CLABSI Prevention Bundle Skills Validation Team STEPPS Infusion

CLABSI Prevention Bundle Skills Validation Team. STEPPS Infusion Unit Audit Form Policy Review
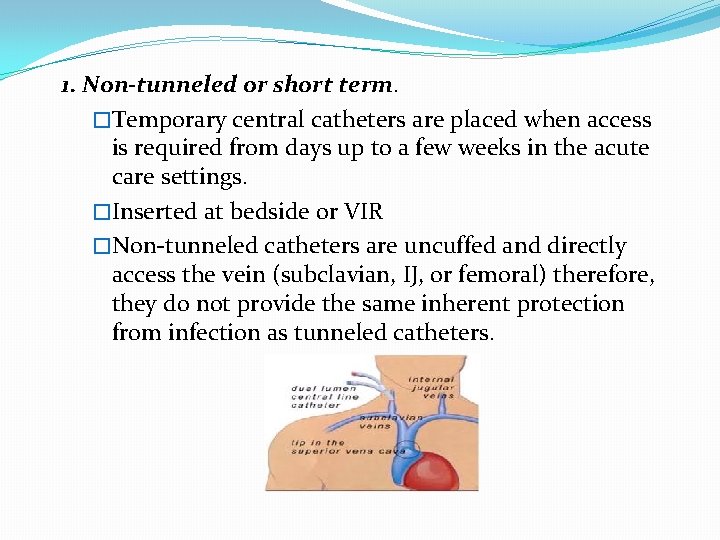
1. Non-tunneled or short term. �Temporary central catheters are placed when access is required from days up to a few weeks in the acute care settings. �Inserted at bedside or VIR �Non-tunneled catheters are uncuffed and directly access the vein (subclavian, IJ, or femoral) therefore, they do not provide the same inherent protection from infection as tunneled catheters.

2. Port, tunneled 3. PICC Line

Central Line Dressing Change �CVAD dressings are to be changed: �Immediately for a wet, soiled or loose dressing. � Team. STEPPS – Person identifying need for immediate dressing change, call for a huddle to determine who can change the dressing and any mutual support needed to cover current unit patient care needs. �At least every seven (7) days for transparent dressings � Team. STEPPS - During AM rounds – demonstrate leadership - leader asks or team members speak up and confirm shared mental model that dressing is intact and day X of 7 for planned dressing change. �Within 24 hours of admission for patients admitted with existing catheters � Team. STEPPS - During first briefing after patient arrival – leader asks, or team members speak up and confirm shared mental model about dressing condition and when dressing change will occur.

Central Line Dressing Change 1. Gather Equipment �Central line dressing kit, with Biopatch™ �If IJ being accessed, Sorbaview dressing �Disposable mask(s) �Sterile gloves �Clean gloves �Team. STEPPS – Ask for mutual support by letting team member know that you will be unavailable to others while doing the dressing change.

Central Line Dressing Change 2. Put on clean gloves- dark blue 3. Put on mask, mask patient if necessary. 4. Remove dressing in direction of line insertion. 5. Discard gloves- dark blue Team. STEPPS – Invite the patient to be involved by explaining the infection prevention steps and importance of alerting nurses and doctors if dressing is ever wet, soiled or loose
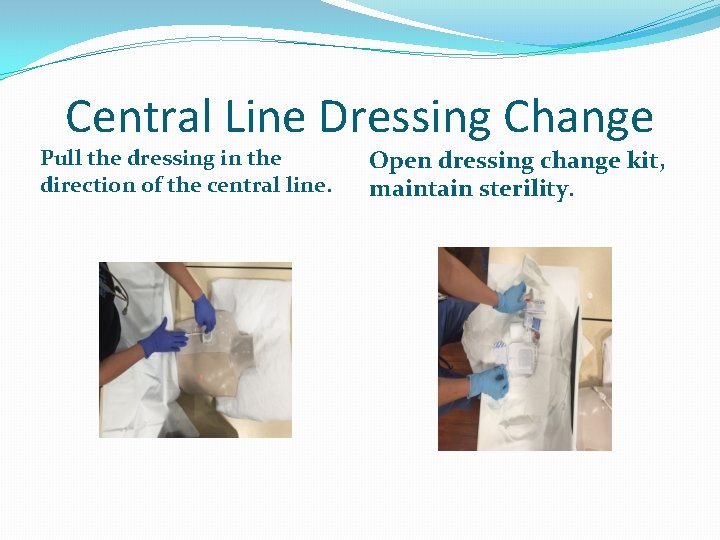
Central Line Dressing Change Pull the dressing in the direction of the central line. Open dressing change kit, maintain sterility.

Central Line Dressing Change 6. Observe the site for redness, swelling or discharge 7. Perform hand hygiene. 8. Open sterile dressing change kit. 9. Put on sterile gloves. Team. STEPPS – if you ever observe a deviation from these exact steps, offer mutual support by calling out the deviation and offering to get additional supplies and assist.

Central Line Dressing Change 10. Cleanse with CHG for 30 seconds using back and forth motion, cleanse skin and catheter covered by dressing.

Central Line Dressing Change 11. Allow CHG to dry for 30 sec-2 min. 12. Apply Biopatch. Print side up. Align slit with line and turn at least 5 degrees off center. ***There are different sizes of Biopatch…use appropriate size for the catheter (central line vs Vas Cath)***

Central Line Dressing Change 13. Apply dressing with initials, date and time of dressing change. 14. Remove gloves, perform hand hygiene. 15. Record dressing change in EPIC. Team. STEPPS – if you ever observe a deviation from these exact steps, offer mutual support by calling out the deviation and offering to get additional supplies and assist.
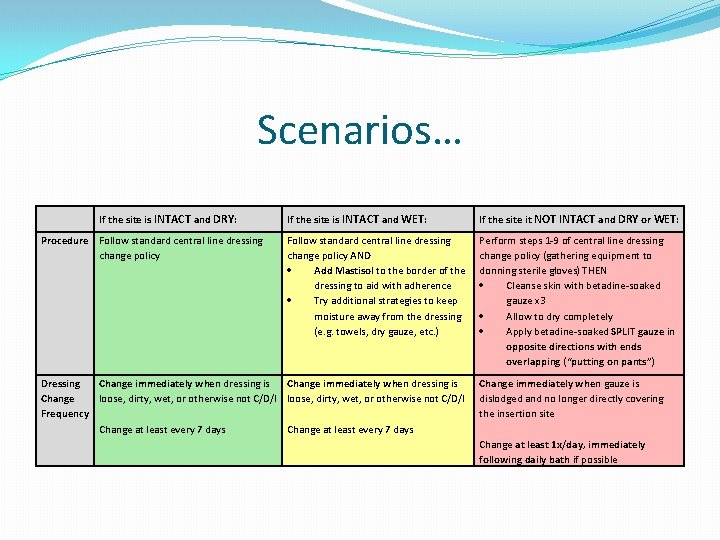
Scenarios… If the site is INTACT and DRY: If the site is INTACT and WET: If the site it NOT INTACT and DRY or WET: Procedure Follow standard central line dressing change policy AND Add Mastisol to the border of the dressing to aid with adherence Try additional strategies to keep moisture away from the dressing (e. g. towels, dry gauze, etc. ) Perform steps 1 -9 of central line dressing change policy (gathering equipment to donning sterile gloves) THEN Cleanse skin with betadine-soaked gauze x 3 Allow to dry completely Apply betadine-soaked SPLIT gauze in opposite directions with ends overlapping (“putting on pants”) Dressing Change immediately when dressing is Change loose, dirty, wet, or otherwise not C/D/I Frequency Change at least every 7 days Change immediately when dressing is loose, dirty, wet, or otherwise not C/D/I Change at least every 7 days Change immediately when gauze is dislodged and no longer directly covering the insertion site Change at least 1 x/day, immediately following daily bath if possible

IV Tubing and needleless access connector should be changed: �Every 96 hours �Every 12 hours for Propofol �Every 24 hours for all unit mixed IV fluids �Label ALL tubing with a label or when to be changed including initials, date hung, date to be changed

The Eyes of the NA/therapies �Please ensure central lines are covered completely for bathing. If they get wet, then notify RN immediately to change dressing. �When working with patients’, glance at dressing and ensure it is clean, dry and intact. Tape pulling up or soiled and damaged dressings should be reported to RN immediately. � Team. STEPPS – During change of shift briefing, discuss important role of the NA for observing dressings. �Watch those IV lines when ambulating/OOB. We want to avoid lines dragging on the floor at all cost. � Team. STEPPS – Use situation monitoring to look for the potential for lines to drag on the floor and provide mutual support to prevent.

What can we do to reduce the risk of infection… � Always wash hands or use hand sanitizer prior to accessing the line � Scrub the hub for 15 seconds (song) prior to accessing the central line via lab draws, IV push, or IV piggy back � Cap the lines with white leur caps (found in the bedside cart) � NEVER medlock with looping the line and connecting to the same line. � Team. STEPPS – incorporate leadership, communication, situation monitoring and mutual support skill and strategies to emphasize a team approach for infection prevention.

Seconds Count!

Lab Draws 101 Wash hands and put on gloves 1. 2. Place infusion on hold, cap line with white leur cap 3. Scrub hub for 15 seconds (song) 4. Connect 10 cc NS syringe and flush forward, withdraw waste (10 cc of blood) using slow steady pressure 5. Connect vacutainer, draw blood, remove vacutainer 6. Scrub hub for 15 seconds (song) 7. Flush with 10 cc NS flush 8. Reconnect line to infuse Team. STEPPS – if you ever observe a deviation from these exact steps, offer mutual support by calling out the deviation and offering to get additional supplies and assist.

Blood Cultures 101 �Always obtain using aseptic technique to prevent contamination �Obtain at least 2 blood culture sets from 2 different sites �Prep the top of the tube from a rare pathogen culture with povidone iodine �Stop all infusions to all ports of catheter being accessed for draw unless contraindicated. �Change claves before drawing blood cultures.

�Label bottle properly � Mark patient identification label with an L to indicate the culture is being collected from a central line. Identify the color of the lumen as appropriate. �Fill the bottles with the proper volume (8 -10 mls) �Once blood has been obtained from central line, inject bottles in the following order: o BACTEC Aerobic bottle o BACTEC Lytic Anaerobic bottle �Document time blood culture was obtained

Daily Assessment for Catheter NEED �Central catheters should be removed when no longer indicated �Utilize new communication tool during rounds to determine if CVAD can be removed �Assess whether the patient has adequate PIV access and convert CL to PIV when appropriate �Removing central catheters that is no longer needed eliminates significant risk of infection for your patient Team. STEPPS - During rounds – demonstrate leadership - leader asks or team members speak up and confirm shared mental model regarding removing the central catheter, adequate PIV or converting CL to PIV.
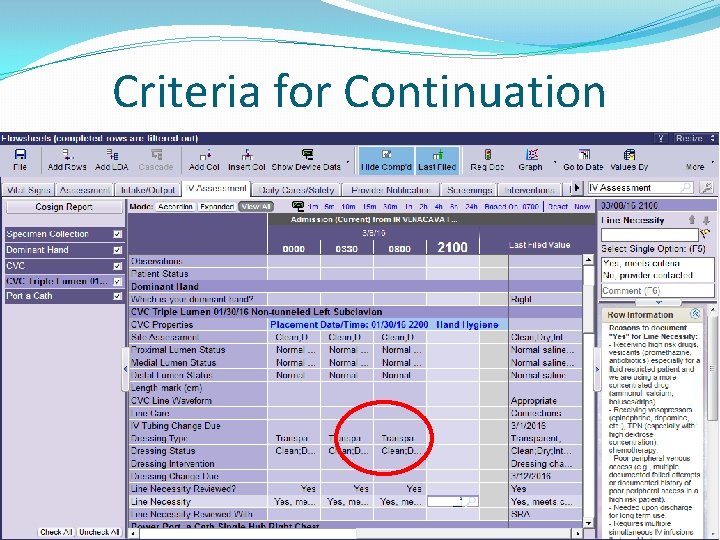
Criteria for Continuation
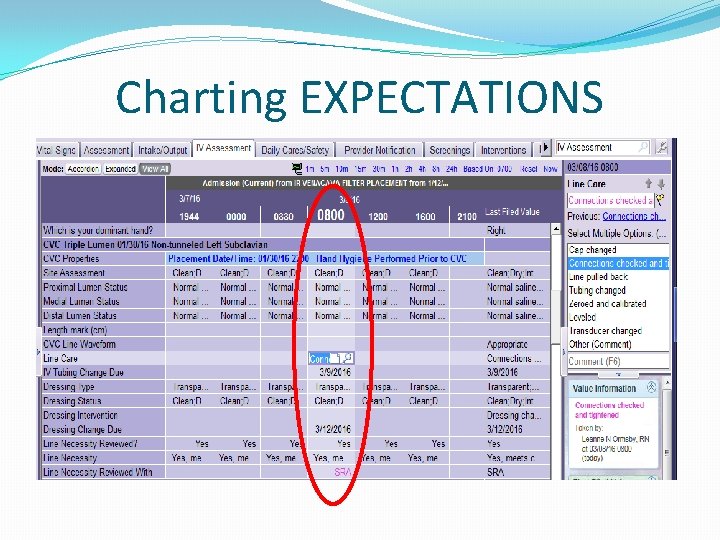
Charting EXPECTATIONS
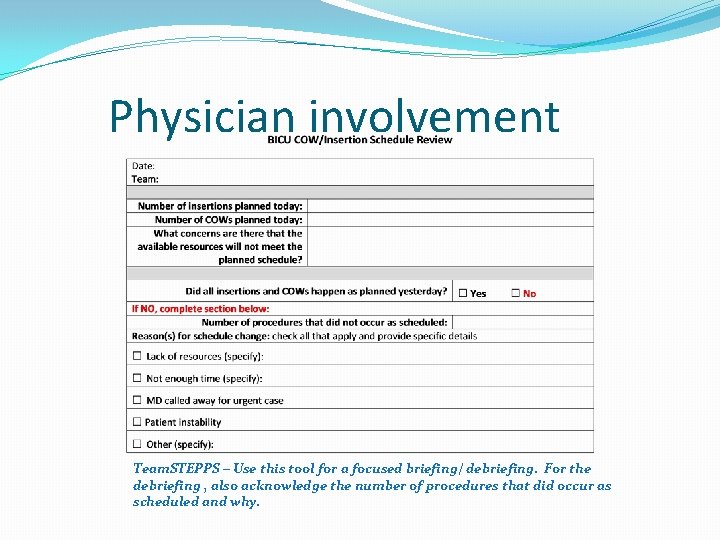

Physician involvement Team. STEPPS – Use this tool for a focused briefing/ debriefing. For the debriefing , also acknowledge the number of procedures that did occur as scheduled and why.

Central Line Process Measure Audit Tool Completed by Unit Leadership team �https: //survey. unch. unc. edu/Take. Survey. aspx? Survey ID=783 L 5861

BICU Skills Validation Team. STEPPS – Discuss with your validator what Team. STEPPS skills contribute to emphasize a team approach for infection prevention.

When CLABSI occurs �Team. STEPPS – As soon as possible after learning of a CLABSI, the formal or situational leader calls for a team debrief �Debriefs can also occur as part of routine team activities, AM rounds, or CAPP rounds �What did we do well? �What should we have done differently? �What will we do differently the next time?
- Slides: 26