Classification of anemias Anemia is defined as decrease














- Slides: 15

Classification of anemias

Anemia is defined as decrease in circulating RBC count which is reflected in decrease in Hb concentration [For adult men, normal Hb level ranges from 14 -16 g /dl; while in adult women it ranges from 12 -14 g /dl]; PCV ranges (40 -47, average 45 ml/dl in adult men, & 37 -42, average 40 ml/dl in adult women). Anemia is present if Hb is less than 11 g/dl in women or less than 13 g/dl in adult men. Main types of anemia are: 1. Dyserythropoetic anemia : This is due to decreased erythropoesis in bone marrow resulting from deficiency of essential factors needed for production of normal RBC ; these are protein, iron , vitamin B 12, folic acid, ascorbic acid, and endocrine factors (erythropoetin & thyroxine ). 2. Aplastic or hypoplastic anemia : Red marrow is replaced by yellow fat. There is pathological damage to stem & progenitor cells in bone marrow leading to impaired haemopoesis.

3. Hemolytic anemia : This is due to increased rate of destruction of circulating RBC leading to decrease in their normal life span of 120 days. It could be due to factors that are either: hereditary or acquired. 4. Anemia of chronic disease : as in chronic infections e. g. TB, or chronic inflammatory disorders e. g. rheumatoid arthritis, or in chronic liver or renal disease. Treatment of anemia depends on its type & cause. Dyserythropoetic anemia is the commonest type of anemia, and needs treatment with deficient hemopoetic factors. Iron deficiency anemia is the commonest cause of anemia in this group

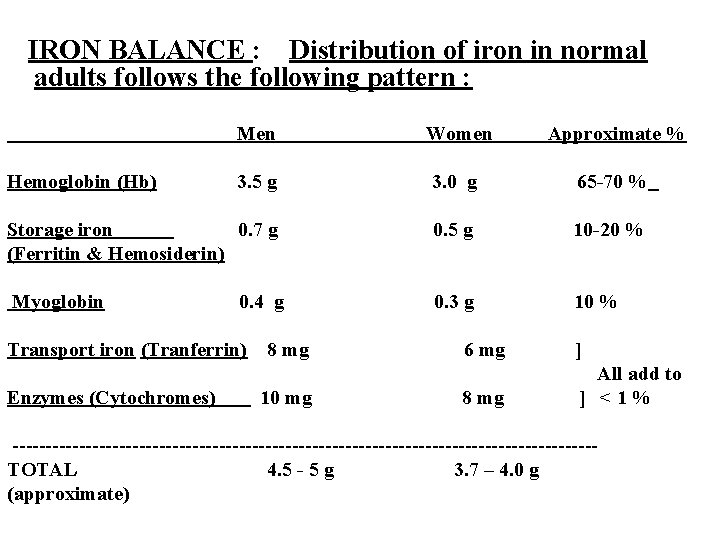
IRON BALANCE : Distribution of iron in normal adults follows the following pattern : Men Women Approximate % 3. 5 g 3. 0 g 65 -70 % Storage iron 0. 7 g (Ferritin & Hemosiderin) 0. 5 g 10 -20 % Myoglobin 0. 3 g 10 % Hemoglobin (Hb) 0. 4 g Transport iron (Tranferrin) Enzymes (Cytochromes) 8 mg 10 mg 6 mg ] 8 mg All add to ] <1% --------------------------------------------TOTAL 4. 5 - 5 g 3. 7 – 4. 0 g (approximate)

In adults, normal daily elemental iron requirement is 1 mg / d ; this comes from a diet containing 10 -15 mg iron i. e. about 10% is absorbed. In normal menstruating women, the total iron requirement and absorption increases to 1 -2 mg / d (about twice that of adult men) to compensate for the iron loss in monthly menstrual blood ( about 25 mg present in about 50 ml menstrual blood i. e. about 7 g of Hb, and each 1 g Hb thus contains about 3. 5 mg of iron ).

There is no excretory mechanism for elemental iron, but small amounts are lost by desquamation of epithelial cells from intestine, and to lesser extent, from urinary tract and skin; these cellular losses account for about 1 mg / d; hence, the normal adult requirements of about 1 mg/d. Since the body ability to increase iron excretion is very limited, then control of iron balance is mainly regulated by changing intestinal absorption of iron, depending on the body needs.

Iron need and absorption increases in response to low iron stores in body as in iron deficiency OR when body demand for iron is increased e. g. pregnancy ( as high as 3 -4 mg/d) or in growing breast-fed infants (there is only little iron in breast milk), and in young children. Source and absorption of iron Red meat is very important source of iron in diet, and iron is absorbed from it as haemin which is a ferric organic form of heme.

Iron in other foods such as green leaves or vegetables, grains, pulses(legumes), or in drugs, must be converted from ferric Fe+++ to ferrous (Fe++) form by gastric acid & ferrireductase in enterocytes before active absorption occurs via DMT in duodenum & proximal jejunum. This absorption is decreased by achlorhydria, by complexing agents in diet e. g. phytates, phosphates; or binding of iron to chelators e. g tetracyclines, aluminum in antacids; or binding to the resin cholestyramine. while it is increased by ascorbic or succinic acid.

Absorbed ferrous iron is converted to ferric iron Fe +++ by ferroxidase within mucosal cells of intestine, and this can then bind to apoferritin protein to form ferritin which is either: stored inside mucosal cell till these cells are shed off in feces OR its ferric iron is made available to plasma transferrin via ferroportin which is the major iron export protein on cell surface of enterocytes. Ferroportin is also located on surface membrane of macrophages (contain stored iron in addition to iron derived from degraded old RBCs esp. in spleen) and hepatocytes (which contain stored iron), and these are thus made capable of releasing iron into plasma for transport by transferrin to bone marrow.

Iron-transferrin complex binds to its specific transferrin receptors on surface of erythroid progenitor cells in bone marrow, & then internalized to release iron to be utilized inside these cells to form Hb for new RBCs. Transferrin, still bound to its receptor, is then recycled back to cell membrane to be released alone into plasma. Transferrin also transports iron for storage in liver &RES. Iron is stored as ferritin or hemosiderine. Stored ferritin is in balance with plasma ferritin which is thus a very sensitive indicator of status of iron stores. If stores are saturated as in hemochromatosis, excess iron is then deposited in the parenchyma of tissues like heart, liver, pancreas, and joints causing their damage.

Hepcidin is the main regulatory hormone for iron absorption; it is synthesized by liver. Hepcidin directly binds to ferroportin causing it to be internalized from cel surface and becomes degraded, thus removing its effect. Cytokine-mediated increase of hepcidin, caused by chronic inflammation or chronic infection, leads to iron being retained by enterocytes, macrophages, & hepatocytes. This might be responsible for the anaemia of chronic disease; its features are: low serum iron & low transferrin saturation, & thus anemia with increased iron stores Reduced hepcidin synthesis increases iron absorption & release into plasma; it occur in iron deficiency & in genetically in primary hemochromatosis, & in thalassemia major (though unexplained).

Iron Deficiency Anemia

Most body iron (65 -70%) is found in Hb, thus anemia is the most prominent feature of iron deficiency. Iron deficiency anemia is a microcytic hypochromic anemia ( low MCV , low MCH & MCHC ) with low serum iron, and low serum ferritin. ITS CAUSES ARE: 1. Chronic blood loss : In women, this is most commonly due to monthly menstrual loss and esp. in disorders causing menorrhagia Chronic blood loss may also occur from : GIT : e. g. hemorrhoids, peptic ulcer, NSAIDs, hookworm, and GIT cancers esp. stomach or colon (esp. caecum) OR Urinary tract : as in urinary stones, urinary schistosomiasis, and cancer of kidney or urinary bladder. 2. Increased iron demand or requirements: as in pregnancy, growing infants and young children.

3. Impaired absorption of iron due to persistent lack of gastric acid as in atrophic gastritis, gastric cancer or postgasrectomy, OR in chronic intestinal disease causing malabsorption e. g. Coeliac disease 4. Poor diet: esp. in elderly and due to declining status of nutrition esp. among the poor & middle class of society. Sequence of events in iron deficiency : At first, the iron stores are depleted, and thus plasma ferritin level is the first to decrease. This is then followed by decrease in serum iron, and subsequent decrease in % transferrin saturation and increase in the available iron binding capacity of plasma. This is followed by hypochromia of RBCs, & finally microcytosis i. e. microcytic hypochromic anemia.

Clinically, anemia is evident as pallor, headache, lassitude, weakness, easy fatigue, palpitation, and dyspnoea on exertion. In more severe cases, dimness of vision, fainting, angina, & ankle oedema may occur; in elderly, confusion can occur. Pica may occur in children. Atrophic Tissue changes can also occur and include : glossitis, atrophy of mucosa of pharynx (sometimes with esophageal web formation) causing dysphagia , atrophy of gastric mucosa (causing achlorhydria or hypochlorhydria), and nail changes causing koilonychia (spooning of nails). The combination of iron deficiency anemia with these tissue changes esp. dysphagia and koilonychia, is known as Plummer-Vinson or Kelly-Patterson syndrome.