chapter 92 EVALUATION AND NONSURGICAL MANAGEMENT OF BENIGN

chapter 92 EVALUATION AND NONSURGICAL MANAGEMENT OF BENIGN PROSTATIC HYPERPLASIA THOMAS ANTHONY MCNICHOLAS, MBBS, FRCS, FEBU L ROGER SINCLAIR KIRBY, MD, MA, FRCS L HERBERT LEPOR, MD

Introduction � Abrams (1994) has suggested using the more clinically descriptive terms BPE, BOO, and LUTS to replace BPH, but the time-honored, although limited, original terminology persists. � The specific molecular events that initiate and promote microscopic BPH have yet to be identified and characterized. Growth factors, such as EGF, are involved through autocrine and paracrine stromalepithelial interactions � DRE provides a relatively crude estimate of prostate size when compared with TRUS or MRI � There are numerous epidemiologic data to confirm that BPH is a slowly progressive disease and that men with a larger prostate (or higher (PSA) are at significantly greater risk of BPH progression, LUTS, impaired quality of life, and complications such as AUR

DIAGNOSIS �The complex of symptoms now commonly referred to as “LUTS” is not specific for BPH. �Nonprostatic causes of symptoms can be excluded in a significant majority of patients on the basis of history, physical examination, and urinalysis �IPSS is recommended as the symptom scoring instrument to be used for the baseline assessment. �The IPSS is the ideal instrument to grade baseline symptom severity, assess the response to therapy, and detect symptom progression in those men managed by watchful waiting

Initial Evaluation(1) � 1 - Medical History � 2 - Physical Examination: A DRE and a focused neurologic examination should usually be perform. DRE provides a sufficiently accurate measurement in most cases. � 3 - Urinalysis: should be done for rule out UTI and hematuria � 4 - Urine cytology: should always be requested in men with severe irritable symptoms and dysuria, especially if they have a smoking history. � 5 - Creatinine: Fifth International Consultation on BPH was suggested that creatinine should be optional or secondary. The AUA guidelines on BPH and the Sixth International Consensus report no longer recommend routine creatinine measurement in the standard patient.

Initial Evaluation(2) � 6 - Serum PSA: �A; should be performed in patients in whom the identification of cancer would clearly alter BPH management. �B; In the absence of prostate cancer the PSA value provides both a guide to prostate volume and also an indication of the likelihood of response to therapy with 5α-reductase inhibitors. �C; recent evidence suggests that 5α-reductase therapy actually increases the sensitivity of PSA as a detector of cancer

Additional Diagnostic Tests Additional testing should be considered if there is a significant chance the patient’s LUTS may not be due to BPH. � 1 - Cystoscopy: should not be done routinely � 2 - frequency-volume chart : is recommended by most clinicians �Mild to mod. IPSS: Medical therapy & follow the patient �Mod to sever IPSS: uroflowmetery or UDS, PVR urine �Complications or other indications for surgery: surgery

Diagnostic Tests in Men Who Require Surgery for Benign Prostatic Hyperplasia � Surgery is generally recommended if the patient has refractory urinary retention (failing at least one attempt of catheter removal) or any of the following conditions clearly secondary to BPH: recurrent UTI, recurrent gross hematuria (resistant to 5αreductase inhibitor therapy), bladder stones, renal insufficiency, or large bladder diverticula � Uroflowmetry � Postvoid Residual Urine Volume � Pressure-Flow Studies � Filling Cystometry (Cystometrography) � Urethrocystoscopy � Imaging of the Upper Urinary Tract

Uroflowmetry(1) The AHCPR Guideline Panel reached the following conclusions regarding uroflowmetry: � Flow rate measurements are inaccurate if the voided volume is less than 125 to 150 m. L. � Flow rate recording is the single best noninvasive urodynamic test to detect lower urinary tract obstruction. Current evidence, however, is insufficient to recommend a given “cutoff” value to document the appropriateness of therapy. � PFR or Qmax is more specifically identifies patients with BPH than does the average flow rate (Qave). � no age or volume correction is currently recommended for clinical practice � patients with a PFR greater than 15 m. L/sec appear to have somewhat poorer treatment outcomes after prostatectomy than patients with a PFR of less than 10 - 15 m. L/ sec. � A PFR of less than 15 m. L/sec does not differentiate between obstruction and bladder decompensation.

Uroflowmetry (2) �Failure rates for surgery were found to decrease with the addition of flow rate measurement to symptom assessment in preoperative evaluation �PFR appears to predict surgical outcome in some studies �Neither subjectively assessed symptoms nor quantified symptom score analysis correlates strongly with uroflowmetry measurements �Patients with very bothersome symptoms suggestive of clinical BPH but having a PFR greater than 15 m. L/sec may benefit from further urodynamic testing

Postvoid Residual Urine Volume � Studies indicate that PVR urine , normally ranges from 0. 09 to 2. 24 m. L. Seventy-eight percent of normal men have PVR volumes of less than 5 m. L, and 100% have volumes of less than 12 m. L AHCPR reached the following conclusions regarding PVR urine volume : � PVR urine volume measurement has significant intraindividual variability that limits clinical usefulness. � PVR urine volume does not correlate well with other signs or symptoms of clinical BPH. � Large PVR urine volumes may predict a slightly higher failure rate with a strategy of watchful waiting. However, the threshold volume defining a poorer outcome is uncertain. � It is uncertain whether PVR urine volume indicates impending bladder or renal damage. � Birch and coworkers (1988) reported that of 30 men with BPH, 66% had wide variations in PVR urine volume when three measurements were done on the same day

Postvoid Residual Urine Volume �Most clinical studies demonstrate minimal correlation between PVR urine volume and baseline measurements of symptoms, flow rate, or urodynamic measures of obstruction �However, Neal and associates (1987) found a significant association in 253 men between PVR urine volume, age, “below normal” PFR, and high urethral resistance �PVR urine volume is best viewed as a “safety parameter. ” Men with significant PVR amounts should certainly be monitored more closely if they elect nonsurgical therapy, particularly if antimuscarinic therapy is chosen
Pressure-Flow Studies �Pressure-flow studies differentiate between patients with a low PFR secondary to obstruction or impaired detrusor contractility �Patients with a history of neurologic diseases known to affect bladder or sphincteric functions, as well as patients with normal flow rates (PFR > 15 m. L/sec) but bothersome symptoms, may also benefit from urodynamic evaluation and especially if surgical therapy is contemplated. �Filling Cystometry (Cystometrography) is not recommended in routine cases (C) definitively

Urethrocystoscopy �Urethrocystoscopy is not ecommended (C, definite). �The linkage between the endoscopic appearance of the lower urinary tract and the treatment outcome is poorly documented �Indications: microscopic or gross hematuria, urethral stricture disease, , bladder cancer or suspicion of carcinoma in-situ, or prior lower urinary tract surgery �Urethroscopy is therefore performed to select (or rule out) specific techniques, not to determine the need for treatment

Imaging of the Upper Urinary Tract �Upper urinary tract imaging is not recommended except in: hematuria, UTI, renal insufficiency , history of urolithiasis, or history of urinary tract surgery �approximately one third of all men with BPH have one or another indication for urinary tract imaging

ASSESSING THE EFFECTIVENESS AND SAFETY OF MEDICAL THERAPY � Clinical End Points : The goals of treatment for BPH include relieving LUTS, decreasing BOO, improving bladder emptying, ameliorating detrusor instability, reversing renal insufficiency, and preventing disease progression, which may include a deterioration of symptoms, future episodes of gross hematuria, UTI, AUR, or the need for surgical intervention � 1 -Symptoms : Symptom outcome should be expressed both as a percentage of patients achieving a threshold reduction response and as group mean changes in the symptom score. The group mean changes in AUASI for subjects rating their improvement as markedly, moderately, or slightly improved, unchanged, or worse were − 8. 8, − 5. 1, − 3. 0, − 0. 7, and +2. 7, respectively

Clinical End Points � 2 - Bladder Outlet Obstruction: Because synchronous pressure-flow urodynamic measurements do not correlate with severity of bladder dysfunction, severity of symptoms, or response to therapy, it is difficult to require these studies � 3 - Bladder Emptying: There are no data clearly documenting that the incidence of UTI is related to the PVR urine volume.

Clinical End Points � 4 - Bladder Overactivity: The definition of bladder overactivity (detrusor instability) is the development of a detrusor contraction exceeding 15 cm H 2 O, The clinical significance of an OAB in men with BPH is unresolved. � 5 - UTI, Renal Insufficiency, and Hematuria: Because their incidences is relatively uncommon and non –disease-specific events , it would be extremely difficult to design a prospective study to determine whether any BPH treatment prevents these events in an unselected cohort of men

NONSURGICAL THERAPY � Watchful Waiting or “Self-Help”: Treatment failure in the watchful waiting group was most often the result of increasing PVR volume or symptom score. �Significant renal impairment was not seen. �Unsuccesful for mod. Symptoms in some studies

MEDICAL THERAPY �α-adrenergic blockers � 5α-reductase inhibitors �aromatase inhibitors � plant extracts � antimuscarinic drugs �PDEIs � combinations of these agent

The Impact of Medical Therapy �the lower morbidity of medical therapy is of paramount importance �Candidates for Medical Therapy: Bothesome LUTS & no indication for surgery �Preventing BPH with Medical Therapy: men with very large prostates (and usually higher PSA values) are at greater risk for developing urinary retention and medical therapy (finasteride or dutasteride) can significantly decrease AUR

α-Adrenergic Blockers � They relief dynamic obstruction � Lepor and associates (1990) reported no significant differences between norepinephrine levels, α 1 receptor density, or isometric contractile responses to phenylephrine � Although the prostates of those subjects achieving symptom improvement had a significantly greater group mean area density of smooth muscle compared with those of nonresponders, a direct relationship between prostate smooth muscle area density and change in symptom scores was not observed. These observations suggest that nonprostate smooth muscle– mediated α 1 receptor events may also be responsible for the effectiveness of α-adrenergic blockade and that α 1 receptor–mediated symptom improvement
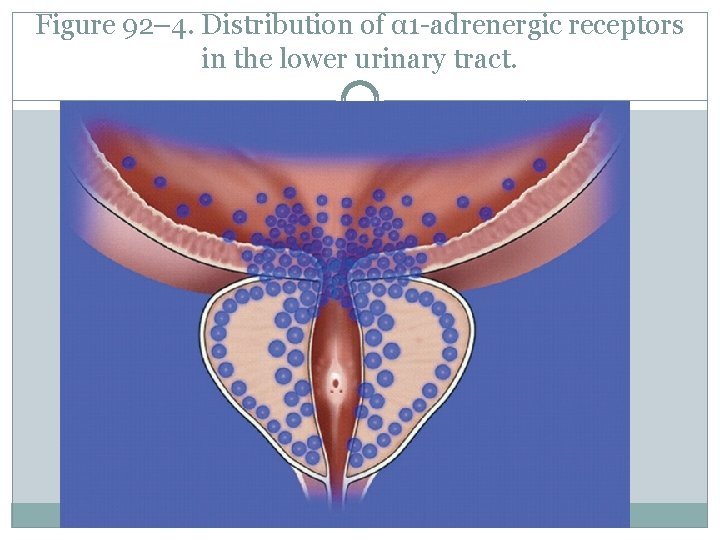
Figure 92– 4. Distribution of α 1 -adrenergic receptors in the lower urinary tract.
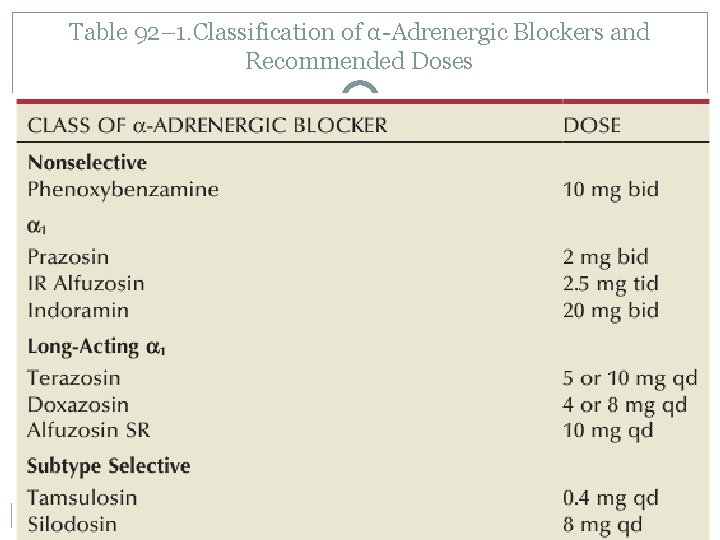
Table 92– 1. Classification of α-Adrenergic Blockers and Recommended Doses

Classification of α-Adrenergic Blockers (C) � The efficacy of phenoxybenzamine and prazosin are comparable; however, prazosin is better tolerated, implying that efficacy and toxicity are mediated primarily by the α 1 and α 2 receptors, respectively � The next advance in the development of α-adrenergic blockers was the development of advanced drugs with serum elimination half-lives that allowed for once-a-day dosing � Tamsulosin is a once-daily administered α 1 antagonist that exhibits some modest degree of selectivity for the α 1 A versus the α 1 B receptor and no selectivity for the α 1 A versus the α 1 D receptor � Recently, silodosin (Rapaflo) has been introduced. This agent shows 162: 1 selectivity for α 1 A versus α 1 B adrenoceptors and is achieving promising results

Interpreting the α-Adrenergic Blocker Literature(Study Designs) � titration to fixed dose: unless significant adverse effects are encountered. An advantage of this study design is that dose-dependent efficacy and safety of different doses are determined � Titration to response : design allows the investigators to titrate the dose to a threshold response or maximal dose. An advantage of this design is a smaller sample size because all subjects receiving active treatment are analyzed as a composite group independent of final dose. A disadvantage of this design is that the maximal therapeutic effect may be underestimated if the titration is not to maximal response. � A randomized dose withdrawal design begins with an open-label dose titration. All responders are randomized to active drug or placebo. An advantage of this design is the enrichment of responders. A disadvantage is that the results are not generalizable to untreated patients. � A titration to maximal dose design, like titration to response, requires a relatively small sample size because there is only one active treatment group. This study design defines maximal clinical response achievable in practice, providing the maximal dose is also the most efficacious tolerable dose

Terazosin(NC) � Statistically significant decreases from baseline obstructive, irritative, and total � � � symptom scores were observed for all terazosin treatment groups. The level of improvements in the symptom scores were dose dependent. A statistically significant improvement from baseline was seen in the peak and mean urinary flow rates for all the treatment groups. The effect of terazosin on PFR was also dose dependent. Although a higher incidence of asthenia, flu syndrome, and dizziness were observed in the terazosin treatment groups, the differences from placebo were not statistically significant. There was a significantly greater incidence of postural hypotension in the 5 -mg terazosin group than in the placebo group. normotensive patients, small, clinically insignificant decreases in blood pressure Untreated hypertensive men had larger and clinically significant decreases in blood pressure. In medically controlled hypertension, terazosin had no clinically significant effect on blood pressure in men with poorly controlled medically treated hypertension, terazosin significantly lowered blood pressure.
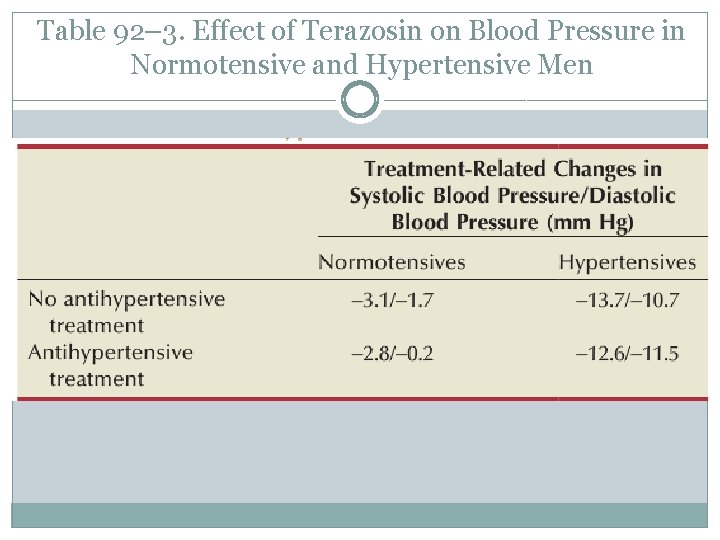

Table 92– 3. Effect of Terazosin on Blood Pressure in Normotensive and Hypertensive Men
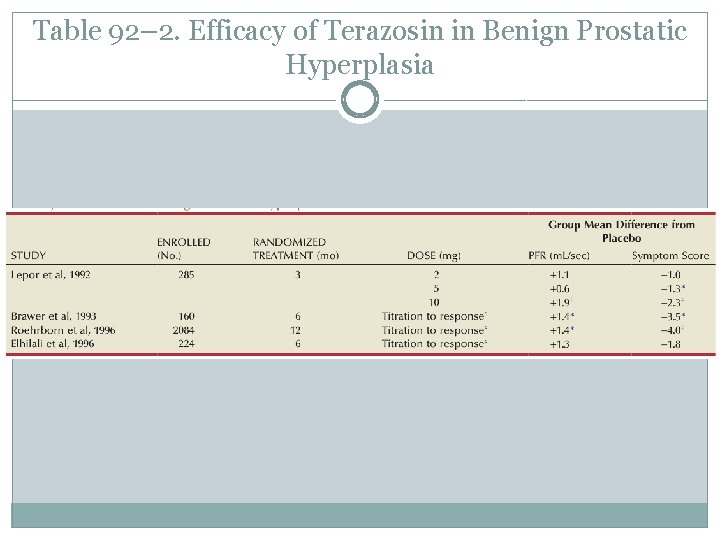
Table 92– 2. Efficacy of Terazosin in Benign Prostatic Hyperplasia
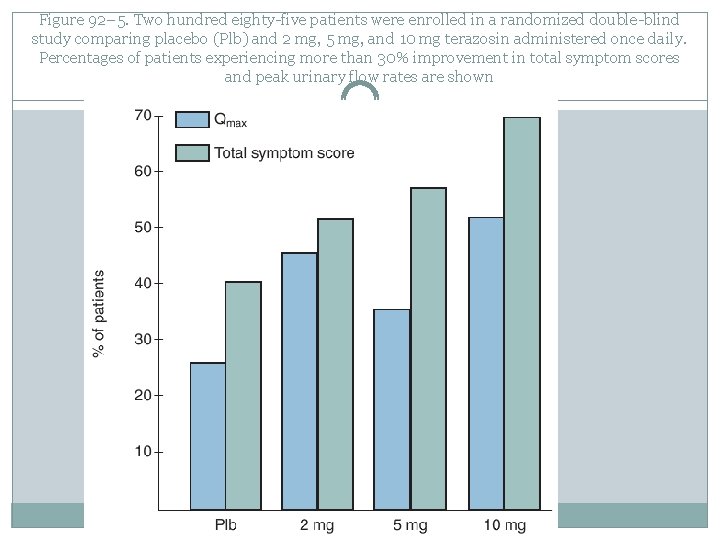
Figure 92– 5. Two hundred eighty-five patients were enrolled in a randomized double-blind study comparing placebo (Plb) and 2 mg, 5 mg, and 10 mg terazosin administered once daily. Percentages of patients experiencing more than 30% improvement in total symptom scores and peak urinary flow rates are shown

Doxazosin (NC) �The half-life of doxazosin is longer than that of terazosin (22 vs. 12 hours) �Statistically significant changes in symptom scores and PFR relative to baseline have been reported �The incidence of adverse effects was slightly higher with doxazosin standard than doxazosin GITS and placebo, which caused a similar incidence �The reduction in blood pressure was similar to terazocin �A comparison of terazosin and doxazosin shows similar efficacy. � Studies of doxazosin versus tamsulosin and doxazosin versus alfuzosin revealed only minor differences in safety and efficacy.

Doxazosin (NC) �In primary cultures of human prostate stroma cells, doxazosin increased apoptosis and decreased cell numbers. It was suggested that the effect of doxazosin may be mediated through TGF-β 1 �Doxazosin may have a mildly beneficial impact on sexual function. The mechanism for this effect is uncertain but may be the result of a vasodilatory action �α-Adrenergic blockers such as doxazosin may influence smooth muscle growth in the prostate. In BPH patients treated with α 1 -adrenoceptor antagonists there is a decreased expression of myosin heavy chain messenger RNA, a functional marker for the smooth muscle phenotype
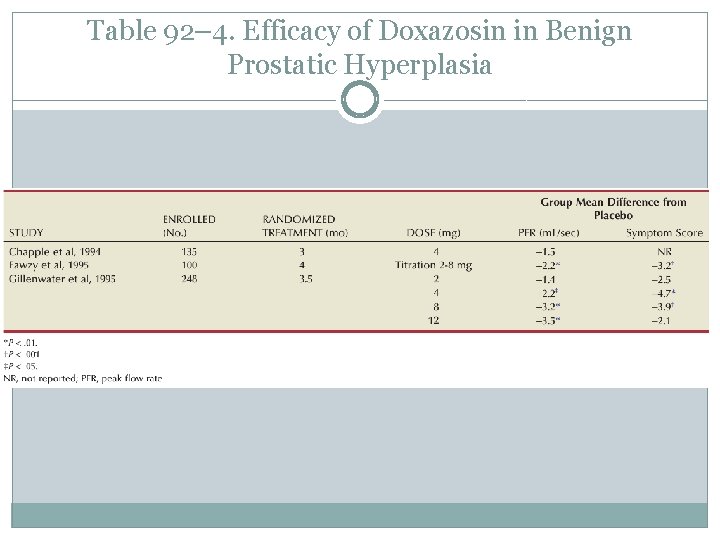
Table 92– 4. Efficacy of Doxazosin in Benign Prostatic Hyperplasia

Tamsulosin(NC) � The mean changes in systolic and diastolic blood pressure in the placebo and tamsulosin groups were not significantly different for both hypertensive and normotensive subjects. � The symptom and flow rate improvements observed at the end of the 13 -week study were maintained throughout the 40 -week extension study. � The treatment-related incidences of asthenia, dizziness, rhinitis, and abnormal ejaculation observed for the 0. 4 -mg tamsulosin group were 2%, 5%, 3%, and 11%, respectively; and for the 0. 8 -mg tamsulosin group they were 3%, 8%, 9%, and 18%, respectively. � The incidences of retrograde ejaculation and rhinitis were significantly greater in the 0. 8 -mg group compared with the 0. 4 -mg group. � No statistically or clinically significant differences were observed for systolic blood pressure between any of the treatment groups.
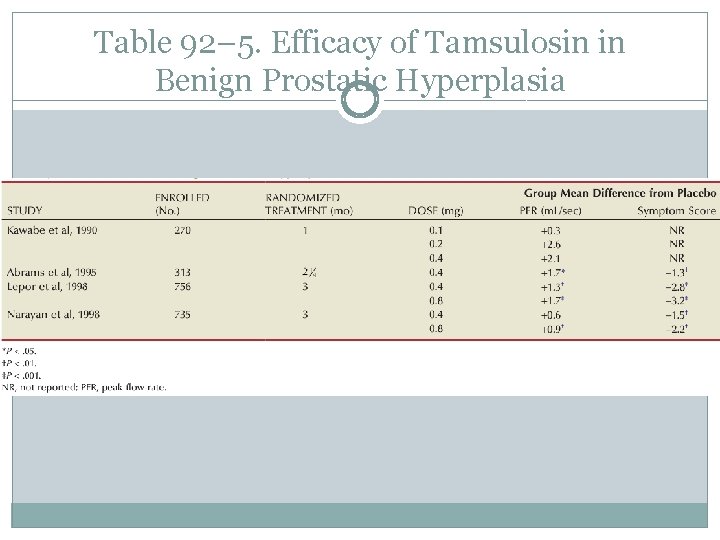
Table 92– 5. Efficacy of Tamsulosin in Benign Prostatic Hyperplasia

Alfuzosin(NC) �Effectiveness of alfuzosin was durable up to 30 months �The incidences of dizziness and asthenia were similar in the SR alfuzosin and placebo groups. �The modest improvements in the PFR were significantly greater in both active treatment groups(the alfuzosin 10 mg/day, alfuzosin 2. 5 -mg three times a day) compared with placebo �There were no statistically or clinically significant treatment-related effects on blood pressure in normotensive or hypertensive subjects(like Tamsulocin)

Alfuzosin(NC)(2) �Because of the lack of adverse effects and blood pressure changes, alfuzosin has been described as a uroselective drug, but Andersson found that SR alfuzosin exhibits no pharmacologic uroselectivity for any of the α 1 subtypes �an explanation for the lack of adverse events has been the low penetration of alfuzosin into the brain. �It is also important to consider that the better tolerance may simply be related to a lower level of α 1 blockade because the treatment-related improvement of the 10 mg of alfuzosin appears to be less than that achieved with 10 mg of terazosin and 8 mg of doxazosin.
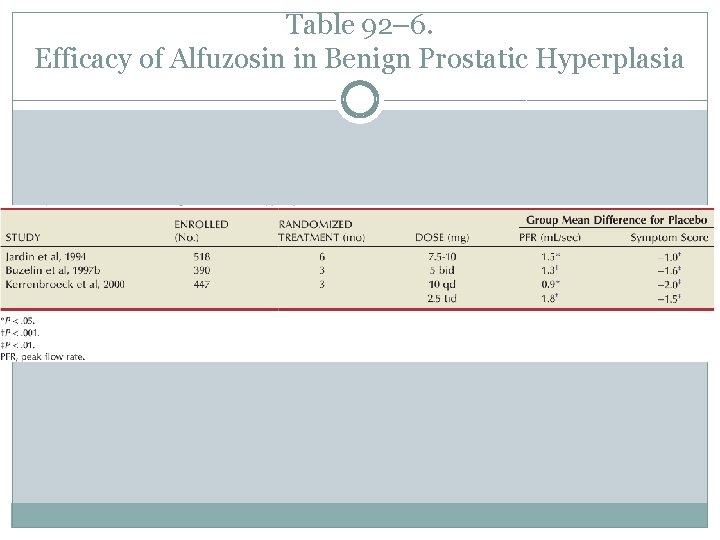
Table 92– 6. Efficacy of Alfuzosin in Benign Prostatic Hyperplasia

Silodosin(N) � In Japan, silodosin, a selective α 1 -adrenergic receptor antagonist, is the BPH market leader � Silodosin was shown to increase urine flow in 2 to 6 hours after the initial dose. Improvement of symptoms was realized in 3 to 4 days � It was associated with a low incidence of orthostatic hypotension and syncope, fainting, and dizziness. � Silodosin demonstrated minimal effects on the cardiovascular system, without any meaningful prolongation of the QT interval � The most common drug-related side effect was retrograde ejaculation , which occurred more often in the silodosin than in the tamsulosin group (22. 3% vs. 1. 6%) � The second most commonly adverse event was dizziness, the rate of which being only slightly higher than in placebo-treated patients. � There were no reported events of symptomatic orthostatic hypotension or dizziness when administered with a single dose of medications for erectile dysfunction (ED) in healthy male subjects

Silodosin(N) �silodosin showed a significant decrease in IPSS versus tamsulosin at 2 weeks �Silodosin showed a significant improvement in quality of life score versus placebo �Noguchi and colleagues (2008) showed that silodosin had the highest selectivity for the vas deferens (7. 5 -fold), followed by naftopidil (4. 3 -fold), alfuzosin (3. 8 -fold), tamsulosin (2. 6 -fold), and prazosin (2. 5 -fold)

Naftopidil(N) �Naftopidil, a relative selective α 1 D-adrenergic receptor antagonist, seems more effective for patients showing a dominant expression of the α 1 Dadrenergic receptor subtype �Whereas naftopidil monotherapy decreased the IPSS for storage symptoms, tamsulosin monotherapy decreased the IPSS for voiding symptoms

Effects of α-Adrenergic Blockers on Bladder Outlet Obstruction �A drug that improves urodynamic parameters of BOO without relieving LUTS would be of limited clinical utility. Conversely, a drug that relieves LUTS without improving urodynamic parameters of BOO would be of great clinical importance. �Martorana and colleagues (1997) reported a randomized, double-blind, placebo-controlled study examining the effect of 1 month of alfuzosin, 2. 5 mg three times a day, on pressure-flow urodynamic parameters. The changes in Pdet at maximum flow, detrusor opening pressure, and maximum Pdet were significantly greater in the alfuzosin -treatment group compared with the placebo group. There were no significant differences between the effects of alfuzosin and those of placebo on PFR.

α-Adrenergic Blockers and Sexual Function and Sexual Side Effects (N) �Erectile and ejaculatory functions are frequently reduced in patients with LUTS/BPH and can impact on their quality of life. Therefore the treatment of BPH should aim to maintain or even restore sexual function. � α 1 -Adrenergic receptor antagonists lack major effects on sexual desire. Reports on erectile function are inconsistent, with both beneficial and adverse effects being reported, but ED can occur in some patients without clear differences between drugs. � Ejaculatory dysfunction occurs more frequently with tamsulosin and even more so for silodosin

α-Adrenergic Blockers in the Elderly (C) � The adverse events associated with α-adrenergic blockers that may be particularly problematic in the elderly are dizziness and orthostatic hypertension � the incidences of adverse events are not age dependent. � Data from population studies such as the 5872 participants in the Osteoporotic Fractures in Men study and a populationbased case-control study using data from a managed care organization in southern California with more than 3 million members suggest that moderate and severe LUTS independently increase the 1 -year risk of falls, particularly recurrent falls, in community-dwelling older men (Parsons et al, 2009) and that there was a modest increase in risk associated with exposure to α -adrenergic blockers that requires further investigation (Jacobsen et al, 2008).

α-Adrenergic Blocker Therapy and Coexisting Hypertension(NC) � The α-adrenergic blockers terazosin and doxazosin are established agents for the treatment of hypertension. � terazosin and doxazosin lower blood pressure primarily in hypertensive men and that the blood pressure lowering is clinically significant � Approximately 30% of men treated for BPH have coexisting hypertension � The ALLHAT study questions the role of doxazosin as firstline therapy for the treatment of hypertension. The study does not assess the relative risks and benefits of doxazosin in men with BPH and hypertension, nor does it have any bearing on the use of doxazosin in combination with other antihypertensive agents. � Doxazosin remains an acceptable agent to treat BPH that coexists with hypertension.

Mechanism of Adverse Events Associated with αAdrenergic Blockade(NC) �Dizziness and asthenia are most common. �It has been assumed that dizziness and possibly asthenia were caused by cardiovascular effects � Men experiencing dizziness and asthenia did not exhibit greater changes in blood pressure while on terazosin therapy. Only postural hypotension was associated with greater changes in blood pressure. � α 1 -Adrenergic-mediated dizziness and asthenia are likely due to effects at the level of the CNS

α-Adrenergic Blockers and Intraoperative Floppy Iris Syndrome(N) � poor preoperative pupil dilation, iris billowing and prolapse, and progressive � � � � intraoperative miosis its association with the α 1 -adrenergic antagonist tamsulosin has become well established. It appears that α 1 A is the predominant receptor subtype in the iris dilator muscle as well. The persistence of IFIS long after the discontinuation of tamsulosin suggests a semipermanent muscular atrophy and loss of tone. It is not clear how long one must take tamsulosin before experiencing these chronic muscular changes. Anecdotal reports suggest that IFIS does not occur until patients have been on tamsulosin therapy for 4 to 6 months. IFIS can also occur up to several years after discontinuation of tamsulosin. IFIS has also been reported but less commonly with non–subtype-specific α 1 adrenergic antagonists, such as terazosin, doxazosin, and alfuzosin Prevention of IFIS by withdrawing tamsulosin preoperatively has not shown consistent benefit Patients should also be encouraged to report any prior or current history of α 1 antagonist use to their ophthalmic surgeon before undergoing any eye surgery.

Comparison of α-Adrenergic Blockers � therapeutic effect and adverse events associated with α- blockers are both dose dependent � Buzelin and coworkers (1997 a) compared IR alfuzosin, 2. 5 mg three times a day, vs. tamsulosin, 0. 4 mg/day. The improvements in Boyarsky symptom score and PFR and the incidences of dizziness and asthenia were not significantly different between the two treatment groups. The effects of alfuzosin and tamsulosin on systolic and diastolic supine or standing blood pressures in the hypertensive patients were also not significantly different. This study suggests that IR alfuzosin and tamsulosin have equivalent effectiveness and tolerability. � The obvious benefit of tamsulosin is that the dose does not have to be titrated � The recommended daily doses of terazosin, doxazosin, tamsulosin, and SR alfuzosin are 10 mg, 8 mg, 0. 4 mg, and 10 mg, respectively.

Comparison of α-Adrenergic Blockers �The clinical data suggest that terazosin, 10 mg, and doxazosin, 8 mg, are more effective than tamsulosin, 0. 4 mg, and alfuzosin, 10 mg (see Tables 92– 2 and 92– 4 to 92– 6). �The incidences of asthenia and dizziness appear to be higher for terazosin and doxazosin. �The apparent better tolerability of tamsulosin and SR alfuzosin may simply be because of degree of α 1 blockade and not uroselectivity

Comparison of α-Adrenergic Blockers �Terazosin and doxazosin exhibit very similar pharmacologic and pharmacokinetic properties. The effectiveness of terazosin and doxazosin are both dose dependent � Although the incidence of adverse events is dose dependent, the 10 -mg and 8 -mg doses of terazosin and doxazosin are generally well tolerated �There is no significant cost advantage between 10 mg of terazosin and 8 mg of doxazosin. � 10 mg of terazosin and 8 mg of doxazosin should be considered equivalent(effect&tolerability)

Comparison of α-Adrenergic Blockers � 0. 8 -mg tamsulosin dose appears to have less asthenia than terazosin and doxazosin, the incidence of dizziness is comparable and rhinitis and abnormal ejaculation are markedly greater. �The most appropriate dose of tamsulosin is 0. 4 mg, owing to the cost and adverse events associated with the 0. 8 -mg dosage. �For men presenting in urinary retention, tamsulosin and SR alfuzosin will likely decrease the time to voiding trial. �The data suggest that tamsulosin and SR alfuzosin exhibit less effect on blood pressure in hypertensive men compared with terazosin and doxazosin.

Summary �Long-term open-label studies have demonstrated that the clinical response to α-blockers is dose dependent, durable. �The long-acting α 1 blockers are well tolerated. The blockers are safe in the elderly, diminish BOO, and reduce the risk of urinary retention. �Their effect on falling needs further research. �Terazosin and doxazosin significantly lower blood pressure only in hypertensive subjects, allowing treatment of coexisting BPH and hypertension. � Direct comparison studies of the α-adrenergic blockers are sparse and involve small numbers of patients; therefore any claims of superiority cannot be justified.

Androgen Manipulation(Rationale) � The rationale for androgen suppression is based on the observation that the embryonic development of the prostate is dependent on the DHT � The genetic deficiency of 5α-reductase in men results in a rudimentary prostate and in feminized external genitalia � The primary limitation of the androgen suppression hypothesis is that the pathophysiology of clinical BPH and LUTS are not sufficiently dependent on prostate size. � Cyproterone acetate, an antiandrogen, was reported to decrease symptoms and increase PFR in the majority of treated subjects � Maximal reduction of prostate volume after initiation of androgen suppression is achieved within 6 months
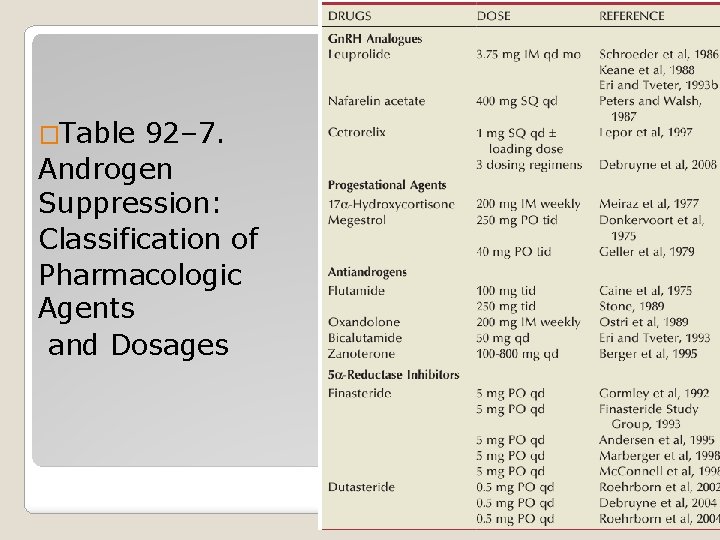
�Table 92– 7. Androgen Suppression: Classification of Pharmacologic Agents and Dosages

Review of the Literature � 1 - Finasteride is a competitive inhibitor of the enzyme 5α-reductase � Finasteride lowers serum and intraprostatic DHT levels. At least two isozymes (types 1 and 2) of 5α-reductase exist. Finasteride is a selective inhibitor of the type 2 isozyme. � Finasteride does not reduce DHT levels to castrate levels because circulating testosterone is converted to DHT by type 1 isozymes that exist in skin and liver � The group mean percentage changes in symptom score at 12 months in the placebo and 1 - and 5 -mg finasteride groups were − 2%, 9%, and 21%, respectively. � The mean percentage changes in PFR were 8%, 23%, and 22% in the placebo and 1 - and 5 -mg finasteride groups, respectively. � The mean percentage changes in prostate volume were − 3%, − 18%, and − 19% in the placebo and 1 - and 5 -mg finasteride groups, respectively

Finasteride �The dose-dependent symptom response was not associated with a dose-dependent prostate volume or PFR response. �The incidences of decreased libido, ejaculatory disorder, and impotence were significantly greater in the finasteride groups compared with the placebo group. �Prostate volume regression was maximal at 6 months. � The greatest change in symptom scores and PFR occurred within the first 2 months of initiating active treatment

Finasteride �The detection of prostate cancer was not significantly different in the placebo and finasteride group, suggesting that finasteride does not mask the diagnosis of prostate cancer �Finasteride reduces group mean serum PSA levels approximately 50% �The Prostate Cancer Prevention Trial (PCPT) (Thompson et al, 2003) showed that finasteride reduced the incidence of diagnosed prostate cancer (vs. placebo). There was an increased incidence of high-grade disease, probably owing to technical pathologic reasons �Finasteride was very effective in relieving the postprostatectomy-associated gross hematuria
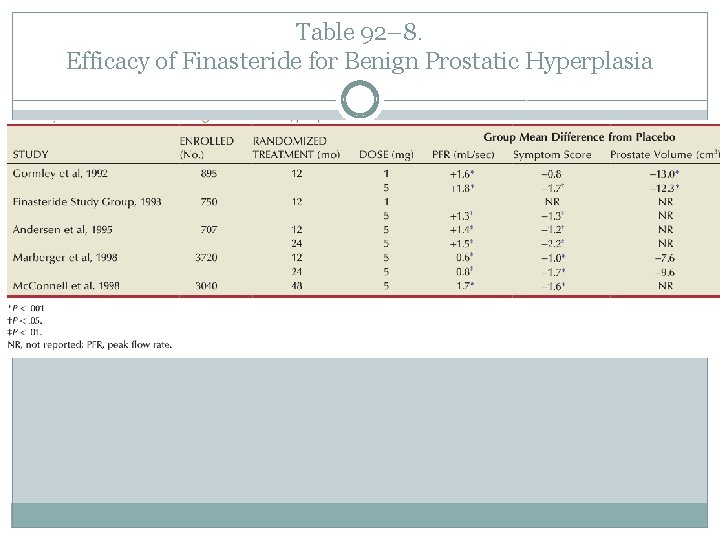
Table 92– 8. Efficacy of Finasteride for Benign Prostatic Hyperplasia

Dutasteride(C) � Dutasteride is a dual inhibitor of 5α- reductase types 1 and 2 and therefore has a greater impact on suppressing serum DHT levels � Similar to finasteride, the principal side effects were loss of libido and ED, but these were most frequently seen at the start of therapy and declined over time with treatment � Recently, the results of the REDUCE study of dutasteride versus placebo in terms of their ability to prevent prostate cancer have been reported by Andriole and associates (2009). A 23% reduction in prostate cancer was seen in the dutasteride study arm, with no increase in less welldifferentiated cancers in the dutasteride arm. Beneficial effects on symptoms, PFR, and risk of progression were also seen in this group of men at high risk for BPH progression as well as for a prostate cancer diagnosis. Further re-analysis has suggested some risk of high-grade cancers, and in December 2010 the FDA Oncologic Drugs Advisory Committee voted against use of dutasteride for reduction in the risk of prostate cancer. The manufacturer has withdrawn this application.

Zanoterone �the differences between placebo and all of the zanoterone groups were not statistically significant. �Fifty-six percent and 22% of all zanoterone subjects reported breast pain and gynecomastia, respectively. � The incidence and severity of adverse clinical events and the equivocal efficacy precluded further development of this drug for BPH.

Flutamide �. Flutamide is an orally administered nonsteroidal antiandrogen that inhibits the binding of androgen to its receptor �Statistically significant differences were not observed between placebo and 300 mg of flutamide for symptoms, prostate size, PVR, and PFR �The incidences of breast tenderness and diarrhea in the flutamide group were 53% and 11%, respectively.

Cetrorelix(C) � Cetrorelix is a gonadotropin-releasing hormone antagonist � Maximal lowering of testosterone was observed within 24 hours. � three dosing regimens were explored: one or two injections weekly for 4 weeks. In all groups a rapid improvement in mean IPSS was obtained, with a peak effect of − 5. 4 to − 5. 9 (placebo: − 2. 8). Changes from baseline and differences to placebo were statistically significant up to week 20. Placebo response was less sustained than usually seen with oral preparations. � The primary disadvantage of cetrorelix and other gonadotropin-releasing hormone antagonists will be the requirement for an injection and the cost. � If single-injection therapy provides desirable clinical response (over, for example, 6 months) with minimal adverse events there may exist a role for these antagonists in the treatment of BPH.

Aromatase Inhibitors � The rationale for aromatase inhibition is that estrogens may be involved in the pathogenesis of BPH. � Estrogens greatly enhanced the ability of androgens to induce BPH in a canine model. This synergistic effect may be mediated by the ability of estrogens to upregulate prostatic androgen receptor content. � Atamestane resulted in a statistically significant decrease in serum estradiol and estrone levels and a statistically significant increase in serum testosterone. � No statistically significant group mean differences were observed for changes in Boyarsky symptom score, PFR, or prostate volume between the atamestane and the placebo groups. � One of the explanations contributing to the failure of atamestane to achieve clinical efficacy was the increase in testosterone

Summary � 1 -Finasteride and dutasteride are the only drugs available that achieve androgen suppression with acceptable tolerability. � The literature also suggests finasteride and dutasteride may be offered to men with hematuria secondary to friable prostatic tissue and in those men with LUTS and enlarged prostates who elect to reduce their risk of developing urinary retention. � The overall treatment-related improvements in symptom score (approximately 1. 0 symptom unit) and PFR (approximately 1. 5 m. L/sec) by finasteriderelative to placebo are modest. � The adverse clinical events associated with finasteride are minimal and are related primarily to sexual function

Summary � 2 -Dutasteride is an inhibitor of both type 1 and type 2 5α-reductase and has similar efficacy and side effects to finasteride. � Finasteride and dutasteride alter the natural history of urinary retention in men with LUTS and enlarged prostates. � In the recently reported REDUCE study, dutasteride reduced the incidence of prostate cancer by 23%. � 3 - The equivocal efficacy and problematic toxicity of antiandrogens limited the enthusiasm for marketing these drugs for the treatment of BPH. � 4 - The role of gonadotropin-releasing hormone antagonists requires further study.

Combination Therapy with α-Adrenergic Blockers and 5α-Reductase Inhibitors �There is no more effect for combination therapy than a-blocker monotherapy, except reducing prostate size(only in MTOPS, was effective) �Finasteride monotherapy (like combination therapy)
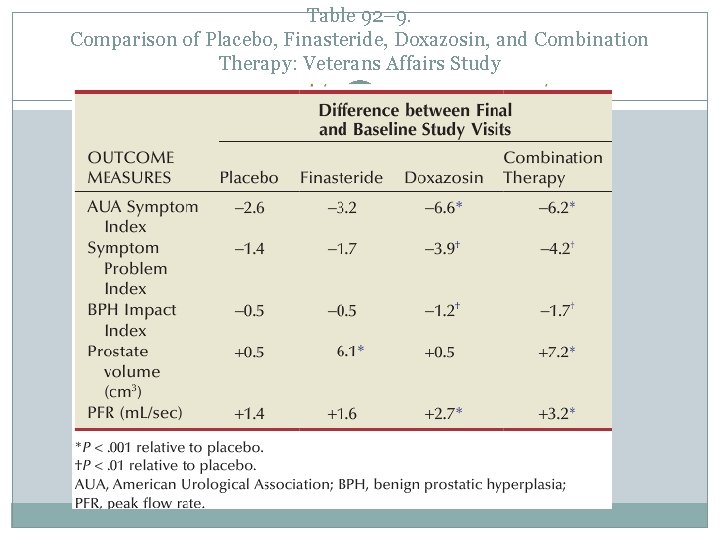
Table 92– 9. Comparison of Placebo, Finasteride, Doxazosin, and Combination Therapy: Veterans Affairs Study
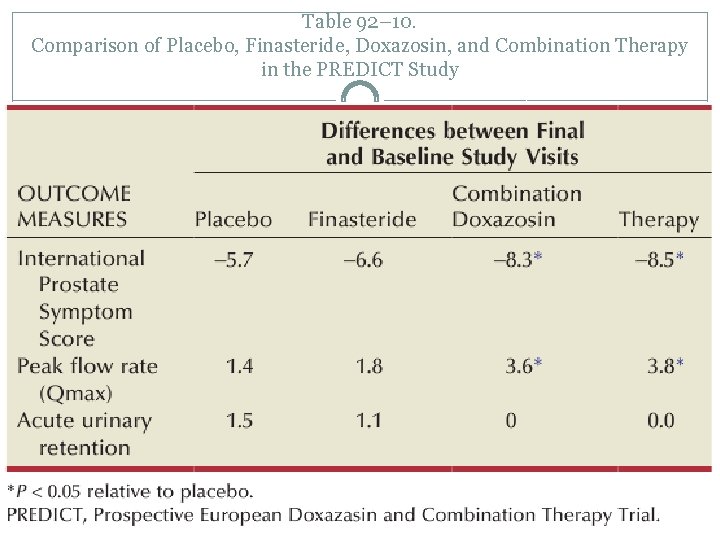
Table 92– 10. Comparison of Placebo, Finasteride, Doxazosin, and Combination Therapy in the PREDICT Study

Medical Therapy of Prostatic Symptoms (MTOPS) Trial � the role of 5α-reductase inhibitors as generalized monotherapy for LUTS may be somewhat limited � combination of doxazosin and finasteride exerts a clinically relevant, positive effect on rates of disease progression. Men who received combination therapy were significantly less likely to experience BPH progression than those receiving either monotherapy or placebo, with risk reduction rates of 39% for doxazosin, 34% for finasteride, and 67% for combination therapy compared with placebo � AUASI score and PFR improved significantly more in the combination therapy group compared with the monotherapy groups � It was concluded that a 5α-reductase inhibitor can be used in combination with an α-adrenergic blocker to achieve rapid onset of symptom relief in patients at risk of underlying disease progression and the α-adrenergic blocker can then be discontinued

Anticholinergic (Antimuscarinic) Receptor Blockers (N) �These results suggest that antimuscarinic agents could be safely administered in men with BOO. �The authors concluded that, although antimuscarinic therapy was safe, more studies were required to define the efficacy of this therapy for men with LUTS/BPH

Combination Therapy: α-Adrenergic Blockers and Anticholinergic (Antimuscarinic) Receptor Blockers �There is minimal available evidence on the long- term outcome of medical therapy of mixed OAB and BOO due to BPH. �The short-term data suggest that combination of antimuscarinic and α-adrenergic blocker therapy is safe with minimal risk of retention or AUR in carefully selected men �Men with significant obstruction and large, persistent residual urine volumes should be considered for surgical therapy rather than the addition of antimuscarinic agents

�Key Points: Antimuscarinic Therapy �l Short-term trial data suggest antimuscarinic agents can be safely given to carefully selected men with OAB/storage symptoms and BPH. �l The combination of antimuscarinic agents and αadrenergic blocker therapy may improve both storage and voiding symptoms. �l It is advisable to avoid treating men with large PVR urine volumes (≥ 200 m. L) with antimuscarinic agents. �l Men with significant obstruction and large persistent residual urine volumes should be considered for surgical therapy. �l Long-term data are not available

Phosphodiesterase Inhibitors(N) � The candidate mechanisms include the following: � 1. Pelvic atherosclerosis � 2. Autonomic hyperactivity � 3. The calcium-independent Rho-kinase activation pathway � 4. Reduced nitric oxide (NO) levels, which is probably the best explored process so far � there is now good level 1 evidence from (currently) four clinical trials clearly showing improvement of LUTS after treatment with PDEIs � The first randomized controlled trial published to elucidate the impact of PDEIs on LUTS was by Mc. Vary and coworkers (2007 a ) � There was no significant difference in PFR, which led the authors to suggest that possibly other mechanisms were involved than simply smooth muscle relaxation in the bladder and prostate.
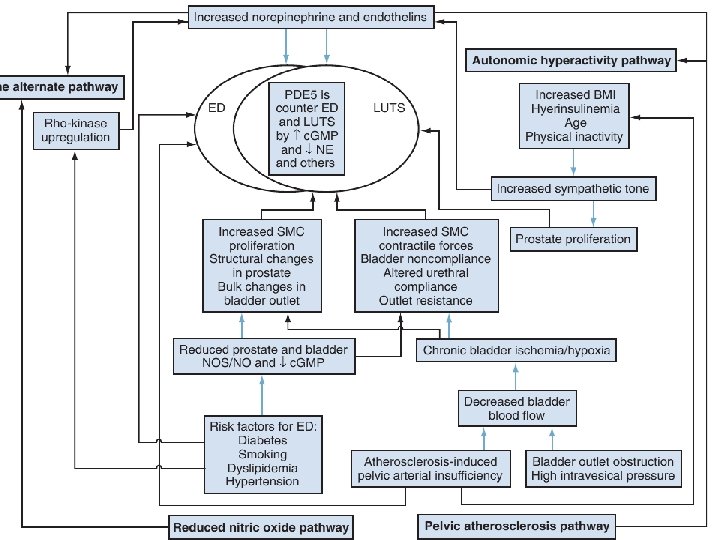
BMI, body mass index; c. GMP, cyclic guanosine monophosphate

Combination Therapy: α-Adrenergic Blockers and Phosphodiesterase Inhibitors �the concomitant use of α-adrenergic blockers and PDEIs may lead to symptomatic hypotension in some patients because both are vasodilators. �The coadministration of doxazosin (4 and 8 mg daily) and tadalafil (5 mg/day or 20 mg as a single dose intermittently) leads to further lowering of blood pressure, and this combination is not recommended by the manufacturers

�Key Points: PDEIs �l There is an as yet undetermined link between LUTS/BPH and ED. �l PDEIs improve urinary symptoms scores. �l PDEIs do not improve flow rates. �l The combination of α-adrenergic blockers and PDEIs may lead to a synergistic benefit, thereby improving LUTS. �l The combination of α-adrenergic blockers and PDEIs may lead to symptomatic hypotension. �l PDEIs or a combination of α-adrenergic blockers and PDEIs may be of value in therapy for men with both ED and LUTS

Phytotherapy �The pharmacologic use of phytotherapy for the treatment of LUTS associated with BPH is common �The composition of plant extracts is very complex �Although experimental data have suggested numerous possible mechanisms of actions for the phytotherapeutic agents it is uncertain which, if any, of these proposed mechanisms is responsible for the clinical responses.

Table 92– 14. Origin of Plant Extracts
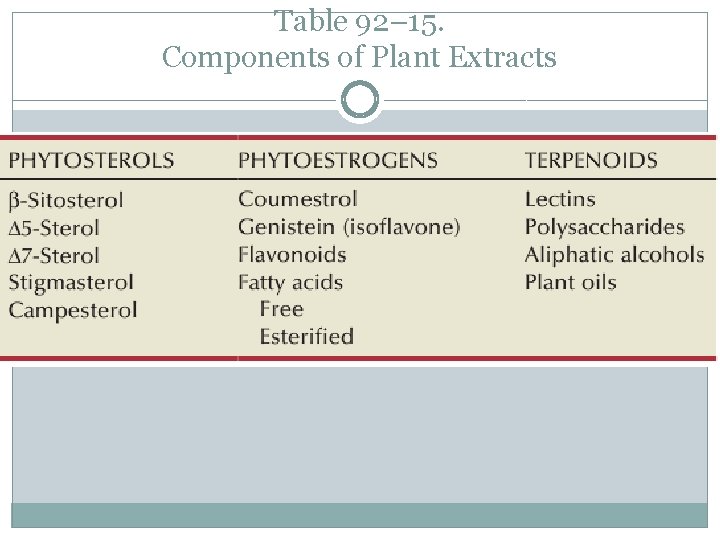
Table 92– 15. Components of Plant Extracts

Table 92– 16. Suggested Mechanisms of Action of Plant Extracts

Serenoa Repens (Saw Palmetto Berry)(C) � Serenoa Repens (Saw Palmetto Berry). The extract of the berry of the American saw palmetto, or dwarf palm plant, Serenoa repens (also known by its botanical name of Sabal serrulatum), is the most popular phytotherapeutic agent available for the treatment of BPH � Wilt and coworkers conducted a systematic review, first published in 1998 and updated in 2002 and again in 2009, to evaluate the efficacy and adverse events of S. repens (Tacklind et al, 2009). Initially their analysis was mildly supportive of the efficacy of S. repens. In this update 9 new trials involving 2053 additional men (a 64. 8% increase) were included. For the main comparison—S. repens versus placebo— 3 trials were added with 419 subjects and three end points (IPSS, peak urine flow, prostate size). Overall, 5222 subjects from 30 randomized trials lasting from 4 to 60 weeks were assessed. Twenty-six trials were double blinded, and treatment allocation concealment was adequate in 18 studies. With these extra data and especially the double-blind, placebo-controlled trial reported by Bent and associates (2006), they concluded that S. repens was not superior to placebo in improving IPSS or PFR or for reducing prostate size. For nocturia, S. repens was significantly better than placebo (weighted mean difference − 0. 78 nocturnal visits, 95% CI − 1. 34 to − 0. 22, P < 0. 05; 9 trials), but with the caveat of significant heterogeneity within studies. A sensitivity analysis, utilizing higher-quality, larger trials demonstrated no significant difference. S. repens was also not superior to finasteride or to tamsulosin. Overall, it was concluded that S. repens was not more effective than placebo for treatment of urinary symptoms consistent with BPH. � Therefore, whereas the efficacy of S. repens has not been completely determined, current meta-analysis suggests that S. repens is not more effective than placebo for treatment of urinary symptoms consistent with BPH.
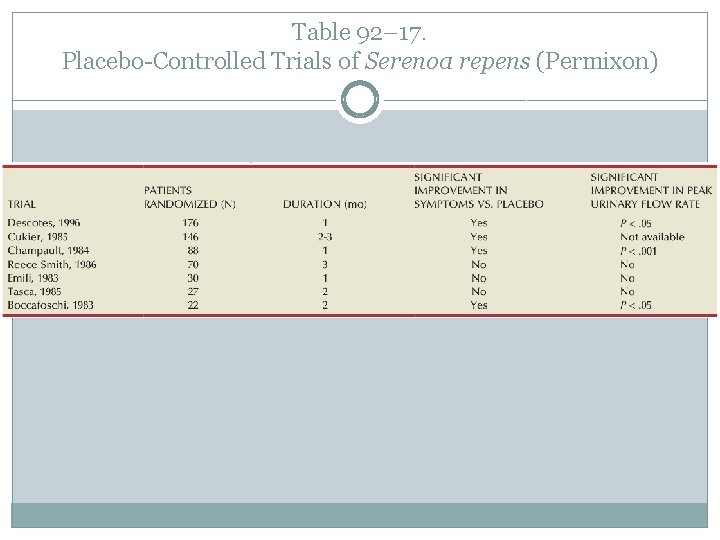
Table 92– 17. Placebo-Controlled Trials of Serenoa repens (Permixon)

Phytotherapy � Pygeum africanum (African Plum): Therefore the data concerning the efficacy of P. africanum are not conclusive. � Hypoxis rooperi (South African Star Grass): The IPSS improved by 7. 4 units for β-sitosterol patients and 2. 3 units for placebo. Similarly, peak urinary flow rates improved by 5. 2 m. L/sec for treated patients compared with 1. 1 m. L/sec for placebo. This magnitude of improvement has not been observed with any other medical therapy previously evaluated for BPH , IPSS scores improved by 8. 2 units for treated patients and 2. 8 units for placebo. PFRs improved by 8. 9 m. L/sec for treated patients and 4. 4 m. L/sec for placebo. This magnitude of improvement has not been reported for any type of medical therapy for BPH. It is hard to believe these results in which the mean post-treatment PFRs are 19. 4 m. L/sec, which is a normal value for younger men and not for the typical age of men in the study. If these results are reproducible, they would rival surgical intervention.

Other Extracts. Urtica dioica, Cucurbita pepo, Secale cereale, and Opuntia—have even fewer relevant clinical studies published than the aforementioned ones � More recently Zhang and coworkers (2008) have reported a randomized, double- blind, placebo-controlled clinical trial of a flaxseed lignan extract containing 33% secoisolariciresinol diglucoside (SDG). SDG was evaluated for its ability to alleviate LUTS in 87 subjects with BPH with repeated measurements conducted over a 4 month period using treatment dosages of 0 (placebo), 300, or 600 mg/day SDG. After 4 months of treatment, 78 of the 87 subjects completed the study. For the 0, 300, and 600 mg/day SDG groups, respectively, the IPSS decreased − 3. 67 ± 1. 56, − 7. 33 ± 1. 18, and − 6. 88 ± 1. 43 (mean ± SE, P =. 100, <. 001, and <. 001 compared with baseline), the quality of life score improved by − 0. 71 ± 0. 23, − 1. 48 ± 0. 24, and − 1. 75 ± 0. 25 (mean ± SE, P =. 163 and. 012 compared with placebo and P =. 103, <. 001, and <. 001 compared with baseline), and the number of subjects whose LUTS grade changed from “moderate to severe” to “mild” increased by 3, 6, and 10 (P =. 188, . 032, and. 012 compared with baseline). PFR insignificantly increased 0. 43 ± 1. 57, 1. 86 ± 1. 08, and 2. 7 ± 1. 93 m. L/sec (mean ± SE, no statistical significance reached), and postvoid urine volume decreased insignificantly by − 29. 4 ± 20. 46, − 19. 2 ± 16. 91, and − 55. 62 ± 36. 45 m. L (mean ± SE, no statistical significance reached). The observed decreases in IPSS and quality of life score were correlated with the concentrations of plasma total lignans. It was concluded that dietary flaxseed lignan extract appreciably improved LUTS in BPH subjects and that therapeutic efficacy appeared comparable to that of α 1 -adrenergic receptor blockers and 5α-reductase inhibitors.

Summary �Most phytotherapeutic preparations are plant extracts with different components, but it is uncertain which of the actions demonstrated in vitro might be responsible for clinical responses in vivo. � Appropriate randomized placebo-controlled clinical trials monitored by an outside agency are needed to ascertain and to confirm the efficacy of these products.

Acute Urinary Retention(N) � Analysis of the placebo arms of a series of large studies such as the PLESS evaluation of finasteride, MTOPS, and the Comb. AT study indicate that increasing age, the presence of LUTS, a low PFR, and prostatic enlargement and/or raised PSA increase the risk of AUR. � It is reasonable to speculate that urinary retention is caused in part by dynamic as opposed to static outflow obstruction because a significant proportion of men void spontaneously after catheter placement � Unfortunately, even those who succeed will have a high rate of subsequent failure to void and 80% of those who will experience this failure do so within 6 months � The trial data suggest a role for 5α-reductase drugs in the prevention of AUR.

FUTURE STRATEGIES � “neither finasteride nor α-blockers approach the efficacy of prostatic surgery in terms of improvement in either symptoms or flow rates…. ” � endothelin elicits a very potent contraction in the human prostate � Both endothelin-A and endothelin-B receptors are present in the human prostate. These receptors are localized primarily in the stroma and glandular epithelium, respectively. � Endothelin antagonists may emerge as another treatment for BPH. � Several observations suggest that nonprostatic factors may also contribute to clinical BPH � In addition, the changes in symptom scores after therapy for BPH are poorly correlated with changes in PFR and obstruction grade � Role of NO in prostatic smooth muscle has been deleted in this edition of Campbell.

- Slides: 87