Chronic Illness Social Issues Illness Behavior Roles Stigma

Chronic Illness: Social Issues Illness Behavior & Roles, Stigma, Adaptation, Social Isolation, Self-Efficacy, Body Image Quality of Life, Adherence

Special Care Issues

All Clients Need Special Care

Illness Behavior and Roles

The Sick Role

Mind-Body Connection

Prognosis: Full Recovery vs Partial Recovery with Continuing Illness

Modifying/Adapting Previous Behavior With Current Expectations

A Diagnosis Changes One’s Actions, Relationships, Self-image & Behavior

Illness Behavior The varying ways individuals respond to bodily indications, how they monitor internal states, define and interpret symptoms, make attributions, take remedial actions and utilize various sources of informal and formal care.

Role Changes Role insufficiency ambiguity conflict strain

Studying Illness Behavior Earliest concept described by Henry Sigerist in a 1929 Essay “Special Position of the Sick” Talcott Parsons developed this concept further and described the “sick role” in his 1951 “The Social System” Work.

Parson’s Sick Role Model Designed in the 1950’s by Talcott Parsons First theoretical concept that explicitly concerned medical sociology Parsons described the sick role as a temporary, medically sanctioned form of deviant behavior

Parson’s Sick Role Model Parsons viewed sickness as a response to social pressure that permitted the avoidance of social responsibilities Anyone could identify and take on any role; the role was therefore achieved through failure to keep well

Sickness=Social Change

Parson’s Sick Role Model 4 major components: Sick person is exempt from normal social roles Sick person is not responsible for his/her condition Obligation to want to become well Obligation to seek and cooperate with technically competent help

Sick Role carried into Healthcare System

Strengths of Model Idea of the sick role has generated a lot of useful far-reaching research It also still has a role in the cross-cultural comparison of ways in which “time-out” from normal duties can be achieved or in which deviant behavior may be explained and excused Example: mental illness vs demonic possession vs religious inspiration (comparing ideas)

Weaknesses of Parsons’ Model Does not examine how the interests of doctor and client might conflict nor explore how this creates imbalances of power Being sick does not automatically lead to being a client. May rely on lay opinions and advice Being a client does not always involve being sick (i. e. pregnancy, contraception, vaccinations, etc)

Weaknesses of Parson’s Model Chronic diseases do not fill the model’s criteria of being a temporary condition. How can it be deviant? The model has no place for “abnormal” illness behaviors (i. e. denial of illness) The patrician model of medicine is simply out of date. Clients more likely view themselves as critical consumers, not under the sole authority of healthcare providers.

Impaired Role

Model Application to Impaired Role Gordon, 1966 first developed the model for the Impaired Role It was his view that the idea of the sick role was more applicable to clients with acute illnesses and injuries than to chronic illnesses He viewed clients with chronic illness as “Impaired” clients rather than sick clients

Gordon’s Study “Gordon identified behaviors, responses and expectations of several socioeconomic groups toward illnesses that differed in both severity and duration” Findings: the major factor in defining someone as “sick” was diagnosis Once someone was diagnosed as sick, the behaviors became consistent with Parson’s Model

Gordon’s Study Gordon identified two roles: 1. Sick Role: sick role is valid if the illness or diagnosis is uncertain or very serious 2. Impaired Role: if society did not have evidence that the sickness was either not known or not very serious, the individual was expected to return to normal behavior within the limitations of the condition.

The Impaired Role Characteristics The individual has an impairment that is permanent The individual does not give up normal role responsibilities but is expected to maintain normal behavior within limits of the health condition The individual does not have to “want to get well, ” but rather is encouraged to make the most of remaining capabilities

Factors Influencing the Sick Role Number and persistence of symptoms Individual’s ability to recognize symptoms Perceived seriousness of symptoms Available information/medical knowledge Cultural background of the defining person, group, or agency Extent of social and physical disability Available sources of help

How Do Clients Respond to Care? What have you seen?

Attitudes and Behaviors Does the client who maintains sick role behaviors prevent them from managing their own care? How difficult is it for the client to accept the impaired role? If accepted, does it result in full realization of potentialities for the client?

Impaired Role=At Risk Role? “The impaired role, sometimes called the “at risk” role, is seen as a transitional state, one in which individuals make changes in a variety of role behaviors in which they engaged before the illness” (Larsen, p 27) This role is seen to have less impact on multiple social roles than does the sick role as it is associated with more uncertainty

Mechanic’s Study Formulated in 1995 Based on Parson’s Work Defines illness behavior as the “varying ways individuals respond to bodily indications, how they monitor internal states, define and interpret symptoms, make attributions, take remedial actions and utilize various sources of formal and informal care” (Larsen, p 27)

Additional Studies Kasl & Cobb (1966) identified various types of health related behavior: 1. Illness behavior 2. Health behavior 3. Sick Role Behavior

Additional Studies Mc. Hugh and Vallis (1986) Suggested that illness behavior be viewed as on a continuum since they are arbitrary at times Throughout chronic illness literature, “illness behavior” terminology has been used interchangeably with the sick role.

Additional Studies Pilowsky (1986) Viewed clients with that presented with incongruent behaviors (either excessive or inadequate response to symptoms) constitute abnormal behavior Examples: displaying extreme or inadequate responses (e. g. ingrown toenail, hypochondriasis, somatization, denial of illness)

The Real Issue “How do we as healthcare professionals describe behavior as normal or abnormal when it is not we who are diagnosed with the chronic condition and have the resulting illness experience?

Influences to Illness Behavior & Roles Social Factors Financial Factors Culture of Poverty (deny sickness until unable to function) Demographics (marital status, gender, increasing age) Past Experience

Social Representation Theory Is a theory concerned with the effect of societal belief systems and how they impact and influence interpretation of illness Herzlich in 1973 (Classic Study): identified 3 lay reactions to illness: 1. “Illness as destructive: The experience of those actively involved in society 2. Illness as liberator: The experience of those with excessive social obligations 3. Illness as an occupation: The experience of those who accept illness and feel they must contribute to its alleviation. ” (Larsen, p 29)

Five Attributes of Illness Representations Described by Levanthal, Levanthal and Cameron (2001) “These attributes form the basis of lay models of illness and guide/shape how we select and use coping strategies”

Five Attributes of Illness Representation “The identity of the threat or the symptoms that define it The time line for development and duration of the disease, treatment regimen, and time needed for cure, treatment or death The causes of the threat (internal or external) The anticipated and experienced consequences of the disease” The controllability of the condition” (Larsen, p 29)

The Illness Experience Interpreted and experienced by client and family uniquely Loss of self (identity issues) Moral Work (need to demonstrate their moral worth? ) Continuity and discontinuity of self following severe chronic illness during the aging process

Who Legitimizes Chronic Illness? Issues of legitimization arise particularly in cases where diagnosis is difficult even though client has symptoms The client doesn’t know if sick or not. Negative responses from family members, workplace, their physicians May result in doctor “hopping” Examples: Chronic fatigue Syndrome, Fibromyalgia

Professional Responses to Illness Behavior What expectations do healthcare professionals have when a client enters the hospital? (Retain much of the control) What expectations to chronically ill clients have when they enter the hospital? (Managing the current acute disorder vs maintaining stability of their condition(s) to prevent unnecessary symptoms Clients may be hospital savy if they have had previous admissions

Nursing’s Key Role Overall, the nursing goal is to empower clients to self-manage as much as possible In order for the nurse to empower the client, must have an understanding of client expertise and capability. Healthcare professionals need to work in a flexible partnership with the client, being free from feeling threatened with an expert client.

Studying Client Issues: Means Listening to Them

Advanced Practitioner: Spends Time to understand Roles & Teach

…As Well as Thoroughly Assessing Them

Interventions Dealing with dependency (allow more client control, help set goals, client teaching, empower, encourage verbalization) Role supplementation -Role clarification -Role rehearsal -Role modeling -Role taking -Dealing with inter- role conflict

Interventions Norms for the impaired role Assisting those in the impaired role Learning to deal with biases Frameworks and models for practice -Chronic illness and quality of life -Trajectory framework Research

Stigma

Definition “Mark of shame or discredit” Arises from widely held social beliefs about personality, behavior and illness Communicated to individuals through a process of socialization
Stigma and Discrimination

Social Identity Includes personal (e. g. , competence) and structural (e. g. , occupation) attributes One’s social identity may include: -Physical activities -Professional roles -Concept of self

Are You Still Like Everyone Else?

Types of Stigma of physical deformity -The actual stigma is the deficit between the expected norm of perfect physical condition and the actual physical condition Character blemishes -May occur in individuals with AIDS, alcoholism, mental illness, or homosexuality Prejudice -Originates when one group perceives features of race, religion, or nationality of another group as deficient compared with their own socially constructed norm

Responses of Individuals Who Are Stigmatized to Others Disregard -May choose not to reflect on or discuss the painful incidents Isolation -May separate themselves into small groups Secondary gains -Individuals may capitalize on their conditions in order to achieve special favors

Responses of Individuals Who Are Stigmatized to Others Resistance -Individuals may speak out and challenge rules and protocol if their needs are not met Passing -Pretending to have a less stigmatic identity Covering -An attempt to make the difference seem smaller or less significant than it really is

Responses of Nonstigmatized People to Stigmatized Individuals Devaluing -Nonstigmatized individuals often believe that the person with the stigma is less valuable Stereotyping -A negative type of category that is a social reaction to ambiguous situations Labeling -Influences the way we think about an individual

Interventions Responses toward self (changes in attitudes) Developing a support group of one’s own Developing supportive others Advocacy Changing definitions of disability

Interventions Nonacceptance versus nonparticipation Professional attitudes (cure versus care) -Selecting an appropriate model for health care delivery -Inservice Education Community education programs

Adaptation Life-Course Navigation of the Challenges of Chronic Illness

Course of Disease/Illness Clients must normally rely on the technology of the healthcare system throughout their illness in order to manage/cure their disease processes However, there additional issues of social, psychological and emotional needs that need to be met as well

Adaptation Definition Adaptation and Adjustment are generally used interchangeably “The term Adaptation means that there is an event, or something that is unusual or different that is perceived as a stressor to the individual that dictates a reaction, a change, or a behavior by the individual” “Adjustment …is the absence of a diagnosed psychological disorder, psychological symptoms or negative mood” (See Larsen p. 68)

General Understanding of Terms In general, means the individual has coped with the illness and has a “good quality of life, well-being, vitality, positive affect, life satisfaction and global self-esteem” Is the client well adjusted or maladjusted? Based on Lazarus Stress Theory Many Models

A Multidimensional Dynamic Process It is the client’s appraisal of their adjustment, their perception, not the healthcare provider’s Positive Adjustment: usually follows emotionally supportive relationships Negative Adjustment: usually follows criticism, social constraints, social isolation

Research Findings Most individuals with chronic illness to eventually adjust well There is, however, a wide variability in adjustment levels in the different studies

Family and Clients Must Adjust

Self-Efficacy

This trait develops early!

Definition “The conviction that one can successfully execute the behavior required to produce the outcome” Varies on 3 dimensions: -Magnitude -Generality -Strength

Human Capabilities in Self-Efficacy Symbolizing capability Forethought capability Vicarious capability Self-regulatory capability Self-reflective capability

Concepts Related to Self-Efficacy Health Locus of Control Self-esteem Coping Learned helplessness

Sources of Self-Efficacy Beliefs Mastery experience -Gives us an indicator of our capabilities Vicarious experience -May cause us to alter our behavior when we compare ourselves with others Verbal persuasion/other social influences Physiological and affective states -Help us judge our capability and vulnerability to dysfunction

Self-Efficacy Processes Cognitive processes Motivational processes Affective processes Selection processes

Interventions Self-management programs Social persuasion Reinterpreting physiologic symptoms Interventions using skills mastery, modeling, verbal persuasion

Social Isolation

Sick? Stay Home !

Existence on a lonely island?

Definition “Aloneness experienced by the individual and perceived as imposed by others as a negative or threatening state”

Distinctions of Social Isolation Number, frequency, and quality of contacts Longevity or durability of contacts Negativism attributed to the isolation felt by the individual

Layers of Social Isolation Community Organization Confidantes Person
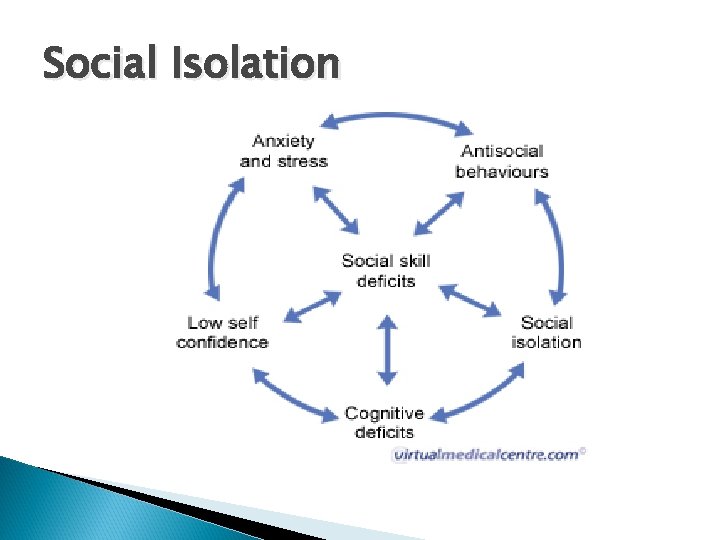
Social Isolation

Patterns of Social Isolation Integrated: persons who have been integrated into social groups throughout their lifetime “Early isolate”-isolated as an adult but is relatively active in old age “Recent isolate”-active in early adulthood but is not in old age “Lifelong isolate”-life is one of isolation

Feelings that Reflect Isolation Boredom -Occurs due to lack of validation of one’s work or daily routines Marginality -Sense of being excluded from desired networks or groups

Social Isolation vs. Similar States of Human Apartness Alienation Loneliness Aloneness

Characteristics of Social Isolation Absence of supportive significant others Verbalized feelings of aloneness imposed by others Verbalized feelings of rejection Apathy Seclusion Few contacts with peers Verbalized awareness of social isolation

Problems and Issues Isolation process Stigma Social roles Culture Social networks Demographic variables Illness factors Health care perspectives

Interventions Assessment of social isolation Management of self: identify development Integrating culture into health care Respite Support groups and other mutual aid Spiritual well-being Rebuilding family networks Communication technologies

Body Image

Definition Mental image of one’s physical self -Attitudes and perceptions of one’s physical appearance -State of health -Skills -Sexuality How One perceives one’s own body How body image influences interactions and others’ reactions

How Do Others See Me?

Self-Concept and Self-Esteem Self-concept-total perception an individual holds of self -Who one believes one is -How one believes one looks -How one feels about one’s self Self-esteem “the evaluative component of an individual’s self-concept”

Factors Influencing Adjustment to Body Image Meaning and significance Influence of time Social influences Cultural influences

Factors Influencing Adjustment of Body Image Influence of health care team members Age Gender Prior experience and coping mechanisms

Assessment of Body Image Assess client’s perception of the experience, knowledge of the illness and its effects, and others’ perceptions of the client’s illness Assess client’s psychosocial history and support systems Assess client’s self-esteem and perceived attitude of others

Body Image Issues External changes -Appearance -Visibility and invisibility Functional limitations (e. g. ADL’s)

Interventions Communication Self-help groups Self-care Prostheses Education and anticipatory guidance

Quality of Life

In General Shift in emphasis from a health care system focused on cure and quantity of life to enhancement of quality of life Greater emphasis on quality of life issues parallels the growth in medical knowledge and use of technology

Research Quality of life is studied to identify and evaluate specific problems and needs of clients with illness or disability Research is conducted to test and compare the impact of interventions on quality of life

Defining Quality of Life: General Meaning Socioeconomic, demographic, and lifestyle factors Personality characteristics Social and community environments Well-being in physical and mental health

Defining Health-Related Quality of Life Health and physical function Emotional well-being General health perceptions Role and social function

Changes in Quality of Life

Health and Function Issues Perceived health Energy level Pain experiences Stress levels Independence Capacity to meet responsibilities Access to and use of health care Usefulness to others

Psychological and Spiritual Issues Life satisfaction Happiness Peace of mind Control Goal of achievement Belief System

Social and Economic Issues Emotional support Home Employment Finances Neighborhood Friends Social support Cultural influences

Family Issues Family health Spousal relationships Family happiness Children

Interventions Health and function Psychosocial and spiritual Social and economic Family

Adherence Formerly Known as “Compliance” with Medical Regimens

Encouraging Client Adherence

Key Terms Adherence: all behavior consistent with health care recommendations Non-Adherence: behaviors that are not consistent with health care recommendations Concordance: partnership between practitioner and client in achieving health outcomes

Models and Theories Health Belief Model Health Promotion Model Common Sense Model Self-Regulation Theory of Reasoned Action Theory of Planned Behavior Cognitive Social Learning Theory Transtheoretical Model of Change

Variables of Nonadherence Individual characteristics Psychological factors Social support Prior health behavior Somatic factors

Variables of Nonadherence Regimen characteristics Economic factors Sociocultural factors Client-provider interactions Motivation

Interventions Assessment Measuring adherence behaviors -Self-report -Practitioner report -Observation -Physiological measures -Medication monitors -Electronic monitoring

Follow-through with Instructions

Interventions Educational strategies Behavioral strategies -Tailoring -Simplifying the regimen -Providing reminders -Enhancing coping -Contracting Ethnocultural interventions
- Slides: 115