Chest Tubes Samantha Soto BSN RNBC University of
Chest Tubes Samantha Soto BSN, RN-BC University of Central Florida MSN Candidate
Objectives After participating in this class the learner will be able to… § Describe the anatomy and physiology of the lung § Identify potential conditions requiring need for a chest tube § List equipment and supplies used to place, maintain, and remove chest tubes § Outline the process of insertion, maintenance, and removal of chest tubes
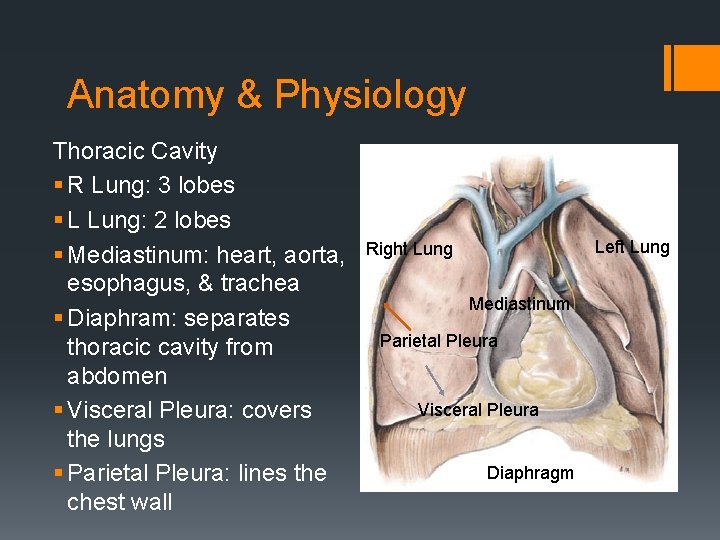
Anatomy & Physiology Thoracic Cavity § R Lung: 3 lobes § L Lung: 2 lobes § Mediastinum: heart, aorta, esophagus, & trachea § Diaphram: separates thoracic cavity from abdomen § Visceral Pleura: covers the lungs § Parietal Pleura: lines the chest wall Left Lung Right Lung Mediastinum Parietal Pleura Visceral Pleura Diaphragm
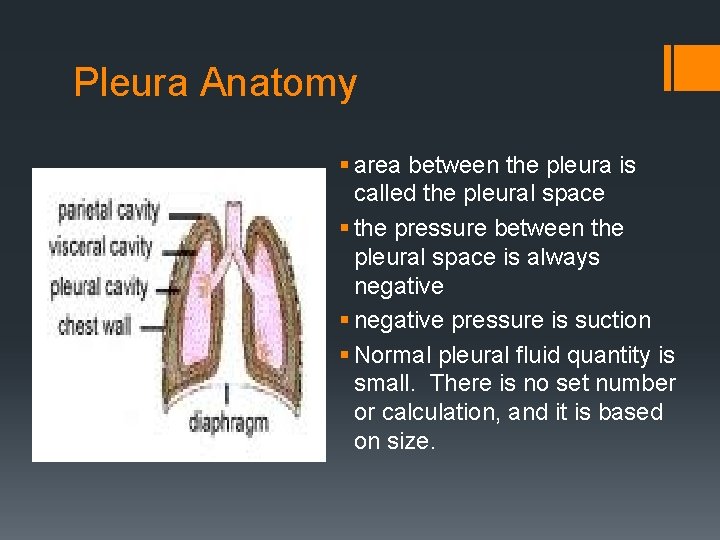
Pleura Anatomy § area between the pleura is called the pleural space § the pressure between the pleural space is always negative § negative pressure is suction § Normal pleural fluid quantity is small. There is no set number or calculation, and it is based on size.
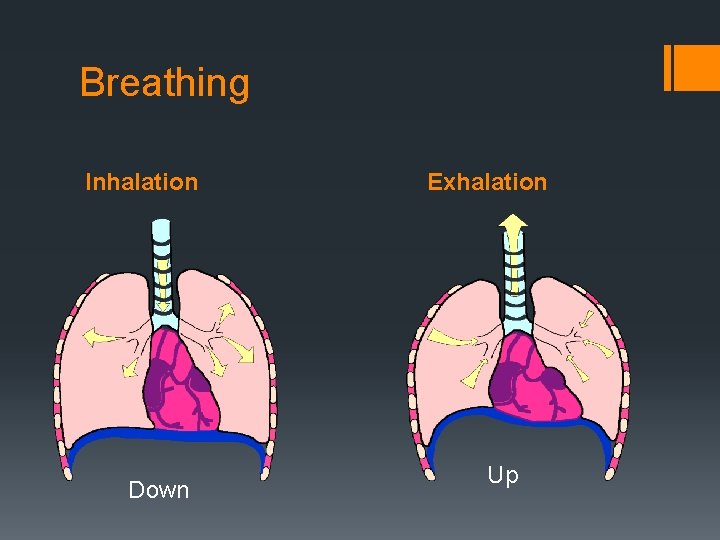
Breathing Inhalation Down Exhalation Up
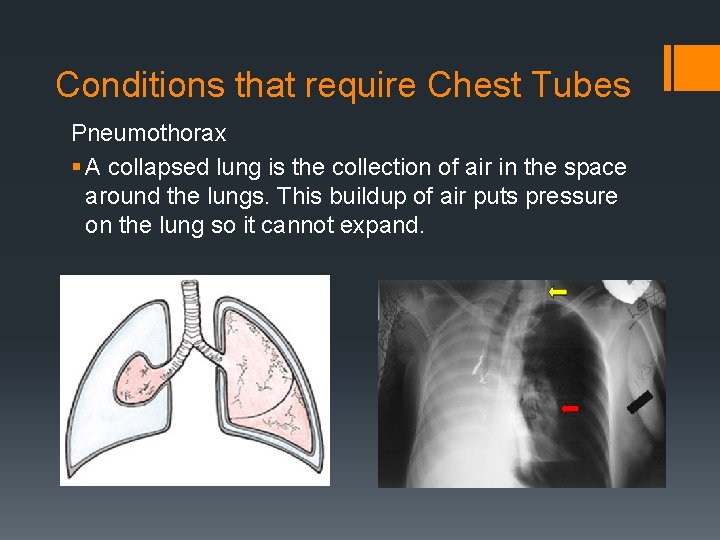
Conditions that require Chest Tubes Pneumothorax § A collapsed lung is the collection of air in the space around the lungs. This buildup of air puts pressure on the lung so it cannot expand.
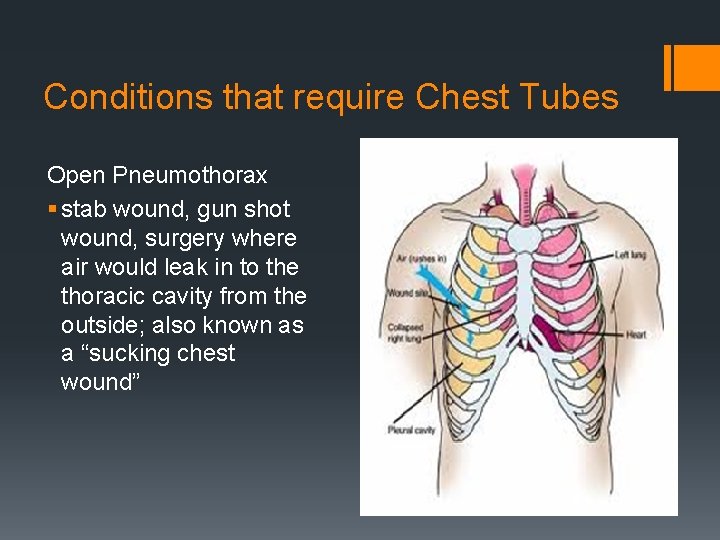
Conditions that require Chest Tubes Open Pneumothorax § stab wound, gun shot wound, surgery where air would leak in to the thoracic cavity from the outside; also known as a “sucking chest wound”
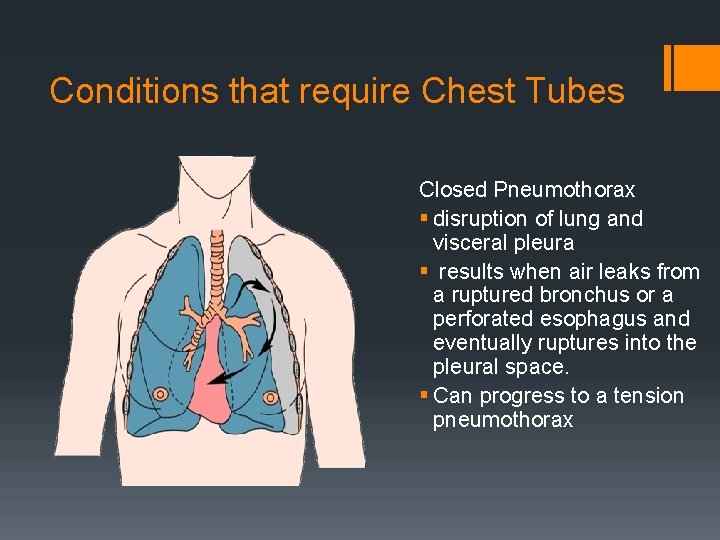
Conditions that require Chest Tubes Closed Pneumothorax § disruption of lung and visceral pleura § results when air leaks from a ruptured bronchus or a perforated esophagus and eventually ruptures into the pleural space. § Can progress to a tension pneumothorax
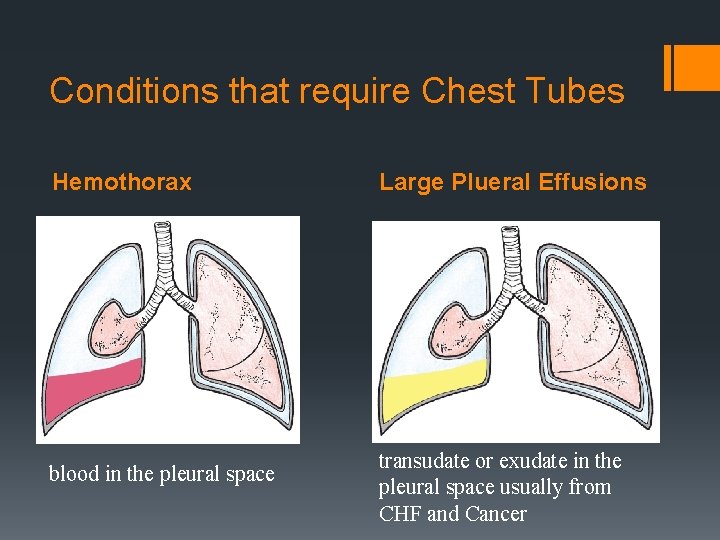
Conditions that require Chest Tubes Hemothorax blood in the pleural space Large Plueral Effusions transudate or exudate in the pleural space usually from CHF and Cancer
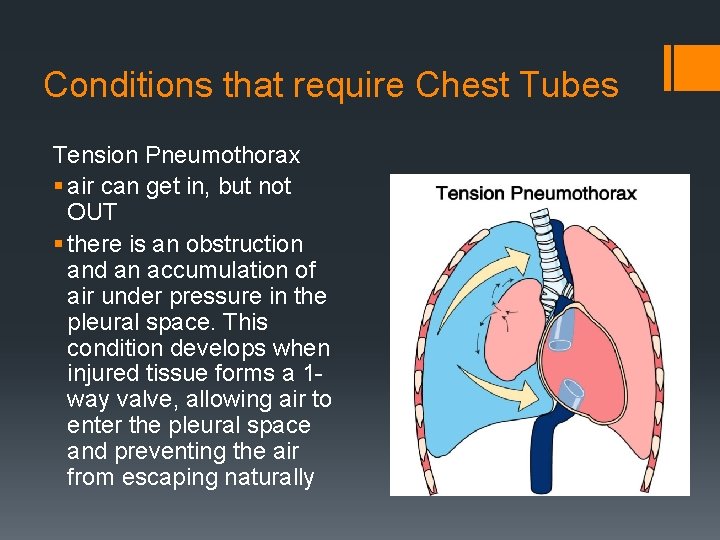
Conditions that require Chest Tubes Tension Pneumothorax § air can get in, but not OUT § there is an obstruction and an accumulation of air under pressure in the pleural space. This condition develops when injured tissue forms a 1 way valve, allowing air to enter the pleural space and preventing the air from escaping naturally
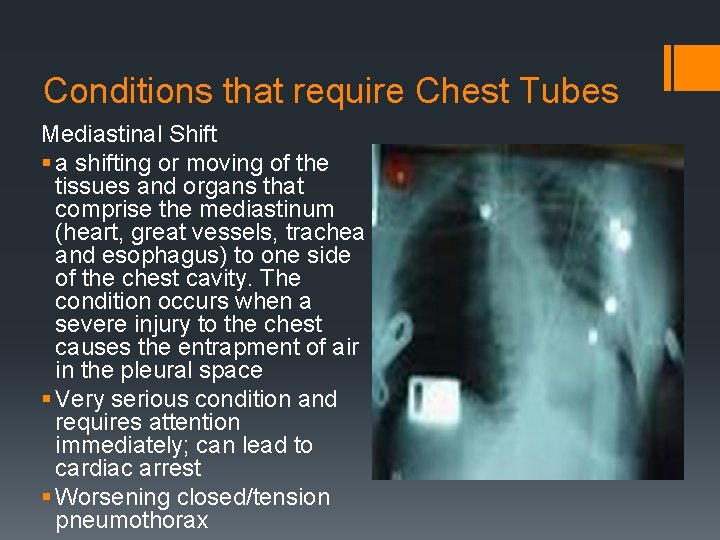
Conditions that require Chest Tubes Mediastinal Shift § a shifting or moving of the tissues and organs that comprise the mediastinum (heart, great vessels, trachea and esophagus) to one side of the chest cavity. The condition occurs when a severe injury to the chest causes the entrapment of air in the pleural space § Very serious condition and requires attention immediately; can lead to cardiac arrest § Worsening closed/tension pneumothorax

Conditions that require Chest Tubes Thoracic surgery § Coronary Artery Bypass Graft (CABG) and Valve replacements § Chest tubes are used to drain the chest cavity of fluid and blood (which is temporary and normal) after surgery. § Occasional placement of tubes in the left or right pleurae are used for collapsed lung during and post procedure

Signs & Symptoms § Dyspnea § Tachycardia § Chest pain § Crepitus § Decreased breath sounds on the side where the pneumothorax is § Cough § Fatigue § Cyanosis
Diagnostic Tools § Pulse oximetry § Ausculatation § Chest x-ray § CT scan

Equipment for Chest Tube placement Chest tube cart § Clamps § Pleur Evac § Vaseline guaze § Trocar § Chloraprep § Chest tube § Suction set up § Suture with needles § Dry sterile 4 x 4 s § Some medications will be pulled from pyxis

Drainage Systems Heimlich Valve • used primarily to release air • Mobile Pleur Evac • used for both fluid and air drainage Pluer. X • used for effusions that rapidly reaccumulate
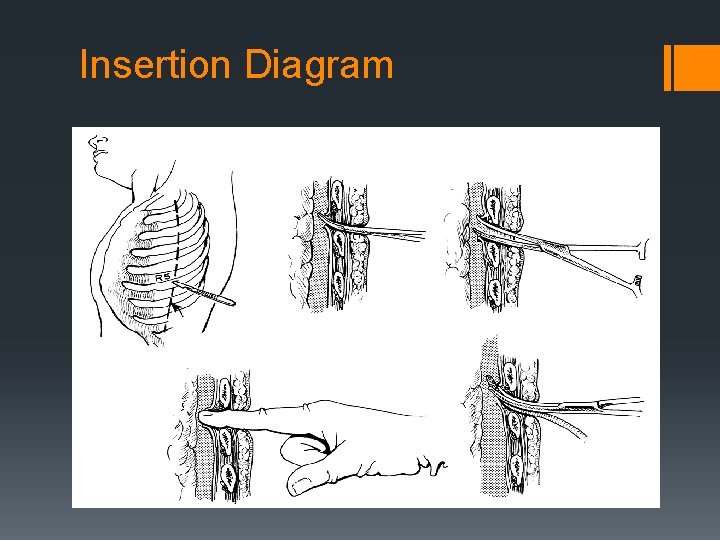
Insertion Diagram
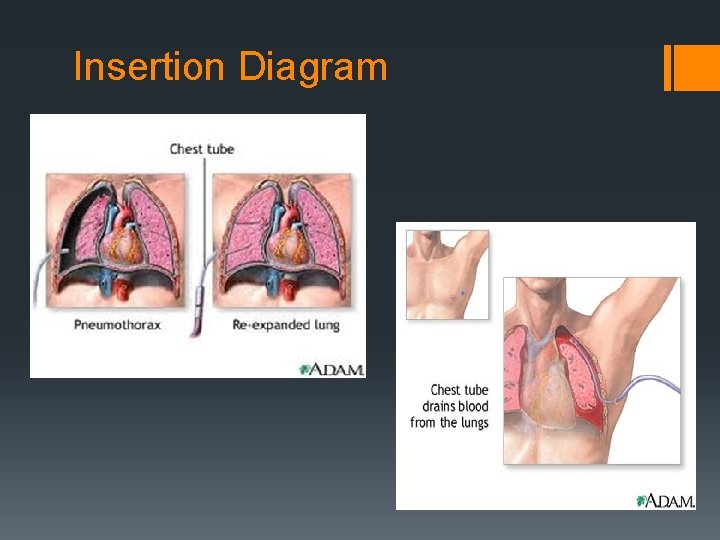
Insertion Diagram
Maintenance of the Chest Tube Vital Signs § with O 2 sats as per hospital policy § q 15 min x 4, q 30 min x 2, q 1 hr x 4, then q 4 hr until removed Site § tape securely § check for bleeding, crepitus around insertion site, § mark it with a marker, if its growing…that’s could be a problem § assess color at insertion and for swelling or bruising
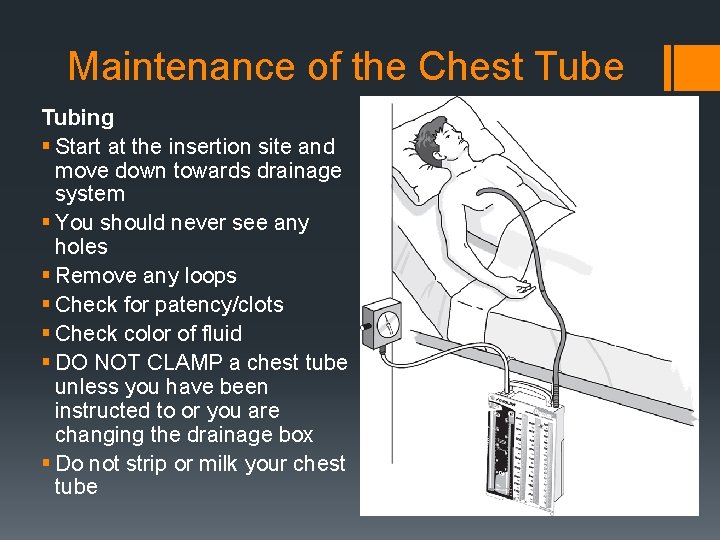
Maintenance of the Chest Tube Tubing § Start at the insertion site and move down towards drainage system § You should never see any holes § Remove any loops § Check for patency/clots § Check color of fluid § DO NOT CLAMP a chest tube unless you have been instructed to or you are changing the drainage box § Do not strip or milk your chest tube

Maintenance of the Chest Tube Pleur Evac/Drainage System § Do not touch sterile tip, you will hand this to the physician during insertion § Fill in the H 2 O chamber with sterile water § If air is leaking then you will see it in this chamber as shown. It is numbered 1 -5 to indicate the grade of the air leak. § you will almost always have an air leak when the tube is inserted, but is resolves § Hang drainage box at the foot of the bed
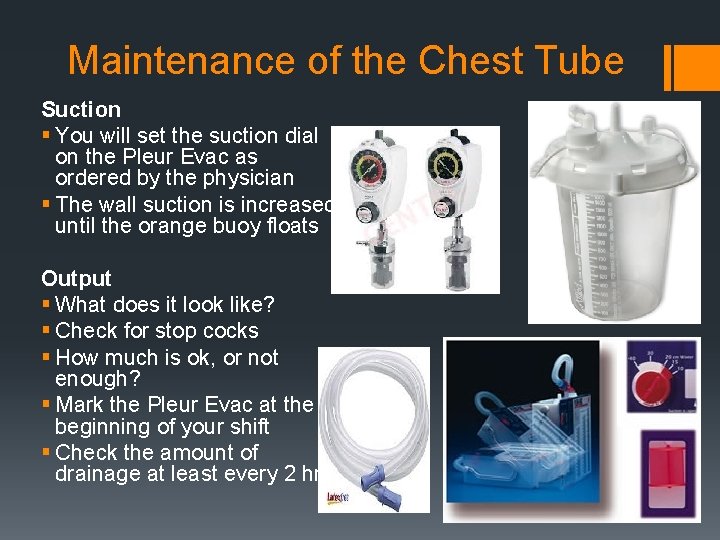
Maintenance of the Chest Tube Suction § You will set the suction dial on the Pleur Evac as ordered by the physician § The wall suction is increased until the orange buoy floats Output § What does it look like? § Check for stop cocks § How much is ok, or not enough? § Mark the Pleur Evac at the beginning of your shift § Check the amount of drainage at least every 2 hrs.

Maintenance of the Chest Tube What is water seal? § Water seal acts as a one way valve § Fluid and air can go out, but not back in. What if your water seal is low? § You can refill it with a syringe and a bottle of sterile water How often does the dressing need to be changed? § Daily unless it is saturated and needs to be changed sooner § Is this a sterile procedure? § No, but should be as clean a technique as possible

Patient Education § Description of procedure § IS and cough/deep breath § Ambulation/sitting up in chair(pts can do these things even with a chest tube!) § Pain management § The pt can expect to have chest x-rays performed daily until the tube is removed

When to call for HELP! § My patient’s having trouble breathing § My patient’s sats are below 90% and staying there § My patient’s chest tube is making whistling noises § My patient pulled out their chest tube
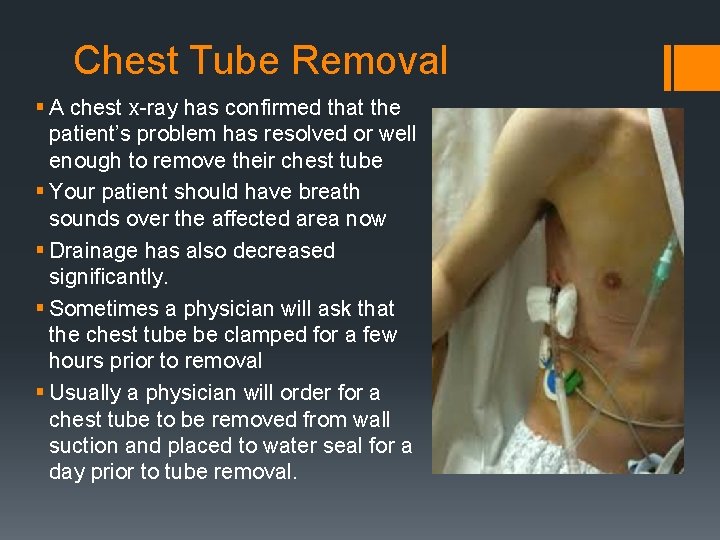
Chest Tube Removal § A chest x-ray has confirmed that the patient’s problem has resolved or well enough to remove their chest tube § Your patient should have breath sounds over the affected area now § Drainage has also decreased significantly. § Sometimes a physician will ask that the chest tube be clamped for a few hours prior to removal § Usually a physician will order for a chest tube to be removed from wall suction and placed to water seal for a day prior to tube removal.

Chest Tube Removal What will you need? § Kelly Clamps to clamp the chest tube § Chloraprep or betadine swab to clean the site before you remove the chest tube § Suture removal kit-to remove the sutures § Vaseline gauze or Adaptic-to help create a seal § Dry sterile 4 x 4, that will go over the Vaseline dressing § Tegaderm or Occlusive Dressing (at first you want a dressing that will help make a seal) § Red Bag for disposal of the chest tube and Pleur Evac

Chest Tube Removal Procedure § make sure you have an order first § Explain what your going to do to the patient. § The patient must be in bed, always § Pre-medicate: some physicians will pre-medicate for large bore chest tubes 15 -30 min prior to pull. § Practice breathing deep. Explain to the pt that on the third breath they will hold it until you say so, at that time you will pull the chest tube quickly § Get your red bag ready and place the Pleur Evac in the bag prior to pulling the chest tube § Clamp the chest tube with the Kelly Clamps

Chest Tube Removal Procedure continued… § Remove old dressing § Cleanse the area with chloraprep or betadine prior to pull and make sure it is dry. § Remove sutures § As you pull the chest tube you will place the Vaseline gauze and dry sterile 4 x 4 s. § Remind your patient to breath and that IT’S OVER! § Place Tegaderm over the gauze. Time and date the dressing. § Instruct your patient on when to call for help § Dispose of your waste in the red bin
- Slides: 29