CHRONIC CONGESTIVE HEART FAILURE American Heart Association in





































































- Slides: 94

CHRONIC CONGESTIVE HEART FAILURE American Heart Association in collaboration with Sociedad Española de Cardiología date posted: March, 2003

Chronic Congestive Heart Failure Committee on Post Graduate Education, Council on Clinical Cardiology, American Heart Association Developed in collaboration with the Sociedad Española de Cardiología Prepared by: Ann F. Bolger, MD José López-Sendón, MD The content of these slides is current as of March 2003 Future revisions will be posted on the American Heart Association website (www. americanheart. org).

Chronic Congestive Heart Failure The Problem (USA) • 5, 000 patients • 6, 500, 000 hospital days / year • 300, 000 deaths / year • 6% - 10% of people > 65 years • 5. 4% of health care budget (38 billion) • Incidence x 2 in last ten years Gottdiener J et al. JACC 2000; 35: 1628 Haldeman GA et al. Am Heart J 1999; 137: 352 Kannel WB et al. Am Heart J 1991; 121: 951 O’Connell JB et al. J Heart Lung Transplant 1993; 13: S 107

Chronic Congestive Heart Failure Definition of heart failure Clinical syndrome that can result from any structural or functional cardiac disorder that impairs the ability of the ventricle to fill with or eject blood AHA / ACC HF guidelines 2001 Clinical symptoms / signs secondary to abnormal ventricular function ESC HF guidelines 2001

Chronic Congestive Heart Failure Suspected Heart Failure because of SYMPTOMS and/or SIGNS Assess presence of CARDIAC DISEASE by ECG, X-Ray or BNP (if available) NORMAL No Heart Failure Tests abnormal VENTRICULAR FUNCTION Imaging by ECHO-Doppler, NORMAL No Heart Failure Nuclear angiography or MRI if available Tests abnormal Heart Failure: Systolic / Diastolic Identify etiology, evaluate severity, choose therapy ESC HF guidelines 2001

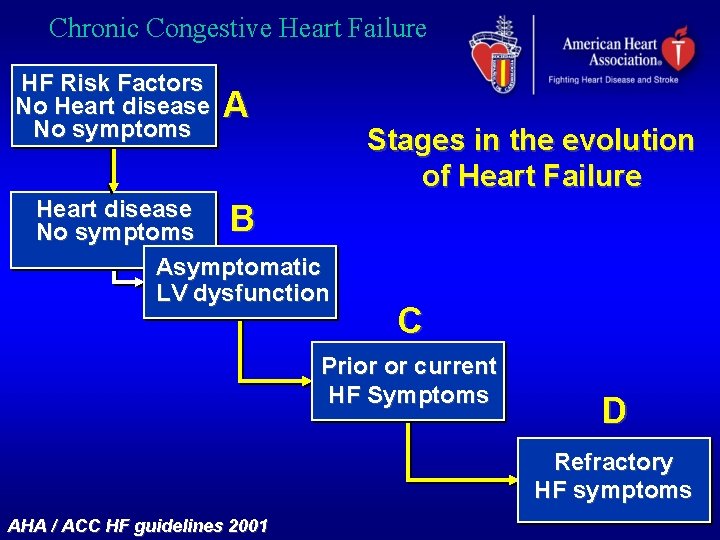
Chronic Congestive Heart Failure HF Risk Factors No Heart disease No symptoms A Stages in the evolution of Heart Failure Heart disease No symptoms B Asymptomatic LV dysfunction C Prior or current HF Symptoms D Refractory HF symptoms AHA / ACC HF guidelines 2001

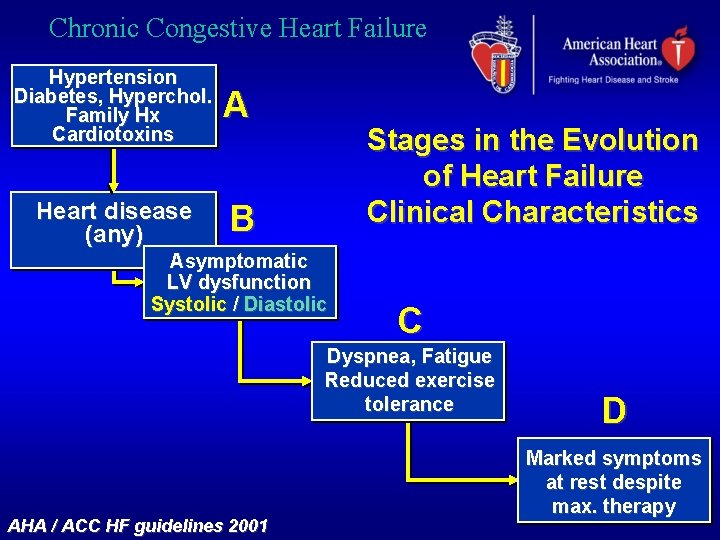
Chronic Congestive Heart Failure Hypertension Diabetes, Hyperchol. Family Hx Cardiotoxins A Heart disease (any) B Stages in the Evolution of Heart Failure Clinical Characteristics Asymptomatic LV dysfunction Systolic / Diastolic C Dyspnea, Fatigue Reduced exercise tolerance AHA / ACC HF guidelines 2001 D Marked symptoms at rest despite max. therapy

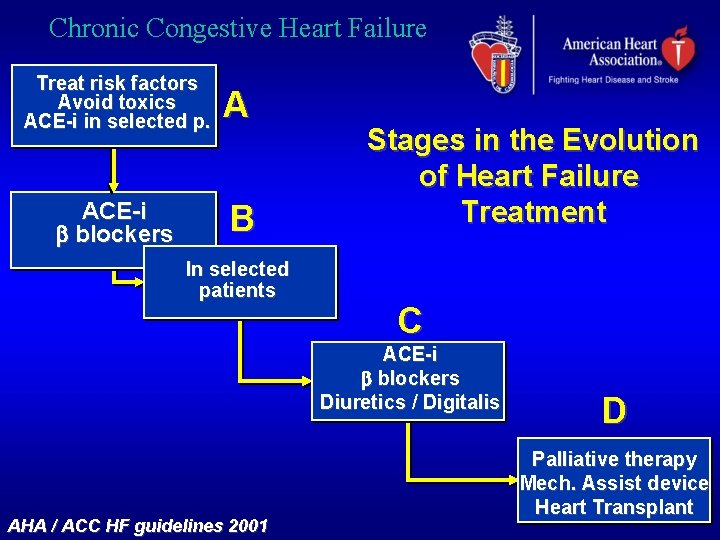
Chronic Congestive Heart Failure Treat risk factors Avoid toxics ACE-i in selected p. A ACE-i blockers B In selected patients Stages in the Evolution of Heart Failure Treatment C ACE-i blockers Diuretics / Digitalis AHA / ACC HF guidelines 2001 D Palliative therapy Mech. Assist device Heart Transplant

Chronic Congestive Heart Failure Incidence • n = 5888 • Age > 65 y • Follow-up 5. 5 y • 4 different locations in the US • INCIDENCE: 19. 3 / 1000 person-years The Cardiovascular Health Study Gottdiener J et al. JACC 2000; 35: 1628

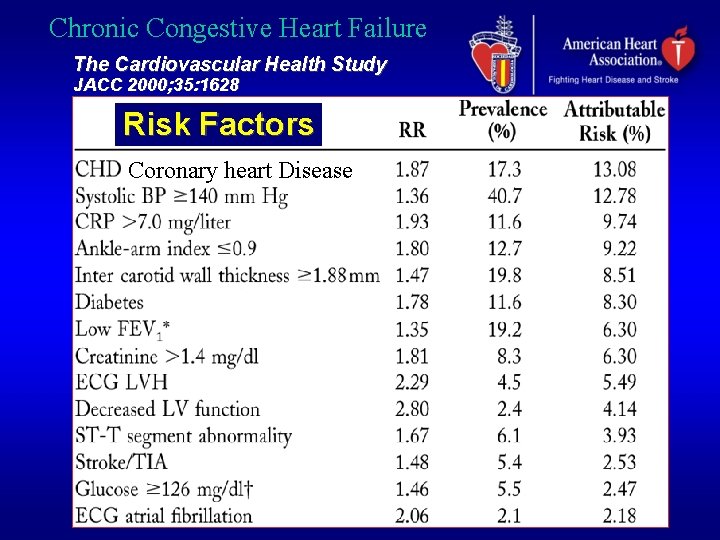
Chronic Congestive Heart Failure The Cardiovascular Health Study JACC 2000; 35: 1628 Risk Factors Coronary heart Disease

Chronic Congestive Heart Failure Direct Causes 1 - Myocardial abnormalities (CHD!) 2 - Hemodynamic overload 3 - Ventricular filling abnormalities 4 - Ventricular dyssynergy 5 - Changes in cardiac rhythm

Chronic Congestive Heart Failure Aggravating Factors • Medications • New heart disease • Myocardial ischemia • Pregnancy • Endocarditis • Arrhythmias (AF) • Obesity • Infections • Hypertension • Thromboembolism • Physical activity • Hyper/hypothyroidism • Dietary excess

Chronic Congestive Heart Failure Initial / Ongoing Evaluation • Identify heart disease • Assess functional capacity (NYHA, 6 min walk, …) • Assess volume status: (edema, rales, jugular, hepatomegaly, body weight) • Lab assessment: routine: electrolytes, renal funct. Repeat ECHO, RX only if significant changes in functional status • Assess prognosis

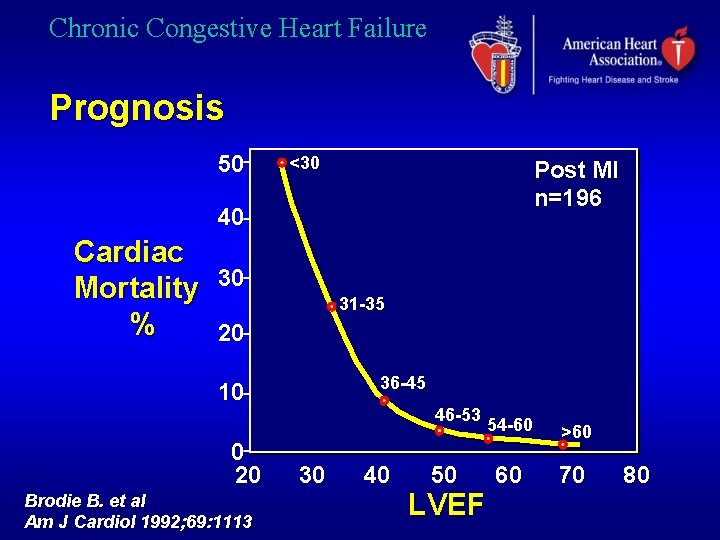
Chronic Congestive Heart Failure Prognosis 50 <30 Post MI n=196 40 Cardiac Mortality % 30 31 -35 20 36 -45 10 0 20 Brodie B. et al Am J Cardiol 1992; 69: 1113 46 -53 30 40 50 LVEF 54 -60 >60 60 70 80

Chronic Congestive Heart Failure Treatment Objectives Survival Morbidity Exercise capacity Quality of life Neurohormonal changes Progression of CHF Symptoms (Cost)

Chronic Congestive Heart Failure Treatment Selected patients • Prevention. Control of risk factors • Life style All • Treat etiologic cause / aggravating factors • Drug therapy • Personal care. Team work • Revascularization if ischemia causes HF • ICD (Implantable Cardiac Defibrillator) • Ventricular resyncronization • Ventricular assist devices • Heart transplant • Artificial heart • Neoangiogenesis, Gene therapy

Chronic Congestive Heart Failure Treatment Pharmacologic Therapy • Diuretics • ACE inhibitors • Beta Blockers • Digitalis • Spironolactone • Other

Chronic Congestive Heart Failure Diuretics • Essential to control symptoms secondary to fluid retention • Prevent progression from HT to HF • Spironolactone improves survival • New research in progress

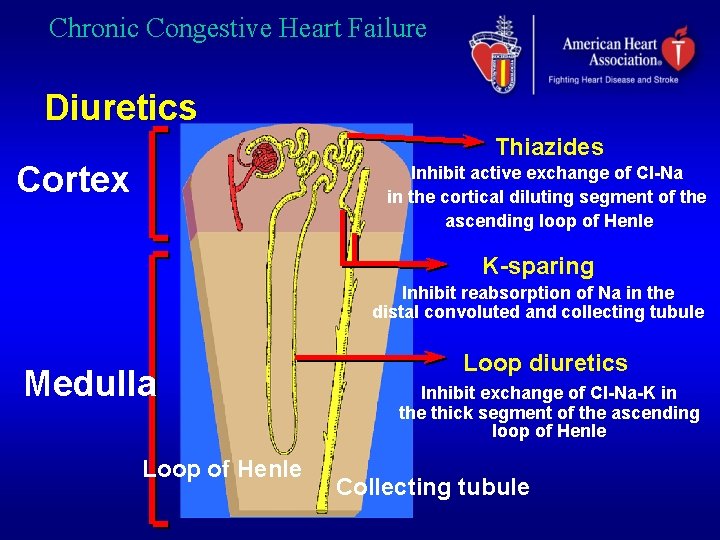
Chronic Congestive Heart Failure Diuretics Thiazides Cortex Inhibit active exchange of Cl-Na in the cortical diluting segment of the ascending loop of Henle K-sparing Inhibit reabsorption of Na in the distal convoluted and collecting tubule Medulla Loop of Henle Loop diuretics Inhibit exchange of Cl-Na-K in the thick segment of the ascending loop of Henle Collecting tubule

Chronic Congestive Heart Failure Diuretics. Indications 1. Symptomatic HF, with fluid retention • Edema • Dyspnea • Lung Rales • Jugular distension • Hepatomegaly • Pulmonary edema (Xray) AHA / ACC HF guidelines 2001 ESC HF guidelines 2001

Chronic Congestive Heart Failure Loop Diuretics / Thiazides. Practical Use • Start with variable dose. Titrate to achieve dry weight • Monitor serum K+ at “frequent intervals” • Reduce dose when fluid retention is controlled • Teach the patient when, how to change dose • Combine to overcome “resistance” • Do not use alone

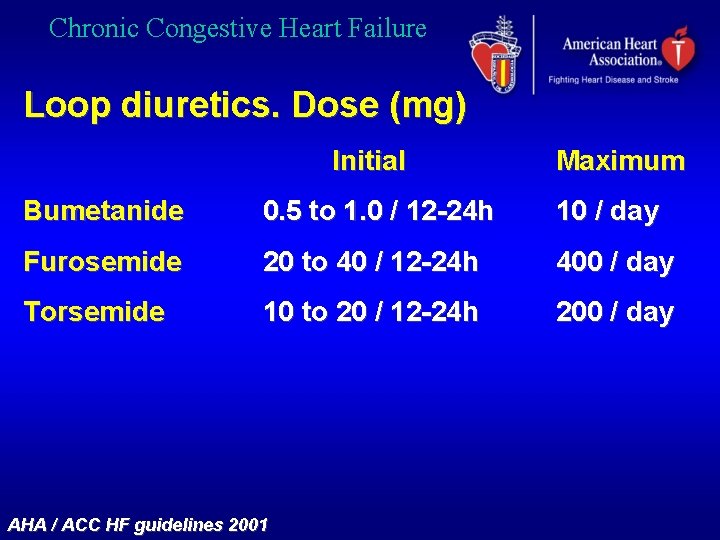
Chronic Congestive Heart Failure Loop diuretics. Dose (mg) Initial Maximum Bumetanide 0. 5 to 1. 0 / 12 -24 h 10 / day Furosemide 20 to 40 / 12 -24 h 400 / day Torsemide 10 to 20 / 12 -24 h 200 / day AHA / ACC HF guidelines 2001

Chronic Congestive Heart Failure Thiazides, Loop Diuretics. Adverse Effects • K+, Mg+ (15 - 60%) (sudden death ? ? ? ) • Na+ • Stimulation of neurohormonal activity • Hyperuricemia (15 - 40%) • Hypotension. Ototoxicity. Gastrointestinal. Alkalosis. Metabolic Sharpe N. Heart failure. Martin Dunitz 2000; 43 Kubo SH , et al. Am J Cardiol 1987; 60: 1322 MRFIT, JAMA 1982; 248: 1465 Pool Wilson. Heart failure. Churchill Livinston 1997; 635

Chronic Congestive Heart Failure Diuretic Resistance • Neurohormonal activation • Rebound Na+ uptake after volume loss • Hypertrophy of distal nephron • Reduced tubular secretion (renal failure, NSAIDs) • Decreased renal perfusion (low output) • Altered absortion of diuretic • Noncompliance with drugs Brater NEJM 1998; 339: 387 Kramer et al. Am J Med 1999; 106: 90

Chronic Congestive Heart Failure Managing Resistance to Diuretics • Restrict Na+/H 2 O intake (Monitor Natremia) • Increase dose (individual dose, frequency, i. v. ) • Combine: furosemide + thiazide / spiro / metolazone • Dopamine (increase cardiac output) • Reduce dose of ACE-i • Ultrafiltration Motwani et al Circulation 1992; 86: 439

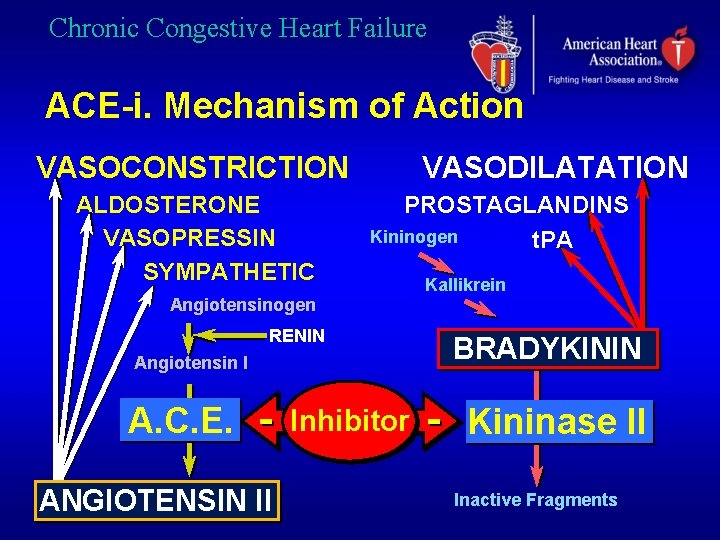
Chronic Congestive Heart Failure ACE-i. Mechanism of Action VASOCONSTRICTION ALDOSTERONE VASOPRESSIN SYMPATHETIC VASODILATATION PROSTAGLANDINS Kininogen t. PA Angiotensinogen RENIN Angiotensin I A. C. E. ANGIOTENSIN II Inhibitor Kallikrein BRADYKININ Kininase II Inactive Fragments

Chronic Congestive Heart Failure ACE-I. Clinical Effects • Improve symptoms • Reduce remodelling / progression • Reduce hospitalization • Improve survival

Chronic Congestive Heart Failure Mortality Reduction with ACE-i Study CONSENSUS SOLVD treatment AIRE Vheft-II TRACE SAVE ACE-i Enalapril Ramipril Enalapril Trandolapril Captopril Clinical Seting CHF CHF CHF / LVD SMILE HOPE Zofenopril Ramipril High risk

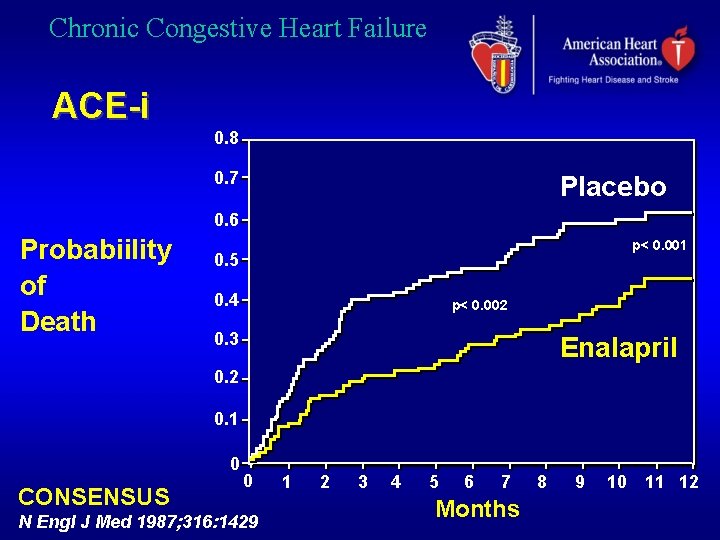
Chronic Congestive Heart Failure ACE-i 0. 8 0. 7 Placebo 0. 6 Probabiility of Death p< 0. 001 0. 5 0. 4 p< 0. 002 0. 3 Enalapril 0. 2 0. 1 0 CONSENSUS 0 N Engl J Med 1987; 316: 1429 1 2 3 4 5 6 7 Months 8 9 10 11 12

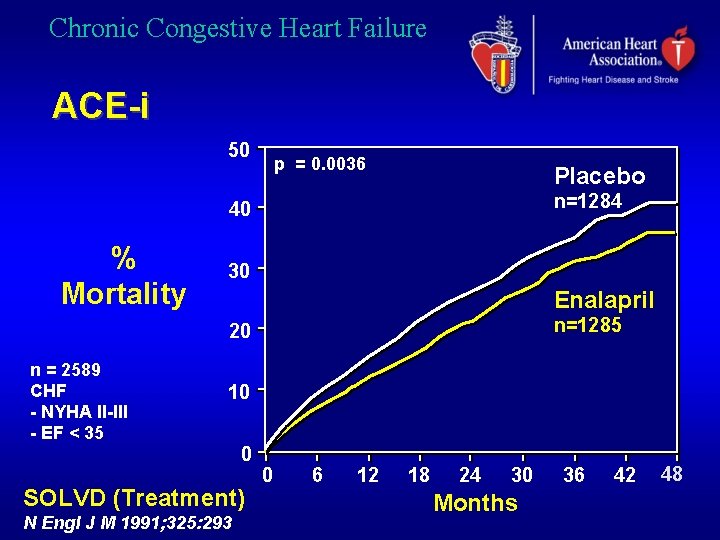
Chronic Congestive Heart Failure ACE-i 50 p = 0. 0036 Placebo n=1284 40 % Mortality 30 Enalapril n=1285 20 n = 2589 CHF - NYHA II-III - EF < 35 10 0 SOLVD (Treatment) N Engl J M 1991; 325: 293 0 6 12 18 24 30 Months 36 42 48

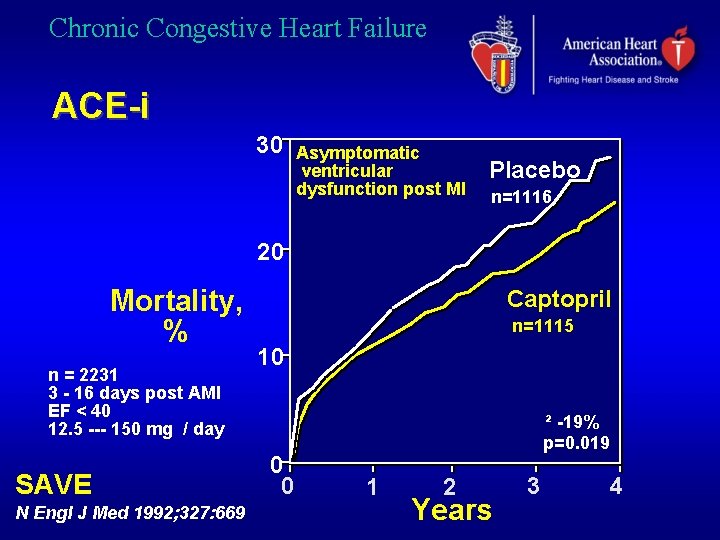
Chronic Congestive Heart Failure ACE-i 30 Asymptomatic ventricular dysfunction post MI Placebo n=1116 20 Mortality, % n = 2231 3 - 16 days post AMI EF < 40 12. 5 --- 150 mg / day SAVE N Engl J Med 1992; 327: 669 Captopril n=1115 10 0 0 ² -19% p=0. 019 1 2 Years 3 4

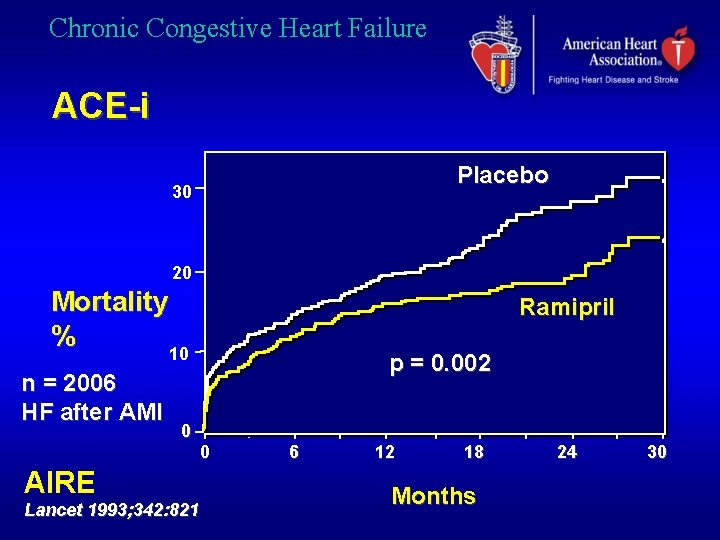
Chronic Congestive Heart Failure ACE-i Placebo 30 20 Mortality % 10 Ramipril 10 n = 2006 HF after AMI 0 p = 0. 002 0 AIRE Lancet 1993; 342: 821 6 12 18 Months 24 30

Chronic Congestive Heart Failure ACE-i. Indications • Symptomatic heart failure • Asymptomatic ventricular dysfunction - LVEF < 35 - 40 % • Selected high risk subgroups AHA / ACC HF guidelines 2001 ESC HF guidelines 2001

Chronic Congestive Heart Failure ACE-i. Practical Use • Start with very low dose • Increase dose if well tolerated • Renal function & serum K+ after 1 -2 w • Avoid fluid retention / hypovolemia (diuretic use) • Dose NOT determined by symptoms • Combine to overcome “resistance” • Do not use alone

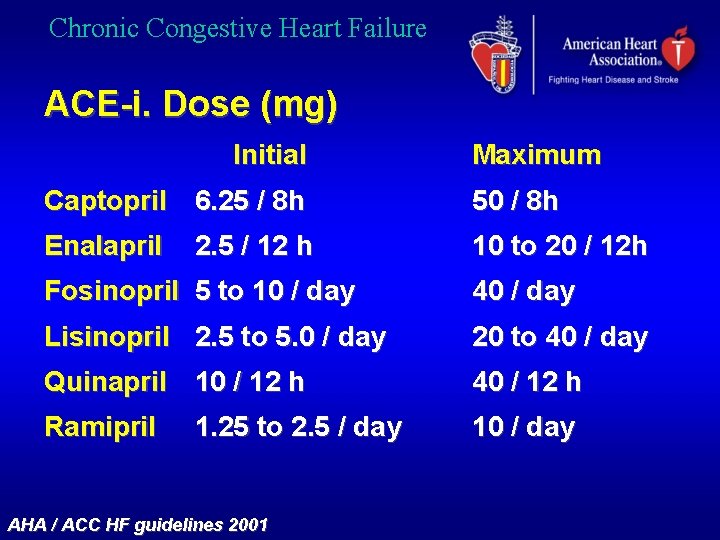
Chronic Congestive Heart Failure ACE-i. Dose (mg) Initial Maximum Captopril 6. 25 / 8 h 50 / 8 h Enalapril 10 to 20 / 12 h 2. 5 / 12 h Fosinopril 5 to 10 / day 40 / day Lisinopril 2. 5 to 5. 0 / day 20 to 40 / day Quinapril 10 / 12 h 40 / 12 h Ramipril 10 / day 1. 25 to 2. 5 / day AHA / ACC HF guidelines 2001

Chronic Congestive Heart Failure ACE-I. Adverse Effects • Hypotension (1 st dose effect) • Worsening renal function • Hyperkalemia • Cough • Angioedema • Rash, ageusia, neutropenia, …

Chronic Congestive Heart Failure ACE-I. Contraindications • Intolerance (angioedema, anuric renal fail. ) • Bilateral renal artery stenosis • Pregnancy • Renal insufficiency (creatinine > 3 mg/dl) • Hyperkalemia (> 5, 5 mmol/l) • Severe hypotension

Chronic Congestive Heart Failure ß-Adrenergic Blockers Mechanism of action • Density of ß 1 receptors • Inhibit cardiotoxicity of catecholamines • Neurohormonal activation • HR • Antiischemic • Antihypertensive • Antiarrhythmic • Antioxidant, Antiproliferative

Chronic Congestive Heart Failure ß-Adrenergic Blockers Clinical Effects • Improve symptoms (only long term) • Reduce remodelling / progression • Reduce hospitalization • Reduce sudden death • Improve survival

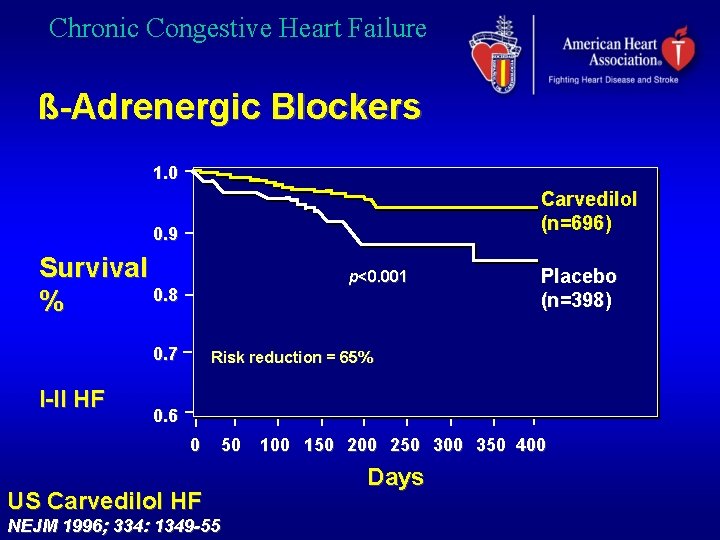
Chronic Congestive Heart Failure ß-Adrenergic Blockers 1. 0 Carvedilol (n=696) 0. 9 Survival 0. 8 % p<0. 001 0. 7 I-II HF Placebo (n=398) Risk reduction = 65% 0. 6 0 50 US Carvedilol HF NEJM 1996; 334: 1349 -55 100 150 200 250 300 350 400 Days

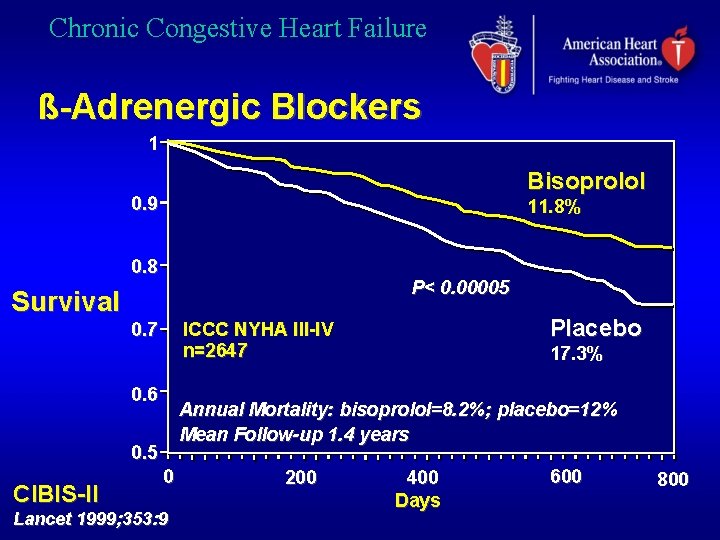
Chronic Congestive Heart Failure ß-Adrenergic Blockers 1 Bisoprolol 0. 9 11. 8% 0. 8 P< 0. 00005 Survival 0. 6 17. 3% Annual Mortality: bisoprolol=8. 2%; placebo=12% Mean Follow-up 1. 4 years 0. 5 CIBIS-II Placebo ICCC NYHA III-IV n=2647 0. 7 0 Lancet 1999; 353: 9 200 400 Days 600 800

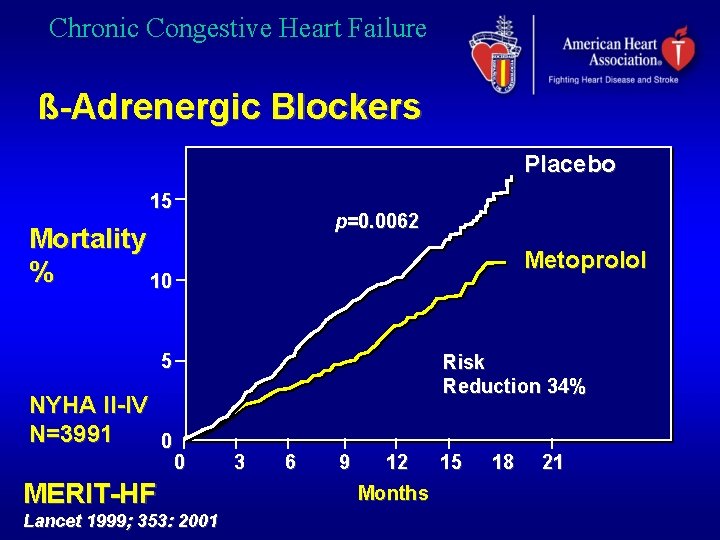
Chronic Congestive Heart Failure ß-Adrenergic Blockers Placebo 15 p=0. 0062 Mortality % 10 Metoprolol 5 NYHA II-IV N=3991 0 Risk Reduction 34% 0 MERIT-HF Lancet 1999; 353: 2001 3 6 9 12 Months 15 18 21

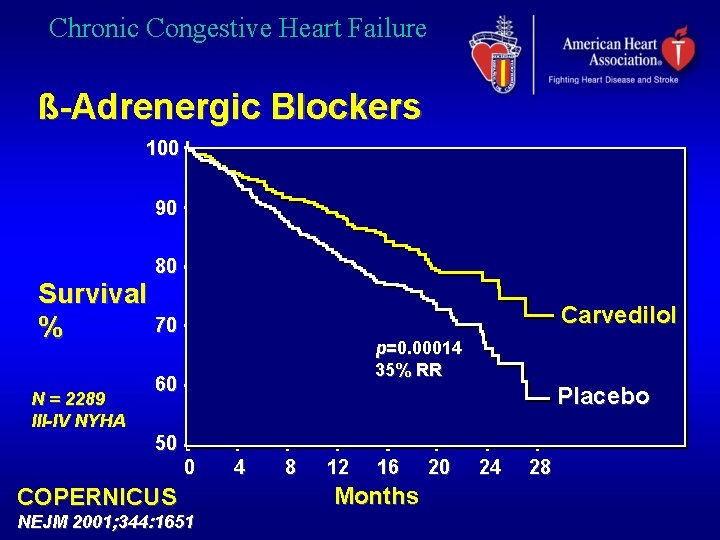
Chronic Congestive Heart Failure ß-Adrenergic Blockers 100 90 80 Survival 70 % N = 2289 III-IV NYHA Carvedilol p=0. 00014 35% RR 60 Placebo 50 0 COPERNICUS NEJM 2001; 344: 1651 4 8 12 16 Months 20 24 28

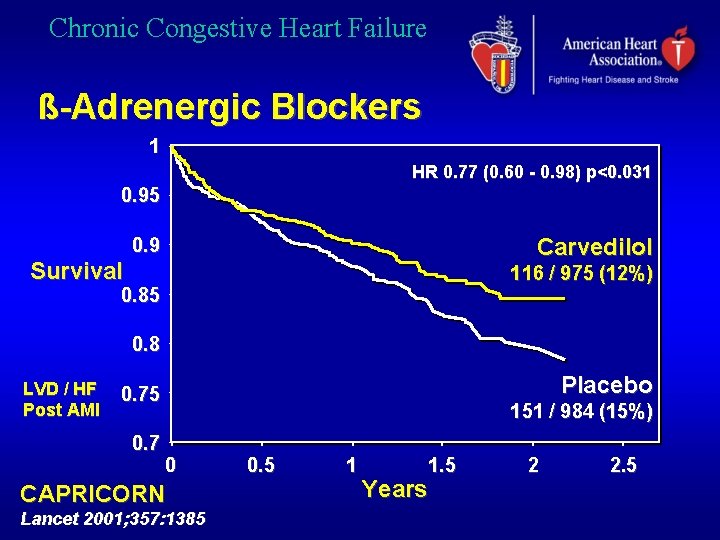
Chronic Congestive Heart Failure ß-Adrenergic Blockers 1 HR 0. 77 (0. 60 - 0. 98) p<0. 031 0. 95 Carvedilol 0. 9 Survival 116 / 975 (12%) 0. 85 0. 8 LVD / HF Post AMI Placebo 0. 75 0. 7 151 / 984 (15%) 0 CAPRICORN Lancet 2001; 357: 1385 0. 5 1 1. 5 Years 2 2. 5

Chronic Congestive Heart Failure ß-Adrenergic Blockers Indications • Symptomatic heart failure • Asymptomatic ventricular dysfunction - LVEF < 35 - 40 % • After AMI AHA / ACC HF guidelines 2001 ESC HF guidelines 2001

Chronic Congestive Heart Failure ß-Adrenergic Blockers When to start • Patient stable • No physical evidence of fluid retention • No need for i. v. inotropic drugs • Start ACE-I / diuretic first • No contraindications • In hospital or not

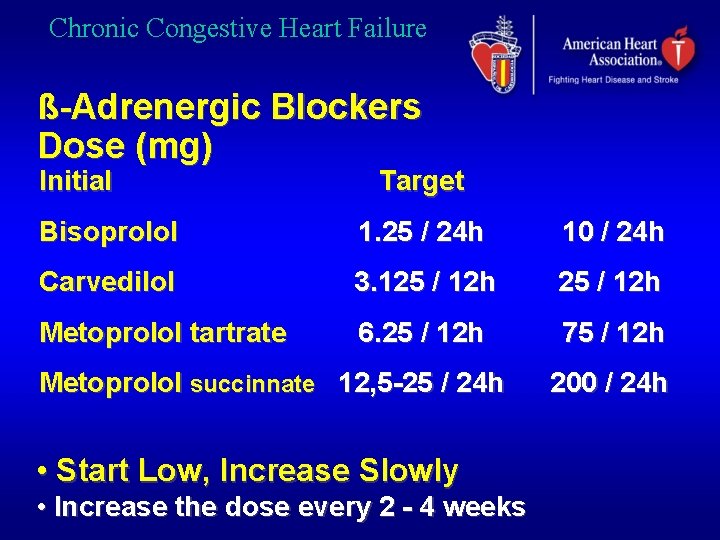
Chronic Congestive Heart Failure ß-Adrenergic Blockers Dose (mg) Initial Target Bisoprolol 1. 25 / 24 h 10 / 24 h Carvedilol 3. 125 / 12 h Metoprolol tartrate 6. 25 / 12 h 75 / 12 h Metoprolol succinnate 12, 5 -25 / 24 h • Start Low, Increase Slowly • Increase the dose every 2 - 4 weeks 200 / 24 h

Chronic Congestive Heart Failure ß-Adrenergic Blockers Adverse Effects • Hypotension • Fluid retention / worsening heart failure • Fatigue • Bradycardia / heart block • Review treatment (+/-diuretics, other drugs) • Reduce dose • Consider cardiac pacing • Discontinue beta blocker only in severe cases

Chronic Congestive Heart Failure ß-Adrenergic Blockers Contraindications • Asthma (reactive airway disease) • AV block (unless pacemaker) • Symptomatic hypotension / Bradycardia • Diabetes is NOT a contraindication

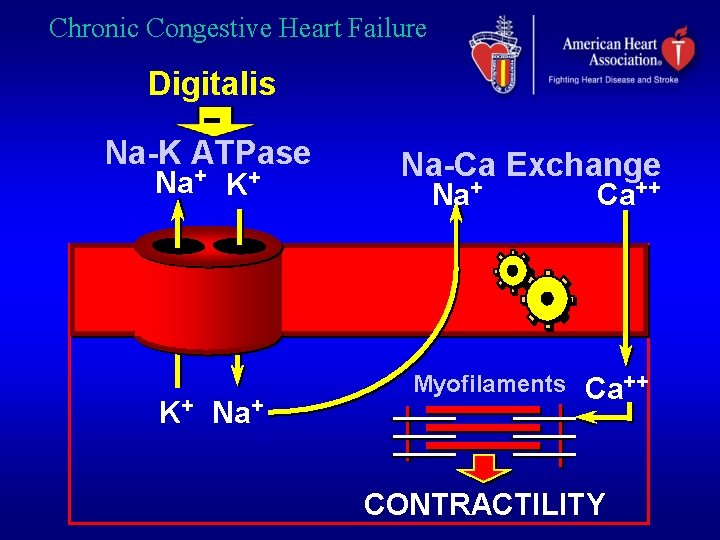
Chronic Congestive Heart Failure Digitalis Na-K ATPase Na+ K+ K+ Na-Ca Exchange Na+ Myofilaments Ca++ CONTRACTILITY

Chronic Congestive Heart Failure Digitalis. Mechanism of Action Blocks Na+ / K+ ATPase => Ca+ + • Inotropic effect • Natriuresis • Neurohormonal control - Plasma Noradrenaline - Peripheral nervous system activity - RAAS activity - Vagal tone - Normalizes arterial baroreceptors NEJM 1988; 318: 358

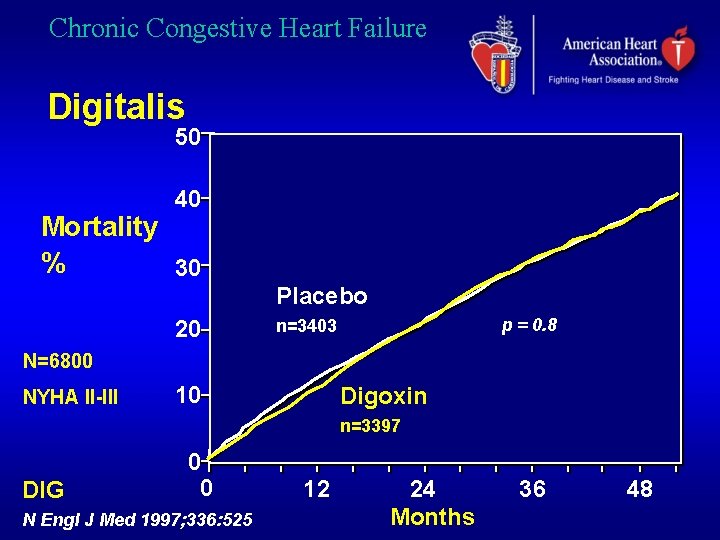
Chronic Congestive Heart Failure Digitalis. Clinical Effects • Improve symptoms • Modest reduction in hospitalization • Does not improve survival

Chronic Congestive Heart Failure Digitalis 50 40 Mortality % 30 Placebo 20 p = 0. 8 n=3403 N=6800 NYHA II-III 10 Digoxin n=3397 DIG 0 0 N Engl J Med 1997; 336: 525 12 24 Months 36 48

Chronic Congestive Heart Failure Digitalis. Indications • When no adequate response to ACE-i + diuretics + beta-blockers AHA / ACC Guidelines 2001 • In combination with ACE-i + diuretics if persisting symptoms ESC Guidelines 2001 • AF, to slow AV conduction Dose 0. 125 to 0. 250 mg / day

Chronic Congestive Heart Failure Digoxin. Contraindications • Digoxin toxicity • Advanced A-V block without pacemaker • Bradycardia or sick sinus without PM • PVC’s and VT • Marked hypokalemia • W-P-W with atrial fibrillation

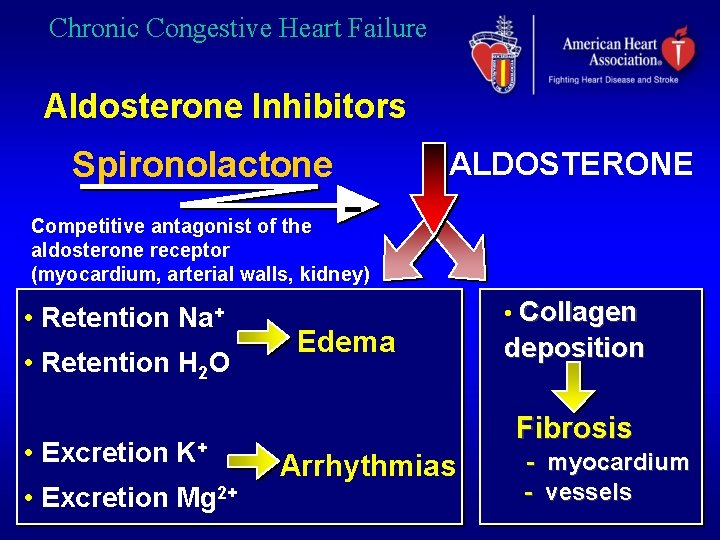
Chronic Congestive Heart Failure Aldosterone Inhibitors Spironolactone - ALDOSTERONE Competitive antagonist of the aldosterone receptor (myocardium, arterial walls, kidney) • Retention Na+ • Retention H 2 O • Excretion K+ • Excretion Mg 2+ Edema • Collagen deposition Fibrosis Arrhythmias - myocardium - vessels

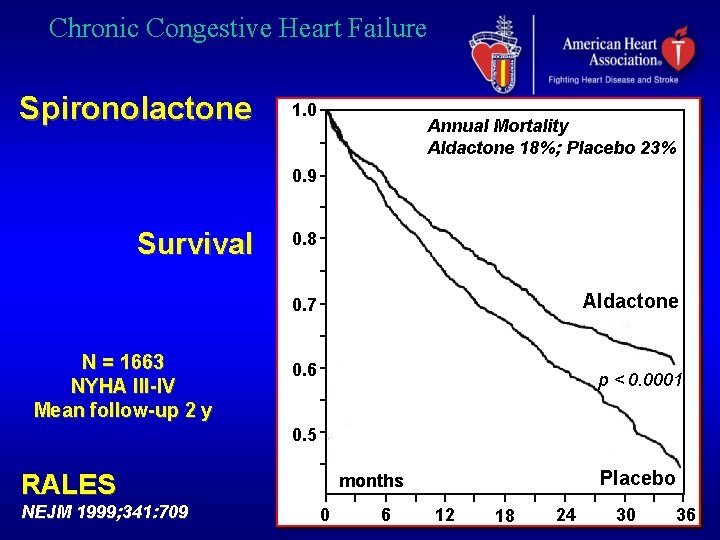
Chronic Congestive Heart Failure Spironolactone 1. 0 Annual Mortality Aldactone 18%; Placebo 23% 0. 9 Survival 0. 8 Aldactone 0. 7 N = 1663 NYHA III-IV Mean follow-up 2 y 0. 6 p < 0. 0001 0. 5 RALES NEJM 1999; 341: 709 Placebo months 0 6 12 18 24 30 36

Chronic Congestive Heart Failure Spironolactone. Indications • Recent or current symptoms despite ACE-i, diuretics, dig. and -blockers AHA / ACC HF guidelines 2001 • Recommended in advanced heart failure (III-IV), in addition to ACE-i and diuretics • Hypokalemia ESC HF guidelines 2001

Chronic Congestive Heart Failure Spironolactone. Practical use • Do not use if hyperkalemia, renal insuf. • Monitor serum K+ at “frequent intervals” • Start ACE-i first • Start with 25 mg / 24 h • If K+ >5. 5 mmol/L, reduce to 25 mg / 48 h • If K+ is low or stable consider 50 mg / day New studies in progress

Chronic Congestive Heart Failure Other Drugs. (only in selected patients) • Inotropics: refractory HF • Nitrates: ischemia, angina, pulmonary congestion • ARB: Contraindications to ACE-i • Antiarrhythmics: (only amiodarone) H risk arrhyth. • Anticoagulants: High risk of embolysm • Ca channel blockers: (only amlodipine) ischemia

Chronic Congestive Heart Failure Angiotensin II Receptor Blockers (ARB) RENIN Angiotensinogen Other pathways AT 1 Receptor Blockers AT 1 Vasoconstriction Angiotensin I ACE ANGIOTENSIN II RECEPTORS Proliferative Action AT 2 Vasodilatation Antiproliferative Action

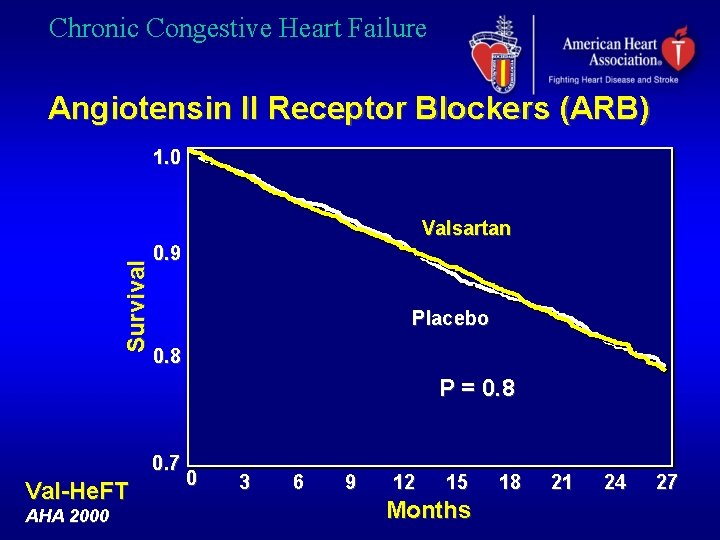
Chronic Congestive Heart Failure Angiotensin II Receptor Blockers (ARB) • Candesartan, Eprosartan, Irbesartan Losartan, Telmisartan, Valsartan • Efficacy not equal / superior to ACE-I • Not indicated with beta blockers • Indicated in patients intolerant to ACE-I AHA / ACC HF guidelines 2001 ESC HF guidelines 2001

Chronic Congestive Heart Failure Angiotensin II Receptor Blockers (ARB) 1. 0 Survival Valsartan 0. 9 Placebo 0. 8 P = 0. 8 0. 7 Val-He. FT AHA 2000 0 3 6 9 12 15 Months 18 21 24 27

Chronic Congestive Heart Failure Vasodilators VENOUS Nitrates Molsidomine MIXED Venous Vasodilatation Calcium antagonists a-adrenergic Blockers ACE-I, ARBs K+ channel activators Nitroprusside Arterial Vasodilatation ARTERIAL Minoxidil Hydralazine

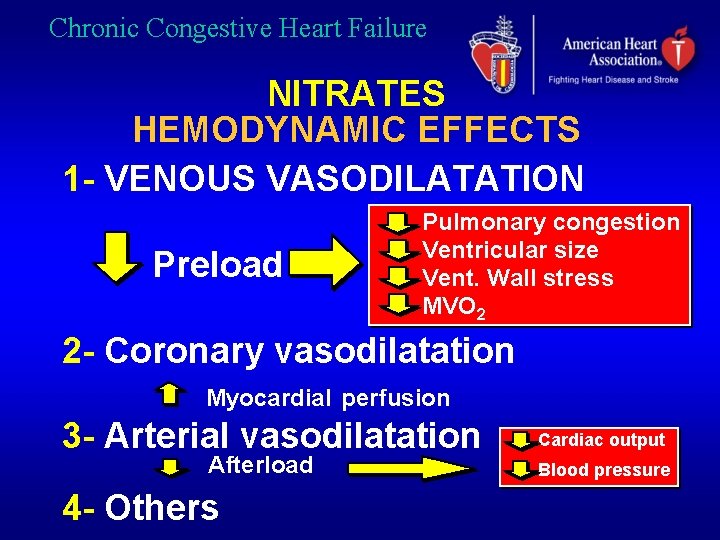
Chronic Congestive Heart Failure NITRATES HEMODYNAMIC EFFECTS 1 - VENOUS VASODILATATION Preload Pulmonary congestion Ventricular size Vent. Wall stress MVO 2 2 - Coronary vasodilatation Myocardial perfusion 3 - Arterial vasodilatation Afterload 4 - Others • Cardiac output • Blood pressure

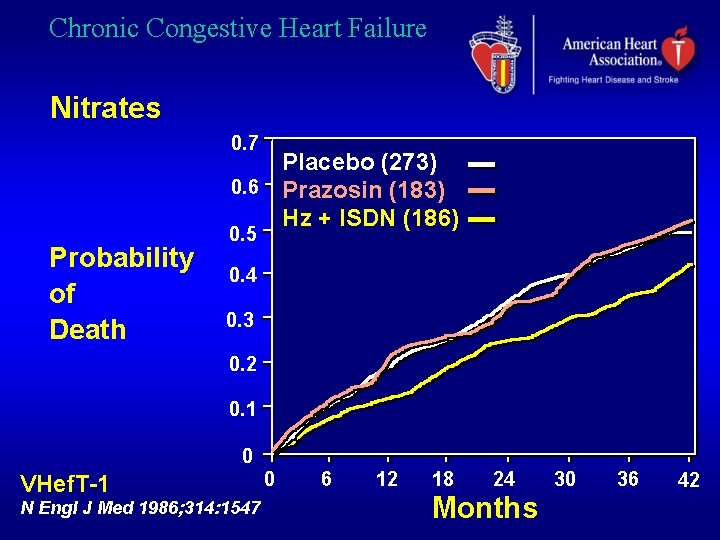
Chronic Congestive Heart Failure Nitrates 0. 7 Placebo (273) 0. 6 Prazosin (183) Hz + ISDN (186) Probability of Death 0. 5 0. 4 0. 3 0. 2 0. 1 0 VHef. T-1 N Engl J Med 1986; 314: 1547 0 6 12 18 24 Months 30 36 42

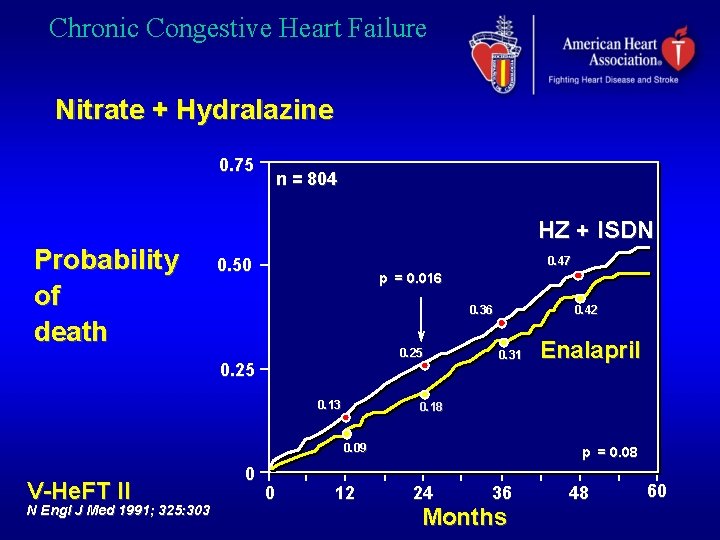
Chronic Congestive Heart Failure Nitrate + Hydralazine 0. 75 n = 804 HZ + 0, 54 ISDN Probability of death 0. 47 0. 50 p = 0. 016 0, 48 0. 36 0. 25 0. 13 0. 42 0. 31 0. 18 0. 09 V-He. FT II N Engl J Med 1991; 325: 303 0 0 Enalapril 12 p = 0. 08 24 36 Months 48 60

Chronic Congestive Heart Failure Nitrates. Clinical Use • CHF with myocardial ischemia • Orthopnea and paroxysmal nocturnal dyspnea • In acute CHF and pulmonary edema: NTG sl / iv • Nitrates + Hydralazine in intolerance to ACE-I (hypotension, renal insufficiency)

Chronic Congestive Heart Failure Positive Inotropes • Digitalis • Sympathomimetics • Catecholamines • B-adrenergic agonists • Phosphodiesterase inhibitors • Amrinone, Milrinone, Enoximone • Calcium sensitizers • Levosimendan, Pimobendan

Chronic Congestive Heart Failure Positive Inotropic Therapy • May increase mortality Exception: Digoxin, Levosimendan • Use only in refractory CHF • NOT for use as chronic therapy

Chronic Congestive Heart Failure Drugs to Avoid (may increase symptoms, mortality) • Inotropes, long term / intermittent • Antiarrhythmics (except amiodarone) • Calcium antagonists (except amlodipine) • Non-steroidal antiinflammatory drugs (NSAIDS) • Tricyclic antidepressants • Corticosteroids • Lithium ESC HF guidelines 2001

Chronic Congestive Heart Failure NEW DRUGS (ongoing research) 1. New neurohormonal modulators 2. New inotropics 3. Gene therapy 4. Myocyte transplant and mitosis 5. Neoangiogenesis / Growth factors

Chronic Congestive Heart Failure New Drugs (ongoing research) 1. New neurohormonal modulators • Beta-blockers • Aldosterone receptor antagonists • Angiotensin II receptor antagonists • Endothelin inhibitors • Vasopresin inhibitors • Natriuretic Peptides • Endopeptidase inhibitors • Vasopeptidase inhibitors

Chronic Congestive Heart Failure Other Drugs (ongoing research) • Erythropoietin • Ranolazine • Matrix metalloproteinases • Growth Hormone • L-Thyroxine • Inhibitors of carnitine palmitoyltransferse-I • Dopamine- -hyydroxylase inhibitors • Antithrombotics

Chronic Congestive Heart Failure Refractory End-Stage HF • Review etiology, treatment & aggrav. factors • Control fluid retention • Resistance to diuretics • Ultrafiltration ? • iv inotropics / vasodilators during decompensation • Consider resynchronization • Consider mechanical assist devices • Consider heart transplantation

Chronic Congestive Heart Failure Heart Transplant. Indications • Refractory cardiogenic shock • Documented dependence on IV inotropic support to maintain adequate organ perfusion • Peak VO 2 < 10 ml / kg / min • Severe symptoms of ischemia not amenable to revascularization • Recurrent symptomatic ventricular arrhythmias refractory to all therapeutic modalities Contraindications: age, severe comorbidity

Chronic Congestive Heart Failure and Myocardial Ischemia • Coronary HD is the cause of 2/3 of HF • Segmental wall motion abnormalities are not specific if ischemia • Angina coronary angio and revascularization • No angina • Search for ischemia and viability in all ? • Coronary angiography in all ?

Chronic Congestive Heart Failure Supraventricular Arrhythmias • Risk of embolization (AF) • Anticoagulation in AF • Systolic & diastolic dysfunction • Digoxin, beta blockers • Amiodarone if b-blocker ineffective/ contraind. • Conversion to sinus rhythm in all ? ongoing research

Chronic Congestive Heart Failure Ventricular Arrhythmias / Sudden Death • Antiarrhythmics ineffective (may increase mortality) Amiodarone do not improve survival • -blockers reduce all cause mortality and SD • Control ischemia • Control electrolyte disturbances • ICD (Implantable Cardiac Defibrillator) • In secondary prevention of SD • In sustained, hemodynamic destabilizing VT • Ongoing research will establish new indications

Chronic Congestive Heart Failure Diastolic Heart Failure • Incorrect diagnosis of HF • Inaccurate measurement of LVEF • Primary valvular disease • Restrictive (infiltrative) cardiomyopathies (Amyloidosis…) • Pericardial constriction • Episodic or reversible LV systolic dysfunction • Severe hypertension, ischemia • High output states: Anemia, thyrotoxicosis, etc • Chronic pulmonary disease with right HF • Pulmonary hypertension • Atrial myxoma • LV Hypertrophy • Diastolic dysfunction of uncertain origin

Chronic Congestive Heart Failure Diastolic Heart Failure • Treat as HF with low LVEF • Control: • Hypertension • Tachycardia • Fluid retention • Myocardial ischemia • Ongoing research

Chronic Congestive Heart Failure HEART FAILURE MODELS CONGESTIVE - Digoxin, Diurétics HEMODYNAMIC - Vasodilators NEUROHUMORAL - ACE inhibitors, - Blockers, Spironolactone IMMUNOLOGICAL - Cytokine inhibitors

Chronic Congestive Heart Failure TREATMENT STRATEGIES Diuretics Vasodilators Inotropics Neurohumoral activation ACE-is, -blockers Spironolatone ARBs? , ANP? ET-1? Gene therapy? Symptom relief Prevention of disease progression Anti-remodeling Reversal strategies of HF Mann. Circulation 1999; 100: 999 -1008

Chronic Congestive Heart Failure AHA / ACC Recommendations for the Evaluation of Patients Class I 1. Thorough history and physical examination 2. Patient’s ability to perform desired activities 3. Volume status (fluid retention, edema) 4. Lab: blood count, electrolytes, creatinine, glucose, … 5. Initial 12 -lead ECG and chest radiograph 7. Initial 2 -D ECHO or radionuclide ventriculography to assess left ventricular systolic function 8. Coronary arteriography in patients with angina AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for the Evaluation of Patients Class III 1. Routine endomyocardial biopsy 2. Routine Holter monitoring or signal-averaged electrocardiography. 3. Repeat coronary arteriography or noninvasive testing for ischemia in patients with already excluded coronary artery disease 4. Routine measurement of norepinephrine or endothelin AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Patients at High Risk of Developing HF (Stage A) Class I 1. Control of systolic and diastolic hypertension 2. Treatment of lipid disorders 3. Control other risk factors (e. g. , smoking, alcohol, drugs) 4. ACE inhibition in patients with a history of atherosclerotic vascular disease, diabetes mellitus, or hypertension 5. Control of ventricular rate in supraventricular arrhythmias 6. Treatment of thyroid disorders 7. Periodic evaluation for signs and symptoms of HF AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Patients at High Risk of Developing HF (Stage A) Class IIa 1. Noninvasive evaluation of left ventricular function in patients with a strong family history of cardiomyopathy or in those receiving cardiotoxic interventions Class III 1. Exercise to prevent the development of HF 2. Reduction of dietary salt beyond that which is prudent 3. Routine testing to detect left ventricular dysfunction 4. Routine use of nutritional supplements AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Patients With Asymptomatic Left Ventricular Systolic Dysfunction (Stage B) Class I 1. ACE inhibition in patients with previous AMI 2. ACE inhibition in patients with a reduced LVEF 3. Beta-blockade in patients with a recent AMI 4. Beta-blockade in patients with a reduced LVEF 5. Valve repair for significant valvular stenosis / regurgitation 6. Regular evaluation for signs and symptoms of HF 7. Also Class I recommendations for patients in Stage A AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Patients With Asymptomatic Left Ventricular Systolic Dysfunction (Stage B) Class IIb 1. Systemic vasodilators in severe aortic regurgitation Class III 1. Digoxin in patients in sinus rhythm 2. Reduction of dietary salt beyond that which is prudent 3. Exercise to prevent the development of HF 4. Routine use of nutritional supplements AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Treatment of Symptomatic Left Ventricular Systolic Dysfunction (Stage C) Class I 1. Diuretics in patients with fluid retention. 2. ACE inhibition in all patients 3. Beta-blockers in all stable patients 4. Digitalis for the treatment of symptoms of HF 5. Withdrawal of drugs adversely affecting clin. status (most antiarrhythmics, most calcium channel blockers, nonsteroidal anti-inflammatory drugs, …) AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Treatment of Symptomatic Left Ventricular Systolic Dysfunction (Stage C) Class IIa 1. Spironolactone in patients with recent or current Class IV symptoms 2. Exercise training to improve clinical status 3. Angiotensin receptor blockade in patients who cannot be given ACE-I because of cough or angioedema 4. Hydralazine and a nitrate in patients who cannot be given ACE-i because of hypotension or renal insufficiency AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Treatment of Symptomatic Left Ventricular Systolic Dysfunction (Stage C) Class IIb 1. Addition of angiotensin receptor blocker to ACE-i 2. Addition of a nitrate to ACE-I in patients Class III 1. Long-term intermittent use inotropics infusion 2. Use of angiotensin blocker instead of ACE-i 3. Use of angiotensin blocker before a beta-blocker 4. Use of Ca channel blocker for HF 5. Routine use of nutritional supplements AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Patients With Refractory End-Stage HF (Stage D) Class I 1. Meticulous identification and control of fluid retention 2. Referral for cardiac transplantation in eligible patients 3. Referral to an HF program 4. Other class I recommendations for Stages A, B, and C AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841

Chronic Congestive Heart Failure AHA / ACC Recommendations for Patients With Refractory End-Stage HF (Stage D) Class IIb 1. Pulmonary artery catheter to guide therapy 2. Mitral valve repair for severe secondary mitral regurg. 3. Continuous infusion of inotropics for symptoms Class III 1. Partial left ventriculectomy 2. Routine intermittent infusions of inotropics AHA / ACC HF guidelines 2001 http: //www. americanheart. org/presenter. jhtml? identifier=11841