Chronic PostSurgical Abdominal Pain Treated With Percutaneous Peripheral
Chronic Post-Surgical Abdominal Pain Treated With Percutaneous Peripheral Nerve Stimulation of Iliohypogastric and Ilioinguinal Nerves Harnek Singh Bajaj, M. D. 1, Denise Lester, M. D. 1, 2, 3 1 VCU Department of PM&R 2 Hunter Holmes Mc. Guire VAMC, Department of PM&R 3 Hunter Holmes Mc. Guire VAMC, Department of Interventional Pain Introduction Intraoperative Image The procedure resulted in no complications. After the first week of stimulation, patient had complete resolution of pain, with a score of 0 out of 10. At the patient’s 60 day follow up, the pain score remained 0 out of 10, and the leads were successfully removed. Chronic pelvic and lower abdominal pain can be a severely debilitating condition that affects between 7% to 24% of the general population (4). The anterior rami of L 1 and T 12 give contributions to the ilioinguinal and iliohypogastric nerves which provide sensory innervation to the lower abdomen and pubic regions (3). Entrapment or damage of these nerves can occur due to a variety of mechanisms, usually including lower abdominal surgeries, blunt trauma, mesh placement, and restrictive clothing (3). Common treatment options have included medications (2), nerve blocks (1), and in rare cases, surgical resection of the involved nerve (1), although these modalities generally provide transient relief. Here, we report a case of post-surgical iliohypogastric/ilioinguinal neuralgia successfully treated with percutaneous peripheral nerve stimulation. Case Description Pain relief remains several months later. Discussion and Conclusion In plane ultrasound view of needle tip prior to advancement into fascial plane in vicinity of ilioinguinal and iliohypogastric nerve for percutaneous implantation of PNS leads. Green (Abdominal Muscle Layers): External Oblique, Internal Oblique, Transverse abdominis) Blue (Nerves): Iliohypogastric Nerve, Ilioinguinal Nerve Red (Bony Landmark)): Anterior Superior Iliac Spine Purple: Needle Tip prior to advancement over nerves A 47 year old morbidly obese female presented to the pain clinic with chronic left sided lower abdominal and flank pain about 7 months after undergoing Roux-en-Y gastric bypass surgery. The pain was described as a 6 out of 10, and was constant and stabbing. Movement exacerbated the pain. Examination revealed tenderness to palpation at the left lower quadrant, with no guarding, or signs of peritonitis. A CT abdomen and pelvis showed post-operative changes related to the surgical procedure, but no other abnormalities. Results Methods Previously attempted treatments included neuropathic pain medications, as well as two iliohypogastric nerve blocks (anesthetic, followed by steroid) which elicited significant, but transient, pain reduction, and were both diagnostic and therapeutic. The patient subsequently underwent percutaneous peripheral nerve stimulation lead implantation remote from the iliohypogastric and ilioinguinal nerves to provide coverage of the painful region. The leads are intended to be implanted for up to 60 days of PNS before removal. Chronic pelvic and abdominal pain can be challenging conditions to treat. When first line options of treatment have been exhausted, it can be helpful to try additional options. In this case, peripheral nerve stimulation was used after positive results were elicited from iliohypogastric nerve block. This resulted in complete resolution of the patient’s chronic abdominal pain, and may potentially induce more effective pain relief than conventional methods. For this reason, we believe peripheral nerve stimulation should be considered as a modality for relief of iliohypogastric/ilioinguinal neuralgia and to address central sensitization as seen in chronic pain References 1. Acar, F. , Ozdemir, M. , Bayrakli, F. , Cirak, B. , Coskun, E. , & Burchiel, K. (2013). Management of medically intractable genitofemoral and ilioingunal neuralgia. Turkish Neurosurgery. doi: 10. 5137/1019 -5149. jtn. 7754 -12. 0 2. Benito-León, J. , Picardo, A. , Garrido, A. , & Cuberes, R. (2001). Gabapentin therapy for genitofemoral and ilioinguinal neuralgia. Journal of Neurology, 248(10), 907– 908. doi: 10. 1007/s 004150170080 3. Elkins, N. , Hunt, J. , & Scott, K. M. (2017). Neurogenic Pelvic Pain. Physical Medicine and Rehabilitation Clinics of North America, 28(3), 551– 569. doi: 10. 1016/j. pmr. 2017. 03. 007 4. Possover, M. , & Forman, A. (2012). Voiding Dysfunction Associated with Pudendal Nerve Entrapment. Current Bladder Dysfunction Reports, 7(4), 281– 285. doi: 10. 1007/s 11884012 -0156 -5

Introduction/Background • Chronic pelvic and lower abdominal pain 7% to 24% of the general population 4. • Sensory innervation via ilioinguinal and iliohypogastric nerves (anterior rami of L 1 and T 12 )3. • Entrapment or damage of can occur due to: – Lower abdominal surgeries, blunt trauma, mesh placement, and restrictive clothing 3. • Common treatment options include: – Medications 2, nerve blocks 1, surgical resection of the involved nerve 1, although these modalities generally provide transient relief. • Here, we report a case of post-surgical iliohypogastric/ilioinguinal neuralgia successfully treated with percutaneous peripheral nerve stimulation. 17 th Annual GME Resident and Fellow Research Day June 4, 2020 2

Methods • 47 year old morbidly obese female presents with 7 months of chronic left sided lower abdominal after undergoing Roux-en-Y gastric bypass surgery. • Pain described as 6/10, constant and stabbing, exacerbated by movement • PE: TTP at LLQ, with no guarding, or signs of peritonitis. • CT A/P: showed post-operative changes related to the surgical procedure, but no other abnormalities. • Previously attempted treatments: – – neuropathic pain medications, two iliohypogastric nerve blocks Both diagnostic and therapeutic for several months • Patient subsequently underwent percutaneous peripheral nerve stimulation lead implantation remote from the iliohypogastric and ilioinguinal nerves to provide coverage of the painful region. • The leads are intended to be implanted for up to 60 days of PNS before removal. 17 th Annual GME Resident and Fellow Research Day June 4, 2020 3
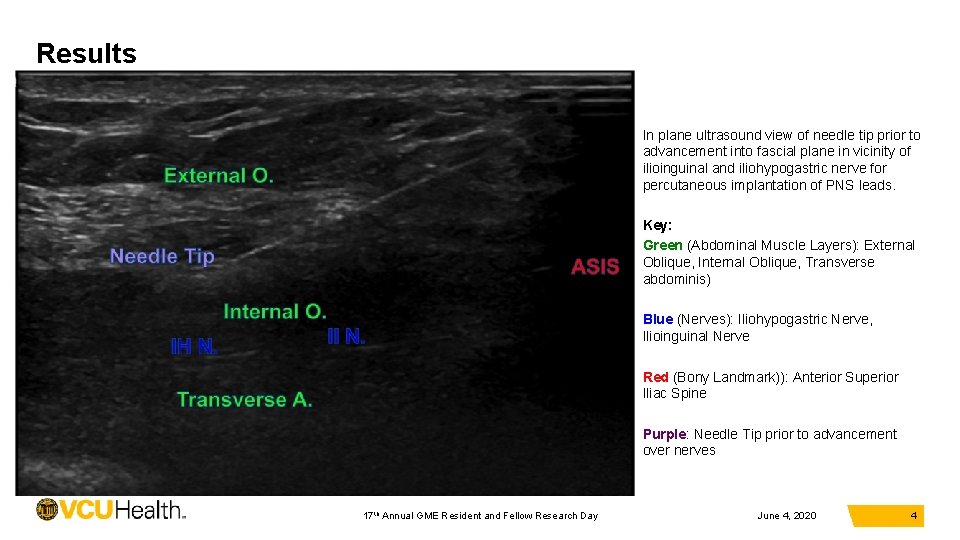
Results In plane ultrasound view of needle tip prior to advancement into fascial plane in vicinity of ilioinguinal and iliohypogastric nerve for percutaneous implantation of PNS leads. Key: Green (Abdominal Muscle Layers): External Oblique, Internal Oblique, Transverse abdominis) Blue (Nerves): Iliohypogastric Nerve, Ilioinguinal Nerve Red (Bony Landmark)): Anterior Superior Iliac Spine Purple: Needle Tip prior to advancement over nerves 17 th Annual GME Resident and Fellow Research Day June 4, 2020 4

Results • The procedure resulted in no complications. • Upon introduction of leads, patient felt immediate and complete pain relief • After the first week of stimulation, patient had complete resolution of pain, with a score of 0 out of 10. • At the patient’s 60 day follow up, the pain score remained 0 out of 10, and the leads were successfully removed. • Pain relief remains several months later. 17 th Annual GME Resident and Fellow Research Day June 4, 2020 5

Discussion and Conclusion • Chronic pelvic and abdominal pain can be challenging conditions to treat. • When first line options of treatment have been exhausted, it can be helpful to try additional options. • In this case, peripheral nerve stimulation was used after positive results were elicited from iliohypogastric nerve block. • This resulted in complete resolution of the patient’s chronic abdominal pain, and may potentially induce more effective pain relief than conventional methods. • Peripheral nerve stimulation should be considered as a modality for relief of iliohypogastric/ilioinguinal neuralgia • Multiple possible mechanisms at work (Gate theory of pain, continued relief after lead removal addresses central sensitization 17 th Annual GME Resident and Fellow Research Day June 4, 2020 6
- Slides: 6