Childhood Disorders Externalizing Disorders Intellectual Disability SW 8340

Childhood Disorders Externalizing Disorders Intellectual Disability SW 8340 A. Antonio González-Prendes, Ph. D. School of Social Work Wayne State University

Externalizing Disorders • Disorders of childhood or adolescence characterized by: – Disruptive behaviors; Impulsive; Hyperactive; Aggressiveness; Delinquency…. • Conflict with his/her social world’s rules and expectations. • Primary problem: behavioral • Secondary problem: emotional • Two domains of externalizing disorders – ADHD • Characterized by: Poor academic achievement, poor executive functioning (attention, concentration), parental inattention and impulsivity. – Conduct problems • Characterized by: socioeconomic disadvantages , dysfunctional family background, parental criminality and antisocial behaviors. • Two main diagnoses are: – Oppositional defiant disorders. – Conduct disorders.

Risk Factors • Risk factors that create a vulnerability for externalizing disorder are multiple. – Risk factors are not causative • General categories may include: – Individual • Poor impulse control, social skills and emotional regulation; low intelligence. – Familial • Parental psychopathology, inadequate parenting, drug use, disruptive/chaotic home life, etc. – Genetic – Social • Deviant peer group, poor school performance, truancy, delinquency, etc. – Environmental • Exposure to violence, living in high crime areas, environmental toxins, poverty, lack of educational/vocational opportunities.
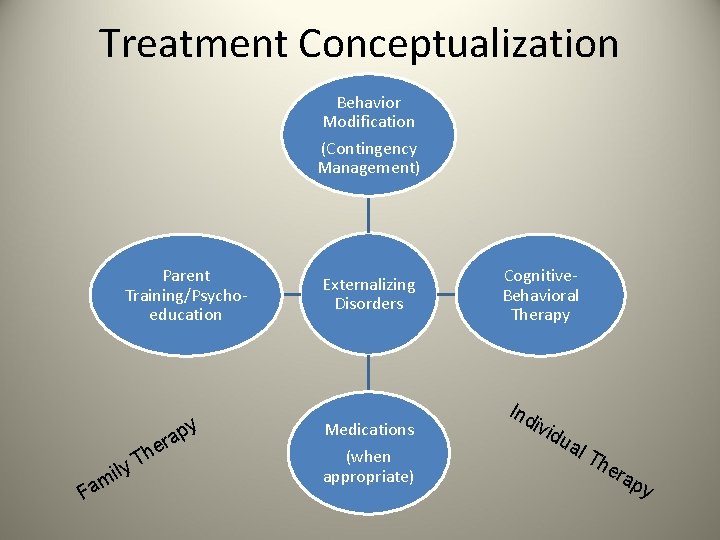
Treatment Conceptualization Behavior Modification (Contingency Management) Parent Training/Psychoeducation he y p a r Fa m T ily Externalizing Disorders Medications (when appropriate) Cognitive. Behavioral Therapy Ind ivid ua l Th era py

Attention-Deficit Hyperactivity Disorder (ADHD) • Types: 1) Hyperactive/Impulsive (18%); 2) Inattentive(27%); 3) Combined (55%). • The triad of ADHD symptoms: Hyperactivity Impulsivity Inattention • Russell Barkley suggests that ADHD involves a motivational deficit. • Symptoms show fluctuations according to situational demands and child’s degree of interest in the task at hand (Anastopoulos et al. , 2003, coursepack).

ADHD • Behavioral manifestation of inattentive symptoms: – – – – – Failing to give attention to details, careless at school or work. Difficulty staying focused on tasks: work or play. Does not seem to listen when spoken to directly; appears distracted. Does not follow through with instructions; gets sidetracked; loses focus. Poor at organizing or managing tasks and activities. Avoids/dislikes tasks that required sustained mental effort. Often loses things necessary for tasks or activities Easily distracted by extraneous stimuli. Forgetful in daily activities. • Six or more of these signs must be present for children and 5 or more for adolescents and adults over a 6 month period.

ADHD • Behavioral manifestations of hyperactive/impulsive symptoms: – – – – Fidgety, taps hands or feet, squirming. Leaves seat unexpectedly and inappropriately. Runs or climbs in inappropriate situations; restlessness. Cannot play or engage in pleasure activities quietly. Often “on the go”; difficulties being still for extended time. Blurts out answers before question is completed; cannot wait his/her turn. Cuts in line or in play activities. Often interrupts or intrudes on others. • Six or more of these signs must be present for children and 5 or more for adolescents and adults over a 6 month period. • Several of the hyperactive/impulsive symptoms must have been present prior to age 12.

Prevalence • DSM 5 states that about 5% of children have ADHD; 2. 5% of adults. • Sadock and Sadock(2007): 4% prevalence in the general population with 3% 7% of pre-pubertal school children. • According to the CDC (http: //www. cdc. gov/ncbddd/adhd/data. html): – Approximately 11% of children 4 -17 years of age (6. 4 million) have been diagnosed with ADHD as of 2011. – The percentage of children with an ADHD diagnosis has increased from 7. 8% in 2003 to 9. 5% in 2007 and to 11. 0% in 2011. – 1997 -2006: 3% increase in ADHD diagnoses; 2003 -2011: 5% increase. – Boys (13. 2%) were more likely than girls (5. 6%) to have ever been diagnosed with ADHD. – Average of diagnosis = 7 years of age. – Prevalence of ADHD diagnosis by state In the USA: – Highest prevalence: Kentucky 18. 7%. – Lowest prevalence: Nevada 5. 6% • Boys to girls ratio varies from 2: 1 to 9: 1 (Sadock & Sadock, 2007).

ADHD – Etiology (Anastopoulos et al. coursepack) • Inconsistent findings. • Biological factors – various hypotheses have been put forth. Multiple pathways may lead to ADHD. Abnormalities in brain chemistry, brain structure, brain function. Genetic components. Dopamine deficiencies in the frontostriatal circuitry of the brain affect cognitive control deficits in ADHD. – Pregnancy complications associated with excessive use of alcohol or nicotine by the mother. – Post-natal factors: head injury, elevated lead levels – –

ADHD – Etiology (continued). • Little empirical support for the social environment (e. g. poor parenting, poverty, etc. ) causing ADHD. • Twins studies show that among monozygotic (identical) concordance rates are 58% to 82% for ADHD, and 31% to 38% rates for dizygotic twins (Willcut et al. , 2000). • According to Faraone and Doyle (2000) twin studies have found genetic influence on hyperactivity and inattentive symptoms: – Heritability of hyperactivity ranges from 64% to 91%. – Heritability of inattention ranges from 39% to 98%.

ADHD • Developmental course (Anastopoulos et al. course pack) – Most symptoms appear around ages 3 to 4. – 50% to 80% of children diagnosed with ADHD continue to meet criteria as adolescents. – 30% will continue to meet criteria as adults and 50% will have subclinical levels of ADHD. • Comorbidity – 50% of children with ADHD have either CD or ODD and about 65% - 90% of children diagnosed with either ODD or CD also have ADHD (Kimonis & Frick, 2013) – Oppositional defiant disorder – 33. 3%; 54% - 84%. – Conduct disorder – 25% – Anxiety disorder > 25% – Learning disorder – 45%

ADHD - Assessment • Diagnosing ADHD should be done only after a careful and detailed assessment of the child’s (or adult’s) behaviors and environment. – Detail history of the behavior obtained from collateral sources. – Medical examination by pediatrician or psychiatrist specializing in childhood disorders to rule out any medical conditions. – Multimodal Assessment – Parent – teacher observations in various settings (e. g. home, school, playground, social settings, etc. ). – Behavioral assessment with standardized rating scales (e. g. Conner’s Rating Scale, 3 rd ed. , 2009). – Child interview (not as reliable as parent- teacher input).

Treatment of ADHD • Standard treatment – Medication: Ritalin, Concerta, Adderall (stimulants); Strattera (nonstimulant) – Behavior therapy • Behavior modification • Contingency management • Social skills – Cognitive therapy • Child – Restructure distorted thinking about the self. • Parents – Adopt a more realistic perception of ADHD. – Reframe perception of the child (e. g. to eliminate anger). – Parent skills training (i. e. parenting) and education • Recognize situational variability regarding presence of symptoms. • Help parents learn to manage environmental cues and tasks around the child. – Address comorbid disorders when present (e. g. depression etc. )

Disruptive disorders - ODD • Oppositional defiant disorder (ODD) • Enduring pattern of negativistic, hostile, defiant behavior towards authority figures and lasting at least 6 months. • Characterized by argumentativeness, refusal to comply with rules, deliberately annoying others, easily annoyed by others, deflecting his/her responsibility by blaming others, anger, vindictive.

Disruptive Disorders - CD • Conduct disorder – Enduring pattern of behavior that violates the right of others as well as major age-appropriate societal norms. Childhood type: onset of symptoms prior to age 10. Adolescent type: absence of symptoms prior to age 10. If age 18, must not meet criteria for Antisocial Personality Disorder. Characterized by the presence of 3 of the following criteria in the past 12 months and at least one in the past 6 months. • Characteristics: • • – Aggression to people and animals (e. g. bullying, fighting, assault with weapons, mugging/robbing others, cruelty to people or animals, forced sexual activity). – Destruction of property (e. g. fire setting) – Deceitfulness or theft (e. g. breaking & entering, stealing). – Serious violations of rules (e. g. stays out at night, truancy, runs away from home).

General Framework for Treatment of Disruptive Disorders • Multimodal treatment approaches that may include: – Behavior modification (contingency management) • Reinforce desired behaviors: reward systems, token economy, • Social skills training, problem solving, role-playing, reverse role-playing. – Cognitive therapy: that is congruent with cognitive development • Problem-solving, self-instructional training – Psychoeducation/training of parents on… • Understanding the disorder. • Child management skills: how to respond effectively to the child’s behavior ; how to use behavior modification to reward non-aggressive, pro-social behaviors; use of discipline measures (i. e. time-out, etc. ) – Pharmacotherapy if indicated – Individual and family therapy. – For children with violent or aggressive behaviors treatment may focus on creating a supportive and structured environment to reduce and eventually eliminate violence and aggression. This may include among others: • Peer-support programs; clearly defined and consistent rules; clearly defined consequences; responding to crisis and the threat of violence.

Intellectual Developmental Disorder (DSM-5) Mental Retardation (DSM-IV) • DSM-5 no longer uses the term “mental retardation”. • Intelligence Quotient (IQ) – “Classification of a total test score in relation to norms established by a group” – “IQ is a measure of present functioning ability. It does not measure future potential” (Sadock & Sadock, 2007, p. 178) • Standardized IQ scores – Wechsler Adult Intelligence Scale ( age 16) – Wechsler Intelligence Scale for Children (age = 7 -16) – Wechsler Preschool and Primary Scale for Intelligence (age = 3 -7) • Mean = 100 • Standard deviation = 15 • Mental retardation/Intellectual disability = 2 SD’s below the mean
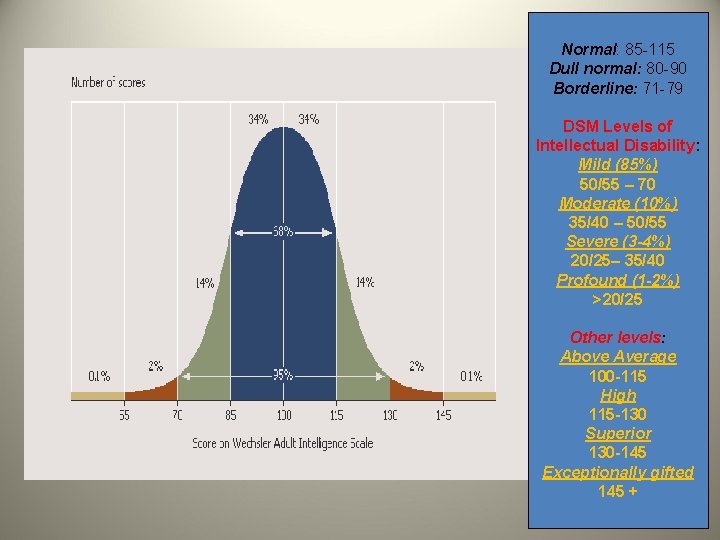
Normal: 85 -115 Dull normal: 80 -90 Borderline: 71 -79 DSM Levels of Intellectual Disability: Mild (85%) 50/55 – 70 Moderate (10%) 35/40 – 50/55 Severe (3 -4%) 20/25– 35/40 Profound (1 -2%) >20/25 Other levels: Above Average 100 -115 High 115 -130 Superior 130 -145 Exceptionally gifted 145 +
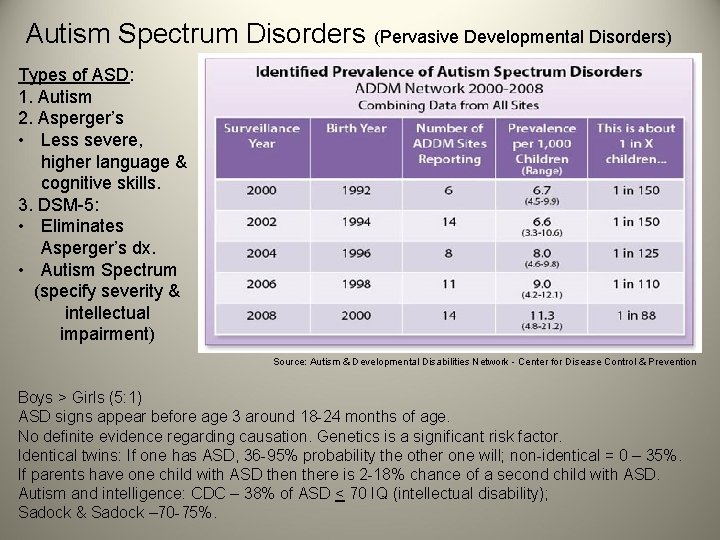
Autism Spectrum Disorders (Pervasive Developmental Disorders) Types of ASD: 1. Autism 2. Asperger’s • Less severe, higher language & cognitive skills. 3. DSM-5: • Eliminates Asperger’s dx. • Autism Spectrum (specify severity & intellectual impairment) Source: Autism & Developmental Disabilities Network - Center for Disease Control & Prevention Boys > Girls (5: 1) ASD signs appear before age 3 around 18 -24 months of age. No definite evidence regarding causation. Genetics is a significant risk factor. Identical twins: If one has ASD, 36 -95% probability the other one will; non-identical = 0 – 35%. If parents have one child with ASD then there is 2 -18% chance of a second child with ASD. Autism and intelligence: CDC – 38% of ASD < 70 IQ (intellectual disability); Sadock & Sadock – 70 -75%.

Signs of possible ASD: Signs of possible ASD (cont. ): Not responding to name by 12 mos. of age. Not pointing at objects to show interest. Not playing “pretend” games. Avoiding eye contact & wanting to be alone. Trouble understanding others’ feelings or talking about their feelings. Have delayed speech and language skills. Repeat words and phrases over and over. Giving unrelated answers to questions. Getting upset by minor changes Obsessive interests. Flapping hands, rocking the body, spinning in circles. Unusual reactions to sounds, smells, tastes, sights, sensations. Treatment: Behavioral treatments and/or medications. • There is no cure for ASD. Medications can help the individual function better by curbing aggressive behaviors, hyperactivity, controlling seizures, managing mood, etc. • Early intervention improves development (e. g. walk, talk) social interaction, learn skills. • Behavior management and communication approaches – Applied Behavior Analysis. See: www. autismspeaks. org • Tailored to the person’s needs; positive reinforcement (reward) of desired behaviors & social skills, discourage (no reinforcement) negative behaviors. • Parental education and support. • Occupational therapy, speech therapy, sensory integration therapy. NCBDDD: National Board of Birth Defects and Developmental Disabilities
- Slides: 20