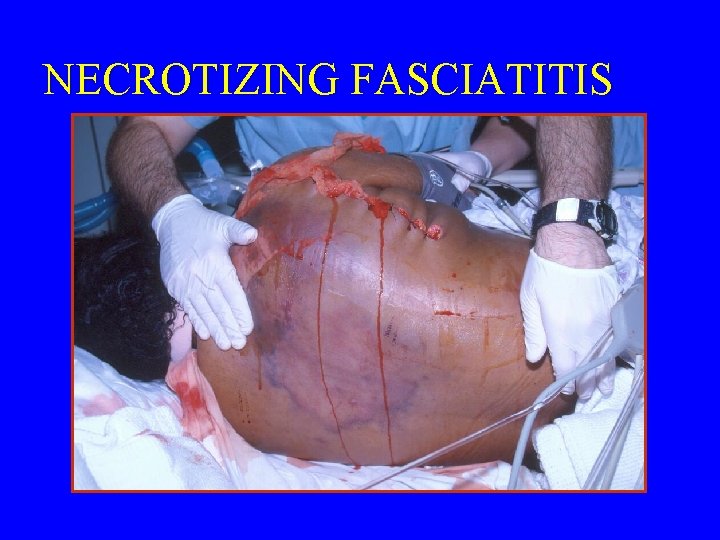
NECROTIZING FASCIATITIS
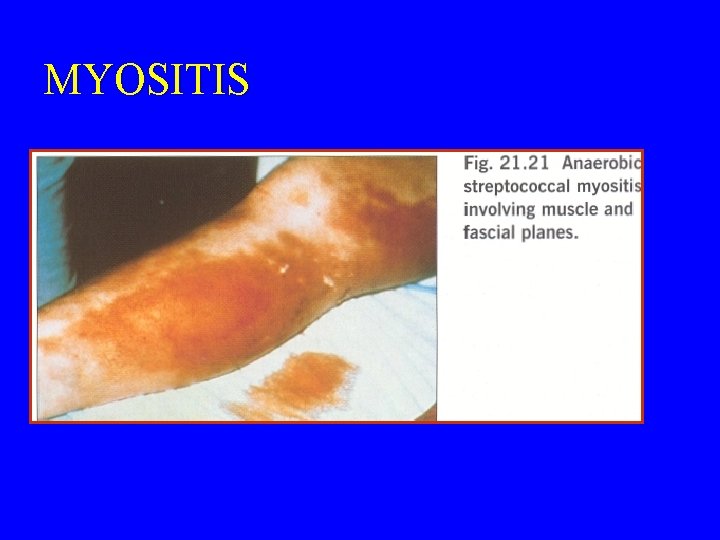
MYOSITIS
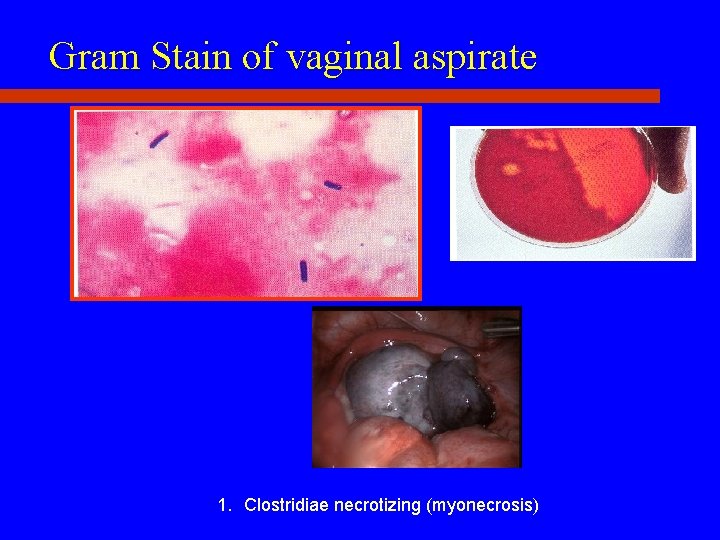
Gram Stain of vaginal aspirate 1. Clostridiae necrotizing (myonecrosis)

Prevention and Treatment • • • Remove dead tissue Remove debris Foreign bodies Penicillin Hyperbaric oxygen

TETANUS

Cl. tetani • Causative organism Cl. tetani • Morphology gram +ve anaerobic with terminal spore • • • Drum Stick appearance Lives in soil and animal feaces. e, g horse Any wound can infected if contaminated by spores Face & neck wounds are more dangerous why ?
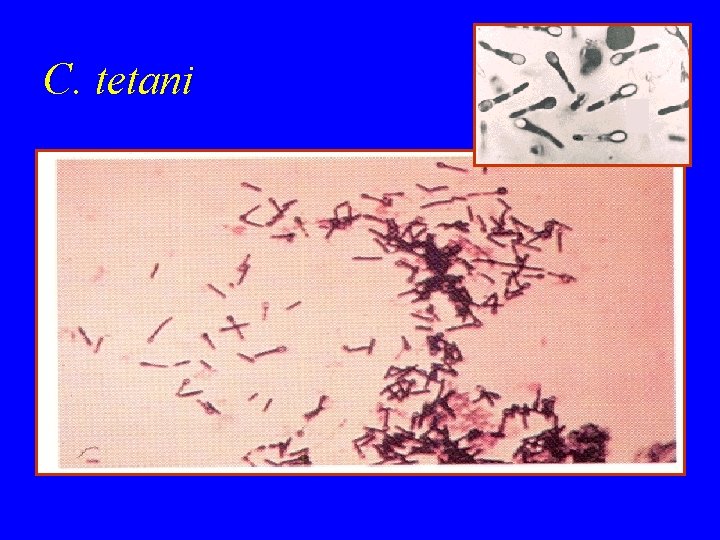
C. tetani
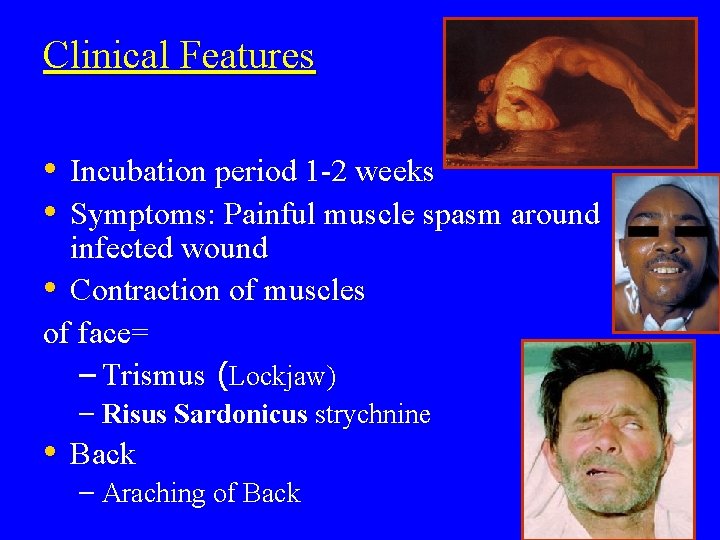
Clinical Features • Incubation period 1 -2 weeks • Symptoms: Painful muscle spasm around infected wound • Contraction of muscles of face= – Trismus (Lockjaw) – Risus Sardonicus strychnine • Back – Araching of Back
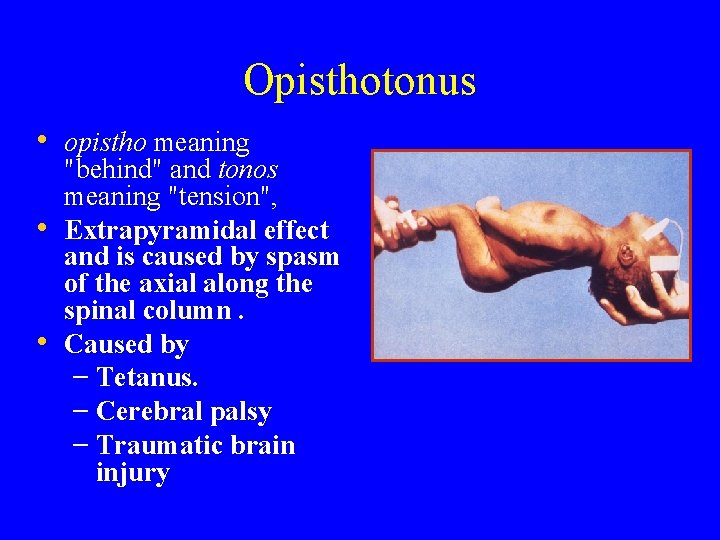
Opisthotonus • opistho meaning • • "behind" and tonos meaning "tension", Extrapyramidal effect and is caused by spasm of the axial along the spinal column. Caused by – Tetanus. – Cerebral palsy – Traumatic brain injury

Pathogenesis • 1 ) Tetanospasmin most important powerful • • exotoxin 2) Totanolysin No invasion or Bacteraernia Toxin is a protein It inhibits transmission of normal inhibitory messages from central nervous system at anterior horn cells of cord
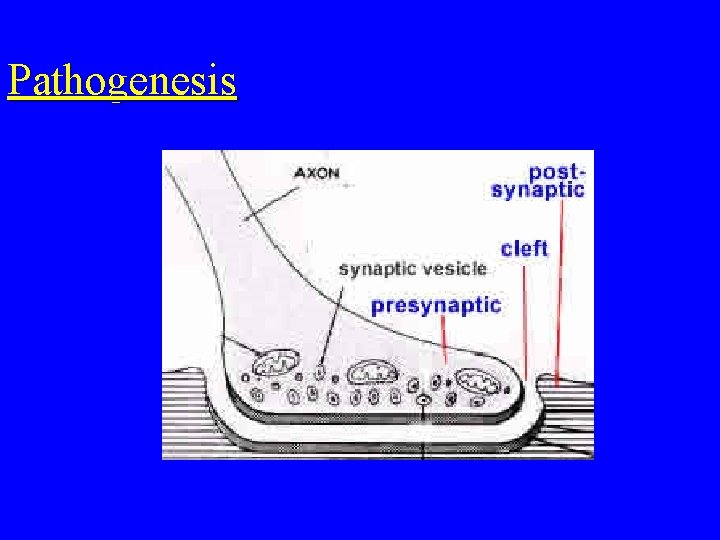
Pathogenesis

Diagnosis • Mainly by clinical • Laboratory not important • Lab – Organism strict anaerobe – Very motile , spread on agar.
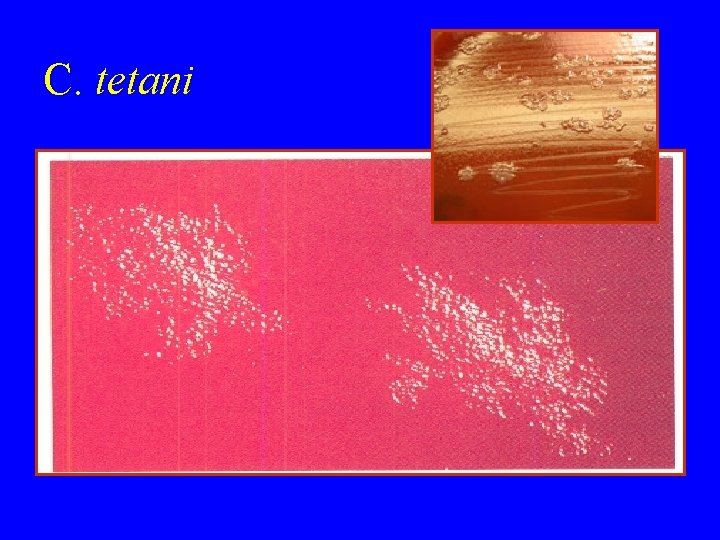
C. tetani

Prevention • • Toxoid vaccine: Vaccination D P T 2 , 4 , 6 , 18 months & 5 Year Booster every 10 years

Treatment. • • Cleaning of wound Removal of Foreign body Specific by antitoxin – Horse serum can caused anaphylaxis & shock must be tested first – Human immunoglobulin – Antibiotics. Penicillin Supportive treatment – 2. Dark pace, fluids – 3. Sedative valium

CLOSTRIDIUM BOTULINUIM

Habitat • Soil, Ponds AND Lakes

Toxin • • • Exotoxin Protein Heat labile at 100 OC • • • 3 kg kill all population of the world Dictated for by lysogenic phage Resist gastrointestinal enzymes – The most powerful toxin known Lethal dose 1 µg human

Botulism • • From canned food. , sea food e_g. salmon Not well cooked Spores resist heat at 100 o. C then multiply and produce toxin

ENFANTILE BOTULISM • Ingestion of Spores germination in the • • gut Botulism Week child Cranial nerve Constipation Other

Botulism Patogenesis • • • Ingested - incubation period 12 -36 hour 7 Types Mainly types A, B, E, F Attacks neuromuscular junctions Prevents release of acetylcholine

Symptoms • Funny eye movement as if cranial nerve • affected when bulbar area of the brain affected Respiratory and circulatory collapse

SPECIMENS • Suspected food • From the patient – Faeces – Serum growth • Toxin detection by mouse – incubation paralysis and death

INFANTILE BOTULISM • • • Week lethargic child Constipation Respiratory and cardiac arrest Due to colonization of intestine by CI. botulinum Diagnosis by - Culture of stools Detection of toxin in feaces

• Treatment • 1) Supportive • 2) Horse antitoxin • Prevention • 1) Adequate pressure • cooking autoclaving 2) Heating of food for 10 minutes at 100 OC

Botox

C. DIFFICILE • PSEUDOMEMBRANOUS COLITIS – 90% OF CASES CAUSED BY C. DIFF – LONG TERM TREATMENT WITH BROAD SPECTRUM ANTIBIOTICS OR CHEMO • NOSOCOMIAL DISEASE • KNOCK DOWN NORMAL FLORA • CLINDAMYCIN, AMPICILLIN, CEPHALOSPORINS • CHEMOTHERAPEUTIC AGENTS

C. DIFFICILE • OVERGROWTH OF C. DIFFICILE – TOXIN THEN PRODUCED • A -FRAGMENT = ENTEROTOXIN • B -FRAGMENT = CYTOLYTIC TOXIN • PSEUDOMEMBRANE SIMILAR TO THAT OF C. DIPHTHERIAE – BACTERIA, FIBRIN, WBC, DEAD – TISSUE CELLS - TOUGH

C. DIFFICILE • DIARRHEA FIRST – ELECTROLYTE & FLUID LOSS – LEADS TO DEHYDRATION • INTESTINAL BLOCKAGE – CONTENTS BLOCKED – COLON BULGES • PERFORATION, RUPTURE SEPSIS
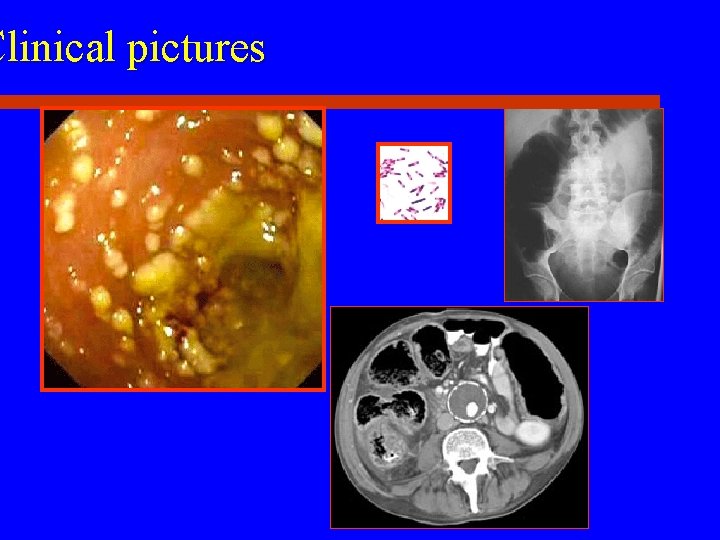
Clinical pictures

C. DIFFICILE • RAPID AGGRESSIVE COURSE IN YOUNG • • CHILDREN DIFFICULT TO SELECTIVELY CULTURE – 5 -10% CULTURE + EVEN WITH CONFIRMED DISEASE – TOO MANY NORMAL ANO 2 PRESENT

C. DIFFICILE • SPECIALIZED ISOLATION MEDIA – CCFA – CYCLOSERINE , CEFOXITIN, FRUCTOSE, EGG YOLK AGAR – CCMA – CCFA BUT MANNITOL FOR FRUCTOSE – CDMN – CYSTEINE HYDROCHLORIDE, MOXALACTAM, NORFLOXACIN AGAR
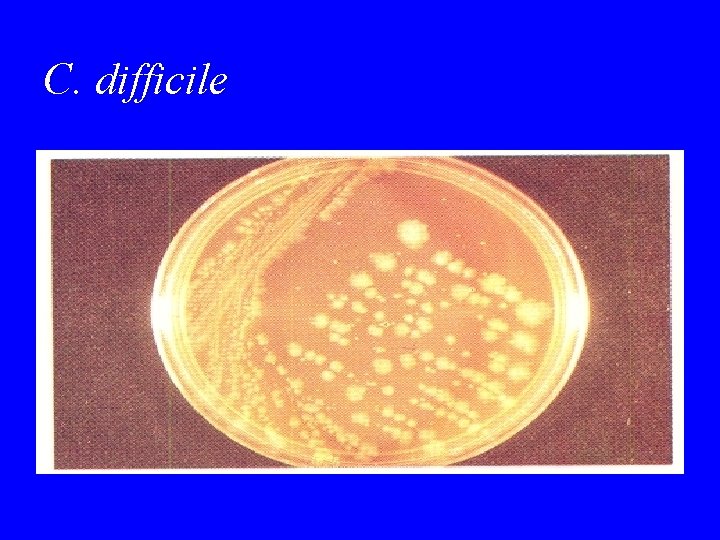
C. difficile

C. difficile

C. DIFFICILE • C. DIFFICILE IS NORMAL FLORA – ISOLATION NOT ENOUGH • NEED TOXIN ASSAY TO CONFIRM • CELL-FREE STOOL EXTRACT – LATEX AGGLUTINATION SCREEN • SOME CROSS-REACTIVITY – EIA TO CONFIRM

Major Clostridial Diseases
- Slides: 106