Classification of patella morphology by Wiberg and Baumgartl


Classification of patella morphology by Wiberg and Baumgartl Fulkerson JP Disorders of the PF joint 4 th Ed 2004

Patellofemoral (PF) disorder PF dysplasia n PF pain n PF instability n OKU 9 p. 763 -764

Etiology of PF disorder n PF dysplasia n Hypoplasia of the trochlear groove Genetic Miller GF JBJS(Br) 1978 n Developmental n Various trochlear morphologies Fulkerson JP Disorders of the PF joint 4 th Ed 2004

Etiology of PF disorder n PF instability Joint laxity n Connective tissue disorders n OKU-9 1998 Brighton Criteria

Imbalance around the PF articulation n Rapid growth in adolescents n n Thicker and less compliant vastus lateralis n n Imbalances around the PF articulation Exert a relatively unbalanced laterally directed force Quadriceps tightness n Lead to patella alta OKU-9

PF reaction force is high Imbalance Maltracking may comtribute to the onset of anterior pain and instability OKU-9

Merchants’ classification of PF disorders n Trauma n n PF dysplasia n n n n Acute trauma Repetitive trauma (overuse syndrome) Later effects of trauma Lateral patellar compression syndrome Chronic subluxation of the patella Recurrent dislocation of the patella Chronic dislocation of the patella Idiopathic chondromalacia patellae Osteochondritis dissecans Syniovial plicae Insall surgery of the knee 4 th Ed 2006

Characteristics of PF pain Dull and poorly localized n Correlated with activity and position n Jumping n Climbimg n Prolonged sitting n OKU-9

History of PF disorder n Overuse Frequency n Duration n Intensity n n Previous surgeries Fulkerson JP Disorders of the PF joint 4 th Ed 2004

History of PF disorder Complaint n Pain Exacerbated by climbing or descending stairs n Prolonged periods of knee flexion n Fulkerson JP Disorders of the PF joint 4 th Ed 2004

Onset of the problem n Acute onset n Indirect trauma n n n Valgus /external rotation Blunt trauma – Dashboard injury Insidious Underlying strength/flexibility deficits n Potential bony malalignment n Fulkerson JP Disorders of the PF joint 4 th Ed 2004

Nature of pain n Activity related n n n PF malalignment Acute injury Constant pain n n Postsurgical neuroma Referred neurogenic pain Reflex Sympathetic dystrophy Symptoms magnification Psychologic issues Fulkerson JP Disorders of the PF joint 4 th Ed 2004
Physical examination of PF disorder n n n n Gait Lower extremity alignment Q angle Hip and foot examination Knee stability Generalized ligamentous laxity Knee ROM OKU-9

Physical examination of PF disorder PF tracking n Translation n Crepitus n Apprehension n Grinding test n Patellar tilt n OKU-9
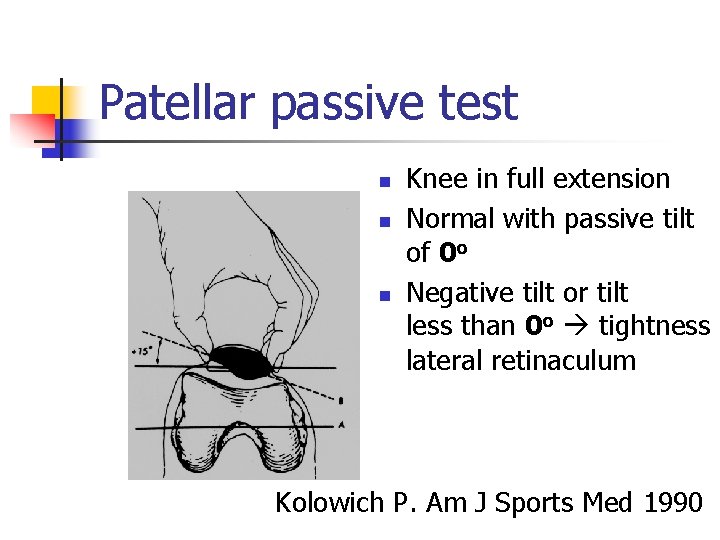
Patellar passive test n n n Knee in full extension Normal with passive tilt of 0 o Negative tilt or tilt less than 0 o tightness lateral retinaculum Kolowich P. Am J Sports Med 1990
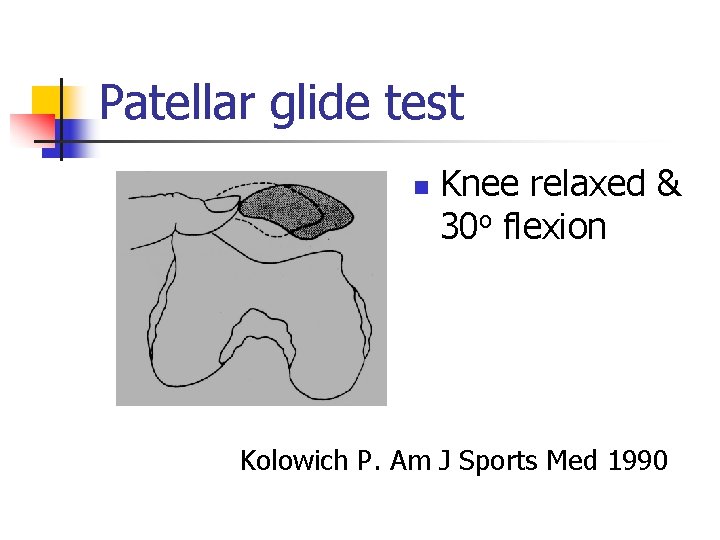
Patellar glide test n Knee relaxed & 30 o flexion Kolowich P. Am J Sports Med 1990

Physical examination of PF disorder Atrophy n Q angle n Leg-length measurement n Foot alignment n OKU-9
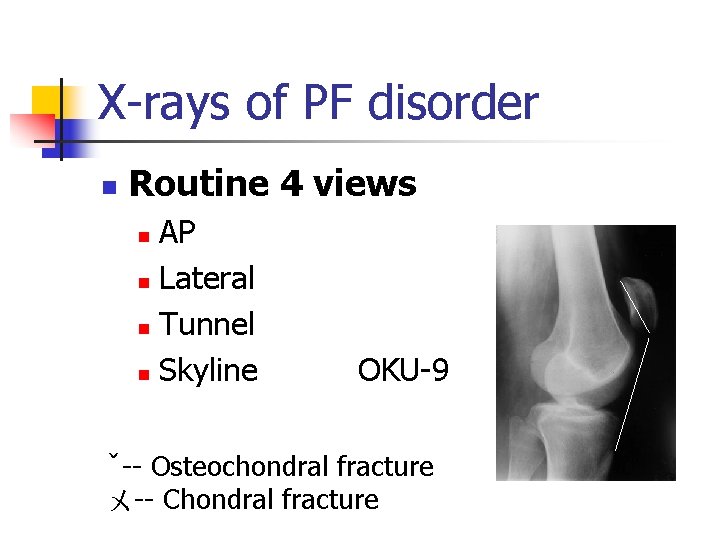
X-rays of PF disorder n Routine 4 views AP n Lateral n Tunnel n Skyline n OKU-9 ˇ-- Osteochondral fracture ㄨ-- Chondral fracture

Various dysplastic patellar morphologies Fulkerson JP Disorders of the PF joint 4 th Ed 2004

X-rays measurement of PF disorder Patellar height n Congruence n Tilt n Subluxation n Dysplasia n
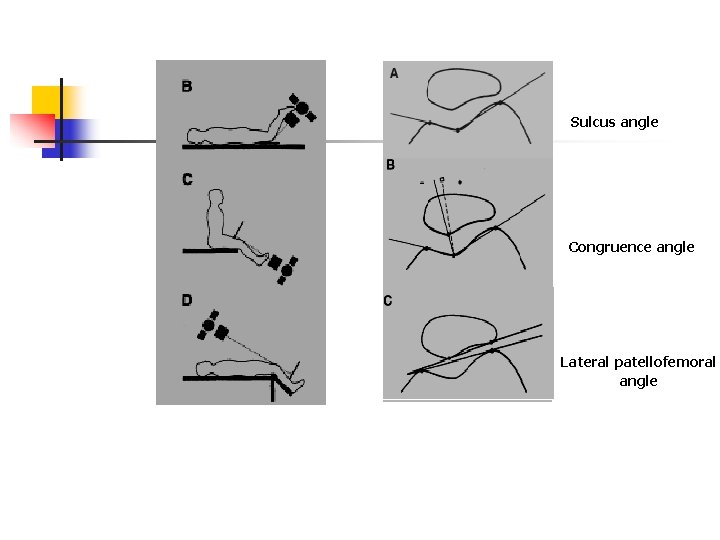
Sulcus angle Congruence angle Lateral patellofemoral angle
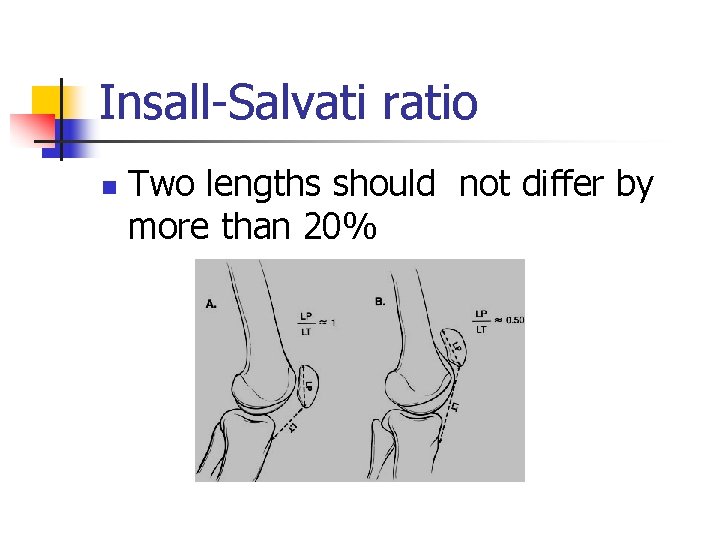
Insall-Salvati ratio n Two lengths should not differ by more than 20%

Congruence angle Sulcus angle COD- Sulcus angle o EOF - Congruence angle o • O is the sulcus central point. C and D are the most lateral and medial points of the femoral trochlea, respectively • OF is the line connecting the point of patellar central ridge and the sulcus central point. • OE is the line bisecting SA.
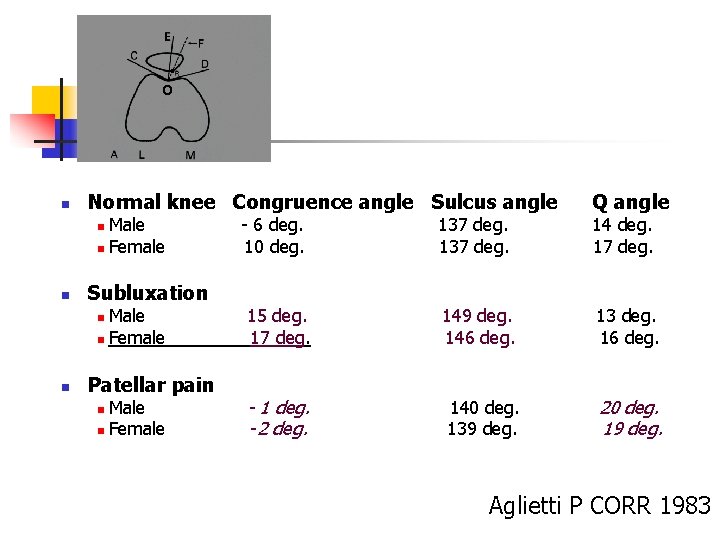
o n Normal knee Congruence angle Sulcus angle Male n Female n n Subluxation Male n Female n n Patellar pain Male n Female n - 6 deg. 10 deg. Q angle 137 deg. 14 deg. 17 deg. 15 deg. 17 deg. 149 deg. 146 deg. 13 deg. 16 deg. - 1 deg. -2 deg. 140 deg. 139 deg. 20 deg. 19 deg. Aglietti P CORR 1983
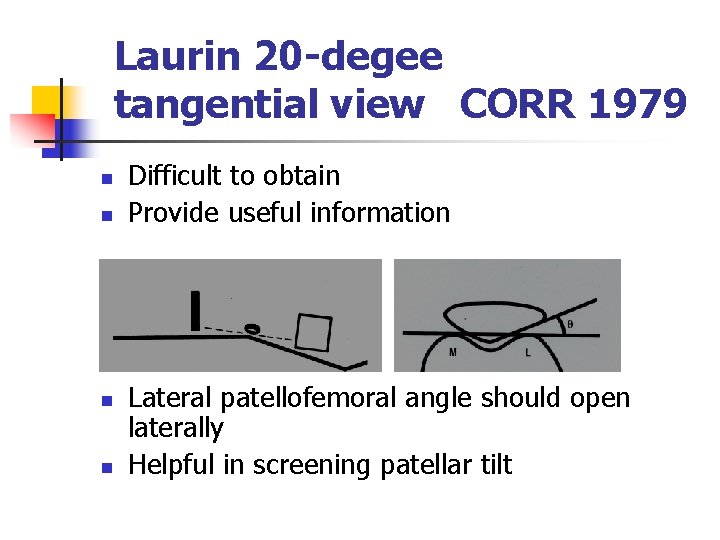
Laurin 20 -degee tangential view CORR 1979 n n Difficult to obtain Provide useful information Lateral patellofemoral angle should open laterally Helpful in screening patellar tilt
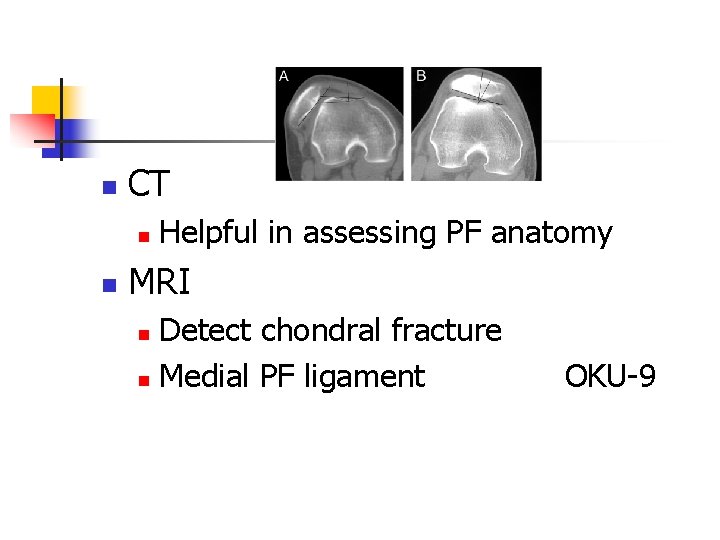
n CT n n Helpful in assessing PF anatomy MRI Detect chondral fracture n Medial PF ligament n OKU-9
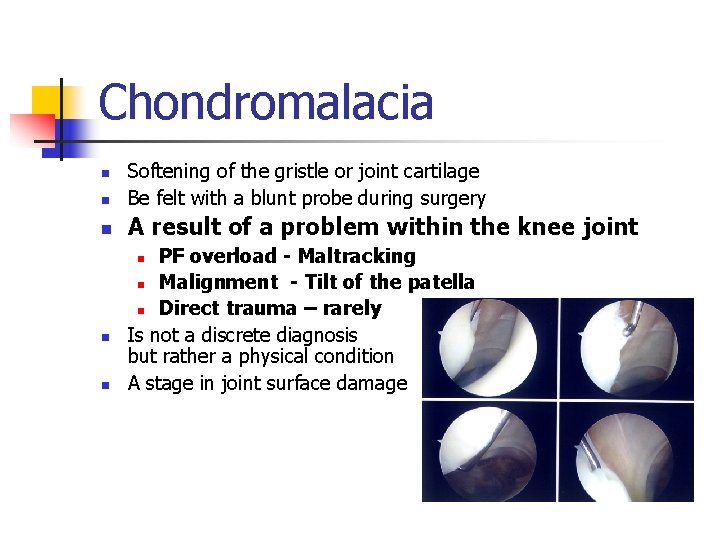
Chondromalacia n Softening of the gristle or joint cartilage Be felt with a blunt probe during surgery n A result of a problem within the knee joint n PF overload - Maltracking n Malignment - Tilt of the patella n Direct trauma – rarely Is not a discrete diagnosis but rather a physical condition A stage in joint surface damage n n n

Grade of chondromalacia n n n Grade Grade I : softing II : fissuring III: superficial fibrillation IV: deep fibrillation V: erosin down to subchondral bone Recorded the depth, size and location Aglietti P. Insall Surgery of the knee 4 th ED 2006

Treatment of PF disorder Nonsurgical n Exercise Stretching the iliotibial band n Mobilize the patella n Medial quadriceps strengthening n Straight leg rising o) n Short-arc (Less than 40 exercise but should be avoided if painful OKU-9 n

Refrain from activities that produce high PF compressive force Running n Jumping n Climbing n Squatting n Long-arc knee extension n Hyperflexion activity n OKU-9

n n Most PF disorder can be successfully treated with nonsurgical treatment Supervised therapy for 6 months Recur symptom – Return to physical therapy Recalcitrant cases – Surgery may be considered OKU-9

Lateral retinacular release n Wildly used Results – unpredictable n Indications n n n OKU-9 Recurrent subluxation Relatively normal Q angle Tight lateral structures - decreased medial glide Lateral tilt with minimal lateral subluxation on radiograph in combination with realignment procedure

Johnson RP Lateral restrain analysis and use of lateral resection CORR 1986 n Primary restrain to medial glide of the patella n n Vastus lateralis oblique - 47. 5% Iliotibial band - 16% Lateral retinaculum – 5% Three structure contributed equally – 31. 5%
Lateral release n Complications n n Hemarthrosis – 10% (1% - 42%) Imcomplete release Medial subluxation Arthroscopic release n n n 7. 1% complications 65% - hemaarthrosis Reduced with electrosurgery Insall Surgery of the knee 4 th ED 2006

Proximal realignment procedure Medial plication n Vastus medialis advancement OKU -9 n

Management of instability Magnitude n Frequency n Presence of associated injury n PF alignment OKU-9 n

Management of acute traumatic patellar dislocation n Immediately surgical repair n n Initial nonsurgical, surgical if subsequent instability n n Hinton RY Orthop Clin North Am 2003 Nikku R Acta Orthop 2005 Associated with osteochondral fracture (40%) n Initial surgery is indicated OKU-9

Atraumatic PF instability Ligament laxity n PF malalignment n OKU-9

Management of atraumatic PF instability n Rehabilitation n n Stretching of lateral structure Patellar mobilization Strengthening VMO Bracing Orthotics for correct malalignment of pronation or pes planovalgus OKU-9

Surgical treatment of PF instability n Proximal realignment n n n Lateral release Medial plication Vastus medialis advancement Medial PF ligament repair or reconstruction Distal realignment n Tibial tubercle n n Medialization Anteriomedialization OKU-9
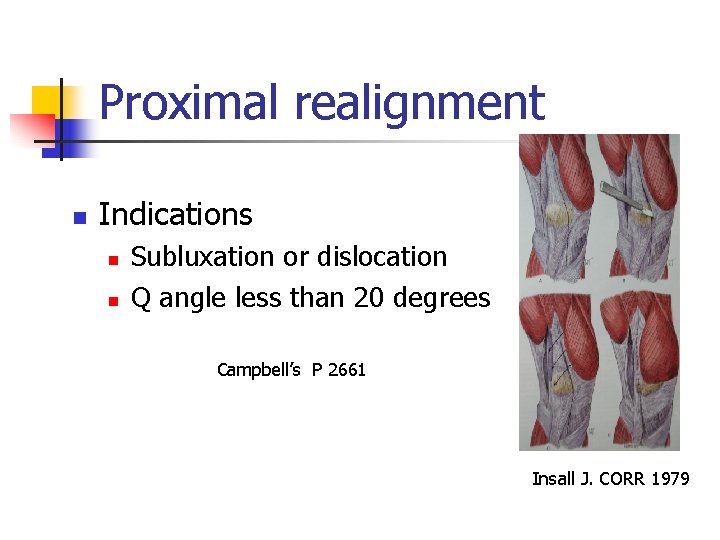
Proximal realignment n Indications n n Subluxation or dislocation Q angle less than 20 degrees Campbell’s P 2661 Insall J. CORR 1979

Distal realignment Skeletal immature - Growth disturbance n Indications n n n Semitendinosus transfer (Galeazzi procedure) n n Recurrent dislocation or subluxation Q angle > 20 degrees 81% - Good and excellent Patellar tendon hemitransfer (Goldthwaite procedure) Campbell’s OP Orthop 2008 P 2661 Baker RH JBJS 1972

Distal realignment Skeletal mature Maquet’s anteriorization of tibial tuberosity n Fulkerson’s anteromedialization of tibial tuberosity n Indications n Recurrent dislocation or subluxation n Q angle > 20 degrees n Campbell’s Op Orthop P. 2661
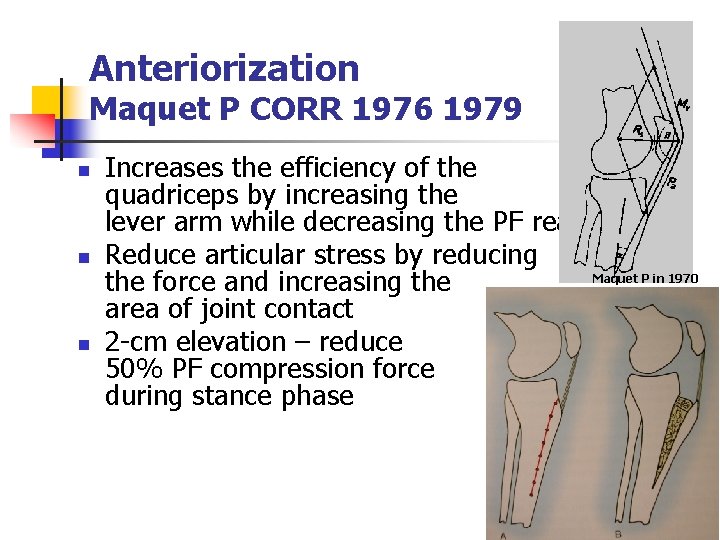
Anteriorization Maquet P CORR 1976 1979 n n n Increases the efficiency of the quadriceps by increasing the lever arm while decreasing the PF reaction Reduce articular stress by reducing Maquet P in 1970 the force and increasing the area of joint contact 2 -cm elevation – reduce 50% PF compression force during stance phase

Anteriorization n 2 cm elevation –> reduce ½ PF joint reaction force Maquet CORR 1979 1 cm –> Reduce 1/3 PF joint reaction force Bandi 1974 Progressive decreases and proximal migration of the contact area Nakamura JBJS 1985
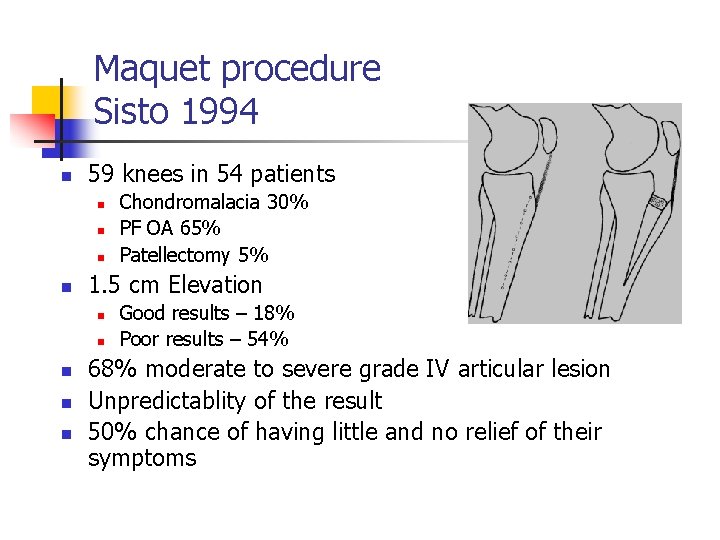
Maquet procedure Sisto 1994 n 59 knees in 54 patients n n 1. 5 cm Elevation n n Chondromalacia 30% PF OA 65% Patellectomy 5% Good results – 18% Poor results – 54% 68% moderate to severe grade IV articular lesion Unpredictablity of the result 50% chance of having little and no relief of their symptoms
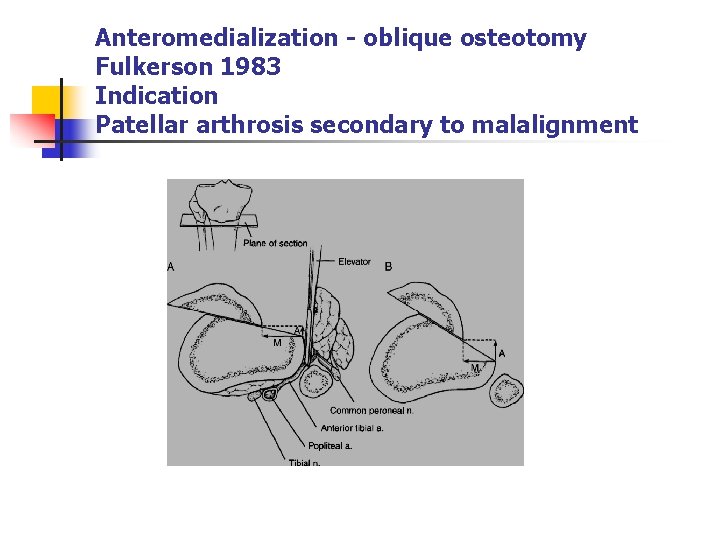
Anteromedialization - oblique osteotomy Fulkerson 1983 Indication Patellar arthrosis secondary to malalignment

Results of anteromedialization Pidoriano Am J Sports Med 1997 n n Depend on the locations and severity of articular disease Best results - Distal, central zone and lateral facet lesions (Type I & II) n n Proximal medial facet that receives loading after AMZ Poor results – Proximal crush lesions & diffuse articular change Location is far more than important than the grade severity Distal Lateral Medial proximal
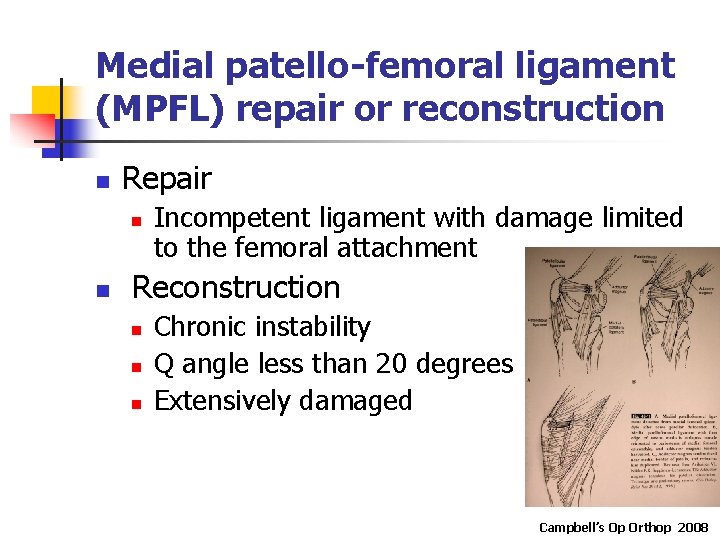
Medial patello-femoral ligament (MPFL) repair or reconstruction n Repair n n Incompetent ligament with damage limited to the femoral attachment Reconstruction n Chronic instability Q angle less than 20 degrees Extensively damaged Campbell’s Op Orthop 2008

Thanks for your attention
- Slides: 51