Client Indiabulls Group Remark Benefit Manual Employee Benefit

Client Indiabulls Group Remark Benefit Manual Employee Benefit Manual Policy period 1 st April 2017 to 31 st March 2018

Disclaimer: This benefit summary will serve as a guide to the benefits provided by Indiabulls Group. The information contained here is only a summary of the policy documents which are kept by the company. If there is a conflict in interpretation, terms & conditions of the policy will prevail. Prepared by Marsh India Insurance Brokers Private Limited 1201 -02, Tower 2, One Indiabulls Centre, Jupiter Mills Compound 841, Senapati Bapat Marg, Elphinstone Road (W), Mumbai 400 013 Tel: +91 22 66512900 Fax: +91 22 66512901 Copyright © 2005. All rights reserved. No part of this publication may be reproduced, stored in the retrieval system, or be transmitted in any form or by any means, electronic or mechanical, photocopying, recording or otherwise, without the prior written permission of the publishers.

Program Details Group Mediclaim This insurance scheme is to provide insurance coverage to Indiabulls Group employees and dependents for expenses related to hospitalization due to illness, disease or injury
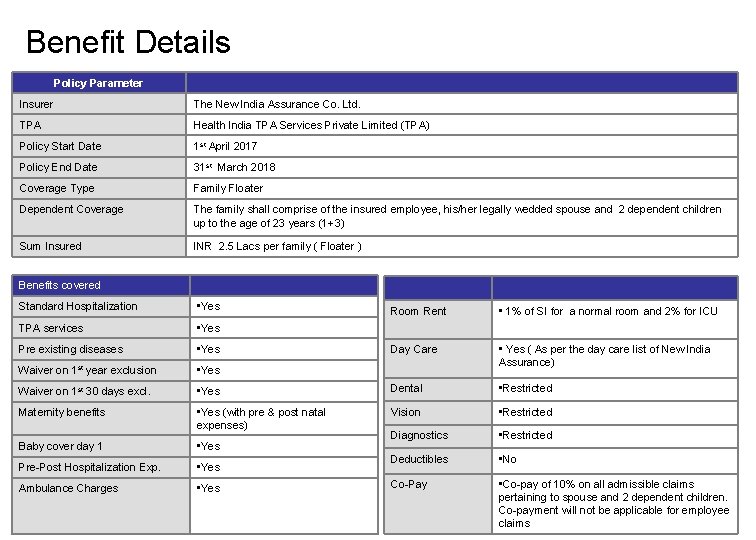
Benefit Details Policy Parameter Insurer The New India Assurance Co. Ltd. TPA Health India TPA Services Private Limited (TPA) Policy Start Date 1 st April 2017 Policy End Date 31 st March 2018 Coverage Type Family Floater Dependent Coverage The family shall comprise of the insured employee, his/her legally wedded spouse and 2 dependent children up to the age of 23 years (1+3) Sum Insured INR 2. 5 Lacs per family ( Floater ) Benefits covered Standard Hospitalization • Yes TPA services • Yes Pre existing diseases • Yes Waiver on 1 st year exclusion • Yes Waiver on 1 st 30 days excl. Room Rent • 1% of SI for a normal room and 2% for ICU Day Care • Yes ( As per the day care list of New India Assurance) • Yes Dental • Restricted Maternity benefits • Yes (with pre & post natal expenses) Vision • Restricted Baby cover day 1 • Yes Diagnostics • Restricted Pre-Post Hospitalization Exp. • Yes Deductibles • No Ambulance Charges • Yes Co-Pay • Co-pay of 10% on all admissible claims pertaining to spouse and 2 dependent children. Co-payment will not be applicable for employee claims
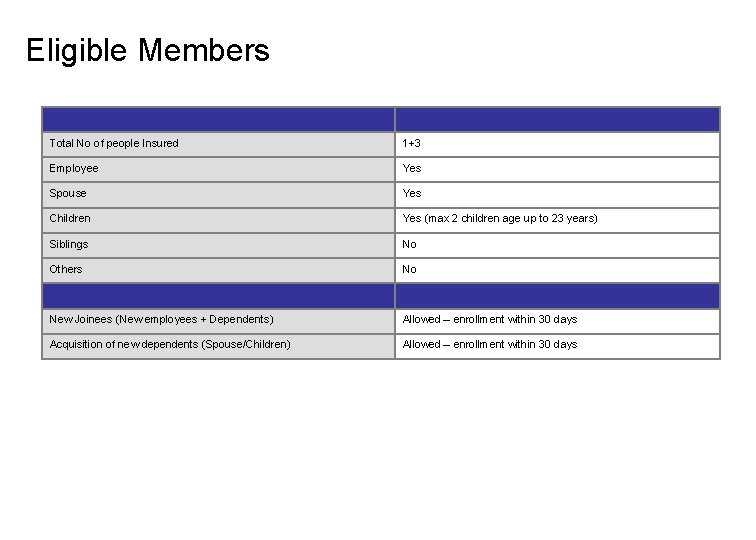
Eligible Members Total No of people Insured 1+3 Employee Yes Spouse Yes Children Yes (max 2 children age up to 23 years) Siblings No Others No New Joinees (New employees + Dependents) Allowed – enrollment within 30 days Acquisition of new dependents (Spouse/Children) Allowed – enrollment within 30 days
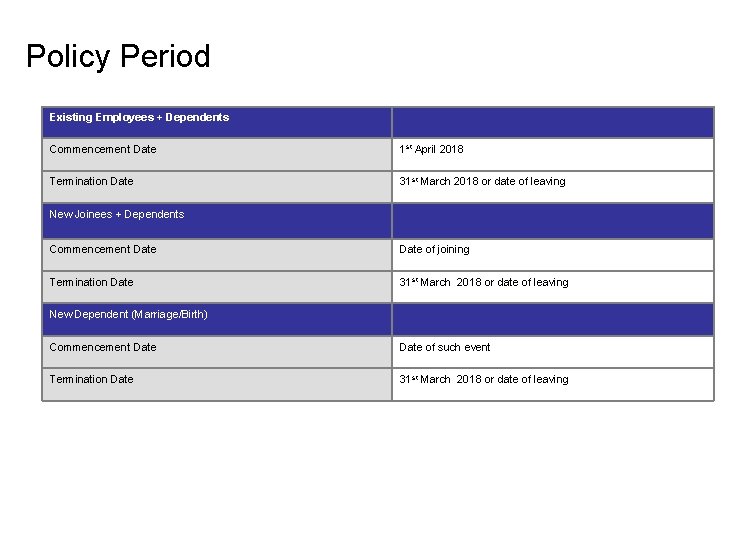
Policy Period Existing Employees + Dependents Commencement Date 1 st April 2018 Termination Date 31 st March 2018 or date of leaving New Joinees + Dependents Commencement Date of joining Termination Date 31 st March 2018 or date of leaving New Dependent (Marriage/Birth) Commencement Date of such event Termination Date 31 st March 2018 or date of leaving

Standard Hospitalization Reimbursement of expenses related to • Room and boarding • Doctors fees • Intensive Care Unit • Nursing expenses • Surgical fees, operating theatre, anesthesia and oxygen and their administration • Physical therapy • Drugs and medicines consumed on the premises • Hospital miscellaneous services (such as laboratory, x-ray, diagnostic tests) • Dressing, ordinary splints and plaster casts • Costs of prosthetic devices if implanted during a surgical procedure • Radiotherapy and chemotherapy • Organ transplantation including the treatment costs of the donor but excluding the costs of the organ A) The expenses shall be reimbursed provided they are incurred in India and within the policy period. Expenses will be reimbursed to the covered member depending on the level of cover that he/she is entitled to. B) Expenses on Hospitalization for minimum period of 24 hours are admissible. However this time limit will not apply for specific treatments i. e. Dialysis, Chemotherapy, Radiotherapy, Eye surgery, Dental Surgery, Lithotripsy (kidney stone removal), Tonsillectomy, D & C taken in the Hospital/Nursing home and the insured is discharged on the same day of the treatment will be considered to be taken under Hospitalization Benefit. C) A security deposit may be collected from the empanelled hospitals which may be reimbursed fully or partially post deduction of non admissible expenses and once cashless settlement is done by the TPA.

Room Rent Capping √ Applicable Room Rent / Nursing / Bed Expenses charged by the hospital / nursing home applicable as follows: Room Rent Capping Example Floater : • 1 % of Sum Insured for Normal Room per day • 2% of Sum Insured for ICU per day Floater : • For a sum insured of Rs. 2. 5 lakhs the room rent cap shall be Rs. 2, 500/- per day for normal room and Rs 5, 000/- for ICU per day Note: All other related charges except for medicines will be in accordance with room rent restriction. In the event of the insured utilizing room rent higher than his/her limits , expenses for all associated charges will be deducted on pro-rata basis

Maternity Benefits Reimbursement of expenses related to maternity as per √ Applicable • The maximum benefit allowable will be Rs. 35, 000/- within the Sum Insured, max up to 2 children. There are special conditions applicable to the Maternity Expenses Benefits as below: • These benefits are admissible only if the expenses are incurred in Hospital/Nursing Home as in-patients in India. • Claim in respect of delivery for only first two children and/or operations associated therewith will be considered in respect of any one Insured Person covered under the Policy or any renewal thereof. Those Insured Persons who already have two or more living children will not be eligible for this benefit. • Expenses incurred in connection with voluntary medical termination of pregnancy during the first 12 weeks from the date of conception are not covered. Benefit Details Maximum Benefit allowable INR 35, 000 Restriction on no of children Maximum of 2 children 9 Months waiting period Not Applicable (waived off) Pre & post natal Covered up to INR 10, 000 within maternity limit Only Hospitalization expenses will be covered
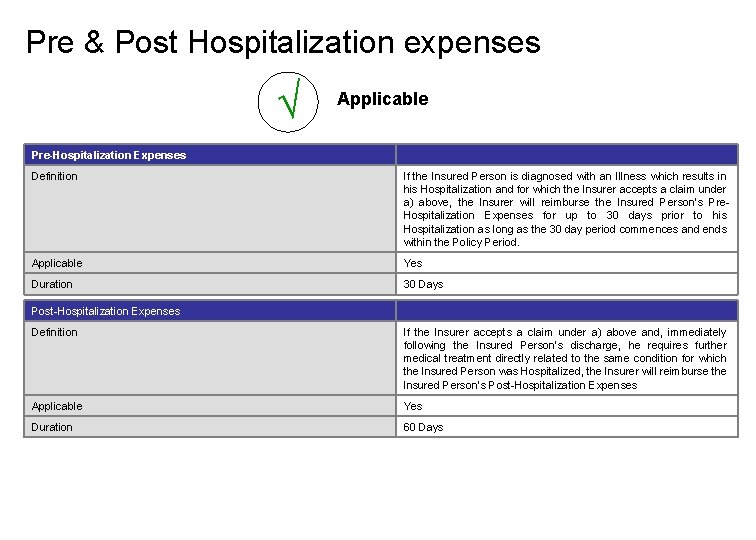
Pre & Post Hospitalization expenses √ Applicable Pre-Hospitalization Expenses Definition If the Insured Person is diagnosed with an Illness which results in his Hospitalization and for which the Insurer accepts a claim under a) above, the Insurer will reimburse the Insured Person’s Pre. Hospitalization Expenses for up to 30 days prior to his Hospitalization as long as the 30 day period commences and ends within the Policy Period. Applicable Yes Duration 30 Days Post-Hospitalization Expenses Definition If the Insurer accepts a claim under a) above and, immediately following the Insured Person’s discharge, he requires further medical treatment directly related to the same condition for which the Insured Person was Hospitalized, the Insurer will reimburse the Insured Person’s Post-Hospitalization Expenses Applicable Yes Duration 60 Days
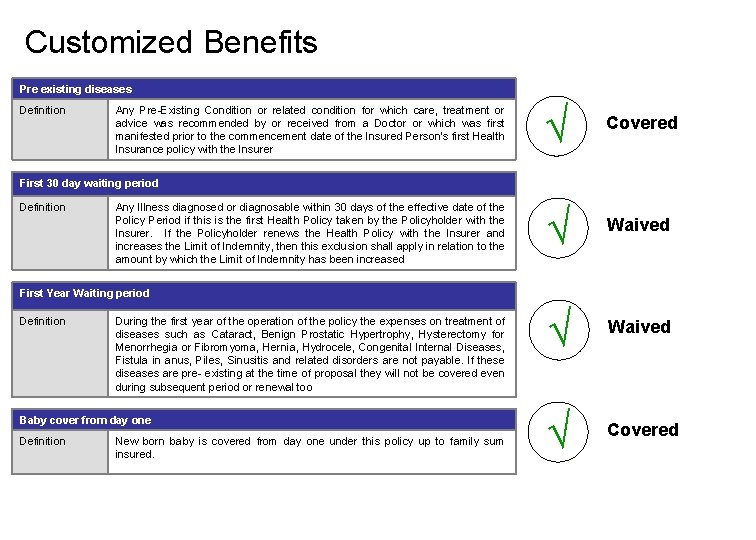
Customized Benefits Pre existing diseases Definition Any Pre-Existing Condition or related condition for which care, treatment or advice was recommended by or received from a Doctor or which was first manifested prior to the commencement date of the Insured Person’s first Health Insurance policy with the Insurer √ Covered √ Waived √ Covered First 30 day waiting period Definition Any Illness diagnosed or diagnosable within 30 days of the effective date of the Policy Period if this is the first Health Policy taken by the Policyholder with the Insurer. If the Policyholder renews the Health Policy with the Insurer and increases the Limit of Indemnity, then this exclusion shall apply in relation to the amount by which the Limit of Indemnity has been increased First Year Waiting period Definition During the first year of the operation of the policy the expenses on treatment of diseases such as Cataract, Benign Prostatic Hypertrophy, Hysterectomy for Menorrhegia or Fibromyoma, Hernia, Hydrocele, Congenital Internal Diseases, Fistula in anus, Piles, Sinusitis and related disorders are not payable. If these diseases are pre- existing at the time of proposal they will not be covered even during subsequent period or renewal too Baby cover from day one Definition New born baby is covered from day one under this policy up to family sum insured.
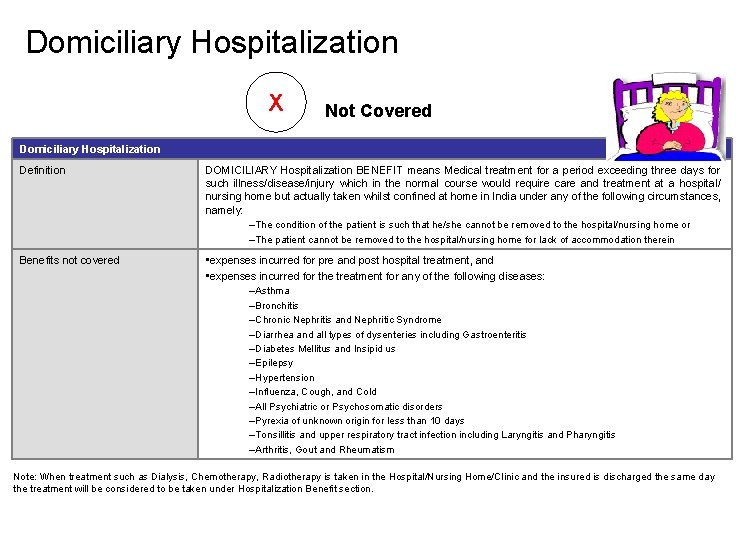
Domiciliary Hospitalization X Not Covered Domiciliary Hospitalization Definition DOMICILIARY Hospitalization BENEFIT means Medical treatment for a period exceeding three days for such illness/disease/injury which in the normal course would require care and treatment at a hospital/ nursing home but actually taken whilst confined at home in India under any of the following circumstances, namely: –The condition of the patient is such that he/she cannot be removed to the hospital/nursing home or –The patient cannot be removed to the hospital/nursing home for lack of accommodation therein Benefits not covered • expenses incurred for pre and post hospital treatment, and • expenses incurred for the treatment for any of the following diseases: –Asthma –Bronchitis –Chronic Nephritis and Nephritic Syndrome –Diarrhea and all types of dysenteries including Gastroenteritis –Diabetes Mellitus and Insipid us –Epilepsy –Hypertension –Influenza, Cough, and Cold –All Psychiatric or Psychosomatic disorders –Pyrexia of unknown origin for less than 10 days –Tonsillitis and upper respiratory tract infection including Laryngitis and Pharyngitis –Arthritis, Gout and Rheumatism Note: When treatment such as Dialysis, Chemotherapy, Radiotherapy is taken in the Hospital/Nursing Home/Clinic and the insured is discharged the same day the treatment will be considered to be taken under Hospitalization Benefit section.
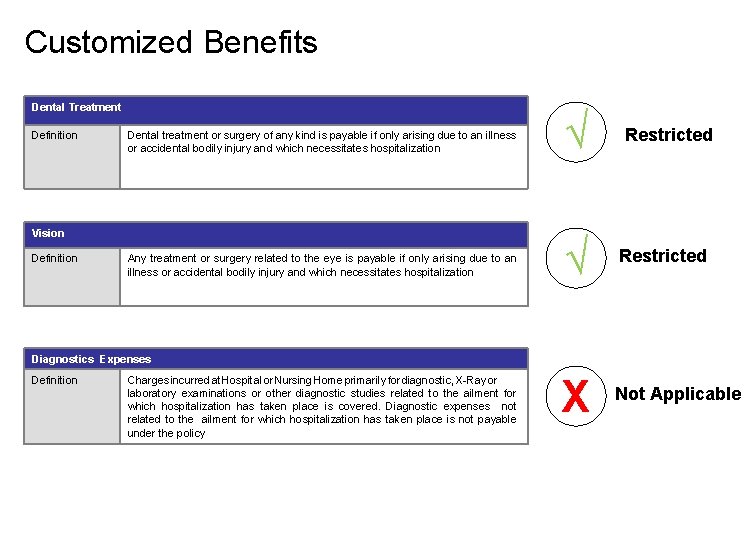
Customized Benefits Dental Treatment Definition Dental treatment or surgery of any kind is payable if only arising due to an illness or accidental bodily injury and which necessitates hospitalization Vision Definition Any treatment or surgery related to the eye is payable if only arising due to an illness or accidental bodily injury and which necessitates hospitalization √ Restricted X Not Applicable Diagnostics Expenses Definition Charges incurred at Hospital or Nursing Home primarily for diagnostic, X-Ray or laboratory examinations or other diagnostic studies related to the ailment for which hospitalization has taken place is covered. Diagnostic expenses not related to the ailment for which hospitalization has taken place is not payable under the policy

Ambulance services √ Covered Ambulance Services Definition The Insurer will pay for Emergency ambulance road transportation by a licensed ambulance service to the nearest Hospital where Emergency Health Services can be rendered. Coverage is only provided in the event of an Emergency. Amount restriction One way of Ambulance Costs for emergency transportation- Maximum INR 2, 000 person

General Exclusions • Injury or disease directly or indirectly caused by or arising from or attributable to War or War-like situations • Circumcision unless necessary for treatment of disease, vaccination, inoculation • Dental treatment or surgery of any kind unless requiring hospitalization. • Congenital external diseases or defects/anomalies • HIV and AIDS • Hospitalization for convalescence, general debility, run down condition or rest cure, intentional self-injury, use of intoxicating drugs/ alcohol. • Venereal diseases • Injury or disease caused directly or indirectly by nuclear weapons • Naturopathy/acupressure/acupuncture, magnetic and such otherapies • Any non-medical expenses like registration fees, service charges, surcharges, admission fees, charges for medical records, cafeteria charges, telephone charges, etc (Refer slide 20 and 21) • Ayurvedic treatment –Permitted only if taken in a government hospital as in-patient. • Cost of spectacles, contact lenses, hearing aids • Any cosmetic or plastic surgery except for correction of injury/as part of any illness. • Hospitalization for diagnostic tests only Vitamins and tonics unless used for treatment of injury or disease • Infertility treatment/sterilization • Voluntary termination of pregnancy during first 12 weeks (MTP) • Procedures/treatments normally done on OPD even if converted as inpatient in hospital for more than 24 hours or carried out in day care centers. • External and or durable Medical/Non medical equipment of any kind used for diagnosis and or treatment including CPAP, CAPD infusion, ambulatory devices like walkers, crutches, braces, glucometer and any medical equipment which subsequently is used at home. • The above are only indicative and not exhaustive. 15

Non Payable Expenses under Mediclaim Policy • • • • Admission charges or Kit / Registration/Token/Supplementary /service charges/Pre – post Consultants home visit charges Transportation/Ambulance/Local conveyance charges where ambulance is not required medically and as per the policy conditions. Administrative/Charges of Identification Band/Identification card Attendee or attendance staff /cleaner charges Amenity of the hospital/water , electricity, luxurious utility charges/establishment charges/ charges related to linen/laundry/washing charges/establishment charges/any sort of overhead/lodging charges. Any charges named as Sundry/Stationary/File/Folder/Documentation/ xerox charges/medico legal charges/ charges of birth or medical certificate or related to any certificate issuance. Telephone charges/TV charges/Video charges/Cable charges/internet charges/AC charges/cost of cassette/CD charges in case of endoscopy, color doppler etc/camera and related charges Mess/ Food charges/Diet charges/Nutrition and nutrition planning charges/Diabetic charges/cost related to mineral water Input & Output charges/Daily pass charges, /relative stay/extra bed charges/companion stay or related charges/donor screening/organ harvesting charges/, private nursing charges during hospitalisation. Biomedical Waste charges/waste maintenance charges Rehabilitation charges/charity or charity related charges/donations, miscellaneous charges whose details are not provided and details which are not related to the treatment. Charges of nebuliser/mask with T pipe/bandages/ dynaplast/ dynacrepe/ oxygen cylinder/mask/Tissue papers/diapers/underpads/head caps/face mask/under sheet/gloves/gown/baby powder/oil/tooth paste/brush/soap/bathing charges/sponging charges/cologne/spray/room freshener/olive oil/soap charges/mouth wash/ear buds/hair removers/ razors/gallant blades/ glucotrend strips/ECG electrodes/Diasticks/glucometer/stockings/nasal CPAP machine charges or rentals/vaccination charges/rentals or charges of any machinery billed in the hospitalisation bill Any type of belt charges/knee caps/braces/walker charges, arm pouch/arm sling charges/crutches/wheel chair charges/hot water bottle charges/ baby kit/urine pot charges/charges of urometer/spirometer/thermometer/commode/nursing charges related to commode maintenance Cardiac rehabilitation charges The above are only indicative and not exhaustive. Refer policy terms and conditions 16
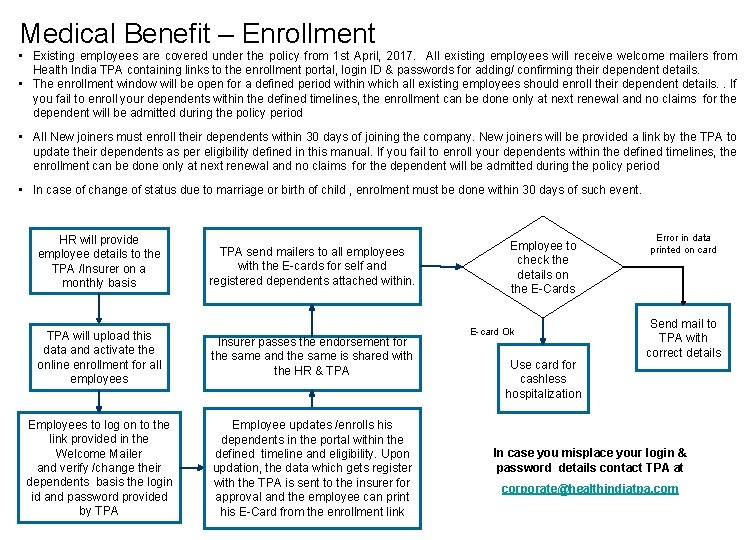
Medical Benefit – Enrollment • Existing employees are covered under the policy from 1 st April, 2017. All existing employees will receive welcome mailers from Health India TPA containing links to the enrollment portal, login ID & passwords for adding/ confirming their dependent details. • The enrollment window will be open for a defined period within which all existing employees should enroll their dependent details. . If you fail to enroll your dependents within the defined timelines, the enrollment can be done only at next renewal and no claims for the dependent will be admitted during the policy period • All New joiners must enroll their dependents within 30 days of joining the company. New joiners will be provided a link by the TPA to update their dependents as per eligibility defined in this manual. If you fail to enroll your dependents within the defined timelines, the enrollment can be done only at next renewal and no claims for the dependent will be admitted during the policy period • In case of change of status due to marriage or birth of child , enrolment must be done within 30 days of such event. HR will provide employee details to the TPA /Insurer on a monthly basis TPA send mailers to all employees with the E-cards for self and registered dependents attached within. TPA will upload this data and activate the online enrollment for all employees Insurer passes the endorsement for the same and the same is shared with the HR & TPA Employees to log on to the link provided in the Welcome Mailer and verify /change their dependents basis the login id and password provided by TPA Employee updates /enrolls his dependents in the portal within the defined timeline and eligibility. Upon updation, the data which gets register with the TPA is sent to the insurer for approval and the employee can print his E-Card from the enrollment link Employee to check the details on the E-Cards E-card Ok Use card for cashless hospitalization Error in data printed on card Send mail to TPA with correct details In case you misplace your login & password details contact TPA at corporate@healthindiatpa. com

Medical Benefit – Cashless Process Cashless means the TPA Administrator may authorize upon a Policyholder’s request for direct settlement of eligible services and it’s according charges between a Network Hospital and the Administrator. In such case the Administrator will directly settle all eligible amounts with the Network Hospital. The Insured Person may have to pay a security deposits at the commencement of the treatment. All non medical expenses and non admissible expenses will be deducted from the security deposit by the hospital and the balance will be refunded to Insured. NOTE: Claim Documents for Reimbursement can be couriered to the below mentioned address: Health India TPA Services Private Limited Address: Number 406 -412, Floor IV Neelkanth Corporate IT Park Kirol Road, Vidyavihar (West), Mumbai-400088 List of hospitals in the Health India TPA Services Private Limited (TPA) network eligible for cashless process www. healthindiatpa. com Note : Please refer Website or contact your Relationship Managers for updated hospital list at all times since the list is subject to changes Contact the below 24 X 7 call center number : Customer Care No: - 02266131199 Senior. Citizens Toll free no: 1800226970 Toll free no: - 1800220102 In case of anything related to cashless please call at Cashless Cell No: - 8450957103 Cashless Landline: - 022 -66867559 / 66867545 / 66867533 Note : Patients seeking treatment under cashless hospitalization are eligible to make claims under pre and post hospitalization expenses. For all such expenses the bills and other required documents needs to submitted separately as part of the claims reimbursement.
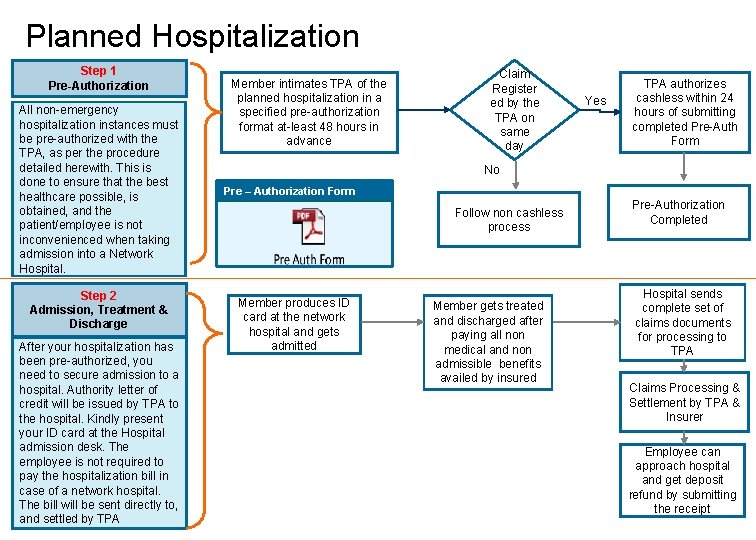
Planned Hospitalization Step 1 Pre-Authorization All non-emergency hospitalization instances must be pre-authorized with the TPA, as per the procedure detailed herewith. This is done to ensure that the best healthcare possible, is obtained, and the patient/employee is not inconvenienced when taking admission into a Network Hospital. Step 2 Admission, Treatment & Discharge After your hospitalization has been pre-authorized, you need to secure admission to a hospital. Authority letter of credit will be issued by TPA to the hospital. Kindly present your ID card at the Hospital admission desk. The employee is not required to pay the hospitalization bill in case of a network hospital. The bill will be sent directly to, and settled by TPA Member intimates TPA of the planned hospitalization in a specified pre-authorization format at-least 48 hours in advance Claim Register ed by the TPA on same day Yes TPA authorizes cashless within 24 hours of submitting completed Pre-Auth Form No Pre – Authorization Form Follow non cashless process Member produces ID card at the network hospital and gets admitted Member gets treated and discharged after paying all non medical and non admissible benefits availed by insured Pre-Authorization Completed Hospital sends complete set of claims documents for processing to TPA Claims Processing & Settlement by TPA & Insurer Employee can approach hospital and get deposit refund by submitting the receipt
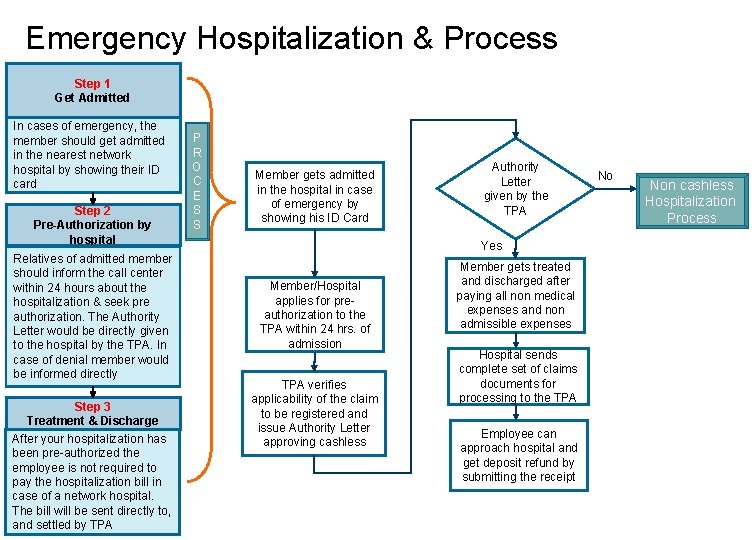
Emergency Hospitalization & Process Step 1 Get Admitted In cases of emergency, the member should get admitted in the nearest network hospital by showing their ID card Step 2 Pre-Authorization by hospital Relatives of admitted member should inform the call center within 24 hours about the hospitalization & seek pre authorization. The Authority Letter would be directly given to the hospital by the TPA. In case of denial member would be informed directly Step 3 Treatment & Discharge After your hospitalization has been pre-authorized the employee is not required to pay the hospitalization bill in case of a network hospital. The bill will be sent directly to, and settled by TPA P R O C E S S Member gets admitted in the hospital in case of emergency by showing his ID Card Authority Letter given by the TPA Yes Member/Hospital applies for preauthorization to the TPA within 24 hrs. of admission TPA verifies applicability of the claim to be registered and issue Authority Letter approving cashless Member gets treated and discharged after paying all non medical expenses and non admissible expenses Hospital sends complete set of claims documents for processing to the TPA Employee can approach hospital and get deposit refund by submitting the receipt No Non cashless Hospitalization Process

Non-Cashless Claim Process Admission procedure • In case you choose a non-network hospital you will have to liaise directly with the hospital for admission. Kindly check with the TPA before admission if the Hospital you are planning to go to is blacklisted. Discharge procedure • In case of non network hospital, you will be required to clear the bills and submit the claim to TPA for reimbursement from the insurer. Please ensure that you collect all necessary documents such as – discharge summary, investigation reports etc. for submitting your claim. Submission of hospitalization claim • You must submit the final claim with all relevant documents within 30 days from the date of discharge from the hospital.
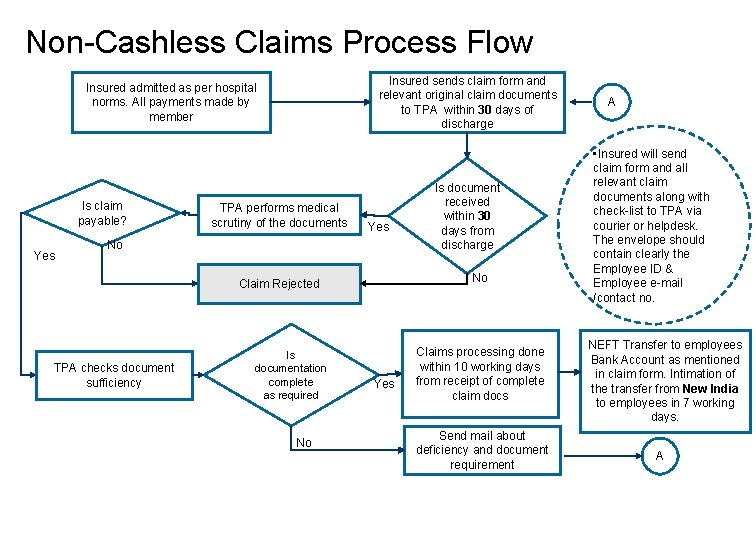
Non-Cashless Claims Process Flow Insured sends claim form and relevant original claim documents to TPA within 30 days of discharge Insured admitted as per hospital norms. All payments made by member Is claim payable? Yes TPA performs medical scrutiny of the documents Yes No No Claim Rejected TPA checks document sufficiency Is documentation complete as required No Is document received within 30 days from discharge Yes Claims processing done within 10 working days from receipt of complete claim docs Send mail about deficiency and document requirement A • Insured will send claim form and all relevant claim documents along with check-list to TPA via courier or helpdesk. The envelope should contain clearly the Employee ID & Employee e-mail /contact no. NEFT Transfer to employees Bank Account as mentioned in claim form. Intimation of the transfer from New India to employees in 7 working days. A

Claim Form and Document Checklist Documents and links Claim Form Checklist for reimbursement Claim Documents Note : Please retain photocopies of all documents submitted
Important Documents and Links Documents and links FAQ’s Definitions Cashless and Reimbursement claim Process IRDA (Insurance Regulatory and Development Authority) http: //www. irdaindia. org/
- Slides: 24