Clean intermittent catheterization as initial management for persistent









- Slides: 13

Clean intermittent catheterization as initial management for persistent cloaca: experience in a regional care center Katie L. Canalichio, Jennifer Ahn, Samuel Rice-Townsend, Caitlin Smith, Anne-Marie Amies Oelschlager, Jeffrey Avansino, Mark Cain, Paul Merguerian, Margarett Shnorhavorian AUA/SPU 2020

Disclosures • None

Background/Aims • Methods for urinary drainage in cloaca: spontaneous voiding, clean intermittent catheterization (CIC), genitourinary diversion (vesicostomy or vaginostomy). • To determine if CIC is a safe method. • To describe the initial management for urinary drainage and reasons for change.

Methods • Retrospective: past 20 years at single center • Inclusion: female cloaca patients status post repair • Exclusion: variant diagnoses, no data • Primary Outcomes: Renal function (trend in serum creatinine and GFR using Bedside Schwartz), upper tract findings on imaging & urinary tract infections (UTIs) were captured for each group.

Results: Patient Characteristics All patients Median age cloacal repair (years) Median follow-up (years) Common channel Short Intermediate Long Not recorded N=22 0. 9 (0. 7, 1. 5) 6. 8 (1. 9, 15. 0) 8/22, 36% 3/22, 14%

Results: Management Groups All patients N=22 Spontaneous Voiding N=7 CIC N=9 GU Diversion N=6

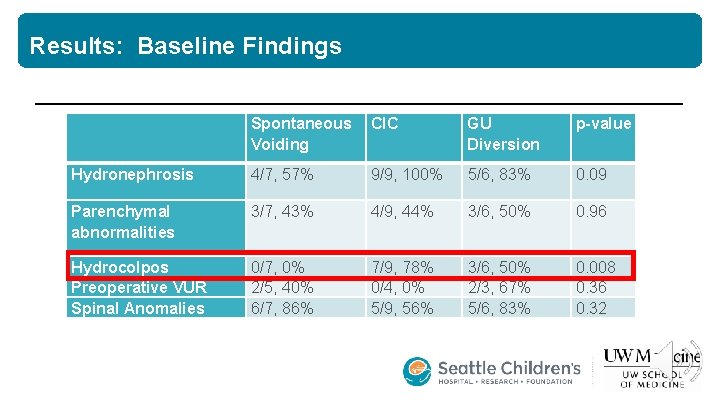
Results: Baseline Findings Spontaneous Voiding CIC GU Diversion p-value Hydronephrosis 4/7, 57% 9/9, 100% 5/6, 83% 0. 09 Parenchymal abnormalities 3/7, 43% 4/9, 44% 3/6, 50% 0. 96 Hydrocolpos Preoperative VUR Spinal Anomalies 0/7, 0% 2/5, 40% 6/7, 86% 7/9, 78% 0/4, 0% 5/9, 56% 3/6, 50% 2/3, 67% 5/6, 83% 0. 008 0. 36 0. 32

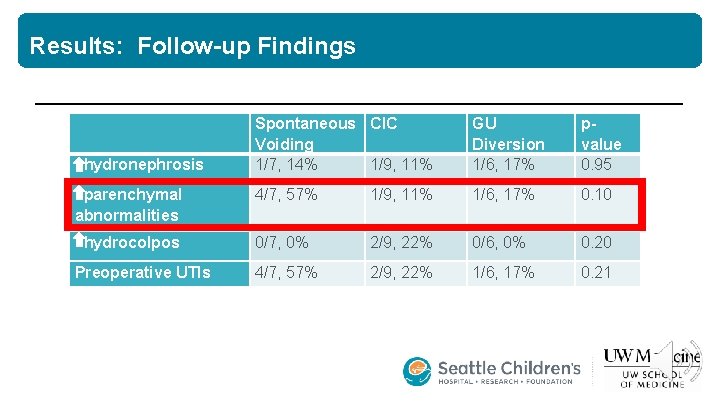
Results: Follow-up Findings Spontaneous CIC Voiding 1/7, 14% 1/9, 11% GU Diversion 1/6, 17% pvalue 0. 95 parenchymal abnormalities 4/7, 57% 1/9, 11% 1/6, 17% 0. 10 hydrocolpos 0/7, 0% 2/9, 22% 0/6, 0% 0. 20 4/7, 57% 2/9, 22% 1/6, 17% 0. 21 hydronephrosis Preoperative UTIs

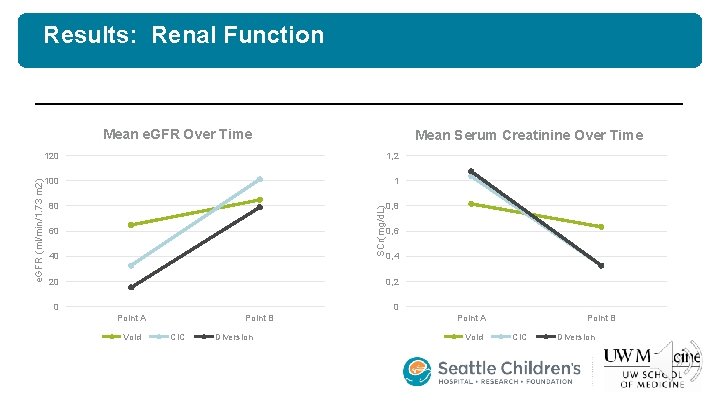
Results: Renal Function Mean Serum Creatinine Over Time 120 1, 2 100 1 80 0, 8 SCr(mg/d. L) e. GFR (ml/min/1. 73 m 2) Mean e. GFR Over Time 60 40 20 0, 6 0, 4 0, 2 0 0 Point A Void Point B CIC Diversion

Change in Management • Two patients from each group required a change in management Reasons Hydronephrosis 3/6, 50% Caregiver burden 2/6, 33% Hydrocolpos 1/6, 17% Urinary retention 1/6, 17% UTI 1/6, 17%

Discussion • Limitations: small study size, retrospective, limited evaluation of renal function in neonate • Strengths: three groups evaluated, all baseline characteristics similar (except for hydrocolpos)

Conclusions • We recommend CIC as first line management. • Reserve diversion in those that CIC is not successful. • Require close follow-up with ultrasounds, labs, urodynamics.

Thank you