Chest Development Congenital Diaphragmatic Hernia Cystic Adenomatoid Malformation




















- Slides: 36


Chest Development Congenital Diaphragmatic Hernia Cystic Adenomatoid Malformation Bronchopulmonary Sequestration

Chest Development Congenital Diaphragmatic Hernia Cystic Adenomatoid Malformation Bronchopulmonary Sequestration

Chest Development (1) V Heart most obvious finding in chest ¼ to 1/3 of thoracic cavity Apex direct to left Cardiac axis approximately 45% Normal axis excludes significant chest mass V Lungs Homogenous intermediate echo Echo G. A Right side > left side TC/AC > 0. 8


Chest Development (2) Clinical Importance Pulmonary hypoplasia:single most important factor determining survival for many conditions. Oligohydramnios:important etiology component of pulmonary hypoplasia. (oligo as short as 6 days may cause P. H. )

Chest Development Congenital Diaphragmatic Hernia (CDH) Cystic Adenomatoid Malformation Bronchopulmonary Sequestration

CDH The commonest contents of a left If the defect is right-sided the usual intrathoracic organs are: -sided hernia are: 80~90% 10% stomach liver bowel spleen gallbladder bilateral < 5%

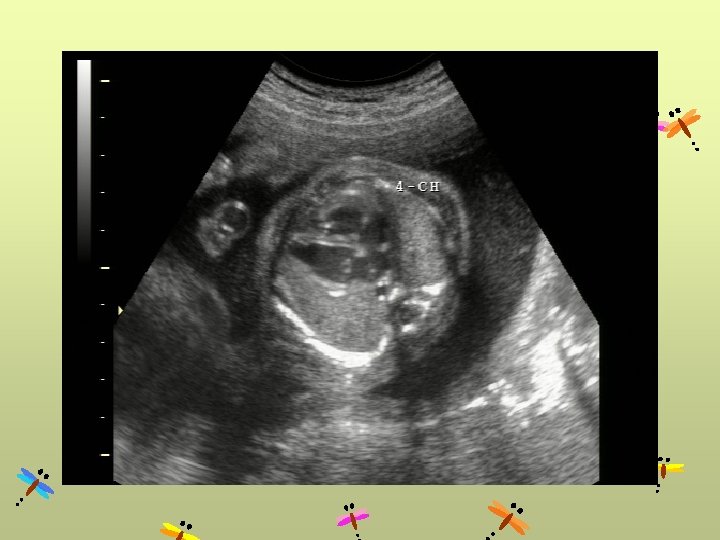
CDH Abnormal AC Most prenatal diagnosed CDH are large Hydrops uncommon (unless associated malformations) Small CDHs are easily missed (ex. stomach not herniated;note cardiac axis)

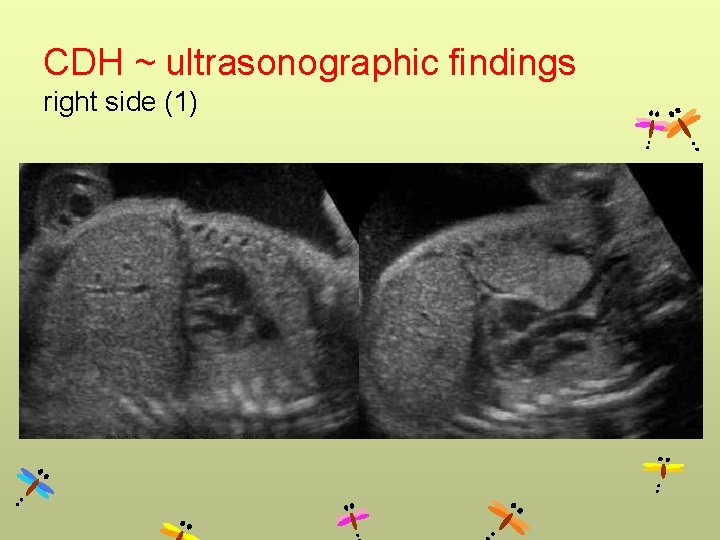
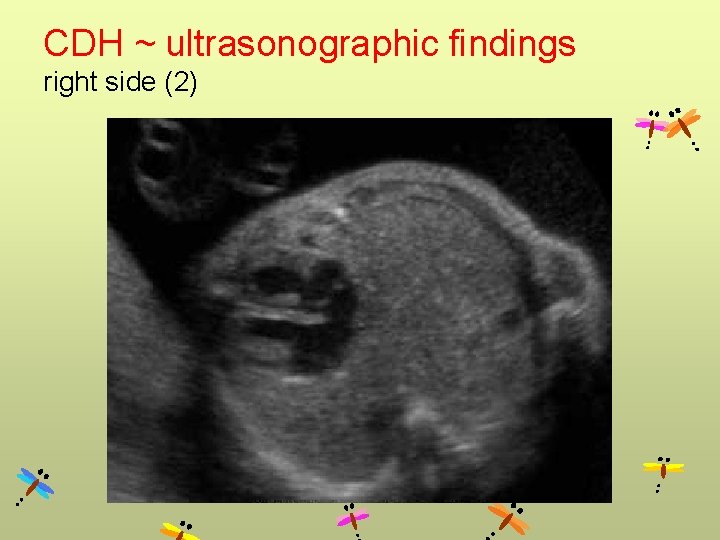
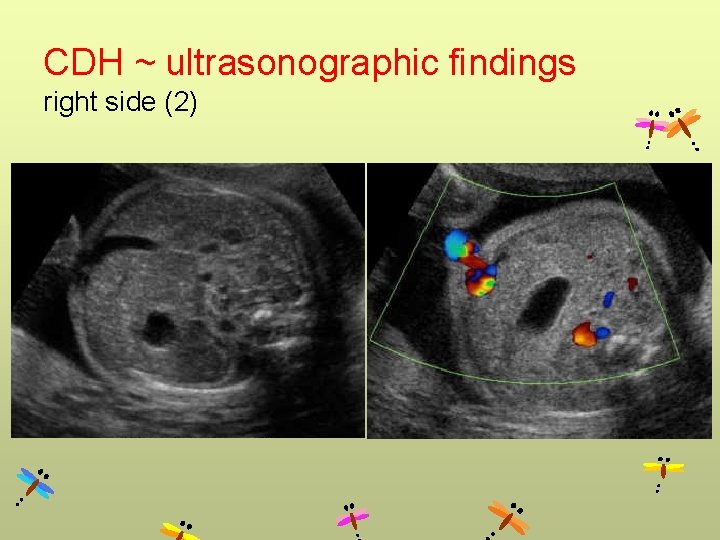
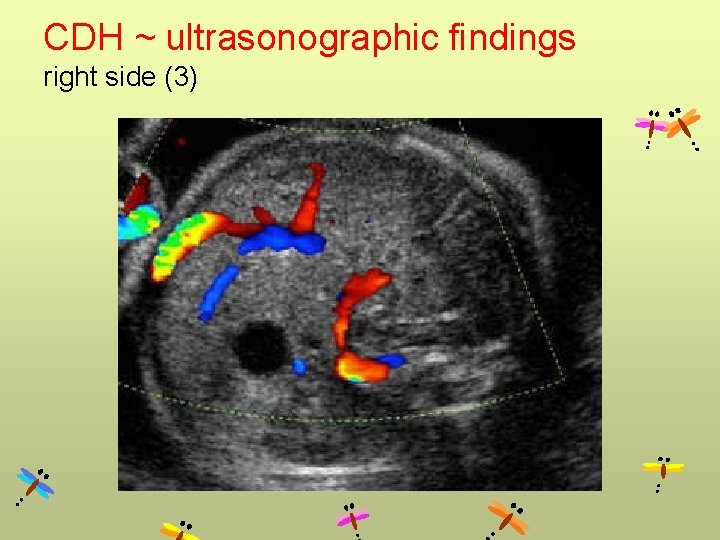
CDH Left side Right side • Cystic mass • Absence of fluid-filled stomach • Heart to right • Polyhydramnios • Up to 85% contain herniated liver (liver up) • Use Doppler to follow portal vein (to left) • More difficult • May be confused for chest mass • Contain liver & intestine (use Doppler showing portal vein) • Stomach below diaphragm • Gallbladder often herniated

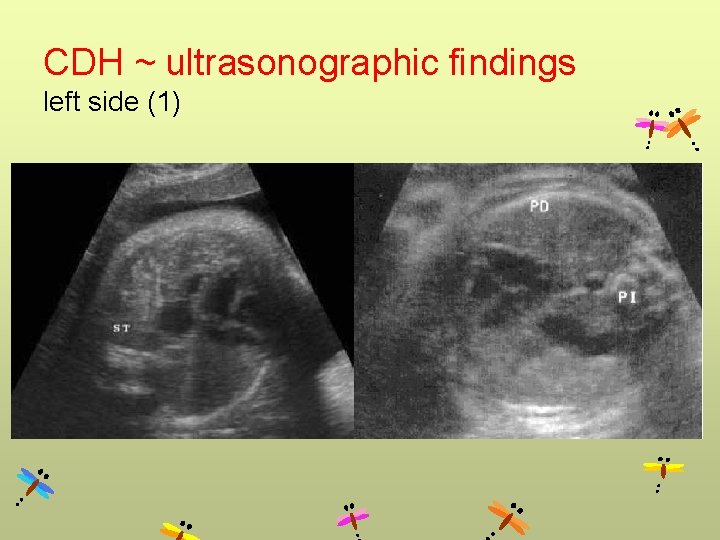
CDH ~ ultrasonographic findings left side (1)

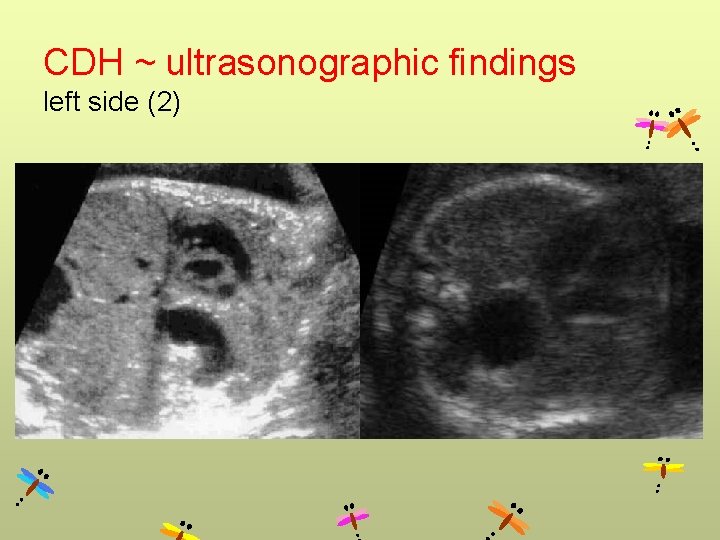
CDH ~ ultrasonographic findings left side (2)

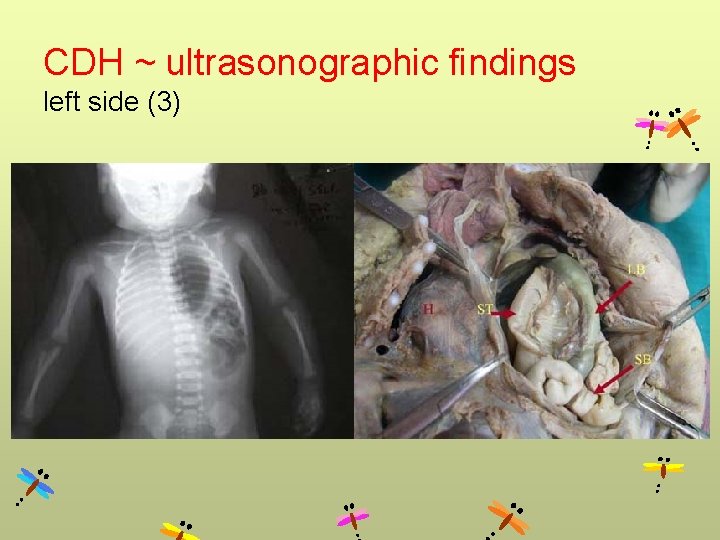
CDH ~ ultrasonographic findings left side (3)

CDH ~ ultrasonographic findings right side (1)

CDH ~ ultrasonographic findings right side (2)

CDH ~ ultrasonographic findings right side (2)

CDH ~ ultrasonographic findings right side (3)

CDH ~ Pathology • Pulmonary hypoplasia • Up to 50% associated an abnormality – 30% CNS malformation – 20% cardiac anomalies – Renal & spinal • Chromosomal abnormalities common – 16~37% – Trisomy 18,13,21,9 • Epidemiology: 1: 2000~5000 births • Embryology:failure of fusion of posterior pleuroperitoneal membranes

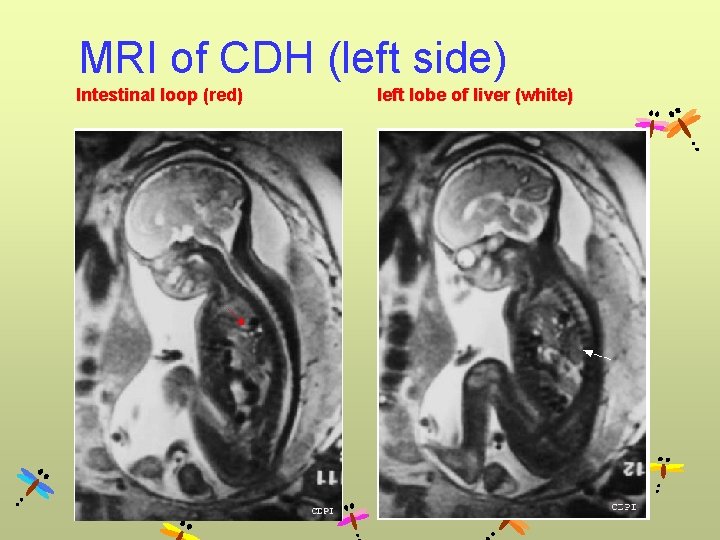
MRI of CDH (left side) Intestinal loop (red) left lobe of liver (white)

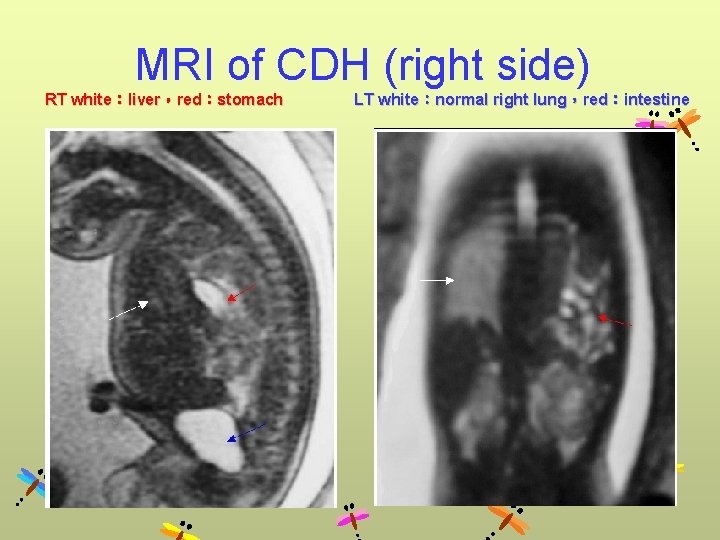
MRI of CDH (right side) RT white:liver,red:stomach LT white:normal right lung,red:intestine

CDH ~ Clinical Issues • 65% survival if isolated • Factors which worsen prognosis – – – • Other abnormalities Liver in chest (liver up: 57% mortality;liver down: 7%) Diagnosed before 24 wks GA Large size Right or bilateral Polyhydramnios Treatment – – – In utero repair:not useful Tracheal occlusion Postpartum surgery

Chest Development Congenital Diaphragmatic Hernia (CDH) Cystic Adenomatoid Malformation Bronchopulmonary Sequestration

CCAM Lung hamartoma with proliferation of terminal bronchioles and lack of normal alveoli. The other classification is based on the size of the cysts a. Microcystic (cysts less than 5 mm in diameter) b. macrocystic (cysts equal to or greater than 5 mm in diameter) c. mixed

CCAM Type of development Gestational age Description Pseudoglandular 5 -17 weeks Bronchiolar division; differentiation into air conducting system Type III Canalicular 16 -25 weeks Beginning terminal sacs development (primitive alveoli); vascularization of lung Type II Terminal sac 24 weeks – birth Proliferation of terminal sacs; marked thinning of the epithelium; bulging of capillaries into sacs CCAM development

CCAM ~ Ultrasonographic Findigs • Best diagnostic clue:solid or cystic lung mass with arterial supply from P. A. • Size:variable,usually contained with one lobe • 95% unilateral and one lobe • Right = Left • May spontaneously regress • Hydrops:most important prognostic factor (< 10%) • Color Doppler:vascular supply from P. A. (D/D with sequestration)

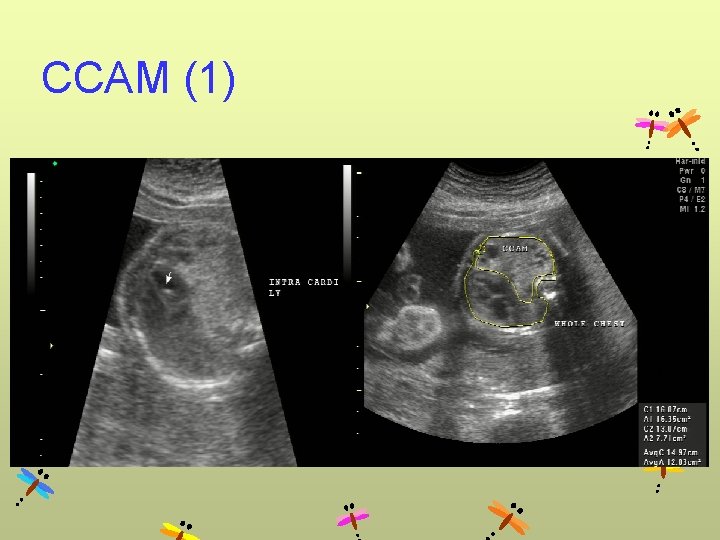
CCAM (1)

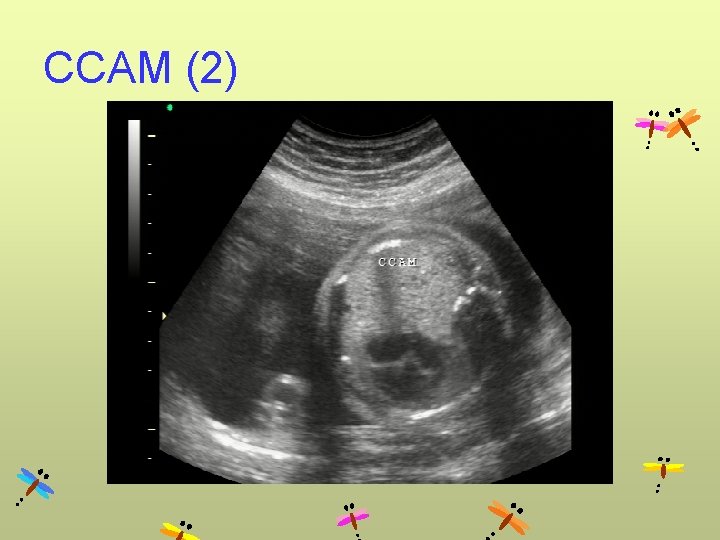
CCAM (2)

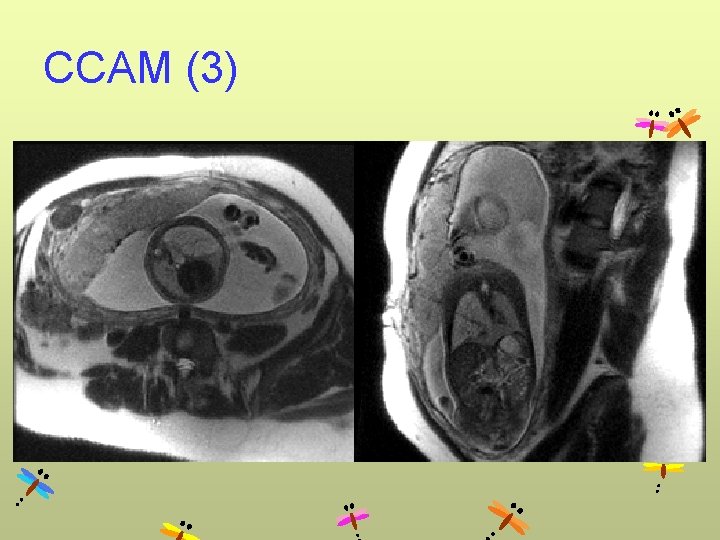
CCAM (3)

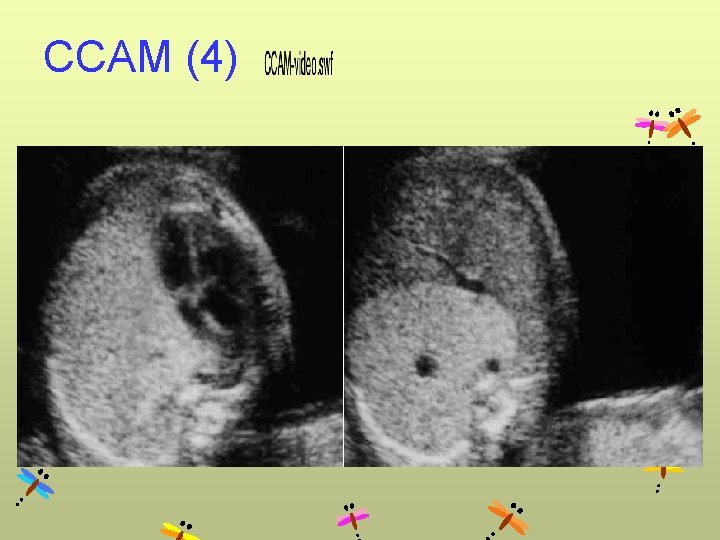
CCAM (4)

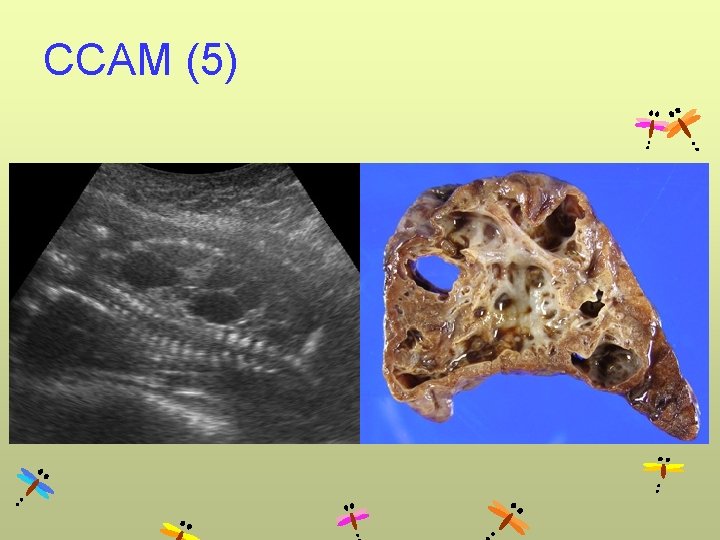
CCAM (5)

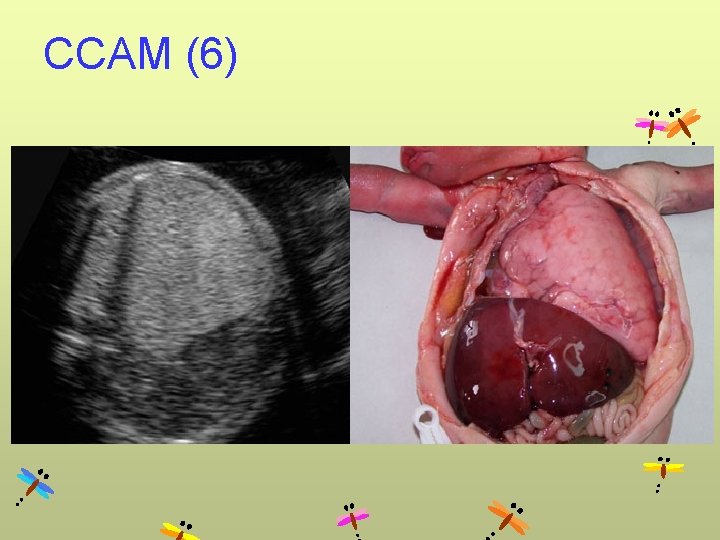
CCAM (6)

CCAM ~ Image Recommendation • Use Doppler to identify feeding vessels • Monitor closely:every 1~2 wks • Calculate CCAM volume and the ratio to lung

CCAM ~ Pathology • Genetics:sporadic inheritance,no recurrence risk • Most common fetal lung lesion (75%) • Associated anomalies: 3~12%

CCAM ~ Clinical Issues • Usually accidently diagnosed • Large for date or polyhydramnios • Prognosis – Majority remain stable or regress in utero – Near 100% mortality with hydrops – Dominant large cyst and CVR > 1. 6:indicate poor prognosis (CVR = CCAM vol. /HC) • Treatment – None unless hydrops

Chest Development Congenital Diaphragmatic Hernia (CDH) Cystic Adenomatoid Malformation Bronchopulmonary Sequestration (To Be Continued)

For God hath not given us the spirit of fear; but of power, and of love, and of a sound mind. 2 Timothy 1: 7 Thanks for Listening