Classification of Adrenoreceptor Antagonists n blockers n n

Classification of Adrenoreceptor Antagonists n α– blockers n n β– blockers n n Non selective Relatively selective Selective Both α and β adrenergic antagonists Adrenergics & Antiadrenergic drugs 1

α– Adrenoceptor Antagonists (α– blockers) ﻳﺆﺜﺮ ﻋﻠﻰ ﻭﺍﺣﺪﺓ ﻭﺍﺫﺍ ﺯﺩﻧﺎ ﺍﻟﺠﺮﻋﺔ ﻓﺎﻧﻪ ﻳﺆﺜﺮ ﻋﻠﻰ ﺍﻷﺨﺮﻯ Non selective Relatively selective phenoxybenzamine prazosin tamsolusin phentolamine terazosin alfuzosin tolazoline doxazosin Adrenergics & Antiadrenergic drugs 2

Non selective α– blockers (act on α 1 and α 2 receptors) n Phentolamine and Tolazoline (Reversible) n n n Induce reversible competitive blockade for α 1 – adrenoreceptors which can be overcome by increase of NE T 1/2 = 3 – 5 hours Phenoxybenzamine (Irreversible) n n It alkylates the receptors & binds by methyl covalent bond. Thus, it produces irreversible α– blockade which cannot be overcome by increase of NE t 1/2 = 14 – 48 hours Adrenergics & Antiadrenergic drugs 3

Pharmacological effects of α– blockers n I. Effects Mediated by blocking n A. Cardiovascular Effects: n 1) They block α– receptors α 1 causing VD. So, decrease TVR n The pressor effect of α– agonists So, they decrease BP (hypotension) n But they are of limited clinical use in treating hypertension because they may cause: n n n Tachycardia (Reflex Type) Cardiac arrhythmia Angina pectoris Peptic ulcer Sexual dysfunction 4

Cont…. n 2) They produce tachycardia more than the α 1 – selective blockers by n Producing reflex tachycardia. n n Increase HR by n n All α blocker (selective and non selective) block α 1 to inhibit the effect of sympathetic tone on blood vessels. This leads to VD & decrease BP (more obvious during standing ) leading to postural hypotension. This will stimulate the baroreceptors to send impulses to CNS to increase HR Block α 2 cause increase NE in synapse. NE will bind to β 1 receptor leading to ↑HR Phenoxy benzamine n Block NE reuptake. This will increase NE in synapse leading to increase HR. So, more tachycardia with Phenoxybenzamine as compared to phentolamine. Adrenergics & Antiadrenergic drugs So both drugs block α 2 leading to ↑NE but pehnoxybenzamine block reuptake of NE leading to more NE in synap 5

B. Non-cardiac Effects of α– blockers A) Miosis b) Nasal stuffness c)decrease resistance to the flow of urine d) They decrease adrenergic sweating. So they produce dry skin e) Inhibit ejaculation II. Effects mediated by non- α–adrenergic blocking effects: They induce weak blockade for: • H 1 receptors (Histamine) (Sedation; antinausea) • Serotonin receptors • Muscarinic receptors (dry mouth)

Side effects of Phenoxybenzamine n n n Fatigue Nausea (because it enters CNS) Diarrhea Postural hypotension. Tachycardia. Adrenergics & Antiadrenergic drugs 7

α– blockers Relatively selective n n n Prazosin Terazosin Doxazosin Adrenergics & Antiadrenergic drugs 8

1. Prazosin Mechanism of action n It is a relatively selective α 1 – adrenoceptor competitive antagonist Its action can be overcome by increasing agonist concentration(reversible) T 1/2 = 3 hours Adrenergics & Antiadrenergic drugs 9

Prazosin Actions: n n n It produces arterial & venous dilation. So it decreases BP, so it is used for the treatment of hypertension It causes less tachycardia than non–selective vasodilators (because it doesn’t act on α 2 receptors) It precipitates less angina & cardiac arrhythmia It may increase HDL / cholesterol ratio. HDL protects against ischemic heart disease There is tolerance to it’s action Dose 2 – 3 times daily for Hypertension and congestive heart failure (CHF). Adrenergics & Antiadrenergic drugs 10

In heart failure the following happens: 1. Decreased C. O leads to sympathetic stimulation. 2. Sympathetic stimulation ↑HR & ↑contractility (which increase the pressure on the heart thus, worsening the situation). Furthermore, NE will increase the release of renin and this leads to incerease preload and after load In this case we will use β blockers to decrease HR and contractility and inhibit renin release.

n n n Side effect of prazosin 1 st dose produce hypotension & syncope, but this disappears after continuous treatment(we prevent this effect by decreasing the 1 st dose and giving it at bedtime) Infrequent postural hypotension (rare and less than the non selective) Nasal stiffness due to VD & congestion Dizziness, headache & faintness. These are caused by hypotension Sexual dysfunction but less than the nonselective.

α– blockers Relatively selective 2. Terazosin & Doxazosin: n n n They are relatively α 1 – selective blockers, with higher selectivity than prazosin T 1/2 = Terazosin 12 hours; Doxazosin 22 hrs They produce VD with less tachycardia than prazosin Like prazosin they produce postural hypotension They produce relaxation of smooth muscle of the bladder neck and prostate capsule. So, they facilitate micturition. For this action, they can be used in case of urine retention associated with benign prostatic hyperplasia(BPH) in which prostate compresses the urethra & prevent micturition. Adrenergics & Antiadrenergic drugs 13

α– blockers Selective Tamsolusin & Alfuzosine n n n It is selective for α 1 A – adrenoreceptors in the sphincter of urinary bladder α 1 A blockade leads to relaxation of the sphincter. So, it facilitates micturition Tamsolusin is used clinically in treating urine retention associated with BPH. It is better here than prazosin, Terazosin and Doxazosin It causes less hypotension than prazosin or terazosin. Because: It has low potency in inhibiting receptors in vascular smooth muscle 14

Tamsolusin Adverse affects: Retrograde ejaculation 15% n Hypersensitivity reaction: skin rash & urticaria n Nausea and vomiting n Nasal stiffness n Over dose will cause hypotension, tachycardia and fatigue Note: Similar to prazosin but with less magnitude. n Adrenergics & Antiadrenergic drugs 15

Tamsolusin Contraindications: n Renal impairment n n Tamsolusin is metabolized in the liver to an active metablite which is entirely excreted via the renal tubules, therefore, In case of renal impairment, Tamsolusin will accumulate in blood & lead to toxicity Adrenergics & Antiadrenergic drugs 16

Clinical Uses of adrenergic aantagonists: 1) Pheochromocytoma (phenoxybenzamine, phentolamine) with β blockers to reduce cardiac effect from increased catecholamines 2) Hypretensive Crisis (Labetalol) 3) Essential Hypertension (Prazosin, Terazosin) 4) Peripheral Vascular Occlusion Diseases (Raynaud’s phenomenon) e. g: Prazosin (but Calcium Channel Blockers are better choice) 5) Urinary Obstruction associated with BPH (Tamsolusin)
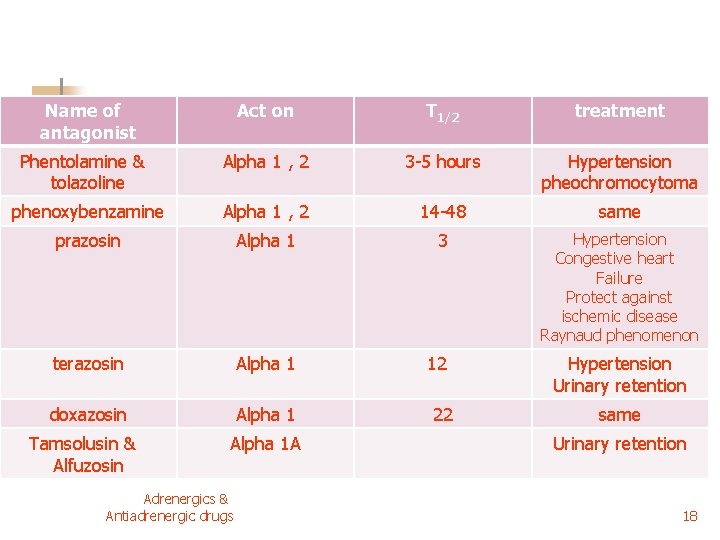
Name of antagonist Act on T 1/2 treatment Alpha 1 , 2 3 -5 hours Hypertension pheochromocytoma phenoxybenzamine Alpha 1 , 2 14 -48 same prazosin Alpha 1 3 Hypertension Congestive heart Failure Protect against ischemic disease Raynaud phenomenon terazosin Alpha 1 12 doxazosin Alpha 1 Phentolamine & tolazoline Tamsolusin & Alfuzosin Alpha 1 A Adrenergics & Antiadrenergic drugs 22 Hypertension Urinary retention same Urinary retention 18

Adrenoreceptor Antagonists β– blockers: Non selective Relatively selective Alpha and beta blockers Propranolol Atenolol Labetalol Timolol Esmolol carvedilol Nadolol Metoprolol Labetalol Practolol pindolol Acebutol bisoprolol More potent than atenolol Adrenergics & Antiadrenergic drugs 19
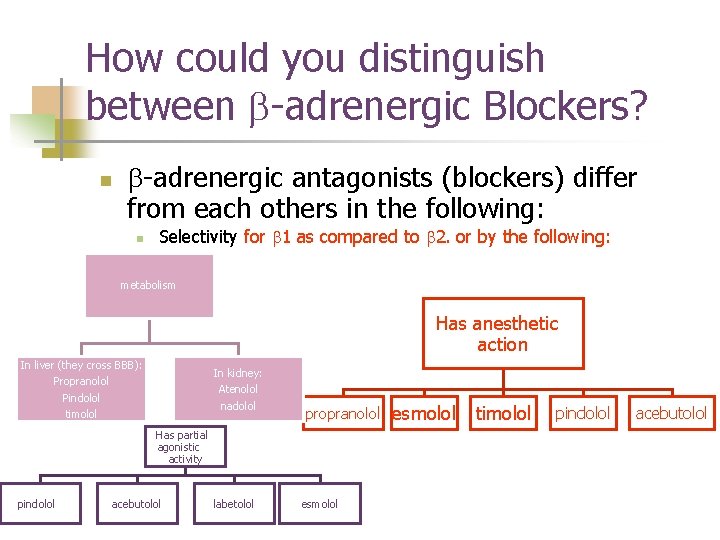
How could you distinguish between b-adrenergic Blockers? n b-adrenergic antagonists (blockers) differ from each others in the following: n Selectivity for b 1 as compared to b 2. or by the following: metabolism Has anesthetic action In liver (they cross BBB): Propranolol Pindolol timolol In kidney: Atenolol nadolol propranolol Has partial agonistic activity pindolol acebutolol labetolol esmolol timolol pindolol acebutolol

β– blockers Pharmacological actions: n CVS n Angiotensin normally induces the release of NE from postganglionic sympathetic fibers BP = CO * TVR. Clinically β blockers lower BP By these mechanisms: n n Blockade of β 1 in the heart will cause decreased HR and CO Blockade β 1 in the kidney will cause decreased rennin leading to decreased angiotensin 2. this will lead to n n NE ﺑﺎﻟﻌﺮﺑﻲ ﻳﻄﻠﻊ ﻳﻠﻘﻰ ﺍﻟﺮﻳﺴﻴﺒﺘﻮﺭ ﻣﻘﻔﻠﺔ ﻳﻀﻄﺮ ﺍﻧﻪ 2α ﻳﺮﻭﺡ ﻟـ n n n VD and ultimately decreased BP decrease aldosterone. This will lead to decerased salt and water retention and finally decreased BP decrease release of NE that will cause VD and decreased BP Blockade of central β adrenergic in adrenergic nerve terminals. This will makes NE acts at a 2 -adrenergic agonist leading to a decrease in its own release and decrease sympathetic tone to blood vessels, leading to VD and decreased BP Which one of the above mechanism is more important for treating hypertension? Decreasing renin secretion

Cont…. n The respiratory system n n n Blockade of β 2 receptors in bronchi will cause bronchoconstriction Non–selective β blocker (are contraindicated in the bronchial asthma (propranolol) The β 1 selective blockers (e. g: Atenolol; Bisoprolol) are also should be avoided in the acute bronchial asthma because their selectivity is relative and they may have antagonistic affects on the β 2 receptors at therapeutic doses. Adrenergics & Antiadrenergic drugs 22

Cont…. n The eye n β–blockers are used in treatment of glaucoma (Timolol). They act by: n n Blocking β 2 in ciliary epithelium. This will decrease production of aqueous humor ↓ intraocular pressure (IOP) Block β 2 in ciliary muscle. This will cause of contraction of the ciliary muscle leading to n Opening of the canal of Schlemm this Increases outflow of aqueous humor which leads to Decreased IOP Adrenergics & Antiadrenergic drugs 23

Cont…. n Metabolic and endocrine effects n n ü ü ü n β blocker inhibit lipolysis In type 1 diabetes The patient depends on catecholamines to increase blood glucose if he took overdose of insulin. If he took β blockers, they will impair the recovery from hypoglycemia β 1 blockers are advised in the case of diabetic patients β – blockers cause increase VLDL & triglycerides (TG) and decrease HDL / Cholesterol ratio. So, they will n n Increase risk of coronary artery disease contraindicated in a patients with familial hypercholesterolemia because VLDL & TGs are atherogenic & may cause myocardial infarction Adrenergics & Antiadrenergic drugs 24

Cont…. n Intrinsic sympathomimetic activity (ISA ) n n Some of the β antagonist produce some action of β agonist e. g. Pindolol & Labetalol…, so, they are less dangerous when given to patients with bronchial asthma or excessive bradycardia Membrane Stabilizing Action (MSA) n Some β blockers stabilize the cell membrane by blocking Na+ channels. Therefore, produce “local anesthetic action” e. g. Propranolol & Pindolol … Adrenergics & Antiadrenergic drugs 25

β– blockers Side effects of β blockers n n n Rash & fever Worsening of asthma CNS include n Sedation and Depression and sleep disturbances n n These are more sever in Lipid – soluble β blockers (e. g. Propranolol) than in water soluble β blocker (e. g. Atenolol) Heart failure Some β blockers are effective in treating chronic heart failure but not acute because you want to decrease the work load & O 2 consumption on the (see slide 11) myocardium Adrenergics & Antiadrenergic drugs 26

β– blockers Contraindications of β-blockers: n n n Bronchial asthma Peripheral vascular disease Heart failure (in severe cases only) (acute) Adrenergics & Antiadrenergic drugs 27

β– blockers Drug interactions: n n Verapamil (Ca++ ) channel blocker If it is combined with β – blockers, this can cause : n n n Congestive heart failure Severe bradycardia Severe hypotension Adrenergics & Antiadrenergic drugs 28

β– blockers Withdrawal of β blockers: On chronic use, abrupt withdrawal of β – blockers causes the β receptors to become supersensitive and even the circulating catecholamine can stimulate them & cause severe arrhythmia. So, withdrawal should be very gradual over weeks Adrenergics & Antiadrenergic drugs 29

β– blockers Propranolol n n n It is non – selective β blocker T 1/2 = 2 – 5 h It is Lipid soluble Can be given orally or I. V It undergoes extensive 1 st pass metabolism (90% of the drug) Adrenergics & Antiadrenergic drugs 30

Cont…. n n It is excreted in urine as Propranolol or as Glucouronide conjugate It’s duration of action is increased in n n n Hepatic disease Decreased hepatic BF Metabolic inhibition e. g. when giving Cimetidine, it inhibits the metabolism of propranolol, so, increase t 1/2 It has no ISA It has MSA. SO, It is used as antiarrhythmic drug but not in hypertension. n It stabilize the cardiac cell membrane & decrease the activity of ectopic foci Adrenergics & Antiadrenergic drugs 31

Side effect of propranolol Bradycardia Cold extremities Fatigue Sedation Mental depression Sleep disturbances Heart failure A – V block Bronchospasm Impotence 32

β– blockers Timolol: n n n It is a non – selective β blocker T 1/2 = 4 – 5 h No ISA Low MSA so not good for arrethmia. Lipid – soluble n Pass via the cornea. So, it is used as eye – drops to treat glaucoma Adrenergics & Antiadrenergic drugs 33

β– blockers Labetalol: n n n It is a non-selective β blocker & selective α 1 blocker T 1/2 = 4 – 6 h Weak lipid – soluble It has ISA Has MSA It differs from other β blockers in that it produce less bradycardia. n n It block α 1 in blood vessels. So, causes VD and decrease BP (postural hypotension). This will stimulate baroreceptors to send impulses to CNS to increase HR (reflex tachycardia) but this tachycardia is less than seen with other α blockers It is used in Pheochromocytoma and hypertension of pregnancy Adrenergics & Antiadrenergic drugs 34

Cont…. n Adverse effects include: n n n n n Nausea skin rash tiredness Aching limbs Bronchospasm Heart failure Sleep disturbance & nightmares Sexual dysfunction (more than other β blockers) Postural hypotension (because it is selective α 1 blocker) Raynaud syndrome (peripheral vasospasm) n n It is intermittent claudication or peripheral vascular disease It is due to decreased blood supply to the periphary by β blockers due to n n Bradycardia Block β 2 in blood vessels to skeletal muscle causing VC and decrease blood supply Adrenergics & Antiadrenergic drugs 35

β– blockers Pindolol: n n n It is a non-selective β blocker T 1/2 = 3 – 4 h Has ISA (very important) lead to bradycardia. Weak lipid soluble Has MSA but less than Propranolol Adrenergics & Antiadrenergic drugs 36

β– blockers Carvedilol : like labitolol n n It is non – selective β blocker and non – selective α blocker It can be used in patients with heart failure due to: n n It is a peripheral vasodilator (unlike other β blockers) It has antioxidant activity n n It can neutralize (scavenge) the free radicals which cause heart failure It used in renal impairment n Because it improves kidney function. So, it’s used in patients with Renal impairment Adrenergics & Antiadrenergic drugs 37

β– blockers Atenolol: n n It is a relative β 1 selective blocker Hydrophilic so it has: n Longer t 1/2= 12 – 18 h because it stays in tissue for a long time n n n For this reason, the dose is once daily Less severe side effects on CNS No ISA No MSA Adverse effects include n CNS : insomnia, headache & dizziness Impairment of glucose tolerance Bradycardia Bronchospasm Sexual dysfunction* Fatigue : due to decreased blood supply to the periphery* n *all β blockers cause sexual dysfunction and fatigue. n n n Adrenergics & Antiadrenergic drugs 38

β– blockers Practolol: n n n It is a relatively β 1 selective blocker It is used in intensive care unit for severe ventricular arrhythmia It is not used to treat hypertension because of it’s side effect Adrenergics & Antiadrenergic drugs 39

β– blockers Esmolol : n n n It is a selective β 1 blocker Has very short duration of action (t 1/2 = 8 min) Has low ISA Has MSA (good for arrhythmia ) It is given I. V when short term β blockade is required Safer to use than longer acting antagonists in critically ill patients. Adrenergics & Antiadrenergic drugs 40
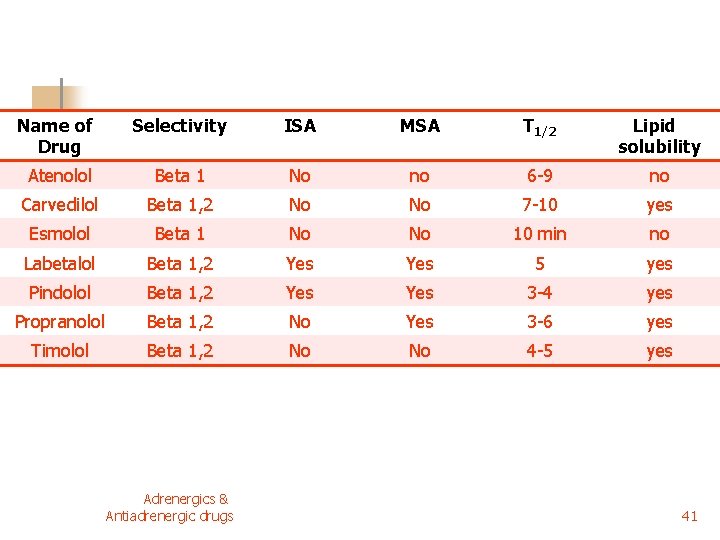
Name of Drug Selectivity ISA MSA T 1/2 Lipid solubility Atenolol Beta 1 No no 6 -9 no Carvedilol Beta 1, 2 No No 7 -10 yes Esmolol Beta 1 No No 10 min no Labetalol Beta 1, 2 Yes 5 yes Pindolol Beta 1, 2 Yes 3 -4 yes Propranolol Beta 1, 2 No Yes 3 -6 yes Timolol Beta 1, 2 No No 4 -5 yes Adrenergics & Antiadrenergic drugs 41
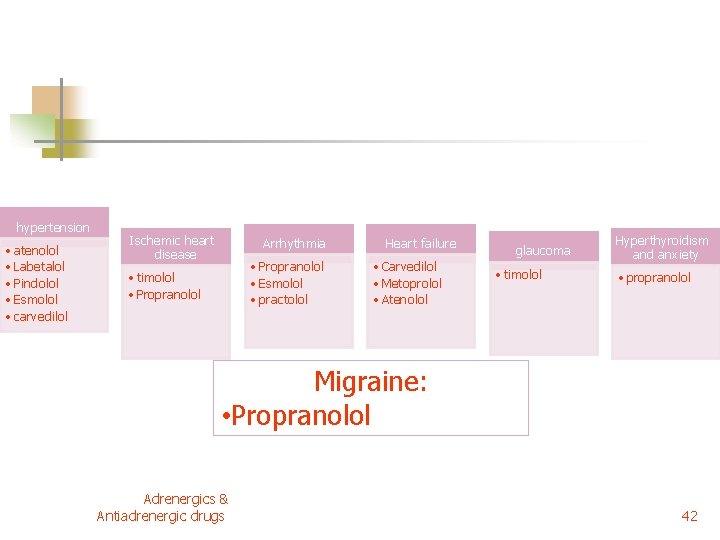
hypertension • atenolol • Labetalol • Pindolol • Esmolol • carvedilol Ischemic heart disease Arrhythmia • Propranolol • Esmolol • practolol • timolol • Propranolol Heart failure • Carvedilol • Metoprolol • Atenolol glaucoma • timolol Hyperthyroidism and anxiety • propranolol Migraine: • Propranolol Adrenergics & Antiadrenergic drugs 42

Centrally acting sympatholytic drugs Adrenergics & Antiadrenergic drugs 43

Centrally acting sympatholytic drugs n n These drugs have the opposite effect to those of the sympathomimetic drugs by acting on the CNS. Examples: n n α-methyldopa Clonidine Adrenergics & Antiadrenergic drugs 44

α– methyldopa n Mechanism of action n n α–methyldopa is given orally then absorbed from GIT & enters the circulation It freely passes BBB & reaches CNS then it is converted to α– methylenorepinephrine which acts as an agonist at central α 2 – adrenoreceptors then It will decrease the sympathetic tone to blood vessels (VD) ↓BP These α 2 – adrenoreceptors are found in the medulla & pons α– methylenorepinephrine is called “false neurotransmitter” or (reactive metabolic of α– methyldopa) Action of α– methyldopa n VD lead to decrease TVR without significant effects on CO or HR or renal blood flow Adrenergics & Antiadrenergic drugs 45

Cont…. n Clinical uses: n n n Treat pregnancy – associated hypertension Treat mild to moderate hypertension (not common used) Side effects include: n It may cause fluid retention n It may produce postural hypotension when standing from the sleeping position n n This not severe like α– blockers Sedation, insomnia, depression n n Lead to increase ECF and increase in BP slightly This negates it’s therapeutic use in the beginning of treatment & disappears after continuous use Serious extrapyramidal signs n n It interferes with neurotransmitter of extra pyramidal tract May lead to muscle incoordination Adrenergics & Antiadrenergic drugs 46

Cont…. n Lactation n n n Even in male : the breast may produce milk Hepatitis & drug fever (can be serious) Impotence A lupus – like reaction : skin rash and pustules Hemolytic anemia Leukopenia : sometimes Adrenergics & Antiadrenergic drugs 47
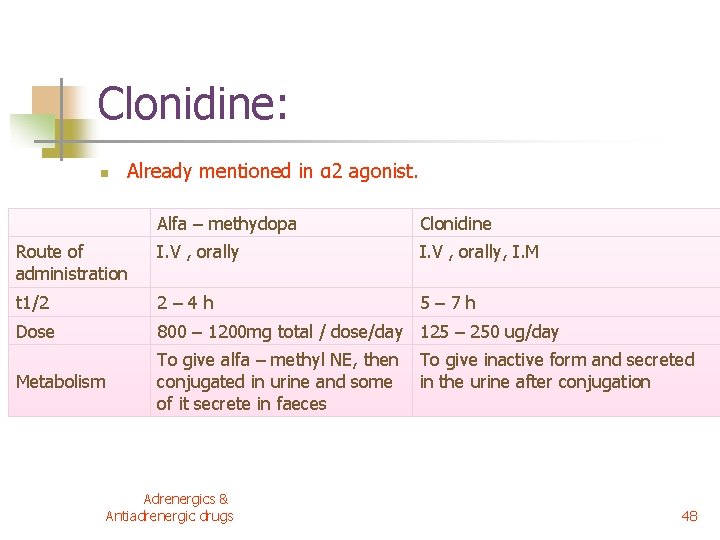
Clonidine: n Already mentioned in α 2 agonist. Alfa – methydopa Clonidine Route of administration I. V , orally, I. M t 1/2 2– 4 h 5– 7 h Dose 800 – 1200 mg total / dose/day 125 – 250 ug/day Metabolism To give alfa – methyl NE, then conjugated in urine and some of it secrete in faeces Adrenergics & Antiadrenergic drugs To give inactive form and secreted in the urine after conjugation 48

Adrenergics & Antiadrenergic drugs 49

: ﻗﻮﺍﻋﺪ ﺟﻮﻫﺮﻳﺔ • All adrenergic blockers reduce BP But : α blockers produce postural hypotension • Any α 2 agonist is considered an antagonist because it inhibits the release of NE. • Relatively selective, means in high dose it may act on other receptors. (α 1 blocker may act on α 2 in high doses).
- Slides: 50