Choosing the best feeds for preterm infants evidence

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews Roger F. Soll, MD H. Wallace Professor of Neonatology Larner College of Medicine, University of Vermont Coordinating Editor, Cochrane Neonatal President, Vermont Oxford Network Trusted evidence. Informed decisions. Better health. 1

Editorial Team Roger F. Soll Coordinating Editor Bill Mc. Guire Hull York Medical School Coordinating Editor Colleen Ovelman Managing Editor Caitlin O’Connell Assistant Managing Editor

Editorial Team Michael Bracken Yale University Jeffrey Horbar University of Vermont Jackie Ho Penang Medical College Prakeshkumar Shah University of Toronto Lisa Askie University of Sydney Gautham Suresh Baylor University David Osborn University of Sydney

Associate Editors 4

Guest Discussants Heather C. Kaplan, MD, MSCE Associate Professor, University of Cincinnati Department of Pediatrics Brenda Poindexter, MD, MS Professor, University of Cincinnati Department of Pediatrics

Sponsors Section on Neonatal-Perinatal Medicine

Sponsors Cochrane Neonatal received unrestricted grant support to update reviews on feeding preterm infants from the Gerber Foundation

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews Disclosure Roger F. Soll, M. D. is the President of the Vermont Oxford Network and the Coordinating Editor of Cochrane Neonatal No other relevant financial issues to disclose

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews To develop an understanding of the strengths and weaknesses of evidence provided by systematic reviews and meta-analyses to inform our practice of neonatal-perinatal medicine in specific reference to what we feed preterm infants.

The Evidence Hierarchy What evidence should I use to inform my practice?

Strategies for Feeding the Preterm Infant William W. Hay, Jr. Neonatology. 2008; 94(4): 245– 254. Published online 2008 Oct 2. doi: 10. 1159/000151643

What is the evidence to support feeding mother’s own breast milk to preterm babies? As a greater number of smaller and smaller preterm infants survive, caregivers have been called on to develop more effective nutritional strategies, including optimizing breast feeding, developing newer formulas, supplements to enteral feeds, and parenteral feeding solutions.

Goal of Nutrition for Preterm Infants Most neonatologists have accepted the recommendation of the American Academy of Pediatrics that growth of the postnatal preterm infant, both their anthropometric indices and body composition, should be the same as the normal fetus of the same gestational age growing in its mother’s uterus. . In reality, this proves to be a challenge…… American Academy of Pediatrics Committee on Nutrition: Nutritional needs of low-birth-weight infants. Pediatrics. 1985; 76: 976– 986.

What is the evidence to support feeding mother’s own breast milk to preterm babies? Reports from NICUs across the world demonstrate that we have considerable room for improvement. The growth of nearly all preterm infants during their hospitalization in intensive care, especially those at the earliest gestational ages, lag far behind fetal growth curves in the third trimester. In the Vermont Oxford Network database, 31% of VLBW infants have extreme growth failure, defined as being less than the 3 rd percentile on the Fenton Growth Chart at discharge. However, this failure in sustaining adequate growth varies greatly between centers (1 st quartile 20%, 3 rd quartile 40%).

What is the evidence to support feeding mother’s own breast milk to preterm babies? Hay notes that this same pattern of growth failure was observed over 60 years ago, indicating that despite major advances in neonatal medicine, strategies to provide adequate nutrition to preterm infants and achieve better rates of growth has not kept pace with other improvements in neonatal care and survival.

What is the evidence to support feeding mother’s own breast milk to preterm babies? Variation in practice A great deal of variation is seen in feeding practices worldwide. (Klingenberg and colleagues. Arch Dis Child 2012). Successful use of human milk, such that infants are receiving any human milk at time of discharge home occurs in an average of 57% of discharged VLBW infants with great variation between centers (1 st quartile 44. 4%, 3 rd quartile 73%). (VON database 2018)

What is the evidence to support feeding mother’s own breast milk to preterm babies? What is the underlying cause of growth failure in preterm infants? In his excellent review of “Strategies for feeding the preterm infant”, Hay notes that the main answer is the obvious answer; we have not fed infants enough protein and enough energy to meet the requirements for fetal growth. More aggressive parenteral and enteral feeding practices can ameliorate, but not completely address, these deficiencies.

What is the evidence to support feeding mother’s own breast milk to preterm babies? What are the downstream effects of undernutrition and growth failure? Numerous studies have shown that failure to meet the preterm infant’s nutritional goals at critical stages of development produces serious problems for the preterm infant, including: - short stature, - growth failure - abnormalities of brain growth and development.

What is the evidence to support feeding mother’s own breast milk to preterm babies? What is the importance of enteral nutrition? The aggressive use of parenteral nutrition has ameliorated some of the gross nutritional deficiencies experienced by preterm infants but cannot meet all goals and is associated with many adverse consequences. Lack of enteral feeding leads to mucosal and villous atrophy and reduction of the enzymes necessary for digestion, substrate absorption, and growth. These underlying conditions contribute to serious diseases, such as necrotizing enterocolitis (NEC).

What is the evidence to support feeding mother’s own breast milk to preterm babies? What are the current gaps in caregiver knowledge and practice regarding early enteral nutrition for preterm infants? We have identified three key areas of gaps in preterm infant nutrition knowledge and practice for the proposed project: (1) types of feeding, (2) optimizing nutritional content of feeds, and (3) feeding strategies and methods.

So…. What do we know from trials?

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews 1. Formula versus maternal breast milk for feeding preterm or low birth weight infants 2. Formula versus donor breast milk for feeding preterm or low birth weight infants 3. Banked preterm versus banked term human milk to promote growth and development in very low birth weight infants 4. Nutrient-enriched formula versus standard formula for preterm infants 5. Dilute versus full strength formula in exclusively formula-fed preterm or low birth weight infants 6. Protein hydrolysate versus standard formula for preterm infants

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews Formula versus maternal breast milk for feeding preterm or low birth weight infants Brown JVE, Walsh V, Mc. Guire W. Cochrane Database of Systematic Reviews 2019, Issue 8. Art. No. : CD 002972. DOI: 10. 1002/14651858. CD 002972. pub 3.

What is the evidence to support feeding mother’s own breast milk to preterm babies? The “substrate” (type of feeding) matters greatly. Breast milk is the optimal enteral feed! Maternal breast milk is the recommended form of enteral nutrition for preterm or LBW infants (Agostoni 2010; AAP 2012; Cleminson 2015).

Formula versus maternal breast milk for feeding preterm or low birth weight infants Why might maternal breast milk be best? In addition to macro- and micro-nutrients that are optimized by evolution for digestion and absorption by human infants, maternal breast milk contains numerous 'immuno-nutrients' such as secretory immunoglobulin A (Ig. A), lactoferrin, cytokines, enzymes, growth factors, and leucocytes (Walsh 2019). An important benefit of maternal breast milk for preterm or LBW infants is that delivery of these immunological and growth factors to the immature intestinal mucosa promotes postnatal physiological, neuro-endocrinological, and metabolic adaptation (Jones 2007; Embleton 2017).

Formula versus maternal breast milk for feeding preterm or low birth weight infants Why might maternal breast milk be best? Evidence from observational studies suggests that feeding with maternal breast milk rather than formula is associated with a reduced risk of serious adverse outcomes including necrotizing enterocolitis and infection in very preterm and VLBW infants. Lucas A, Cole TJ. Breast milk and neonatal necrotizing enterocolitis. Lancet. 1990; 336: 1519– 1523. Schanler RJ, Shulman RJ, Lau C. Feeding strategies for premature infants: beneficial outcomes of feeding fortified human milk versus preterm formula. Pediatrics. 1999; 103: 1150– 1157. Sisk PM, Lovelady CA, Dillard RG, Gruber KJ, O’Shea TM. Early human milk feeding is associated with a lower risk of necrotizing enterocolitis in very low birth weight infants. J Perinatol. 2007; 27: 428– 433.

Formula versus maternal breast milk for feeding preterm or low birth weight infants Why might maternal breast milk NOT be the best feed for preterm infants? The nutritional requirements of preterm infants may not be met by enteral feeding with maternal breast milk alone (Agostoni 2010). Maternal breast milk varies in energy and protein content depending upon the stage of lactation at which it is collected, the duration of lactation, and the method of storage and delivery. Many of the processes involved in handling maternal breast milk, including refrigeration, freeze-thawing, and pasteurization, can reduce its macro-nutrient and immuno-nutrient content (Zachariassen 2013; Gidrewicz 2014).

Formula versus maternal breast milk for feeding preterm or low birth weight infants Supplementation of maternal breast milk with nutrient fortifiers (typically extracted from cow milk) is an option for increasing nutrient density (Klingenberg 2012; Tudehope 2013; Underwood 2013). Although this results in faster short-term growth, uncertainty remains about whether fortification using bovine milk extracts increases the risk of enteral feed intolerance or necrotizing enterocolitis in very preterm or VLBW infants (Brown 2016; Ellis 2019). To be discussed in future Cochrane seminars!

Formula versus maternal breast milk for feeding preterm or low birth weight infants What do we mean when we say “formula”? As an alternative to breast milk, a variety of artificial formulas (usually modified cow milk) for feeding preterm or LBW infants are available commercially (Agostoni 2010; Tudehope 2012). These vary in energy, protein and micro-nutrient content and, broadly, can be categorized as: - standard 'term' formulas; designed for term infants, based on the composition of mature breast milk ‒ the typical energy content is between about 67 and 70 k. Cal/100 m. L; - nutrient-enriched 'preterm' formulas; designed for preterm infants to provide nutrient intakes to match intra-uterine accretion rates ‒ these are energy-enriched (typically up to about 80 k. Cal/100 m. L) and are variably protein- and mineralenriched.

Formula versus maternal breast milk for feeding preterm or low birth weight infants What are the pros and cons of “preterm” formula? Artificial formula, particularly nutrient-enriched 'preterm' formula, might provide consistently higher levels of nutrients than maternal breast milk does. However, artificial formulas do not contain the same immuno-nutritional factors that are present in maternal breast milk (Tudehope 2012; Underwood 2013). Furthermore, although bovine proteins, carbohydrates and lipids in artificial formulas are modified to improve digestibility for newborn infants, these are less likely to be tolerated than human milk macronutrients, especially by the immature preterm intestine. Formula feeding might therefore delay the functional adaptation of the gastrointestinal tract and disrupt the patterns of microbial colonization (Embleton 2017).

Formula versus maternal breast milk for feeding preterm or low birth weight infants The disappointing truth… Objectives: To determine the effect of feeding preterm or LBW infants with formula compared with maternal breast milk on growth and developmental outcomes. Selection criteria: Randomized or quasi-randomized controlled trials that compared feeding preterm or low birth weight infants with formula versus maternal breast milk. Main results: We did not identify any eligible trials.

Formula versus maternal breast milk for feeding preterm or low birth weight infants Authors' conclusions: There are no trials of formula versus maternal breast milk for feeding preterm or low birth weight infants. Such trials are unlikely to be conducted because of the difficulty of allocating an alternative form of nutrition to an infant whose mother wishes to feed with her own breast milk. Maternal breast milk remains the default choice of enteral nutrition because observational studies and meta-analyses of trials comparing feeding with formula versus donor breast milk, suggest that feeding with breast milk has major immunonutritional advantages for preterm or low birth weight infants.

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews Formula versus donor breast milk for feeding preterm or low birth weight infants. Quigley M, Embleton ND, Mc. Guire W. Cochrane Database of Systematic Reviews 2019, Issue 7. Art. No. : CD 002971. DOI: 10. 1002/14651858. CD 002971. pub 5.

Formula versus donor breast milk for feeding preterm or low birth weight infants. What to do if breast milk is not available? Maternal breast milk is the recommended form of enteral nutrition for preterm or low birth weight (LBW) infants (AAP 2012). When sufficient maternal breast milk is not available, the two common alternatives available for feeding preterm or LBW infants are artificial formula and donor breast milk (donated by other lactating women). These may be given either as the sole form of enteral feeding or as a supplement to maternal breast milk (Klingenberg 2012).

Formula versus donor breast milk for feeding preterm or low birth weight infants. Artificial formulas (usually adapted from cow's milk) are available. - standard 'term' formula, designed for term infants based on the composition of mature breast milk; - nutrient-enriched 'preterm' formula, designed to provide nutrient intakes to match intrauterine accretion rates (Tsang 1993). Donor breast milk. Expressed breast milk from donor mothers, usually mothers who have delivered at term, generally has a lower content of energy and protein than term formula milk (Gross 1980; Gross 1981). The macronutrient content of donor breast milk is not compromised substantially by modern pasteurization methods but levels of immunoactive components might be reduced (Peila 2016; Castro 2019). Donor human milk also varies regarding fat, energy and protein content, depending upon the stage of lactation at which it is collected.

Formula versus donor breast milk for feeding preterm or low birth weight infants. The pros and cons of donor breast milk The nutritional requirements of preterm or LBW infants may not be fully met by enteral feeding with donor breast milk (Hay 1994; Schanler 1995). These deficiencies may have adverse consequences for growth and development. However, a major putative benefit of donor breast milk is that the delivery of immunoprotective and growth factors to the immature gut mucosa may prevent serious adverse outcomes, including necrotizing enterocolitis and invasive infection (Lucas 1990; Beeby 1992).

Formula versus donor breast milk for feeding preterm or low birth weight infants. Main results Twelve trials with a total of 1879 infants fulfilled the inclusion criteria. Four trials compared standard term formula versus donor breast milk and eight compared nutrient-enriched preterm formula versus donor breast milk. Only the five most recent trials used nutrient-fortified donor breast milk. The trials contain various weaknesses in methodological quality, specifically concerns about allocation concealment in four trials and lack of blinding in most of the trials. Most of the included trials were funded by companies that made the study formula.
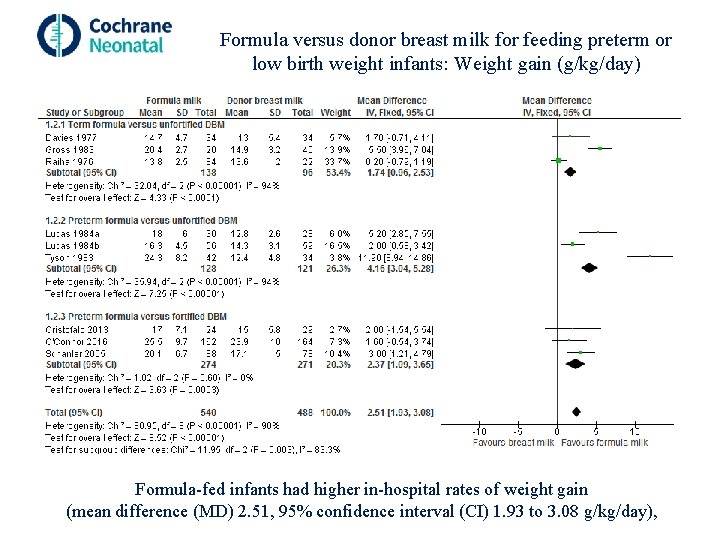
Formula versus donor breast milk for feeding preterm or low birth weight infants: Weight gain (g/kg/day) Formula-fed infants had higher in-hospital rates of weight gain (mean difference (MD) 2. 51, 95% confidence interval (CI) 1. 93 to 3. 08 g/kg/day),
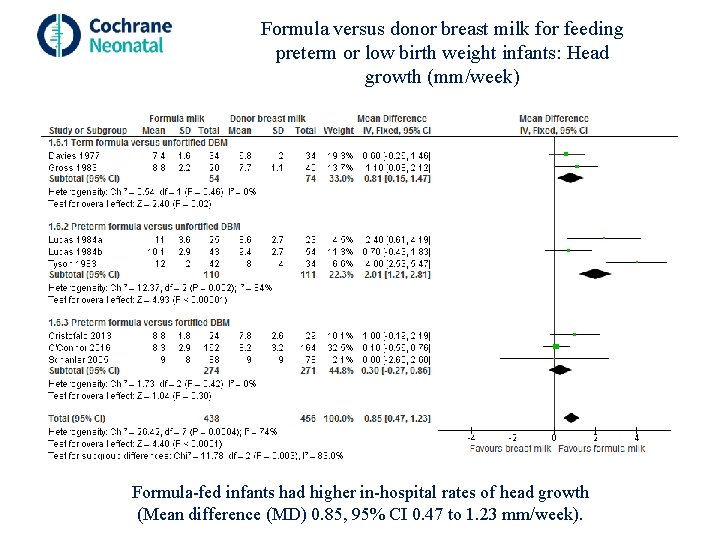
Formula versus donor breast milk for feeding preterm or low birth weight infants: Head growth (mm/week) Formula-fed infants had higher in-hospital rates of head growth (Mean difference (MD) 0. 85, 95% CI 0. 47 to 1. 23 mm/week).
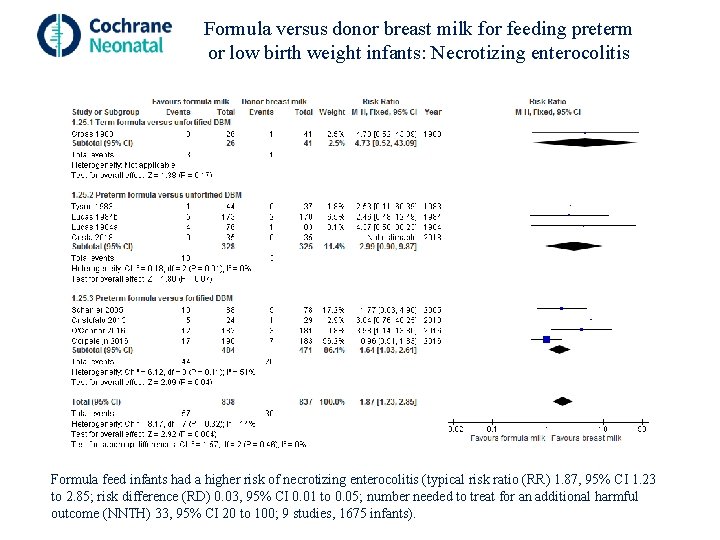
Formula versus donor breast milk for feeding preterm or low birth weight infants: Necrotizing enterocolitis Formula feed infants had a higher risk of necrotizing enterocolitis (typical risk ratio (RR) 1. 87, 95% CI 1. 23 to 2. 85; risk difference (RD) 0. 03, 95% CI 0. 01 to 0. 05; number needed to treat for an additional harmful outcome (NNTH) 33, 95% CI 20 to 100; 9 studies, 1675 infants).

Formula versus donor breast milk for feeding preterm or low birth weight infants. Subgroup analysis: Formula versus donated breast milk (DBM) given as (i) sole diet or (ii) a supplement to maternal expressed breast milk
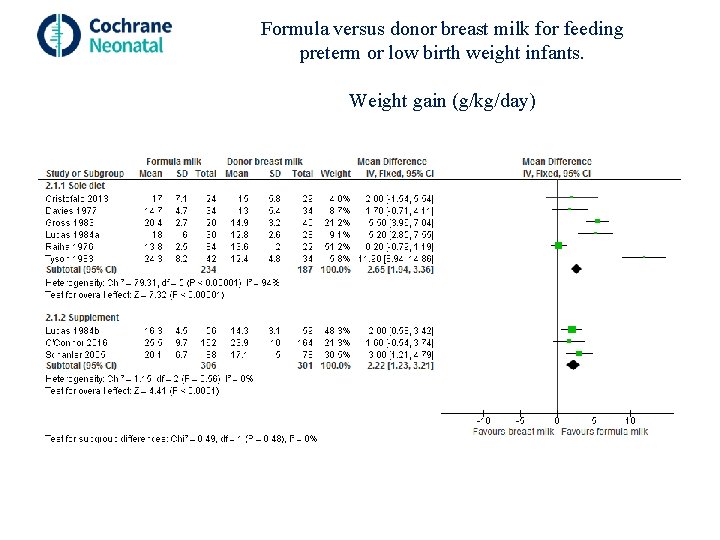
Formula versus donor breast milk for feeding preterm or low birth weight infants. Weight gain (g/kg/day)
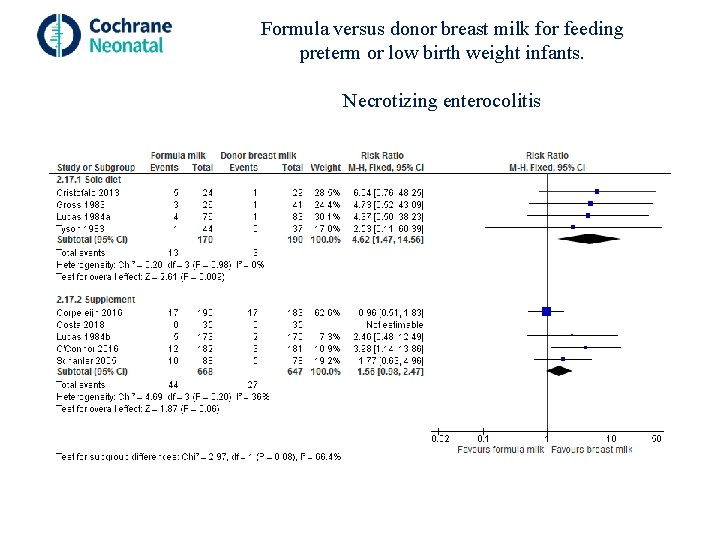
Formula versus donor breast milk for feeding preterm or low birth weight infants. Necrotizing enterocolitis

Formula versus donor breast milk for feeding preterm or low birth weight infants. Authors' conclusions In preterm and LBW infants, moderate-certainty evidence indicates that feeding with formula compared with donor breast milk, either as a supplement to maternal expressed breast milk or as a sole diet, results in higher rates of weight gain, linear growth, and head growth and a higher risk of developing necrotizing enterocolitis. The trial data do not show an effect on all-cause mortality, or on long-term growth or neurodevelopment.

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews Banked preterm versus banked term human milk to promote growth and development in very low birth weight infants Dempsey E, Miletin J. Cochrane Database of Systematic Reviews 2019, Issue 6. Art. No. : CD 007644. DOI: 10. 1002/14651858. CD 007644. pub 3.

Banked preterm versus banked term human milk to promote growth and development in very low birth weight infants Other feeding alternatives when mother’s milk is unavailable Human milk banking has been available in many countries for the last three decades and has played an important role in neonatal care. The milk provided from milk banking is predominantly term breast milk (often produced later in lactation so it has a different nutrient content), although many breast milk banking services now also batch and provide donated preterm breast milk (Tully 2001; Wight 2001). The nutritional and non-nutritional components of human milk differ as gestational age advances (Boyce 2016). The relative constituents of protein, fat and carbohydrate differ (Gross 1980; Butte 1984), as do the nonnutritional components including variations in digestive hormones, growth factors, immunological factors, vitamins, minerals and trace elements (Schanler 1980; Saarela 2005).

Banked preterm versus banked term human milk to promote growth and development in very low birth weight infants Objectives: To determine the effect of banked donor preterm milk compared with banked donor term milk regarding growth and developmental outcomes in very low birth weight infants (infants weighing less than 1500 grams). Selection criteria: Randomized and quasi-randomized trials comparing banked donor preterm milk with banked donor term milk regarding growth and developmental outcomes in very low birth weight infants. Main results: No studies met the inclusion criteria. Authors' conclusions: We found no evidence to support or refute the effect of banked donor preterm milk compared to banked term milk regarding growth and developmental outcomes in very low birth weight infants.

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews Nutrient-enriched formula versus standard formula for preterm infants. Walsh V, Brown JVE, Askie LM, Embleton ND, Mc. Guire W. Cochrane Database of Systematic Reviews 2019, Issue 7. Art. No. : CD 004204. DOI: 10. 1002/14651858. CD 004204. pub 3.

Nutrient-enriched formula versus standard formula for preterm infants. Preterm infants especially very preterm infants have fewer nutrient reserves at birth than term infants and are subject to physiological and metabolic stresses that increase their nutrient needs. Most very preterm infants accumulate substantial energy, protein, mineral, and other nutrient deficits during their initial hospital stay (Embleton 2001; Horbar 2015). By the time they are ready to go home, typically at around 36 to 40 weeks' postmenstrual age, many infants are growth restricted relative to their term-born peers (Clark 2003; Dusick 2003). Growth deficits, which can persist through childhood and adolescence, are associated with neurodevelopmental impairment and with poor cognitive and educational outcomes (Bracewell 2008; Cooke 2003; Farooqi 2006; Ford 2000; Hack 1991; Leppänen 2014; Trebar 2007).

Nutrient-enriched formula versus standard formula for preterm infants. When sufficient human breast milk is not available, an artificial formula, given as the sole form of enteral nutrition or as a supplement to human breast milk, may be used as an alternative (Klingenberg 2012). A variety of formulas, typically adapted from cow's milk, are available. These vary in energy, protein, and mineral content and can be categorized broadly as follows: Standard (‘term') formulas based on the composition of mature breast milk; the typical energy content is 67 to 70 k. Cal/100 m. L, the concentration of protein is about 1. 4 g to 1. 7 g/100 m. L, and the calcium and phosphate content is about 50 mg/100 m. L and 30 mg/100 m. L, respectively. Nutrient-enriched (‘preterm') formulas, designed to provide nutrient intakes to match intrauterine accretion rates; these are energy enriched (typically to about 75 to 80 k. Cal/100 m. L), protein enriched (2. 0 to 2. 4 g/100 m. L) and variably enriched with minerals, vitamins, electrolytes, and trace elements (Hay 2017).

Nutrient-enriched formula versus standard formula for preterm infants. Main results We identified seven trials in which a total of 590 preterm infants participated. Most participants were clinically stable preterm infants of birth weight less than 1850 grams. Few participants were extremely preterm, extremely low birth weight, or growth restricted at birth. Trials were conducted more than 30 years ago, were formula industry funded, and were small with methodological weaknesses (including lack of masking) that might bias effect estimates. Meta-analyses of in-hospital growth parameters were limited by statistical heterogeneity.
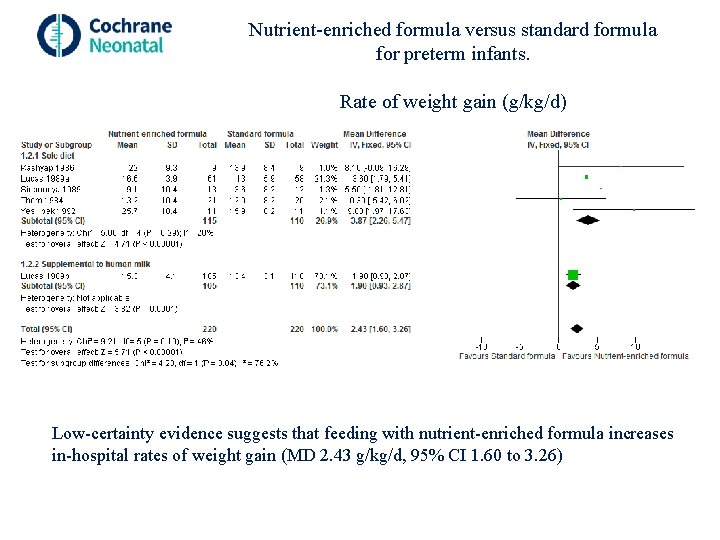
Nutrient-enriched formula versus standard formula for preterm infants. Rate of weight gain (g/kg/d) Low-certainty evidence suggests that feeding with nutrient-enriched formula increases in-hospital rates of weight gain (MD 2. 43 g/kg/d, 95% CI 1. 60 to 3. 26)
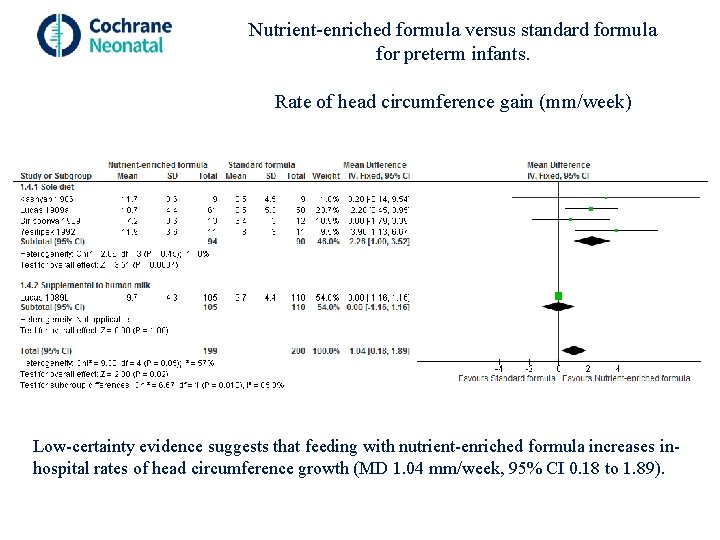
Nutrient-enriched formula versus standard formula for preterm infants. Rate of head circumference gain (mm/week) Low-certainty evidence suggests that feeding with nutrient-enriched formula increases inhospital rates of head circumference growth (MD 1. 04 mm/week, 95% CI 0. 18 to 1. 89).
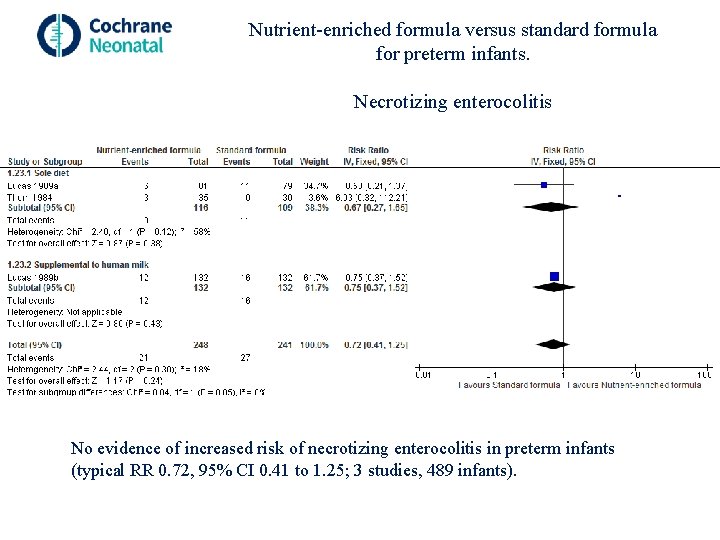
Nutrient-enriched formula versus standard formula for preterm infants. Necrotizing enterocolitis No evidence of increased risk of necrotizing enterocolitis in preterm infants (typical RR 0. 72, 95% CI 0. 41 to 1. 25; 3 studies, 489 infants).

Nutrient-enriched formula versus standard formula for preterm infants. Fewer data are available for growth and developmental outcomes assessed beyond infancy, and these do not show consistent effects of nutrient-enriched formula feeding. Data from two trials did not show an effect on Bayley Mental Development Index scores at 18 months post term (MD 2. 87, 95% CI -1. 38 to 7. 12; moderate-certainty evidence). Infants who received nutrient-enriched formula had higher Bayley Psychomotor Development Index scores at 18 months post term (MD 6. 56. 95% CI 2. 87 to 10. 26; low-certainty evidence), but no evidence suggested an effect on cerebral palsy (typical RR 0. 79, 95% CI 0. 30 to 2. 07; 2 studies, 377 infants).

Nutrient-enriched formula versus standard formula for preterm infants. Authors' conclusions Available trial data show that feeding preterm infants nutrientenriched (compared with standard) formulas has only modest effects on growth rates during their initial hospital admission. No evidence suggests effects on long-term growth or development. The GRADE assessment indicates that the certainty of this evidence is low, and that these findings should be interpreted and applied with caution. Further randomized trials would be needed to resolve this uncertainty.

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews Dilute versus full strength formula in exclusively formula-fed preterm or low birth weight infants Basuki F, Hadiati DR, Turner T, Mc. Donald S, Hakimi M. Cochrane Database of Systematic Reviews 2019, Issue 6. Art. No. : CD 007263. DOI: 10. 1002/14651858. CD 007263. pub 3.

Dilute versus full strength formula in exclusively formula-fed preterm or low birth weight infants Description of the condition Increased milk osmolality has been suggested as a risk factor for developing feeding intolerance and necrotizing enterocolitis (NEC), either through damaging the bowel mucosa or by influencing the development or growth of the gut. However, the evidence to support either mechanism is limited (Pearson 2011). The osmolality of breast milk from mothers of term babies is 300 m. Osmol/kg, and from mothers of preterm babies is 276 m. Osmol/kg. Preterm formulas vary in osmolality from 250 to 350 m. Osmol/kg. The addition of fortifiers increases the osmolality of milk (Pearson 2011). Dilution of formula might be one way of reducing osmolality and, therefore, feeding intolerance and NEC.

Dilute versus full strength formula in exclusively formula-fed preterm or low birth weight infants Objectives: To assess the effects of dilute versus full-strength formula on the incidence of necrotizing enterocolitis, feeding intolerance, weight gain, length of stay in hospital and time to achieve full calorie intake in exclusively formula-fed preterm or low birth weight infants. Selection criteria: Randomized or quasi-randomized trials comparing strengths of formula milk in exclusively formula-fed preterm or low birth weight infants. We excluded studies if infants received formula as a supplement to breast milk. Main results: The authors identified three studies involving 102 preterm or low birth weight infants in the review. The studies compared dilute (double-volume, half-strength) formula with full-strength (20 kcal/oz (~ 68 to 70 kcal/100 m. L)) formula. All three studies were assessed as having unclear risk of bias due to the likely absence of blinding of study personnel and the potential for selection bias in the largest trial. Data for the primary outcome of necrotizing enterocolitis were not reported in any of the studies.

Dilute versus full strength formula in exclusively formula-fed preterm or low birth weight infants Main results: The authors combined two of the studies (88 infants) in the metaanalysis. The evidence suggests that dilute formula with double-volume (half-strength) may lead to - fewer episodes of gastric residuals per day (mean difference (MD) − 1. 20, 95% confidence interval (CI) − 2. 20 to − 0. 20; one study, low-certainty evidence) - fewer episodes of gastric residuals per baby until attaining 100 kcal/kg (MD − 0. 80, 95% CI − 1. 32 to − 0. 28; one study, low-certainty evidence) - fewer episodes of vomiting per day (MD − 0. 04, 95% CI − 0. 07 to − 0. 01; one study, low-certainty evidence) and - fewer occurrences of abdominal distension greater than 2 cm (MD − 0. 16, 95% CI − 0. 19 to − 0. 13; 2 studies, low-certainty evidence).

Dilute versus full strength formula in exclusively formula-fed preterm or low birth weight infants Main results: For the secondary outcomes, data suggest that infants in the dilute formula with double-volume (half-strength) group may have attained an adequate energy intake earlier than infants in the fullstrength group (two studies; MD − 2. 26, 95% CI − 2. 85 to − 1. 67; low-certainty evidence). There was no evidence of a difference between groups for weight gain one week after commencement of intragastric feeds (one study; MD 0. 05 kg, 95% CI − 0. 06 to 0. 15; low-certainty evidence). Data were not reported for length of hospital stay.

Dilute versus full strength formula in exclusively formula-fed preterm or low birth weight infants Authors' conclusions There is low-certainty evidence from three small, old trials that use of dilute formula in preterm or low birth weight formula-fed infants may lead to an important reduction in the time taken for preterm infants to attain an adequate energy intake. However, our confidence in this result is limited due to uncertainty over risk of bias and sparsity of available data. Dilute formula may reduce incidence of feeding intolerance, but the clinical significance of the reduction is uncertain. The impact on serious gastrointestinal problems, including necrotizing enterocolitis, was not reported in any of the trials. Further randomized trials are needed to confirm these results.

Choosing the best feeds for preterm infants: evidence from Cochrane systematic reviews Protein hydrolysate versus standard formula for preterm infants. Ng DHC, Klassen JRL, Embleton ND, Mc. Guire W. Cochrane Database of Systematic Reviews 2019, Issue 7. Art. No. : CD 012412. DOI: 10. 1002/14651858. CD 012412. pub 3.

Protein hydrolysate versus standard formula for preterm infants. Background: Hydrolyzed cow's milk formulas, originally developed for infants with cow's milk protein allergy or intolerance, are used as enteral feeding alternatives for preterm infants for whom human milk is unavailable. These formulas contain hydrolyzed, rather than intact, proteins and may also differ from standard cow's milk formulas in carbohydrate, lipid, and micronutrient type and content (Oldaeus 1997). Their use as a sole, or supplemental, enteral feed source for preterm infants has increased since the late 1990 s, particularly in high-income countries, because they are perceived as being tolerated better and less likely to lead to complications than standard cow's milk formulas (Zuppa 2005). However, hydrolyzed formulas are more expensive than standard formulas, and concern exists that their use in practice is not supported by high-certainty evidence (Foucard 2005).

Protein hydrolysate versus standard formula for preterm infants. Main results: The authors identified 11 trials for inclusion in the review. All trials were small (total participants 665) and had various methodological limitations including uncertainty about methods to ensure allocation concealment and blinding. Most participants were clinically stable preterm infants of less than about 34 weeks' gestational age or with birth weight less than about 1750 grams. Fewer participants were extremely preterm, extremely low birth weight, or growth restricted

Protein hydrolysate versus standard formula for preterm infants. Main results: Most trials found no effects on feed intolerance, assessed variously as mean pre-feed gastric residual volume, incidence of abdominal distension or other gastrointestinal signs of concern, or time taken to achieve full enteral feeds (meta-analysis was limited because studies used different measures).
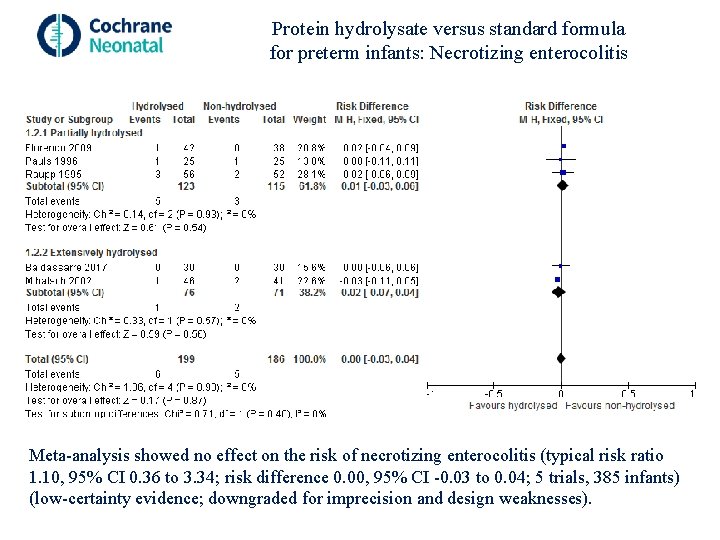
Protein hydrolysate versus standard formula for preterm infants: Necrotizing enterocolitis Meta-analysis showed no effect on the risk of necrotizing enterocolitis (typical risk ratio 1. 10, 95% CI 0. 36 to 3. 34; risk difference 0. 00, 95% CI -0. 03 to 0. 04; 5 trials, 385 infants) (low-certainty evidence; downgraded for imprecision and design weaknesses).
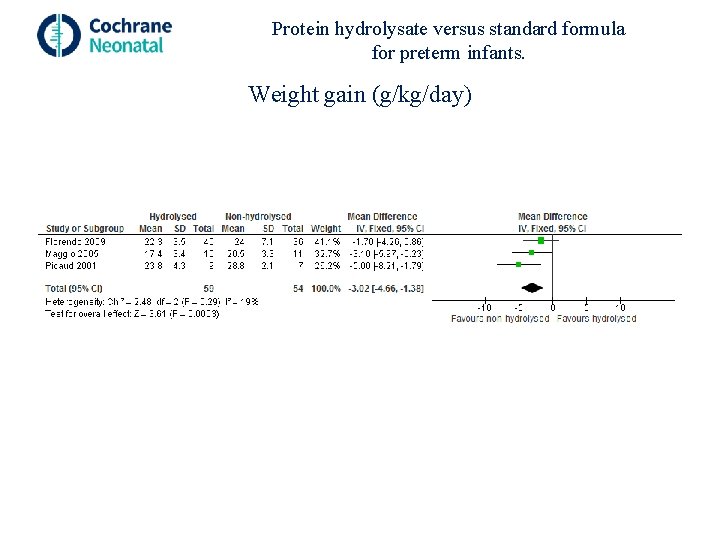
Protein hydrolysate versus standard formula for preterm infants. Weight gain (g/kg/day)

Protein hydrolysate versus standard formula for preterm infants. Authors' conclusions: The identified trials provide only low-certainty evidence about the effects of feeding preterm infants protein hydrolysate versus standard formula. Existing data do not support conclusions that feeding protein hydrolysate affects the risk of feed intolerance or necrotizing enterocolitis. Additional large, pragmatic trials are needed to provide more reliable and precise estimates of effectiveness and costeffectiveness.

Guest Discussants Heather C. Kaplan, MD, MSCE Associate Professor, University of Cincinnati Department of Pediatrics Brenda Poindexter, MD, MS Professor, University of Cincinnati Department of Pediatrics

Surveys of enteral feeding practices in preterm infants Klingenberg C, Embleton ND, Jacobs SE, et al. Enteral feeding practices in very preterm infants: an international survey. Archives of Disease in Childhood - Fetal and Neonatal Edition 2012; 97: F 56 -F 61. Xu JH, Coo H, Fucile S, Ng E, Ting JY, Shah PS, Dow K, Canadian Neonatal Network Investigators. A national survey of the enteral feeding practices in Canadian neonatal intensive care units. Paediatrics & Child Health. pxz 112. Gregory KE, Connolly TC. Enteral feeding practices in the NICU: results from a 2009 Neonatal Enteral Feeding Survey. Adv Neonatal Care. 2012 Feb; 12(1): 46 -55.

Enteral Feeding Practices for Extremely Preterm or Extremely Low Birth Weight Infants Does your unit have access to donor human milk? 67% If yes, do you obtain donor human milk from: a. Your own milk bank b. An external milk bank c. Source not known 17. 8% 80. 5% 1. 7% 1 b. If yes, do you have access to preterm donor breast milk? 50. 8%

Enteral Feeding Practices for Extremely Preterm or Extremely Low Birth Weight Infants Do you routinely initiate enteral feeds with: a. Full strength breast milk or formula 98. 1% b. Diluted breast milk or formula 2. 6% Does your unit have written guidelines and policies regarding the use of hydrolyzed formula? 26. 1%

CME Credit Survey: https: //www. surveymonkey. com/r/3 CWQRL 9 Nursing Contact Hours Survey: https: //www. surveymonkey. com/r/3 YBPPKD Ø The surveys will be open within an hour after the webinar. We will send an email with the links to registered participants. Ø You must take a survey within 2 weeks of the webinar in order to receive credit. Ø Once you take the survey, you will be redirected to our website where you can download and save a certificate for your records. Ø Credit can only be given to those who participate in the live webinar. You cannot receive credit for watching the recording of the webinar, which will be posted on our website within approximately 2 weeks. Please contact Caitlin O’Connell Eckert at ceckert@vtoxford. org with questions.

Evidence Based Medicine: Basics and Beyond Upcoming Sessions: Session 5: Making the GRADE! GRADE recommendations in neonatal-perinatal medicine March 23, 2020 @ 12: 00 pm EDT Session 6: Translating evidence-based medicine to evidencebased practice June 2020, TBD Past sessions, along with supplementary materials, can be viewed on our website: neonatal. cochrane. org/evidence-classroom 1

Get your facts first, then you can distort them as you please Mark Twain
- Slides: 77