Chronic Obstructive Pulmonary Disease COPD Omer Alamoudi MD

Chronic Obstructive Pulmonary Disease (COPD) Omer Alamoudi, MD, FRCP, FCCP, FACP Professor, consultant Pulmonologist dramoudi@yahoo. com

Definition of COPD ØCOPD is a chronic obstructive pulmonary disease that is characterized by airflow limitation that is not fully reversible. ØThe airflow limitation is usually both progressive and associated with an abnormal inflammatory response Ø COPD is a preventable and treatable disease

Chronic Obstructive Pulmonary disease (COPD) Ø Chronic bronchitis Ø Emphysema

COPD Ø Definitions ØChronic bronchitis: Cough and sputum production for at least 3 months in each of two consecutive years in albescence of other endobronchial disease such as bronchiectasis ØEmphysema: overinflation of the distal airspaces with destruction of alveolar septa
Prevalence of COPD worldwide and in KSA

Prevalence/Risk Factors Cigarette Smoking Ø Cigarette smoking is the primary cause of COPD. Ø Approximately 90% of COPD patients have a smoking history Ø The WHO estimates 1. 1 billion smokers worldwide, increasing to 1. 6 billion by 2025. Ø In low- and middle-income countries, rates are increasing at an alarming rate • .

Smoking Prevalence Among Doctors Country Male% Female% UK 8 5 USA 9 7 Germany 9 6 Korea 46 28 China 42 35 S. Arabia 38 15

Global Burden of Disease (1990– 2020) 2020 1990 Lower respiratory tract infections 1 Diarrhoeal diseases 2 Conditions during perinatal period 3 Unipolar major depression 4 Ischaemic heart disease 5 Cerebrovascular disease 6 Tuberculosis 7 Measles 8 Road traffic accidents 1 Ischaemic heart disease 2 Unipolar major depression 3 Road traffic accidents 4 Cerebrovascular disease 5 COPD 6 Lower respiratory tract infections 7 Tuberculosis 8 War 9 9 Diarrhoeal diseases Congenital anomalies 10 10 HIV Malaria 11 11 Conditions during perinatal period COPD 12 12 Violence
COPD Prevalence in KSA
COPD Prevalence in KSA (Contd. ) Ø According to one report released by the executive office of the GCC Health Ministers Council, Saudi Arabia is the world’s fourth largest importer of cigarettes. Ø During the year of 2004, the kingdom imported 41, 000 tons of tobacco at a value of SR 1. 45 billion.
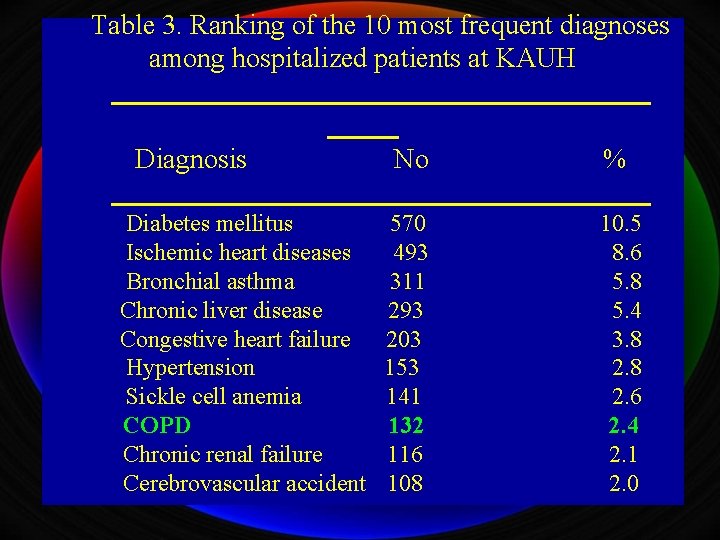
Table 3. Ranking of the 10 most frequent diagnoses among hospitalized patients at KAUH Diagnosis Diabetes mellitus Ischemic heart diseases Bronchial asthma Chronic liver disease Congestive heart failure Hypertension Sickle cell anemia COPD Chronic renal failure Cerebrovascular accident No % 570 493 311 293 203 153 141 132 116 108 10. 5 8. 6 5. 8 5. 4 3. 8 2. 6 2. 4 2. 1 2. 0

Risk Factors

Risk Factors for COPD Host Factors Genes (e. g. alpha 1 -antitrypsin deficiency) Hyperresponsiveness Exposure Tobacco smoke Occupational dusts and chemicals Infections Socioeconomic status
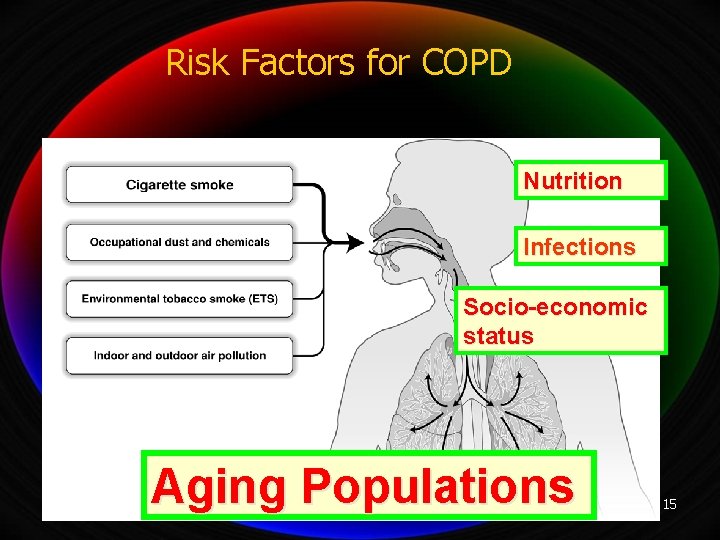
Risk Factors for COPD Nutrition Infections Socio-economic status Aging Populations 15
Pathogenesis of COPD
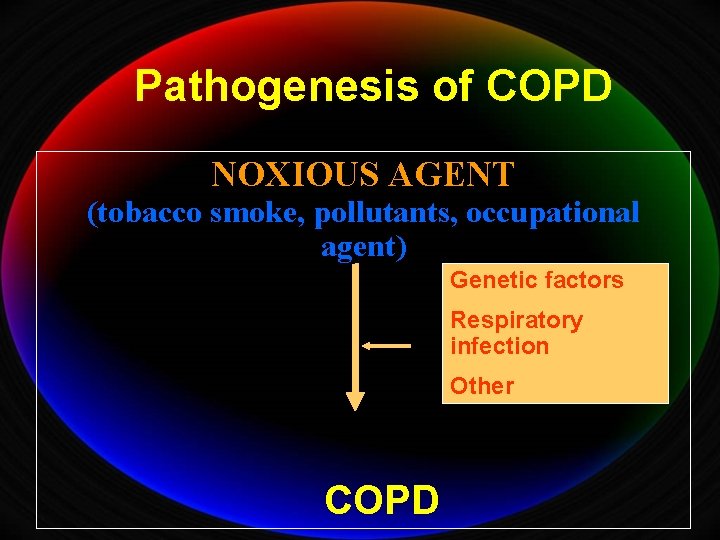
Pathogenesis of COPD NOXIOUS AGENT (tobacco smoke, pollutants, occupational agent) Genetic factors Respiratory infection Other COPD
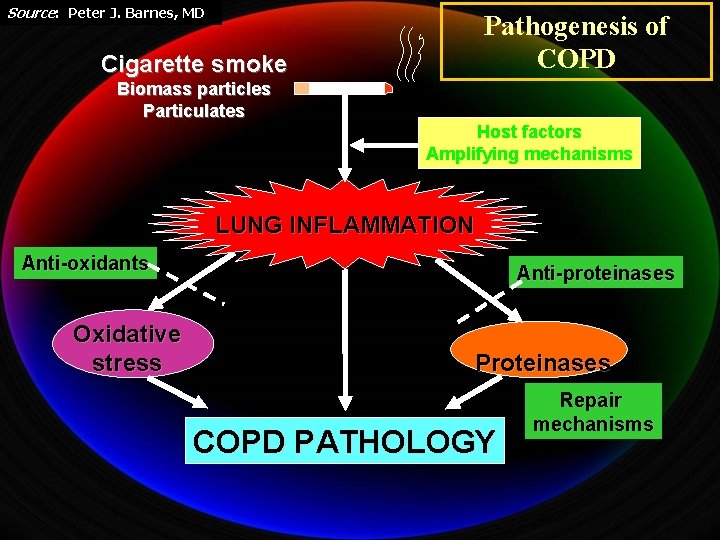
Source: Peter J. Barnes, MD Pathogenesis of COPD Cigarette smoke Biomass particles Particulates Host factors Amplifying mechanisms LUNG INFLAMMATION Anti-oxidants Oxidative stress Anti-proteinases Proteinases COPD PATHOLOGY Repair mechanisms
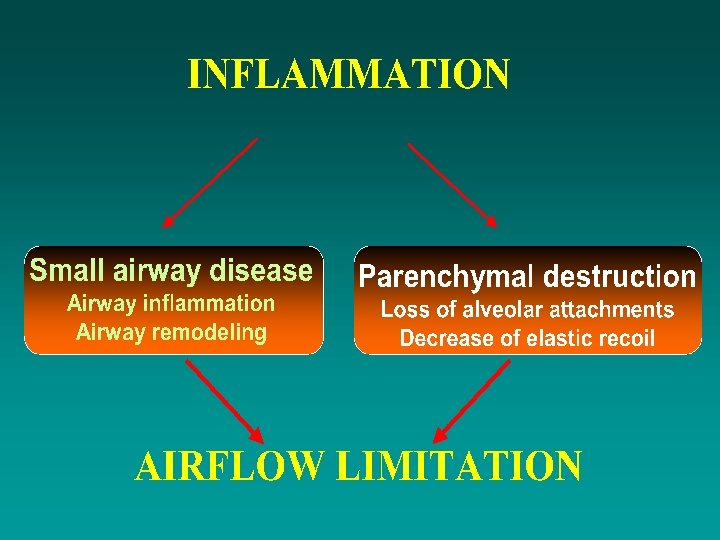

Causes of Airflow Limitation Ø Irreversible ØFibrosis and narrowing of the airways ØLoss of elastic recoil due to alveolar destruction ØDestruction of alveolar support that maintains patency of small airways

Airway Pathology in COPD

Airway pathology in COPD

Airway pathology in COPD
Diagnosis of COPD

Diagnosis of COPD § A clinical diagnosis of COPD should be considered in any patient who has dyspnea, chronic cough or sputum production, and/or a history of exposure to risk factors for the disease. § The diagnosis should be confirmed by spirometry. post-bronchodilator FEV 1/FVC < 0. 70 confirms the presence of airflow limitation that is not fully reversible. § Comorbidities are common in COPD and should be actively identified. A 25
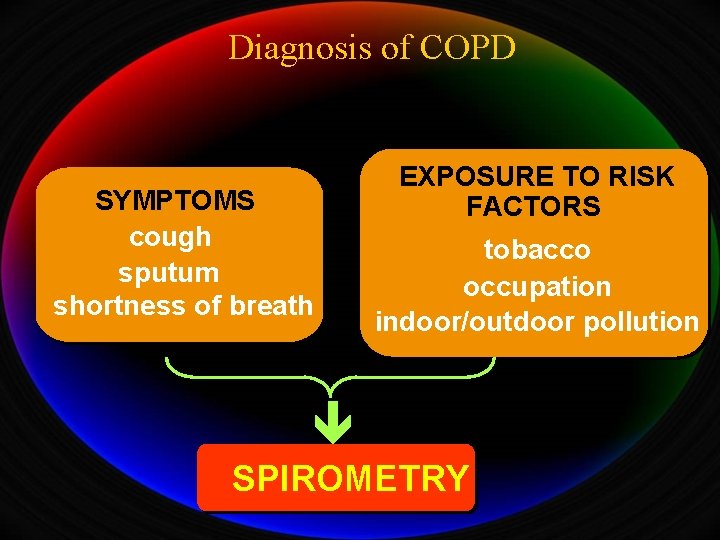
Diagnosis of COPD SYMPTOMS cough sputum shortness of breath EXPOSURE TO RISK FACTORS tobacco occupation indoor/outdoor pollution è SPIROMETRY
Diagnosis of COPD Ø Signs Ø Hands ØFlapping tremor, dilated veins, collapsing pulse, warm hands (CO 2 retention) ØCyanosis, clubbing of the finger (ca lung) Ø Chest (signs of hyperinflation) ØBarrel chest, use of accessory ms, decreased expansion, absence cardiac dullness, tracheal tug ØHyperesonant on percussion
Diagnosis of COPD Ø Sign of pulmonary HTN ØIncreased JVP, left parasternal heave, Loud P 2, Hepatomegaly, Ascitis, lower limb edema Ø Fundus examination ØPapilloedema Ø Extrapulmonary manifestation ØMs wasting
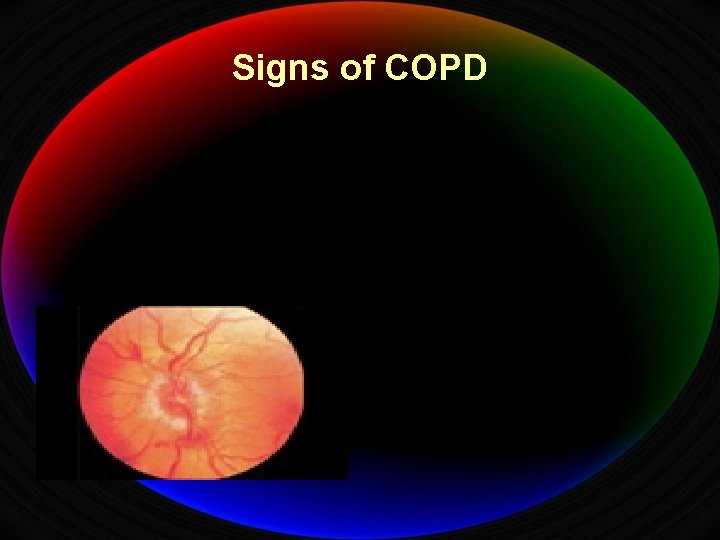
Signs of COPD



Diagnosis of COPD: Spirometry § Spirometry should be performed after the administration of an adequate dose of a shortacting inhaled bronchodilator to minimize variability. § A post-bronchodilator FEV 1/FVC < 0. 70 confirms the presence of airflow limitation that is not fully reversible. 32
Diagnosis of COPD / Spirometry
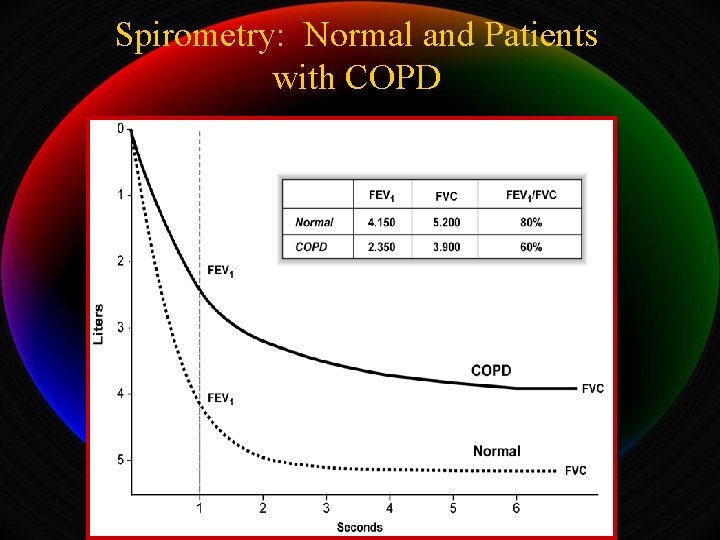
Spirometry: Normal and Patients with COPD
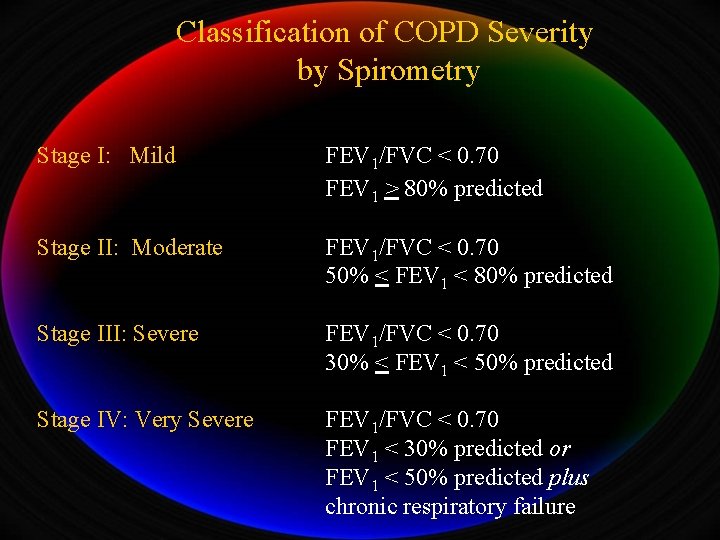
Classification of COPD Severity by Spirometry Stage I: Mild FEV 1/FVC < 0. 70 FEV 1 > 80% predicted Stage II: Moderate FEV 1/FVC < 0. 70 50% < FEV 1 < 80% predicted Stage III: Severe FEV 1/FVC < 0. 70 30% < FEV 1 < 50% predicted Stage IV: Very Severe FEV 1/FVC < 0. 70 FEV 1 < 30% predicted or FEV 1 < 50% predicted plus chronic respiratory failure
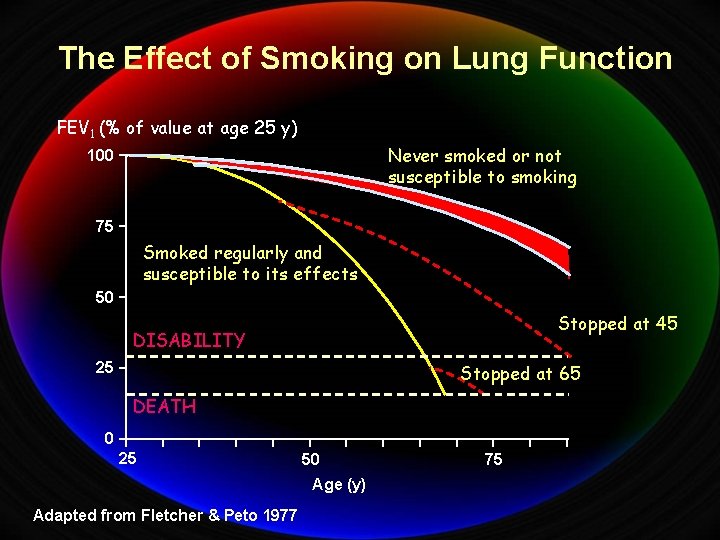
The Effect of Smoking on Lung Function FEV 1 (% of value at age 25 y) Never smoked or not susceptible to smoking 100 75 Smoked regularly and susceptible to its effects 50 Stopped at 45 DISABILITY 25 Stopped at 65 DEATH 0 25 50 Age (y) Adapted from Fletcher & Peto 1977 75
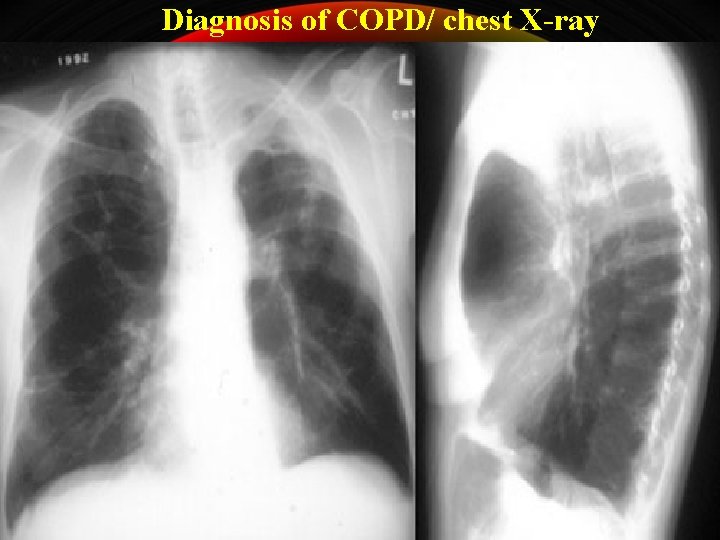
Diagnosis of COPD/ chest X-ray
Diagnosis of COPD/ HRCT scan
Diagnosis of COPD Ø CBC Ø ESR WBC (increased with infection) Hb (secondary Polycthemia) Increased with infection malignancy

Diagnosis of AECOPD
Diagnosis of AECOPD Ø Diagnosis of AECOPD was based on ATS criteria ØMajor ØIncreased dyspnea ØIncreased sputum production ØPurulent sputum ØMinor ØCough, wheeze, sore throat, and cold and nasal discharge
Diagnosis of AECOPD/sputum culture Ø Pathogens isolated during exacerbation Ø Bacterial ØMoraxella catarrhalis ØPseudomonas ØHaemophilus influenzae Ø Viral ØInfluenza Ø Atypical bacteria ØMycoplasma ØChlamydia


Differential Diagnosis COPD VS Asthma

Differential Diagnosis: COPD and Asthma COPD • Onset in mid-life • Symptoms slowly progressive • • • Long smoking history Dyspnea during exercise Largely irreversible airflow limitation ASTHMA • Onset early in life (often childhood) • Symptoms vary from day to day • Symptoms at night/early morning • Allergy, rhinitis, and/or eczema also present • Family history of asthma • Largely reversible airflow limitation

COPD and Co-Morbidities COPD patients are at increased risk for: • Myocardial infarction, angina • Osteoporosis • Respiratory infection • Depression • Diabetes • Lung cancer

Pulmonary Hypertension in COPD Chronic hypoxia Pulmonary vasoconstriction Muscularization Pulmonary hypertension Cor pulmonale Intimal hyperplasia Fibrosis Obliteration Edema Death Source: Peter J. Barnes, MD
Management of COPD and Exacerbation
Management of COPD Prevention § Smoking cessation: is the single most effective — and cost effective — intervention in most people to reduce the risk of developing COPD and stop its progression § Controlling pollution: Reduction of total personal exposure to tobacco smoke, occupational dusts and chemicals, and indoor and outdoor air pollutants are important goals to prevent the onset and progression of COPD. 50

Management of COPD Smoking cessation § Counseling delivered by physicians § Numerous effective pharmacotherapies for smoking cessation are available § § § Nicotine chewing gum, transcutaneous patches, nicotine inhalers or nasal spray Buproprion (aminoketone) (reduce nicotine withdrawal symptoms) § Epilepsy, tremor, insomnia, tachycardia 51 Nortiptyline
Management of COPD Bronchodilators §Anticholinergics § Ibratropium bromide (short acting) § Improve nocturnal O 2 saturation § Improve quality of sleep § Doses: 40 ug 1 -2 puffs q 6 h §Mainly used during exacerbation and symptomatic patients 52

Management of COPD Bronchodilators Tiotropium bromide (long acting anticholinergic) § Once daily § No systemic cholinergic effect §M 3 receptors antagonist §Dose: 18 ug/day § Used in combination with LAB ± ICS or alone in stable COPD § Decrease symptoms, improve exercise tolerance §Decrease exacerbation 53

Management of COPD Bronchodilators § ß 2 -agonists (Salbutamol, Terbutaline) §Rapid relief of symptoms §Dose: 120 ug, 2 puffs q 4 - 6 h §Tachycardia, tremors § Methylxanthines (Theophylline) § week bronchodilator effect §Monitor serum level (55 -110 umol/l) §Hepatic disease, heart failure, drugs; erythromycin, ciprofloxacin increase serum level 54
Management of COPD Long Acting Bronchodilators (LAB) § LAB is more effective and convenient than treatment with short-acting bronchodilators § Salmeterol (50 ug) § Formoterol (9 ug) §Doses: q 12 h § It should be added with Ibratropium or tiotropium if further improvement in symptoms is required 55

Management of COPD Glucocorticosteroids § Long term use of ICS treatment is appropriate for: ● symptomatic COPD patients with an FEV 1 < 50% predicted (stage 111, 1 V) ● repeated exacerbations ● Allergy § § Budesonide 800 ucg BD Fluticasone 500 ucg BD § Chronic treatment with oral corticosteroids should be avoided because of an unfavorable benefit-to-risk ratio 56
Management of COPD Other Pharmacologic Treatments Antibiotics: Only used to treat infectious exacerbations of COPD § Respiratory stimulants (improve ABG) §Doxapram §Almitrine § Mucolytic agents, Antitussives: Not recommended in stable COPD 57

Management of COPD Pharmacotherapy: Vaccines § Influenza vaccines can reduce serious illness and should be given yearly § Pneumococal polysaccharide vaccine may be given although there is no conclusive evidence to support is it use in COPD 58
Management of COPD Non-Pharmacologic Treatments § Rehabilitation: All COPD patients benefit from exercise training programs, improving with respect to both exercise tolerance and symptoms of dyspnea and fatigue § Oxygen Therapy: LTOT (> 15 hours per day) to patients with chronic respiratory failure has been shown to increase survival §PO 2: 55 mm. Hg or less §PO 2: 59 mm. Hg + Polycythemia, Corpulmonale 59
Management of COPD Surgical management Ø Bullectomy Ø Resection bulla allow expansion of the surrounding lung tissue Ø Lung Volume Reduction Surgery Ø FEV 1 < 35% Ø Lung transplant Ø Age <65 Ø FEV<35% Ø Pao 2<55 mm. Hg, Pa. CO 2 >55 mm. Hg Ø Secondary pulmonary HTN, absence of IHD

Management COPD Exacerbations § Antibiotics § 2 nd generation cephalosporin § Amoxicillin / clavulinate § Quinolones § Inhaled bronchodilators, combination of § Ibratropium § B 2 agonist 61

Management COPD Exacerbations § Corticosteroid § IV methyl prednisone § Oral prednisone Should be used in moderate to severe COPD § Hydration § Chest physiotherapy 62

Management COPD Exacerbations § Noninvasive mechanical ventilation §Decreases the need for endotracheal intubation § Mechanical ventilation §Deterioration of level of consciousness §Pa. O 2 40 mm. Hg, p. H < 7. 25 § Medications and education to help prevent future exacerbations should be considered as part of follow-up
- Slides: 62