Chemotherapy induced nausea and vomiting By Alan OKane

Chemotherapy induced nausea and vomiting By Alan O’Kane Specialist Pharmacist Oncology and Aseptic Ninewells Hospital

Chemotherapy-induced nausea and vomiting Most feared side effect May be more distressing than future concerns of life expectancy Medical complications: dehydration, electrolyte imbalance, risk of aspiration pneumonia Many treatments palliative intent = maintain QOL Effective management of N + V is essential
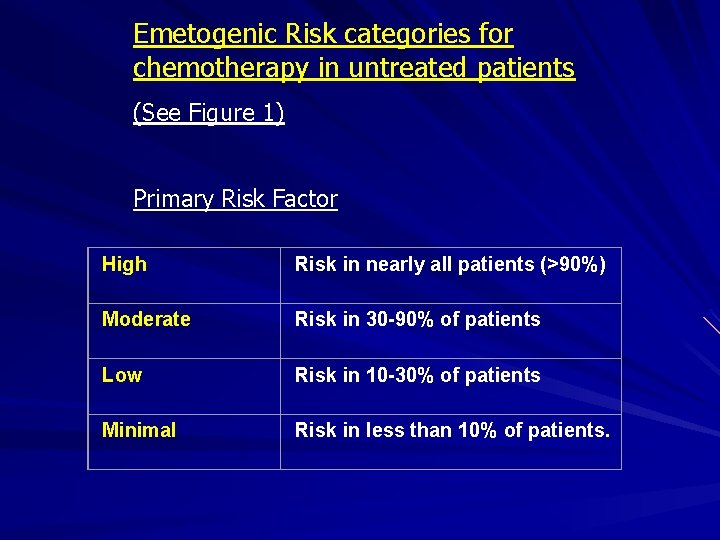
Emetogenic Risk categories for chemotherapy in untreated patients (See Figure 1) Primary Risk Factor High Risk in nearly all patients (>90%) Moderate Risk in 30 -90% of patients Low Risk in 10 -30% of patients Minimal Risk in less than 10% of patients.

Patient risk factors Age <50 years Female Alcohol intake Prone to N +V
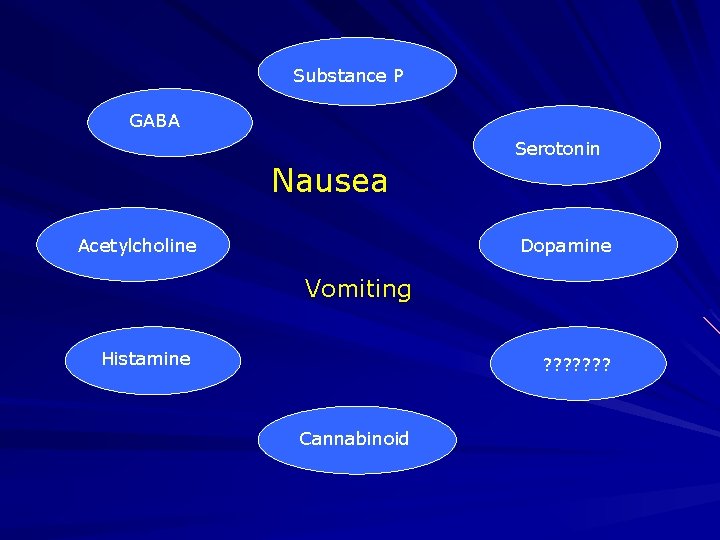
Substance P GABA Serotonin Nausea Acetylcholine Dopamine Vomiting Histamine ? ? ? ? Cannabinoid

Categories of CINV Acute within 24 hours of chemotherapy Delayed 24 hours to 7 days post chemo The most effective way of controlling CINV is to prevent symptoms of acute and delayed CINV by using a combination of an NK 1 antagonist, 5 HT 3 antagonist and dexamethasone.
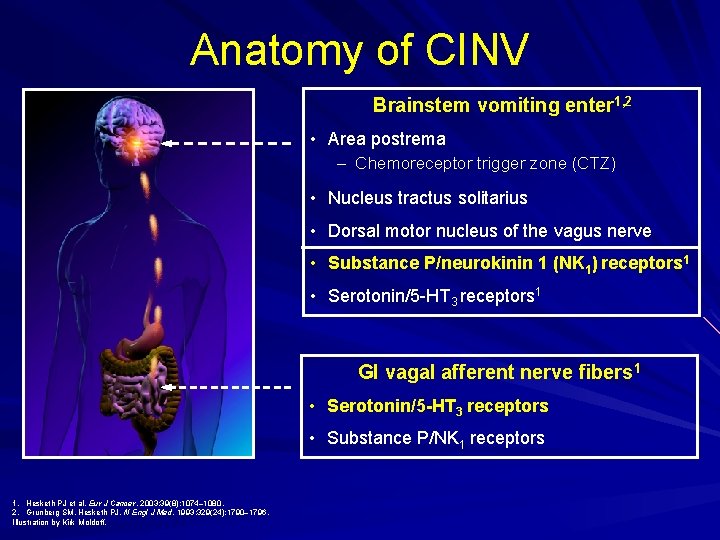
Anatomy of CINV Brainstem vomiting enter 1, 2 • Area postrema – Chemoreceptor trigger zone (CTZ) • Nucleus tractus solitarius • Dorsal motor nucleus of the vagus nerve • Substance P/neurokinin 1 (NK 1) receptors 1 • Serotonin/5 HT 3 receptors 1 GI vagal afferent nerve fibers 1 • Serotonin/5 -HT 3 receptors • Substance P/NK 1 receptors 1. Hesketh PJ et al. Eur J Cancer. 2003; 39(8): 1074– 1080. 2. Grunberg SM, Hesketh PJ. N Engl J Med. 1993; 329(24): 1790– 1796. Illustration by Kirk Moldoff.
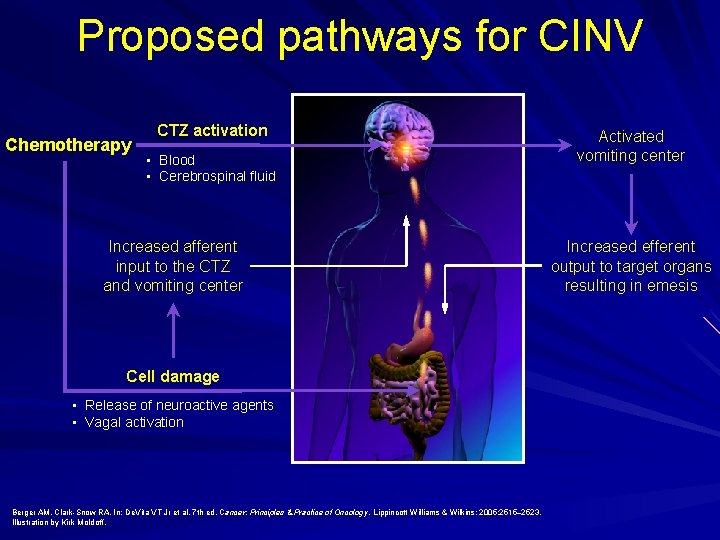
Proposed pathways for CINV Chemotherapy CTZ activation • Blood • Cerebrospinal fluid Increased afferent input to the CTZ and vomiting center Cell damage • Release of neuroactive agents • Vagal activation Berger AM, Clark Snow RA. In: De. Vita VT Jr et al. 7 th ed. Cancer: Principles & Practice of Oncology. Lippincott Williams & Wilkins; 2005: 2515– 2523. Illustration by Kirk Moldoff. Activated vomiting center Increased efferent output to target organs resulting in emesis

Serotonin and 5 HT 3 receptor pathway Introduction of 5 -HT 3 receptor antagonists offered an improved treatment option. 2 – Effective in acute vomiting; very limited efficacy for delayed events Primary mechanism of action appears to be peripheral. 2 1. Berger AM, Clark Snow RA. In: De. Vita VT Jr et al. 7 th ed. Cancer: Principles & Practice of Oncology. Lippincott Williams & Wilkins; 2005: 2515– 2523. 2. Hesketh PJ et al. Eur J Cancer. 2003; 39(8): 1074– 1080.

Substance P and NK 1 receptor pathway Substance P relays noxious sensory information to the brain High density of substance P/NK 1 receptors located in brain. NK 1 receptor blockade effective for delayed vomiting: Less effective for acute vomiting: needs a 5 HT 3 antagonist Less effective for nausea: needs dexamethasone

NK 1 antagonists Aprepitant 125 mg 1 hour before chemotherapy on Day 1, 80 mg Day 2 and Day 3 SMC approved for cisplatin containing regimens (other regimens? ? ) Some interactions: clinical significance

5 HT 3 Antagonists Block release of serotonin release from enterochromaffin cells in GI tract Most effective for acute vomiting All equally effective e. g ondansetron/granisetron (? palonesetron) Best given as a stat dose pre chemo Oral and IV equally effective Side effects: constipation, abdominal spasms, headaches
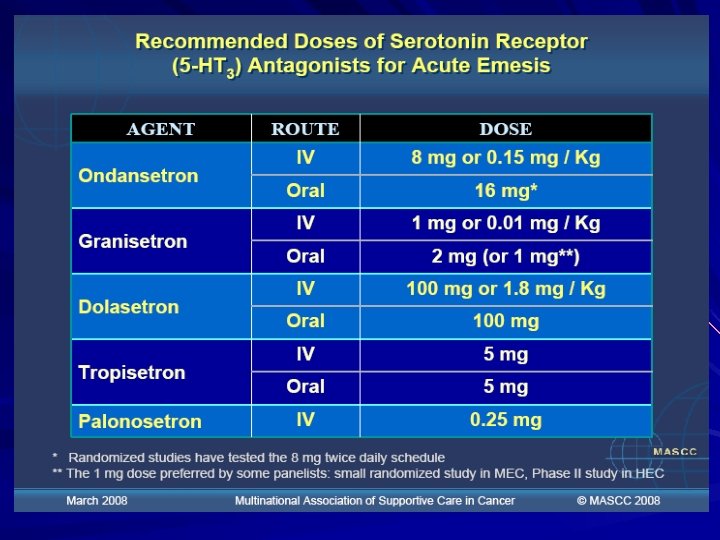
Multi Association of Supportive Cancer Care (MASCC) (See Handout)

Dexamethasone M. O. A not fully understood. Very effective for nausea, acute and delayed vomiting Acute: pre dose before chemo Delayed: 2 4 days after Side effects: heartburn/indigestion, agitation, hiccups, abnormal BM’s (all manageable in most instances)
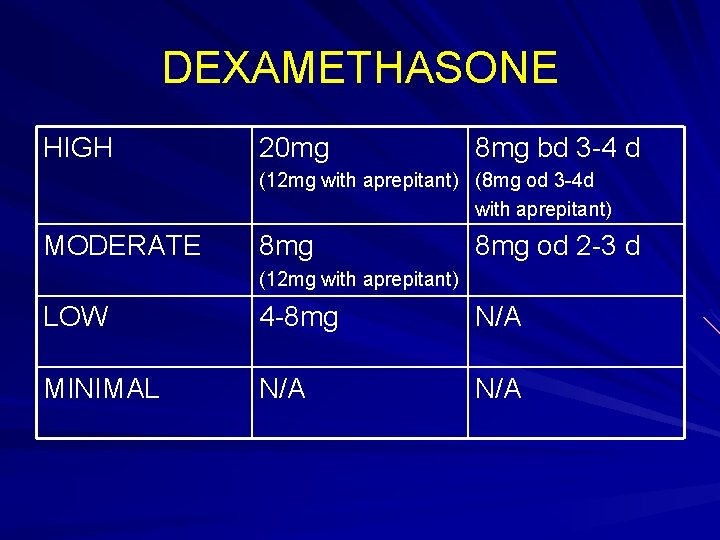
DEXAMETHASONE HIGH 20 mg 8 mg bd 3 4 d (12 mg with aprepitant) (8 mg od 3 4 d with aprepitant) MODERATE 8 mg od 2 3 d (12 mg with aprepitant) LOW 4 8 mg N/A MINIMAL N/A

Anticipatory N + V Conditional response Sights and smells Involves higher cortical centres of brain Occurs in 30% of patients Lorazepam is an effective treatment

Other situations… Breakthrough symptoms N + V in spite of optimal preventative treatment. Rescue therapy Treatment of breakthrough symptoms Refractory CINV recurs in subsequent cycles of therapy when all previous preventative and rescue treatments have failed.

Breakthrough symptoms- which anti-emetic? Less well conducted trials available to guide treatment decisions. Diagnosis of the cause of nausea and vomiting is crucial for deciding on which anti emetic to use. Key questions when did symptoms start? when was last dose of chemo/XRT? When did steroid course stop? Nausea related to smells/taste of food? How many vomiting episodes? VAS to assess nausea? Appetite/food and fluid intake? The only evidence available to rescue patients who have CINV is with the use of a D 2 antagonist e. g. metoclopramide or a 5 HT 3 antagonist such as ondansetron. Consider the side effect profile of each anti emetic. There may be more than one cause of nausea and vomiting therefore do not prescribe an anti emetic that may worsen symptoms e. g. ondansetron and cyclizine may constipate avoid if constipation and nausea present use metoclopramide instead. Severe cases consider syringe driver for 48 hours then review. Domperidone is supplied at a dose of 20 mg qds with the majority of chemotherapy regimens. Consider if you want to add or substitute. If patient feels ineffective consider compliance in view of low confidence in medicine.
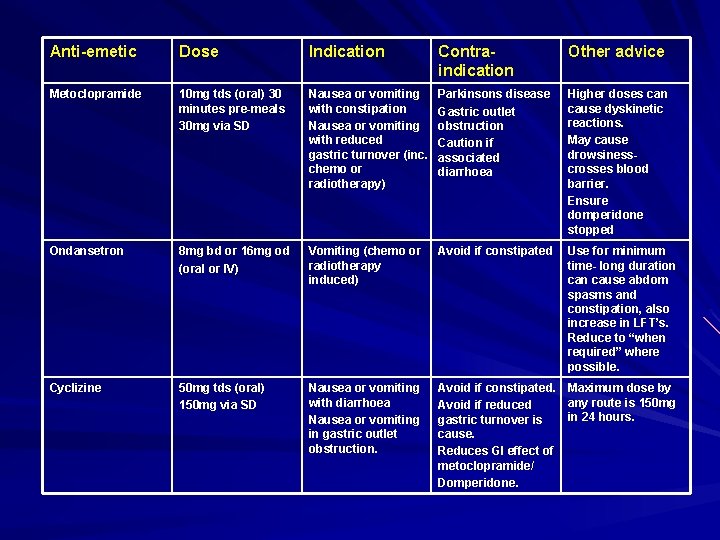
Anti-emetic Dose Indication Contraindication Other advice Metoclopramide 10 mg tds (oral) 30 minutes pre-meals 30 mg via SD Nausea or vomiting with constipation Nausea or vomiting with reduced gastric turnover (inc. chemo or radiotherapy) Parkinsons disease Gastric outlet obstruction Caution if associated diarrhoea Higher doses can cause dyskinetic reactions. May cause drowsiness- crosses blood barrier. Ensure domperidone stopped Ondansetron 8 mg bd or 16 mg od od 8 mg bd or 16 mg (oral or IV) Vomiting (chemo or radiotherapy induced) Avoid if constipated Use for minimum time- long duration cause abdom can cause abdom spasms and constipation, also increase in LFT’s. Reduce to “when required” where possible. Cyclizine 50 mg tds (oral) 150 mg via SD Nausea or vomiting with diarrhoea Nausea or vomiting in gastric outlet obstruction. Avoid if constipated. Maximum dose by any route is 150 mg Avoid if reduced in 24 hours. gastric turnover is cause. Reduces GI effect of metoclopramide/ Domperidone.
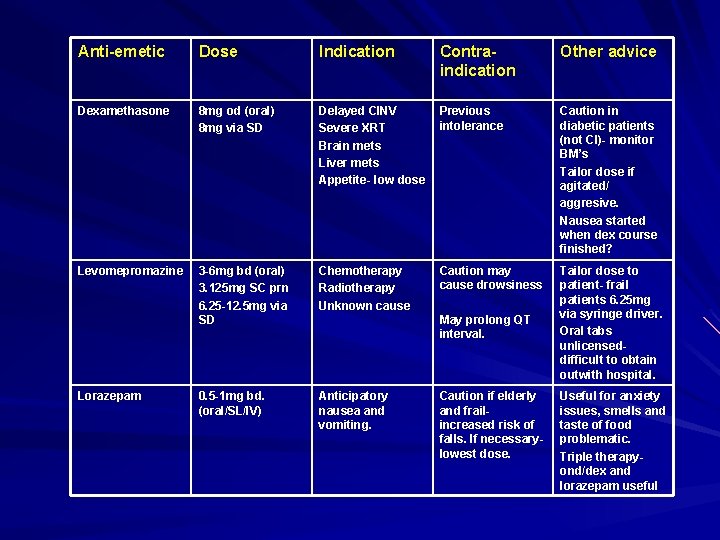
Anti-emetic Dose Indication Contraindication Other advice Dexamethasone 8 mg od (oral) 8 mg via SD Delayed CINV Severe XRT Brain mets Liver mets Appetite- low dose Previous intolerance Caution in diabetic patients (not CI)- monitor BM’s Tailor dose if agitated/ aggresive. Nausea started when dex course finished? Levomepromazine 3 -6 mg bd (oral) 3. 125 mg SC prn 6. 25 -12. 5 mg via SD Chemotherapy Radiotherapy Unknown cause Caution may cause drowsiness Tailor dose to patient- frail patients 6. 25 mg via syringe driver. Oral tabs unlicensed- difficult to obtain outwith hospital. 0. 5 -1 mg bd. (oral/SL/IV) Anticipatory nausea and vomiting. Lorazepam May prolong QT interval. Caution if elderly and frail- increased risk of falls. If necessary- lowest dose. Useful for anxiety issues, smells and taste of food problematic. Triple therapy- ond/dex and lorazepam useful

Effective control Give appropriate antiemetic medicines before chemo and after at correct dose, route, frequency, duration and timing Start “prophylaxis” Cycle 1 and then throughout “Breakthrough symptoms” diagnosis cause and chose anti emetic wisely (consider anti emetic choice, dose, frequency, duration and side effect profile). Counsel patient on diet when feeling sick or vomiting importance of small amounts of food frequently (5 6 meals instead of 3), plenty fluid, eat easy to swallow foods with minimal smell e. g. clear broth, white toast, yoghurt, custard, crackers.

Any Questions?
- Slides: 22