Cholestatic Liver Disease Primary Biliary Cirrhosis Causes of

Cholestatic Liver Disease Primary Biliary Cirrhosis

Causes of Alk Phosphatase Elevation n n Hepatic: cirrhosis, tumors, Steatosis, PBC, PSC, drugs, TPN Biliary: Cholangitis, Obstruction Bone: Paget’s, Hyperparathyroid, Mets Septicemia cholestasis of sepsis Physiologic puberty, pregnancy

Medications n n Anabolic steroids Chlorpromazine Erythromycin Oral contraceptives

ALP of hepatic origin n n < 2 x Normal Repeat in 4 wks Normal ____ No action Unchanged ___ US__ dil ducts __ ERCP CT = mets__ FNA

ALP > 2 x Normal n CT …. Normal – hepatitis(immune, viral disease)… Liver biopsy CT …. . Dilated ducts, stone or mass Proceed with ERCP/ CT Bx or Surg ( Bile duct obstruction, PSC, PBC )

Primary Biliary Cirrhosis n n n Autoimmune cholestatic disorder Female to male ratio of 9 : 1 Inflammatory destruction of bile ducts, leads to cholestasis and cirrhosis Autoantibodies reactive with antigens on the surface of biliary epithelium Antimitochondrial antibodies

PBC: Symptoms and Signs n n n n Fatigue Pruritis Jaundice Hepatomegaly Splenomegall Xanthelasma None 70 % 55 10 25 15 10 25

PBC: Associated Diseass n n n Keartoconjuntivitis sicca Arthritis Scleroderma Thyroiditis RTA Gallstones 75% 4 – 40 15 20 50 33

Diag: Liver Profile n n n Alk phosphatase elevation AST / ALT less than 5 x N Increase in bilirubin, albumin and prothrombin time = poor prognosis
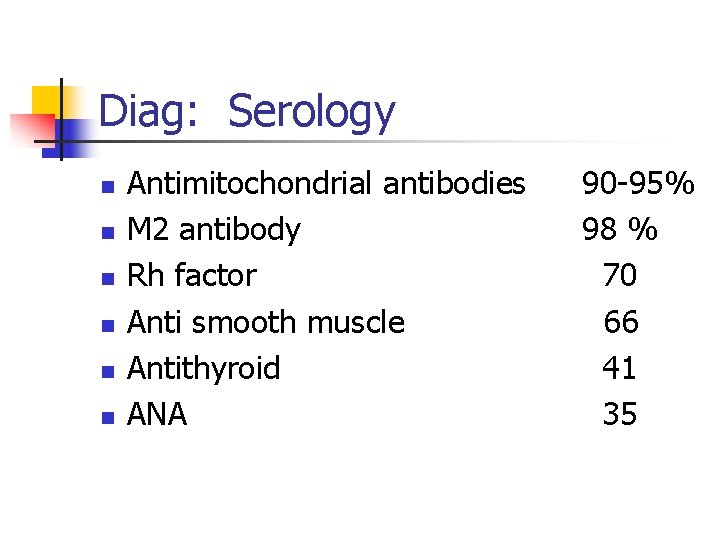

Diag: Serology n n n Antimitochondrial antibodies M 2 antibody Rh factor Anti smooth muscle Antithyroid ANA 90 -95% 98 % 70 66 41 35

Liver Histology n Ludwig’s Classification Stage III. Stage IV. Inflammation within portal space Focussed on bile ducts Inflam extending into hepatic parenchyma Fibrosis Regenerative nodules ( cirrhosis)

Natural History: Asymptomatic PBC n n n Mitchison et al 1986 29 patients with normal LFT’s Followed for 17. 8 years (11 – 24 yrs) Abnormal LFT’s in 5. 6 yrs Symptoms developed in 76 %

Natural History: Symptomatic PBC Once symptoms develop, life expectancy falls sigficantly, with a median survival time of approximately 10 years.

Prediction of Survival Mayo Risk Score n Advanced age Serum bilirubin Serum albumin Fluid retention ( ascites and edema) Variceal bleeding Advanced histologic stage n Bilirubin > 10 mg = Life expectancy < 2 yrs n n n

Medical Treatment n n n Glucocorticoids Budeonide D-Penicillamine Colchicene Azathioprine Cyclosporine Methotrexate no improvent in survival

treatment n n n n Ursodeoxycholic acid Small quantities in bile --- < 4 % Endogenous Bile acids ( cholic, cheno, litho) hepatoxic Treatment increases Urso content to 30 -60% Level of Urso parallels improvement in liver profile and Mayo Risk Score Dose : 13 – 15 mg/kg/day If pt on Cholestyramine, Urso to be taken 2 hrs before or after cholestyramine administration

PBC: Complications n n n Bone Disease: osteoporosis and fractures vitamin D 25, 000 to 50, 000 iu / week Fat-Soluble Vit Deficiency vit A 25, 000 IU 3/WK vit K 5 mg/d vit E 50 – 200 u / d Steatorrhea Low fat diet, substitute MCT Hypercholestrolemia RX Urso Pruritis Cholystyramine, Rifampin, liver transplant.
- Slides: 18