Classification of Chronic Hepatitis NonBiliary 1 Viral HBV

Classification of Chronic Hepatitis • Non-Biliary 1 - Viral: HBV, HCV, HBV+HDV 2 - Non-Viral: AIH, , NASH, Wilson, s Hemochromatosis…… • Biliary 1 -PBC 2 -PSC 3 -AIC (Overlap Syndrome)
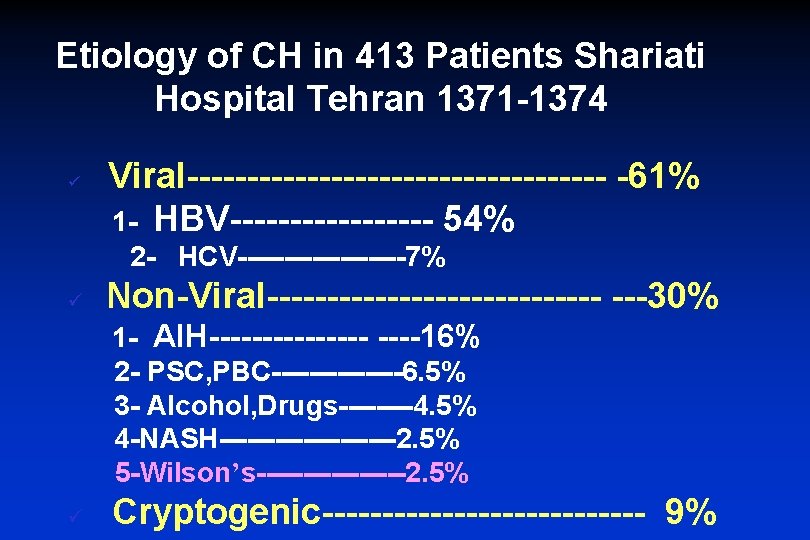
Etiology of CH in 413 Patients Shariati Hospital Tehran 1371 -1374 ü Viral------------------ -61% 1 - HBV--------- 54% 2 - HCV---------7% ü Non-Viral-------------- ---30% 1 - AIH--------16% 2 - PSC, PBC-------6. 5% 3 - Alcohol, Drugs----4. 5% 4 -NASH----------2. 5% 5 -Wilson’s--------2. 5% ü Cryptogenic-------------- 9%
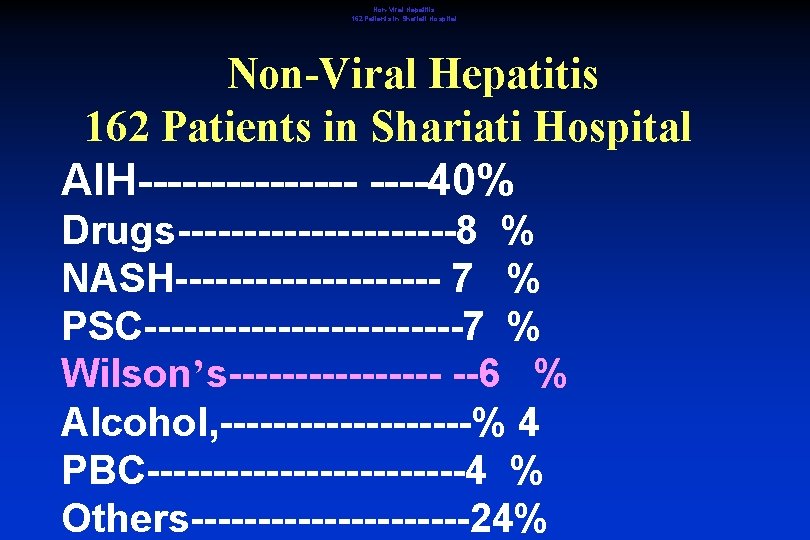
Non-Viral Hepatitis 162 Patients in Shariati Hospital AIH--------40% Drugs-----------8 % NASH---------- 7 % PSC------------7 % Wilson’s-------- --6 % Alcohol, ----------% 4 PBC------------4 % Others-----------24%

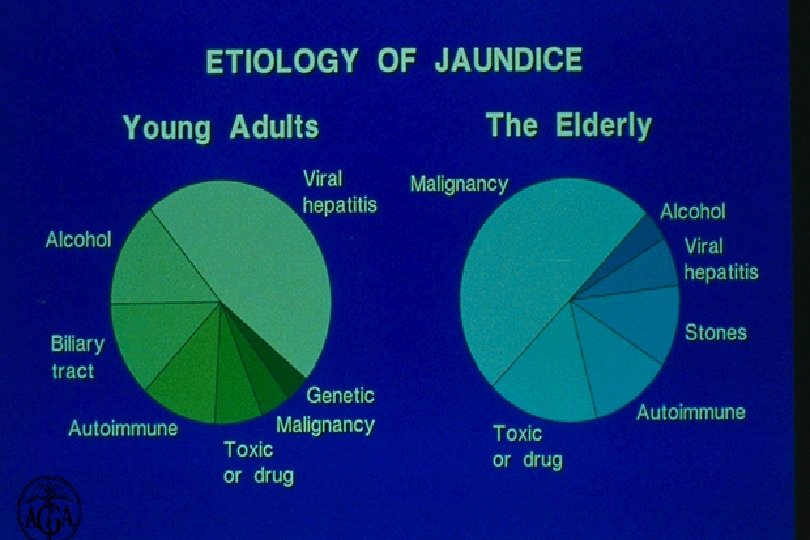
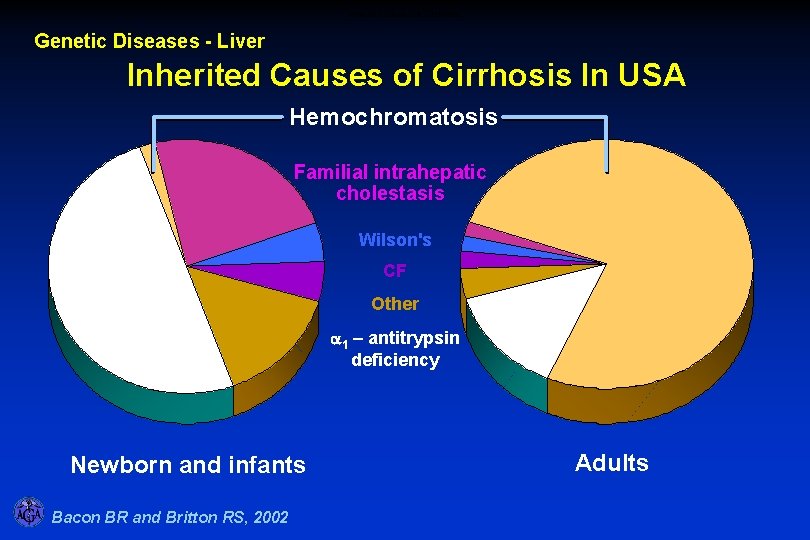
Inherited Causes of Cirrhosis Genetic Diseases - Liver Inherited Causes of Cirrhosis In USA Hemochromatosis Familial intrahepatic cholestasis Wilson's CF Other a 1 – antitrypsin deficiency Newborn and infants Bacon BR and Britton RS, 2002 Adults
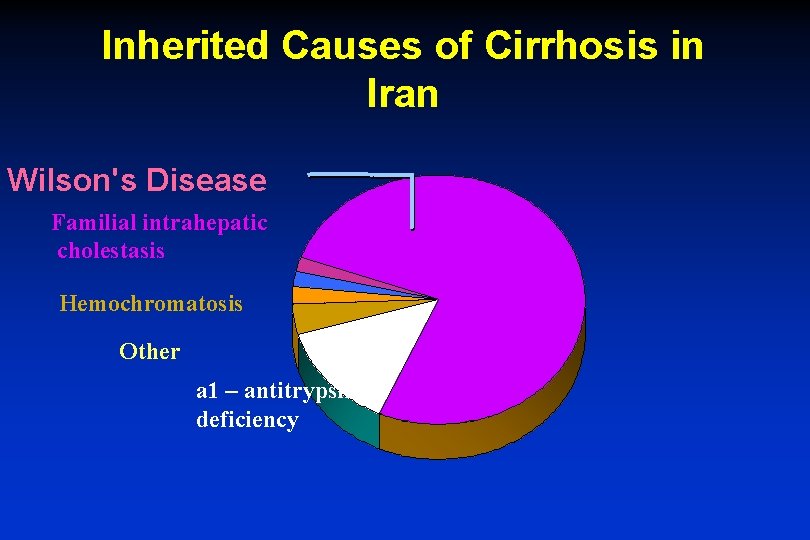
Inherited Causes of Cirrhosis in Iran Wilson's Disease Familial intrahepatic cholestasis Hemochromatosis Other a 1 – antitrypsin deficiency

Wilson’s Disease In Iran
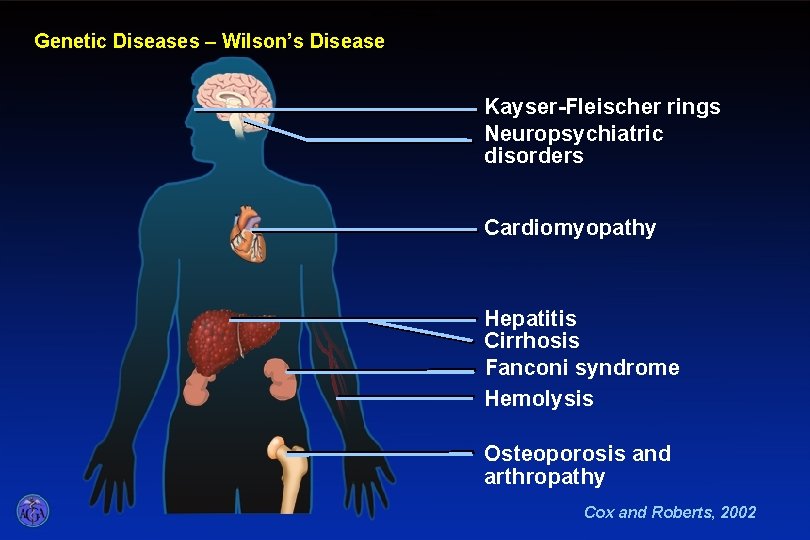
Wilson’s Disease Genetic Diseases – Wilson’s Disease Kayser-Fleischer rings Neuropsychiatric disorders Cardiomyopathy Hepatitis Cirrhosis Fanconi syndrome Hemolysis Osteoporosis and arthropathy Cox and Roberts, 2002

Normal Copper Balance • 0. 6 to 3 mg/day Cu intake (2/3 absorbed in the upper SB) Alb. Binding take up by dif tissues • Cu + apo. CLP (in the liver) CLP (90% of the circulating Cu) • Excretion via bile: 85 -95% of the total daily intake, the rest by the liver
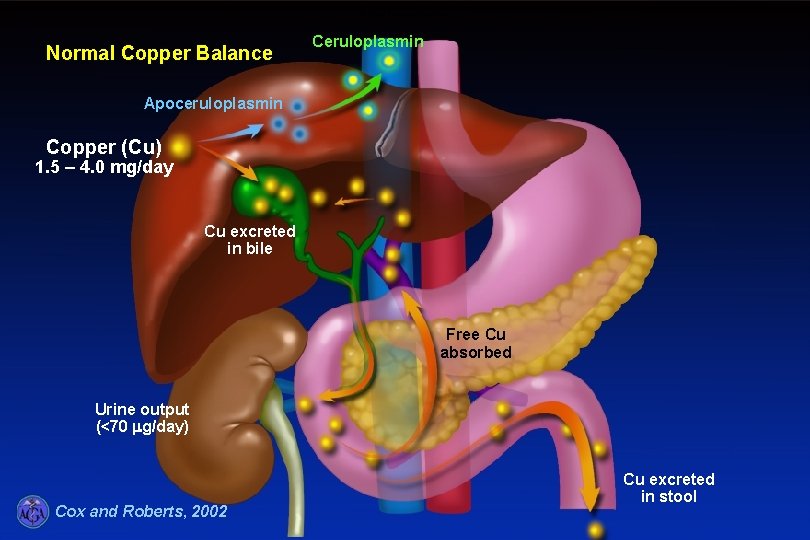
Normal Copper Balance Ceruloplasmin Apoceruloplasmin Copper (Cu) 1. 5 – 4. 0 mg/day Cu excreted in bile Free Cu absorbed Urine output (<70 mg/day) Cox and Roberts, 2002 Cu excreted in stool
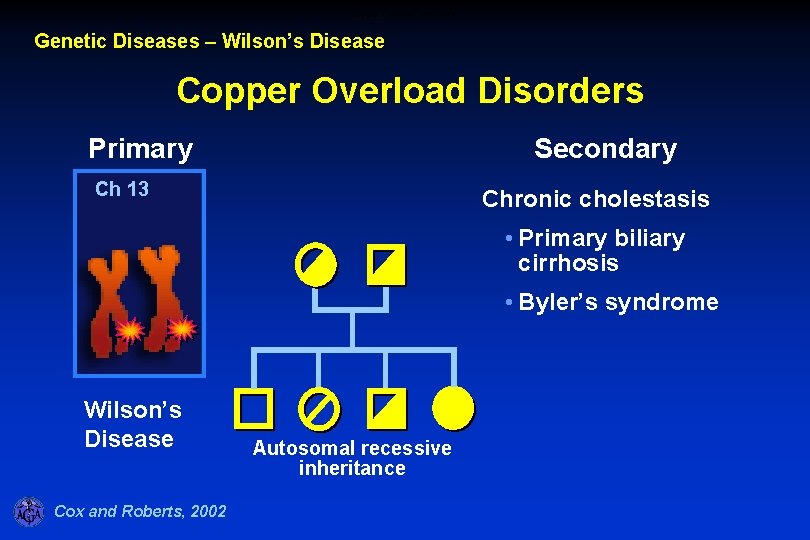
Copper Overload Disorders Genetic Diseases – Wilson’s Disease Copper Overload Disorders Primary Secondary Ch 13 Chronic cholestasis • Primary biliary cirrhosis • Byler’s syndrome Wilson’s Disease Cox and Roberts, 2002 Autosomal recessive inheritance

Increased serum ceruloplasmin is seen in: • Pregnancy or estrogen therapy. • The stress of acute inflammation, such as hepatitis. • Thus, 5% of patients with Wilson's disease have a ceruloplasmin level in the normal range.

A low serum CLP: not specific for WD, also in • • • Heterozygous carriers Acute viral hepatitis Chronic hepatitis Drug-induced liver disease Alcohol-induced liver disease Malabsorption

Wilson’s Disease Gene • Located in Chromosome 13 • ATP 7 B
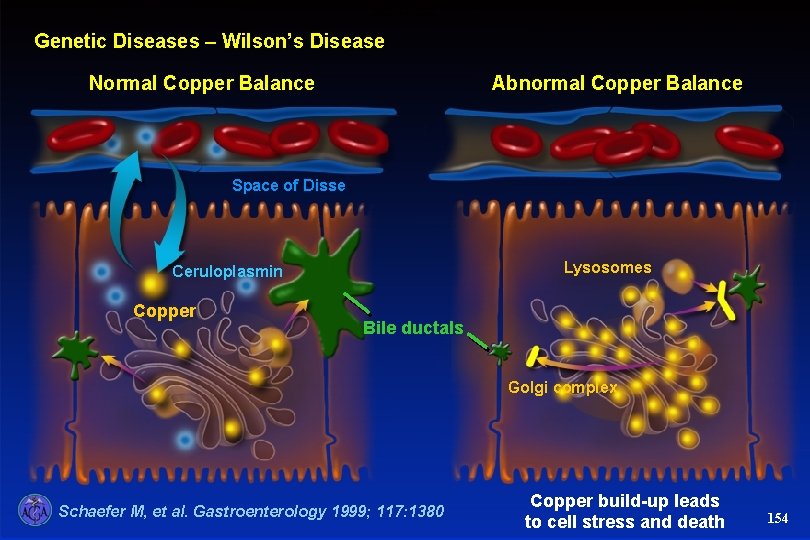
Wilson’s Disease Genetic Diseases – Wilson’s Disease Normal Copper Balance Abnormal Copper Balance Space of Disse Lysosomes Ceruloplasmin Copper Bile ductals Golgi complex Schaefer M, et al. Gastroenterology 1999; 117: 1380 Copper build-up leads to cell stress and death 154

Progressive Cu accumulation • Increase in hepatic Cu • Excess copper: initially bound to metallothionein and distributed evenly in the cytoplasm • Progressive Cu accumulation exceeding the capacity of metallothionein • Cu deposition in lysosomes hepatic dysfunction (? free radicals) • Severe mitochondrial dysfunction in these patients is a sign of oxidative damage

Clinical manifestations • Rare before age 6 and almost always before the age of 30 (later ages also reported) • Adolescents: liver disease • Young adults: neuropsychiatric disease • All patients with neuropsychiatric disease have compensated cirrhosis (often not detected until Wilson's disease is diagnosed)
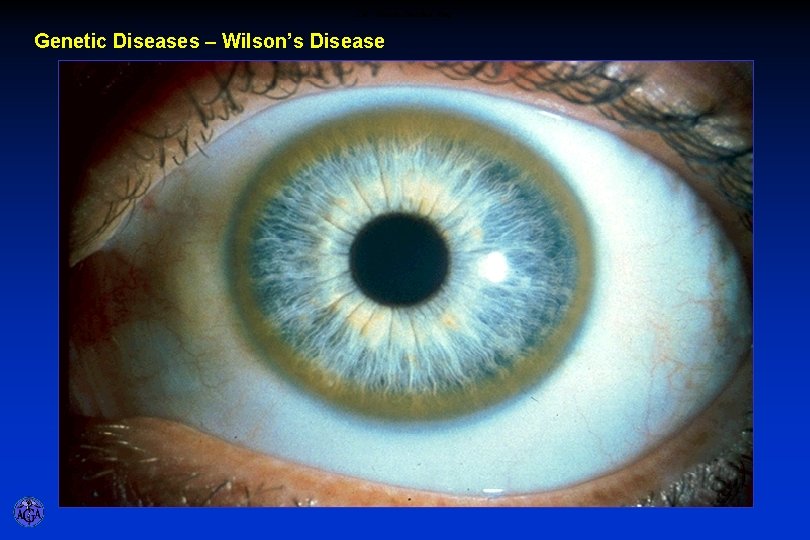
CM - Kayser-Fleischer Ring Genetic Diseases – Wilson’s Disease
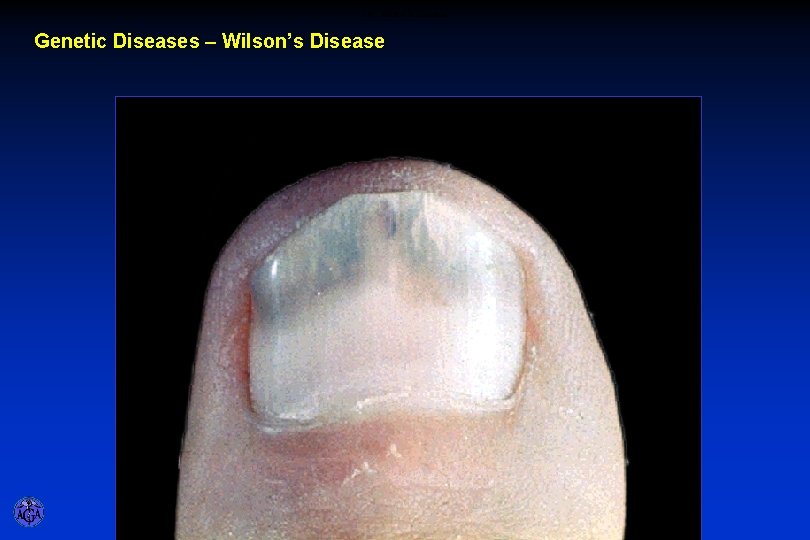
CM - Wilson’s Disease Genetic Diseases – Wilson’s Disease
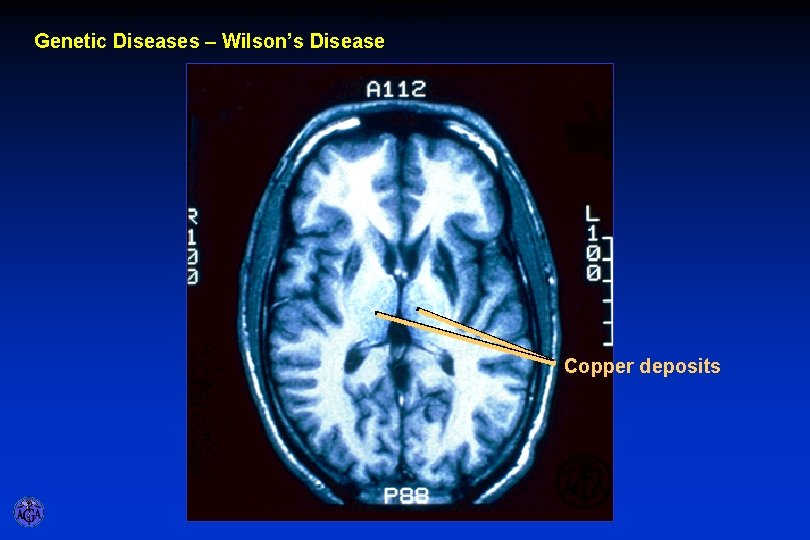
CM - MRI of the Brain Genetic Diseases – Wilson’s Disease Copper deposits

Diagnosis • Serum ceruloplasmin levels are usually, but not invariably, low, below 20 mg/dl, in homozygotes

Features in Homozygotes and Heterozygotes Genetic Diseases – Wilson’s Disease Usual Features in Homozygotes Usual Features in Heterozygotes Ceruloplasmin <20 mg/dl Rarely Urine copper >100 mg/day Rarely Kayser-Fleischer rings Never Hepatic histology abnormal Never Hepatic copper >250 mg/g Rarely Cox DW, Roberts EA. In Sleisenger & Fordtran’s Gastrointestinal and Liver Disease; Pathophysiology, Diagnosis and Management. Edited by M. Fledman, et al. Saunders, Philadelphia 2002; 67: 1269 -1277
Indications for Testing Genetic Diseases – Wilson’s Disease Indications for Testing · Liver disease in children, adolescents, young adults · Hemolysis with liver disease · Neurologic disease in the young · Parkinsonian tremor · Gait disturbance · Psychosis or other mental disorders · Fanconi syndrome · Hypouricemia · Kayser-Fleischer rings · Sunflower cataracts · Siblings of affected patients Cox DW, Roberts EA. In Sleisenger & Fordtran’s Gastrointestinal and Liver Disease; Pathophysiology, Diagnosis and Management. Edited by M. Fledman, et al. Saunders, Philadelphia 2002; 67: 1269 -1277
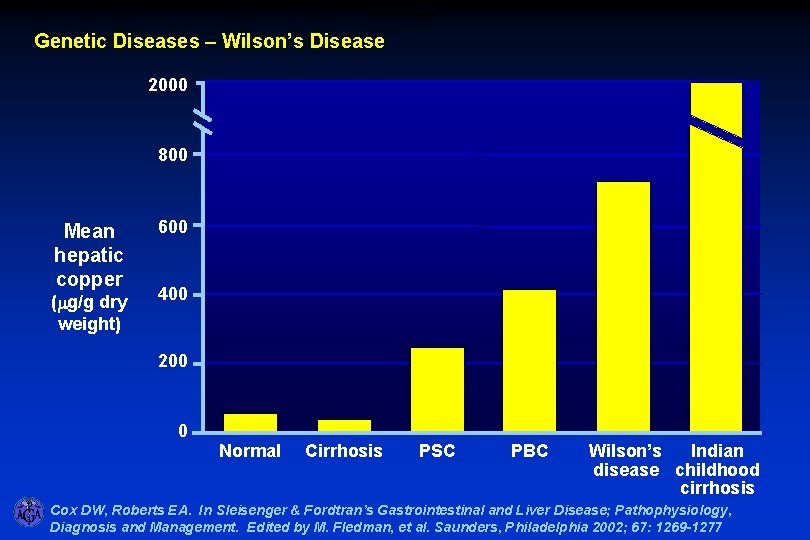
Wilson’s Disease Genetic Diseases – Wilson’s Disease 2000 800 Mean hepatic copper (mg/g dry weight) 600 400 200 0 Normal Cirrhosis PSC PBC Wilson’s Indian disease childhood cirrhosis Cox DW, Roberts EA. In Sleisenger & Fordtran’s Gastrointestinal and Liver Disease; Pathophysiology, Diagnosis and Management. Edited by M. Fledman, et al. Saunders, Philadelphia 2002; 67: 1269 -1277

Presentations Genetic Diseases – Wilson’s Disease Presentations Liver Abnormal liver tests Acute hepatitis Acute hepatic failure Liver disease with hemolysis Chronic hepatitis Cryptogenic cirrhosis CNS Parkinson-like disorders Psychiatric disorders Eye Kayser-Fleischer rings Sunflower cataracts Kidney Fanconi syndrome with hypouricemia Cox DW, Roberts EA. In Sleisenger & Fordtran’s Gastrointestinal and Liver Disease; Pathophysiology, Diagnosis and Management. Edited by M. Fledman, et al. Saunders, Philadelphia 2002; 67: 1269 -1277
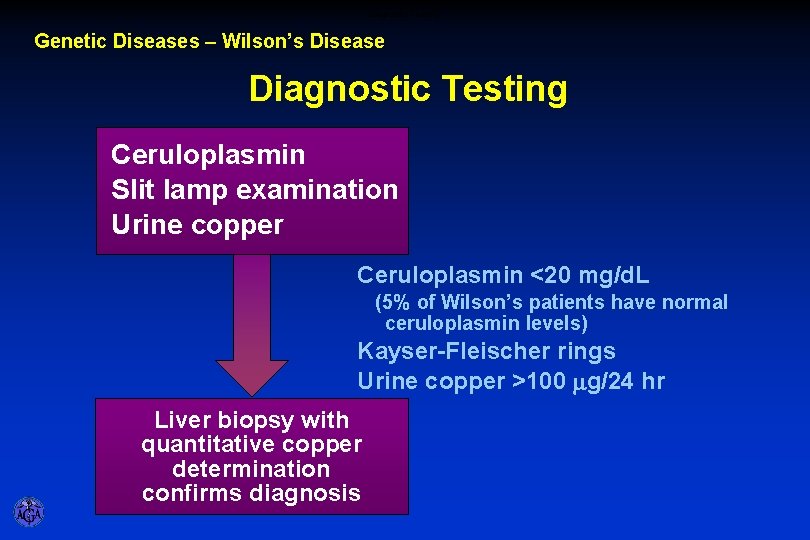
Diagnostic Testing Genetic Diseases – Wilson’s Disease Diagnostic Testing Ceruloplasmin Slit lamp examination Urine copper Ceruloplasmin <20 mg/d. L (5% of Wilson’s patients have normal ceruloplasmin levels) Kayser-Fleischer rings Urine copper >100 mg/24 hr Liver biopsy with quantitative copper determination confirms diagnosis

Copper Chelation • D-Penecillamine 500 mg QID • Trientine • Tetrathiomolybdate (neurologic cases) • Zinc acetate or Zinc Sulphate

Management Genetic Diseases – Wilson’s Disease Management Therapy Chelation + pyridoxine Zinc Avoid high copper foods Transplantation in selected cases Family screening Monitoring Urine copper Non-ceruloplasmin copper Do NOT monitor Kayser-Fleischer rings Results Treatment prevents disease Improves liver and CNS disease Prolongs life Cox DW, Roberts EA. In Sleisenger & Fordtran’s Gastrointestinal and Liver Disease; Pathophysiology, Diagnosis and Management. Edited by M. Fledman, et al. Saunders, Philadelphia 2002; 67: 1269 -1277
- Slides: 29