Chapter 9 The Family After Birth Puerperium Known

Chapter 9 The Family After Birth

Puerperium • Known as postpartum period • Six weeks following childbirth – Sometimes referred to as the fourth trimester of pregnancy

Nursing Considerations for Specific Groups of Patients • Adolescents – Need help to learn parenting skills – Peer group is very important – fit in with peers – Passive in caring for themselves and infant – Single or poor – social problems • Single women – May lack a strong support system – May have to return to work sooner; sole provider • Families at or below the poverty level – Difficulties meeting basic needs before infant arrives – Less prenatal care, increases complications • Families who have twins (or more) – More likely to need NICU bc preterm birth, delays parental attachment – Difficult to see individuality of each infant, attached as a set

Cultural Influences • The nurse must adapt care to fit – Health beliefs – Values – Practices • Birth is a meaningful, emotional, social event • Use an interpreter where appropriate – Should not be a family member or in cultural/religious conflict with the patient/family – Affirmative nod from the woman may be a sign of courtesy to the nurse rather than a sign of understanding or agreement • Dietary practices: “hot” and “cold” theory – not temp

Postpartum Changes in the Mother • Occur because there is a fall in the blood levels of: – – – Placental hormones Human placental lactogen Human chorionic gonadotropin Estrogen Progesterone • Most dramatic changes occur in the womans reproductive system

Reproductive System • Uterus – Involution • Changes that the reproductive organs undergo after birth to return to their preregnancy size and condition • Uterus should return to pre-preg size by 5 -6 weeks after delivery • Failure to return to pre-preg size is subinvolution – Uterine lining • Shed when the placenta detaches • Placental site is fully healed in 6 -7 weeks – Descent of uterine fundus • Descends as muscle cells contract to control bleeding • Immediately after placenta is expelled, the uterine fudus can be felt midline, at or below the level of the umbilicus, as a firm mass – Afterpains • Intermittent uterine contractions - Similar to menstral cramps • Diminishes within 48 hr after birth • Occurs more often in multipara women bc uterus is overly distended • Breastfeeding mothers have more afterpains because suckling causes release of oxytocin

Reproductive System • Lochia – vaginal discharge after delivery • Composed of endometrial tissue, blood, and lymph – Rubra: red – mostly blood – lasts 3 days postpartum – Serosa: pink – blood and mucus – 3 rd day to 10 th day – Alba: clear, colorless, white – mostly mucus – 10 th day to 21 st day • # of pads are counted in the hospital • Fundus should be checked if bleeding is excessive • Check uterus firmness, uncontracted allows blood to flow freely from vessels at the placenta insertion site • NI: teach women to report any foul smell, bright red bleeding after 3 days, lochia that returns to bright red after it had been serosa or alba

More about Lochia • Flow may be briefly heavier when ambulating – A few small clots may be seen • Flow may increase when breastfeeding – Breastfeeding releases oxytocin which contracts the uterus – causes ^ afterpains • Women who had cesarean birth have less lochia in first 24 hours – Because uterine cavity was sponged at delivery • The absence of lochia is abnormal – May be associated with blood clots or infection

Reproductive System • Cervix – Regains muscle tone but never closes as tightly as during prepregnancy state – Some edema persists for weeks after delivery – Constant trickle of bright red blood is associated with bleeding from laceration of the cervix or vagina (fundus remains firm) • Vagina – Regains most of prepregnancy form within 6 weeks – Stress importance of discussing when to resume vaginal intercourse postpartum with HCP – Teach that it is OK to resume intercourse when bleeding stops and episiotomy healed. May need lubrication. Teach Kegel exercises. Don’t forget contraception!

Reproductive System • Breasts – By 3 rd day after birth, milk production begun – Engorgement – hard, erect, uncomfortable • Nonnursing mothers return to normal size in 1 to 2 weeks – Nursing Care • Support bra (nonnursing mothers elastic binder to suppress lactation and avoid nipple stimulation)
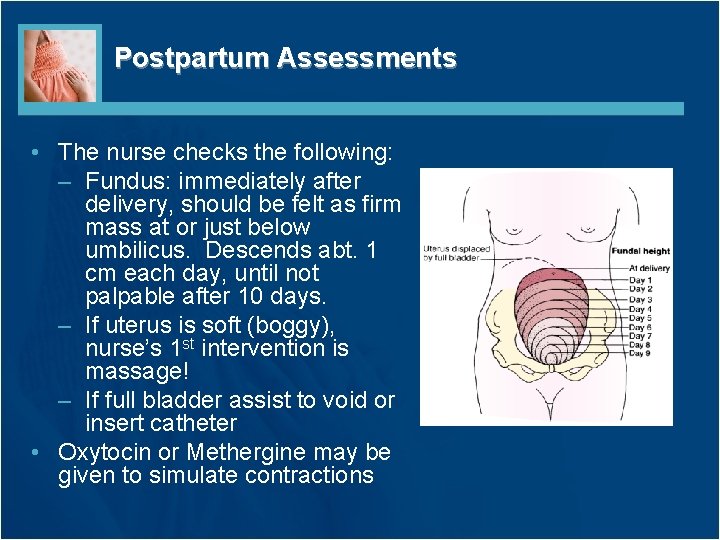
Postpartum Assessments • The nurse checks the following: – Fundus: immediately after delivery, should be felt as firm mass at or just below umbilicus. Descends abt. 1 cm each day, until not palpable after 10 days. – If uterus is soft (boggy), nurse’s 1 st intervention is massage! – If full bladder assist to void or insert catheter • Oxytocin or Methergine may be given to simulate contractions
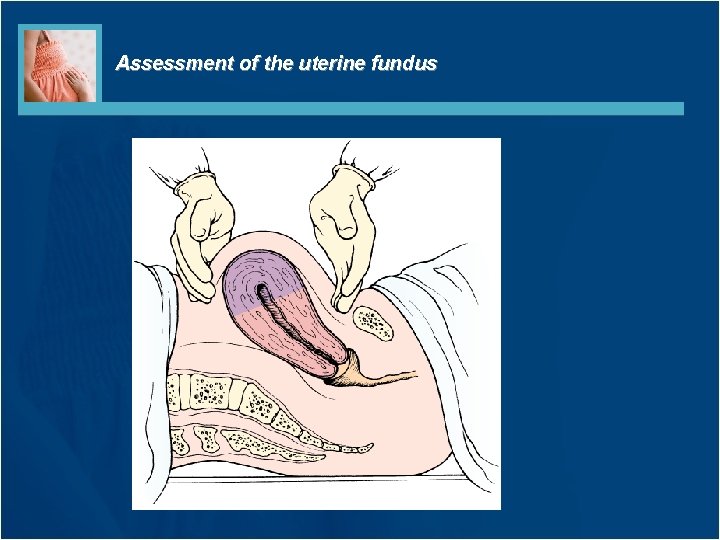
Assessment of the uterine fundus

Reproductive System (cont. ) • Perineum – Episiotomy • REEDA assessment – Nursing care and patient teaching • Cold packs • Sitz baths • Perineal care • Topical and systemic medications • Nonpharmacological pain relief methods • Return of ovulation and menstruation – Menstrual cycle typically resumes in 6 -8 weeks if not breastfeeding – Return of ovulation is delayed if breastfeeding; however, it can occur at any time after birth (pregnancy is possible)

Nursing assessments – Perineum: REEDA • Redness – normal healing or not? • Edema – mild is common • Ecchymosis – a few small bruises OK • Discharge – none from perineal suture line • Approximation – suture line should not be separated • Nursing Interventions: • ice pack to perineum first 12 to 24 hrs • teach woman to do perineal care after voiding or BM, using peribottle in a front-to-back direction • sitz baths • Perineal pads are applied in front to back direction to avoid fecal contamination

Postpartum Changes - Cardio • Blood volume increases 50 % during pregnancy – Normal blood loss at delivery • 500 ml for vaginal and 1000 ml for cesarean • To reestablish normal fluid balance the body rids itself of excess fluid by • Diuresis – increased urine output • Diaphoresis – increased perspiration • Coagulation – clotting factors higher during preg – Prone to clot formation – Dyspnea & tachypnea are classic s/s pulmonary embolism
Postpartum - Cardiovascular • Blood values – Values more accurate at 8 weeks postpartum – WBC count may increase • Response to inflammation, pain, stress • Returns to normal by 12 days postpartum • Chills – – Vasomotor response immediately after birth Stop spontaneously within 20 min after birth If with fever after 24 hrs, s/s infection. Provide warm blanket for comfort • Orthostatic hypotension – d/t resistance to blood flow in the vessels of the pelvis after birth

Postpartum Changes - Urinary • Kidney function returns to normal within a month after birth • May have urinary retention – Can lead to postpartum hemorrhage – UTI d/t stasis of urine in the bladder – Nursing Interventions – Assess for distention – I & O after cath out – Some discomfort expected r/t edema, but continued discomfort abnormal, suggests UTI

Postpartum changes - GI • Gastrointestinal system back to normal soon after birth • Constipation common r/t: – – Meds that slow peristalsis Hard to bear down to expel stool Soreness and swelling of the perineum Slight dehydration & small intake during labor – Nursing Interventions – – Provide food and water to new mother often Increase fiber intake Ambulate Stool Softeners as needed

Postpartum Changes – Skin • Chloasma & linea nigra disappear – Chloasma, hyperpigmentation of skin “mask of pregnancy” • Striae fade – Do not disappear but fade from reddish purple to silver

Postpartum Changes – Musculoskeletal • Abdominal wall weakness may remain for 6 – 8 wks – contributes to constipation • Diastasis recti – Abd muscles that extend from chest to symphysis pubis are separated • Hypermobility of the joints – Increased shoe size due to separation of joints • Exercises – can begin lightly 1 st day after birth in vag del. – Abdominal muscle tightening – Head lift – Pelvic tilt – Kegel exercises

Rh Immune Globulin & Rubella • Rh Immune Globulin – Given to an Rh-negative mother within 72 hours after birth of an Rh-positive infant – Prevents sensitization to Rh-positive erythrocytes that may have entered the mother’s bloodstream when infant was born – IM injection into deltoid muscle • Rubella Vaccine – The mother who is not immune will be given vaccine in immediate postpartum period – Given subcutaneously in upper arm – Vaccine is not given if sensitivity to neomycin – Women should not get pregnant for the next 3 months – Vaccinated women may breastfeed without adverse effect on the newborn

After Cesarean Birth – N. I. • Woman gave birth and had surgery • Reaction depends on expectation • Check fundus – if vertical incision, walk fingers from side to midline • Lochia generally less immediately after birth bc surgical sponges remove the contents of uterus • Check abd. dressing for drainage, s/s infection, staples; REEDA • Remove foley usually within 24 hrs. • Assess lung sounds Q shift; TCDB; I. S. • Leg exercizes, early & frequent ambulation to reduce risk of thrombophlebitis • Pain control: reduces distress and facilitates movement

The New Family • Fathers, siblings, grandparents • Include fathers, be supportive & tactful § Toddlers may resent mom’s attention to baby § Preschoolers may hesitate to touch § Older siblings often enjoy and are curious

Mother • Rubin’s Psychological Changes of the Puerperium – Phase 1: Taking in – Phase 2: Taking hold – Phase 3: Letting go • Postpartum blues – Conflicting feelings of joy and emotional let down – Feelings are normal and temporary • Postpartum depression – Persistant mood of unhappiness – Not expected and should be reported to HCP • Fatigue – Lack opportunities to rest and adapt – Offer assistance so mother can rest

Father • Engrossment – Intense interest in their new child • Past relationships influence present greatly • Four phases of adjustment – Having expectations and personal intentions – Confronting reality and overcoming frustrations – Creating one’s own personal father role – Reaping rewards of fatherhood • Include father when giving instructions about infant care and handling • Remain tactful and supportive

Siblings & Grandparents • Siblings – Influence depends on age and developmental level – Toddlers may respond with regression and anger d/t lack of attention – Preschoolers are hesitant to touch or hold infant – Older children enjoy caring for infant and are very curious • Grandparents – Can be an issue of conflict – Make sure and be open/aware of what grandparents perceive their role to be

Grieving Parents • Therapeutic communication • Even healthy child may cause grief – different than expected • Regret, remorse, sorrow, questioning • If poor condition, baptism may be desired by parents • Stages of grief: disbelief, anger, guilt, depression, gradual resolution • Can be chronic grief with birth defect • Memory packet in case of death – Hair, footprints, ID band, photo, clothing, etc.

Parenthood • Can affect communication between partners • Division of responsibility can be source of conflict • Fatigue increases irritability • Concerned of increased economic responsibilities • Loss of freedom and decreased socializing may cause couple to feel loneliness

Family care plan • Similar to traditional care plan but “patient “ is entire family! • Helps the nurse to integrate knowledge of family structure, culture, and composition into a plan of care

Data Collection for the Family Care Plan • • • Demographic information Family composition Occupation Cultural group Religious/spiritual affiliation • Developmental tasks • Health concerns • Communication patterns • • Decision making Family values Socialization Coping patterns Housing Cognitive abilities Support system Response to care

Phase 2: Care of the Newborn • If infant has adequate cardio and heat-reg fx, usually remains undisturbed during bonding time • Within 1 hour after birth, nurse assesses temp, heart rate, respirations, complete physical and gest. age and gives any prophylactic meds

Phase 2: Nursing Care of the Newborn • Normal: 96. 8 -97. 7 skin or 97. 7 -98. 6 axillary • Infant has less efficient means of generating heat • Risk: Hypothermia – Hypoglycemia – uses glucose to generate heat – Resp. distress – higher metabolic rate consumes more oxygen beyond infants ability to supply it

Phase 2: Care of the Newborn • Supporting thermoregulation – Evaporation: liquids from the skin – dry quickly and thoroughly, cover head of infant – Conduction: direct skin contact with cold surface – pre-warm surfaces – Convection: loss of heat to the surrounding cooler air – keep away from drafts (windows and vents) – Radiation: near a cool surface but not in direct contact – keep away from cold surfaces, place crib away from cold walls, wrap blankets in layers

Phase 2: Care of the Newborn • Observing bowel and urinary function – Some newborns do not urinate for as long as 24 -48 hours – Infant must be voiding and passed meconium prior to discharge – Ensures patency of urinary and GI tracts

Phase 2: Care of the Newborn • ID bands are matched every time the infant is reunited with the parent • Identifying the infant – ID bands are primary means of id the infant & placed in the birthing room – Nurses check to ensure that all numbers are identical • Security measures – OB prox badges with photos – Keep infant away from door to the room

Phase 2 Nursing Care of the Newborn (cont. ) • Gestational age evaluation – – – Skin – transparent (preterm) or peeling (postterm) Vernix – covered (preterm) or just in creases or absent (postterm) Hair – covered with lanugo (preterm) or just patches (term) Ears – spring back when bent slowly (preterm) or quickly Breast tissue – none or minimal (preterm) to 5 mm or more (term) Genitalia • Males: scrotum smooth and small (preterm) or covered with rugae (term) • Females: labia equal size (preterm) or labia major cover minora (term) – Sole creases – anterior only (preterm) or full foot (term) • Observing for anomalies • Obtaining vital signs: 15 -30, hrly, every 4 -8 hrs • Weighing and measuring

Phase 2: Care of the Newborn • Umbilical cord care – Three vessels: 2 arteries and 1 vein “AVA” – Primary concern: infection – ETOH applications at each diaper change to promote drying of the cord – Diaper should be fastened low to allow air circulation to the cord – Report: redness, moist, foul smell – No tub baths until cord falls off (10 -14 days)

Hypoglycemia in the Newborn • A blood glucose below 40 mg/d. L in the term infant indicates hypoglycemia • Confirmed by venous blood sample – fed as soon as sample is obtained • Infants nursed or fed soon after birth to prevent any fall in blood glucose level • Signs and Symptoms • • • Jitteriness Poor muscle tone Respiratory difficulty Low temperature Poor suck High-pitched cry Lethargic Seizures Heel stick Avoid center of heel where bone, nerves, and blood vessels are near the surface

Screening Tests • Heel stick performed on day of discharge • Mandated by state – PKU (started on special formula to reduce disability and prevent severe mental retardation – – – Hypothyroidism Galactosemia (affects ability to metabolize sugar properly) Thalassemia Sickle cell disease Maple syrup urine disease (amino acid condition) Homocystinuria (amino acid/metabolism disorder)

Bonding & Attachment • Bonding – strong emotional tie that forms soon after birth – Actually bonding begins during pregnancy – Both partners should view, hold and touch infant as soon as possible after birth • Attachment – tie that occurs over time • For some, parental feeling don’t come naturally • NC: observe interaction with infant, facilitate parent-infant attachment

Recognizing Hunger in the Newborn • • Hand-to-mouth movements Mouth and tongue movement Sucking motions Rooting movements Clenched fists Kicking of legs Crying (a late sign)

Daily nursing care of newborn • Infant mostly stays in mother’s room • Ask mom about soiled and wet diapers • Assess baby’s skin for problems & teach as needed • Discuss how breastfeeding is going or amount of formula is being taken • Frequency, duration, and any difficulties • Observe infant for jaundice at each assessment • Teaching is so important! • Do encourage, don’t criticize!

Breastfeeding Teaching • Advantages of breastfeeding • Breast milk contains full range of nutrients • easily digested • doesn’t cause allergies • natural immunity • rarely constipated infants • promotes mouth development • Convenient • Economical • promotes uterine contraction • uses maternal fat stores • close mother-child contact • may decrease child respiratory disorders.

Breastfeeding Teaching • Disadvantages of • cannot consume breastfeeding alcohol or abuse • Most maternal drugs. meds enter breast milk • difficult for working moms • untreated TB, Hep B or C, or HIV can’t breastfeed • Cancer may worsen with lactation

Physiology of Lactation • HIV is only absolute contraindication to breastfeeding • Hep C contraindicated in presence of liver failure • Prolactin causes production of breast milk • Oxytocin causes let-down reflex – Infant suckling at breast stimulates release of oxytocin – Prolactin increases as milk is removed from breasts – Infrequent or too short feedings can reduce the amount of milk produced – Very little milk is sored between feeding – most is made as infant nurses

Phases of Milk Production • Foremilk – First milk infant obtains – Watery and quenches infant’s thirst • Hindmilk – Later milk with higher fat content – Satisfies hunger – Feedings that are too short do not allow the infant to obtain the hunger-satisfying hindmilk

Phases of Milk Production • Colostrum (first few days) – Secreted late in pregnancy & first few days after delivery – Yellowish fluid – Rich in protective antibodies but lower in calories – Has laxative effect – aids in passage of meconium • Transitional milk (7 to 10 days) – Fewer immunoglobulins, more lactose, fat, calories • Mature milk (14 days) – Bluish color

Teaching Mom to Breastfeed • • Wash hands first and nipples – no soap Sit comfortably Stroke baby’s cheek with nipple Baby’s mouth should cover entire areola Use last breast first next time (safety pin) Provide breathing space Break suction gently Burp halfway through and when finished

Positions for Breastfeeding Cradle Hold Side-Lying Position Football Hold
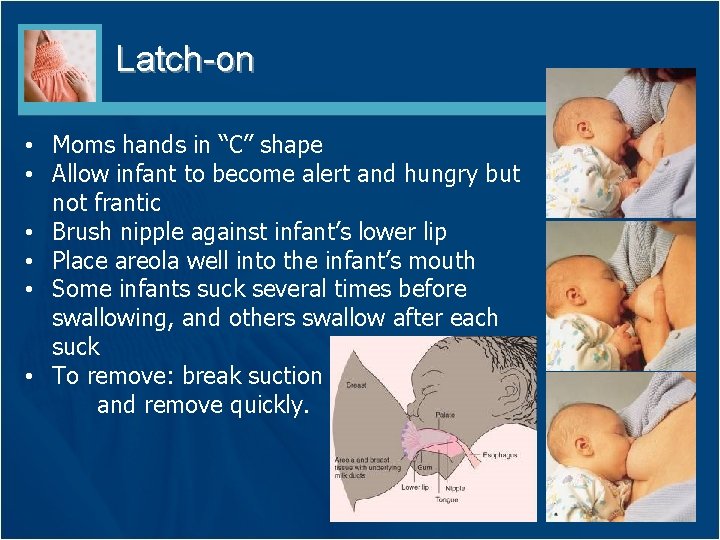
Latch-on • Moms hands in “C” shape • Allow infant to become alert and hungry but not frantic • Brush nipple against infant’s lower lip • Place areola well into the infant’s mouth • Some infants suck several times before swallowing, and others swallow after each suck • To remove: break suction and remove quickly.

Removing Infant From Breast

Evaluating Intake of Infant • Firm breasts before feeding and soft after • Let-down reflex occurs – A tingling sensation with milk dripping from nipple • Infant nurses for 15 minutes per breast 8 to 10 times per day • An audible swallow is heard • Infant appears relaxed after feeding • Infant has 6 -8 wet diapers per day • Infant passes several stools per day • NI: Provide reassurance that infant is receiving adequate milk intake bc milk is not seen by mother

Preventing problems • Nurse frequently in early weeks, Q 2 to 3 hours d/t small stomach capacity • Sleepy baby should be stimulated first • Fussy baby should be calmed first • Supplemental feeding of H 2 O or formula should not be given to breastfed newborn • Avoid engorgement by nursing frequently and regularly – can pump a little if needed • Don’t use ointments on sore nipples; use correct positioning and warm H 2 O compresses • No soap on breasts; wear supportive bra 24/7

Storing breast milk • Milk stored at room temp over 4 hours has increased potential for bacterial contamination • Use glass or hard plastic bottles • OK to freeze for up to 3 months – thaw in refrigerator is best to best preserve components • Store in refrigerator for 24 hours • No microwaving – Destroys immune factors – Hot spots due to uneven heating

Maternal Nutrition • Mother needs an additional 500 calories over the nonpregnant diet • 8 -10 glasses of fluids per day • Some foods eaten by mother may cause a change in the taste of the milk or cause the infant to develop gas (flatus) • Medications taken by the mother may be secreted in the breast milk • Continue Prenatal Vits and Ca supplements

Weaning • Gradual weaning is preferred to abrupt feeding – Can cause engorgement, mastitis, upsetting infant • There is no “best time” to wean • Technique of weaning – Eliminate one feeding at a time – Omit daytime feedings first – Eliminate the favorite feeding last • Infant will need “comfort nursing” if tired or ill • Breast pumping not advised in order to decrease the milk supply cycle

Formula Feeding • Types of formulas – Ready to feed – Concentrated liquid – Powdered • Regardless of type, it is important to follow manufacturer’s instruction on preparation and storage of formula products

Safety Alert • Overdilution or underdilution of concentrated liquid or powdered formulas can result in serious illness – Dilution reduces amount of nutrients the infant receives – Ready-to-feed formulas require no dilution

Feeding the Infant with Formula • Feed every 3 to 4 hours because formula is digested more slowly than breast milk • Do not microwave formula • Do not prop bottle • Involve partner and family in bottle feeding of infant • Burp every 1 -1. 5 oz and at end of feeding • Hold bottle so that nipple is ALWAYS full • Mom should wear supportive bra 24/7 to decrease discomfort

Postpartum Self-Care Teaching • Ample written materials regarding mother and newborn care should be provided and reviewed – Follow-up appointments – 2 weeks and 6 weeks – Hygiene – Sexual intercourse – avoid until episiotomy healed and lochia has stopped – Diet and exercise – risk of constipation – Danger signs to watch for and report – pg 232 – Newborn follow-up care – 4 days and 6 -8 weeks – Infant safety seats – back & rear-facing – Reassure mother that hospital staff is available by telephone should any questions arise

Elsevier items and derived items © 2011, 2007, 2006 by Saunders, an imprint of Elsevier Inc. 61
- Slides: 61