Childhood Endocrine Disorders Paediatric Endocrinology Dr RH Willemsen
































- Slides: 62

Childhood Endocrine Disorders Paediatric Endocrinology Dr. RH Willemsen, Consultant Paediatric Diabetes and Endocrinology Royal London Children’s Hospital Barts Health NHS Trust

The team • 4 NHS consultants: Evelien Gevers, Claire Hughes, Rathi Prasad, Ruben Willemsen, vacancy • 3 academic consultants: Li Chan, Leo Dunkel, Helen Storr • 2 endocrine CNS: Lee Martin, Isabelle Sharatt • 1 GRID registrar, 1 SHO, 1 clinical fellow • Large diabetes team: nurses, dietitians and psychologists working across 3 sites, 600 patients

Objectives • • Basic physiology of the endocrine system Normal growth and puberty Disorders of the thyroid gland

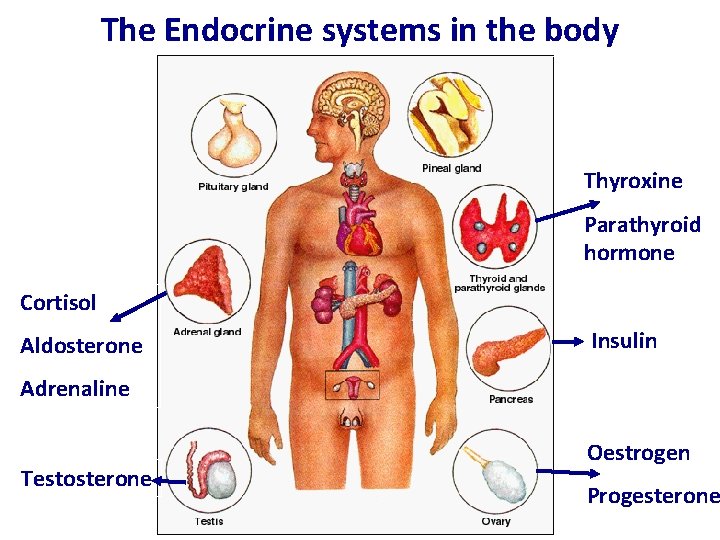
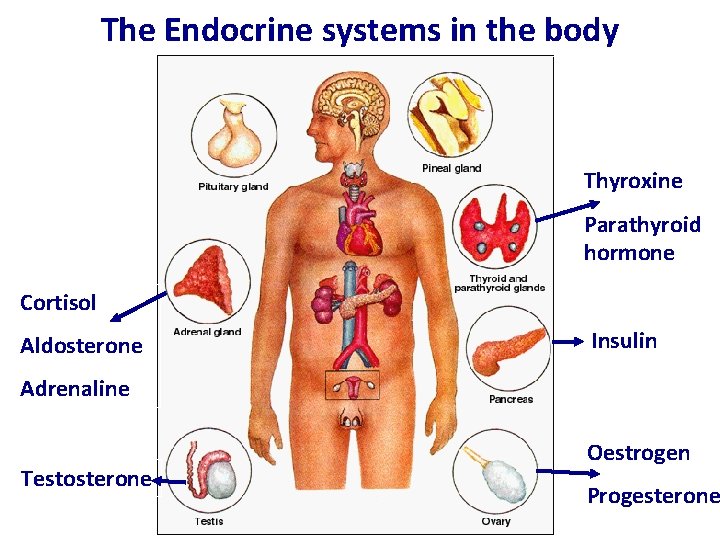
The Endocrine systems in the body Thyroxine Parathyroid hormone Cortisol Aldosterone Insulin Adrenaline Testosterone Oestrogen Progesterone

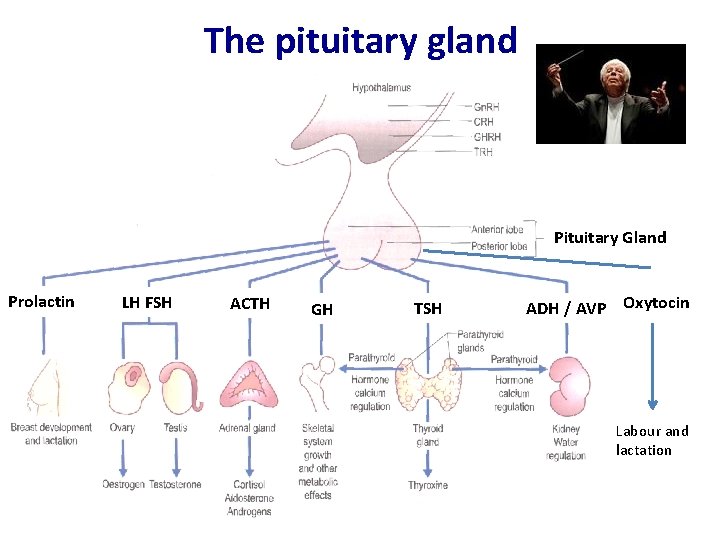
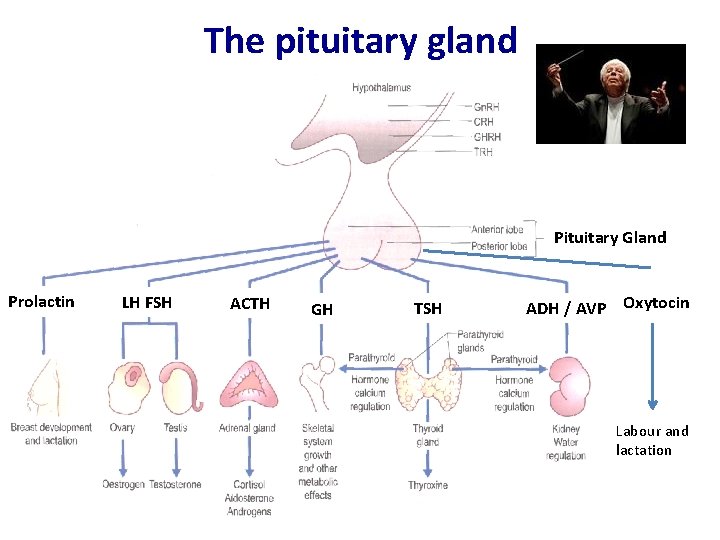
The pituitary gland Pituitary Gland Prolactin LH FSH ACTH GH TSH ADH / AVP Oxytocin Labour and lactation L

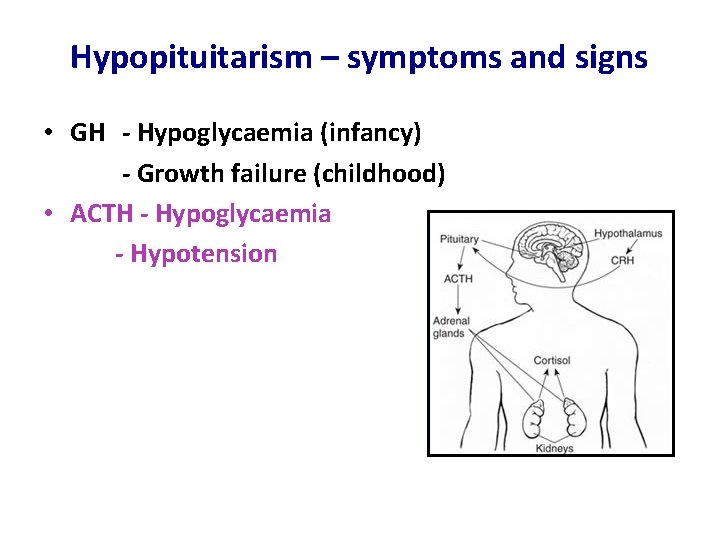
Hypopituitarism – symptoms and signs • GH - Hypoglycaemia (infancy) - Growth failure (childhood)

Hypopituitarism – symptoms and signs • GH - Hypoglycaemia (infancy) - Growth failure (childhood) • ACTH - Hypoglycaemia - Hypotension

Hypopituitarism – symptoms and signs • GH - Hypoglycaemia (infancy) - Growth failure (childhood) • ACTH - Hypoglycaemia - Hypotension • LH - Micropenis / UDT - Failure of puberty

Hypopituitarism – symptoms and signs • GH - Hypoglycaemia (infancy) - Growth failure (childhood) • ACTH - Hypoglycaemia - Hypotension • LH - Micropenis / UDT - Failure of puberty • TSH - Jaundice (unconjugated) - Coarse facial features - Poor growth - Tiredness, dry skin, hair loss

Hypopituitarism – symptoms and signs • GH - Hypoglycaemia (infancy) - Growth failure (childhood) • ACTH - Hypoglycaemia - Hypotension • LH - Micropenis / UDT - Failure of puberty • TSH - Jaundice - Poor growth - Tiredness, dry skin, hair loss • ADH - Cranial Diabetes insipidus

Hypopituitarism - treatment GH (recombinant) - SC injections OD Hydrocortisone - oral TDS or QDS Levothyroxine - oral OD Testosterone injections, topical gel (neonatal, pubertal) Oestrogen (oral, patches) LH and FSH (recombinant) injections • DDAVP (oral, sublingual, nasal) • •

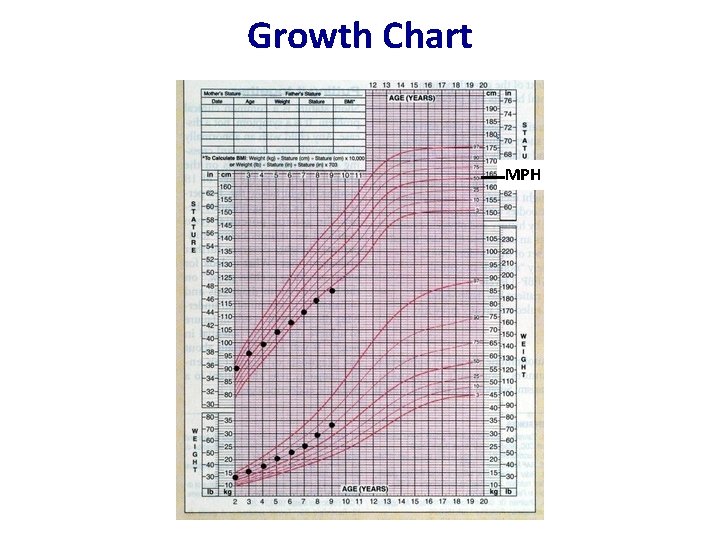
Case 1: 10 yr old girl with short stature • • • Short stature Normal birth weight Poor growth since aged 3 yr Reduced appetite HV 3. 0 cm/yr

Growth Chart MPH

Case 1: 10 yr old girl with short stature • • Short stature Normal birth weight Poor growth since aged 3 yr Reduced appetite HV 3. 0 cm/yr Peak GH 3 μg/L (>7) IGF-1 50 ng/L (70 -300) What is the most likely diagnosis?

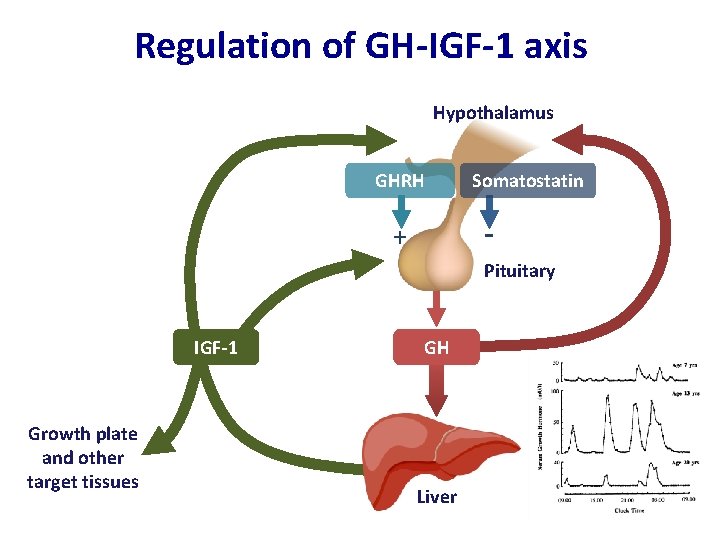
Regulation of GH-IGF-1 axis Hypothalamus GHRH Somatostatin - + Pituitary IGF-1 Growth plate and other target tissues GH Liver

Control of Human Growth • Internal cues: Genotype • External Factors: Nutrition Environment • Internal signalling: Hormones Growth Factors

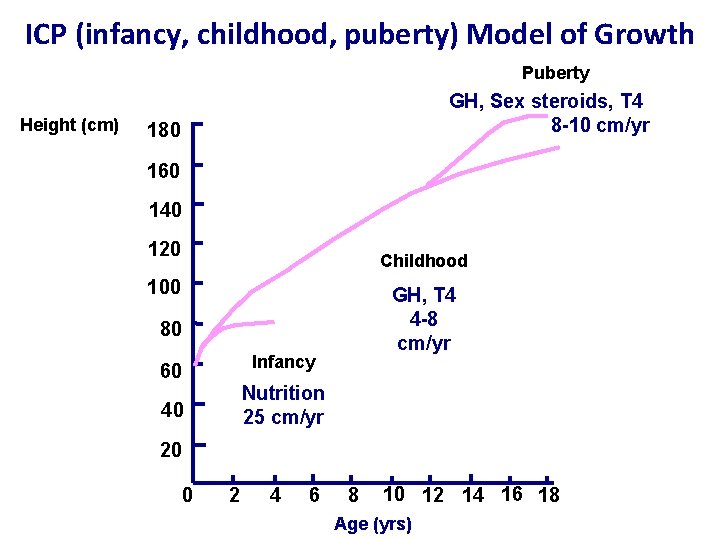
ICP (infancy, childhood, puberty) Model of Growth Puberty Height (cm) GH, Sex steroids, T 4 8 -10 cm/yr 180 160 140 120 Childhood 100 GH, T 4 4 -8 cm/yr 80 Infancy 60 Nutrition 25 cm/yr 40 20 0 2 4 6 8 10 12 14 16 18 Age (yrs)

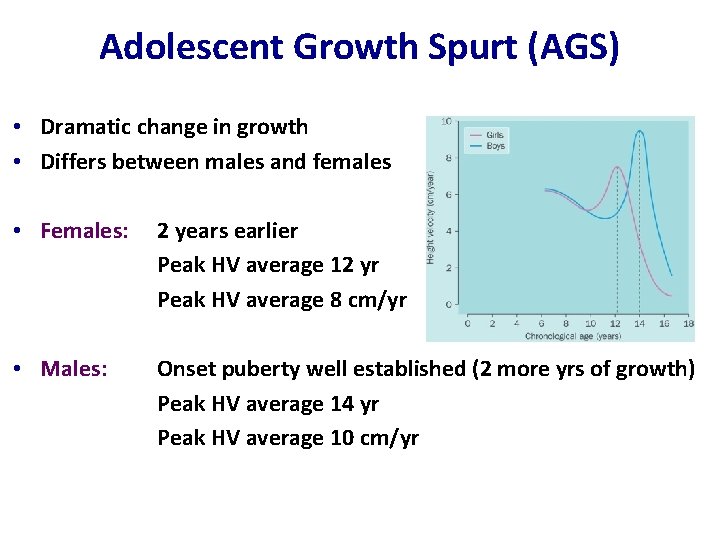
Adolescent Growth Spurt (AGS) • Dramatic change in growth • Differs between males and females • Females: 2 years earlier Peak HV average 12 yr Peak HV average 8 cm/yr • Males: Onset puberty well established (2 more yrs of growth) Peak HV average 14 yr Peak HV average 10 cm/yr

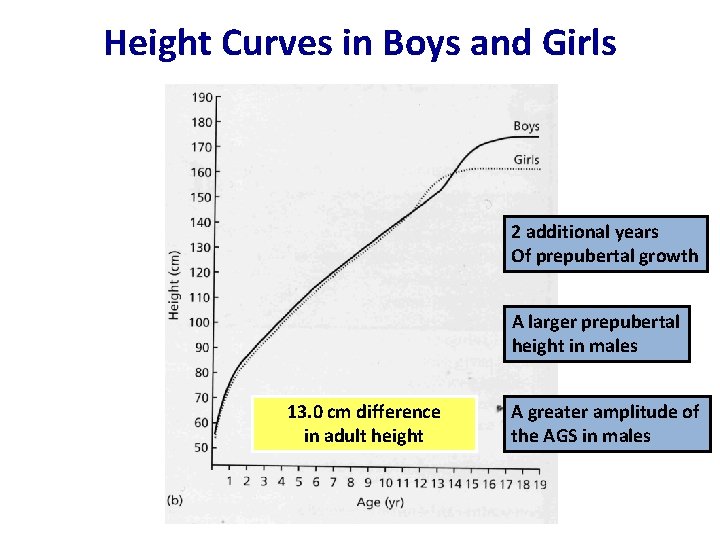
Height Curves in Boys and Girls 2 additional years Of prepubertal growth A larger prepubertal height in males 13. 0 cm difference in adult height A greater amplitude of the AGS in males

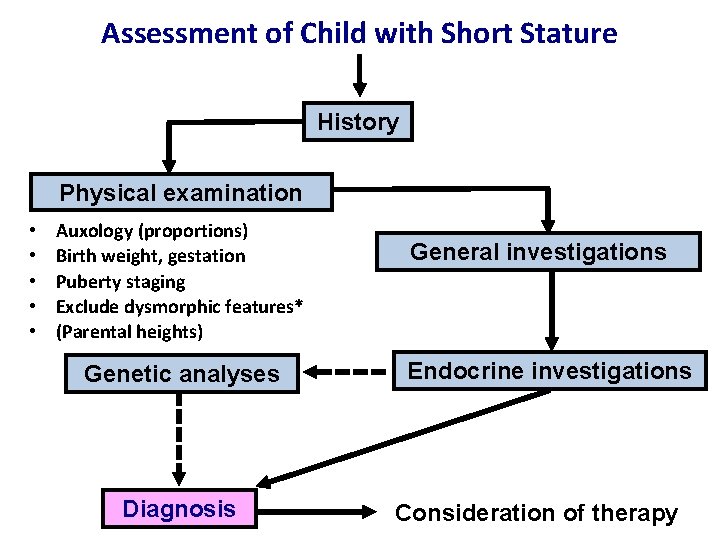
Assessment of Child with Short Stature History Physical examination • • • Auxology (proportions) Birth weight, gestation Puberty staging Exclude dysmorphic features* (Parental heights) Genetic analyses Diagnosis General investigations Endocrine investigations Consideration of therapy

Causes of Growth Failure • Chronic disease (renal failure, asthma, coeliac disease) • Psychosocial deprivation • Familial (genetic) short stature • Short stature following Small for Gestational age (SGA) at birth • Constitutional delay of growth and puberty (CDGP) • Dysmorphic Syndromes: Turner, Noonan, Silver Russell, skeletal dysplasias • Endocrine causes (rare): GHD, hypothyroidism, Cushing’s syndrome

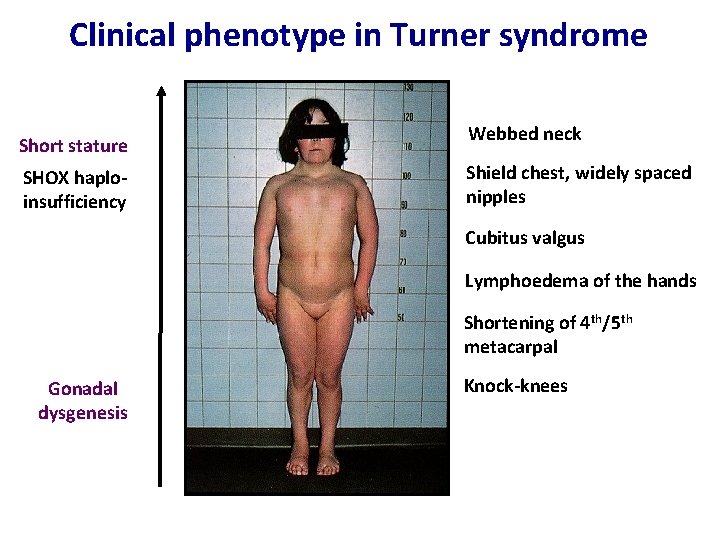
Clinical phenotype in Turner syndrome Short stature SHOX haploinsufficiency Webbed neck Shield chest, widely spaced nipples Cubitus valgus Lymphoedema of the hands Shortening of 4 th/5 th metacarpal Gonadal dysgenesis Knock-knees

Low weight, normal height • general paediatrics

Puberty – some definitions Adrenarche Onset of androgen dependent changes e. g. pubic and axillary hair, body odour, acne Thelarche Onset of female breast development Puberty Development of secondary sexual characteristics. Attain reproductive capacity Menarche Onset of menstruation

Factors that influence the timing and onset of Puberty Genetic Background Environment PUBERTAL DEVELOPMENT General Health of child

Definition of normal puberty GIRLS: Puberty development after the age of 8 years (mean 10 yr) BOYS: Puberty development after the age of 9 years (mean 12 yr)

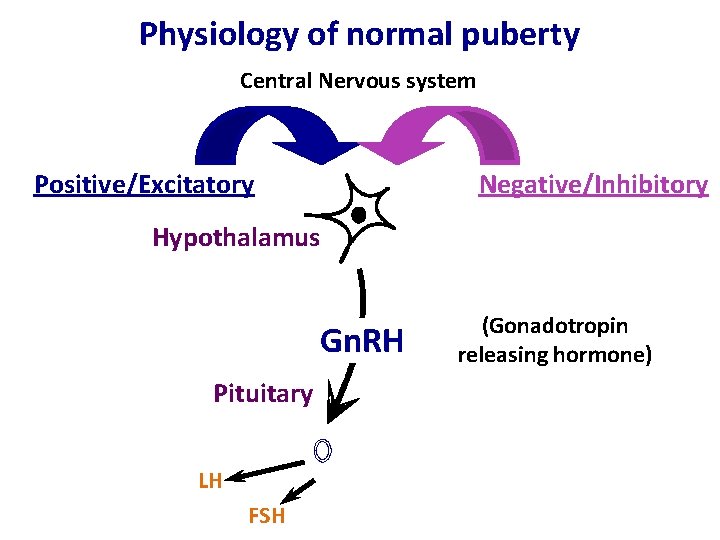
Physiology of normal puberty Central Nervous system Positive/Excitatory Negative/Inhibitory Hypothalamus Gn. RH Pituitary LH FSH (Gonadotropin releasing hormone)

Clinical aspects of normal puberty • Females: Breast (B) development • Males: Genital (G) development Testicular volume • Both: Pubic hair (P) development Axillary (A) hair development Tanner Stages of Puberty (1 prepubertal, 5 mature)

Prader orchidometer Peak HV Start of AGS Puberty onset

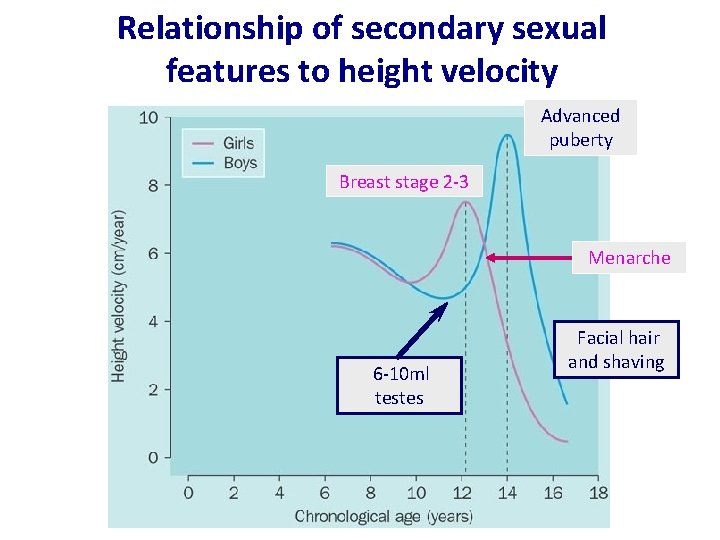
Relationship of secondary sexual features to height velocity Advanced puberty Breast stage 2 -3 Menarche 6 -10 ml testes Facial hair and shaving

Too early ‘puberty’ • Pubarche: – pubic hair, axillary hair, acne, mature body odour – Early: girls <8 yrs, boys <9 yrs • Puberty: – Boys (testicular enlargement): • Early <9 yrs • Girls (breast development): early <8 yrs

The pituitary gland Pituitary Gland Prolactin LH FSH ACTH GH TSH ADH / AVP Oxytocin Labour and lactation L

Pubarche vs. puberty • • Adrenal vs. pituitary gland Different causes But… Premature adrenarche can trigger precocious puberty

Early (precocious) puberty Central precocious puberty: pubertal development caused by early activation of the hypothalamic-pituitary-gonadal axis Peripheral precocious puberty: pubertal development caused by sex steroids secreted without activation of the hypothalamicpituitary-gonadal axis

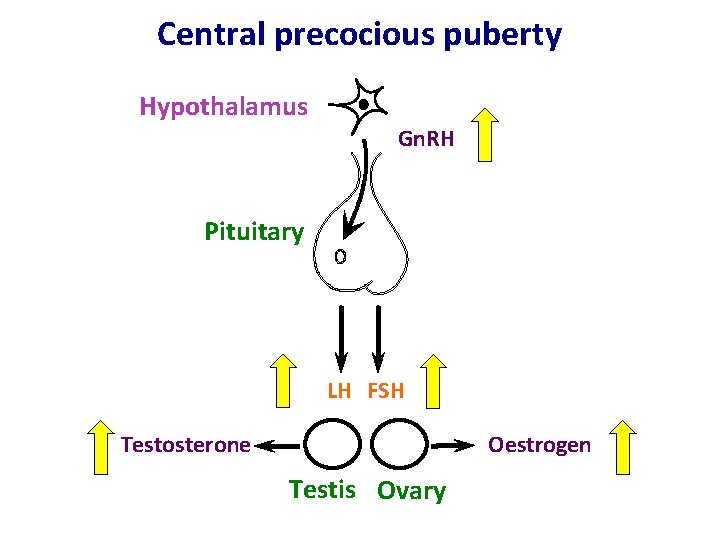
Central precocious puberty Hypothalamus Gn. RH Pituitary LH FSH Oestrogen Testosterone Testis Ovary

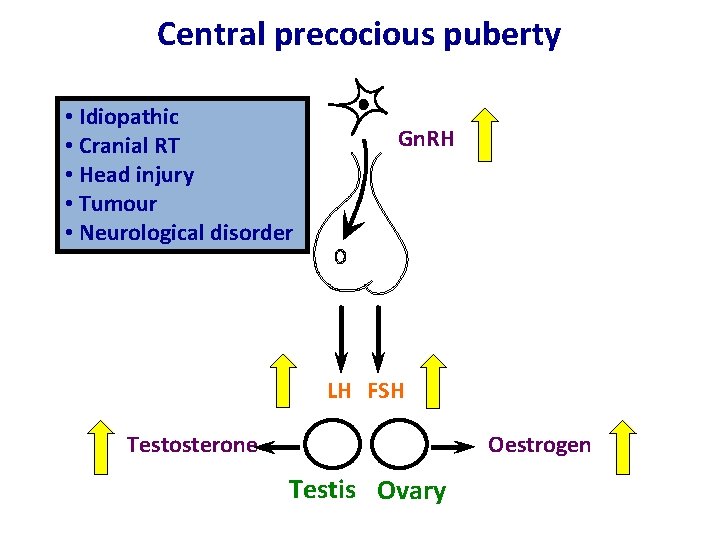
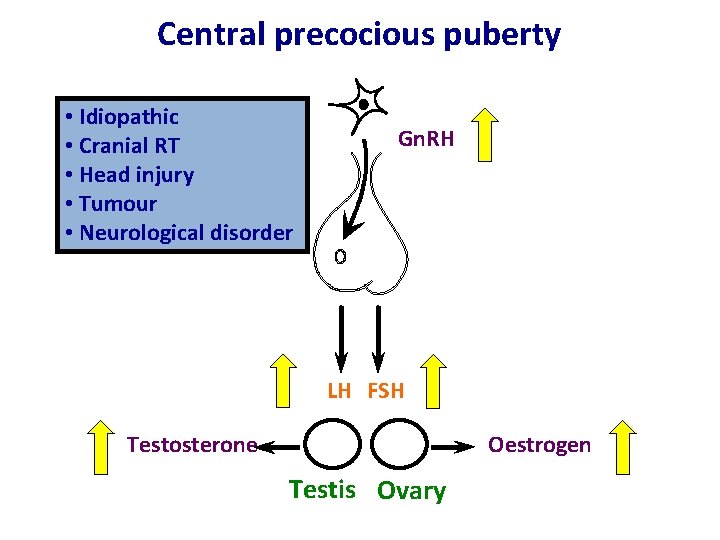
Central precocious puberty Hypothalamus • Idiopathic • Cranial RT • Head injury • Tumour • Neurological. Pituitary disorder Gn. RH LH FSH Oestrogen Testosterone Testis Ovary

Investigation of Precocious Puberty History, Family history Physical examination: • Cutaneous lesions e. g neurofibromatosis, Mc. Cune Albright syndrome • CNS examination - Fundi Auxology: • Pubertal staging (Tanner) + size of testes • Height, weight, MPH, growth velocity • Bone age

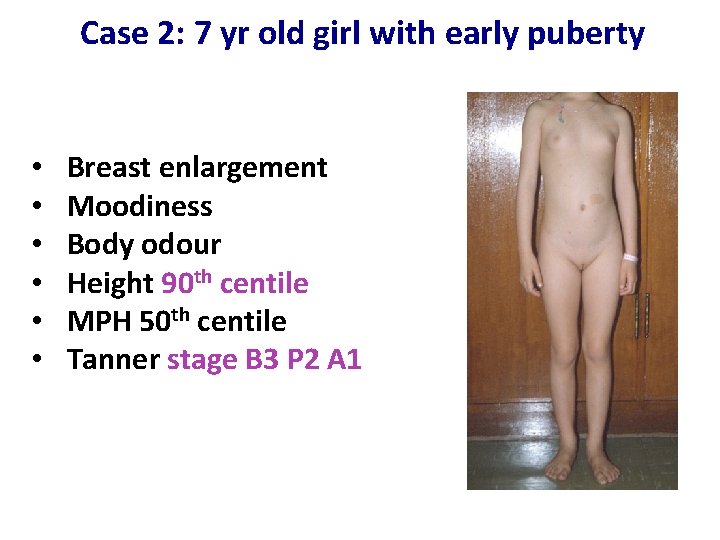
Case 2: 7 yr old girl with early puberty • • • Breast enlargement Moodiness Body odour Height 90 th centile MPH 50 th centile Tanner stage B 3 P 2 A 1

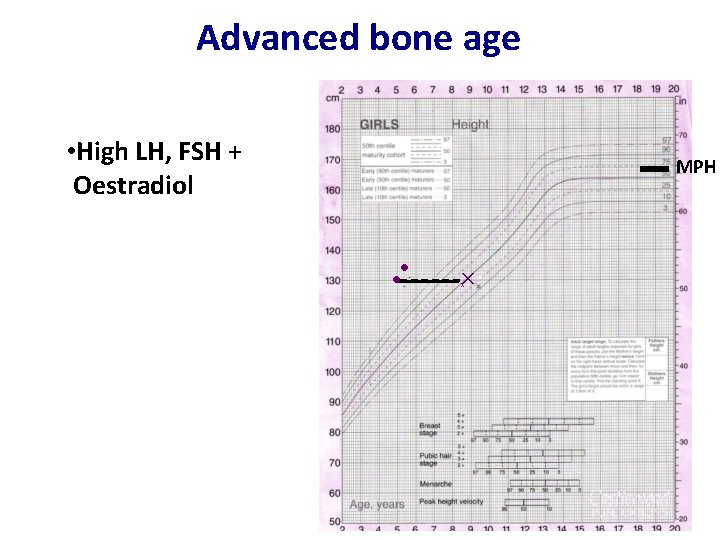
Advanced bone age • High LH, FSH + Oestradiol MPH × x

Central precocious puberty Hypothalamus • Idiopathic • Cranial RT • Head injury • Tumour • Neurological. Pituitary disorder Gn. RH LH FSH Oestrogen Testosterone Testis Ovary

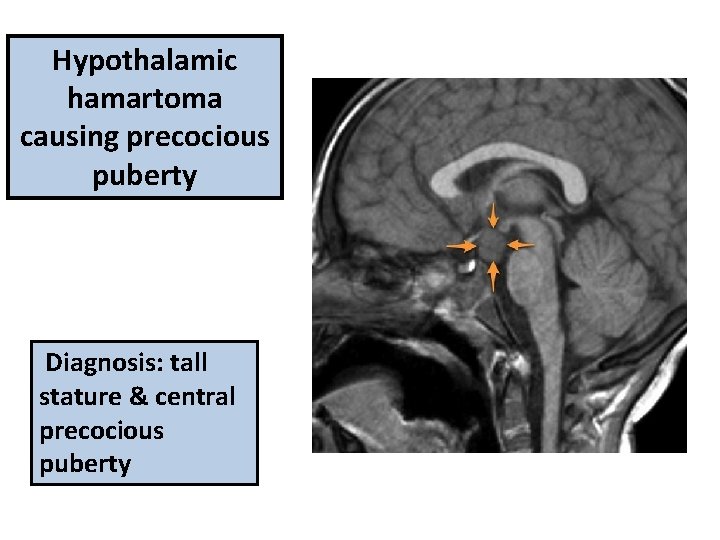
Hypothalamic hamartoma causing precocious puberty Diagnosis: tall stature & central precocious puberty

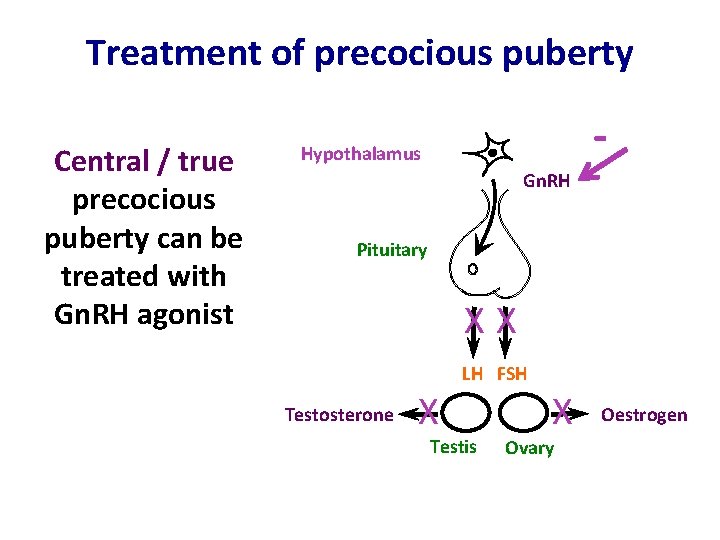
Treatment of precocious puberty Central / true precocious puberty can be treated with Gn. RH agonist - Hypothalamus Gn. RH Pituitary XX LH FSH Testosterone X Testis X Ovary Oestrogen

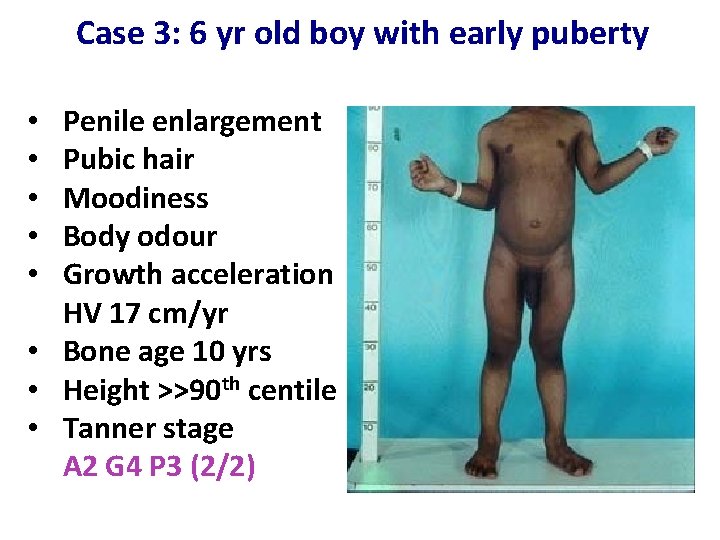
Case 3: 6 yr old boy with early puberty Penile enlargement Pubic hair Moodiness Body odour Growth acceleration HV 17 cm/yr • Bone age 10 yrs • Height >>90 th centile • Tanner stage A 2 G 4 P 3 (2/2) • • •

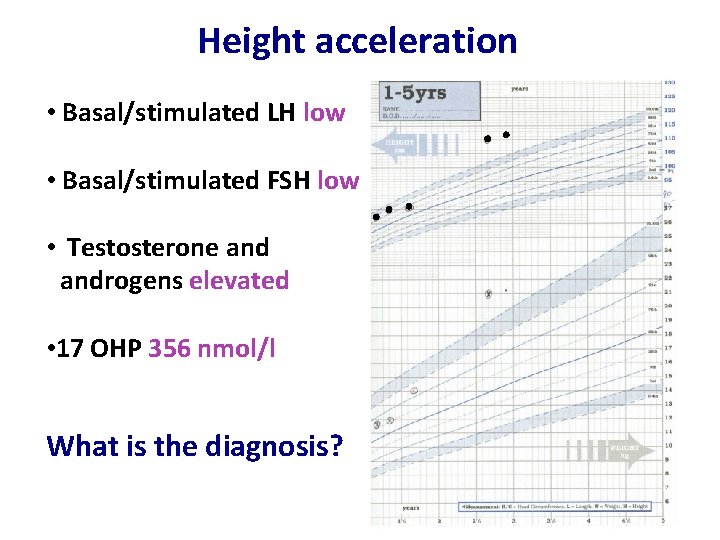
Height acceleration • Basal/stimulated LH low • Basal/stimulated FSH low • Testosterone androgens elevated • 17 OHP 356 nmol/l What is the diagnosis?

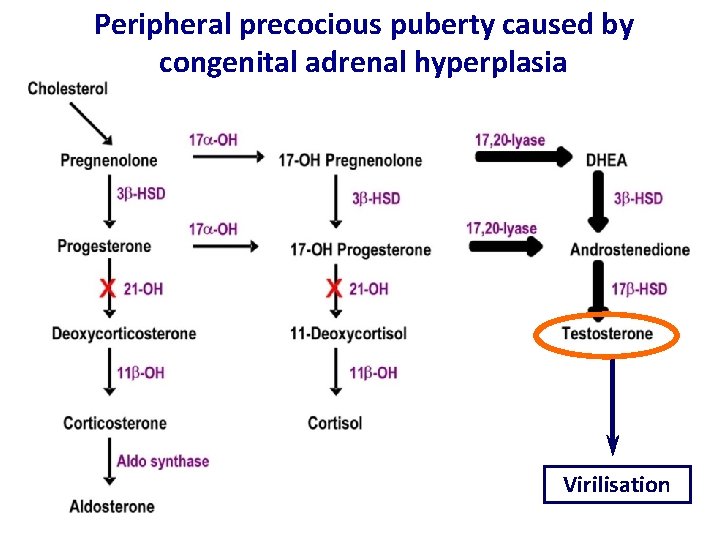
Peripheral precocious puberty caused by congenital adrenal hyperplasia Virilisation

Treatment of precocious puberty Pseudo-precocious puberty is managed by treating the primary problem For example adrenal tumour or congenital adrenal hyperplasia Thereafter consider Gn. RHa

Delayed puberty • More common in boys than girls • Boys (testicular enlargement): • Late >14 yrs • Girls (breast development): • Late >13 yrs (menarche >15 yrs)

Concerns re penile size • • • Age? Testes descended? Hypospadias? Obesity? Suprapubic fat pad? Management: – If otherwise healthy and not yet 14: wait and see – Overweight/obese: explanation re suprapubic fat pads, weight loss

Causes of delayed puberty • Constitutional delay in growth and puberty • Chronic disease • Central causes: Tumour/irradiation/trauma Gn. RH or gonadotropin (LH/FSH) deficiency • Peripheral causes: Testicular damage / cryptorchidism Gonadal dysgenesis (Turner’s, Klinefelter’s) Irradiation/chemotherapy

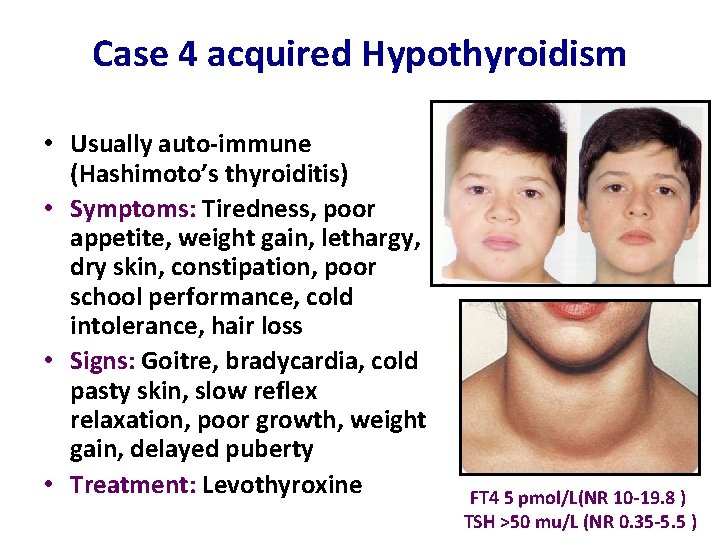
Case 4 acquired Hypothyroidism • Usually auto-immune (Hashimoto’s thyroiditis) • Symptoms: Tiredness, poor appetite, weight gain, lethargy, dry skin, constipation, poor school performance, cold intolerance, hair loss • Signs: Goitre, bradycardia, cold pasty skin, slow reflex relaxation, poor growth, weight gain, delayed puberty • Treatment: Levothyroxine FT 4 5 pmol/L(NR 10 -19. 8 ) TSH >50 mu/L (NR 0. 35 -5. 5 )

Case 5: Subclinical hypothyroidism • 12 yr old girl • Tired and hair loss • Investigations: – TSH 5. 6 m. U/l (N: 0. 27 -4. 2) – FT 4 18 pmol/l (N: 10. 5 -24. 5) • Refer? • Anti-TPO antibodies: – Positive -> monitor annually, refer if TSH >10 or FT 4 low – Negative: unlikely to develop hypothyroidism, if TSH>6, repeat in 3 -6 mo time

Case 6 acquired Hyperthyroidism • Usually auto-immune (Graves’ disease) • Symptoms: Anxiety, increased appetite, hyperactivity, weight loss, heat intolerance, sleep disturbance, diarrhoea, deteriorating school performance • Signs: Goitre, tachycardia, sweatiness, exophthalmos, tremor, tall stature • Treatment: Antithyroid drugs FT 4 >50 pmol/L (NR 10 -19. 8 ) TSH <0. 01 mu/L (NR 0. 35 -5. 5 )

Overt hypo- or hyperthyroidism • Please contact us: • Paed endocrine registrar/consultant via switchboard RLH • Hypothyroidism: start treatment prior to appt • Hyperthyroidism: – needs to be seen urgently – A&E/ ad hoc appt

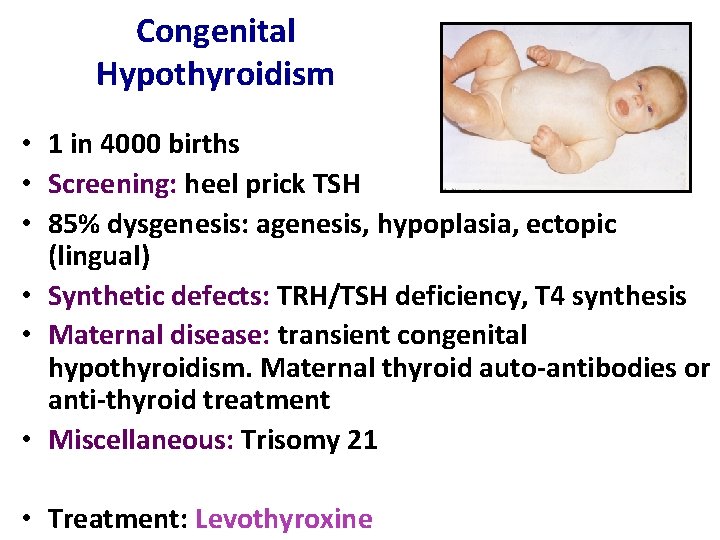
Congenital Hypothyroidism • 1 in 4000 births • Screening: heel prick TSH • 85% dysgenesis: agenesis, hypoplasia, ectopic (lingual) • Synthetic defects: TRH/TSH deficiency, T 4 synthesis • Maternal disease: transient congenital hypothyroidism. Maternal thyroid auto-antibodies or anti-thyroid treatment • Miscellaneous: Trisomy 21 • Treatment: Levothyroxine

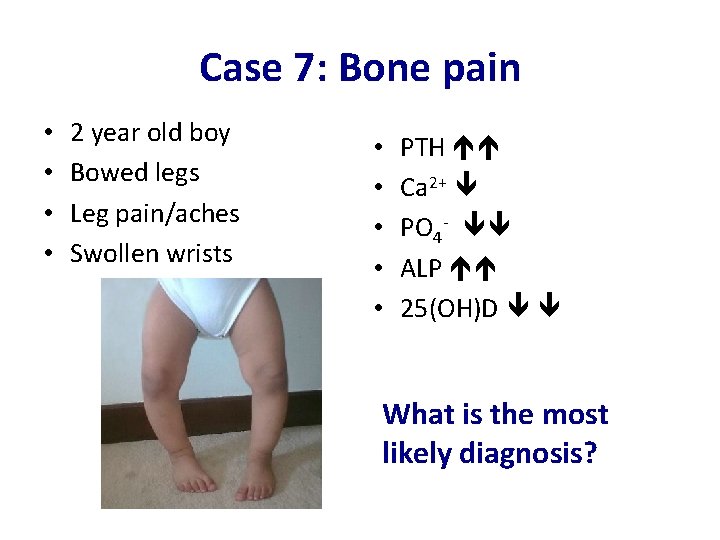
Case 7: Bone pain • • 2 year old boy Bowed legs Leg pain/aches Swollen wrists • • • PTH Ca 2+ PO 4 - ALP 25(OH)D What is the most likely diagnosis?

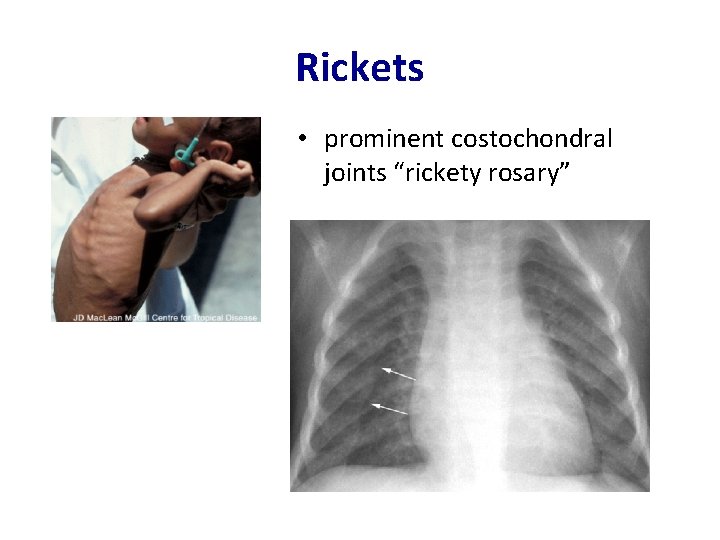
Rickets • prominent costochondral joints “rickety rosary”

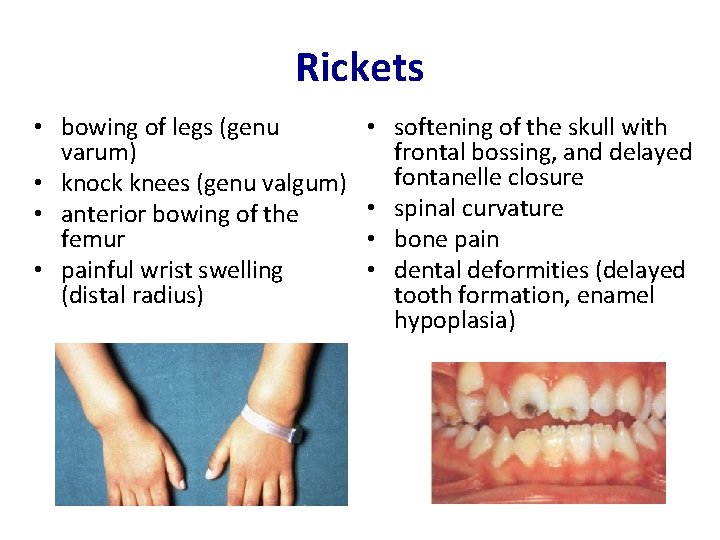
Rickets • bowing of legs (genu varum) • knock knees (genu valgum) • anterior bowing of the femur • painful wrist swelling (distal radius) • softening of the skull with frontal bossing, and delayed fontanelle closure • spinal curvature • bone pain • dental deformities (delayed tooth formation, enamel hypoplasia)

Vitamin D levels - 25(OH)D • Vitamin D deficiency = < 25 nmol/L • Vitamin D insufficiency = 25 - 50 nmol/L • Vitamin D adequate = > 50 nmol/L • More at risk of vitamin D deficiency if less exposure to sunlight, darker skin, limited diet.

Prevention and Management • Primary prevention: – At risk breastfed infants from birth – Formula (containing Vitamin D) fed infants who take less than 500 m. L of formula/day – Children 6 months to 5 years of age • Rickets treatment: – 12 week high dose oral daily dosing colecalciferol • On-going supplementation: – previously treated for rickets or vitamin D deficiency – Children from ethnic minorities who have darker skin – Children who are not exposed to much sun

The Endocrine systems in the body Thyroxine Parathyroid hormone Cortisol Aldosterone Insulin Adrenaline Testosterone Oestrogen Progesterone

Summary • Overview of most common paediatric endocrine conditions • If in doubt please contact us: – Paediatric endo registrar via switchboard RLH

Any questions?