Chapter Six Opportunistic Mycoses Acknowledgments Addis Ababa University

Chapter Six: Opportunistic Mycoses

Acknowledgments • Addis Ababa University • Jimma University • Hawassa University • Haramaya University • University of Gondar • American Society for Clinical Pathology • Center of Disease control and Prevention in Ethiopia. 2

Outline of presentation • Objective • Candidiasis • Asperigilosis • Zygomycosis • Cryptococosis • Pneumocystis jerovecii • Summary

Objective § Upon completion of this chapter, students will be able to: • Describe different cause of opportunistic Mycose • Explain the clinical manifestation of different opportunistic mycoses. • Describe the different laboratory tests used to diagnose each opportunistic mycosis

Introduction • The opportunistic mycoses • caused by fungi that can’t infect healthy humans but can cause serious • often fetal mycoses in people whose resistance has been lowered (immunocompromised patients). • The highly susceptible groups for opportunistic fungal infection are • AIDs patients, • Leukemic patients, • individuals on chemotherapy for treatment of cancer, • alcoholics.

Introduction cont’d… • Many diabetic peoples are also susceptible to pulmonary infection by common saprophytic mold of genera Rhizoples and mucor (both Zygomycetes) and Aspergillus. • Unless the predisposing conditions are corrected, many opportunistic mycosis can be fetal, even with antibiotic treatment.

Introduction cont’d • Many fungi previously considered non- pathogenic are now recognized as etiological agents of the opportunistic fungal infections. • The laboratory must identify and report completely the presence of all fungi recovered from immunocompromised patient, since every organism is a potential pathogen.

Introduction cont’d… • Although there is an ongoing list of opportunistic mycosis, some are seen more often and includes : » Candidousis (candidiasis), » Cryptococcosis, » Aspargillosis, » Zygomycosis » Trichosporonsis

6. 1. Candidiasis • Candidiasis is a relatively common human infection that can take form of superficial, mucocutanous or systemic disease. • Principally it is caused by the three species of genus candida, namely, C. krusei, C. tropicalis and C. albicans. • Candida albicans is the most common cause of infection. Since the species of candida, including C. albicans are the part of the normal endogenous microbial flora, candidiasis is usually the result of autoinfection during a metabolic or an immunologic disturbance. • The organisms may be recovered from the genitourinary tracts, and skin. oropharynx , GI,

Pathogenesis and clinical pictures A. Superficial and mucocutaneous candidiasis • It is superficial infections of skin and mucous membranes • Through, oral and vaginals candidiasis • Oesophagial candidiasis • Skin lesions of folds, growin, axilla, and interdigital • Napkin cruptions in infants • Paranychial candidiaiasis

Pathogenesis cont’d… B. Systemic (disseminated or invasive) candidiaiasis • Pulmonary and kidney infection occur on top of a preexisting disease e. g. malignancy or tuberculosis • Invasive candidiasis of many organs occurs in immunosuppresed and leukaemic patients Tissue phase • C. albicans is not a dimorphic fungus, as both yeast & hyphae are seen in tissue • The hyphae are thought to represent the tissue-invasive form of the fungus.

Predisposing factors § Diabetes § Immunosupperession § T-cell immunodeficiency disorders § Acquired- immunodeficiency syndrome, (AIDS) § Leukaemias, Lymphomas § Steroid treatments § Broad spectrum antibiotics

Laboratory diagnosis • superficial or mucocutaneous candidiasis is diagnosed by finding the fungus in tissue scraping and culture • systemic candidiasis is difficult to diagnose. • Definitive diagnosis is made by the histopathologic demonstration of the invasion of tissue by the yeast. • Specimens from surface lesions, mouth, vaginal, sputum, exudates e. t. c are examined using different methods

Lab dx cont’d • Direct examination KOH • Exposed lesions can usually be easily diagnosed by clinical appearance together with finding typical budding yeast cells and pseudohyphae and /or true hyphea in lesion scrapings treated with KOH. Gram- stain • Gram stain smears shows large gram positive budding yeast cells with pseudohyphea.

Culture and identification • Growth is rapid on sabouroud’s dextrose blood agar, trypticase soy, and many other media. • Creamy yeast colonies are formed after overnight incubation at temperature of 210 C or 370 C; the optimum growth temperature is around 300 C. • C. albicans grows as round-to-oval yeast cells that are 46µm in diameter. • Psudohyphae and hyphae also seen; especially at lower incubation temperature nutritionally poor media. (i. e. 220 C-250 C) and on

Culture cont’d § Candida albicans is differentiated from other candida species by: §Budding of yeast cell. §Germ-tube test: - Rapid development of germ tubes when yeast cells incubated at 370 c in 1 -2 hrs in serum. § Chlamydospore formation when incubated at 220 c on cornmeal agar.
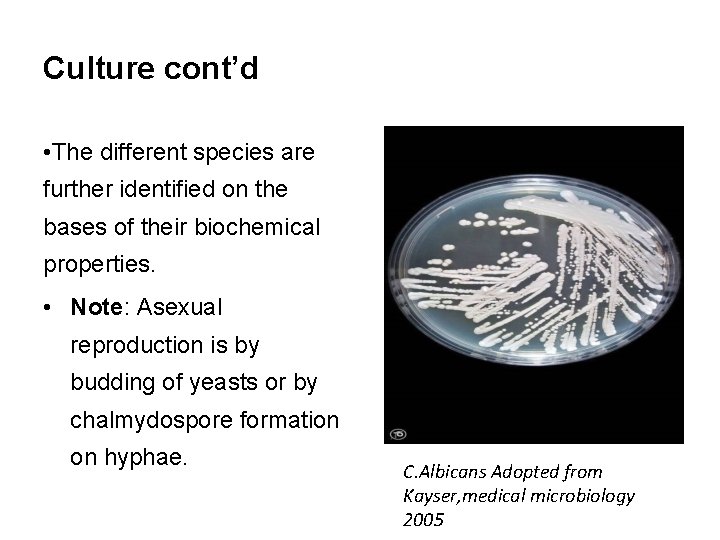
Culture cont’d • The different species are further identified on the bases of their biochemical properties. • Note: Asexual reproduction is by budding of yeasts or by chalmydospore formation on hyphae. C. Albicans Adopted from Kayser, medical microbiology 2005
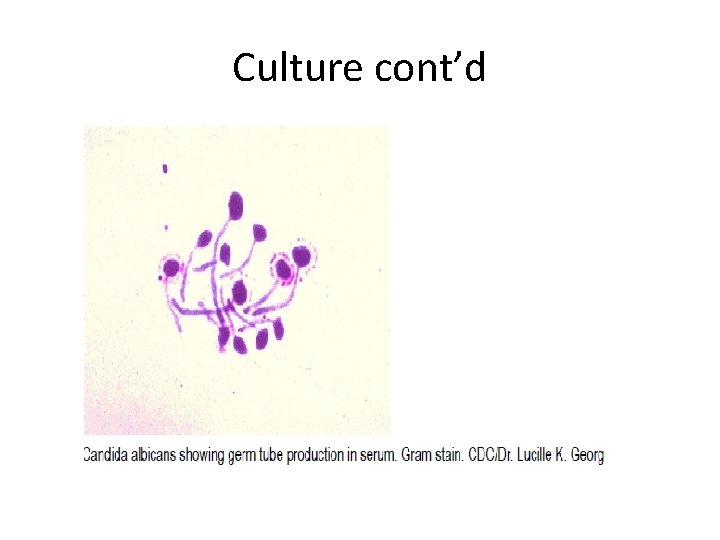
Culture cont’d

6. 2. Aspergillosis • Definition • Aspergillosis comprises a group of world wide human disease caused by about dozen fungal species of the genus Aspargillus. • Since Aspergillus species are many and are widespread in soil, air, and decaying vegetable matter many person are heavily exposed to inhalation of spores.

Pathogenesis and clinical picture • The spectrum of human disease caused by Asperagillus ranges from allergy to disseminated infection. • Most of the disease processes are caused by the inhalation of conidia. • Allergy: - Persons may develop Ig. E. against Aspergillus and present with allergic condition. Example, asthma • Non-invasive colonization: - Aspergillus can colonize a pre-existing lung cavity e. g. , tuberculosis, forming fungus ball or aspergilloma.

Pathogenesis cont’d • Invasive aspergillosis • may occur in severely immunocompromised patients, organ transplant recipients, . • Patients under corticosteroid therapy and patients with leukaemia. • Toxin production • e. g. aflatoxin of Aspergillus flavus is carcinogenic; cause liver cancer and necrosis.

Predisposing factors • Infections occur principally in individuals who have disease or predisposing abnormalities such as cystic fibrosis, bronchietasis, chronic bronchitis, tuberculosis etc. or who are immunosuppressed. • Aspergillus species are not dimorphic; they are characterized by chains of conidia borne or condiophore. • Speciation is based on principally morphology; some 150 species are recognized.

Predisposing factor cont’d… • Aspergillus fumigatus is most commonly recovered from immunocompromised patients, and most often seen in clinical laboratories. • Aspergillus niger and A. flavus are also recognized as significant cause of infection in immunocompromised patients.

Laboratory diagnosis § The diagnosis of aspergillosis is difficult due to their wide spread in nature. § Direct examination § Microscopic examination of KOH preparations of sputum show characteristic branching hyphae filaments and may show the conididophores attached to the spare head. § Demonstration of hyphal fragments in tissue biopsy is diagnostic of tissue invasion
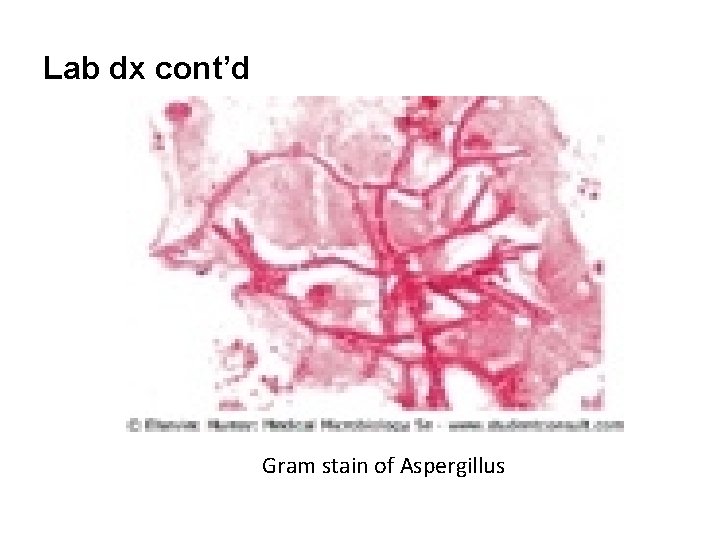
Lab dx cont’d Gram stain of Aspergillus

Lab dx cont’d Aspergillus in tissue showing acute angle branching, septate hyphae

Culture and identification • A. fumigatus is rapidly growing mold (2 to 5 days) that produce a fluty to granular, white to blue- green colony, on blood enriched medium. • Mature sporulating colonies most often exhibits the bluegreen powdery appearance. Serologic test • Antibodies to Aspergillus extracts are detected in serum and positive skin testing in allergic cases

6. 3. Zygomycosis (phycomycosis, mucormycosis) • Definition • Zygomycosis is caused by several genera belonging to zygomycetes, e. g. mucor, rhizopus, and Abiedia. • It is some what less common infection when compared with Aspergillosis; however it is a significant cause of morbidity and mortality in immunocompromised patients. • Like Aspergillus species, members of the zygomycetes are common environmental moulds of low intrinsic pathogencity.

Zygomycosis con’t • The disease occurs in debilitated persons, metabolic acidosis, malignancies, uraemia, malnutrition, steroid therapy and hepatic failure. • The organisms produce broad non septate hyphea, aerial mycelia, sporangiospores and sexual zygospores; grow rapidly on routine media to produce profuse cottony colonies.
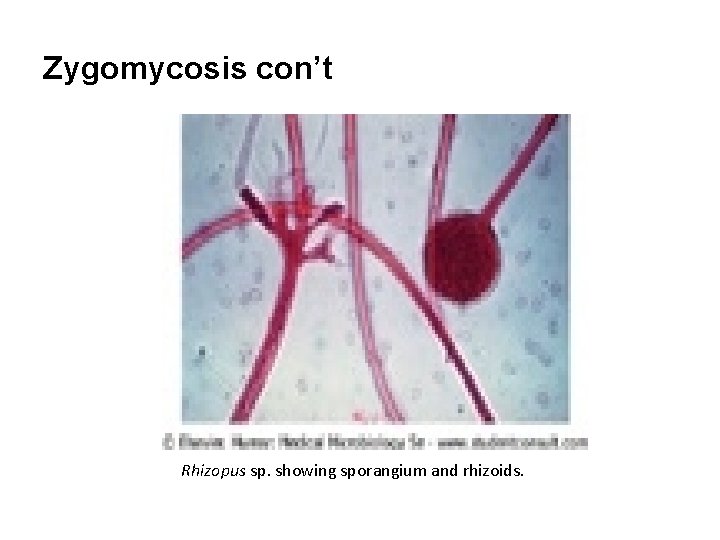
Zygomycosis con’t Rhizopus sp. showing sporangium and rhizoids.

Pathogenesis and clinical picture • One of the most common forms observed in the rhinocerebral form in which the nasal mucosa, plate, Sinuses, orbit, face, and brain are involved; each shows massive necrosis with vascular invasion and infraction. • Other types of infection involved the lungs and gastrointestinal tract; some patients develop disseminated infection. • Organs including the liver, spleen, pancreas, and kidney may be involved.

Pathogenesis cont’d… • The hyphae usually invade the upper or lower respiratory tract or through burn wound of the skin. • Lesion progression is usually rapid, spore do not from in vivo. • Laboratory diagnosis • Is based on the demonstration of non-septate hyphae in smears and biopsy sections. • Culture show sporangium containing sporangiospores

6. 4. Cryptococcosis

Cryptococcus cont’d… Definition • The causative organism is cryptoceccus neoformas • Cryptococcosis occurs in sporadic form and as an opportunistic infection associated with immunosupperession. • The organism is found in soil contaminated with bird excreta particularly pigeons. • Infection occurs by inhalation that results in lung infection (Cryptococcus pneumonia). • The infection spreads to the central nervous system and meninges (cryptococcus meningitis).
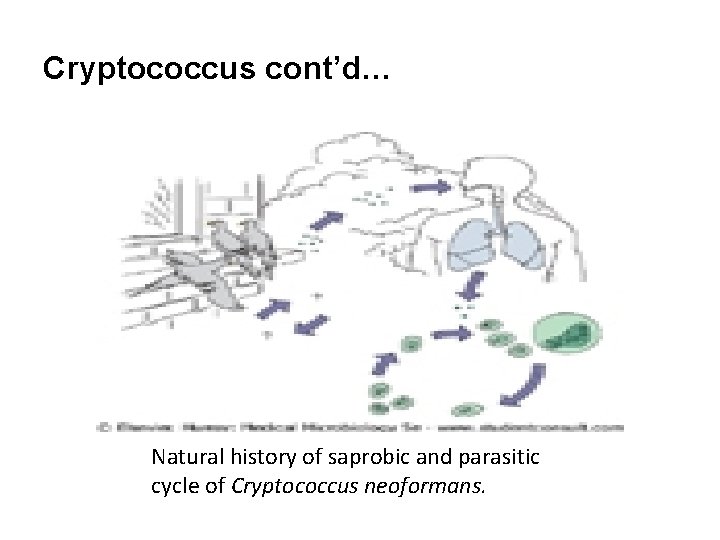
Cryptococcus cont’d… Natural history of saprobic and parasitic cycle of Cryptococcus neoformans.

Laboratory Diagnosis • Detection of Cryptococcus neoformans in sputum and CSF. • The organism is characterized by the presence of large gelationous carbohydrate capsule that surrounds the budding yeast cell. • Direct examination • The capsulated yeast cells are best seen in an India ink preparation (wet mount) • Immunofluorescent stain is applied to dried smear.
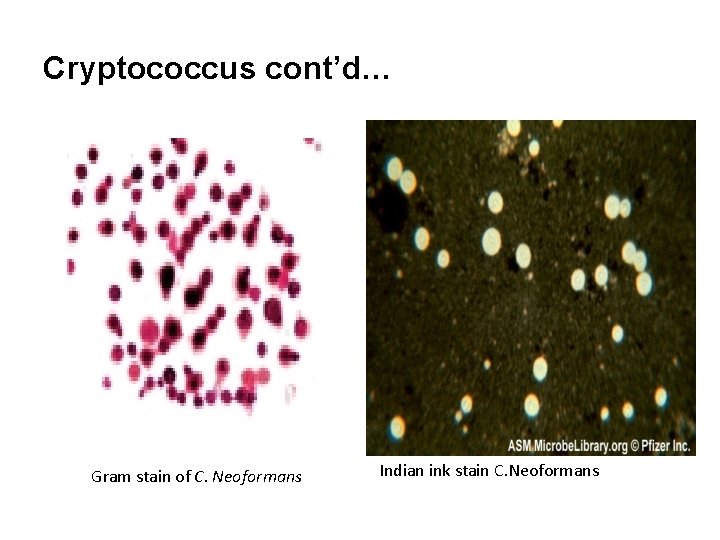
Cryptococcus cont’d… Gram stain of C. Neoformans Indian ink stain C. Neoformans

Laboratory diagnosis cont’d… • Culture and identification • The organism grows easily giving rise to mucoid colonies with the typical capsulated yeast cells. • The organism is ureases positive. • Serologic test • Capsular antigens are detected in C. S. F and in the circulation by using anticapsular antibodies. • Antibodies can be detected in the serum of patients.
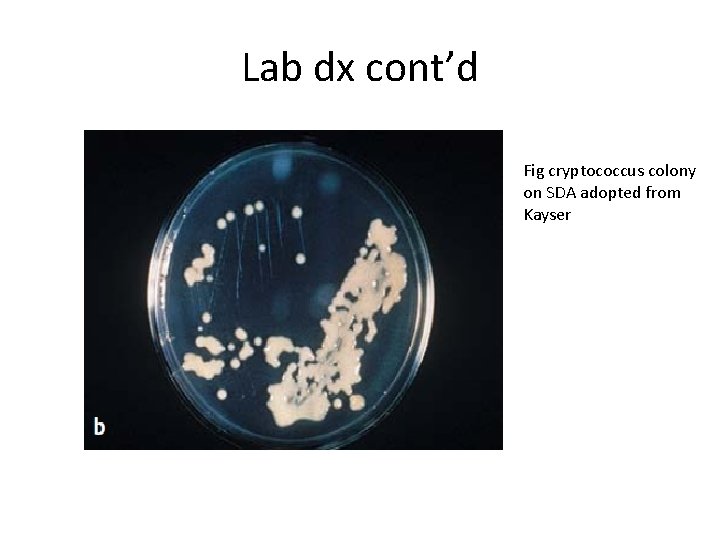
Lab dx cont’d Fig cryptococcus colony on SDA adopted from Kayser

6. 5. Pnemocystis jervocii • Definition • The taxonomy of P. jervocii remains in question, with evidence of classification as both a fungus and a protozoan. • Ribonuclic acid (RNA) sequencing, cell wall composition, ulterastructure, and method of reproduction seem to indicate the organism is fungus. • P. jervocii may thus be reclassified with the fungi. P. carinii is wide spread I nature and often found in several mammals; especially rodents, cats, dogs, sheep, and goats

Pneumocyst jervocii cont’d • The organism has two forms • Cyst stage • It measures 5 -8µm in diameter • May contain up to eight oval interacystic bodies • Trophic or pleomorphic form • It measures 1 -4µm in diameter • Covered with tiny projections for attachment to the host epithelial cells.

Pneumocyst jervocii cont’d • The cyst form is inhaled and the intracystic bodies released in to the alveoli of the lungs. • The tropic form develops and multiplies asexually on the surface of the epithelial cells. • The trophic form than rounds up forming a cyst stages. None of the stage is intera cellular

Pathogenesis and clinical picture • P. jervocii produces a symptomatic pneumonia in debilitated or premature infants who are immunodeficent. • A rapid, progressive pneumonia is also seen is patients with leukemia, following transplants, and most recently in AIDS patients. • In fact. P. jervocii pneumonia was one of the first opportunistic pathogens linked to AIDS. • To days, more than half of all AIDS patients have P. jervocii infection and it is remains a leading cause of death in these patients.

P. jervocii cont’d • The infection may disseminate in AIDS patients in to the eyes, lives, spleen or bone marrow. • Laboratory diagnosis Direct examination • Microscopic observation of the cyst or trophic form in lung secretion or lung tissue after staining using toluidine blue O, Modified Gomori methenamine silver nitrate, or Giemsa
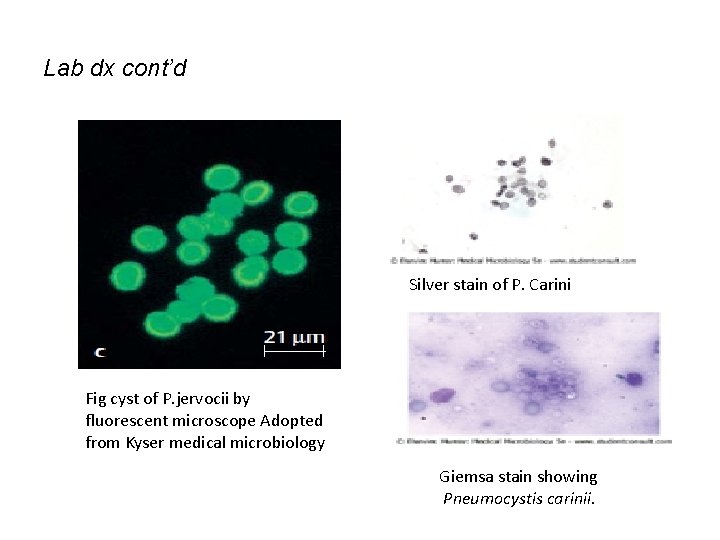
Lab dx cont’d Silver stain of P. Carini Fig cyst of P. jervocii by fluorescent microscope Adopted from Kyser medical microbiology Giemsa stain showing Pneumocystis carinii.
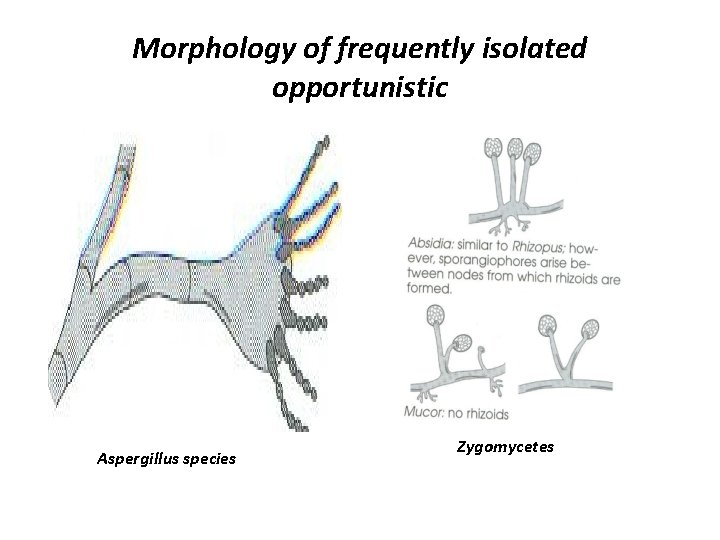
Morphology of frequently isolated opportunistic Aspergillus species Zygomycetes

Summery of opportunistic mycoses Adopted from Kayser, Medical Microbiology © 2005

Summary • Write the predisposing factors for candidiasis • list the laboratory test used to diagnose candidiasis • How do you differentiate candida albican from other candida species • Explain the clinical presentation of Aspergilloma

References • Murry Medical Microbiology • Sherris Medical Microbiology an introduction to infection • Kyser Medical Microbiology 2005 • Lippincott’s Illustrated review in Medical Microbiology • Jawetz, Melnick, & Adelberg's Medical Microbiology, 24 th Edition
- Slides: 49