Chapter 7 Bone Tissue 7 1 Bone as

Chapter 7: Bone Tissue 7 -1

Bone as a Tissue • Connective tissue with a matrix hardened by minerals (calcium phosphate) • Individual bones consist of bone tissue, marrow, blood, cartilage and periosteum • Continually remodels itself • Functions of the skeletal system – support, protection, movement, electrolyte balances, acid-base balance and blood formation 7 -2
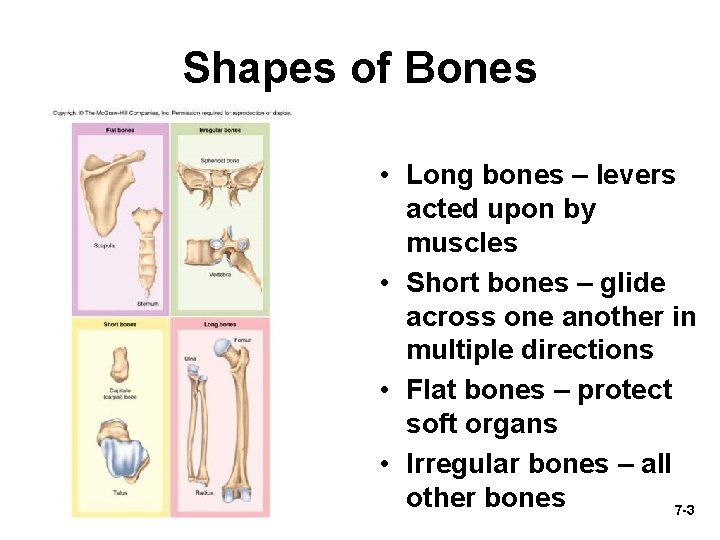
Shapes of Bones • Long bones – levers acted upon by muscles • Short bones – glide across one another in multiple directions • Flat bones – protect soft organs • Irregular bones – all other bones 7 -3
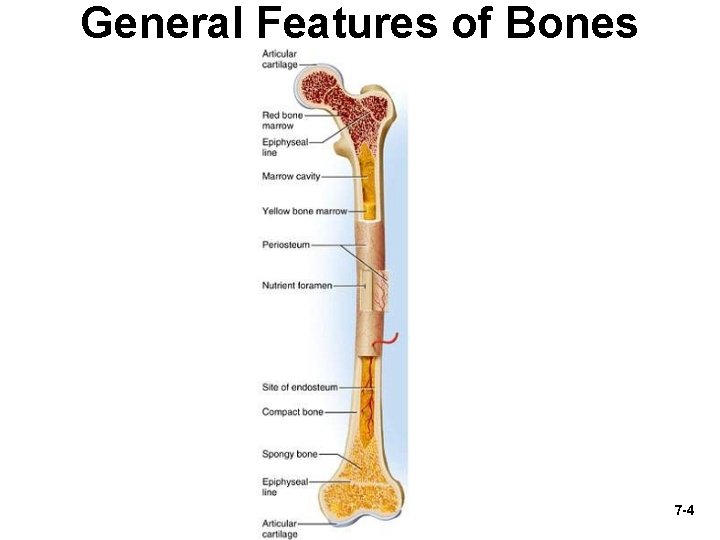
General Features of Bones 7 -4
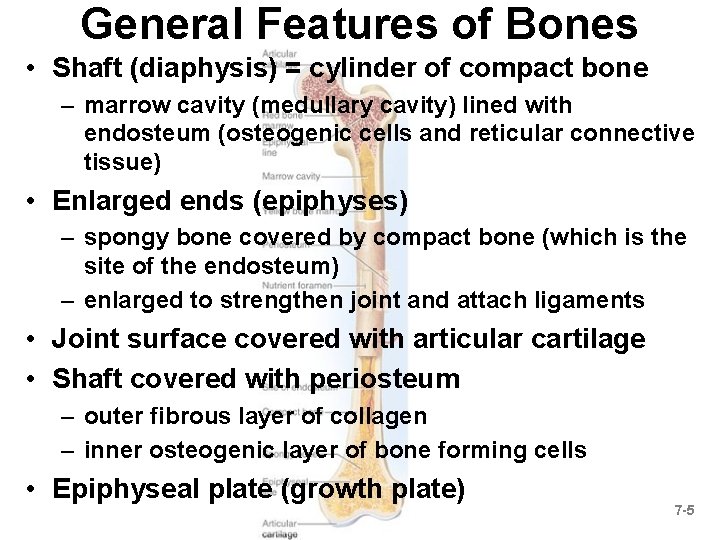
General Features of Bones • Shaft (diaphysis) = cylinder of compact bone – marrow cavity (medullary cavity) lined with endosteum (osteogenic cells and reticular connective tissue) • Enlarged ends (epiphyses) – spongy bone covered by compact bone (which is the site of the endosteum) – enlarged to strengthen joint and attach ligaments • Joint surface covered with articular cartilage • Shaft covered with periosteum – outer fibrous layer of collagen – inner osteogenic layer of bone forming cells • Epiphyseal plate (growth plate) 7 -5
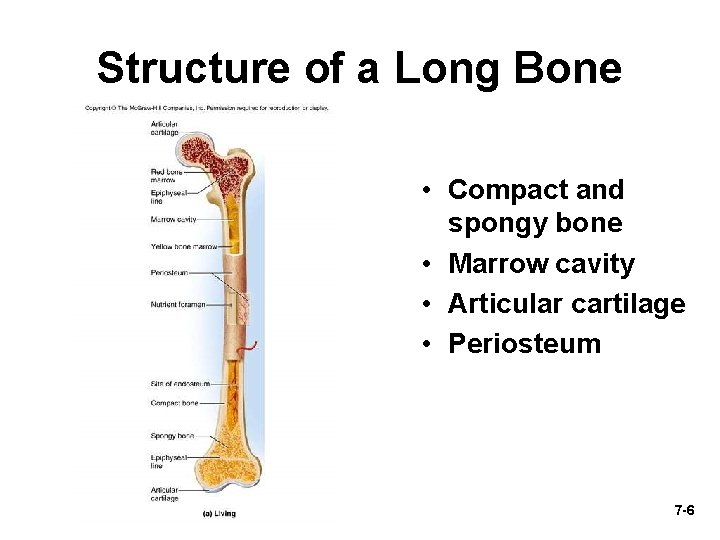
Structure of a Long Bone • Compact and spongy bone • Marrow cavity • Articular cartilage • Periosteum 7 -6
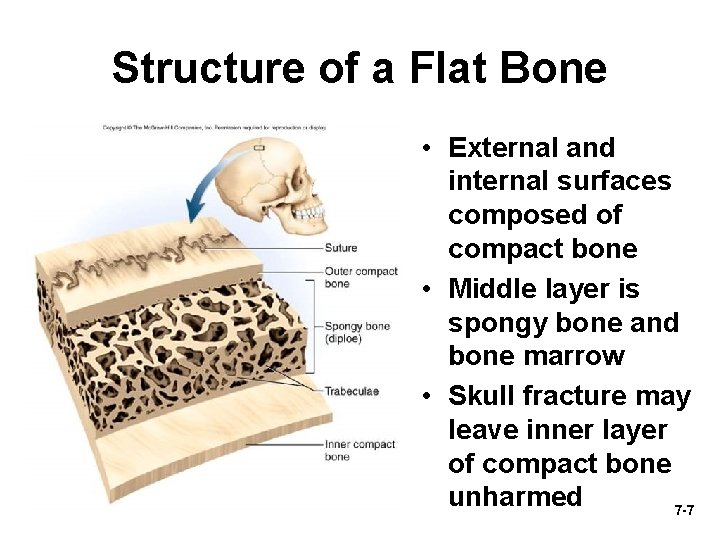
Structure of a Flat Bone • External and internal surfaces composed of compact bone • Middle layer is spongy bone and bone marrow • Skull fracture may leave inner layer of compact bone unharmed 7 -7

Histology of Osseous Tissue • • osteogenic cells osteoblasts osteocytes osteoclasts 7 -8
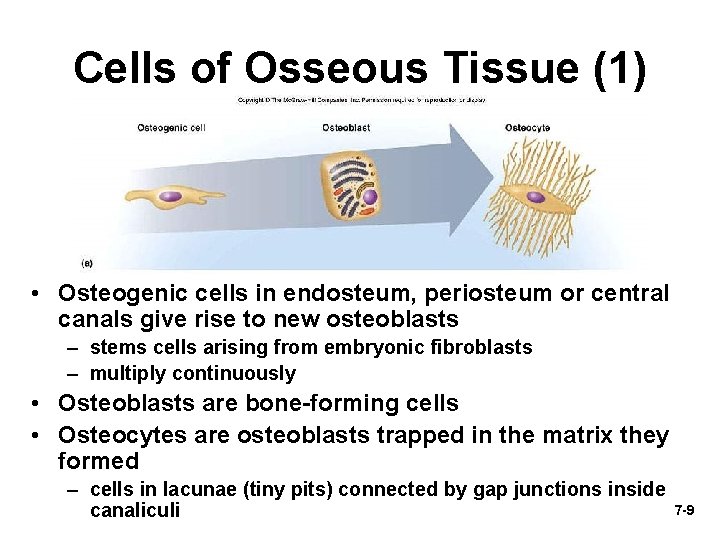
Cells of Osseous Tissue (1) • Osteogenic cells in endosteum, periosteum or central canals give rise to new osteoblasts – stems cells arising from embryonic fibroblasts – multiply continuously • Osteoblasts are bone-forming cells • Osteocytes are osteoblasts trapped in the matrix they formed – cells in lacunae (tiny pits) connected by gap junctions inside canaliculi 7 -9
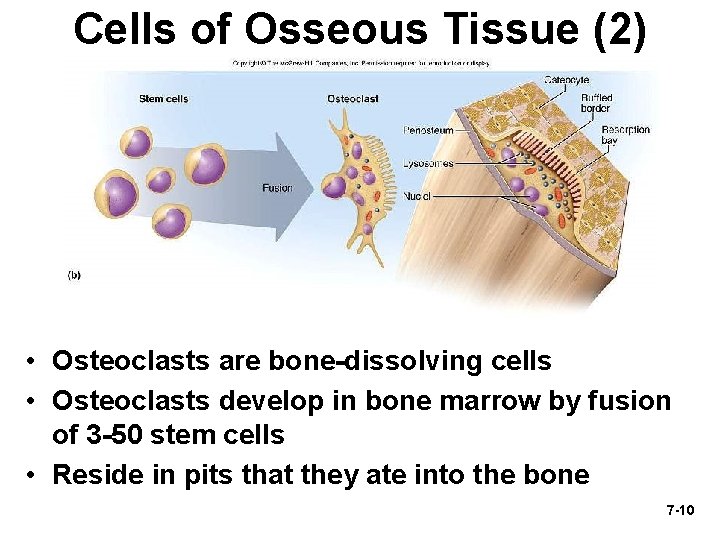
Cells of Osseous Tissue (2) • Osteoclasts are bone-dissolving cells • Osteoclasts develop in bone marrow by fusion of 3 -50 stem cells • Reside in pits that they ate into the bone 7 -10

The Matrix of Osseous Tissue • Dry weight = 1/3 organic and 2/3 inorganic matter • Organic matter – collagen, glycosaminoglycans, proteoglycans and glycoproteins • Inorganic matter – 85% hydroxyapatite – 10% calcium carbonate – other minerals (fluoride, potassium, magnesium) • Combination provides for strength and resilience – minerals support weight; collagen provides flexibility – mineral: collagen ratio varies with bone use 7 -11
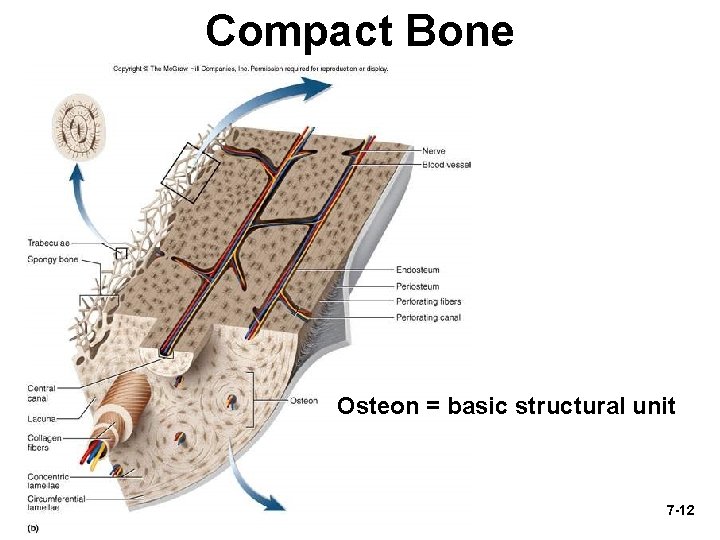
Compact Bone Osteon = basic structural unit 7 -12
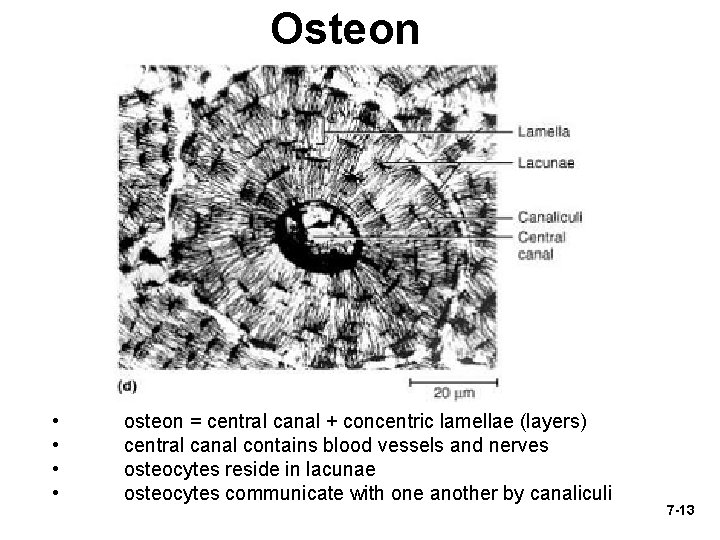
Osteon • • osteon = central canal + concentric lamellae (layers) central canal contains blood vessels and nerves osteocytes reside in lacunae osteocytes communicate with one another by canaliculi 7 -13
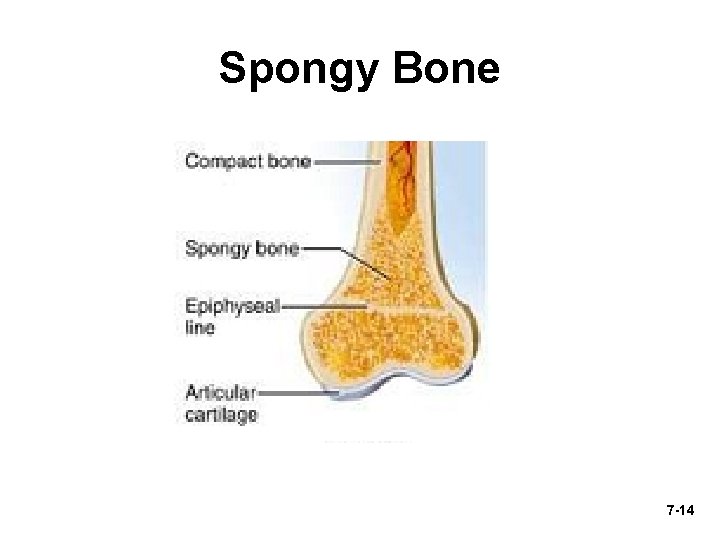
Spongy Bone 7 -14

Spongy Bone • Spongelike appearance formed by plates of bone called trabeculae – spaces filled with red bone marrow • Trabeculae have few osteons or central canals – no osteocyte is far from blood of bone marrow • Provides strength with little weight – trabeculae develop along bone’s lines of 7 -15 stress
Bone Marrow • In medullary cavity (long bone) and among trabeculae (spongy bone) • Red marrow like thick blood – reticular fibers and immature cells – Hemopoietic (produces blood cells) – in vertebrae, ribs, sternum, pelvic girdle and proximal heads of femur and humerus in adults • Yellow marrow – fatty marrow of long bones in adults 7 -16

Bone Development • the formation of bone is called ossification or osteogenesis • two mechanisms of bone formation in fetal or infant development – intramembranous ossification – endochondral ossification • mature bone growth and remodeling 7 -17

Intramembranous Ossification • intramembranous ossification produces the flat bones of the skull and most of the clavicle • four stages 7 -18
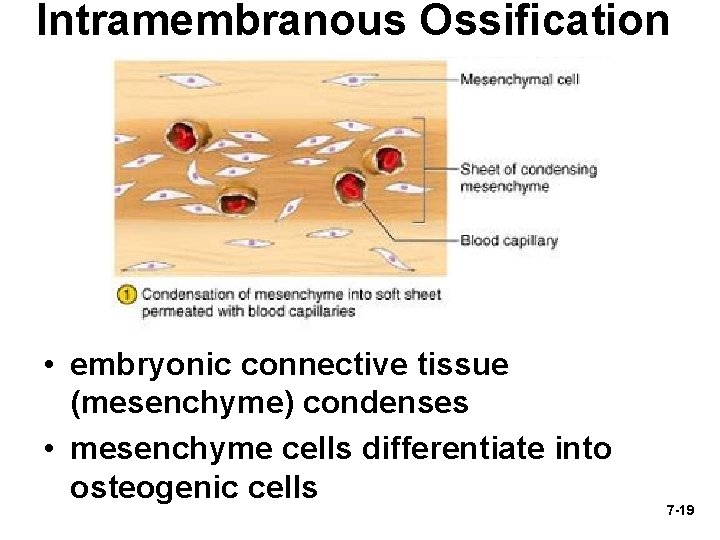
Intramembranous Ossification • embryonic connective tissue (mesenchyme) condenses • mesenchyme cells differentiate into osteogenic cells 7 -19
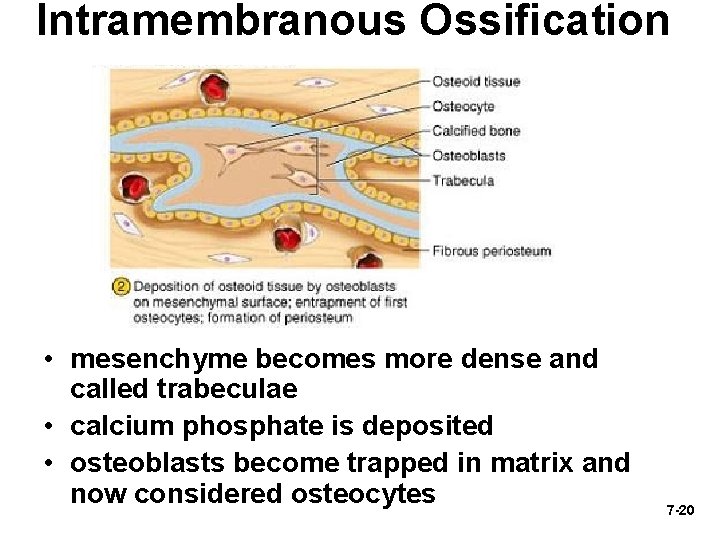
Intramembranous Ossification • mesenchyme becomes more dense and called trabeculae • calcium phosphate is deposited • osteoblasts become trapped in matrix and now considered osteocytes 7 -20
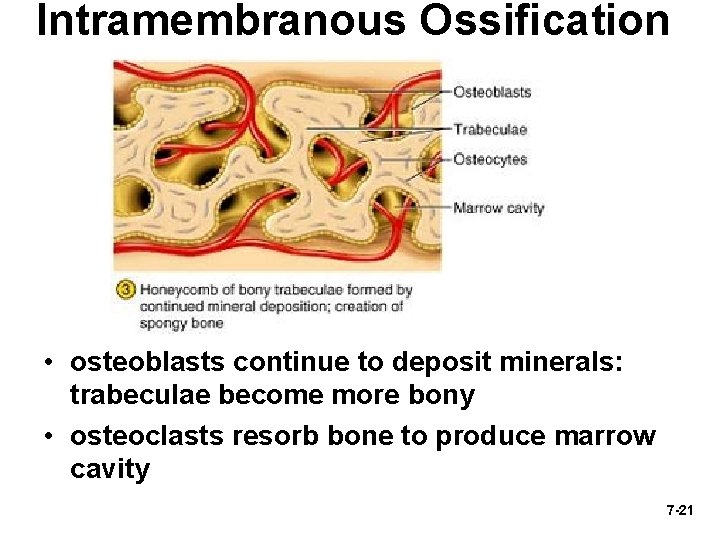
Intramembranous Ossification • osteoblasts continue to deposit minerals: trabeculae become more bony • osteoclasts resorb bone to produce marrow cavity 7 -21
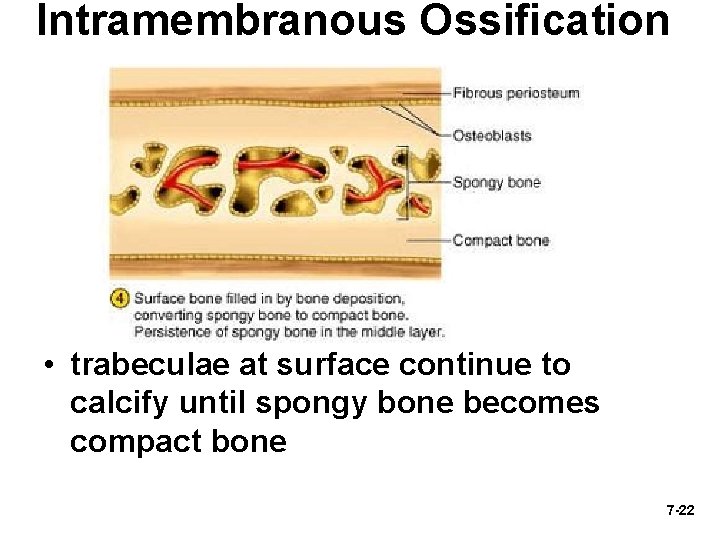
Intramembranous Ossification • trabeculae at surface continue to calcify until spongy bone becomes compact bone 7 -22

Endochondral Ossification • bone develops from a pre-existing model composed of hyaline cartilage • applies to most bones of the body: vertebrae, ribs, sternum, scapula, pelvis, and limb bones • six stages (example is a metacarpal bone of the hand) 7 -23
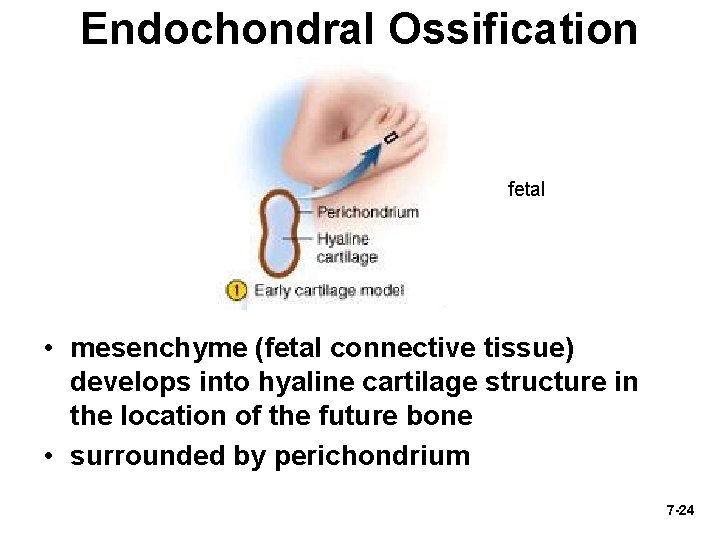
Endochondral Ossification fetal • mesenchyme (fetal connective tissue) develops into hyaline cartilage structure in the location of the future bone • surrounded by perichondrium 7 -24
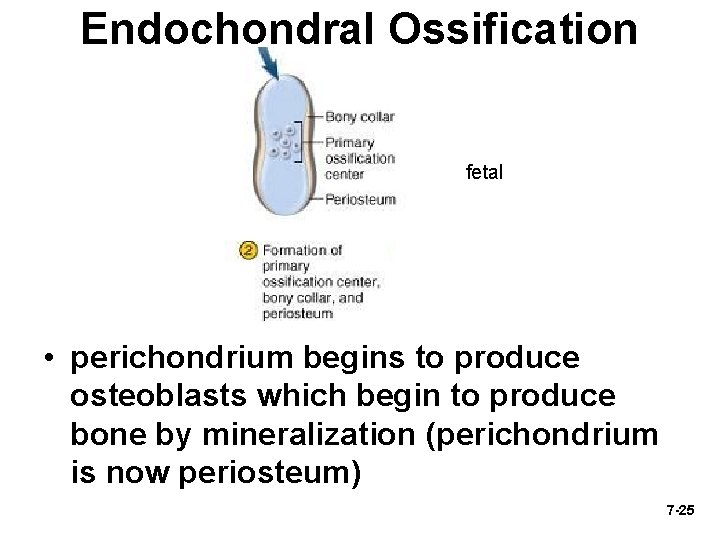
Endochondral Ossification fetal • perichondrium begins to produce osteoblasts which begin to produce bone by mineralization (perichondrium is now periosteum) 7 -25
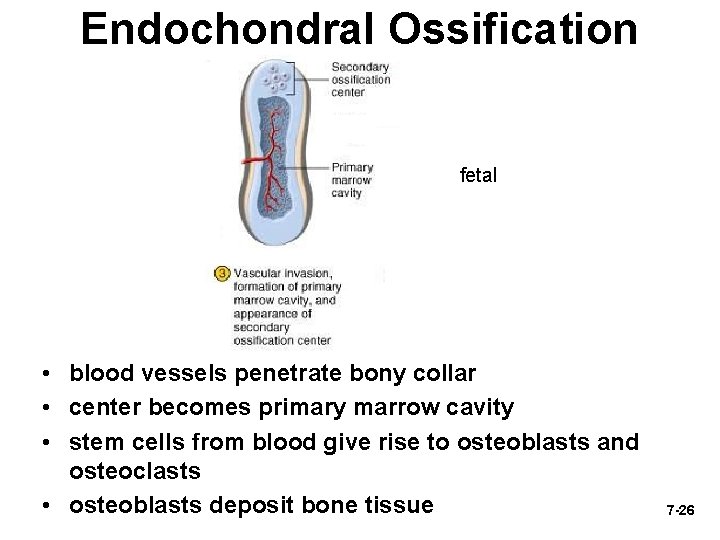
Endochondral Ossification fetal • blood vessels penetrate bony collar • center becomes primary marrow cavity • stem cells from blood give rise to osteoblasts and osteoclasts • osteoblasts deposit bone tissue 7 -26
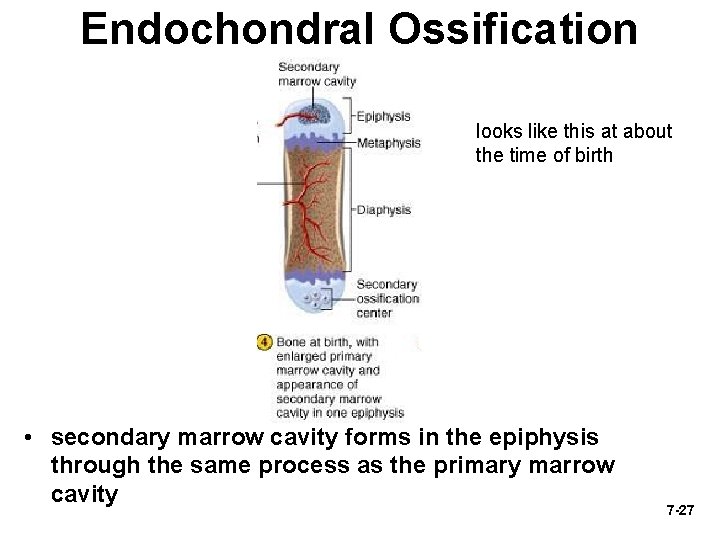
Endochondral Ossification looks like this at about the time of birth • secondary marrow cavity forms in the epiphysis through the same process as the primary marrow cavity 7 -27
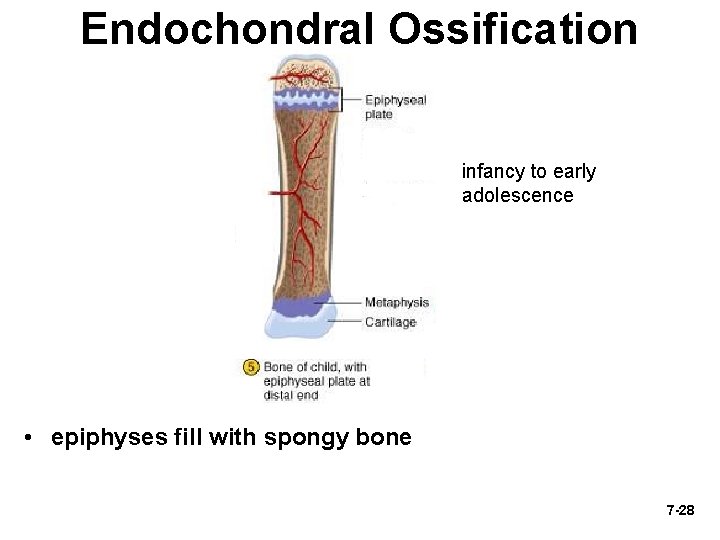
Endochondral Ossification infancy to early adolescence • epiphyses fill with spongy bone 7 -28
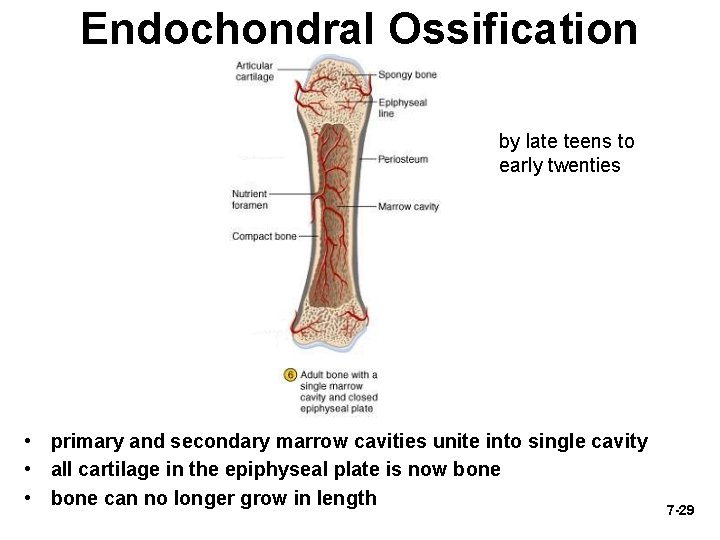
Endochondral Ossification by late teens to early twenties • primary and secondary marrow cavities unite into single cavity • all cartilage in the epiphyseal plate is now bone • bone can no longer grow in length 7 -29

Bone Growth • Bone Elongation • Bone Remodeling 7 -30

Bone Elongation and Remodeling • Bones increase in length – interstitial growth of epiphyseal plate – epiphyseal line is left behind when cartilage gone • Bones increase in width = appositional growth – osteoblasts lay down matrix in layers on outer surface and osteoclasts dissolve bone on inner surface • Bones remodeled throughout life – Wolff’s law of bone = architecture of bone determined by mechanical stresses • action of osteoblasts and osteoclasts – greater density and mass of bone in athletes or manual worker is an adaptation to stress 7 -31
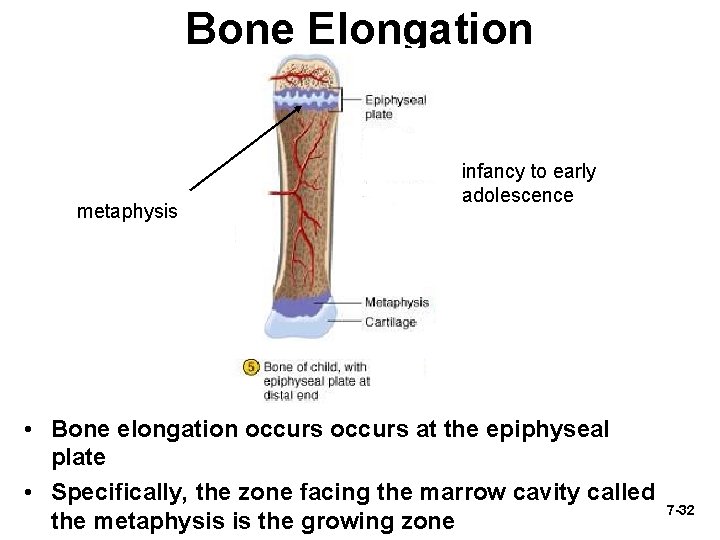
Bone Elongation metaphysis infancy to early adolescence • Bone elongation occurs at the epiphyseal plate • Specifically, the zone facing the marrow cavity called the metaphysis is the growing zone 7 -32

Physiology of Osseous Tissue • Mineral Deposition • Mineral Resporption • Calcium and Phosphate Homeostasis 7 -33

Mineral Deposition • Mineralization is crystallization process – osteoblasts produce collagen fibers spiraled the length of the osteon – minerals cover the fibers and harden the matrix • ions (calcium and phosphate and from blood plasma) are deposited along the fibers • ion concentration must reach the solubility product for crystal formation to occur • Abnormal calcification (ectopic) – may occur in lungs, brain, eyes, muscles, tendons or arteries (arteriosclerosis) 7 -34

Mineral Resorption from Bone • Bone dissolved and minerals released into blood – performed by osteoclasts “ruffled border” – hydrogen pumps in membrane secrete hydrogen into space between the osteoclast and bone surface – chloride ions follow by electrical attraction – hydrochloric acid (p. H 4) dissolves bone minerals – enzyme (acid phosphatase) digests the collagen 7 -35

Calcium and Phosphate • Phosphate is component of DNA, RNA, ATP, phospholipids, and p. H buffers – ~750 g in adult skeleton – plasma concentration is ~ 4. 0 mg/d. L • Calcium needed in neurons, muscle contraction, blood clotting and exocytosis – ~1100 g in adult skeleton – plasma concentration is ~ 10 mg/d. L 7 -36

Ion Imbalances • Changes in phosphate levels have little effect • Changes in calcium can be serious – hypocalcemia is deficiency of blood calcium • causes excitability of nervous system if too low – muscle spasms, tremors or tetany ~6 mg/d. L – laryngospasm and suffocation ~4 mg/d. L • with less calcium, sodium channels open more easily, sodium enters cell and excites neuron – hypercalcemia is excess of blood calcium • binding to cell surface makes sodium channels less likely to open, depressing nervous system – muscle weakness and sluggish reflexes, cardiac arrest ~12 mg/d. L • Calcium phosphate homeostasis depends on calcitriol, calcitonin and PTH hormone regulation 7 -37

Calcium and Phosphate Homeostasis • Calcitriol – produced by skin, liver and kidney (sequentially) – active vitamin D – raises blood calcium • Calcitonin – secreted by thyroid gland – lowers blood calcium • Parathyroid Hormone (PTH) – secreted by parathyroid gland – PTH raises blood calcium levels 7 -38
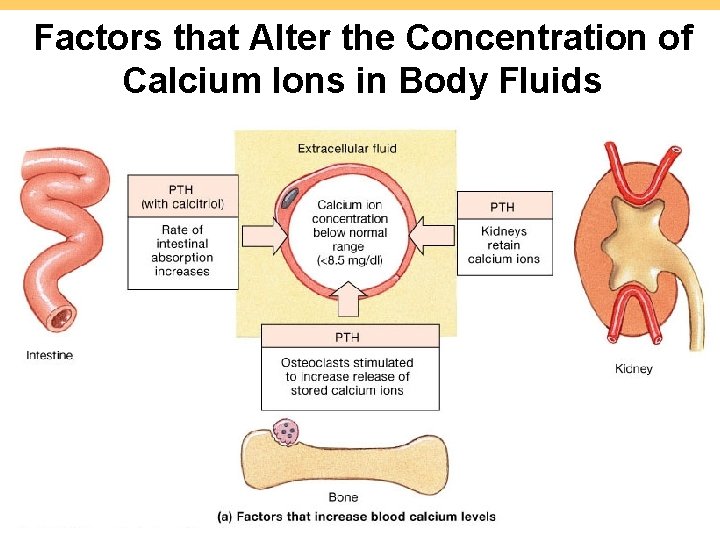
Factors that Alter the Concentration of Calcium Ions in Body Fluids 7 -39 Figure 6. 14 a
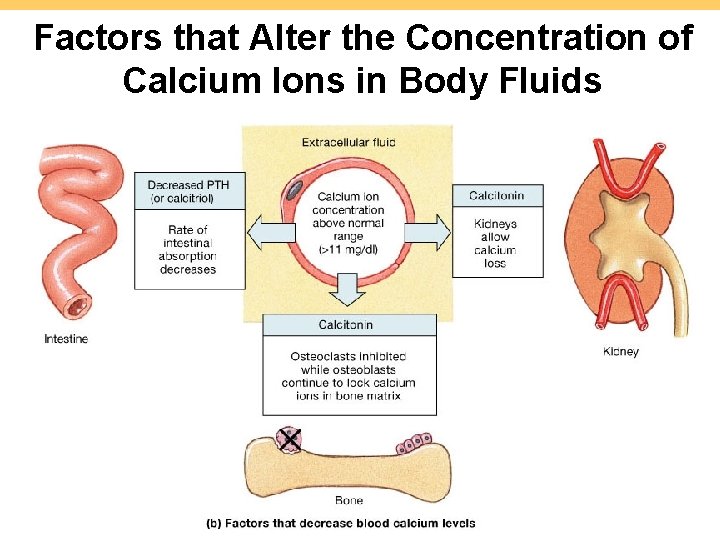
Factors that Alter the Concentration of Calcium Ions in Body Fluids 7 -40 Figure 6. 14 b

End 7 -41
- Slides: 41