Chronic Kidney DiseaseDialysis Belinda Jim MD January 15

Chronic Kidney Disease/Dialysis Belinda Jim, MD January 15, 2009

Definition n NKF’s (National Kidney Foundation’s) K/DOQI (Kidney Disease Outcomes Quality Initiative) Work Group criteria for CKD are: n Kidney damage for >3 months, with or without decreased GFR manifest by either: n Pathological abnormalities or n Markers of kidney damage, including abnormalities in the composition of the blood or urine, or abnormalities in the imaging tests. OR n GFR < 60 ml/min/1. 73 m 2 for >3 months

Causes of ESRD Regardless of acute or chronic, should calculate renal function by e. GFR n Used to evaluate extent of impairment, follow course of disease and response to therapy n Dose adjustments n

Equations to Estimate GFR n Gold Standard – inulin clearance, I-iothalmate, Tc. DTPA clearance. These tests are not uniform. n Cockcroft-Gault equationn (140 -age) x wt/ 72 x SCr. (x 0. 85 for women). n MDRD (Modification of Diet in Renal Disease) – Abbreviated version n 186 x SCr. To power of -0. 203 (x 0. 742 if female) and (x 1. 210 if black). n 24 hr. Urine for Cr. Cl – n GFR = UCr. V/PCr x 0. 70 (to convert to ml/min)
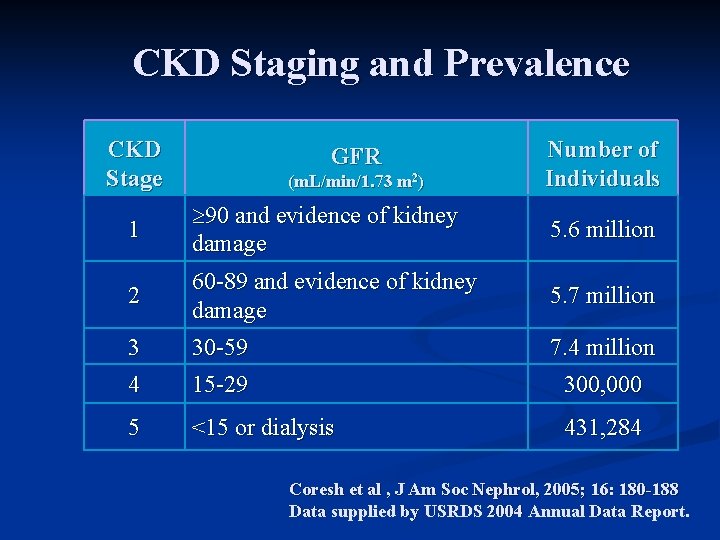

CKD Staging and Prevalence CKD Stage GFR (m. L/min/1. 73 m 2) Number of Individuals 1 90 and evidence of kidney damage 5. 6 million 2 60 -89 and evidence of kidney damage 5. 7 million 3 30 -59 7. 4 million 4 15 -29 300, 000 5 <15 or dialysis 431, 284 Coresh et al , J Am Soc Nephrol, 2005; 16: 180 -188 Data supplied by USRDS 2004 Annual Data Report.

Natural History of Renal Disease n n n Initial injury may vary in pathogenesis Kidney adapts by increasing filtration rate in remaining normal nephrons adaptive hyperfiltration Long-term damage, manifested by proteinuria and progressive renal insufficiency Gradual decline usually asymptomatic No exact correlation between level of BUN and symptoms Uremic symptoms: anorexia, nausea, vomiting, fatigue, hiccups, pruritis

General Management n Treatment of reversible causes Decreased renal perfusion n Administration of nephrotoxic drugs n Urinary tract obstruction n Prevention or slow the progression n Treatment of complications n Identification and adequate preparation of renal replacement therapy (RRT) n

Factors Affecting Progression of CKD Non-Modifiable Risk Factors: n Age – incidence climbs after 65 n Gender – more common in males with a faster rate of decline. n Race – incidence higher in AA and Hispanics. n Genetics – diabetic and non-diabetic nephropathies cluster in families.

Modifiable Risk Factors n n n Proteinuria – aim for <500 mg/24 hr. Hypertension – aim for <130/80 or MAP <90 with ACE I/ARB. Glycemic control – Evidence is conflicting in progression of CKD. Dyslipidemia – elevated levels associated with more rapid decline – esp in DN. Obesity - linked to faster rate of progression in CKD. Hyperuricemia – May cause renal injury and HTN through stimulation of renin-angiotensin system.

Treatment of Complications Volume overload n Hyperkalemia n Metabolic acidosis n Hyperphosphatemia n Anemia n Hyperparathyroidism n Bone disease n Uremic symptoms n

Volume Overload Sodium and intravascular volume balance usually maintained until GFR falls below 10 to 15 ml/min n Mild to moderate CKD less able to respond to rapid infusions of sodium, prone to overload n Respond to combination of dietary sodium restriction and diuretic therapy n

Hyperkalemia n Problem with n n Aldosterone Distal flow in kidney (e. GFR<10 -15 ml/min). Patient is either: n Oliguric. n Has high K diet. n Has increased tissue breakdown. n Has Hypoaldosteronism (eg. ACE Inhibitors, type IV RTA). Treatment consists of low K diet (2 gm/day), diuretics and kayexalate.
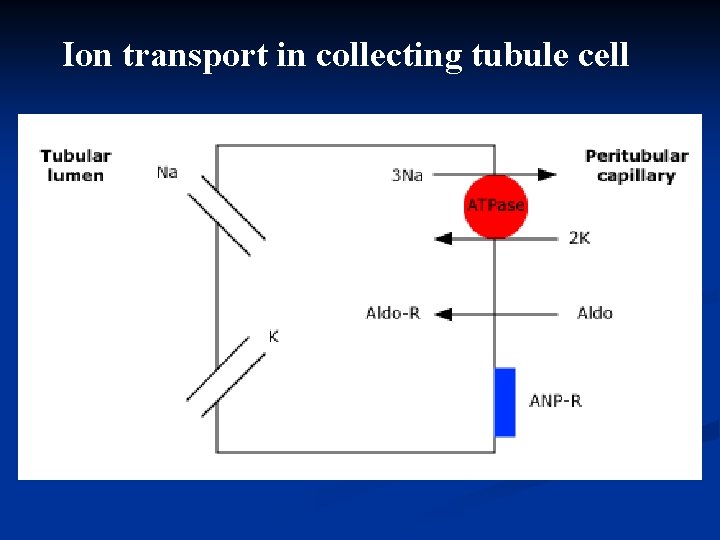
Ion transport in collecting tubule cell

Metabolic Acidosis n n n Increasing tendency to retain H+ Decreased HCO 3 -, usually between 12 -20 meq/L Bone buffering of excess H+ ions associated with release of Ca 2+ and Phos from bone Uremic acidosis increase skeletal muscle breakdown and diminish albumin synthesis loss of lean muscle mass and fatigue Sodium bicarbonate or sodium citrate to keep HCO 3 above 22 meq/L
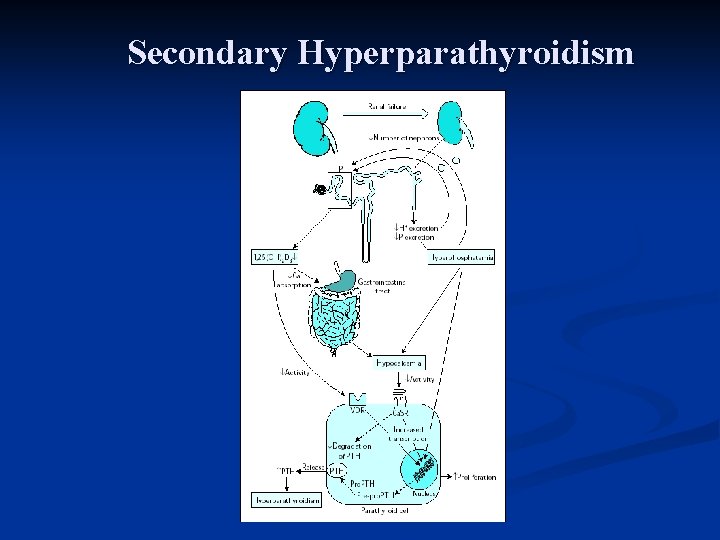
Secondary Hyperparathyroidism

Treatment of Secondary Hyperparathyroidism n Phosphate binders: n Ca based: n Ca. CO 3 n Ca acetate n Non absorbable agent: n Sevelamer Hydrochloride (Renagel) n Sevelamer Carbonate (Renvela) n Lanthanum carbonate (Fosrenol) n Aluminum binders. Vitamin D analogs: n Calcitriol (Rocaltrol) n Paricalcitol (Zemplar) n Doxercalciferol (Hectoral) Calcimimetic: Cinacalcet (Sensipar) n n n Low Phos diet (<800 mg/day)

Renal Osteodystrophy n Types of Bone Disease Osteitis fibrosa n Osteomalacia n Adynamic bone disease n n Target PTH Stage 3 (GFR 30 -59): 35 -70 pg/m. L n Stage 4 (GFR 15 to 29): 70 -110 pg/m. L n Stage 5 (GFR less than 15): 150 -300 pg/m. L n
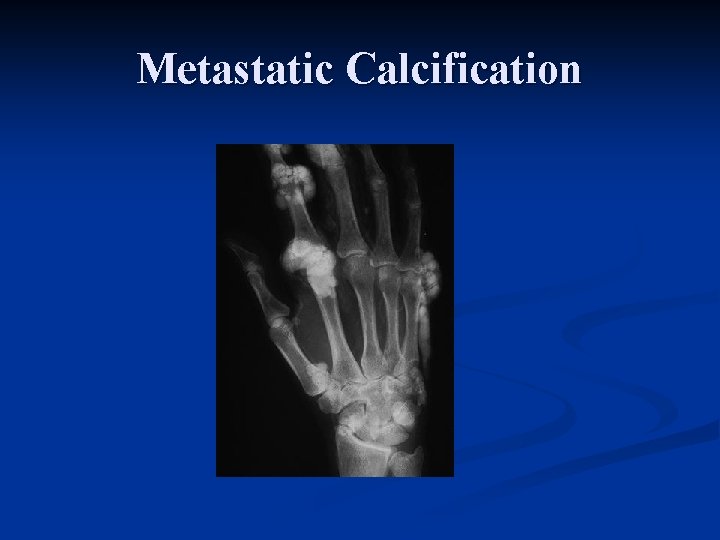
Metastatic Calcification

Hypertension Mostly volume mediated n Start with ACEI/ARB and diuretic n Thiazides become ineffective when GFR falls below 20 n Goal is less than 130/80, but even lower systolic with urine prot/creat >1 n

Anemia in CKD The primary cause of anemia in patients with CKD is insufficient production of erythropoietin (EPO) by the diseased kidneys. n Other causes include: n Iron deficiency. n Secondary hyperparathyroidism. n Decreased RBC lifespan. n Folate deficiency. n

K/DOQI Guidelines for Anemia in CKD n n n Target Hgb between 11 -12 g/d. L Anemia work-up when n Hgb <11 g/d. L (Hct is <33 percent) in premenopausal females and pre-pubertal patients. n Hgb <12 g/d. L (Hct is <37 percent) in adult males and post-menopausal females. Use of erythropoietic agents (Epo, Procrit, Aranesp)

Dyslipidemia n Primary finding in CKD is hypertriglyceridemia n Goal of LDL in CKD in similar to CHD – LDL <100, but there is not much evidence whether this is beneficial. n One large study in CKD Stage V showed a negative association with very low cholesterol levels

Preparation for Renal Replacement Therapy n n n Refer to nephrology when GFR < 60 Early education of CKD Choice of renal replacement therapy n n In-center hemodialysis Peritoneal dialysis Home hemodialysis Access placement n Referral to vascular surgery of AVF placement if patient choses HD and advising patient to save non-dominant arm from venopuctures and heplocks.

What is Dialysis?

Initiation of Emergent Dialysis • • • Uremic syndrome Refractory volume overload Uncontrollable hyperkalemia Severe metabolic acidosis Steady worsening of renal function, with BUN exceeding 70 -100 mg/d. L or creatinine clearance of less than 15 -20 ml/min/1. 73 m 2

Diffusion n Transport process by which a solute passively diffuses down its concentration gradient from one fluid compartment into the other
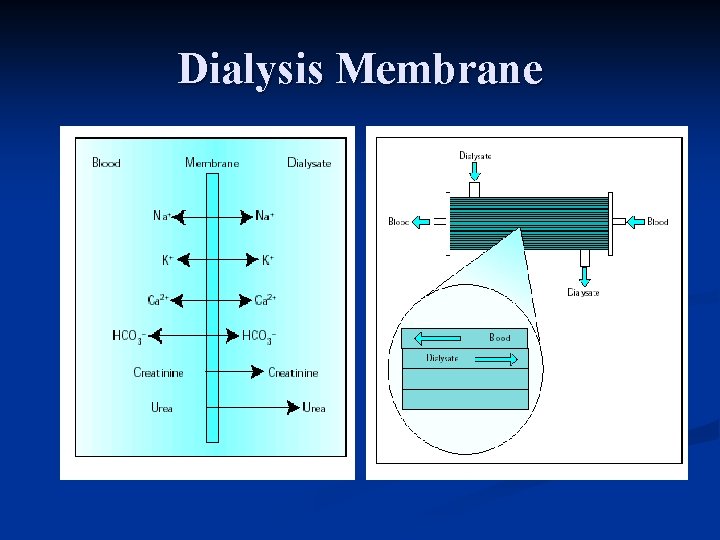
Dialysis Membrane

Contents of Dialysate Solution

Ultrafiltration (UF) n Fluid removal occurs via hydrostatic pressure gradient across membrane generated by dialysis machine
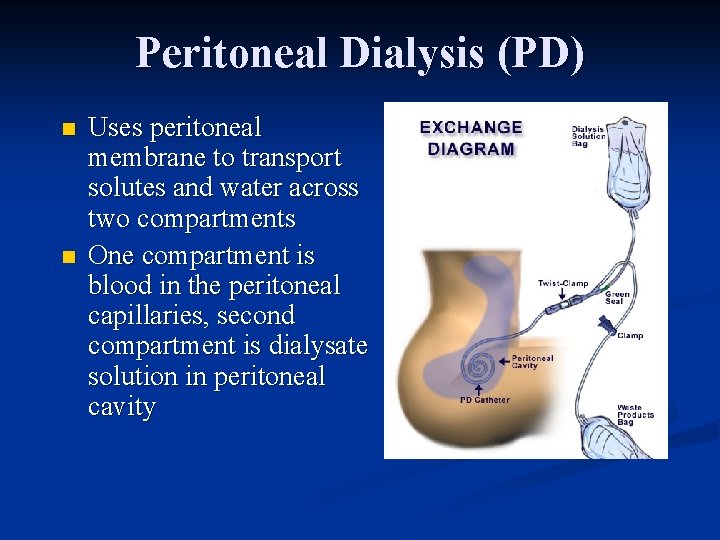
Peritoneal Dialysis (PD) n n Uses peritoneal membrane to transport solutes and water across two compartments One compartment is blood in the peritoneal capillaries, second compartment is dialysate solution in peritoneal cavity

Continuous Renal Replacement Therapies (CRRTs) Slower rate of solute or fluid removal per unit of time § Slower blood flow rate for the hemodynamically unstable patient n Better tolerated than conventional therapy §

Complications Hypotension n Infection n Catheter Dysfunction n

Hypotension n Common Causes Fluctuations in UF rate High UF rate Target dry weight set too low Dialysis solution too warm Food ingestion Autonomic neuropathy Antihypertensive medications

Hypotension-Cardiac Diastolic dysfunction due to LVH, ischemic heart disease n Failure to increase cardiac rate n Inability to increase cardiac output for other reasons n

Hypotension n Less common reasons Pericardial tamponade n Myocardial infarction n Arrhythmia n Occult hemorrhage n Dialyzer reaction n Hemolysis n Air embolism n

Dialysis Catheter Infections n Localized exit site infection n n Tunnel Infection n n Erythema and/or crust, no purulent discharge, treat with antibiotics for up to 2 weeks Purulent exudate present, and pain/warmth along the tunnel, removal of catheter with antibiotic administration for 3 weeks Systemic Infection n Fever, leukocytosis, may have no overt signs of catheter infection

Microbiology Staph species (40 -81%) n Enterococci, gram neg organisms, fungal organisms n Empiric treatment with Vancomycin and Gentamicin n Treat with Nafcillin if MSSA! n

Complications of Catheter Infection Endocarditis n Osteomyelitis n Thrombophlebitis n Spinal epidural abscess n

Catheter Dysfunction n Early less than 5 days n Due to malposition or to intracatheter thrombosis n n Fibrin sleeves and mural thrombi n Treatment n n Catheter exchange TPA

Catheter Dysfunction n Late (more than 5 days) n n More likely due to intracatheter thrombosis than malposition Treatment n n TPA Catheter exchange

Vascular Access Permanent catheter n AV graft n AV fistula n
Permanent Catheter Cuffed venous catheters an alternative form of long-term access n High rate of complications n Thrombosis n Infection n n Inadequate blood flow

AV Graft Advantages • • AV connection made using a tube graft from synthetic material Maturation requires 2 -3 weeks for adhesion of subcutaneous tunnel and graft Disadvantages • • • Higher rates of infection Higher rates of thrombosis Shorter lifespan

AV fistula Advantages • • • Subcutaneous anastomosis of artery to adjacent vein Safest longest lasting permanent access Excellent patency Lower morbidity Lower complication Disadvantages • • • Long maturation time Failure to mature in some patients May not be feasible in patients with vascular disease
- Slides: 44