Chapter 6 Osseous Tissue and Bone Structure Lecture

Chapter 6 Osseous Tissue and Bone Structure Lecture Presentation by Lee Ann Frederick University of Texas at Arlington © 2015 Pearson Education, Inc.

An Introduction to the Skeletal System • Learning Outcomes • 6 -1 Describe the primary functions of the skeletal system. • 6 -2 Classify bones according to shape and internal organization, giving examples of each type, and explain the functional significance of each of the major types of bone markings. • 6 -3 Identify the cell types in bone, and list their major functions. © 2015 Pearson Education, Inc.

An Introduction to the Skeletal System • Learning Outcomes • 6 -4 Compare the structures and functions of compact bone and spongy bone. • 6 -5 Compare the mechanisms of endochondral ossification and intramembranous ossification. • 6 -6 Describe the remodeling and homeostatic mechanisms of the skeletal system. • 6 -7 Discuss the effects of exercise, hormones, and nutrition on bone development and on the skeletal system. © 2015 Pearson Education, Inc.

An Introduction to the Skeletal System • Learning Outcomes • 6 -8 Explain the role of calcium as it relates to the skeletal system. • 6 -9 Describe the types of fractures, and explain how fractures heal. • 6 -10 Summarize the effects of the aging process on the skeletal system. © 2015 Pearson Education, Inc.

An Introduction to the Skeletal System • The Skeletal System is all of the 206 bones in the human body • Includes: • Bones of the skeleton • Cartilages, ligaments, and connective tissues © 2015 Pearson Education, Inc.

6 -1 Functions of the Skeletal System • Five Primary Functions of the Skeletal System 1. Support 2. Storage of Minerals (calcium) and Lipids (yellow marrow) 3. Blood Cell Production (red marrow) 4. Protection 5. Leverage (force of motion) © 2015 Pearson Education, Inc.

Functions of the Skeletal System Support The main job of the skeleton is to provide support for our body. Without your skeleton your body would collapse into a heap. Your skeleton is strong but light. © 2015 Pearson Education, Inc.

Functions of the Skeletal System Protection Your skeleton also helps protect your internal organs and fragile body tissues. The brain, eyes, heart, lungs and spinal cord are all protected by your skeleton. Cranium (skull) protects your brain and eyes, the ribs protect your heart and lungs and your vertebrae (spine, backbones) protect your spinal cord © 2015 Pearson Education, Inc.

Functions of the Skeletal System Movement Bones provide the structure for muscles to attach so that our bodies are able to move. Tendons are tough inelastic bands that hold attach muscle to bone. © 2015 Pearson Education, Inc.

6 -2 Classification of Bones • Are classified by: • Shape • Internal tissue organization • Bone markings (surface features; marks) © 2015 Pearson Education, Inc.

6 -2 Classification of Bones • Six Bone Shapes 1. Sutural bones 2. Irregular bones 3. Short bones 4. Flat bones 5. Long bones 6. Sesamoid bones © 2015 Pearson Education, Inc.
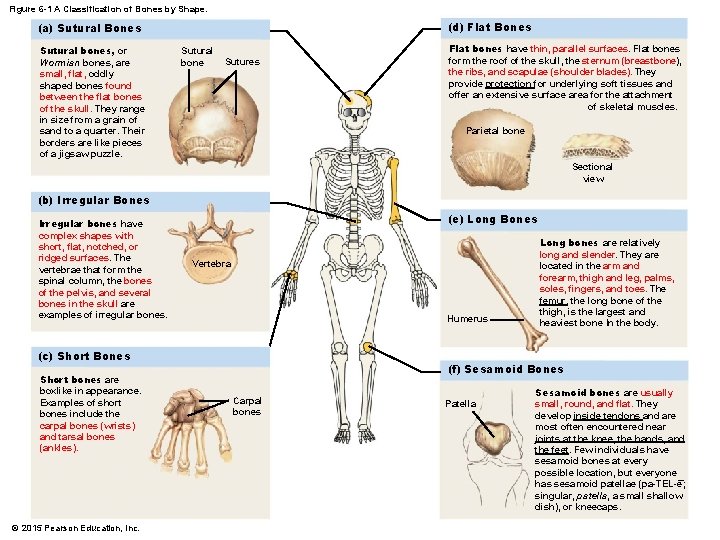
Figure 6 -1 A Classification of Bones by Shape. (d) Flat Bones (a) Sutural Bones Sutural bones, or Wormian bones, are small, flat, oddly shaped bones found between the flat bones of the skull. They range in size from a grain of sand to a quarter. Their borders are like pieces of a jigsaw puzzle. Sutural bone Sutures Flat bones have thin, parallel surfaces. Flat bones form the roof of the skull, the sternum (breastbone), the ribs, and scapulae (shoulder blades). They provide protection for underlying soft tissues and offer an extensive surface area for the attachment of skeletal muscles. Parietal bone Sectional view (b) Irregular Bones Irregular bones have complex shapes with short, flat, notched, or ridged surfaces. The vertebrae that form the spinal column, the bones of the pelvis, and several bones in the skull are examples of irregular bones. (e) Long Bones Vertebra Humerus (c) Short Bones Short bones are boxlike in appearance. Examples of short bones include the carpal bones (wrists) and tarsal bones (ankles). © 2015 Pearson Education, Inc. Long bones are relatively long and slender. They are located in the arm and forearm, thigh and leg, palms, soles, fingers, and toes. The femur, the long bone of the thigh, is the largest and heaviest bone In the body. (f) Sesamoid Bones Carpal bones Patella Sesamoid bones are usually small, round, and flat. They develop inside tendons and are most often encountered near joints at the knee, the hands, and the feet. Few individuals have sesamoid bones at every possible location, but everyone – has sesamoid patellae (pa-TEL-e; singular, patella, a small shallow dish), or kneecaps.
6 -2 Classification of Bones • Sutural Bones • Small, irregular bones • Found between the flat bones of the skull • Irregular Bones • Have complex shapes • Examples: spinal vertebrae, pelvic bones © 2015 Pearson Education, Inc.
6 -2 Classification of Bones • Short Bones • Small and thick • Examples: ankle and wrist bones • Flat Bones • Thin with parallel surfaces • Found in the skull, sternum, ribs, and scapulae © 2015 Pearson Education, Inc.
6 -2 Classification of Bones • Long and thin • Found in arms, legs, hands, feet, fingers, and toes • Sesamoid Bones • Small and flat • Develop inside tendons near joints of knees, hands, and feet © 2015 Pearson Education, Inc.

6 -2 Classification of Bones Bone Markings • Depressions or grooves: Along bone surface • Elevations or projections • Where tendons and ligaments attach • Tunnels: Where blood and nerves enter bone © 2015 Pearson Education, Inc.
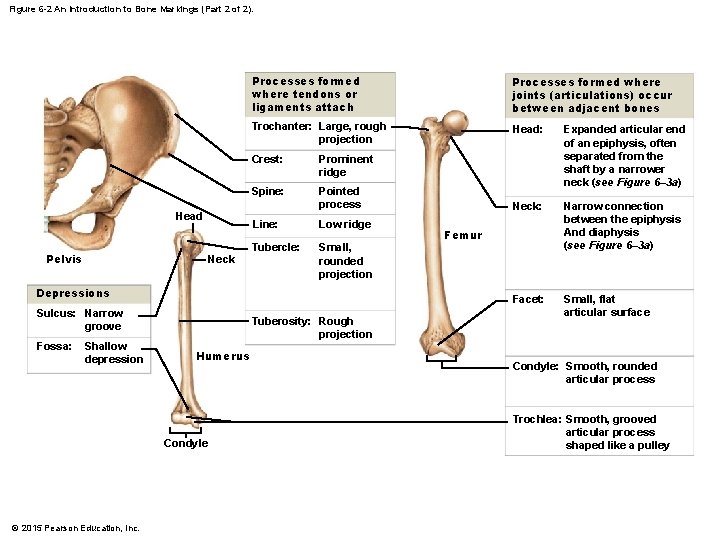
Figure 6 -2 An Introduction to Bone Markings (Part 2 of 2). Head Pelvis Neck Processes formed where tendons or ligaments attach Processes formed where joints (articulations) occur between adjacent bones Trochanter: Large, rough projection Head: Expanded articular end of an epiphysis, often separated from the shaft by a narrower neck (see Figure 6– 3 a) Neck: Narrow connection between the epiphysis And diaphysis (see Figure 6– 3 a) Facet: Small, flat articular surface Crest: Prominent ridge Spine: Pointed process Line: Low ridge Tubercle: Small, rounded projection Depressions Sulcus: Narrow groove Fossa: Shallow depression Tuberosity: Rough projection Humerus Condyle © 2015 Pearson Education, Inc. Femur Condyle: Smooth, rounded articular process Trochlea: Smooth, grooved articular process shaped like a pulley
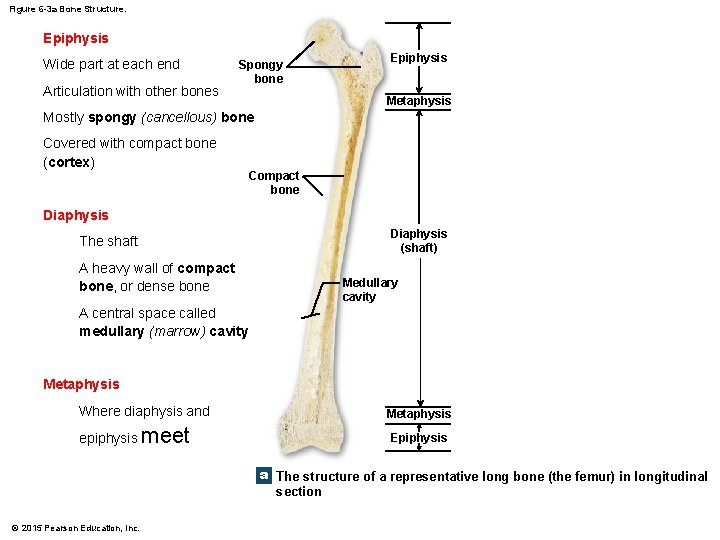
Figure 6 -3 a Bone Structure. Epiphysis Wide part at each end Articulation with other bones Spongy bone Epiphysis Metaphysis Mostly spongy (cancellous) bone Covered with compact bone (cortex) Compact bone Diaphysis The shaft A heavy wall of compact bone, or dense bone Diaphysis (shaft) Medullary cavity A central space called medullary (marrow) cavity Metaphysis Where diaphysis and epiphysis meet Metaphysis Epiphysis a The structure of a representative long bone (the femur) in longitudinal section © 2015 Pearson Education, Inc.
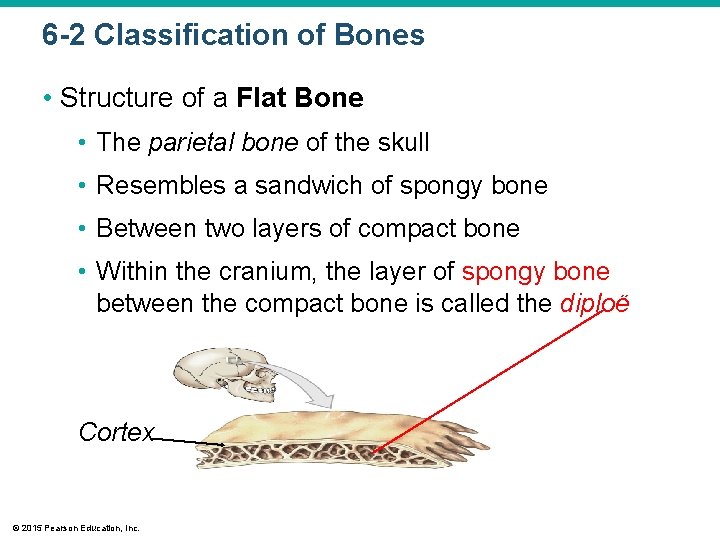
6 -2 Classification of Bones • Structure of a Flat Bone • The parietal bone of the skull • Resembles a sandwich of spongy bone • Between two layers of compact bone • Within the cranium, the layer of spongy bone between the compact bone is called the diploë Cortex © 2015 Pearson Education, Inc.

6 -3 Bone (Osseous) Tissue • Dense, supportive connective tissue • Contains specialized cells • Produces solid matrix of calcium salt deposits • Around collagen fibers © 2015 Pearson Education, Inc.

6 -3 Bone (Osseous) Tissue • Characteristics of Bone Tissue • Dense matrix, containing: • Deposits of calcium salts • Osteocytes (bone cells) within lacunae organized around blood vessels • Periosteum • Covers outer surfaces of bones • Consists of outer fibrous and inner cellular layers © 2015 Pearson Education, Inc.

6 -3 Bone (Osseous) Tissue • Bone Matrix Minerals • Two-thirds of bone matrix is calcium phosphate, Ca 3(PO 4)2 which reacts with calcium hydroxide, Ca(OH)2 • To form crystals of hydroxyapatite, Ca 10(PO 4)6(OH)2 to incorporates other calcium salts and ions Matrix proteins • One-third of bone matrix is protein fibers (collagen) © 2015 Pearson Education, Inc.

6 -3 Bone (Osseous) Tissue • Bone Cells • Make up only 2 percent of bone mass • Bone contains four types of cells 1. Osteocytes 2. Osteoblasts 3. Osteoprogenitor cells 4. Osteoclasts © 2015 Pearson Education, Inc.
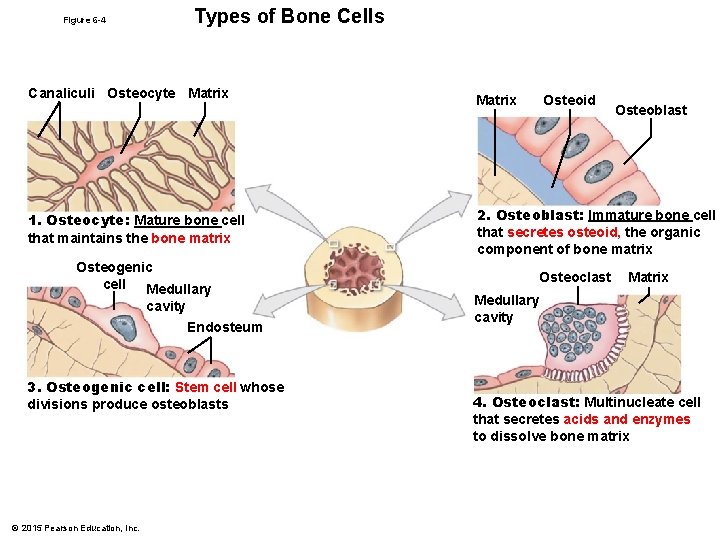
Types of Bone Cells Figure 6 -4 Canaliculi Osteocyte Matrix 1. Osteocyte: Mature bone cell that maintains the bone matrix Osteogenic cell Medullary cavity Endosteum 3. Osteogenic cell: Stem cell whose divisions produce osteoblasts © 2015 Pearson Education, Inc. Matrix Osteoid Osteoblast 2. Osteoblast: Immature bone cell that secretes osteoid, the organic component of bone matrix Osteoclast Matrix Medullary cavity 4. Osteoclast: Multinucleate cell that secretes acids and enzymes to dissolve bone matrix
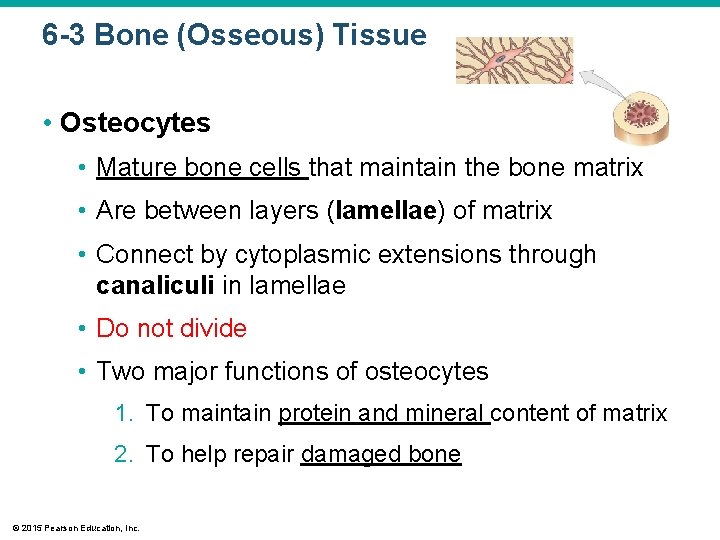
6 -3 Bone (Osseous) Tissue • Osteocytes • Mature bone cells that maintain the bone matrix • Are between layers (lamellae) of matrix • Connect by cytoplasmic extensions through canaliculi in lamellae • Do not divide • Two major functions of osteocytes 1. To maintain protein and mineral content of matrix 2. To help repair damaged bone © 2015 Pearson Education, Inc.
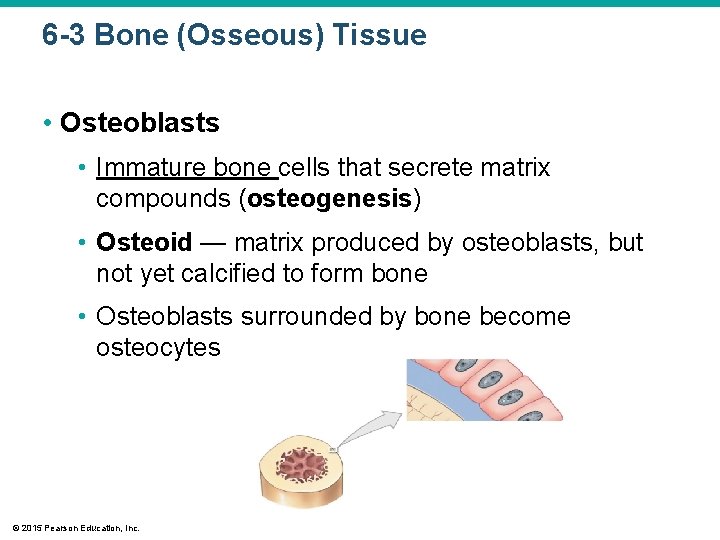
6 -3 Bone (Osseous) Tissue • Osteoblasts • Immature bone cells that secrete matrix compounds (osteogenesis) • Osteoid — matrix produced by osteoblasts, but not yet calcified to form bone • Osteoblasts surrounded by bone become osteocytes © 2015 Pearson Education, Inc.
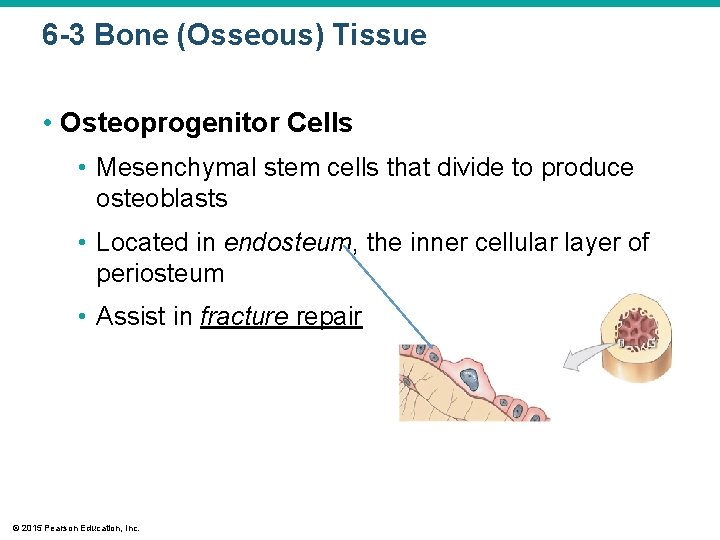
6 -3 Bone (Osseous) Tissue • Osteoprogenitor Cells • Mesenchymal stem cells that divide to produce osteoblasts • Located in endosteum, the inner cellular layer of periosteum • Assist in fracture repair © 2015 Pearson Education, Inc.
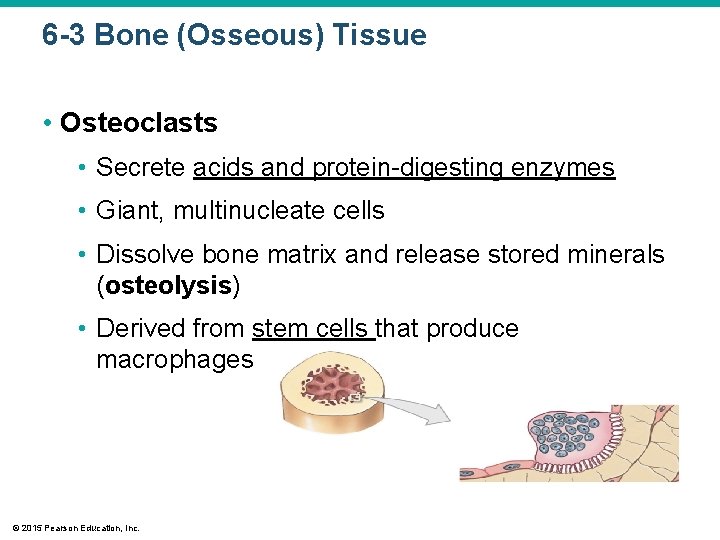
6 -3 Bone (Osseous) Tissue • Osteoclasts • Secrete acids and protein-digesting enzymes • Giant, multinucleate cells • Dissolve bone matrix and release stored minerals (osteolysis) • Derived from stem cells that produce macrophages © 2015 Pearson Education, Inc.

6 -3 Bone (Osseous) Tissue • Homeostasis • Bone building (by osteoblasts) and bone recycling (by osteoclasts) must balance • More breakdown than building, bones become weak • Exercise, particularly weight-bearing exercise, causes osteoblasts to build bone © 2015 Pearson Education, Inc.
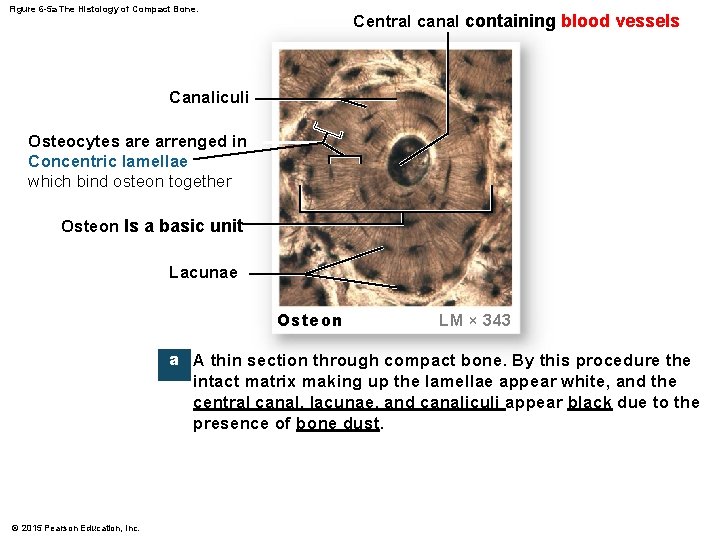
Figure 6 -5 a The Histology of Compact Bone. Central canal containing blood vessels Canaliculi Osteocytes are arrenged in Concentric lamellae which bind osteon together Osteon Is a basic unit Lacunae Osteon LM × 343 a A thin section through compact bone. By this procedure the intact matrix making up the lamellae appear white, and the central canal, lacunae, and canaliculi appear black due to the presence of bone dust. © 2015 Pearson Education, Inc.
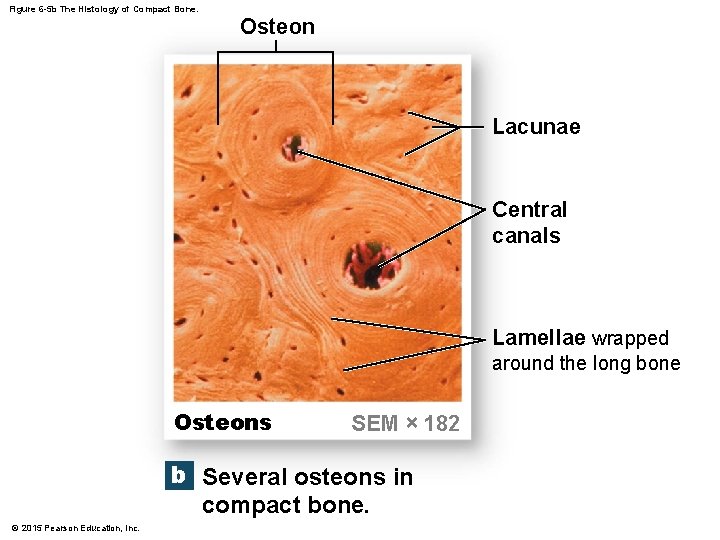
Figure 6 -5 b The Histology of Compact Bone. Osteon Lacunae Central canals Lamellae wrapped around the long bone Osteons SEM × 182 b Several osteons in compact bone. © 2015 Pearson Education, Inc.
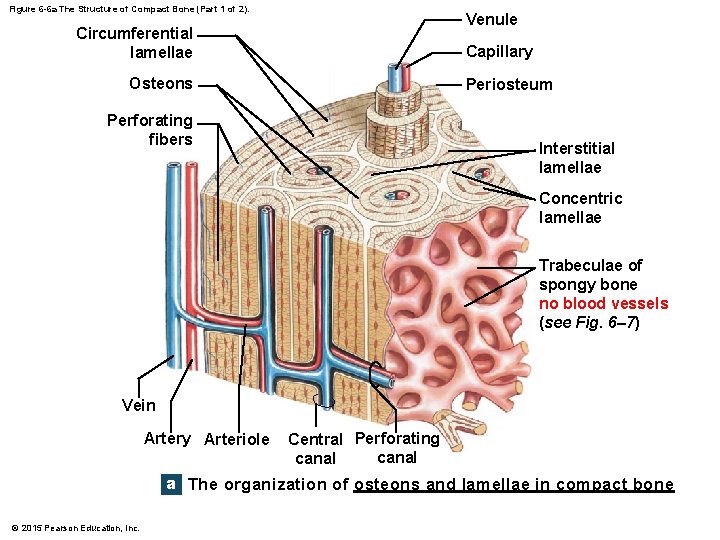
Figure 6 -6 a The Structure of Compact Bone (Part 1 of 2). Venule Circumferential lamellae Capillary Osteons Periosteum Perforating fibers Interstitial lamellae Concentric lamellae Trabeculae of spongy bone no blood vessels (see Fig. 6– 7) Vein Artery Arteriole Central Perforating canal a The organization of osteons and lamellae in compact bone © 2015 Pearson Education, Inc.

6 -4 Compact Bone and Spongy Bone • The Structure of Spongy Bone • The space between trabeculae is filled with red bone marrow • Which has blood vessels • Forms red blood cells • And supplies nutrients to osteocytes • Yellow bone marrow • In some bones, spongy bone holds yellow bone marrow • Is yellow because it stores fat © 2015 Pearson Education, Inc.
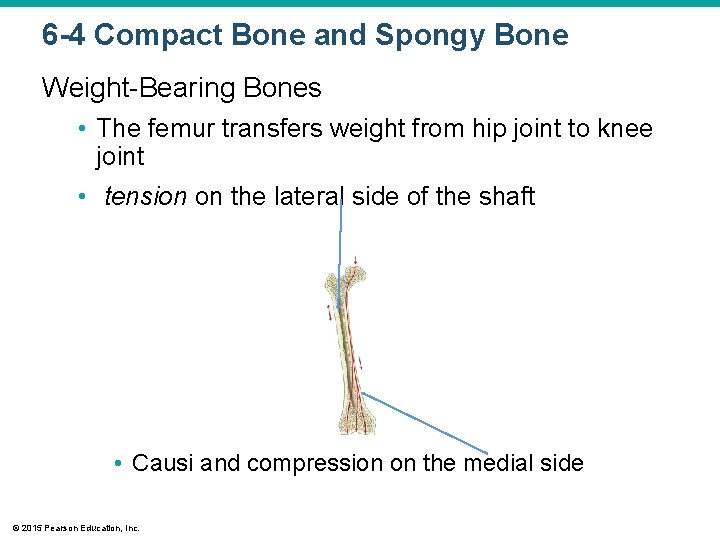
6 -4 Compact Bone and Spongy Bone Weight-Bearing Bones • The femur transfers weight from hip joint to knee joint • tension on the lateral side of the shaft • Causi and compression on the medial side © 2015 Pearson Education, Inc.

6 -4 Compact Bone and Spongy Bone • Compact Bone Is Covered with a Membrane • Periosteum on the outside • Covers all bones except parts enclosed in joint capsules • Made up of an outer, fibrous layer and an inner, cellular layer • Perforating fibers: collagen fibers of the periosteum • Connect with collagen fibers in bone • And with fibers of joint capsules; attach tendons, and ligaments © 2015 Pearson Education, Inc.
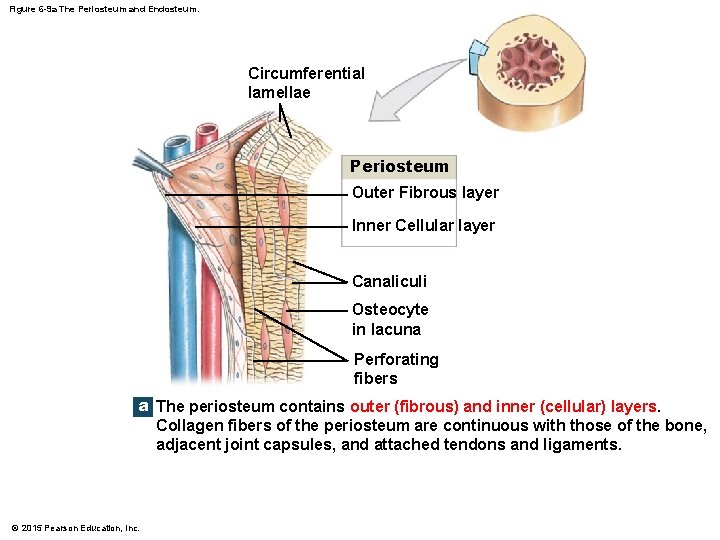
Figure 6 -9 a The Periosteum and Endosteum. Circumferential lamellae Periosteum Outer Fibrous layer Inner Cellular layer Canaliculi Osteocyte in lacuna Perforating fibers a The periosteum contains outer (fibrous) and inner (cellular) layers. Collagen fibers of the periosteum are continuous with those of the bone, adjacent joint capsules, and attached tendons and ligaments. © 2015 Pearson Education, Inc.

6 -4 Compact Bone and Spongy Bone • Functions of Periosteum 1. Isolates bone from surrounding tissues 2. Provides a route for circulatory and nervous supply 3. Participates in bone growth and repair © 2015 Pearson Education, Inc
6 -4 Compact Bone and Spongy Bone • Compact Bone Is Covered with a Membrane Endosteum on the inside • An incomplete cellular layer: • Lines the medullary (marrow) cavity • Covers trabeculae of spongy bone • Lines central canals • Contains osteoblasts, osteoprogenitor cells, and osteoclasts • Is active in bone growth and repair © 2015 Pearson Education, Inc.

6 -5 Bone Formation and Growth • Bone Development • Human bones grow until about age 25 • Osteogenesis • Bone formation • Ossification • The process of replacing other tissues with bone © 2015 Pearson Education, Inc.
6 -5 Bone Formation and Growth • Bone Development • Calcification • The process of depositing calcium salts • Occurs during bone ossification and in other tissues • Ossification • Two main forms of ossification 1. Endochondral ossification 2. Intramembranous ossification © 2015 Pearson Education, Inc.
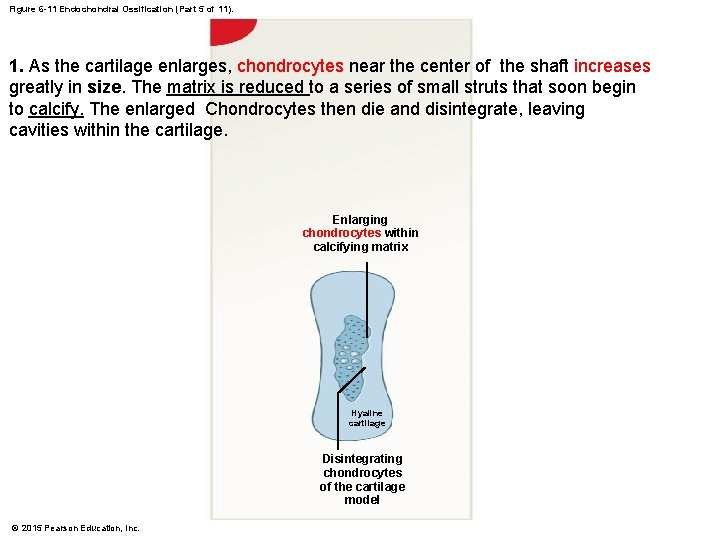
Figure 6 -11 Endochondral Ossification (Part 5 of 11). 1. As the cartilage enlarges, chondrocytes near the center of the shaft increases greatly in size. The matrix is reduced to a series of small struts that soon begin to calcify. The enlarged Chondrocytes then die and disintegrate, leaving cavities within the cartilage. Enlarging chondrocytes within calcifying matrix Hyaline cartilage Disintegrating chondrocytes of the cartilage model © 2015 Pearson Education, Inc.
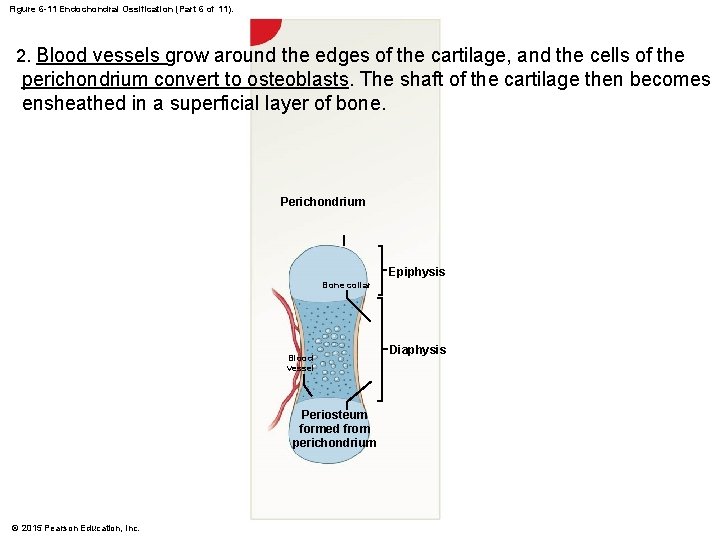
Figure 6 -11 Endochondral Ossification (Part 6 of 11). 2. Blood vessels grow around the edges of the cartilage, and the cells of the perichondrium convert to osteoblasts. The shaft of the cartilage then becomes ensheathed in a superficial layer of bone. Perichondrium Epiphysis Bone collar Blood vessel Periosteum formed from perichondrium © 2015 Pearson Education, Inc. Diaphysis
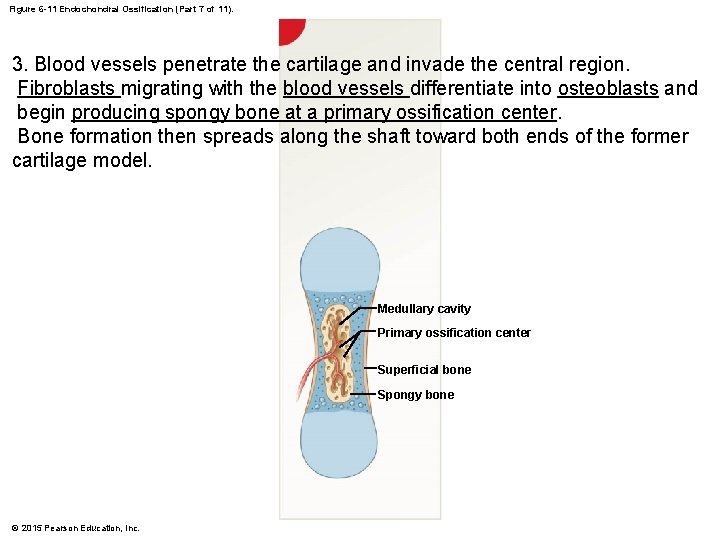
Figure 6 -11 Endochondral Ossification (Part 7 of 11). 3. Blood vessels penetrate the cartilage and invade the central region. Fibroblasts migrating with the blood vessels differentiate into osteoblasts and begin producing spongy bone at a primary ossification center. Bone formation then spreads along the shaft toward both ends of the former cartilage model. Medullary cavity Primary ossification center Superficial bone Spongy bone © 2015 Pearson Education, Inc.
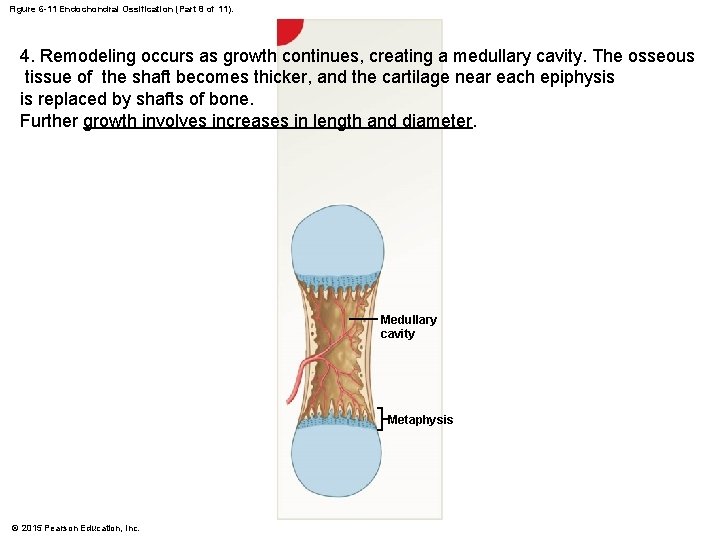
Figure 6 -11 Endochondral Ossification (Part 8 of 11). 4. Remodeling occurs as growth continues, creating a medullary cavity. The osseous tissue of the shaft becomes thicker, and the cartilage near each epiphysis is replaced by shafts of bone. Further growth involves increases in length and diameter. Medullary cavity Metaphysis © 2015 Pearson Education, Inc.
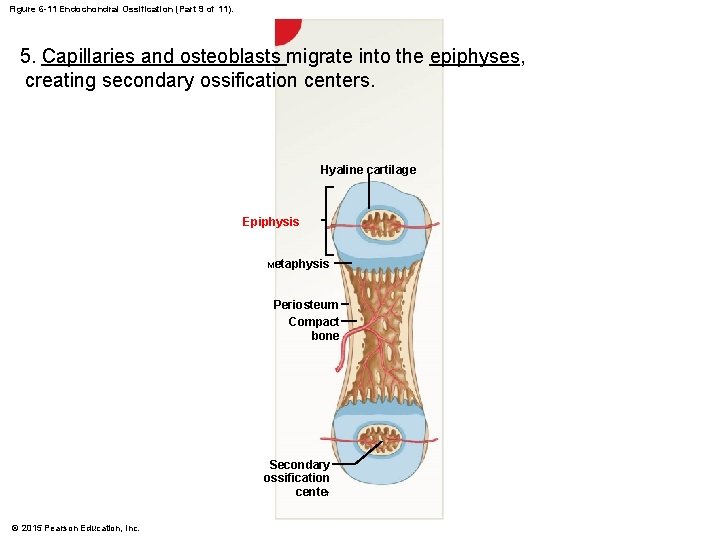
Figure 6 -11 Endochondral Ossification (Part 9 of 11). 5. Capillaries and osteoblasts migrate into the epiphyses, creating secondary ossification centers. Hyaline cartilage Epiphysis Metaphysis Periosteum Compact bone Secondary ossification center © 2015 Pearson Education, Inc.
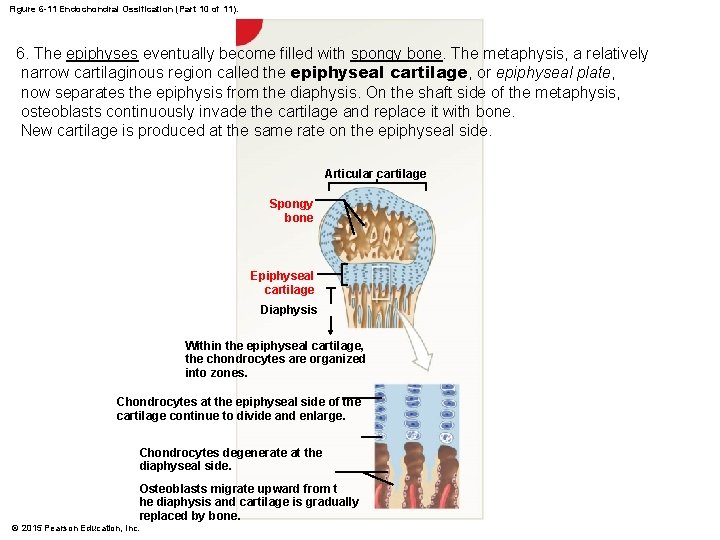
Figure 6 -11 Endochondral Ossification (Part 10 of 11). 6. The epiphyses eventually become filled with spongy bone. The metaphysis, a relatively narrow cartilaginous region called the epiphyseal cartilage, or epiphyseal plate, now separates the epiphysis from the diaphysis. On the shaft side of the metaphysis, osteoblasts continuously invade the cartilage and replace it with bone. New cartilage is produced at the same rate on the epiphyseal side. Articular cartilage Spongy bone Epiphyseal cartilage Diaphysis Within the epiphyseal cartilage, the chondrocytes are organized into zones. Chondrocytes at the epiphyseal side of the cartilage continue to divide and enlarge. Chondrocytes degenerate at the diaphyseal side. Osteoblasts migrate upward from t he diaphysis and cartilage is gradually replaced by bone. © 2015 Pearson Education, Inc.
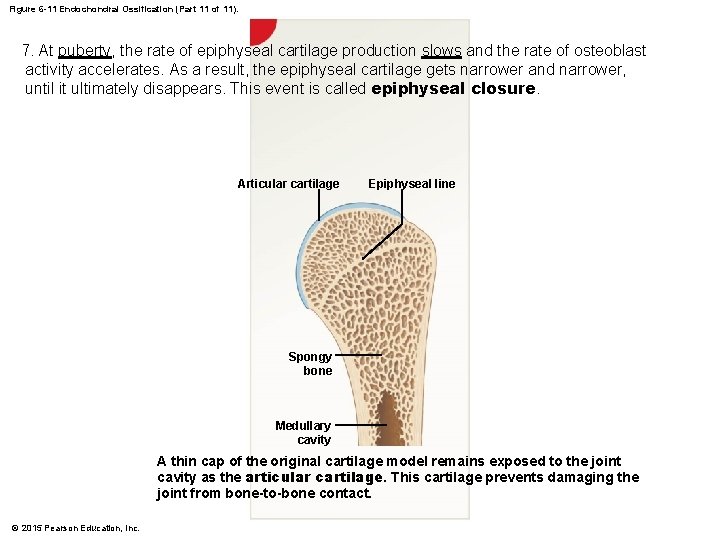
Figure 6 -11 Endochondral Ossification (Part 11 of 11). 7. At puberty, the rate of epiphyseal cartilage production slows and the rate of osteoblast activity accelerates. As a result, the epiphyseal cartilage gets narrower and narrower, until it ultimately disappears. This event is called epiphyseal closure. Articular cartilage Epiphyseal line Spongy bone Medullary cavity A thin cap of the original cartilage model remains exposed to the joint cavity as the articular cartilage. This cartilage prevents damaging the joint from bone-to-bone contact. © 2015 Pearson Education, Inc.
6 -5 Bone Formation and Growth Appositional Growth • Compact bone thickens and strengthens long bone with layers of circumferential lamellae • Epiphyseal Lines • When long bone stops growing, after puberty: • Epiphyseal cartilage disappears • Is visible on x-rays as an epiphyseal line • Mature Bones • As long bone matures: • Osteoclasts enlarge medullary (marrow) cavity • Osteons form around blood vessels in compact bone © 2015 Pearson Education, Inc.
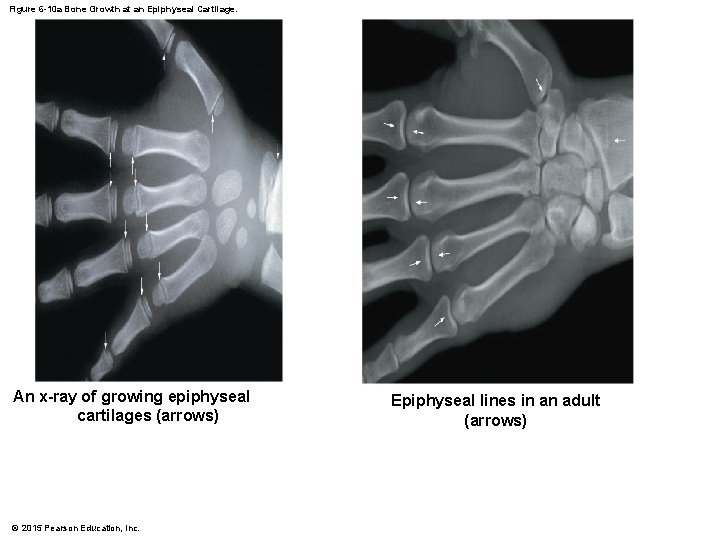
Figure 6 -10 a Bone Growth at an Epiphyseal Cartilage. An x-ray of growing epiphyseal cartilages (arrows) © 2015 Pearson Education, Inc. Epiphyseal lines in an adult (arrows)
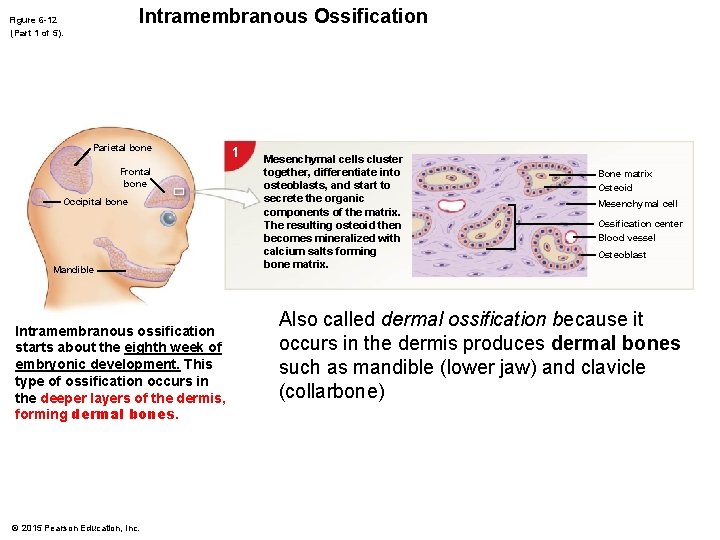
Intramembranous Ossification Figure 6 -12 (Part 1 of 5). Parietal bone Frontal bone Occipital bone Mandible Intramembranous ossification starts about the eighth week of embryonic development. This type of ossification occurs in the deeper layers of the dermis, forming dermal bones. © 2015 Pearson Education, Inc. 1 Mesenchymal cells cluster together, differentiate into osteoblasts, and start to secrete the organic components of the matrix. The resulting osteoid then becomes mineralized with calcium salts forming bone matrix. Bone matrix Osteoid Mesenchymal cell Ossification center Blood vessel Osteoblast Also called dermal ossification because it occurs in the dermis produces dermal bones such as mandible (lower jaw) and clavicle (collarbone)
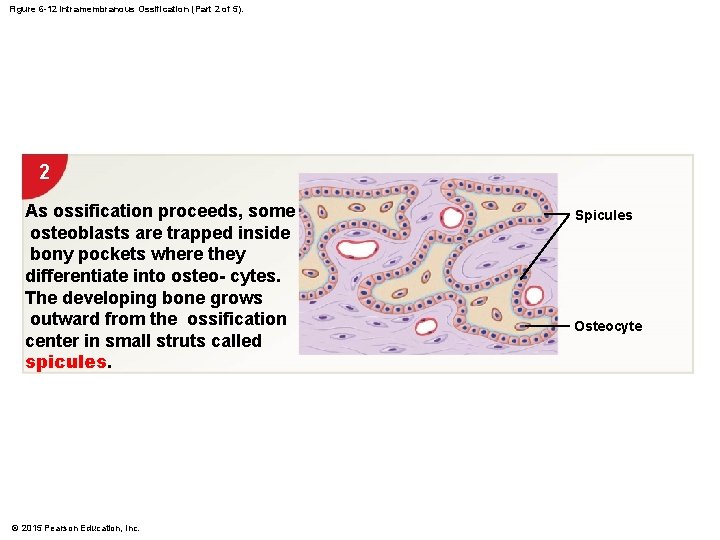
Figure 6 -12 Intramembranous Ossification (Part 2 of 5). 2 As ossification proceeds, some osteoblasts are trapped inside bony pockets where they differentiate into osteo- cytes. The developing bone grows outward from the ossification center in small struts called spicules. © 2015 Pearson Education, Inc. Spicules Osteocyte
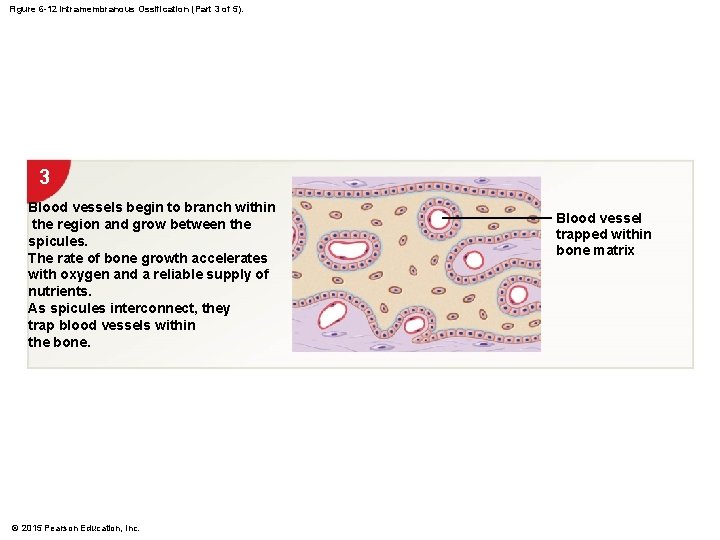
Figure 6 -12 Intramembranous Ossification (Part 3 of 5). 3 Blood vessels begin to branch within the region and grow between the spicules. The rate of bone growth accelerates with oxygen and a reliable supply of nutrients. As spicules interconnect, they trap blood vessels within the bone. © 2015 Pearson Education, Inc. Blood vessel trapped within bone matrix
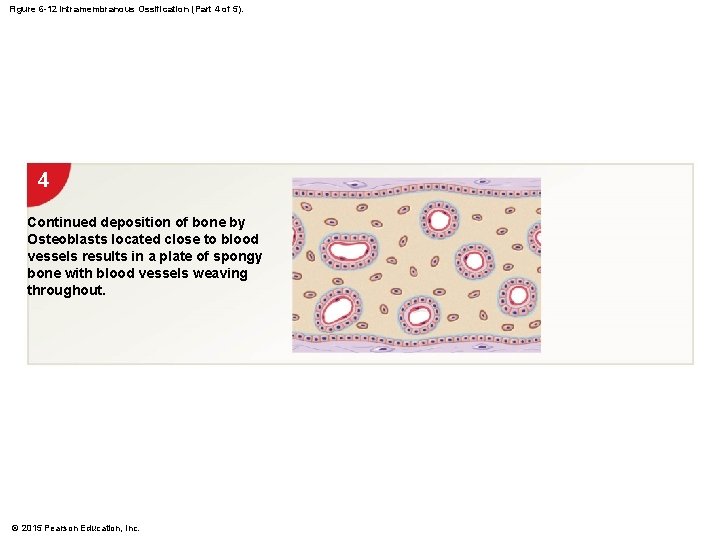
Figure 6 -12 Intramembranous Ossification (Part 4 of 5). 4 Continued deposition of bone by Osteoblasts located close to blood vessels results in a plate of spongy bone with blood vessels weaving throughout. © 2015 Pearson Education, Inc.
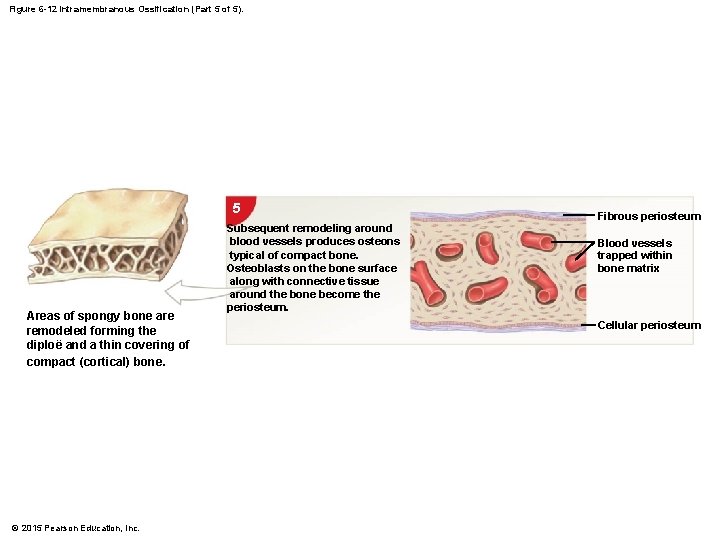
Figure 6 -12 Intramembranous Ossification (Part 5 of 5). 5 Areas of spongy bone are remodeled forming the diploë and a thin covering of compact (cortical) bone. © 2015 Pearson Education, Inc. Subsequent remodeling around blood vessels produces osteons typical of compact bone. Osteoblasts on the bone surface along with connective tissue around the bone become the periosteum. Fibrous periosteum Blood vessels trapped within bone matrix Cellular periosteum
6 -5 Bone Formation and Growth • Blood Supply of Mature Bones 1. Nutrient artery and vein • A single pair of large blood vessels • Enter the diaphysis through the nutrient foramen • Femur has more than one pair 2. Metaphyseal vessels • Supply the epiphyseal cartilage • Where bone growth occurs 3. Periosteal vessels • Blood to superficial osteons • Secondary ossification centers © 2015 Pearson Education, Inc.
6 -5 Bone Formation and Growth • Lymph and Nerves • The periosteum also contains: • Networks of lymphatic vessels • Sensory nerves • Process of Remodeling • The adult skeleton: • Maintains itself • Replaces mineral reserves • Recycles and renews bone matrix © 2015 Pearson Education, Inc.

6 -6 Bone Remodeling Process of Remodeling • Bone continually remodels, recycles, and replaces • Turnover rate varies: 1. If deposition is greater than removal, bones get stronger 2. If removal is faster than replacement, bones get weaker © 2015 Pearson Education, Inc.

6 -7 Exercise, Hormones, and Nutrition • Normal Bone Growth and Maintenance Depend on Nutritional and Hormonal Factors • A dietary source of calcium and phosphate salts • Plus small amounts of magnesium, fluoride, iron, and manganese • The hormone calcitriol • Made in the kidneys • Helps absorb calcium and phosphorus from digestive tract • Synthesis requires vitamin D 3 (cholecalciferol © 2015 Pearson Education, Inc.

6 -7 Exercise, Hormones, and Nutrition • Vitamin C is required for collagen synthesis and stimulation of osteoblast differentiation • Vitamin A stimulates osteoblast activity • Vitamins K and B 12 help synthesize bone proteins © 2015 Pearson Education, Inc.

6 -7 Exercise, Hormones, and Nutrition • Normal Bone Growth and Maintenance Depend on Nutritional and Hormonal Factors • Growth hormone and thyroxine stimulate bone growth • Estrogens androgens stimulate osteoblasts • Calcitonin and parathyroid hormone regulate calcium and phosphate levels © 2015 Pearson Education, Inc.

6 -8 Calcium Homeostasis • The Skeleton as a Calcium Reserve • Bones store calcium and other minerals • Calcium is the most abundant mineral in the body • Calcium ions are vital to: • Membranes • Neurons • Muscle cells, especially heart cells © 2015 Pearson Education, Inc.
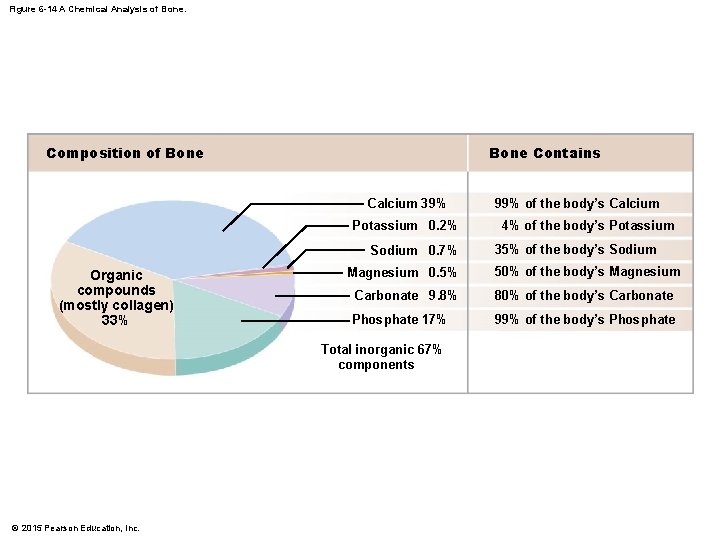
Figure 6 -14 A Chemical Analysis of Bone. Composition of Bone Contains Calcium 39% Potassium 0. 2% Sodium 0. 7% Organic compounds (mostly collagen) 33% 4% of the body’s Potassium 35% of the body’s Sodium Magnesium 0. 5% 50% of the body’s Magnesium Carbonate 9. 8% 80% of the body’s Carbonate Phosphate 17% 99% of the body’s Phosphate Total inorganic 67% components © 2015 Pearson Education, Inc. 99% of the body’s Calcium

6 -8 Calcium Homeostasis Calcium Regulation • Calcium ions in body fluids must be closely regulated • Homeostasis is maintained: By calcitonin and parathyroid hormone (PTH) which control storage, absorption, and excretion © 2015 Pearson Education, Inc.

6 -8 Calcium Homeostasis Calcitonin and Parathyroid Hormone Control • Affect: 1. Bones: Where calcium is stored 2. Digestive tract: Where calcium is absorbed 3. Kidneys: Where calcium is excreted © 2015 Pearson Education, Inc.

6 -8 Calcium Homeostasis • Parathyroid Hormone (PTH): Produced by parathyroid glands in neck • Increases calcium ion levels by: 1. Stimulating osteoclasts 2. Increasing intestinal absorption of calcium 3. Decreasing calcium excretion at kidneys • Calcitonin: Secreted by C cells (parafollicular cells) in thyroid • Decreases calcium ion levels by: 1. Inhibiting osteoclast activity 2. Increasing calcium excretion at kidneys © 2015 Pearson Education, Inc.
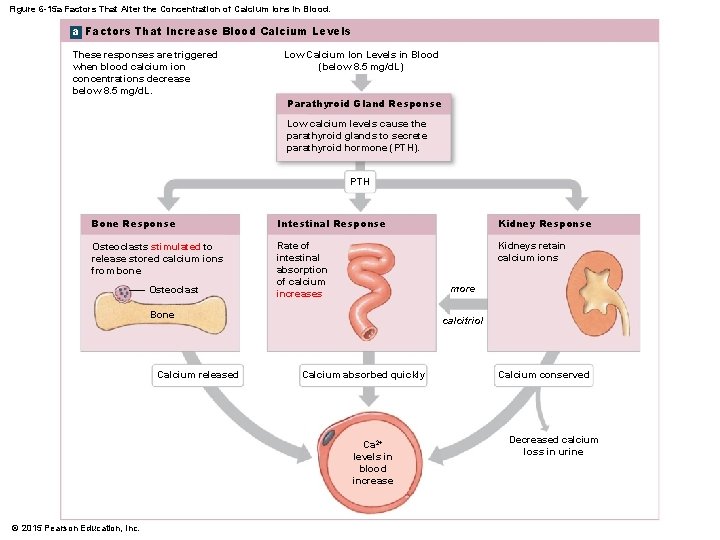
Figure 6 -15 a Factors That Alter the Concentration of Calcium Ions in Blood. a Factors That Increase Blood Calcium Levels These responses are triggered when blood calcium ion concentrations decrease below 8. 5 mg/d. L. Low Calcium Ion Levels in Blood (below 8. 5 mg/d. L) Parathyroid Gland Response Low calcium levels cause the parathyroid glands to secrete parathyroid hormone (PTH). PTH Bone Response Intestinal Response Kidney Response Osteoclasts stimulated to release stored calcium ions from bone Rate of intestinal absorption of calcium increases Kidneys retain calcium ions Osteoclast more Bone Calcium released calcitriol Calcium absorbed quickly Ca 2+ levels in blood increase © 2015 Pearson Education, Inc. Calcium conserved Decreased calcium loss in urine
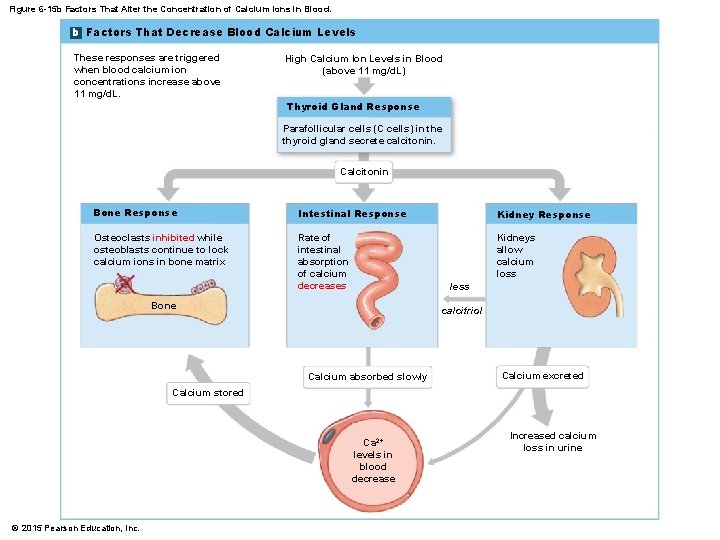
Figure 6 -15 b Factors That Alter the Concentration of Calcium Ions in Blood. b Factors That Decrease Blood Calcium Levels These responses are triggered when blood calcium ion concentrations increase above 11 mg/d. L. High Calcium Ion Levels in Blood (above 11 mg/d. L) Thyroid Gland Response Parafollicular cells (C cells) in the thyroid gland secrete calcitonin. Calcitonin Bone Response Intestinal Response Kidney Response Osteoclasts inhibited while osteoblasts continue to lock calcium ions in bone matrix Rate of intestinal absorption of calcium decreases Kidneys allow calcium loss less Bone calcitriol Calcium absorbed slowly Calcium excreted Calcium stored Ca 2+ levels in blood decrease © 2015 Pearson Education, Increased calcium loss in urine

6 -9 Fractures • Cracks or breaks in bones • Caused by physical stress • Fractures are repaired in four steps 1. Bleeding 2. Cells of the endosteum and periosteum 3. Osteoblasts 4. Osteoblasts and osteocytes remodel the fracture for up to a year © 2015 Pearson Education, Inc.

6 -9 Fractures • Bleeding • Produces a clot (fracture hematoma) • Establishes a fibrous network • Bone cells in the area die • Cells of the endosteum and periosteum • Divide and migrate into fracture zone • Calluses stabilize the break • External callus of cartilage and bone surrounds break • Internal callus develops in medullary cavity © 2015 Pearson Education, Inc.

6 -9 Fractures • Osteoblasts • Replace central cartilage of external callus • With spongy bone • Osteoblasts and osteocytes remodel the fracture for up to a year • Reducing bone calluses (new tissue formed over a wound) © 2015 Pearson Education, Inc.
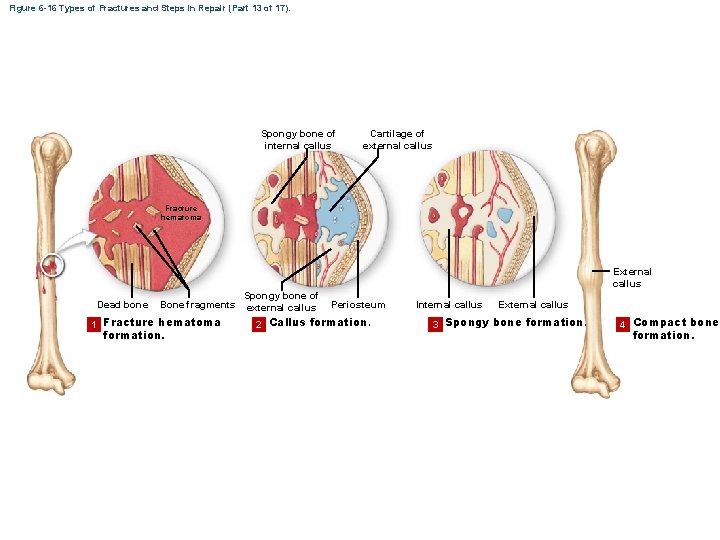
Figure 6 -16 Types of Fractures and Steps in Repair (Part 13 of 17). Spongy bone of internal callus Cartilage of external callus Fracture hematoma External callus Dead bone Bone fragments 1 Fracture hematoma formation. Spongy bone of external callus Periosteum 2 Callus formation. Internal callus External callus 3 Spongy bone formation. 4 Compact bone formation.

6 -9 Fractures • Major Types of Fractures • • • Transverse fractures Displaced fractures Compression fractures Spiral fractures Epiphyseal fractures Comminuted fractures Greenstick fractures Colles fractures Pott’s fractures © 2015 Pearson Education, Inc.
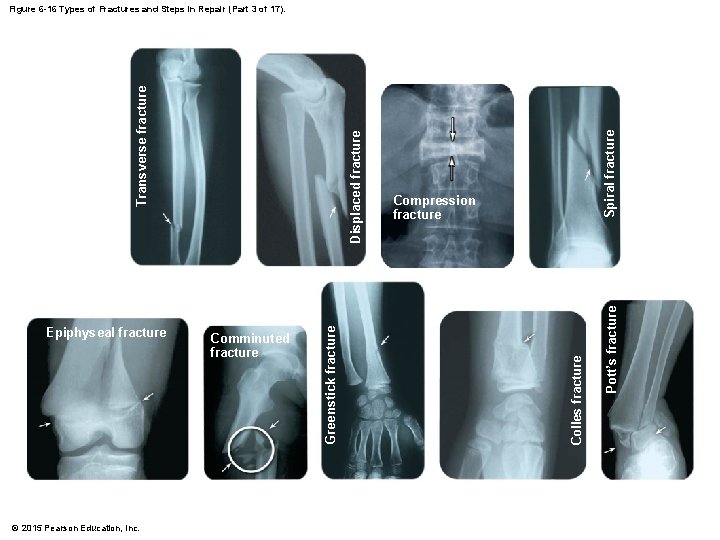
© 2015 Pearson Education, Inc. Spiral fracture Pott’s fracture Compression fracture Colles fracture Comminuted fracture Greenstick fracture Epiphyseal fracture Displaced fracture Transverse fracture Figure 6 -16 Types of Fractures and Steps in Repair (Part 3 of 17).

6 -10 Effects of Aging on the Skeletal System • Age-Related Changes • Bones become thinner and weaker with age • Osteopenia begins between ages 30 and 40 • Women lose 8 percent of bone mass per decade; men lose 3 percent • The epiphyses, vertebrae, and jaws are most affected • Resulting in fragile limbs • Reduction in height • Tooth loss © 2015 Pearson Education, Inc.

6 -10 Effects of Aging on the Skeletal System • Osteoporosis • Severe bone loss • Affects normal function • Over age 45, occurs in: • 29 percent of women • 18 percent of men © 2015 Pearson Education, Inc.
- Slides: 75