Chapter Four subcutaneous mycoses Acknowledgments Addis Ababa University

Chapter Four: subcutaneous mycoses

Acknowledgments • Addis Ababa University • Jimma University • Hawassa University • Haramaya University • University of Gondar • American Society for Clinical Pathology • Center of Disease control and Prevention in Ethiopia. 2

Outline of presentation • Objective • introduction • Sporotrichosis • Maudromycosis • Phaehyphomycosis • Chromoblastomycosis • Rhimosporidiosis • Summary

Objective • Upon completion of this chapter, the student should be able to: § List the common subcutaneous mycosis § Describe the etiological agent, epidemiology, pathogenesis and clinical picture of those fungal infections § List the type of Laboratory tests used to diagnostic feature of those subcutaneous mycoses

Introduction • Subcutaneous mycoses are infections confined to the subcutaneous tissue with out dissemination to distant sites. • This classification is artificial. • The other agents causing subcutaneous infections may also produce disseminated infection occasionally. • Humans and animals serve as accidental hosts after traumatic inoculation of the organism into cutaneous and subcutaneous tissues.

Intro cont’d. . • The following subcutaneous mycoses are considered here: Phaeohypho mycosis, Sporotrichosis Chromoblastomycosis Maduromycosis Rhinosporidiosis

4. 1. Sporotrichosis § Chronic infection caused by sporotrichum schenckiidimorphic fungus. • Epidemology • Sporotrichosis has a worldwide distribution, but unusual circumstances associated with a particular epidemic or a series of cases have called attention to what would seem to be area of high endemicity

Source of infection • Sporotrichum schenckii exists in nature where it has been isolated from soil, wood and plants. • Human being and animals become infected by contact with contaminated materials at the time of an injury to the skin of hand, arm and leg, and inhalation. • Human infections have resulted from contact with infected animals.

Source of infection cont’d… • Handling contaminated dressing from lesions of sporotrichosis may infect man but there is no record of direct transfer of the infection from man to man. • The infection is an occupational hazard for farmers, nursery workers, gardeners, florists, and miners. • It is commonly known as “rose gardener’s”disease.

Pathogenesis and clinical picture • The primary lesion begins as a small, non healing weer, commonly of the index finger or the back of the hand. • The infection is characterized by § the development of nodular lesions of the skin or subcutaneous tissues at the point of contact § It involves lymphatic channels and lymph nodules draining the region.

Pathogenesis cont’d… • The subcutaneous nodules break down and ulcerate to form an infection that becomes chronic. • Only rarely is the disease disseminated; pulmonary infection may be seen Fig. Lymphangitic sporotrichosis Adapted from R. J. Hay & M. K Moore, Mycology

Laboratory diagnosis • A critical examination of cultures obtained from patients with sporotrichosis suggests that one species; S. schenckii is the sole etiologic agent. • Separation into different varieties or species has been based on: - • The different colors of colonies on artificial cultivation. • Variations in distribution of spores on the hyphae and, • The production, of “ray- shaped” hyphae bodies in lesions.

Direct examination • Exudates from unopened subcutaneous nodules or from open draining lesions are often submitted for culture and direct microscopic examination. • 10% KOH • Reveals yeast cells (unicellular reproduced by budding)

Culture and identification • A definitive diagnosis can be made on culture by using pus collected from un opened subcutaneous nodules with a sterile needle and syringe or is obtained from open chancre like lesions by swabbing. • Such materials should be streaked on: § Blood agar and sabouraud’s glucose agar slants maintained at 370 c § and room temperature, respectively. § Antibiotic media are used when open lesions are cultured.

Culture cont’d…. On sabouraud’s glucose agar at room temperature the growth is recognizable with in 3 to 5 days. At first, the colonies are: Small and white No aerial cottony mycelium. As growth increase the surface of the colony becomes moist, Wrinkled and membraneous.

Culture cont’d… § The color may vary from § cream to black; § individual strains are not constant in their pigment formation and will change frequently when transferred to fresh media.

Culture cont’d Microscopically • the delicate (2µ in width), branching, septate hyphae bear conidia laterally or in groups from the ends of lateral branches.

Culture cont’d… The conidia are • pyriform, ovoid to spherical, • but become round and thick-walled in old cultures and are • 2 to 4 µ by 2 to 6µ in size. • Their variable distribution along the hyphae prevents separation into different species. § The tissue or yeast like phase of S. schenckii can be obtained on Francis’ cystin blood agar or brain- heart infusion glucose blood agar cultures at 370 c §.

Culture cont’d…. § Materials inoculated directly from lesions or transfers from sabouraud’s glucose agar cultures develop grayish- § yellow, § soft-bacteria- like colonies in two to three days. § Microscopically such colonies are composed of § cigar shaped, § round, oval and budding cells, § similar to those seen in smears from infected animals. Which stained by Gram’s Method they appear gram positive

Animal inoculation • Pus, saline suspensions of cells from the yeast phase cultures or filamentous cultures should be inoculated intraperitoneally into white rates or mice. • Such inoculated animals develop peritonitis, and organisms can be seen by direct examination and cultured from these infected sites. • Smears of pus from such lesions reveal • numerous gram positive, cigar shaped, intra cellular organisms

4. 2. Maduromycosis (Madura foot, Mycetoma) § resembles actinomycotic mycetoma in § both diseases are caused by a variety of different species of fungi § the infections, which are usually confined to the feet, present the same clinical characteristics. § Whether they are caused by the actinomycetes or the large filament- producing species of the higher fungi.

Maduromycosis cont’d… • In both maduromycosis and actinomycotic mycetoma, the organisms occasionally invade the body, producing lesions in the § brain, § the meninges § other internal organs, including the bones. § Maduromycosis is a chronic infection characterized by the development of tumefactions and sinuses.

Maduromycosis cont’d… § At least six distinct species of filamentous fungi can cause this type of infection. § The infection occurs most often in the feet but may appear on the hands or buttocks. § One of the etiologic agents, Allescheria boydii, can invade the blood stream in the rare instances and cause lesions of the § brain, meninges, § lungs, sinuses, § prostate, bones and other internal organs.

Epidemiology § Geographical distribution § Maduro mycosis is common among persons who live in tropical and sub tropical regions § It is common on peoples with outdoor occupations and failure to wear protective clothing predispose them to trauma. § Monosporium apiospermum and its perfect state, Allescheria boydii are found most frequently in USA, South America and Europe but rarely in Africa.

Epidimiology cont’d… • Leptosphaeria senegalensis was isolated from cases of typical maduromycosis in Africa. • Though madurella mycetomii is found in Europe and second to be the dominant species in Africa.

Source of infection • Exogenous • injury, such as a minor scratch, a bruise or a wound produced by a splinter. • Of the organisms isolated from maduromycosis, most are thought to occur either as saprophytes in the soil or on the plant. e. g. Allescheria bodii • occurs more commonly in men than in women and can be related to the soil and opportunity for trauma or injury to an exposed surface of the body.

Pathogenesis and clinical picture • The mode of onset is neither characteristic nor uniform. • With or with out a history of previous injury, the first detectable lesion may be: • small papule, • a small nodule which is deep- seated and fixed, • an indurated area surmounted by a vesicle or • an abscess which ruptures with subsequent formation of a fistula. • The disease progresses slowly and is at first characterized by periods of remissions and relapses.

Pathogenesis cont’d… • 6 or 8 papules may form in succession, • 12 abscesses may develop and disappear over a period of months or years before the entire foot becomes involved and presents the characteristic clinical picture. • The classical picture of swellings and deformities may develop with in a period of months, but it usually takes much longer

Pathogenesis cont’d… • The infection extends deeper into the tissues like • the muscles bones • fascia and tendons • foot or hand becomes club- shaped or may develop into a globose mass two or three times the normal size. • The skin becomes discolored, and pitted scars, nodules formation and multiple sinuses develop.

Pathogenesis cont’d… • Nodules frequently develop about the openings of fistulas from which a serosanguineous or, “Oily” fluid, containing the diagnostic granules, is draining. • These granules may be white to yellowish or black in color, depending up on the infecting fungus.
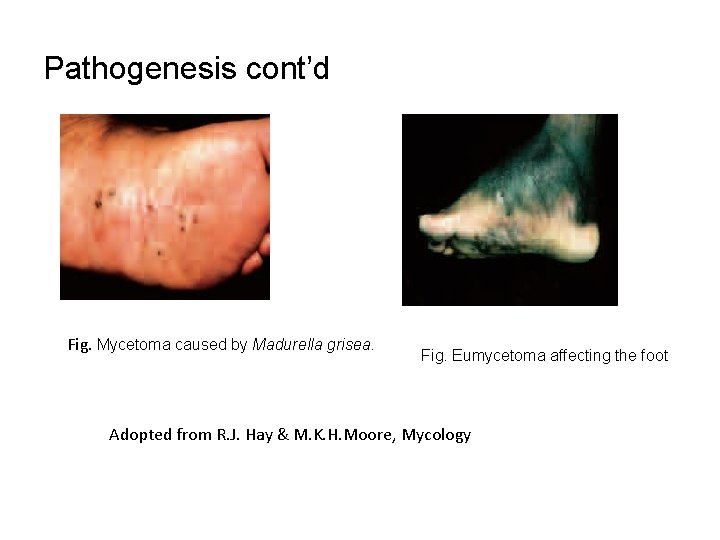
Pathogenesis cont’d Fig. Mycetoma caused by Madurella grisea. Fig. Eumycetoma affecting the foot Adopted from R. J. Hay & M. K. H. Moore, Mycology

Laboratory diagnosis • The numerous fungi that have been isolated from cases of maduromycosis fall into two classes: • ascomycetes • fungi imperfecti. - In the ascomycetes are found the general • allescheria • Leptosphaeria,

Laboratory diagnosis cont’d… In the fungi imperfecti are found species of the genera • Madurella, cephalosporium, • hialophora pyrenochoeta, • Monosporium opiospermum to be the imperfect stage of Allescheria boydii • it also is retained in this group because, the majority of isolates in this fungus do not produce the perfect stage in culture.

Direct examination § Sample § Pus from multiple draining fistulas or aspirated from un opened fluctuant areas with a sterile needle and syringe § Material obtained by curettage or biopsy should be collected in a sterile petri-dish § Gross examination § Pus-currettings, or biopsy tissues should be examined grossly for “grains”. (Grains seen as small (0. 5 to 2 mm) White, yellow, brown or black)

Microscopic examination § Using a drop of water or 10% KOH § Grains contain- wide hyphae with hyphal swelling Chlamydospores, and so forth, and should not be mistaken for the granule seen in actinomyeotic mycetoma • Note: the microscopic distinction of the granules and grains is very important for immediate differentiation of actinomycotic mycetoma and maduromycosis because granules found in actinomycotic mycetoma where as grain is found in maduromycosis.

Cultures § Material aspirated from unopened lesions should be cultured directly on sabouraud’s glucose agar at room temperature. § Grains obtained from open, draining fistulas should be washed in several changes of sterile saline to avoid gross contamination and then planted on sabouraud’s glucose agar to which antibiotic have been added. § Note: - Colony characteristics depends on the individual fungus causing the disease.

Allescheria boydii The grain is: § large, round to lobulated mass hyphae § White to yellowish Hyphae are 2 to 4 µ in diameter § hyphal swellings, particularly at the periphery the colony § grows rapidly, producing a white, cottony aerial mycelium which later turns gray or becomes buff to brown in color

Allescheria boydii cont’d… • Microscopically § asexual conidia, 8 to 10µ long by 5 to 7µ wide, § produced singly at the ends of long conidiophores § or from the sides of the mycelium on short conidiophores • Tufts of conidiophores (coremia), each bearing a single conidium at the tip, are seen occasionally, as are conidiophores which some time branch and produce a whorl of sterigmata each terminating in a conidium.

Allescheria boydii microscopy cont’d… §Dark brown, thin walled perithecia 50 to 200µ in diameter are produced in the culture on the surface of the agar §when; crushed and examined microscopically, the delicate evanescent asci and ascospores emerge from the ruptured percthecia. §The elliptical yellowish brown ascospores are 4. 0 to 4. 5µ x 5. 5 to 7µ in size §Isolates which produce only the asexual condial forms described above are named Mono sporium apiospormum

Allescheria boydii cont’d… §M. apiospermum §The imperfect stage of A. boydii §A. boydii is usually associated with maduromycosis in man, mycotic keratitis, septicemia, meningitis and pulmonary infection

Phialophora jeanselmei The grain may be § crescent shaped, round or ovoid § it is brown in color § produces an olivaceous to black colony which is at first moist and shiny in appearance but quickly becomes over grown with an alive- gray aerial mycelium.

Phialophora jeanselmei cont’d… Microscopically • the primary culture consists of many cells, which reproduce by budding. • Eventually, however, the culture sporulates with clusters of spores produced from the tips of conidiophores, from the sides of conidio phores and from short apiculi from the sides of the hyphae. Animal inoculation • It is possible to inoculate the mice introperitonially and produce maduromycosis

4. 3. Phaeohyphomycosis • is a general term used to describe any infection caused by a dematiaceous organism. • The strict definition does not include chromoblastomycosis or mycetoma. • However, the term used with in this text refers to subcutaneous, localized, or systemic infection caused by any type of dematiaceous fungi. • Infection includes subcutaneous abscess, brain abscess, sinusitis, endocarditis mycotic keratitis, infection, and systemic infection. pulmonary

Phaeohyphomycosis cont’d… • Common etiological agents of subcutaneous infection include: • Exophiala jeanselmei • Phialophora richardsial • Wangiella dermatitidis • Alternaria spp. • Bipolaris spp. • Exsero hilum spp.

Laboratory examination • Direct examination • made by observing yellowish –brown septate, moniliform hyphae with or with out budding cells present. • The methenamine silver stain of tissue often over stains fungal elements and the observation of pigmented hyphae in hematoxyline-eosin or unstained histopathologic sections will provide the diagnosis of this clinical entity.

Culture and identification • Culture of specific etiological agent is necessary for final confirmation. A. Exophiala jeanselmei: • dematiaceous organism that grow slowly (7 to 21 days) and produces- shiny black, yeast like colonies initially. • With age, colonies become filamentous, velvety, and gray to olive to black.

Culture and identification cont’d… • The microscopic features of young colonies exhibit dematiceous budding yeast cells with annellations (difficult to observe). • Filamentous colonies produce dematiaccous hyphae and conidiogenous cells that are cylindrical and have a tapered tip • Annellations may be visible at the tip and clustorsof oval to round conidia are apparent • Cultures can grow at 370 C not at 400 C and can utilize inorganic KNO 3

Culture cont’d B. Wangiella dermatitidis • It is a dematiaceous organism that grown slowly (7 to 21 days) and produces- shiny, black, yeast like colonies initially. • With the age colonies become filamentous, velvety, and gray to olive to black in color. • The microscopic features of young colonies exhibit dematciaceous budding yeast cells

Culture cont’d • Filamentous colonies produce dematiaceous hyphae and long tubular phialides lacking collarettes. • Phialides produce dematiaceous single- called conidia in clusters. • Balls of conidia may appear to slide down the hyphae. • cultures can grow at 400 C and cannot utilize KNO 3 in contrast to E. Jeanselmei

Phialophora richardsial § Dematiaceous organism § Grows rapidly and produces colonies that are wooly, olive- brown to brownish- gray; some may appear to have concentric zones of color. • Microscopically, hyphea are dematiaceous, and sporulation are readily observed. • Pleomorphic phialides may also be seen; however, all produce either or both hyaline elliptical conidia or brown elliptical conidia produced with in the phialides

4. 4. Chromoblastomycosi(chromomycosis, verrucous dermatitis § The name’chromoblastomycosis” is misleading because the fungi do not form buds (blastospores) in tissue. • They have a brownish color when seen un stained in the tissues, but this does not warrant the name chromosmycosis which implies that the lesions have a characteristics color. • The term “Chromoblastomycosis” has been retained because it has become established so firmly in the literature

Chromoblastomycosis cont’d… • • caused by a variety of dematiaceous fungi, characterized by the formation of warty cutaneous nodules which develop very slowly, • ultimately forming prominent papillomatous vegetations which may or may not ulcerate. • Usually, the lesions are confined to the feet and legs but have occurred on the hands, face, ear, neck, chest, sholders and buttocks. • With few exceptions, however, the lesions have been confined to the lower extremities

Epidemiology • Geographical distribution § The disease has been reported from every continent of the world. § Although the majority of cases have been found in the tropical and sub tropical areas of the world. Source of infection • The various fungi, which cause chromoblastomycosis undoubtedly, exist in nature and are introduced into the tissue by trauma. • And it is common among the age groups between 30 and 50 years.

Pathogenesis and clinical picture • The infection is located almost invariably on some exposed part of the body and nearly always is unilateral. • An occasional case has been reported in which both a leg and an arm were affected. • The lesion begins as a small, itchy papule which extends eccentrically and simulates a patch of ring worm. • The original patches are usually sharply limited, dull red or violaceous in color and present marked degrees of infiltration.

Pathogenesis and clinical picture cont’d § After various intervals of time, often months later, crops of new lesions appear along the paths of the superficial lymphatic drainage • The involved areas extend 1 to 2 mm, above the surrounding skin and frequently develop • markedly elevated, hard dull red or grayish nodules in the center, giving to the lesion a cauliflower- like appearance.

Pathogenesis and clinical picture cont’d… • Some lesions become pedunculated; other become secondarily infected and ulcerates, but, in general, the eruption has a rather dry appearance. • The infection progresses so slowly that it may take 4 to 5 years to involve an entire arm or leg. • Extensive fibrosis develops in the deeper tissues and the lymphatics become blocked producing elephantiasis of the extremity.

Pathogenesis and clinical picture cont, d… • The lesions are painless unless they are complicated by secondary bacterial infection. Some lesions heal spontaneously leaving only areas of hyper- pigmentation. • As in tuberculosis and syphilis, the early lesions of chromoblastomycosis are so protean that the diagnosis can be made only by laboratory methods.
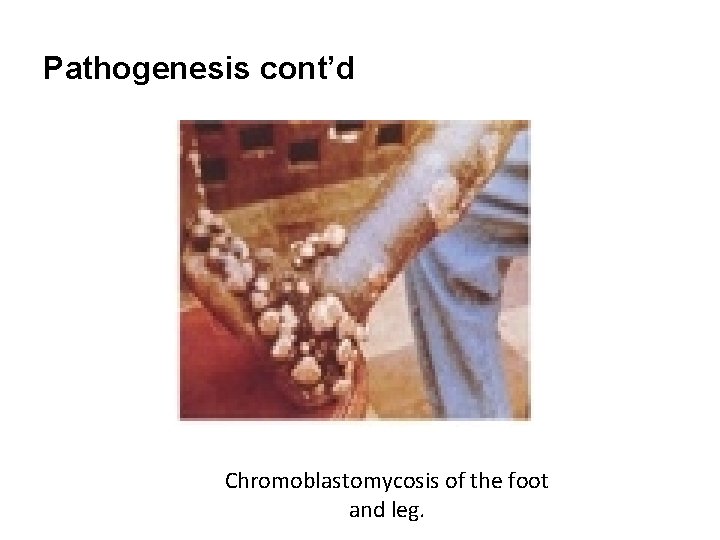
Pathogenesis cont’d Chromoblastomycosis of the foot and leg.

Laboratory diagnosis • A variety of closely related dematiaceous fungi are recognized etiologic agents of chromoblastomycosis. • Fonsecaea pedrosoi, • Fonsecaea compactum and • phialophora verrucosa are three most familiar fungi

Laboratory diagnosis cont’d… • Several new genera have been created for the single species F. pedrosoi because of the great variation displayed in its microscopic morphology in culture. • Depending upon the medium used and the particular strain studied, strains of this species vary in their method of spore production. • Three types of sporulation are recognized • Acrogenous catenate sporlation of the cladosporium type, • Acropleurogenous sporlation of the Acrotheca type and

Laboratory diagnosis cont’d • Semi endogenous sporlation of the phialophora type. • By placing under emphasis on the predominant type of conidial formation in the particular strain being examined, this • acrotheca, Trichosprium, • Gomphinaria, Botrytoides, • Hormodendroides, Phialoconidiophora, Pormodendrum, Phialophora and Fonsecaea.

Direct examination • Crusts from the verrucous lesions should be placed on a slide in a drop of 10% KOH and examined under a cover glass. • The preparation may be heated gently over a low flame of a Bunsen burner or alcohol lamp to hasten clearing. • Exudates from the lesions may press to a thin film under a cover glass and examined directly. .

Direct examination cont, d… • The various fungi, which cause chromoblastomycosis, produce identical forms in tissue • the genus or species of fungus producing the infection cannot be determined by direct examination • The tissue forms appear as: § Single or clustered § Round, thick- walled § Dark brown bodies 6 to 12μ in diameter, which multiply by splitting and not by budding.
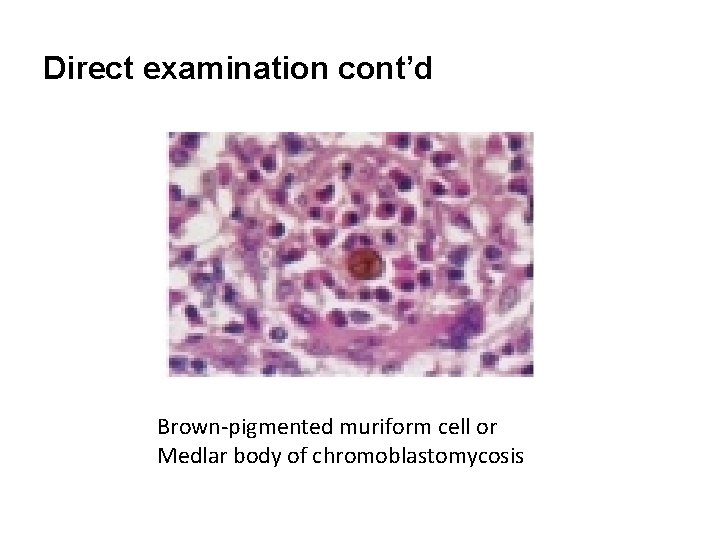
Direct examination cont’d Brown-pigmented muriform cell or Medlar body of chromoblastomycosis

Culture and identification Material from the lesions should be cultured on sabouraud’s glucose agar with antibiotics at RT to maximum of 3 weeks • Forsecaeapedrosoi: - produces slow- growing colonies, • Colonies are dark brown to black on sabouraud’s glucose agar. • Rate of growth • Gross colony characteristics • Individual strains show great variation in - color,

Culture and identification con’t, d. . • Microscopically, different strains of F. pedrosoi vary greatly based on : - § method of conidial formation, § depending upon the strain studied § the medium used. • As noted previously, three different methods of sporulation are recognized.

Culture and identification cont’d • The cladosporium type is characterized by: • Conidiophores of varying lengths bearing conidia terminally in branching chain formation. • Such conidia are single- celled vary from 3 to 6μ in length and 1. 5 to 3 μ in width and are connected in the chain by thick disjuncture • When conidial chains are broken and the spores lie free in the preparation they may be identified by their olive to brown color and the black points on the ends where they had been joined together.

Culture and identification cont’d § The Acrotheca type of sporulation § Develops as a terminal cell or as single lateral branches on the aerial hyphae. § Such cells become swollen, assuming the shape of knotted clubs from which the conidia are borne acropleurogenously on short protuberances along the length of the conidio phore.

Culture and identification cont’d The phialophora type is characterized by: • Flask-shaped conidiophores with a terminal cuplike structure bearing groups of conidia. • Large, round, carbonaceous, cleistothecia- like bodies have been produced by one strain of F. pedrosoi on corn meal agar cultures. Asci and acsospores were not developed with in these structures.

Culture and identification cont’d • The three types of conidial formation mentioned above are found among the difficult strains in varying proportions. • The phialophor type usually scant, or may be lacking. • Some strains will have predominantly the cladosporium type: • others will have predominatly the acrotheca type; and • many strains will have both cladosporium and acrotheca types in approximately equal numbers

Culture and identification cont’d • Fonsecaeacompactum: - grows very slowly on sabouraud’s glucose agar producing a heaped , brittle colony, • Olive black in color, with a short nap like aerial mycelium. • After the 4 to 5 weeks, it will produce, Tufts of brownish mycelium project from the center of the colon. • These tufts should be examined microscopically for the typical conidiophores and spore formation of the species.

Culture and identification cont’d • Microscopically, F. compactum is characterized by the formation of terminal and lateral conidio phores bearing compact masses of short and long branching chains of subspherical conidia 1. 5 to 2 μ by 2 to 3 μ in size. • The phialophora type of conidiophore is produced also in this species when grown on cornmeal agar. • This species differs from F. pedrosoi in the compact arrangement of the conidial chains, which are not easily, dissociated and in the subspherical conidia.

Culture cont’d • Phialophora dermatitidis: - This species has two colony types: at first the colony is black, moist, shiny, soft and yeast like. • In about 3 to 4 weeks, a continued mycelial development at the periphery of the colony converts the growth to one with a more filamentous character sectors of mycelium also form on the colony.

Culture and identification cont’d • Microscopically, F. dermatitidis is composed of oval to spherical budding yeast like cells in the primary culture. • These cells continue to bud, forming masses from which slender hyphae eventually arise. • Along the course of the slender hyphae, a rapid budding of cells from tiny protuberances forms clusters of spores. • This is a characteristic of spore formation in pullularia

Culture and identification cont’d • Rarely clusters of spores may be seen to raise pleurogenously from an occasional hyphal branch. • An occasional cell with a terminal cup of the phialophora type is also seen. In tissue the brown, septate bodies are found in large, compact clusters unlike the scattered isolated cells of the other agents of chromoblastomycosis. Cladosporium carrionii • grows slowly on sabouraud’s glucose agar. • Produce colonies only 2 to 4 cm. in diameter in 3 to 4 weeks.

Culture and identification cont’d • The colony is usually flat with a slightly raised center covered with velvety gray-green to purplish – brown, • Short nopped mycelial surface. • Microscopically, only the cladosporium type of sporulation is seen lateral and terminal conidiophores of varying lengths produce long branching chains of smooth walled conidia which are easily dispersed. • The acrotheca and phialophora types of sporulation are completely lacking.

Culture and identification cont’d Phialophora verrucosa • produces slow growing colonies • Colonies are greenish- brown in color with a close matlike aerial mycelium. • Some strains may be heaped and granular; others may be more flat with a matted appearance.

Culture and identification cont’d • Microscopically, P. verrucosa produces: • Conidia from cups at the tip of flask shaped conidiophores borne terminally or laterally, singly or in groups, on the aerial mycelium. • The conidiophores are about 3 to 4μ long. • The conidia are thin-walled, oval cells, averaging 1. 5 μ in width and 4 μ in length. • In undisturbed preparation such conidia are held in compact masses at the cup- shaped tips of the conidiophores.

Culture and identification cont’d • One strain of this species has produced cleistotheica like bodies similar to those described previously in one strain of F. pediosoi. • This fungus differs from the other etiologic agents of chromoblastomycosis by the development of conidia from flask- shaped conidiophores. Animal inoculation • (Rat, mice, rabbits, guinea pigs, dogs and monkeys) it is possible to inoculate and produce variety of lesions for same of the species of fungus.

4. 5. Rhinosporidiosis • the etiologic agent of Rhinosporidiosis has not been cultured • it is assumed by most observers that it is a fungus because of the Morphologic characteristics of the organism as it appears in tissue. Definition • Rhinosporidiosis, caused by Rhinosporidium seeberi • is an infection of the mucous membranes of the nose, eyes, ears, larynx and occasionally the vagina, penis and skin

Rhinosporidiosis cont’d… characterized by the development of friable, sessile or pedunculated polyps. Epidemiology Geographic distribution • The infection has been found in different countries, but it is endemic in India and Ceylon and sporadic in other parts of the world • Source of infection

Rhinosporidiosis cont’d… • The organism causing this infection has not been cultured and has not been transmitted to man or animals by experimental inoculation. • The disease occurs spontaneously in horses, cows and mules. It is suggested that the infection was carried by dust or water. • The disease developed only in those who dived or swam in water. It has been suggested, also, that the infection is primarily a disease of fish and that man and animals are accidental hosts.

Rhinosporidiosis cont’d… • It is also noted that the disease may develop at any age between 5 and 84 years, but is seen most commonly in children and young adults. • Males are more often infected than females. Pathogenesis and clinical picture • The symptomatology varies according to the site of infection and the size of the tumor masses which develop.

Rhinosporidiosis cont’d… § The first symptom usually is that of a pain less itching sensation in the nose and is accompanied by the development of a profuse mucoid discharge. § Purulent discharges are infrequent and bleeding is rare unless the lesion is traumatized by a blow or by scratching. § The lesions at first are sessile on the mucosal but as the tumor masses develop they become pedunculated by constriction at the base.

Rhinosporidiosis cont’d… § The fully developed swellings are globoid or polypoid and those on the anterior part of the nose may hang down over the upper lip. § If the growth develops in the posterior nares § it may project into the posterior pharynx, where it is seen as a papillomatous tumor with out mucinous bags.

Rhinosporidiosis cont’d… • In the posterior pharynx and in the larynx, the gradually enlarged polypes may produce nasal obstruction, dyspnea and dysphagia. • In general the disease can spread to eye to the extent of causing of infection of lacrimal sac and lesions of the ear, bronchi, genital area and the rectum. • Infections in the vagina and rectum resemble condylomata, hemorrhoids or rectal polyp. • The general health of the patient is not effected by local tumors, and the lesions may persist for as long as 35 years.

Laboratory diagnosis § Rhinosporidum seeberi was said to have been cultured on T. C 199 medium, by Grover. § However, the life cycle of the organism in tissue, as described by Ashworth and others, can be summarized as follows § The infecting spore is a small (6 to 7 μ in diameter) rounded body with a some what thickened chitinous wall, anucleus and a karyosome which increase in size until it becomes 50 to 60 μ in diameter and nuclear division occur, revealing 4 chromosomes.

Lab dx cont’d § Further increase in size 100 μ in diameter at this time a thick layer of cellulose is deposited inside the chitinous outer membrane. § At one point on the periphery, however, a thinning of the wall occurs and the resulting “pore” remains until the sporangium containing approximately 4000 spores § Two more divisions increase the number of spores to approximately 16, 000. uniformly sized granules or spherules.

Lab dx cont’d • Such spores are spherical, 7 to 9 μ in diameter, have a thin chitinous membrane and contain a nucleus with karyosome and servral • Such small granules, about 1. 5 μ in diameter, are not thought to be reproductive bodies. As the spores mature.

Lab dx cont’d • The sporangium becomes • larger (300 to 350 μ in diameter) • the spores are liberated by rupture of the sporangium at the ’pore” Many investigators believe that these spores can infect tissue directly and repeat the life cycle of the fungus. • Can’t transmit from man to man or animal to animal

Direct Examination • Direct examination of material from the polypoid masses reveals sporangia and spores. • Such material may be squeezed gently with a forceps in a drop of water and examined directly under a cover glass. • The exudates which adhere to the bladder of the forceps also may be used, as can materials from nasal secretions. • Round to ovoidspores 7 to 9 μ in diameter, and sporefilled sporangia should be seen in such preparations.
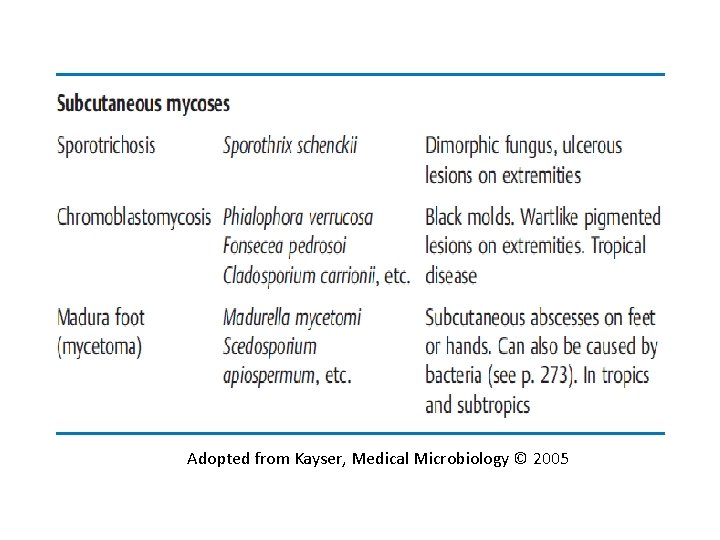
Adopted from Kayser, Medical Microbiology © 2005

Summary 1. one of the following produce a ‘ray shaped’ hyphae bodies in lesions A. phaeohyphomycosis. B. Maduromymycosis C. sporotrichosis D. all 2. What is the difference between grain and granules? 3. Write the colony characteristics of cladosporium carrionii. 4. What do expect from grain during microscopic examination after 10 % KOH.
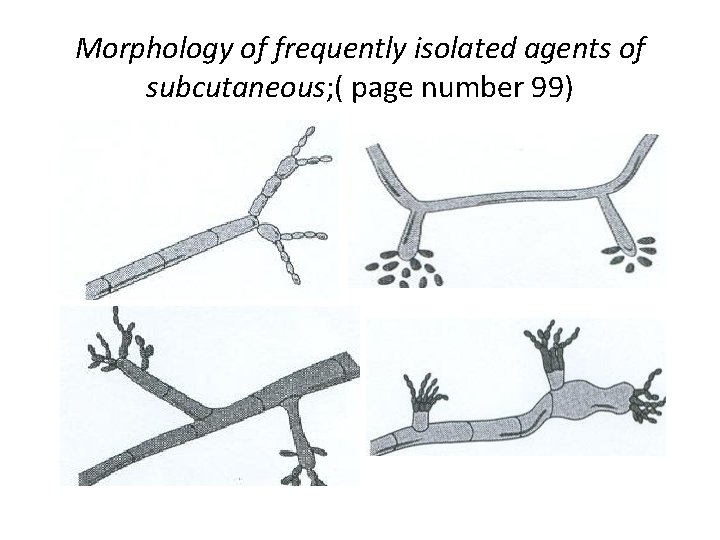
Morphology of frequently isolated agents of subcutaneous; ( page number 99)
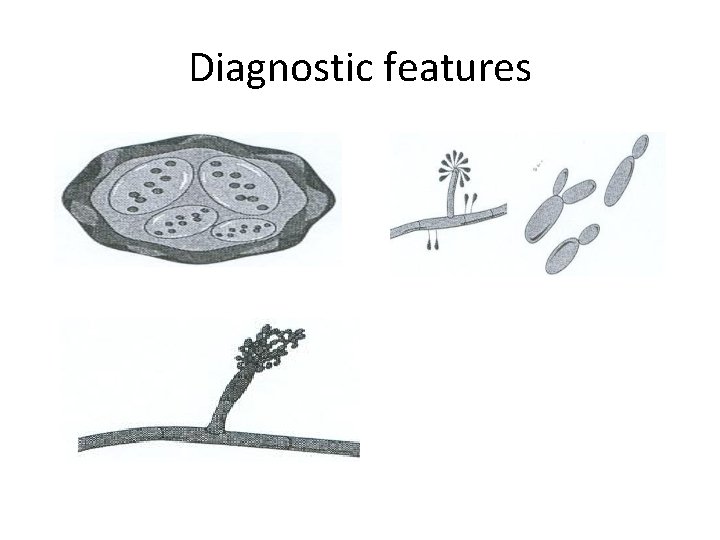
Diagnostic features
- Slides: 95