Chronic Obstructive Pulmonary Disease COPD COPD Description Characterized

Chronic Obstructive Pulmonary Disease (COPD)

COPD Description Characterized by presence of airflow obstruction n Caused by emphysema or chronic bronchitis n Generally progressive n May be accompanied by airway hyperreactivity n May be partially reversible n

Emphysema Description n Abnormal permanent enlargement of the air space distal to the terminal bronchioles n Accompanied by destruction of bronchioles

Chronic Bronchitis Description n Presence of chronic productive cough for 3 or more months in each of 2 successive years in a patient whom other causes of chronic cough have been excluded

COPD Causes n Cigarette smoking Ø Primary cause of COPD*** Ø Clinically significant airway obstruction develops in 15% of smokers Ø 80% to 90% of COPD deaths are related to tobacco smoking Ø > 1 in 5 deaths is result of cigarette smoking

COPD Causes n Cigarette smoking Ø Nicotine stimulates sympathetic nervous system resulting in: n n n HR Peripheral vasoconstriction BP and cardiac workload
COPD Causes n Cigarette smoking Ø Compounds problems in a person with CAD Ø Ciliary activity Ø Possible loss of ciliated cells Ø Abnormal dilation of the distal air space Ø Alveolar wall destruction Ø Carbon monoxide n n Ø O 2 carrying capacity Impairs psychomotor performance and judgment Cellular hyperplasia n n n Production of mucus Reduction in airway diameter Increased difficulty in clearing secretions

COPD Causes n Secondhand smoke exposure associated with: Ø Pulmonary function Ø Risk of lung cancer Ø Mortality rates from ischemic heart disease

COPD Causes n n Infection Ø Major contributing factor to the aggravation and progression of COPD Heredity Ø -Antitrypsin (AAT) deficiency (produced by liver and found in lungs); accounts for < 1% of COPD cases n Emphysema results from lysis of lung tissues by proteolytic enzymes from neutrophils and macrophages
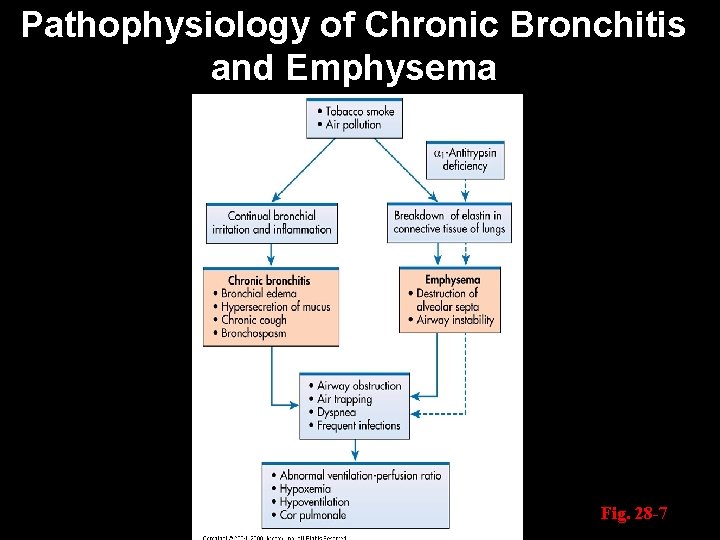
Pathophysiology of Chronic Bronchitis and Emphysema Fig. 28 -7

Emphysema Pathophysiology Ø Hyperinflation of alveoli Ø Destruction of alveolar walls Ø Destruction of alveolar capillary walls Ø Narrowed airways Ø Loss of lung elasticity

Emphysema Pathophysiology Ø Two types: n Centrilobular (central part of lobule) § Most common n Panlobular (destruction of whole lobule) § Usually associated with AAT deficiency

Emphysema Pathophysiology n Structural changes are: Ø Hyperinflation of alveoli Ø Destruction of alveolar capillary walls Ø Narrowed, tortuous small airways Ø Loss of lung elasticity

Emphysema Pathophysiology Ø Small bronchioles become obstructed as a result of n n Ø Mucus Smooth muscle spasm Inflammatory process Collapse of bronchiolar walls Recurrent infections production/stimulation of neutrophils and macrophages release proteolytic enzymes alveolar destruction inflammation, exudate, and edema

Emphysema Pathophysiology Ø Elastin and collagen are destroyed Ø Air goes into the lungs but is unable to come out on its own and remains in the lung n Causes bronchioles to collapse

Emphysema Pathophysiology Trapped air hyperinflation and overdistention Ø As more alveoli coalesce, blebs and bullae may develop Ø Destruction of alveolar walls and capillaries reduced surface area for O 2 diffusion Ø Compensation is done by increasing respiratory rate to increase alveolar ventilation Ø Hypoxemia usually develops late in disease Ø

Emphysema Clinical Manifestations Ø Dyspnea Progresses in severity n Patient will first complain of dyspnea on exertion and progress to interfering with ADLs and rest n

Emphysema Clinical Manifestations Ø Minimal coughing with no to small amounts of sputum Ø Overdistention of alveoli causes diaphragm to flatten and AP diameter to increase

Emphysema Clinical Manifestations Ø Patient becomes chest breather, relying on accessory muscles n Ribs become fixed in inspiratory position

Emphysema Clinical Manifestations Ø Patient is underweight (despite adequate calorie intake)

Chronic Bronchitis Pathophysiology Pathologic lung changes are: Ø Hyperplasia of mucus-secreting glands in trachea and bronchi Ø Increase in goblet cells Ø Disappearance of cilia Ø Chronic inflammatory changes and narrrowing of small airways Ø Altered fxn of alveolar macrophages infections

Chronic Bronchitis Pathophysiology Chronic inflammation n Primary pathologic mechanism causing changes n Narrow airway lumen and reduced airflow d/t § hyperplasia of mucus glands § Inflammatory swelling § Excess, thick mucus

Chronic Bronchitis Pathophysiology Ø Greater resistance to airflow increases work of breathing Ø Hypoxemia and hypercapnia develop more frequently in chronic bronchitis than emphysema

Chronic Bronchitis Pathophysiology Bronchioles are clogged with mucus and pose a physical barrier to ventilation Ø Hypoxemia and hypercapnia d/t lack of ventilation and O 2 diffusion Ø Tendency to hypoventilate and retain CO 2 Ø Frequently patients require O 2 both at rest and during exercise Ø

Chronic Bronchitis Pathophysiology Ø Cough is often ineffective to remove secretions because the person cannot breathe deeply enough to cause air flow distal to the secretions Ø Bronchospasm frequently develops n More common with history of smoking or asthma

Chronic Bronchitis Clinical Manifestations Ø Earliest symptoms: n Frequent, productive cough during winter n Frequent respiratory infections

Chronic Bronchitis Clinical Manifestations Bronchospasm at end of paroxysms of coughing Ø Cough Ø Dyspnea on exertion Ø History of smoking Ø Normal weight or heavyset Ø Ruddy (bluish-red) appearance d/t Ø n n polycythemia (increased Hgb d/t chronic hypoxemia)) cyanosis

Chronic Bronchitis Clinical Manifestations Ø Hypoxemia and hypercapnia n Results from hypoventilation and airway resistance + problems with alveolar gas exchange
COPD Complications Pulmonary hypertension (pulmonary vessel constriction d/t alveolar hypoxia & acidosis) Ø Cor pulmonale (Rt heart hypertrophy + RV failure) Ø Pneumonia Ø Acute Respiratory Failure Ø

COPD Diagnostic Studies Chest x-rays early in the disease may not show abnormalities n History and physical exam n Pulmonary function studies Ø reduced FEV 1/FVC and residual volume and total lung capacity n

COPD Diagnostic Studies n ABGs Ø Pa. O 2 Ø Pa. CO 2 (especially in chronic bronchitis) Ø p. H (especially in chronic bronchitis) Ø Bicarbonate level found in late stages COPD

COPD Collaborative Care n Smoking cessation Ø Most significant factor in slowing the progression of the disease

COPD Collaborative Care: Drug Therapy n Bronchodilators – as maintenance therapy Ø -adrenergic agonists (e. g. Ventolin) n MDI or nebulizer preferred Ø Anticholinergics (e. g. Atrovent)

COPD Collaborative Care: Oxygen Therapy n O 2 therapy Ø Raises PO 2 in inspired air Ø Treats hypoxemia Ø Titrate to lowest effective dose

COPD Collaborative Care: Oxygen Therapy Ø Chronic O 2 therapy at home Improved prognosis n Improved neuropsychologic function n Increased exercise tolerance n Decreased hematocrit n Reduced pulmonary hypertension n
COPD Collaborative Care: Respiratory Therapy n Breathing retraining Ø Pursed-lip n breathing Prolongs exhalation and prevents bronchiolar collapse and air trapping Ø Diaphragmatic breathing n Focuses on using diaphragm instead of accessory n See text re how to teach muscles to achieve maximum inhalation and slow respiratory rate

COPD Collaborative Care: Respiratory Therapy Huff coughing (Table 28 -21) n Chest physiotherapy – to bring secretions into larger, more central airways Ø Postural drainage Ø Percussion Ø Vibration n
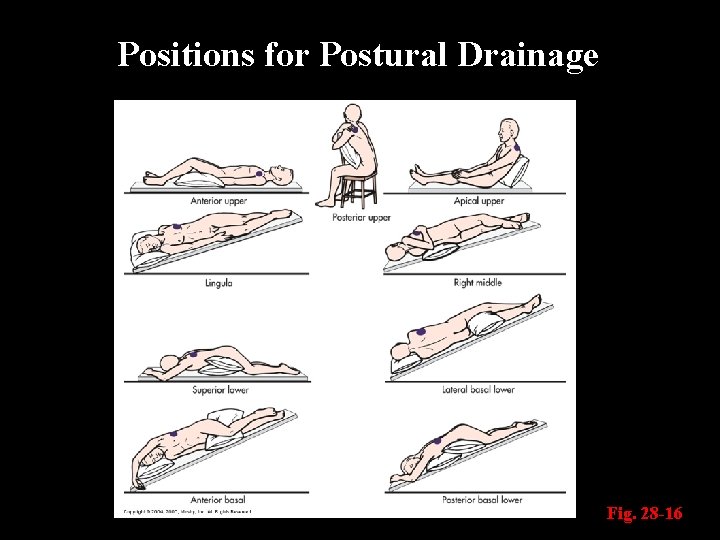
Positions for Postural Drainage Fig. 28 -16

COPD Collaborative Care Ø Encourage as possible patient to remain as active

COPD Collaborative Care n Surgical Therapy Ø Lung volume reduction surgery Ø Lung transplant

COPD Collaborative Care n Nutritional therapy Full stomachs press on diaphragm causing dyspnea and discomfort Ø Difficulty eating and breathing at the same time leads to inadequate amounts being eaten Ø

COPD Collaborative Care Ø Nutritional therapy n n n n To decrease dyspnea and conserve energy Rest at least 30 minutes prior to eating Use bronchodilator before meals Select foods that can be prepared in advance 5 -6 small meals to avoid bloating Avoid foods that require a great deal of chewing Avoid exercises and treatments 1 hour before and after eating

COPD Collaborative Care Ø Nutritional therapy Avoid gas-forming foods n High-calorie, high-protein diet is recommended n Supplements n Avoid high carbohydrate diet to prevent increase in CO 2 load n

Nursing Management Nursing Diagnoses Ineffective airway clearance n Impaired gas exchange n Imbalanced nutrition: less than body requirements n Disturbed sleep pattern n Risk for infection n

Nursing Management Nursing Implementation Health Promotion n STOP SMOKING!!! n Avoid or control exposure to occupational and environmental pollutants and irritants n Early detection of small-airway disease n Early diagnosis of respiratory tract infections

Nursing Management Nursing Implementation Acute Intervention n Required for complications like pneumonia, cor pulmonale, and acute respiratory failure

Nursing Management Nursing Implementation Ambulatory and Home Care n Pulmonary rehabilitation Ø Control and alleviate symptoms of pathophysiologic complications of respiratory impairment

Nursing Management Nursing Implementation Ambulatory and Home Care § Teach patient how to achieve optimal capability in carrying out ADLs n n Physical therapy Nutrition Education Activity considerations n Exercise training of upper extremities to help improve function and relieve dyspnea

Nursing Management Nursing Implementation n n Ambulatory and Home Care Explore alternative methods of ADLs Encourage patient to sit while performing activities Ø Coordinated walking Ø

Nursing Management Nursing Implementation Ambulatory and Home Care Ø Slow, pursed-lip breathing Ø After exercise, wait 5 minutes before using -adrenergic agonist MDI

Nursing Management Nursing Implementation Ambulatory and Home Care n Sexual activity Plan during part of day when breathing is best Ø Slow, pursed-lip breathing Ø Ø Refrain after eating or other strenuous activity Ø Do not assume dominant position Ø Do not prolong foreplay

Nursing Management Nursing Implementation Ambulatory and Home Care n Sleep Nasal saline sprays Ø Decongestants Ø Nasal steroid inhalers Ø Long-acting theophylline Ø n Decreases bronchospasm and airway obstruction

Nursing Management Nursing Implementation Ambulatory and Home Care n Psychosocial considerations Ø Guilt Ø Depression Ø Anxiety Ø Social isolation Ø Denial Ø Dependence Ø Use relaxation techniques and support groups

Nursing Management Nursing Implementation Ambulatory and Home Care Ø Discourage moving to places above 4000 ft.
- Slides: 54