CHRONIC LYMPHOCYTIC LEUKEMIA CLL Curs an IV limba

CHRONIC LYMPHOCYTIC LEUKEMIA (CLL) Curs an IV – limba engleza 2012 -2013

CLL - Definition • CLL is a neoplastic disease characterized by proliferation and accumulation (blood, marrow and lymphoid organs) of morphologically mature but immunologically dysfunctional lymphocytes 10/30/2020 2
CLL - Definition • Clonal B cell malignancy. • Progressive accumulation of long lived mature lymphocytes. • Increase in anti-apoptotic protein bcl-2. • In most cases, the cells are monoclonal B lymphocytes that are CD 5+ • Intermediate stage between pre-B and mature B-cell. • T cell CLL can occur rarely

CLL - Epidemiology • • • Most common leukemia of Western world. Less frequent in Asia and Latin America. Male to female ratio is 2: 1. Median age at diagnosis is 65 -70 years. Uncommon (10%) in patients under 50 years In US population incidence is similar in different races. Cancer statastics 2000; CA J Clin 2000; 50: 7 -33

CLL - Etiology (1) • The cause of CLL is unknown • There is increased incidence in farmers, rubber manufacturing workers, asbestos workers, and tire repair workers • Genetic factors have been postulated to play a role in high incidence of CLL in some families

CLL - Etiology (2) • Cytogenetics – clonal chromosomal abnormalities are detected in approximately 50% of CLL patients – the most common clonal abnormalities are: • trisomy 12 • structural abnormalities of chromosomes 13, 14 and 11 – patients with abnormal karyotypes have a worse prognosis • Oncogenes – in most cases of CLL is overexpressed the protooncogene c-fgr 9 a member of the src gene family of tyrosine kinases

CLL – Initial symptoms • Approximately 40% are asymptomatic at diagnosis – discovered by a CBC • In symptomatic cases the most common complaint is fatigue • Well’s syndrome – increase sensitivity to insects bites • B symptoms – fever, sweats, weight loss • Less often the initial complaint are enlarged nodes or the development of an infection (bacterial)

CLL - Clinical findings • Most symptomatic patients have enlarged lymph nodes (more commonly cervical and supraclavicular) and splenomegaly • The lymph nodes are usually discrete, freely movable, and nontender • Hepatomegaly may occure • Less common manifestation are infiltration of tonsils, mesenteric or retroperitoneal lymphadenopathy, and skin infiltration • Patients rarely present with features of anemia, and bruising or bleeding

CLL – Lab findings a) Blood test lymphocytosis ≥ 5 G/l (4 weeks) b) Morphology monoconal population of small mature lymphocyte c) B-cell CLL phenotype clonal CD 5+/CD 19+ population of lymphocyte d) Markers of clonality κ/λ light chain restriction; cytogenetical abnormalities e) Bone marrow infiltrate > 30% of nuceated cells on aspirate f) Lymph node diffuse infiltrate of small lymphocye

CLL - Laboratory findings (1) • The blood lymphocyte count above 5. 000/mmc • Leukemic cells have the morphologic appearance of normal small lymphocytes • In the blood smears are commonly seen ruptured lymphocytes (“basket” or “smudge” cells) • Careful examination of the blood smear can usually differentiate CLL, and the diagnosis can be confirmed by immunophenotyping
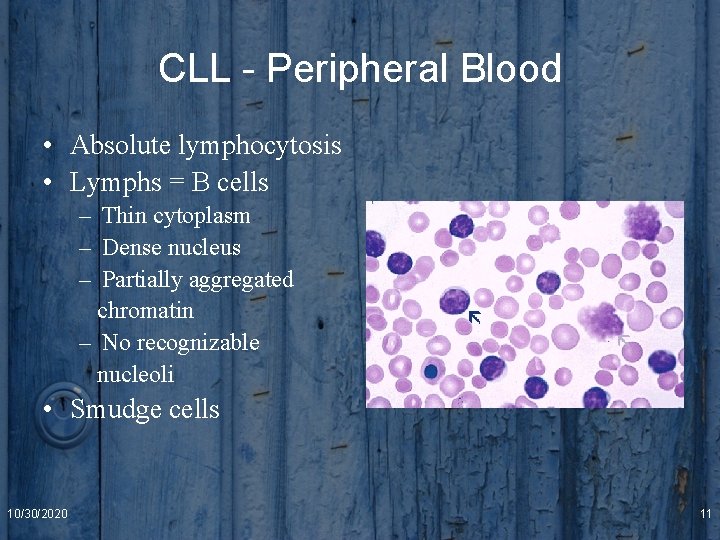
CLL - Peripheral Blood • Absolute lymphocytosis • Lymphs = B cells – Thin cytoplasm – Dense nucleus – Partially aggregated chromatin – No recognizable nucleoli • Smudge cells 10/30/2020 11

CLL - Laboratory findings (2) • Clonal expansion of B (99%) or T(1%) lymphocyte – In B-cell CLL clonality is confirmed by • the expression of either or light chains on the cell surface membrane • the presence of unique idiotypic specificities on the immunoglobulins produced by CLL cells • by immunoglobulin gene rearrangements • typical B-cell CLL are unique in being CD 19+ and CD 5+
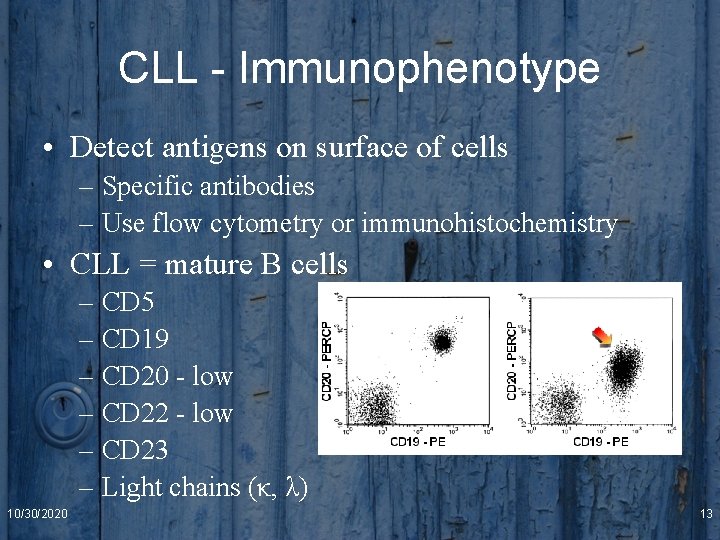
CLL - Immunophenotype • Detect antigens on surface of cells – Specific antibodies – Use flow cytometry or immunohistochemistry • CLL = mature B cells – CD 5 – CD 19 – CD 20 - low – CD 22 - low – CD 23 – Light chains (κ, λ) 10/30/2020 13
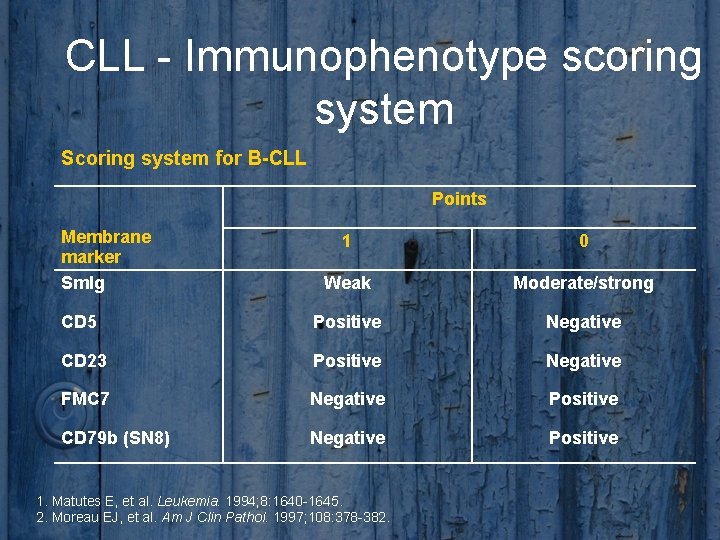
CLL - Immunophenotype scoring system Scoring system for B-CLL Points Membrane marker Smlg 1 0 Weak Moderate/strong CD 5 Positive Negative CD 23 Positive Negative FMC 7 Negative Positive CD 79 b (SN 8) Negative Positive 1. Matutes E, et al. Leukemia. 1994; 8: 1640 -1645. 2. Moreau EJ, et al. Am J Clin Pathol. 1997; 108: 378 -382.

CLL – Other lab tests • Hypogammaglobulinemia or agammaglobulinemia are often observed • 10 - 25% of patients with CLL develop autoimmune hemolytic anemia, with a positive direct Coombs’ test • The marrow aspirates shows greater than 30% of the nucleated cells as being lymphoid 10/30/2020 15
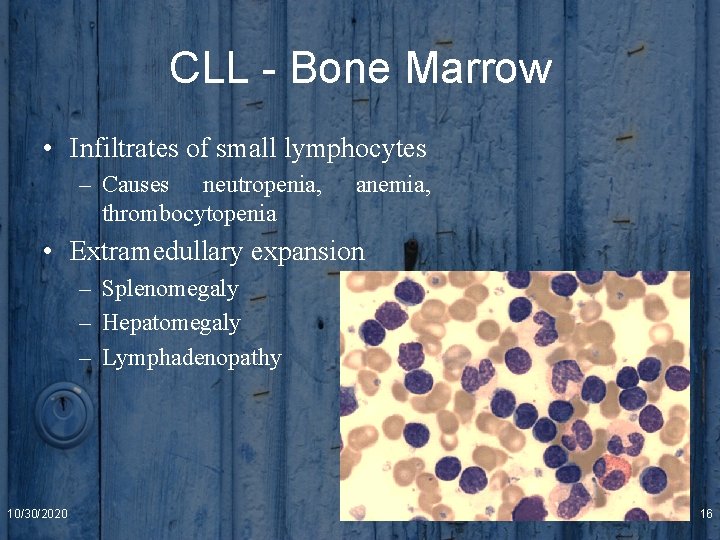
CLL - Bone Marrow • Infiltrates of small lymphocytes – Causes neutropenia, thrombocytopenia anemia, • Extramedullary expansion – Splenomegaly – Hepatomegaly – Lymphadenopathy 10/30/2020 16
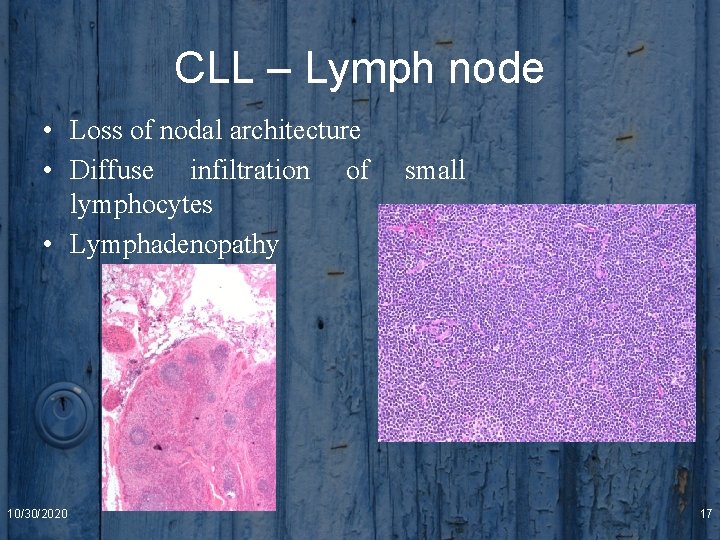
CLL – Lymph node • Loss of nodal architecture • Diffuse infiltration of lymphocytes • Lymphadenopathy 10/30/2020 small 17
CLL - diagnostic criteria 1) A peripheral blood lymphocyte count of greater than 5 G/L, with less than 55% of the cells being atypical 2) The cell should have the presence of Bcellspecific differentiation antigens (CD 19, CD 20, and CD 24) and be CD 5(+) 3) A bone marrow aspirates showing greater than 30% lymphocytes
CLL - Differential diagnosis • Infectious causes – bacterial (tuberculosis) – viral (mononucleosis) • Malignant causes – B-cell – T-cell • • leukemic phase of non-Hodgkin lymphomas Hairy-cell leukemia Waldenstrom macroglobulinemia large granular lymphocytic leukemia

Investigations • Pretreatment studies of patients with CLL should include examination of: – – – – complete blood count peripheral blood smear reticulocyte count Coomb’s test renal and liver function tests serum protein electrophoresis immunoglobulin levels plasma 2 microglobulin level • If available immunophenotyping should be carried out to confirm the diagnosis • Bone marrow biopsy and cytogenetic analysis is not routinely performed in CLL
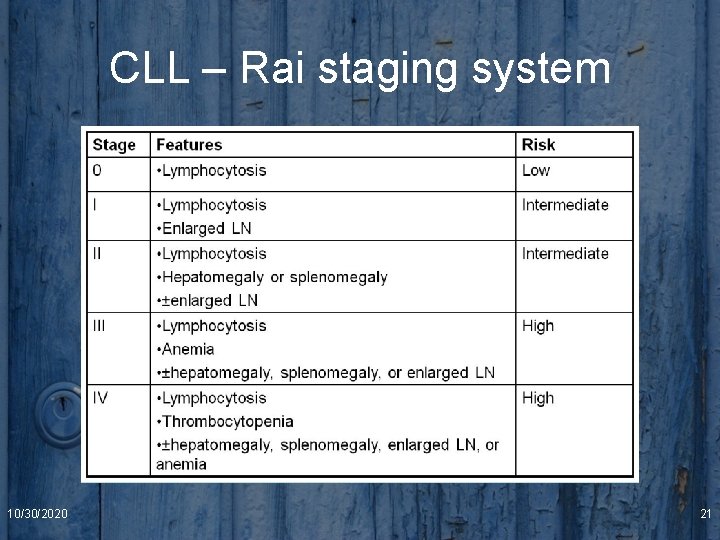
CLL – Rai staging system 10/30/2020 21
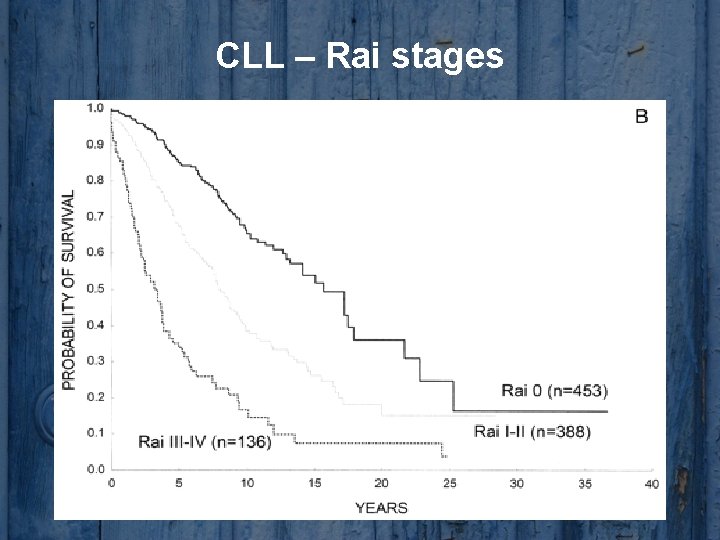
CLL – Rai stages

CLL – Binet staging system 10/30/2020 23
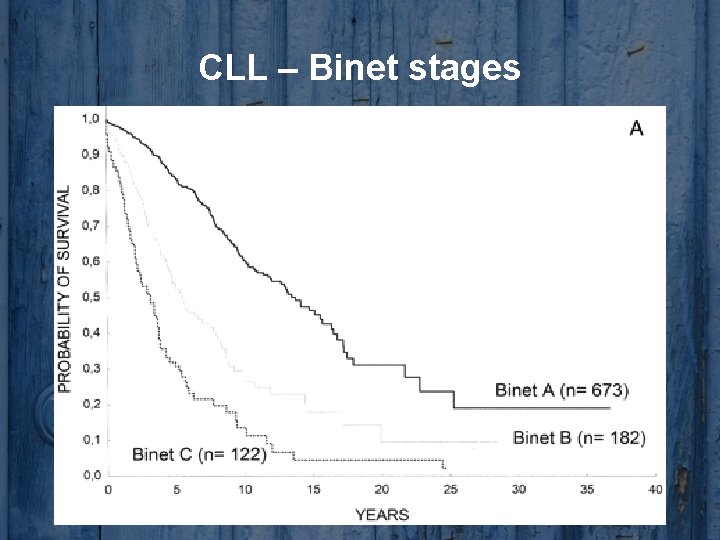
CLL – Binet stages
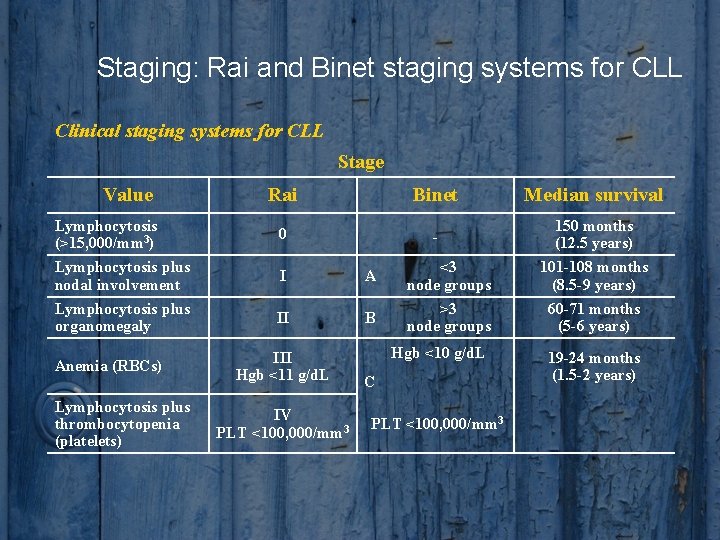
Staging: Rai and Binet staging systems for CLL Clinical staging systems for CLL Stage Value Rai Binet Median survival Lymphocytosis (>15, 000/mm 3) 0 - 150 months (12. 5 years) Lymphocytosis plus nodal involvement I A <3 node groups 101 -108 months (8. 5 -9 years) Lymphocytosis plus organomegaly II B >3 node groups 60 -71 months (5 -6 years) Anemia (RBCs) Lymphocytosis plus thrombocytopenia (platelets) III Hgb <11 g/d. L IV PLT <100, 000/mm 3 Hgb <10 g/d. L C PLT <100, 000/mm 3 19 -24 months (1. 5 -2 years)

CLL - Markers of poor prognosis • • Advanced Rai or Binet stage Peripheral lymphocyte doubling time <12 months Diffuse marrow histology Increased number of prolymphocytes or cleaved cells • Poor response to chemotherapy • High 2 - microglobulin level • Abnormal karyotyping
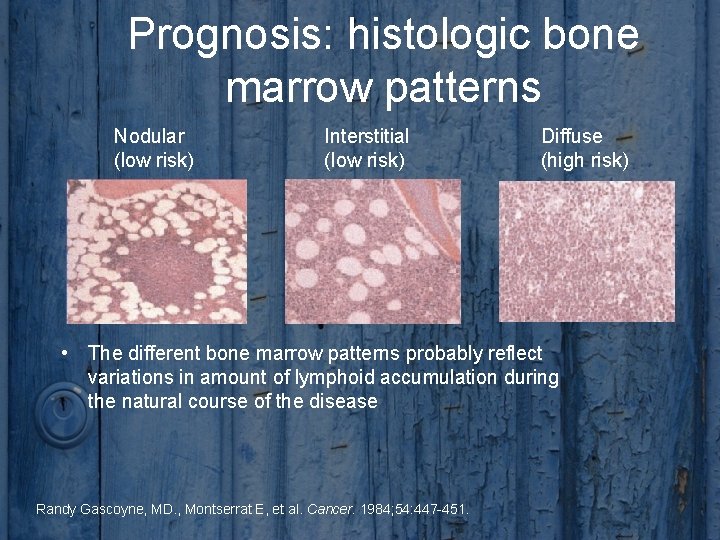
Prognosis: histologic bone marrow patterns Nodular (low risk) Interstitial (low risk) Diffuse (high risk) • The different bone marrow patterns probably reflect variations in amount of lymphoid accumulation during the natural course of the disease Randy Gascoyne, MD. , Montserrat E, et al. Cancer. 1984; 54: 447 -451.

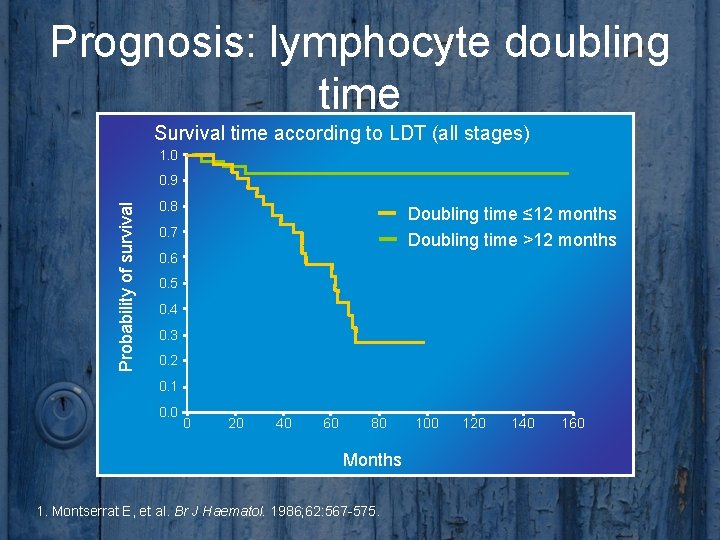
Prognosis: lymphocyte doubling time Survival time according to LDT (all stages) 1. 0 Probability of survival 0. 9 0. 8 Doubling time ≤ 12 months Doubling time >12 months 0. 7 0. 6 0. 5 0. 4 0. 3 0. 2 0. 1 0. 0 0 20 40 60 80 Months 1. Montserrat E, et al. Br J Haematol. 1986; 62: 567 -575. 100 120 140 160
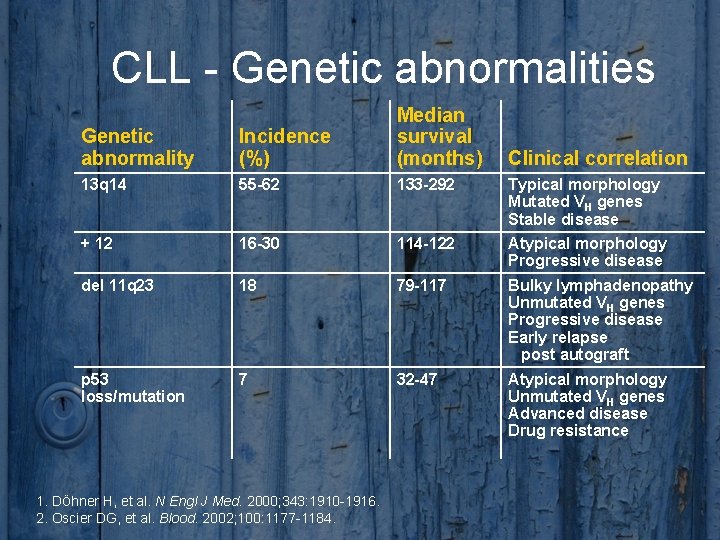
CLL - Genetic abnormalities Genetic abnormality Incidence (%) Median survival (months) 13 q 14 55 -62 133 -292 Typical morphology Mutated VH genes Stable disease + 12 16 -30 114 -122 Atypical morphology Progressive disease del 11 q 23 18 79 -117 Bulky lymphadenopathy Unmutated VH genes Progressive disease Early relapse post autograft p 53 loss/mutation 7 32 -47 Atypical morphology Unmutated VH genes Advanced disease Drug resistance 1. DÖhner H, et al. N Engl J Med. 2000; 343: 1910 -1916. 2. Oscier DG, et al. Blood. 2002; 100: 1177 -1184. Clinical correlation
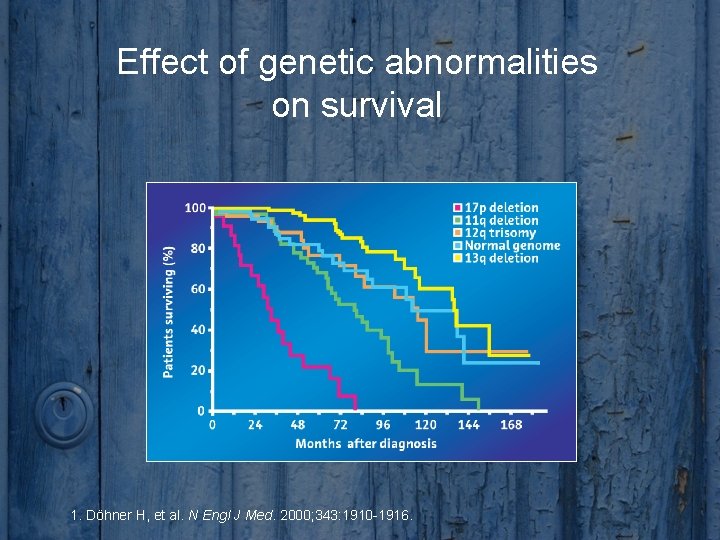
Effect of genetic abnormalities on survival 1. Döhner H, et al. N Engl J Med. 2000; 343: 1910 -1916.
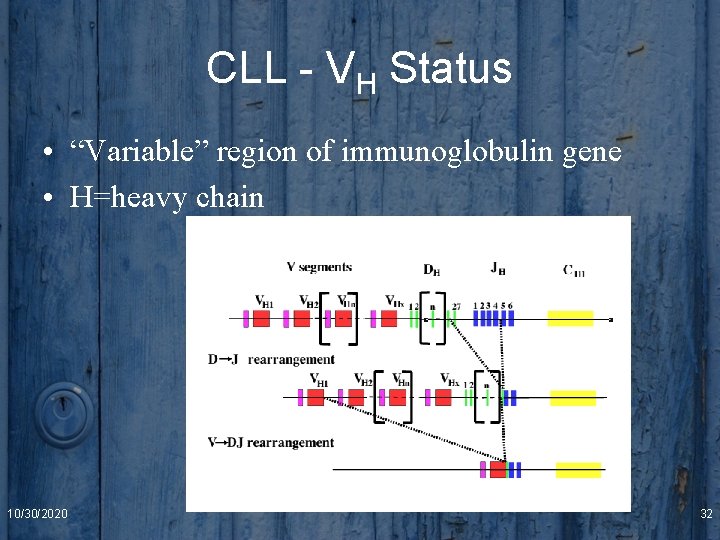
CLL - VH Status • “Variable” region of immunoglobulin gene • H=heavy chain 10/30/2020 32
CLL - VH Mutation • Naïve B cells have unmutated V regions – Make initial Ig. M and Ig. G that bind Ag poorly • Somatic hypermutation of V region creates memory B cells – Make Ab with higher affinity for Ag CLL progression is dependent on mutation status of B cells 10/30/2020 – Unmutated VH = rapid progression, short survival – Mutated VH = slow progression, long survival 33
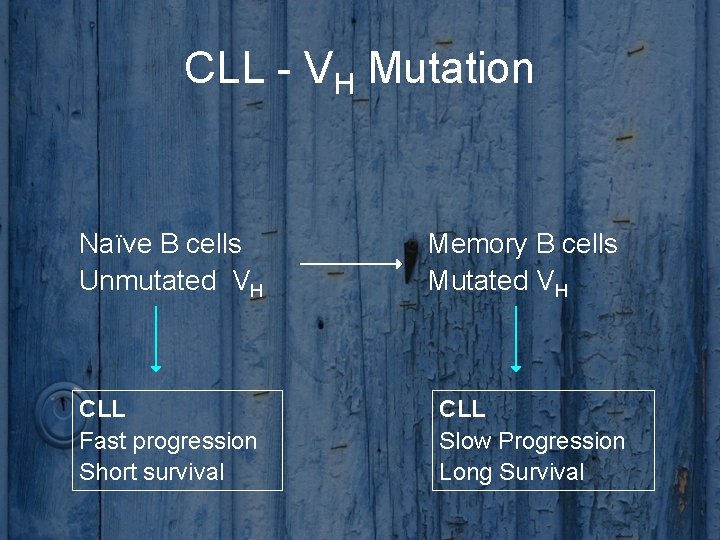
CLL - VH Mutation Naïve B cells Unmutated VH CLL Fast progression Short survival Memory B cells Mutated VH CLL Slow Progression Long Survival
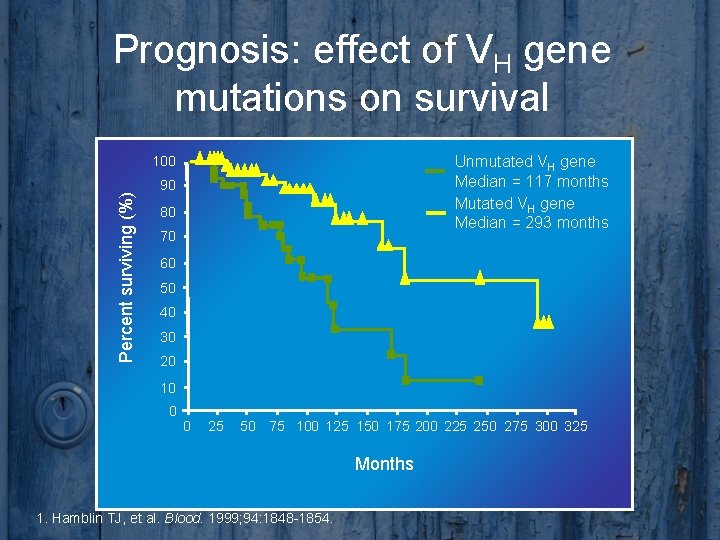
Prognosis: effect of VH gene mutations on survival Unmutated VH gene Median = 117 months Mutated VH gene Median = 293 months Percent surviving (%) 100 90 80 70 60 50 40 30 20 10 0 0 25 50 75 100 125 150 175 200 225 250 275 300 325 Months 1. Hamblin TJ, et al. Blood. 1999; 94: 1848 -1854.

Clinical Course of CLL • Disease has a variable course; however, it often progresses from an indolent lymphocytosis without other evident disease to one of generalized lymphatic enlargement with concomitant pancytopenia • Progression: bone marrow impairment, susceptibility to infection • Complications of pancytopenia, including hemorrhage and infection, represent a major cause of death in these patients
CLL - Immunologic Complications • Autoimmune hemolytic anemia – Coombs’ positive – Clinical hemolysis • Pure red cell aplasia • Immune-mediated thrombocytopenia • Depressed immunoglobin levels • Granulocytopenia • Hypogammaglobulinemia with advanced disease • Long-term complications: autoimmune phenomena, Richter’s transformation

CLL - Complications • • • Severe systemic infections Bleeding Richter’s transformation Prolymphocytoid transformation Secondary malignancies Acute myeloid leukemia

Transforming the way we approach CLL therapy • Traditional treatment goal: Palliation – – Age is a factor Treat to relieve symptoms Continuous/intermittent treatment No survival advantage for any tested treatment to date • New advances may allow treatment for remission and survival – Treat to complete remission (CR) – Eliminate minimal residual disease – Response predicts for survival: More CRs

CLL – treatment (1) • Watch and wait • Monotherapy – glucocorticoids – alkylating agents (Chlorambucil, Cyclophosphamide) – purine analogues (Fludarabine, Cladribine, Pentostatin) • Combination chemotherapy – Chlorambucil/ Cyclophosphamide + Prednisone – Fludarabine + Cyclophosphamide +/- Mitoxantrone – CVP, CHOP • Monoclonal antibodies (monotherapy and in combination) – Alemtuzumab (anti-CD 52) – Rituximab (anti-CD 20) • Splenectomy • Radiotherapy

CLL – treatment (2) • Hematopoietic stem cell transplantation – allogeneic with reduced intesity conditioning – autologous • New and novel agents – – – Oblimersen – bcl 2 -directed antisense oligonucleotide Lenalidomide Flavopiridol Anti-CD 23 Anti-CD 40 • Vaccine strategies • Supportive therapy (allopurinol, G-CSF, blood and platelet transfusion, immunoglobulins, antibiotics)

NCI-WG: Indications to Initiate Treatment for CLL • Constitutional symptoms referable to CLL (B-symptoms) • Progressive marrow failure • Autoimmune anemia and/or thrombocytopenia poorly responsive to corticosteroids • Massive or progressive splenomegaly • Massive or progressive lymphadenopathy • Rapid lymphocyte doubling time
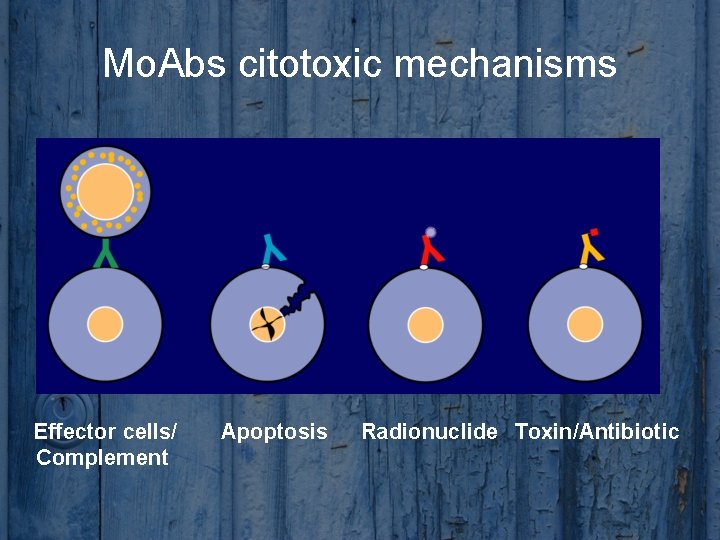
Mo. Abs citotoxic mechanisms Effector cells/ Complement Apoptosis Radionuclide Toxin/Antibiotic

Mo. Abs for CLL Antibody Antigen Alemtuzumab (Campath-1 H) Rituximab (Rituxan, Mabthera) CD 52 CD 20 Epratuzumab (Lympho. Cide) Hu-1 D 10 (Apolizumab) IDEC-152 (Lumiliximab) IDEC-114 Bevacizumab (Avastin) BL-22 CD 22 HLA-DR CD 23 CD 80 VEGF CD 22( conjugate with Pseudomonas)
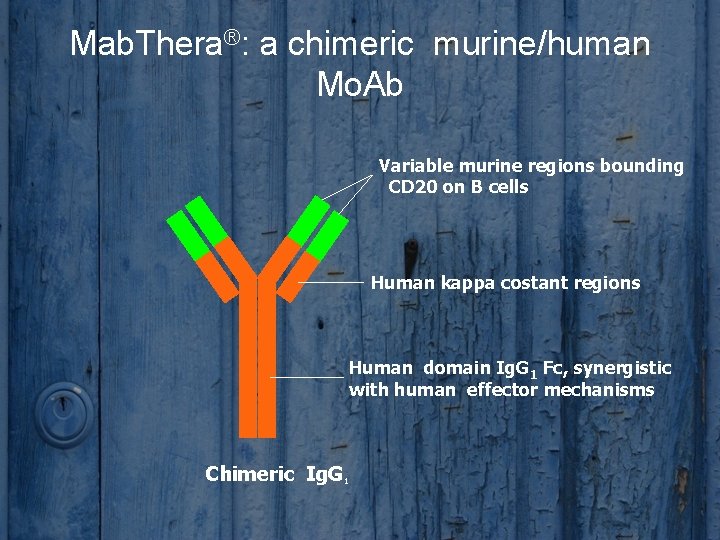
Mab. Thera®: a chimeric murine/human Mo. Ab Variable murine regions bounding CD 20 on B cells Human kappa costant regions Human domain Ig. G 1 Fc, synergistic with human effector mechanisms Chimeric Ig. G 1

Rituximab as part of first-line therapy for CLL: Rationale • Rituximab monotherapy is moderately active in CLL 1, 2 – Activity is dose dependent (between 500– 2250 mg/m 2)1 • Rituximab acts synergistically with other cytotoxic agents in vitro – Increases fludarabine activity in NHL cell lines 3 – Increases activity of bendamustine, mitoxantrone and other chemotherapeutic agents in CLL cells 4 • Rituximab combination therapies (e. g. R-F, R-FC, R-PC, R-FCM, R-Bendamustine, R-Chlorambucil) are now being assessed
Alemtuzumab (anti-CD 52) antibody Ig. G 1 humanised antibody: Low immunogenicity § CD 52 antigen: § Highly expressed on § all lymphocytes § monocytes and macrophages § spermatozoa § eosinophils § Not expressed on haemopoietic stem cells § Does not modulate/shed § Also expressed on the majority of malignant lymphocytes

Treatment of CLL
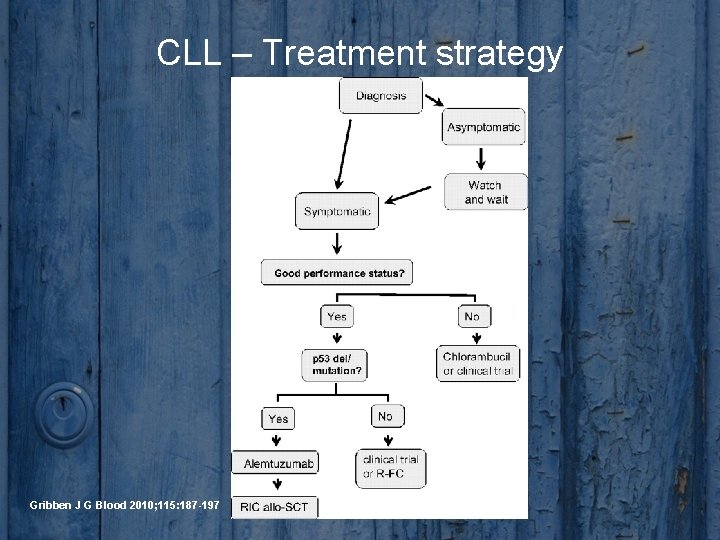
CLL – Treatment strategy Gribben J G Blood 2010; 115: 187 -197
- Slides: 49