CHLAMYDIA DR SUNIL RAO PADMARAJ INTRODUCTION CHLAMYDIAE belong

CHLAMYDIA DR. SUNIL RAO PADMARAJ

INTRODUCTION �CHLAMYDIAE belong to one Family. CHLAMYDIACEAE, Order- CHLAMYDIALES Genus Chlamydia �Revised Classification of the. Genus Family. Chlamydophila Chlamydiaceae C. trachomatis C. pneumoniae C. muritlarum C. psittaci C. S’llis C. pecorum C. abortus C. caviae C. felis

� 3 species causing human disease - C. trachomatis - C. psittaci - C. pneumoniae

ü Diseases caused�Psittacosis �Lymphogranuloma Venerum �Trachoma ü Diverse disease in birds and mammals ü Previously called Psittacosis-Lymphogranuloma. Trachoma(PLT) or Trachoma-Inclusion Conjunctivitis(TRIC)

FEATURES �Generally- 1. small obligate intra cellular Gram negative bacteria(very difficult to stain by Gram’s method. ) 2. They possess both RNA and DNA, ribosomes, cell wall similar to Gram negative bacteria. 3. Absence of peptidoglycan is the only difference between other Gram -ve bacteria. 4. They lack ability to generate their own ATP. So use host ATP. 5. Divide, multiply by binary fission.
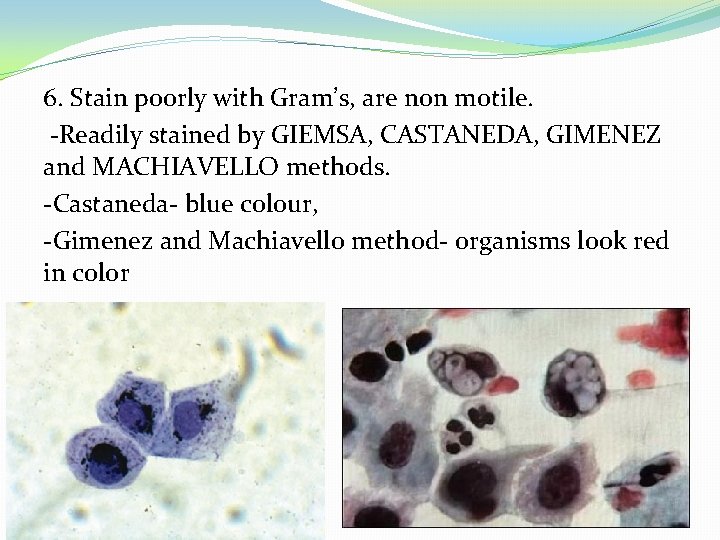
6. Stain poorly with Gram’s, are non motile. -Readily stained by GIEMSA, CASTANEDA, GIMENEZ and MACHIAVELLO methods. -Castaneda- blue colour, -Gimenez and Machiavello method- organisms look red in color
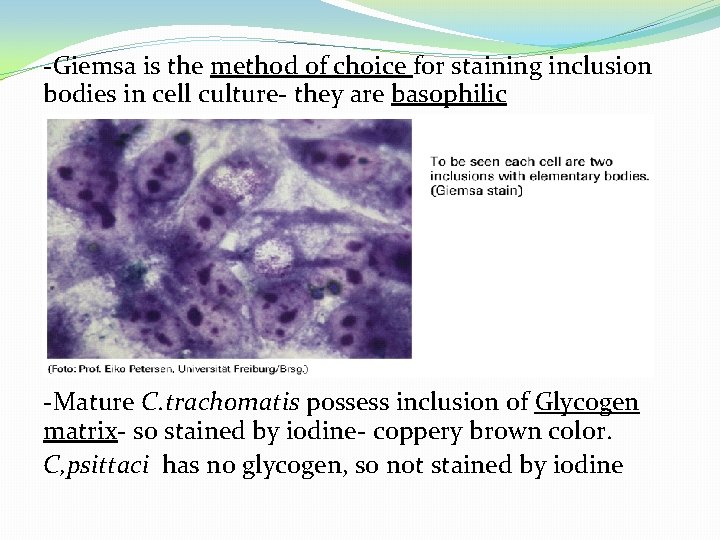
-Giemsa is the method of choice for staining inclusion bodies in cell culture- they are basophilic -Mature C. trachomatis possess inclusion of Glycogen matrix- so stained by iodine- coppery brown color. C, psittaci has no glycogen, so not stained by iodine
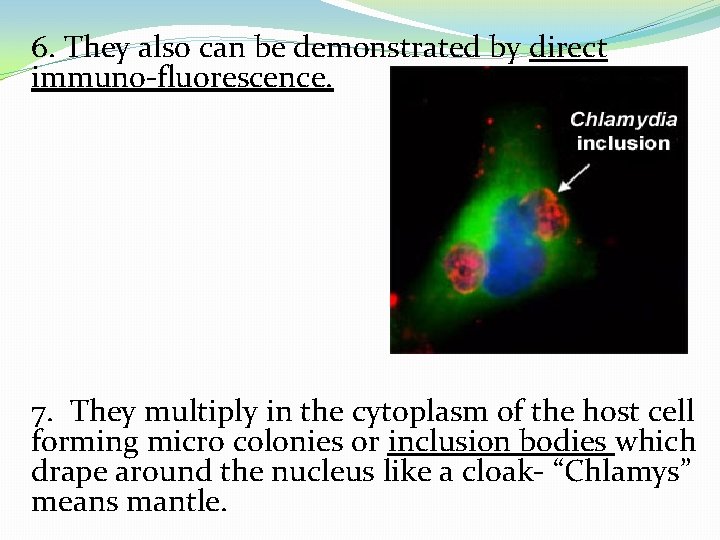
6. They also can be demonstrated by direct immuno-fluorescence. 7. They multiply in the cytoplasm of the host cell forming micro colonies or inclusion bodies which drape around the nucleus like a cloak- “Chlamys” means mantle.

8. most strains of C. trachomatis and C. psittaci possess DNA of 7. 3 and 6. 2 KB pairs respectively. -C. pneumoniae has no plasmid DNA. 9. There is a Major Outer Membrane Protein(MOMP) which has species specific epitopes. 10. Chlamydiae also have Genus specific LPS complex which is antigenic

11. They infect wide spectrum of vertebrate hosts- birds, mammals and humans. 12. They are susceptible to wide range of antibioticstetracycline, erythromycin, macrolides, rifampicin. C. trachomatis also sensitive to sulfonamides whereas C. psittaci and C. pneumoniae are resistant
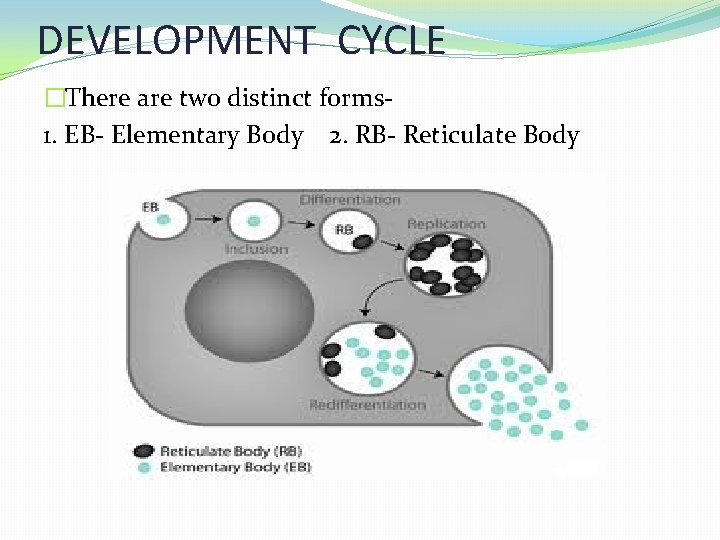
DEVELOPMENT CYCLE �There are two distinct forms 1. EB- Elementary Body 2. RB- Reticulate Body

ELEMENTARY BODY(EB)1. extra-cellular infectious particle 2. small (250 -350 nm in diameter) 3. spherical in case of C. trachomatis and C. psittaci. Pear shaped in C. pneumoniae 4. it has irregular electron dense nucleoli 5. Relatively strong- so capable of extra cellular survival 6. there is no peptidoglycan- cell wall is made up of disulfide cross linking among MOMP and several cysteine rich proteins

�RETICULATE BODIES(RB)1. Intra cellular 2. Metabolically active 3. Divides by binary fision to form EBs. 4. 800 -1200 nm in diameter 5. Cell wall lacks disulfide cross linking

�Infection is initiated by the attachment of infectious EB to susceptible host cells �Type, range of susceptible host cells vary with species and biovar. Eg: Biovars- Trachoma- Squamous, columnar cell C. trachomatis- LGV- lymphoid cell C. psittaci- wide range of cells

1. It is presumed that epitopes in variable domains of MOMP on the surface of EB may act as Adhesin and Trypsin Sensitive Protein on susceptible cells of host act as a specific cell receptor. 2. After attachment organism enters host cell within a vesicle. Chlamydiae dependant modification of endocyte membrane prevents the lysosomal fusion and thus prevent degradation.
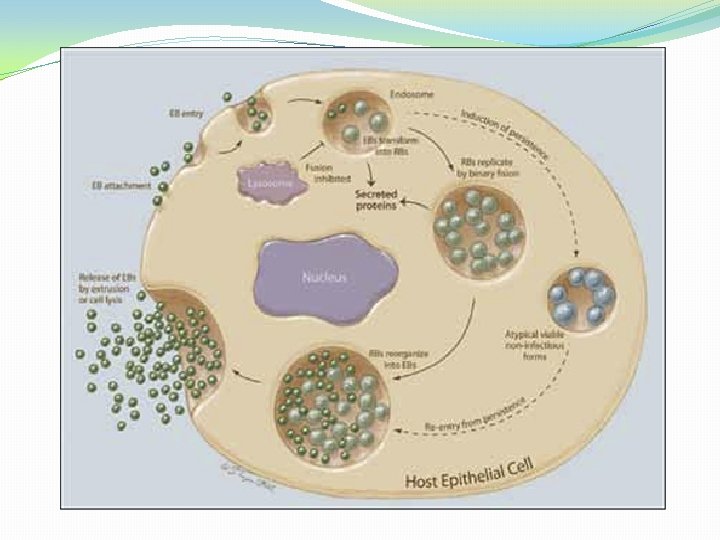

3. 9 hours after infection EB within the vesicle loses its dense DNA core Its cell wall becomes less rigid due to breaking of disulfide bonds, increases in size and differentiate into RB. does not possess cytochromes and lacks ability to generate ATP, so uses host ATP.

4. 18 hours after infectionthe vesicle is enlarged. RB divides by binary fission, yields pleomorphic organisms and genus specific chlamydial antigens become associated with the host cell surface.

5. By 24 hoursthere is condensation of DNA within the RB, disulfide bonds are formed in the outer membrane protein and new EBs develop within the vesicle. Developing chlamydial micro colonies within the vesicle is termed an INCLUSION BODY (IB). It is typically peri-nuclear and may have 100 -500 EBs. 6. By 40 -70 hours. Infectious EBs are released from the cell by rupture and these may infect new cells.
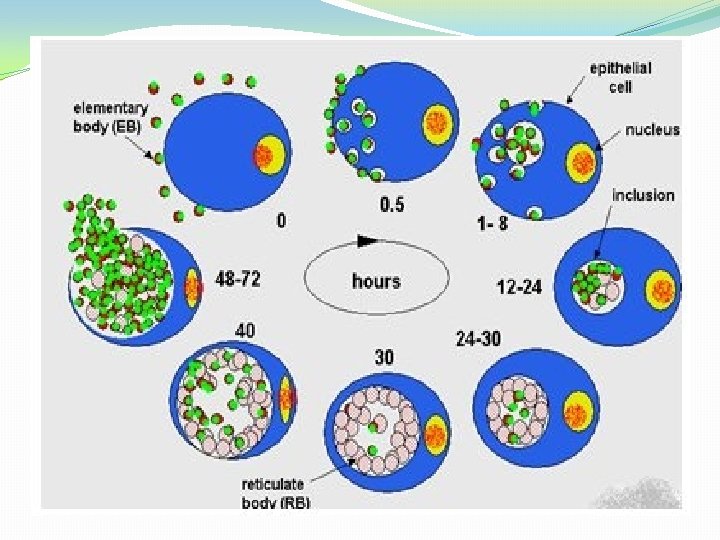

Susceptibility to physical and chemical agents �At 35 -370 C, they lose infectivity within hours. � 560 C- inactivated within minutes �Alcohol, ether, iodine, KMn. O 4, sodium hypochlorite, silver nitrate at concentration used for disinfection inactivate. �Can be preserved at -700 C or liquid nitrogen for months or years.

ANTIGENIC STRUCTURE �Genus specific antigen – C. trachomatis and C. psittaci have a heat stable, complement fixing genus specific antigen. It is present both in RB and EB. It is a LPSprotein complex, extracted by ether, deoxycholate, chloroform or methanol. �Species specific antigen - There are four outer membrane proteins. Species specific epitopes found in MOMP.

�Serotype specific antigens-within each species particularly C. trachomatis a number of serotypes called serovars can be defined. � C. trachomatis possess 3 biovars, a. Those causing trachoma & inclusion conjunctivitis. b. Those causing LGV. c. Causing mouse pneumonitis [Mo. Pn]

�By neutralisation of infectivity and IF, both TRIC and LGV biovars which infect humans can be subdivided into 15 serovars � C. trichomatis biovars has 12 serovars. A, B, Ba, C, D, E, F, G, H, I, J & K. �Biovar LGV has 3 [L 1 – L 3]

CULTURAL CHARACTERS: Imp. for laboratory diagnosis. Introduction of the specimen– � 1. Intranasal, intraperitoneal, intraurethral inoculation into mice. � 2. Into yolk sac of 6 -8 days old chick embryo � 3. Cell cultures.
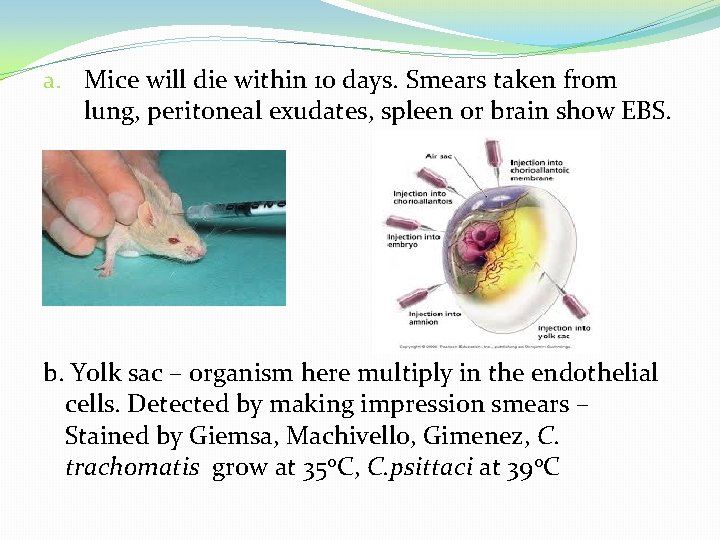
a. Mice will die within 10 days. Smears taken from lung, peritoneal exudates, spleen or brain show EBS. b. Yolk sac – organism here multiply in the endothelial cells. Detected by making impression smears – Stained by Giemsa, Machivello, Gimenez, C. trachomatis grow at 35 o. C, C. psittaci at 39 o. C

c. Cell culture – Cells have to be irradiated or treated with metabolic inhibitor for isolation. Cycloheximide treated Mc. Coy cells most commonly used. C. pneumoniae grow better in He. La cells or Monkey Kidney cell lines. �Mouse fibroblast cells can also be used. �C. psittaci can be propagated in fish or lizard cells. �Presence of organism – detected by staining for inclusions or EBs by IF or Giemsa.

�PATHOGENICITY – Chlamydiae produce infection of eye, male and female genital tract infection and respiratory tract infections.

INFECTION OF EYE�Trachoma – Communicable chronic keratoconjunctivitis. �Follicles, papillary hyperplasia, pannus formation and in late stages cicatrization, blindness. �Occurs only in humans. �Causes blindness in trachoma belt – North Africa to South east Asia. �N. Africa, Middle east and Northern part of Indian sub continent worst effected areas.
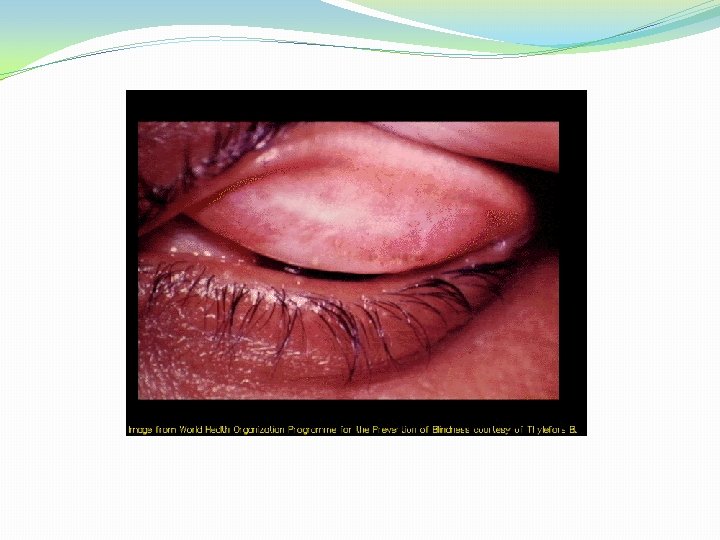

�Seen in children below 9 years age in endemic areas. Caused by biovar TRIC serovar A, B, Ba, C. �Transmission – eye to eye by direct contact with fingers or contaminated towels and clothing. Flies may transmit mechanically. �Incubation period 7 -14 days.

Inclusion – conjunctivitis. C. trachomatis biovar TRIC serovars D-K. �Natural habitat is genital tract of both sexes. �Most prevalent in sexually active young people and is spread from genitalia to eye. �Incubation period 1 -2 weeks. �Onset is acute, intense hyperemia, muco purulent discharge and follicular hyperplasia. �Unlike trachoma lesions most pronounced in the lower than upper lid.
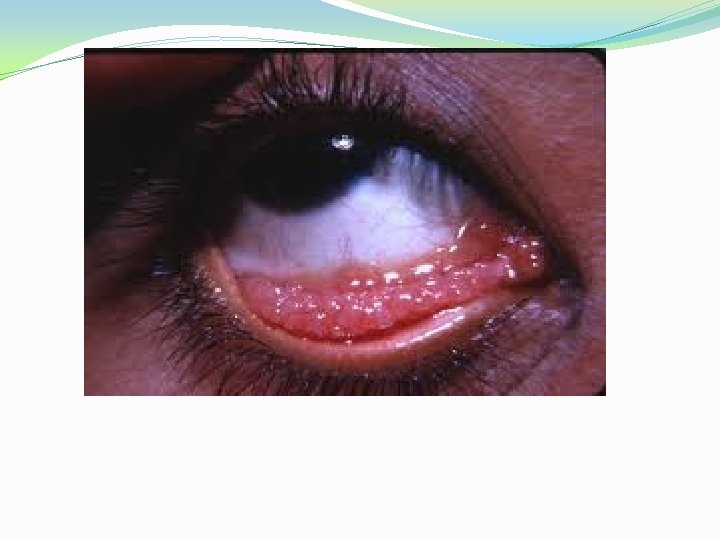
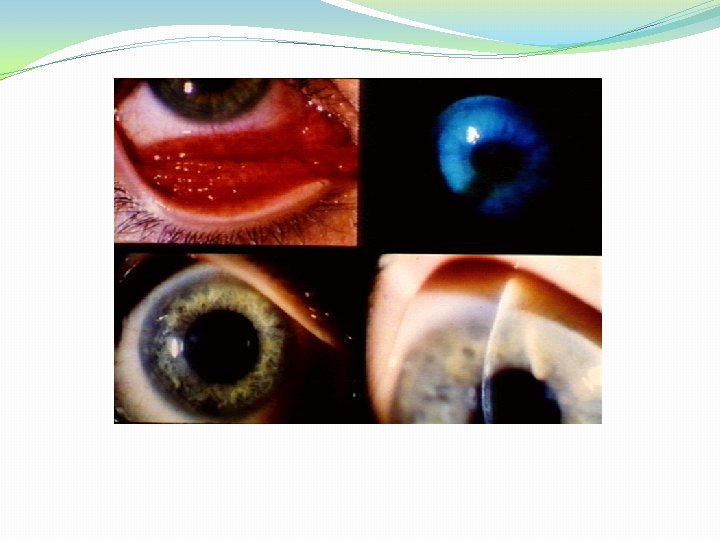

�Some patients develop scarring, corneal lesion or pannus formation. �Genital symptoms are minimum or absent especially in women. �Disease is usually self limited and does not lead to blindness.
![3. Opthalmia neonatrum [ Inclusion blenorrhoea] � Neonatal form of inclusion conjunctivitis. �Infection acquired 3. Opthalmia neonatrum [ Inclusion blenorrhoea] � Neonatal form of inclusion conjunctivitis. �Infection acquired](http://slidetodoc.com/presentation_image_h/0e7590b453f63d108f994774da5876fe/image-36.jpg)
3. Opthalmia neonatrum [ Inclusion blenorrhoea] � Neonatal form of inclusion conjunctivitis. �Infection acquired through birth canal. � 5 -12% pregnant woman have chlamydial infection of cervix. � 50% infants born to such mothers will have conjunctivitis. � 5 -12 days after birth – neonate has swelling of eye lids, hyperemia and a purulent infiltration of conjunctiva. �A proportion of untreated neonates develop pneumonia.

�GENITAL INFECTIONS: �Males: Biovar TRIC – Serovar D-K – cause 30% cases of NGU �It occurs 7 -14 days after sexual intercourse. �Other organisms of NGU are – Ureaplasma, urealyticum, Mycoplasma genitalium, M. hominis, Bacteroides urealyticus, Herpesvirus hominis, CMV, T. vaginalis. �C. trachomatis also responsible for 50% cases of epidydimitis in men under 35 years of age and 15% men above 35 years. �Proctitis occurs in homosexual male.

�Female – C. trachomatis biovar TRIC serovars D-K cause urethritis in female, mucopurulent cervicitis, vaginitis and vaginal discharge, endometritis, salphingitis, infertility, perihepatitis and periappendicitis. �Endometritis and salphingitis singly or together is called PID [Pelvic Inflammatory Disease]. �Ovine strains of C. psittaci can cause abortion and still birth.
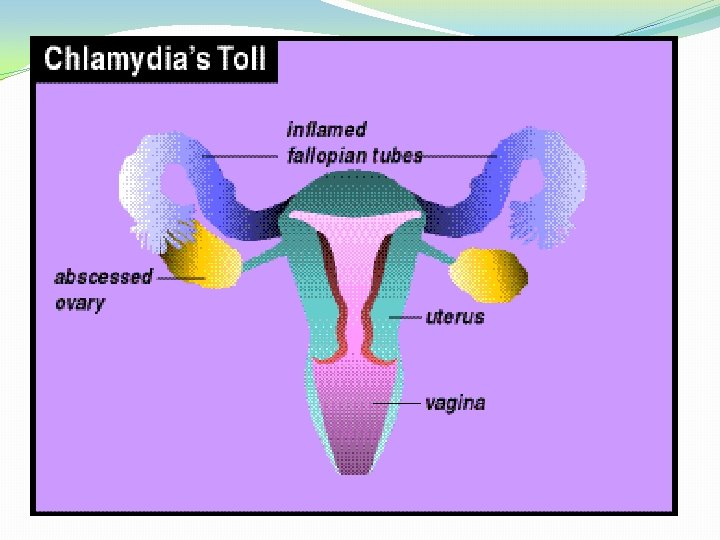

LGV – Biovar TRIC serovars L 1 – L 3 cause lymphogranuloma venerum in both sexes. � 1 -3 weeks after sexual contact, male develop a small 58 mm painless papule or ulcer on the penis. Rectal infections occur in homosexuals. �In woman, same thing can occur in the fourchette.

�In both sexes this primary lesion can pass of unnoticed. �Primary lesions can also occur uncommonly on other sites. Eg. Fingers, tongue. �Primary lesions will heal. �After 1 -2 months – regional lymph node [ inguinal in male and intrapelvic and pararectal in females] become enlarged and tender and may break open with sinuses. These enlarged lymph node are called bubos.
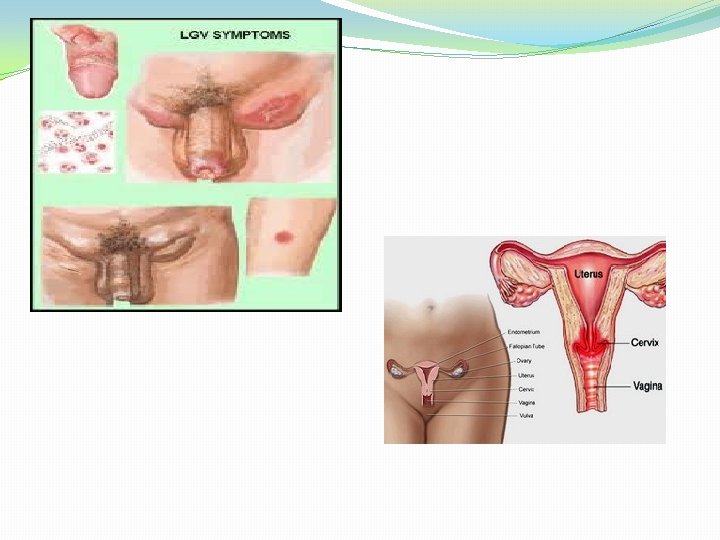

RESPIRATORY TRACT INFECTION: �TW 183 and AR 39 isolated in 1965 from eye of child with trachoma in Taiwan. Same strains also isolated from pharyngitis throat. �These two organism were called TWAR. �But now classified as C. pneumonia. �It appears as the third most common cause of pneumonia after S. pneumoniae & H. influenzae.

�It also causes acute lower respiratory infection in man. �Infection is spread from person to person with out intervention of avian host. �Psittacosis is disease of birds belonging to psittacine family-parrots, transmissible to man (Zoonotic disease).

�Non-psittacine birds-pigeon, ducks, domestic fowlsthese organisms maybe present. �The disease acquired by non-psittacine birds is called ornithosis. �Infection in birds exists as asymptomatic, latent infection which can flare up following stress to birds like caging, overcrowding.

�There will be diarrhea, mucopurulent respiratory discharge and emaciation. �Fecal discharge and nasal discharge of these birds will contain many organisms so a source of infection to other birds and humans. �Man gets infection by inhalation of dried feces of birds. �Incubation period 1 -2 weeks.
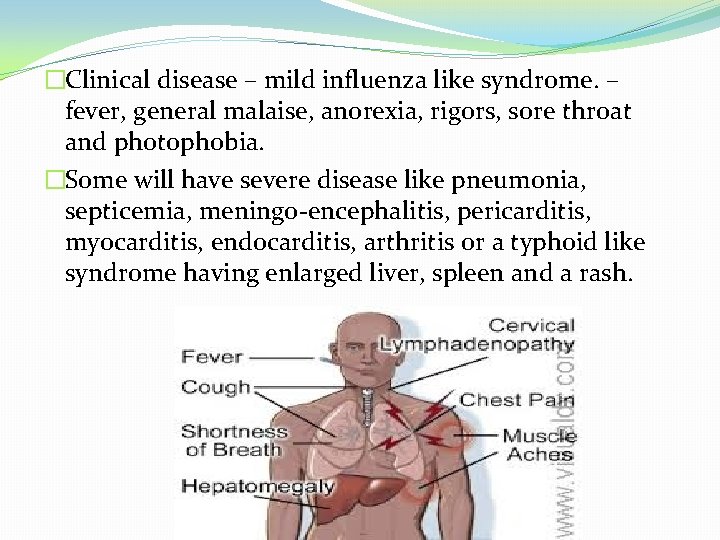
�Clinical disease – mild influenza like syndrome. – fever, general malaise, anorexia, rigors, sore throat and photophobia. �Some will have severe disease like pneumonia, septicemia, meningo-encephalitis, pericarditis, myocarditis, endocarditis, arthritis or a typhoid like syndrome having enlarged liver, spleen and a rash.

LABORATORY DIAGNOSIS: �Collection of specimens – Ocular, urethral, vaginal, cervical specimen are best collected by scraping the mucosa. �In addition depending on the site of involvement blood, respiratory secretions, sputum, lung and other tissues can be collected. �In LGV pus from bubo to be collected.

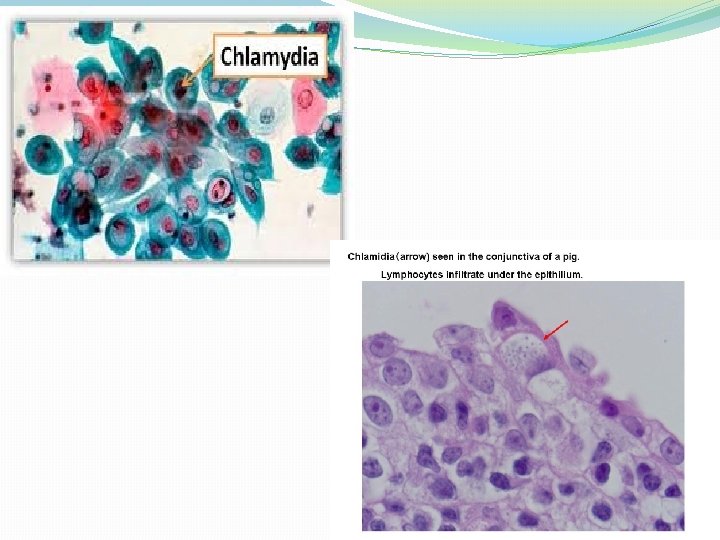
PROCESSING OF SPECIMENDirect detection of chlamydial antigens. 1. Light microscopy – infection of conjunctiva, urethra and cervix may be diagnosed – demonstration of typical reniform inclusion bodies surrounding the nucleus [ HP bodies] – use non absorbent cotton swab. Stain by Giemsa, Castaneda or Macchiaevello methods. Glycogen matrix in C. trachomatis – Iodine staining – but weak or low sensitivity.
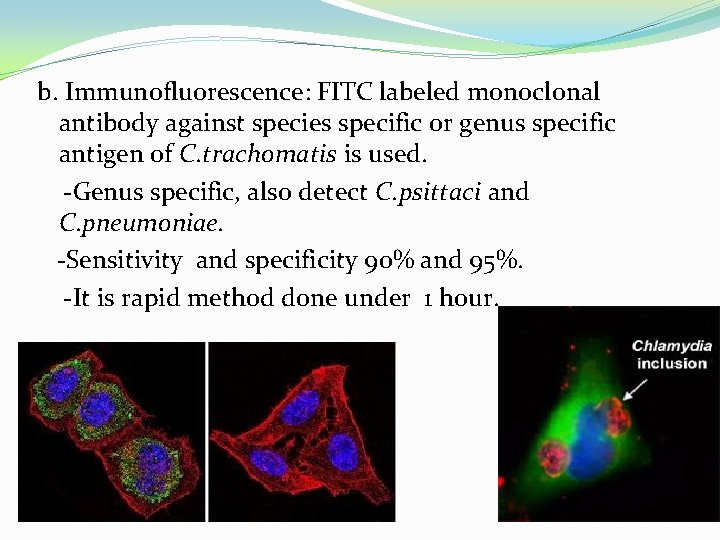
b. Immunofluorescence: FITC labeled monoclonal antibody against species specific or genus specific antigen of C. trachomatis is used. -Genus specific, also detect C. psittaci and C. pneumoniae. -Sensitivity and specificity 90% and 95%. -It is rapid method done under 1 hour.

2. ELISA for chlamydial antigens : Detection of soluble genus specific antigen captured by antibody attached to a solid surface eg. Plastic bead or micortiter well and later detected with enzyme labeled detector system and chromogenic substrate. Sensitivity and specificity similar to IF.

� 3. DNA probes – DNA hybridization can be used for direct detection of C. trachomatis antigen in conjunctival and cervical smears.

4. Chemilumnescence assay – - acridium – ester labeled ss DNA probe which is complementary to RNA of C. trachomatis is used. - The labeled DNA, RNA hybrid is detected in a luminometer. - Luminometer measures the light emitted by the acridium ester label. - Sensitivity and specificity 95%.

� 5. PCR – Polymerase Chain Reaction – - common endogenus plasmid DNA, the ompl gene [codes for MOMP] and the 16 s r. RNA gene can be amplified and detected by PCR. - This method is more sensitive than culture.

6. Isolation of chlamydia – specimen inoculated in mice, yolk sac of 6 -8 day chick embryo and by cell culture. 7. Detection of chlamydial antibody: a. Antibody against C. psittaci and serovars L 1 – L 3 of C. trachomatis can be detected by CF test. b. Antibody against C. trachomatis and C. pneumoniae can be detected by micro immunofluorescence using EB’s of standard serovars. Also can use immunoperoxidase and ELISA test. High level of Ig. M [>1: 64] and rising titer of Ig. G diagnostic.

�Neonatal chlamydial pneumonia – Detection of Ig. M diagnostic because Ig. G cannot distinguish maternal or neonatal infection. �Hightiters of antibody against C. trachomatis is seen in acute salphingitis and infertility.

Treatment �Trachoma -> Azithromycin has replaced erythromycin & Doxycycline �Genital infections & Inclusion conjunctivitis -> Doxycycline & Azithromycin �LGV -> Doxycycline & Sulfonamides �Respiratory tract infections -> Doxycycline, Azithromycin, Clarithromycin

Prophylaxis �Trachoma -> Personal hygiene �Genital infections -> - Detection of cases, contacts & their treatment - Avoiding sexual promiscuity - Safe sex methods (Condom) �Psittacosis -> - Avoiding contact with infected birds - Elimination of infected birds
- Slides: 59