Chickenpox Causative agent VaricellaZoster virus Herpes virus One




![[INSERT DISEASE AT A GLANCE 19. 7] [INSERT DISEASE AT A GLANCE 19. 7]](https://slidetodoc.com/presentation_image/3fb7617a248b4d7883115c2e16d6d52d/image-7.jpg)





![[INSERT TABLE 19. 4] [INSERT TABLE 19. 4]](https://slidetodoc.com/presentation_image/3fb7617a248b4d7883115c2e16d6d52d/image-18.jpg)







![[INSERT TABLE 19. 5] [INSERT TABLE 19. 5]](https://slidetodoc.com/presentation_image/3fb7617a248b4d7883115c2e16d6d52d/image-29.jpg)


- Slides: 31

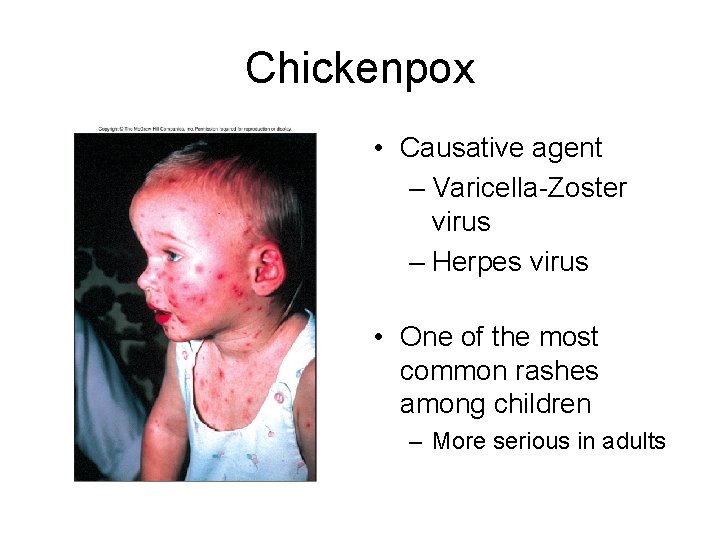
Chickenpox • Causative agent – Varicella-Zoster virus – Herpes virus • One of the most common rashes among children – More serious in adults

• Signs& Symptoms – Skin rash appears on body trunk then spreads to face, neck and limbs • Rash is diagnostic • Itchy rash progresses from red spots to pus filled blisters that break and crust over – Viral incubation period approximately 2 weeks • Infective 1 to 2 days before rash until all blisters crust

• Epidemiology – Disease transmitted by respiratory secretions and skin lesions – Virus typically enters through respiratory route, replicates and moves to the skin via blood stream – Infected cells swell and lyse • Release viruses which enter sensory nerves – Usually self limiting

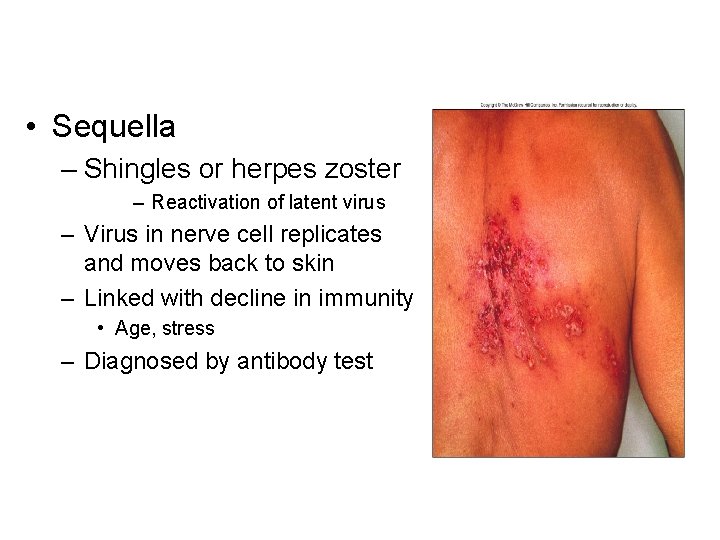
• Sequella – Shingles or herpes zoster – Reactivation of latent virus – Virus in nerve cell replicates and moves back to skin – Linked with decline in immunity • Age, stress – Diagnosed by antibody test

• Prevention and treatment – Prevention directed at vaccination • Attenuated vaccine licensed in 1995 • Recommended for healthy individuals 12 months and older – Treatment is directed at alleviating symptoms • Acyclovir given in high risk cases

– Reye’s Syndrome – Associated with a number of viral infections – Linked to aspirin usage in children – Characterized by vomiting and coma » Liver and brain damage – Mortality around 30%
![INSERT DISEASE AT A GLANCE 19 7 [INSERT DISEASE AT A GLANCE 19. 7]](https://slidetodoc.com/presentation_image/3fb7617a248b4d7883115c2e16d6d52d/image-7.jpg)
[INSERT DISEASE AT A GLANCE 19. 7]

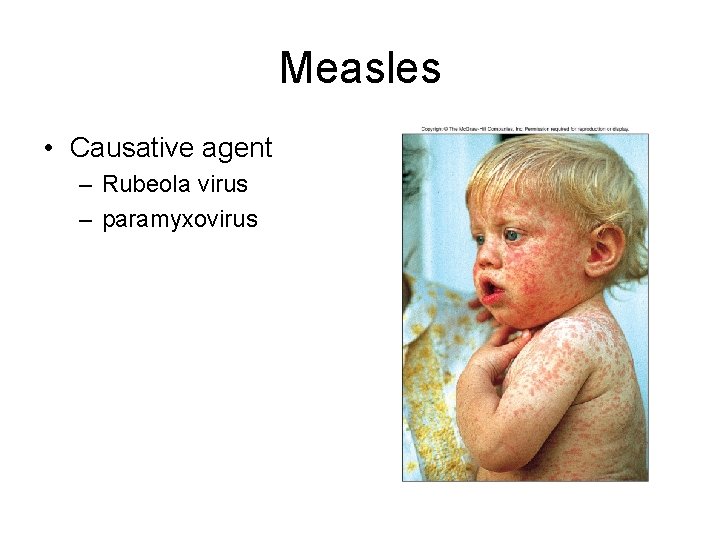
Measles • Causative agent – Rubeola virus – paramyxovirus

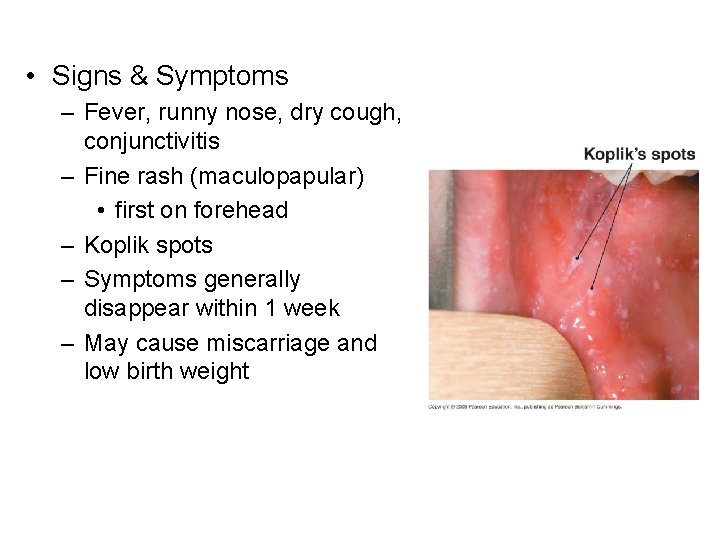
• Signs & Symptoms – Fever, runny nose, dry cough, conjunctivitis – Fine rash (maculopapular) • first on forehead – Koplik spots – Symptoms generally disappear within 1 week – May cause miscarriage and low birth weight

• Epidemiology – Humans are only natural host – Virus spread by respiratory droplets – Replicates in epithelium of upper respiratory tract • 8 -10 day incubation – Spreads to lymph becoming systemic – Typically self-limiting

– Many cases complicated by secondary infections • Pneumonia and earaches – Rare complications • encephalitis and subacute sclerosing panencephalitis (SSPE) • persistent viral infection

• Prevention and treatment – Prevention directed to vaccination • Vaccine is usually given in conjunction with mumps and rubella vaccine – MMR • Before routine immunization, over 99% of population infected • Measles are no longer endemic in US – No antiviral drug exists for rubeola infection • May treat with passive immunotherapy

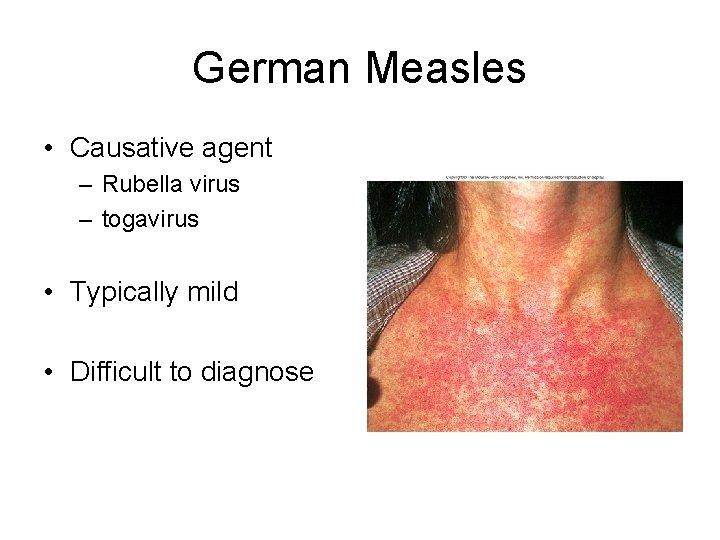
German Measles • Causative agent – Rubella virus – togavirus • Typically mild • Difficult to diagnose

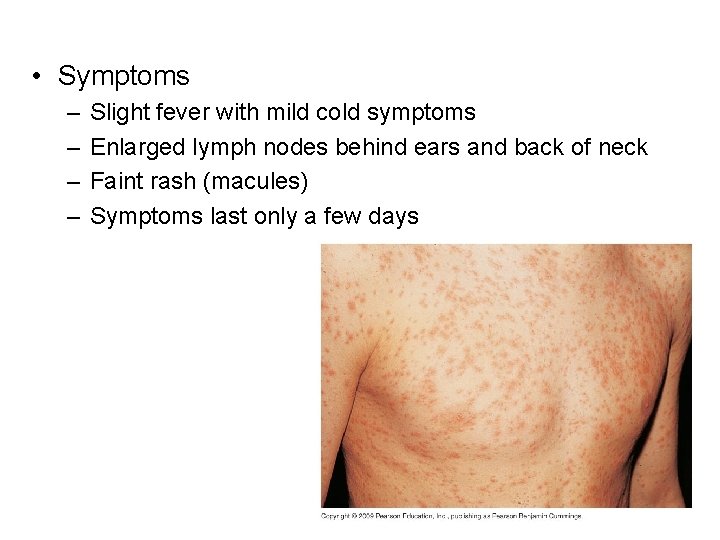
• Symptoms – – Slight fever with mild cold symptoms Enlarged lymph nodes behind ears and back of neck Faint rash (macules) Symptoms last only a few days

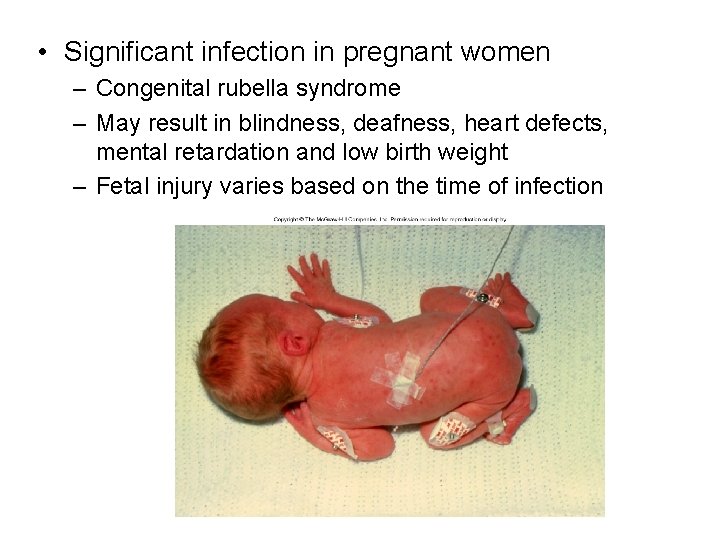
• Significant infection in pregnant women – Congenital rubella syndrome – May result in blindness, deafness, heart defects, mental retardation and low birth weight – Fetal injury varies based on the time of infection

• Epidemiology – Humans are only natural host – Virus spread by respiratory droplets – Multiplies in nasopharynx then enters blood – Disease is highly contagious • Infectious 7 days before appearance of rash and up to 7 days after it disappears

• Prevention and treatment – Vaccination with attenuated rubella virus vaccine • Administered at 12 months and boostered at 4 to 6 years of age • Produces long-lasting immunity
![INSERT TABLE 19 4 [INSERT TABLE 19. 4]](https://slidetodoc.com/presentation_image/3fb7617a248b4d7883115c2e16d6d52d/image-18.jpg)
[INSERT TABLE 19. 4]

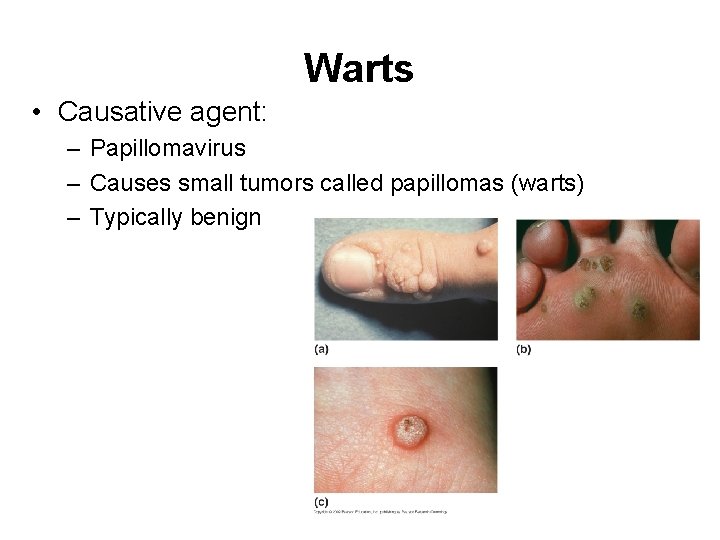
Warts • Causative agent: – Papillomavirus – Causes small tumors called papillomas (warts) – Typically benign

• 50 different papillomaviruses known to infect humans – infect skin through minor abrasions – Direct, indirect or auto- inoculation – Viruses can survive on a number of fomites • Towels • Shower floors

• Treatment involves killing abnormal cells – Freezing – Cauterization – Corrosive chemicals – Surgical removal – Laser

Mycoses of the Integument • Most fungi are opportunistic pathogens • Mycoses classified by location – Superficial – hair, nails, and outer skin layers • most common – Cutaneous – in the skin – Subcutaneous – in the hypodermis and muscles – Systemic – affect numerous systems

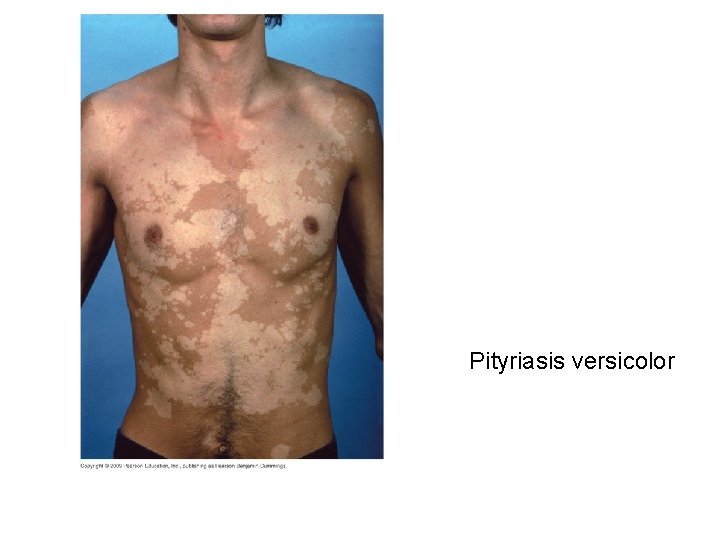
• Superficial Mycoses – Pityriasis versicolor • Caused by Malassezia furfur • Endogenous

Pityriasis versicolor

– Pathogenesis • Superficial fungi produce keratinase, which dissolves keratin – Diagnosis, treatment, and prevention • Identified by green color under ultraviolet light and treated with topical or oral drugs – Tolnaftate; Griseofulvin; Azoles

• Cutaneous Mycoses – May manifest as cutaneous lesions – Dermatophytoses • Immune responses damage deeper tissues

• Causative Agent – Genera responsible for most dermatophytoses • Epidermophyton • Microsporum • Trichophyton – Collectively termed dermatophytes

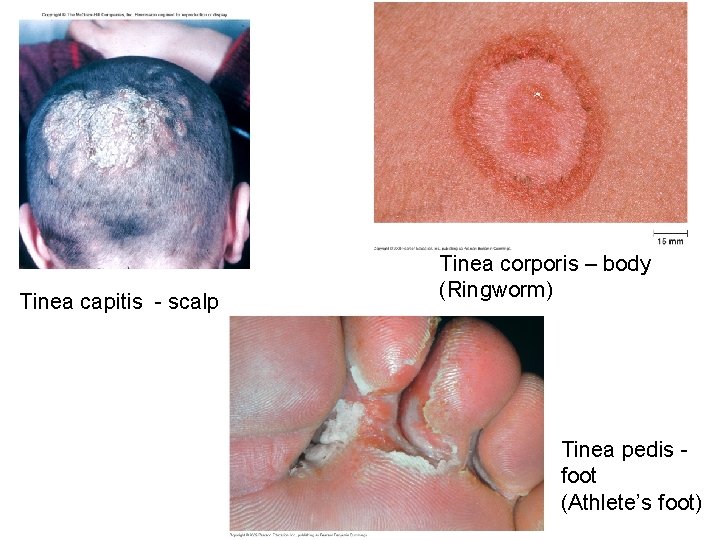
Tinea capitis - scalp Tinea corporis – body (Ringworm) Tinea pedis foot (Athlete’s foot)
![INSERT TABLE 19 5 [INSERT TABLE 19. 5]](https://slidetodoc.com/presentation_image/3fb7617a248b4d7883115c2e16d6d52d/image-29.jpg)
[INSERT TABLE 19. 5]

– Excessive moisture allows invasion of keratinized tissue • Most dermatophytes produce keratinase – Scalp is invaded through hair follicle – Fungal products defuse to dermal layer and evoke an immune response

• Treatment, and prevention – Attention to cleanliness – Maintenance of dryness – Treat limited infections with topical agents • Tolnaftate – Treat widespread infections with oral drugs • Griseofulvin; terbinafine