Chapter 6 Drug Toxicity Adverse drug reactions Paracelsus







![• Population distribution curve sometimes becomes bimodal or multimodal, e. g. [ isoniazid] • Population distribution curve sometimes becomes bimodal or multimodal, e. g. [ isoniazid]](https://slidetodoc.com/presentation_image_h/b78b2c91c65a9e56fe60a594cef7ef89/image-13.jpg)






![elderly (cont. ) • Vd of fat soluble drug e. g. valium [valium] in elderly (cont. ) • Vd of fat soluble drug e. g. valium [valium] in](https://slidetodoc.com/presentation_image_h/b78b2c91c65a9e56fe60a594cef7ef89/image-20.jpg)











![• Recent teratogenes – isotretoin [for acne] and etretinate [for psoriasis]synthetic retinoids (vitamin • Recent teratogenes – isotretoin [for acne] and etretinate [for psoriasis]synthetic retinoids (vitamin](https://slidetodoc.com/presentation_image_h/b78b2c91c65a9e56fe60a594cef7ef89/image-37.jpg)











- Slides: 48

Chapter 6 Drug Toxicity • Adverse drug reactions • Paracelsus, a Swiss physician ( 1493 -1541), proposed dose -toxicity relationship“all substances are poisons; there is none which is not a poison. The right dose differentiates a poison and remedy” • Dose-related and Non-dose related • genetic makeup, age, underlying pathology, status of immune system.

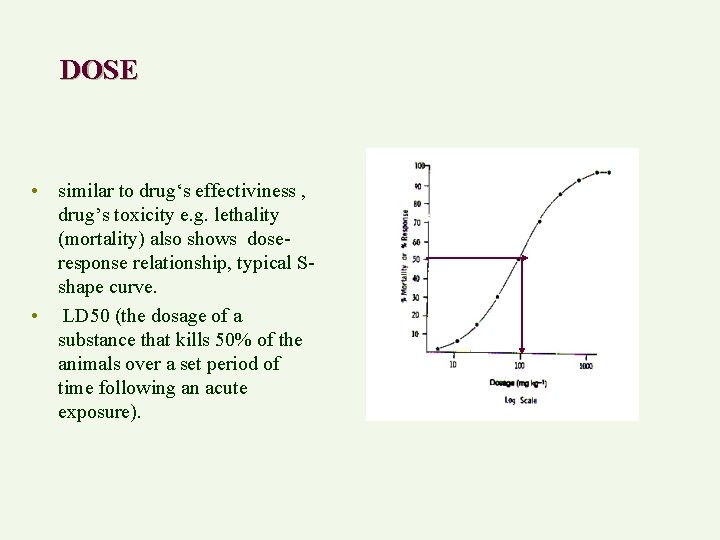
DOSE • similar to drug‘s effectiviness , drug’s toxicity e. g. lethality (mortality) also shows doseresponse relationship, typical Sshape curve. • LD 50 (the dosage of a substance that kills 50% of the animals over a set period of time following an acute exposure).

Therapeutic index (TI)= LD 50/ED 50 The lower TI, the smaller the margin of safety, e. g. digoxin, 2. 0

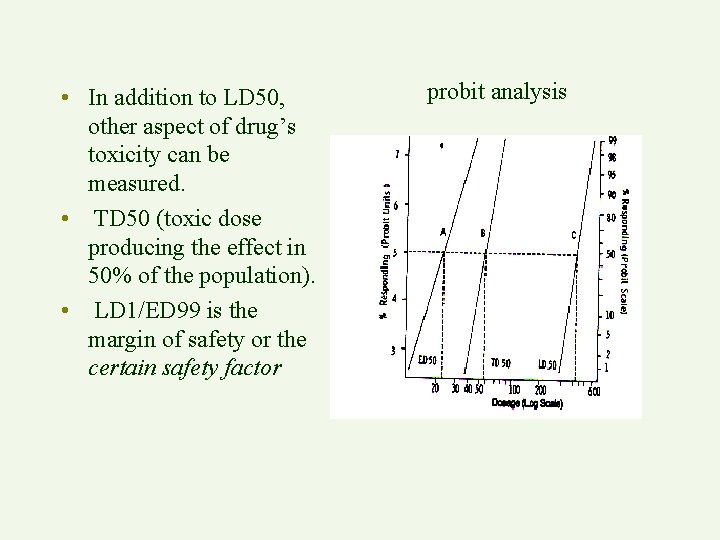
• In addition to LD 50, other aspect of drug’s toxicity can be measured. • TD 50 (toxic dose producing the effect in 50% of the population). • LD 1/ED 99 is the margin of safety or the certain safety factor probit analysis

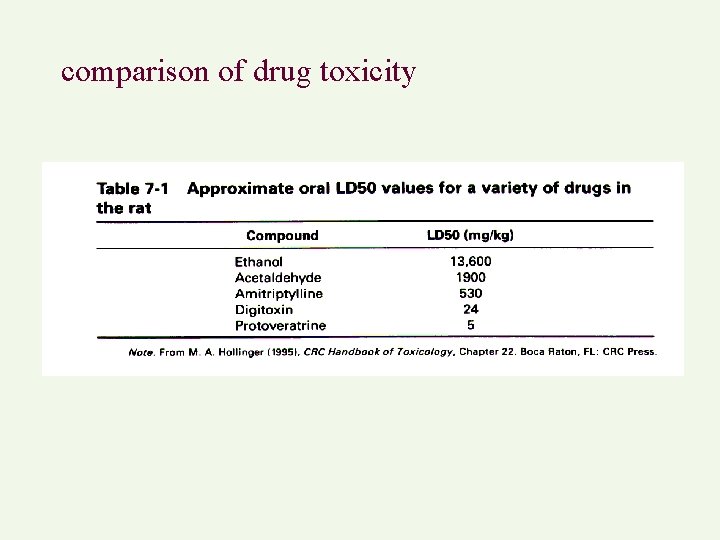
comparison of drug toxicity

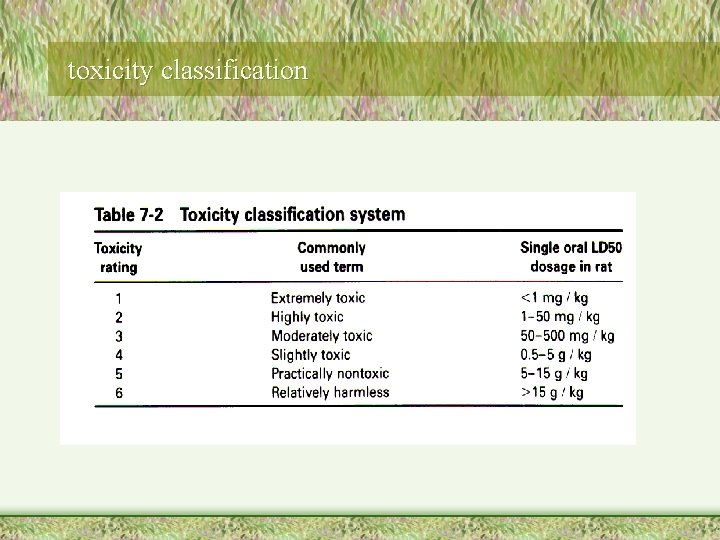
toxicity classification

• cautions – based on lethality alone, false sense, – other toxicity ignored, e. g. thalidomide could be classified as slightly toxic – extrapolation, animal species differences, uncertain for human

Evaluating the toxicity: time factor • Acute basis over a 14 -d period, • subchronic /subacute, 90 -d period (daily given), additional information gained, target organ, major toxic effects, slower onset, • chronic , life time of animal, post-mortem examination. • Story on an antiviral drug for hepatitis- a delayed toxic reaction occurred after administration was discontinued. 5/5 died suddenly, liver failure.

Important factors in these tests: Selections of dosages, species, strain of animal, rout of exposure

Other types of toxicity tests • Specific tests: – reproductive studies, effect of a drug on the reproductive process – mutagenicity test: genetic damage, – carcinogencity test: neoplastic change, – skin sensitization test: drug’s irritancy • The test should be carried out in compliance for Good Laboratory Practice (GLP) for drug approval

GENETICS • Other than dose, factor that influence the body response to drugs: idiosyncratic (occurring for no known reason) • affects pharmacodynamic and pharmacokinetic, e. g. normal difference within a species, between genders and strains, also, ‘abnormal’ genetic expression occurs – disparate response of different species to a drug: e. g. LD 50 of ipomeanol, rat- 12 mg/kg, hamster- 140 mg/kg; – thalidomide, rat- insensitive, New Zealand white rabbits -sensitive; – strain difference, hexobarbital, sleeping time, A/NC 48 min, SWR/He. N- 18 min

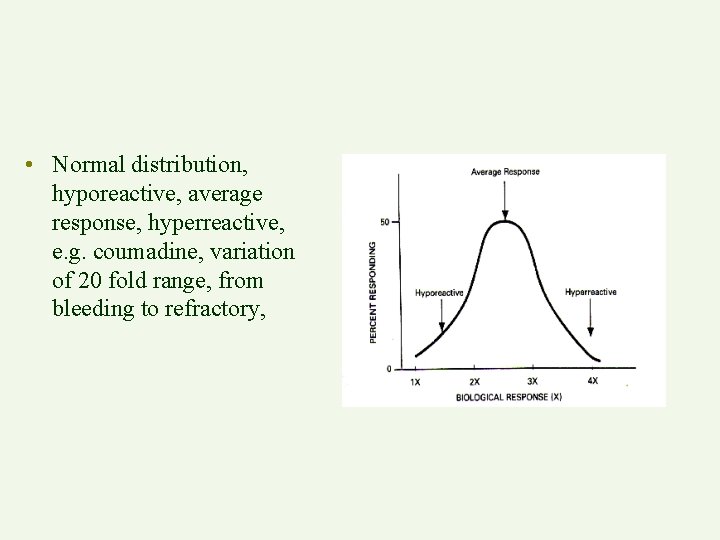
• Normal distribution, hyporeactive, average response, hyperreactive, e. g. coumadine, variation of 20 fold range, from bleeding to refractory,
![Population distribution curve sometimes becomes bimodal or multimodal e g isoniazid • Population distribution curve sometimes becomes bimodal or multimodal, e. g. [ isoniazid]](https://slidetodoc.com/presentation_image_h/b78b2c91c65a9e56fe60a594cef7ef89/image-13.jpg)
• Population distribution curve sometimes becomes bimodal or multimodal, e. g. [ isoniazid] in plasma, statistically separated populations, left and right are fast and slow metabolizers, respectively.

Primaquine sensitivity • Another genetically predisposed toxic reaction to drug • Primaquine (an antimalarial drug) or other oxidant drugs, hemolytic anemia, X chromosome genetic alteration , G 6 PDH (glucose 6 -phosphate dehydrogenase) paucity in erythrocytes • G 6 P + G 6 PDH 6 -phosphogluconolactone + NADPH 2 NADPH + GSSG 2 GSH + 2 NADP, • fail to replenish NADPH and GSH red blood cells damage • [G 6 PDH] in erythrocytes, trimodal distribution - 1. normal; 2. female carrier (heterozygous); 3. male carrier,

Succinylcholine apnea • Another example of “abnormal” gene expression • Succinylcholine (muscle relaxant, reduce skeletal muscle rigidity during operation), • normal duration of action is of minutes; people with the atypical enzyme : hrs, abnormal duration, atypical serum cholinestrase, • dibucaine number : an assay for the atypical enzyme carrier, benzoylcholine (substrate), dibucaine (competitor), % inhibition of benzoylcholine hydrolysis • trimodal distribution (20, 60 and 80% inhibition), in carriers, less inhibition,

GENDER • ethanol consumption, first-pass metabolism, in female LDH lower, • dinitrotoluene-induced hepatic tumor, higher incidence in male: male glucuronide conjugation, biliary excretion, hydrolyzed and reabsorption; urinary excretion predominates in female better clearance; • chloroform-induced kidney damage, higher incidence in male : androgen effect, testosterone-mediated, castration diminished

AGE • age related change: 1. liver metabolism; 2. renal elimination; 3. body composition • liver metabolism- less amount of drug metabolizing enzymes in newborn infants. – Therapeutic disorders • (1) gray baby syndrome : inadequate glucuronidation of chloramphenicol [chloramphenicol] • (2) sulfonamide induced kericterus: displacement of bilirubin from plasma by sulfonamide; In general, reduced binding of drug to plasma proteins in neonatal period.

• Examples of paradoxical pharmacodynamic differences. antihistamine / barbiturates: sedation in adults, hyperexcitation in children differences in receptor-mediated signal transudction • renal function- lower in neonates, blood flow approx. 8 folds during 1 -2 y of birth, development of glomerulus, GFR during first several weeks of life antibiotic (e. g. getamicin) half-life , clearance rate .

In elderly (geriatric pharmacology) • Declined physiological function during aging process, • total body water , liver mass , blood flow , % body fate , • after 40 y, liver mass 1% / y, after 30 y, cardiac output 1% /y, • Vd of water soluble drug , e. g. acetaminophen, alcohol, digoxin; drug sensitivity because of [drugs]
![elderly cont Vd of fat soluble drug e g valium valium in elderly (cont. ) • Vd of fat soluble drug e. g. valium [valium] in](https://slidetodoc.com/presentation_image_h/b78b2c91c65a9e56fe60a594cef7ef89/image-20.jpg)
elderly (cont. ) • Vd of fat soluble drug e. g. valium [valium] in serum , but because of pharmacodynamic change Valium depression • serum albumin , affecting protein bound drugs, highly protein bound drugs, e. g. sulfonylurea (an oral hypoglycemic drug) any drug displaces the drug may lead to toxicity • Pharmacodynamic response change, e. g. b-receptor; b agonists sensitivity , may be due to c-AMP

ALLERGY • not follow dose-response relationship • e. g. chronic beryllium disease, hypersensitivity lung disorder, exposure to beryllium, lack of dose-response relationship

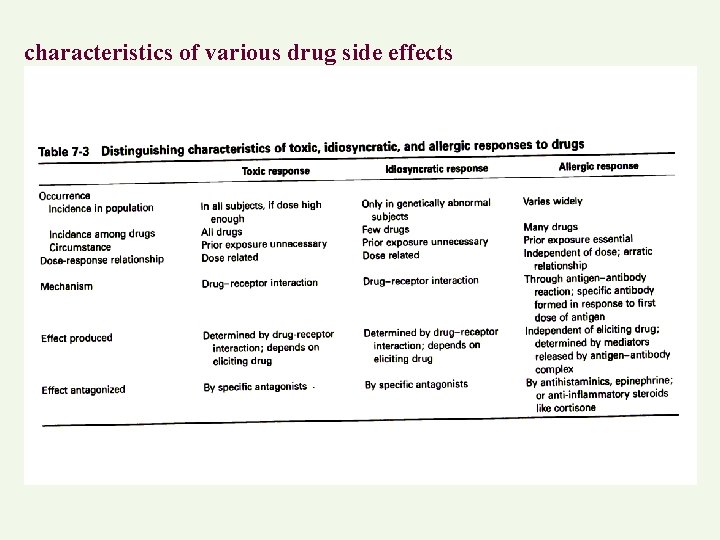
characteristics of various drug side effects

• allergic reactions, immune response • antigens of large molecules; drugs only of 250 -500 daltons, carrier proteins, hapten -an antigenic determinant ( epitope). – e. g. penicillin, penicilloyl groups, initial exposure, 7 -10 d, period of sensitization.


Various types of allergic reactions • Type I. Immediate immune response, Ig. E fixed mast cells and basophiles, Ig. E-hapten-protein complex • release of mediators (e. g. histamine, heparin and tryptase and leutotrienes, prostaglandins and cytokines) • bronchiolar constriction, capillary dilation or urticaria, severe episode-life threatening anaphylaxis

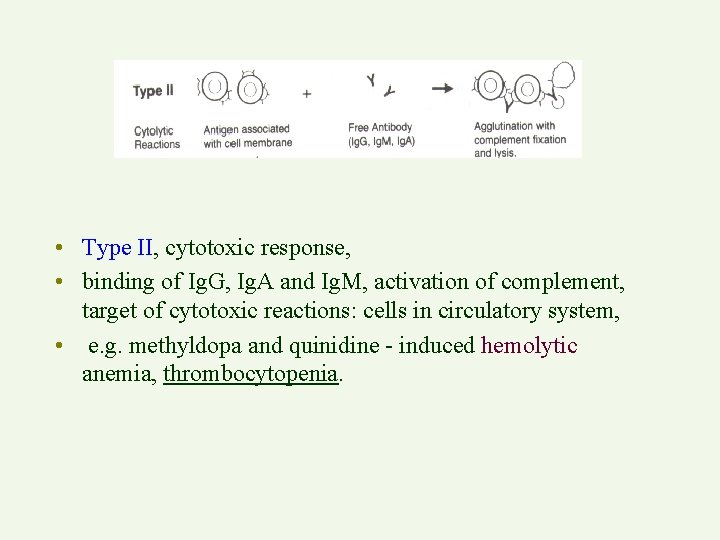
• Type II, cytotoxic response, • binding of Ig. G, Ig. A and Ig. M, activation of complement, target of cytotoxic reactions: cells in circulatory system, • e. g. methyldopa and quinidine - induced hemolytic anemia, thrombocytopenia.

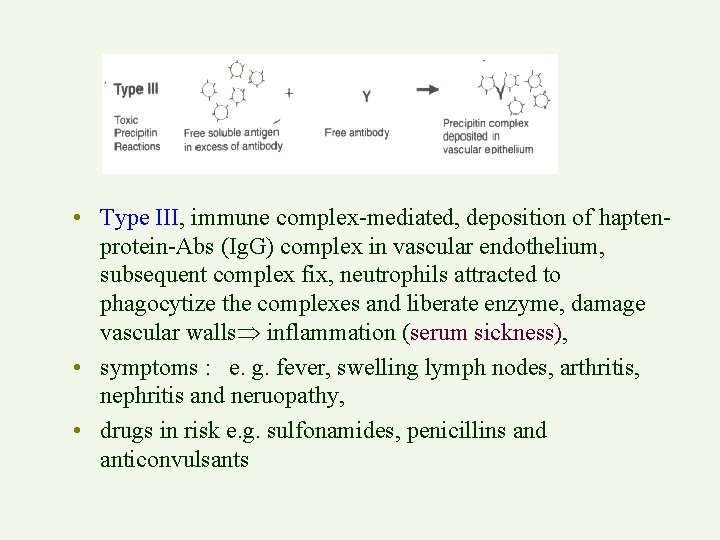
• Type III, immune complex-mediated, deposition of haptenprotein-Abs (Ig. G) complex in vascular endothelium, subsequent complex fix, neutrophils attracted to phagocytize the complexes and liberate enzyme, damage vascular walls inflammation (serum sickness), • symptoms : e. g. fever, swelling lymph nodes, arthritis, nephritis and neruopathy, • drugs in risk e. g. sulfonamides, penicillins and anticonvulsants

• Type IV, cell-mediated response, – delayed reaction to the Ag , activated T-lymphocytes generated, release lymphokines activate macrophages neutrophiles, infiltration of these cells into organ, e. g. halothane-induced hepatitis

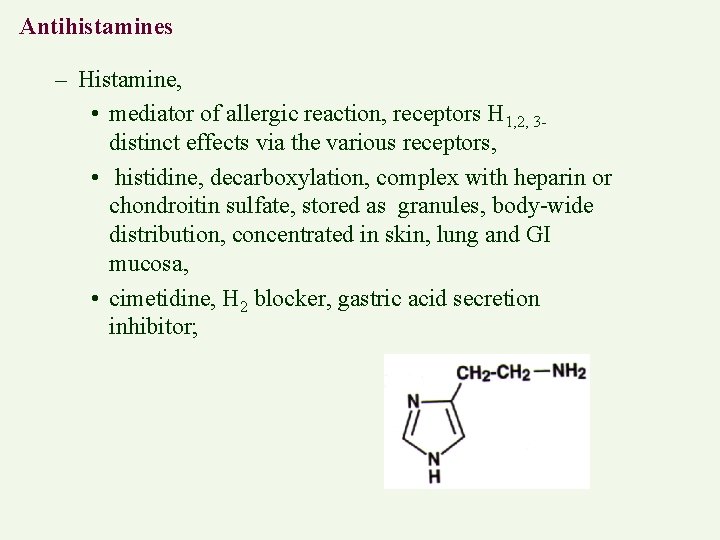
Antihistamines – Histamine, • mediator of allergic reaction, receptors H 1, 2, 3 distinct effects via the various receptors, • histidine, decarboxylation, complex with heparin or chondroitin sulfate, stored as granules, body-wide distribution, concentrated in skin, lung and GI mucosa, • cimetidine, H 2 blocker, gastric acid secretion inhibitor;

– Antihistamine : referred to H 1 antagonist anti- ( urticaria, hay fever, insect bites) – antiemetic, anti-motion sickness, antiparkinsonism, antitussive, – old generation of antihistamines have side effects [blocker of cholinergic muscarinic receptor]: sedation ( used in OTC sleeping pills)

Immune-related drug effects – glucocorticoids or azathioprine (prevent organ rejection), tumor incidence – others modifying the antigenic properties of endogenous molecules without binding, e. g. , hydralazine [antihypertensive] induce autoimmune e. g. SLE disorder

Primary mechanisms of direct drug-induced cell injury • biochemical lesion: initial metabolic alteration morphological change – (1) covalent binding – (2) lipid peroxidation – (3) oxidative stress

• Covalent binding – bioactivation, covalent bonds with endogenous macromolecules e. g. halothane [anesthetic], 2 types hepatotoxicity: one is direct cytotoxicity, the other is immune-related, – another example acetaminophen, oxidation product NAPQI [N-acetyl-p-benzoquinoneimine], conjugation with GSH, overdose, Phase II enzymes saturated, covalent linked with proteins e. g. p 58 (sensor for homeostasis); immune-related response may occur also.

• Lipid peroxidation – free radical, electrophilic species, O 2 superoxide anion, polyunsaturated fatty acids in membrane undergo lipid peroxidation cellular injury

• Oxidative stress – superoxide anion radical, hydrogen peroxide, enzymes to clear the reactive oxygen species: superoxide dismutase, catalase, peroxidase – oxidation stress depletion of cellular reducing agents (e. g. thiols, and NADP/NADPH) can lead to cell necrosis or apoptosis

• Teratogenesis – thalidomide- effects on development of embryo, – alcohol- CNS dysfunction: mental retardation, longlasting effects – diethylstibestrol (was used for miscarriage prevention)carcinogenesis, cervical and vaginal carcinoma found in daughters of treated mothers • Sadly, DES did not prove efficacious in miscarriage prevention
![Recent teratogenes isotretoin for acne and etretinate for psoriasissynthetic retinoids vitamin • Recent teratogenes – isotretoin [for acne] and etretinate [for psoriasis]synthetic retinoids (vitamin](https://slidetodoc.com/presentation_image_h/b78b2c91c65a9e56fe60a594cef7ef89/image-37.jpg)
• Recent teratogenes – isotretoin [for acne] and etretinate [for psoriasis]synthetic retinoids (vitamin A deriv. ) – isotretoin-category X [contraindication for use during pregnancy]; physicians unnoticed the warning label until the problem broke out. – etretinate- serum concentration may last long 2 years, extended period of toxicity

• Bendectin story – antinausea – a report 1979 concerned bendectin’s 80% increase of risk in congenital effects of heart disease – 1983, removed from market by the company – further studies only 0. 89% risk – hospital admission due to excessive vomiting

Treating Drug Overdose • Drug responsible for poisonings: analgesic, antidepressants, sedative/hypnotics, stimulants and street drugs • American Association of Poison Control Centers, ingestion the most likely route (75%): accidental or intentional

• Aspirin – before 1972, aspirin the most frequent in childpoisioning – Poison prevention packaging act, 1970, childrenresistant closures – numbers of death (1972 1989) from 46 to 2

• Iron supplements – iron deficiency anemia – FDA required : iron tablets wrapped and capsules individually, time and dexterity discouraging young child

• Age-related drug poisoning – Intentional poisoning in adolescents (11 -17) – elderly: 64 y older, dementia and confusion, improper use or storage, serum albumin and GFR , drug displacement

• Management trends – initial decontamination; – enhanced elimination; – specific antidote administration

• Initial decontamination – Ipecac syrup, chemoreceptor trigger zone in brain, local irritation of GI tract (gastric lavage ), contraindications with coma or convulsions, ingestion of corrosive substances, impaired gag reflex, – followed by activated charcoal, high adsorptive capacity, 60% if simultaneous administration, 9% if 3 h delay

• Enhanced elimination- facilitated renal excretion or extracorporeal methods – facilitated renal excretion: fluid diuresis, excess fluid, ionized diuresis, or urine p. H – extracorporeal methods -dialysis or hemoperfussion for coma

• Specific antidote administration – Naloxone competes for m and k opoid receptors, reverse sedation and respiratory depression of morphine-like drugs – N-aceylcysteine (NAC) e. g. acetaminophen overdose, provides -SH groups – deferoxamine- for iron poisoning, an chelator – Ab e. g. digoxin-specific Fab antibody

The single most important treatment of poisoned patients is supportive care. You must treat patient not the poison

11/5 mid-term exam, covering the first 4 lectures