Chapter 6 Biopotential Amplifiers From J G Webster

Chapter 6 Biopotential Amplifiers © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

6. 6 Amplifiers for other biopolential signals © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
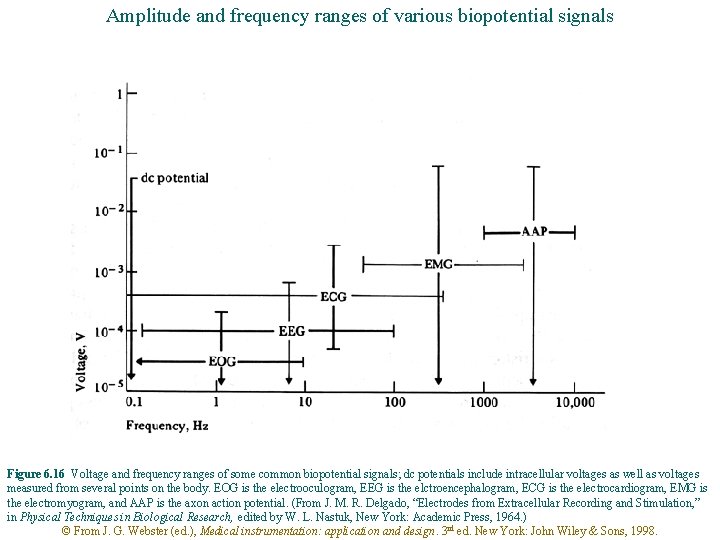
Amplitude and frequency ranges of various biopotential signals Figure 6. 16 Voltage and frequency ranges of some common biopotential signals; dc potentials include intracellular voltages as well as voltages measured from several points on the body. EOG is the electrooculogram, EEG is the elctroencephalogram, ECG is the electrocardiogram, EMG is the electromyogram, and AAP is the axon action potential. (From J. M. R. Delgado, “Electrodes from Extracellular Recording and Stimulation, ” in Physical Techniques in Biological Research, edited by W. L. Nastuk, New York: Academic Press, 1964. ) © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

EMG Amplifiers * Signal frequency: 25 Hz to several kilohertz * Signal amplitude: 0. 1 -90 m. V (depends on the electrode type) * Less sensitive to motion artifacts Higher lowest frequency range than that of ECG [Using skin-surface electrodes: ] • Signal amplitude: 0. 1 -1 m. V • Eletrode impedance: 200 to 5000 Ω (low) requires about the same input characteristics as those of the ECG amplifier [Using intramuscular needle electrodes: ] • Signal amplitude: stronger • Electrode impedance: higher requires higher amplifier input impedance © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

Amplifiers for intracellular electrodes • Signal amplitude: 50 to 100 m. V • Signal frequency: DC (transmembrane potential) to 10 k. Hz • Electrode impedance (of glass micropipette): very high ( very small contact area) + very large shunting capacitance requires very high amplifier input impedance © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
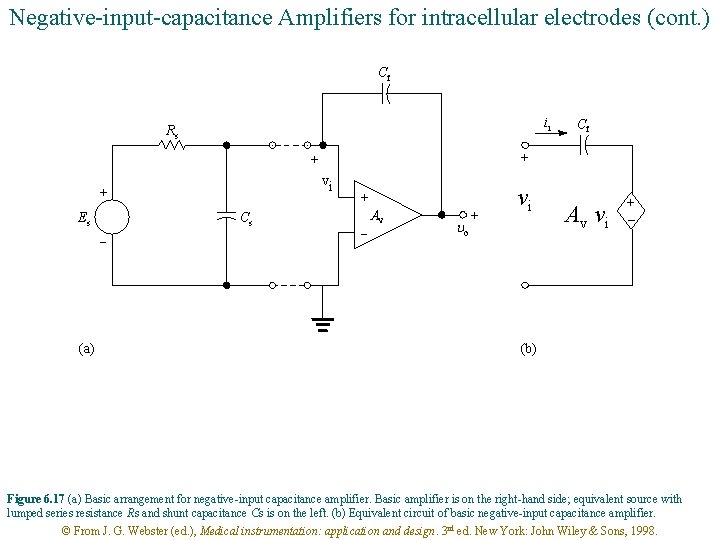
Negative-input-capacitance Amplifiers for intracellular electrodes (cont. ) Cf ii Rs + + vi + Es Cs - (a) Cf + - Av uo + vi Av vi + – (b) Figure 6. 17 (a) Basic arrangement for negative-input capacitance amplifier. Basic amplifier is on the right-hand side; equivalent source with lumped series resistance Rs and shunt capacitance Cs is on the left. (b) Equivalent circuit of basic negative-input capacitance amplifier. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
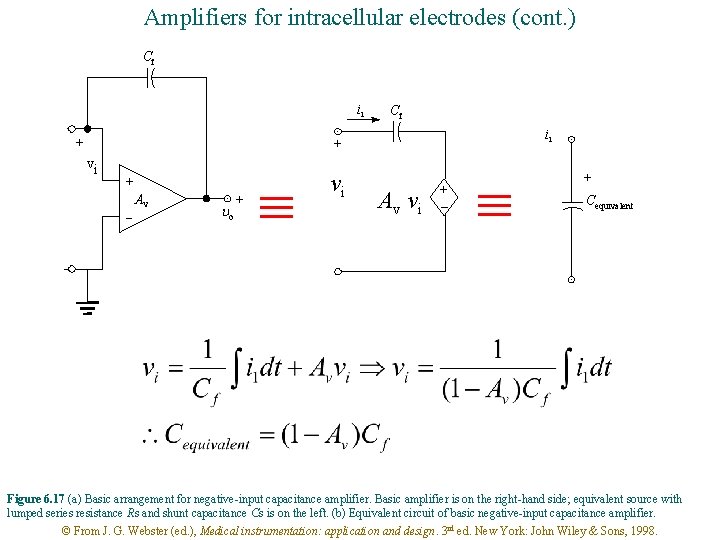
Amplifiers for intracellular electrodes (cont. ) Cf ii + vi + - Av uo + vi Av vi + – + Cequivalent Figure 6. 17 (a) Basic arrangement for negative-input capacitance amplifier. Basic amplifier is on the right-hand side; equivalent source with lumped series resistance Rs and shunt capacitance Cs is on the left. (b) Equivalent circuit of basic negative-input capacitance amplifier. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

Amplifiers for intracellular electrodes (cont. ) Rs ii + + Es Cs Cequivalent - Figure 6. 17 (a) Basic arrangement for negative-input capacitance amplifier. Basic amplifier is on the right-hand side; equivalent source with lumped series resistance Rs and shunt capacitance Cs is on the left. (b) Equivalent circuit of basic negative-input capacitance amplifier. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

EEG amplifiers • Signal frequency: 0. 1 to 100 Hz • Signal amplitude: [using surface electrodes] 25 to 100 V © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

6. 7 Example of a biopotential preamplifier Requirements on preamplifiers: 1. Low noise ------ otherwise will be amplified by the remaining stages 2. Directly coupled to the electrode (No series capacitor) ------- to provide optimal low-frequency response ------- to minimizing charging effects on coupling capacitors from input bias current 3. Low voltage gain ------ to prevent generating large DC offset 4. The preamplifier can have capacitor-coupled to the remaining stages ------ to eleminate the DC offset 5. High input impedance ------- to avoid loading the electrodes © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
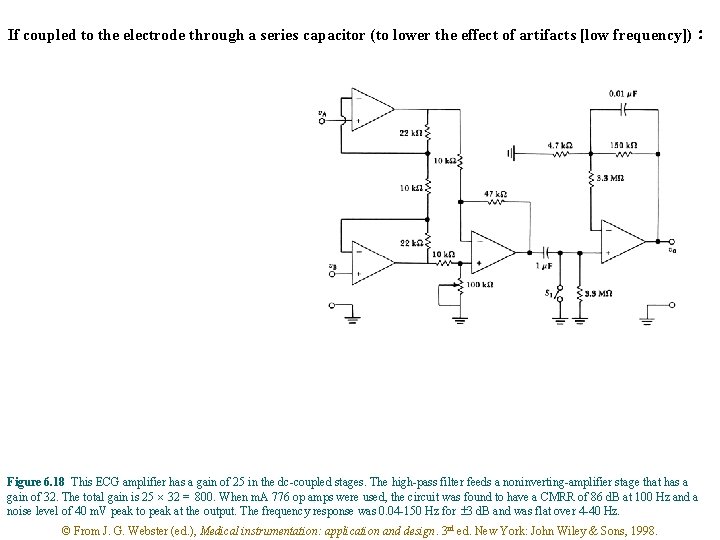
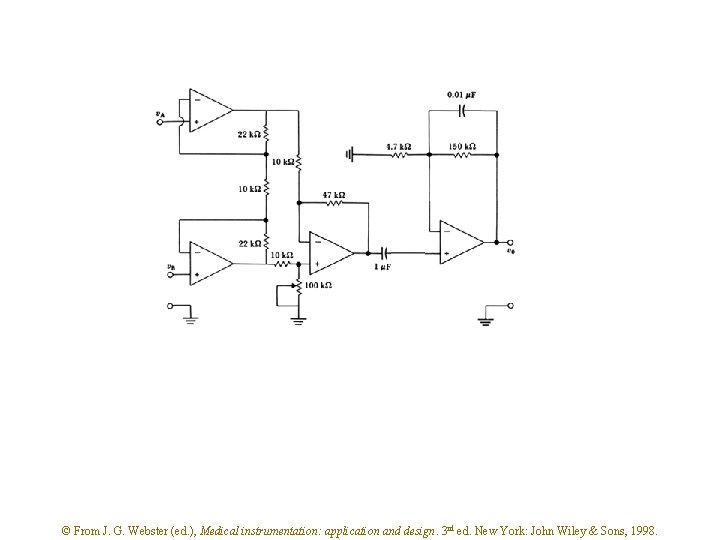
If coupled to the electrode through a series capacitor (to lower the effect of artifacts [low frequency]): Figure 6. 18 This ECG amplifier has a gain of 25 in the dc-coupled stages. The high-pass filter feeds a noninverting-amplifier stage that has a gain of 32. The total gain is 25 32 = 800. When m. A 776 op amps were used, the circuit was found to have a CMRR of 86 d. B at 100 Hz and a noise level of 40 m. V peak to peak at the output. The frequency response was 0. 04 -150 Hz for 3 d. B and was flat over 4 -40 Hz. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
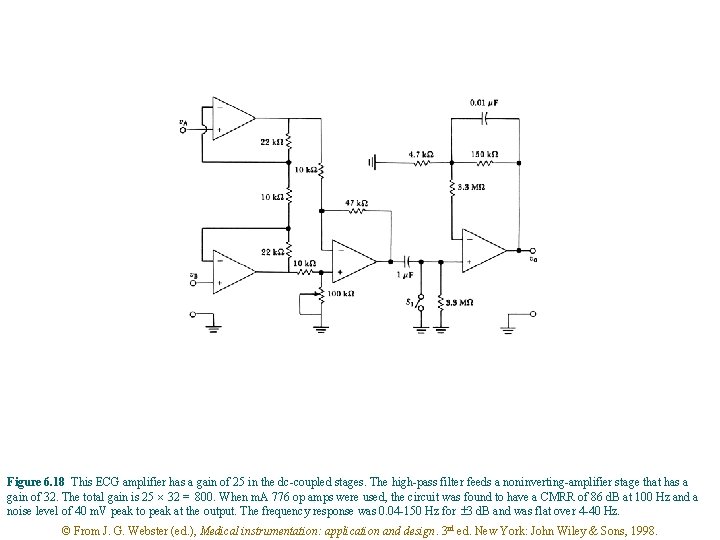
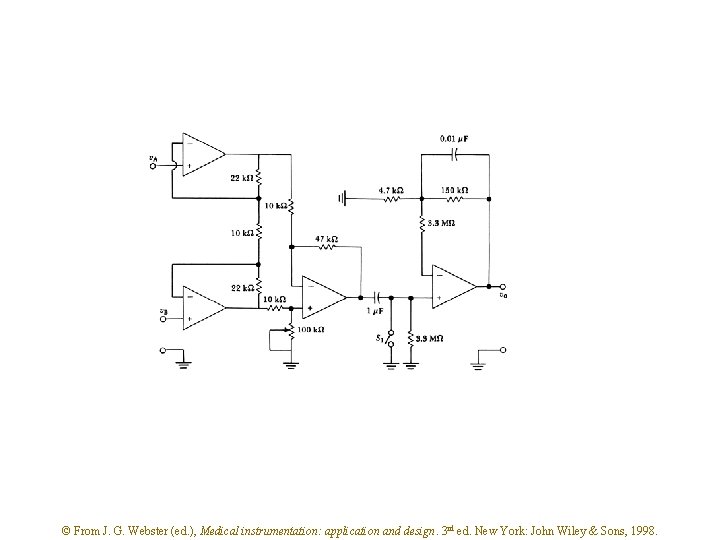
Figure 6. 18 This ECG amplifier has a gain of 25 in the dc-coupled stages. The high-pass filter feeds a noninverting-amplifier stage that has a gain of 32. The total gain is 25 32 = 800. When m. A 776 op amps were used, the circuit was found to have a CMRR of 86 d. B at 100 Hz and a noise level of 40 m. V peak to peak at the output. The frequency response was 0. 04 -150 Hz for 3 d. B and was flat over 4 -40 Hz. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

6. 8 Other biopotential signal processors © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

Cardiotachometer: * Function : to determine the heart rate * Input signal : ECG, arterial pressure, or heart sound * Types : 1) Averaging cardiotachometer ---- counts the heart beat over a period of time 2) Beat-to-beat cardiotachometer ---- determines the time interval between two beats © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
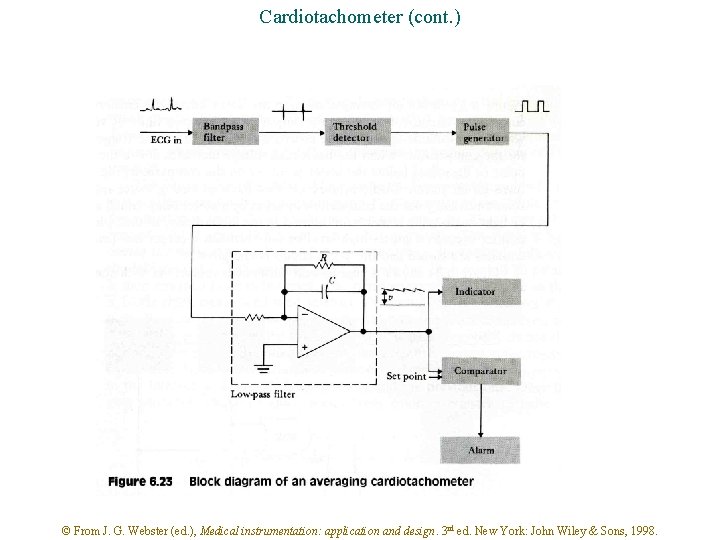
Cardiotachometer (cont. ) © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
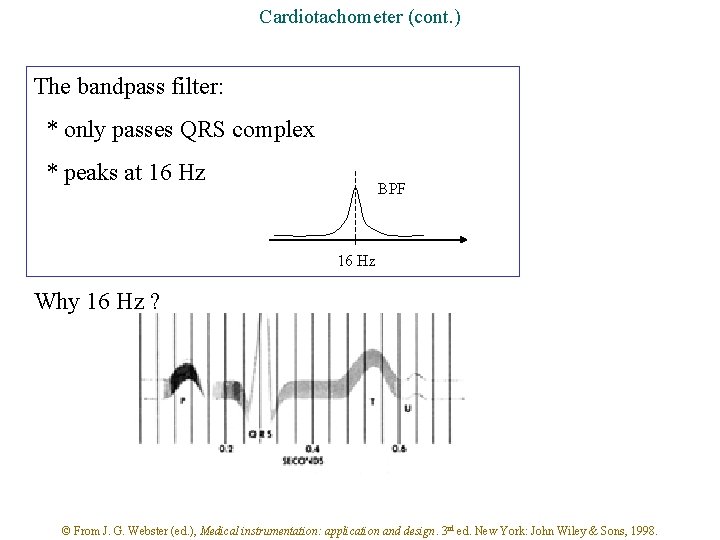
Cardiotachometer (cont. ) The bandpass filter: * only passes QRS complex * peaks at 16 Hz BPF 16 Hz Why 16 Hz ? © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
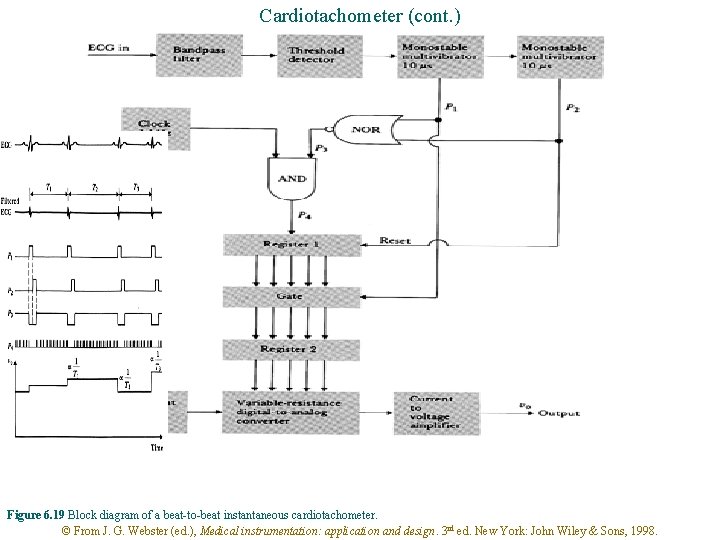
Cardiotachometer (cont. ) Figure 6. 19 Block diagram of a beat-to-beat instantaneous cardiotachometer. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
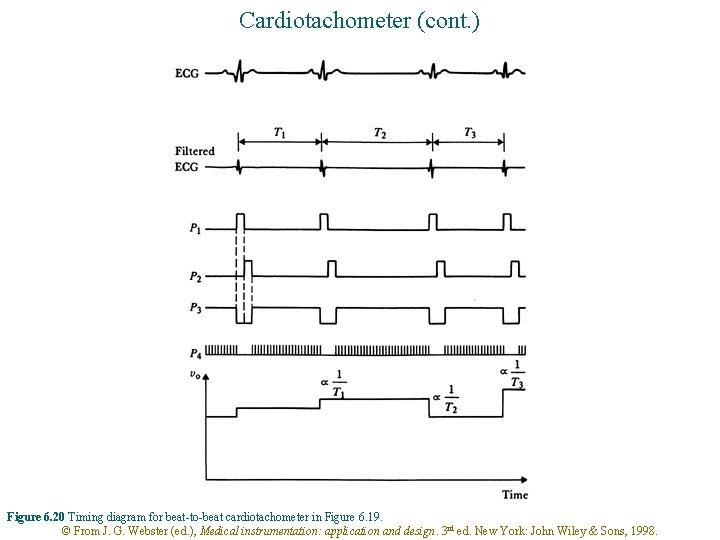
Cardiotachometer (cont. ) Figure 6. 20 Timing diagram for beat-to-beat cardiotachometer in Figure 6. 19. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
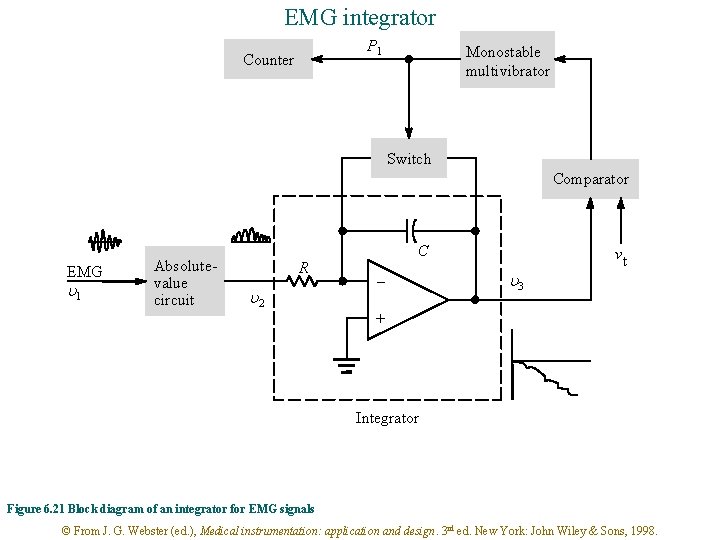
EMG integrator P 1 Counter Monostable multivibrator Switch Comparator EMG u 1 Absolutevalue circuit R u 2 C - u 3 vt + Integrator Figure 6. 21 Block diagram of an integrator for EMG signals © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
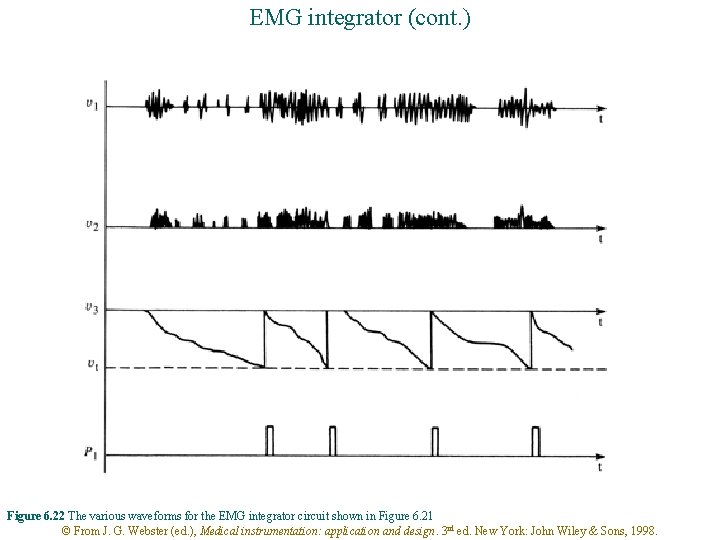
EMG integrator (cont. ) Figure 6. 22 The various waveforms for the EMG integrator circuit shown in Figure 6. 21 © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

Evoked potentials and signal averagers • Object : The neurological response to a particular stimulus • Characteristics : Weak signal + poor SNR (signal-to-noise ratio) Amplification alone does not give adequate signals. Signal averaging: * Enhancement of SNR = n / n 1/2 = n 1/2 n = 9 SNR Enhancement = 3 n = 100 SNR Enhancement = 10 © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
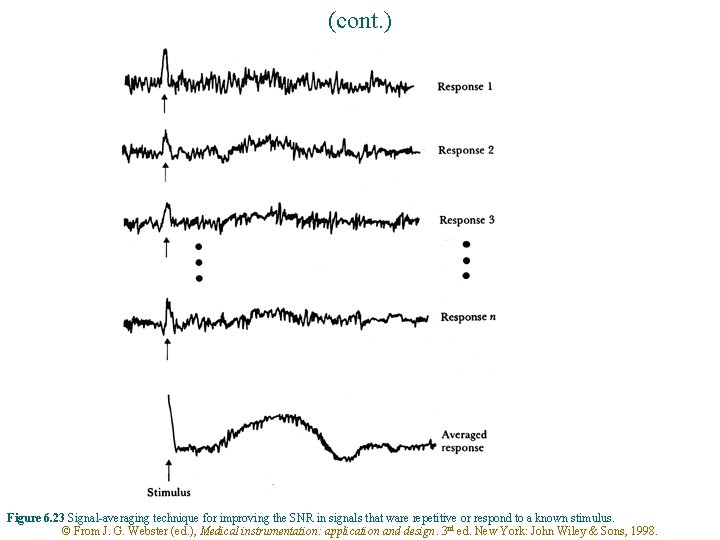
(cont. ) Figure 6. 23 Signal-averaging technique for improving the SNR in signals that ware repetitive or respond to a known stimulus. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

(cont. ) © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

(cont. ) © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

(cont. ) Examples of signal averaging applications: 1. EEG 2. Fetal ECG © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
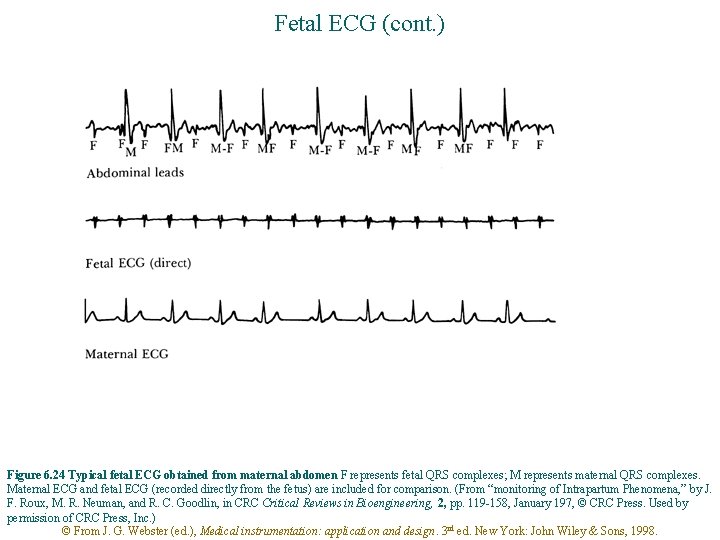
Fetal ECG (cont. ) Figure 6. 24 Typical fetal ECG obtained from maternal abdomen F represents fetal QRS complexes; M represents maternal QRS complexes. Maternal ECG and fetal ECG (recorded directly from the fetus) are included for comparison. (From “monitoring of Intrapartum Phenomena, ” by J. F. Roux, M. R. Neuman, and R. C. Goodlin, in CRC Critical Reviews in Bioengineering, 2, pp. 119 -158, January 197, © CRC Press. Used by permission of CRC Press, Inc. ) © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
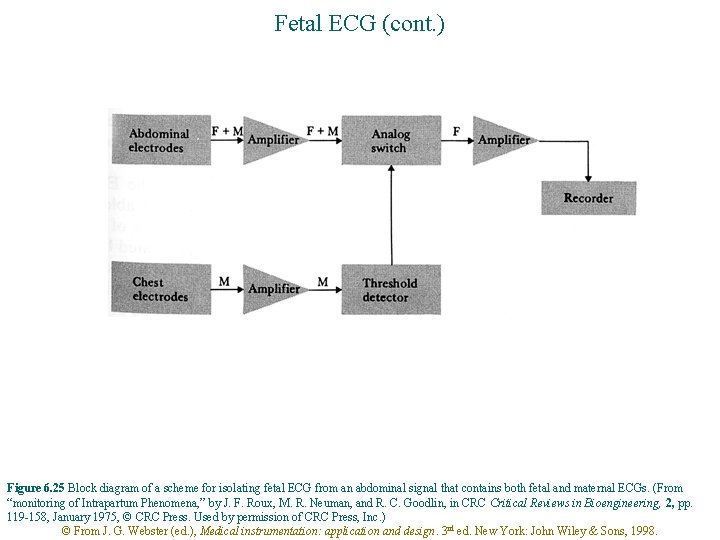
Fetal ECG (cont. ) Figure 6. 25 Block diagram of a scheme for isolating fetal ECG from an abdominal signal that contains both fetal and maternal ECGs. (From “monitoring of Intrapartum Phenomena, ” by J. F. Roux, M. R. Neuman, and R. C. Goodlin, in CRC Critical Reviews in Bioengineering, 2, pp. 119 -158, January 1975, © CRC Press. Used by permission of CRC Press, Inc. ) © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

VCG Vectorcardiography (VCG), or vectorelectrocardiography (VECG) : The measurement and display of the electric heart vector © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

the clinical importance of vectorcardiography 1) The display system provides an opportunity to analyze the progress of the activation front in a different way, especially its initial and terminal parts. 2) It is also much easier to observe the direction of the heart vector from the VCG loops. 3) The area of the loops, which is not easy to observe from a scalar display, may have clinical importance. Note: The information content in the VCG signal is not greater than in the scalar ECG. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
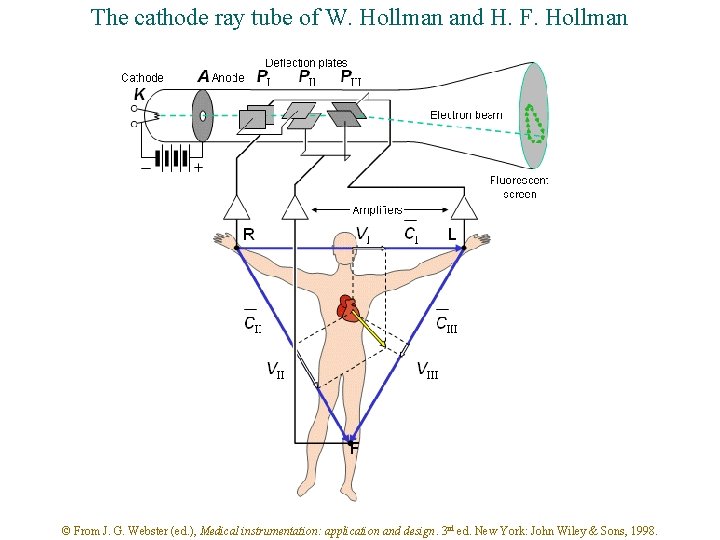
The cathode ray tube of W. Hollman and H. F. Hollman © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
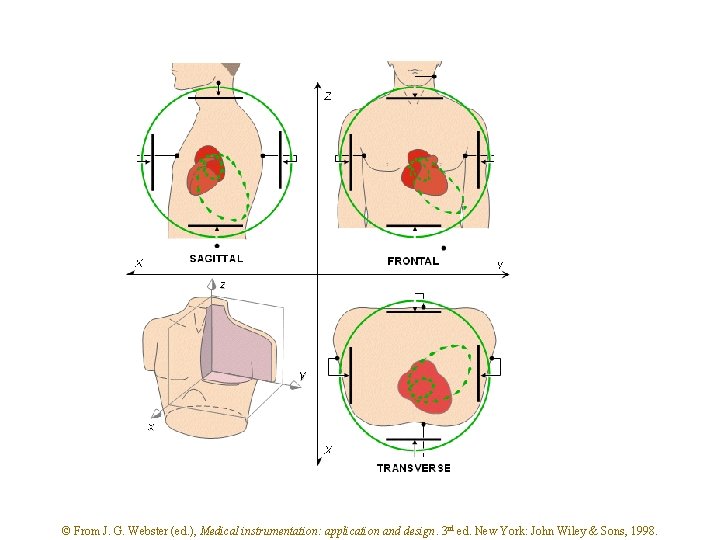
© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
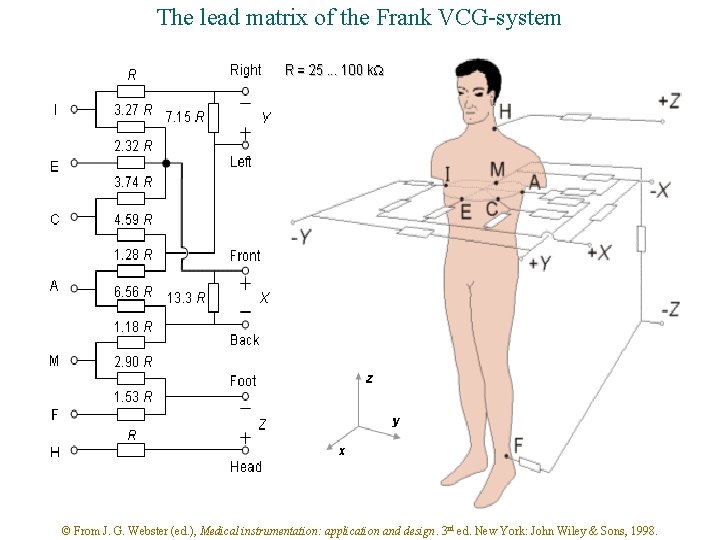
The lead matrix of the Frank VCG-system © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

Compared to ECG, VCG has been recognized as a very useful investigative clinical method for cardiac activity sensing. In addition, it shows the balance of cardiac cycle forces at any moment and contains more information in comparison to ECG that may have diagnostic significance, such as the display of temporal or phase relationships between complexes. The importance of VCG is, for example, in the detection and localization of acute myocardial infarction, right ventricular hypertrophy, and Tawar arm blockade. Source: Rene Jaros, Radek Martinek, Lukas Danys, Comparison of Different Electrocardiography with Vectorcardiography Transformations, Sensors (Basel). 2019 19(14): 3072. © From J. G. Webster (ed. ), Medical instrumentation: application and. Jul; design. 3 rd ed. New York: John Wiley & Sons, 1998.
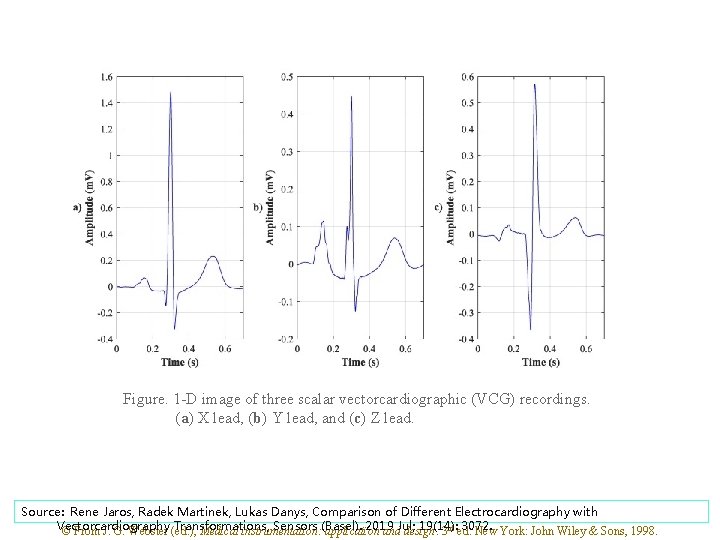
Figure. 1 -D image of three scalar vectorcardiographic (VCG) recordings. (a) X lead, (b) Y lead, and (c) Z lead. Source: Rene Jaros, Radek Martinek, Lukas Danys, Comparison of Different Electrocardiography with Vectorcardiography Transformations, Sensors (Basel). 2019 19(14): 3072. © From J. G. Webster (ed. ), Medical instrumentation: application and. Jul; design. 3 rd ed. New York: John Wiley & Sons, 1998.
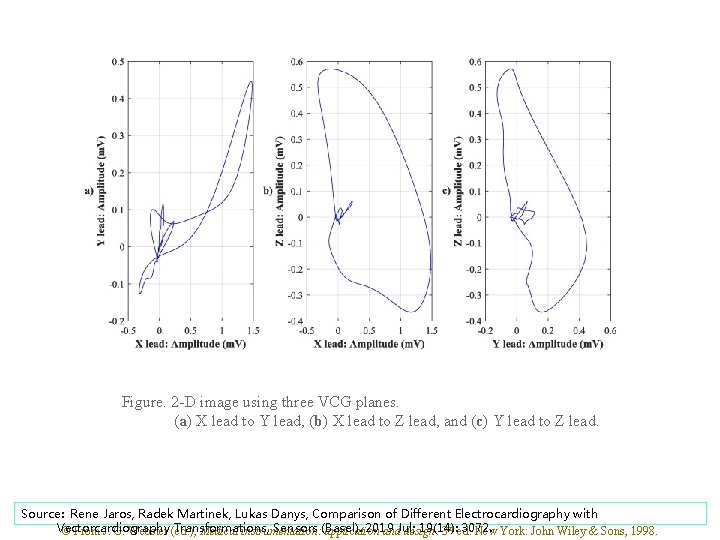
Figure. 2 -D image using three VCG planes. (a) X lead to Y lead, (b) X lead to Z lead, and (c) Y lead to Z lead. Source: Rene Jaros, Radek Martinek, Lukas Danys, Comparison of Different Electrocardiography with Vectorcardiography Transformations, Sensors (Basel). 2019 19(14): 3072. © From J. G. Webster (ed. ), Medical instrumentation: application and. Jul; design. 3 rd ed. New York: John Wiley & Sons, 1998.
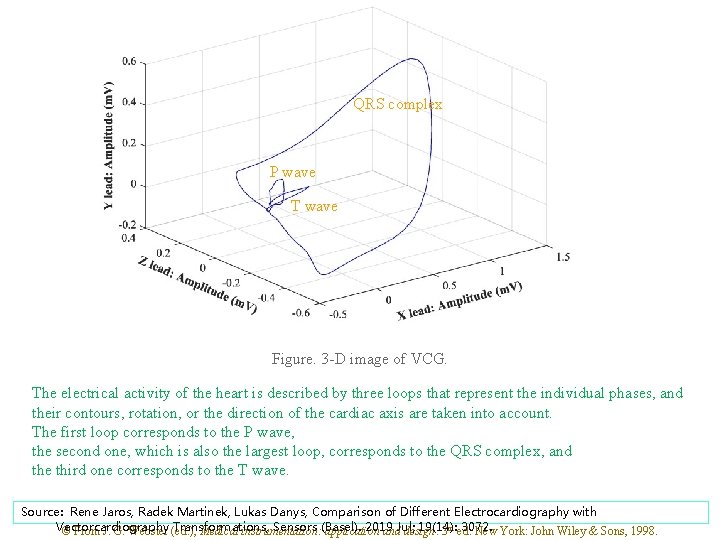
QRS complex P wave T wave Figure. 3 -D image of VCG. The electrical activity of the heart is described by three loops that represent the individual phases, and their contours, rotation, or the direction of the cardiac axis are taken into account. The first loop corresponds to the P wave, the second one, which is also the largest loop, corresponds to the QRS complex, and the third one corresponds to the T wave. Source: Rene Jaros, Radek Martinek, Lukas Danys, Comparison of Different Electrocardiography with Vectorcardiography Transformations, Sensors (Basel). 2019 19(14): 3072. © From J. G. Webster (ed. ), Medical instrumentation: application and. Jul; design. 3 rd ed. New York: John Wiley & Sons, 1998.

© From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.

6. 9 Cardiac monitor Coronary artery 冠狀動脈 1. Monitoring the patient during anesthesia (麻醉) 2. Monitoring patients with cardiac infaction (梗塞) (obstruction of local blood supply ) 3. Monitoring fetus during labor (分娩) * Has narrower frequency respoonse in order to filter out motion artifacts * Should not trigger on pacemaker spikes (which continue even when the hert has stopped) * doesn’t show detailed ECG waveforms © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
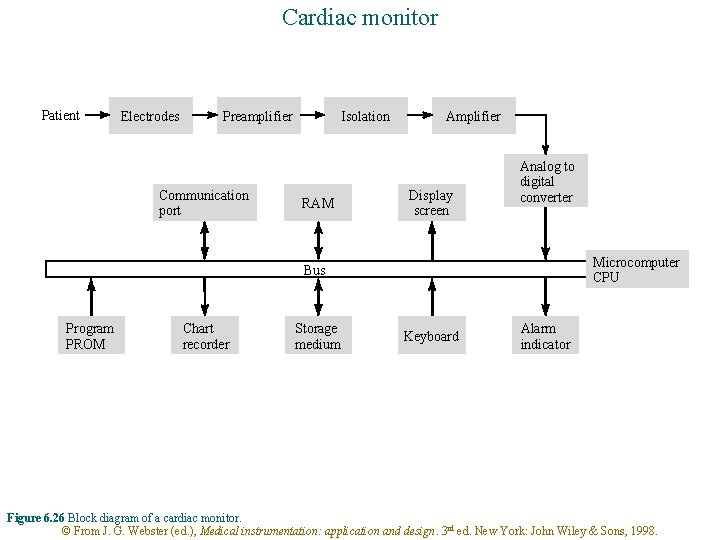
Cardiac monitor Patient Electrodes Preamplifier Communication port Isolation RAM Amplifier Display screen Analog to digital converter Microcomputer CPU Bus Program PROM Chart recorder Storage medium Keyboard Alarm indicator Figure 6. 26 Block diagram of a cardiac monitor. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
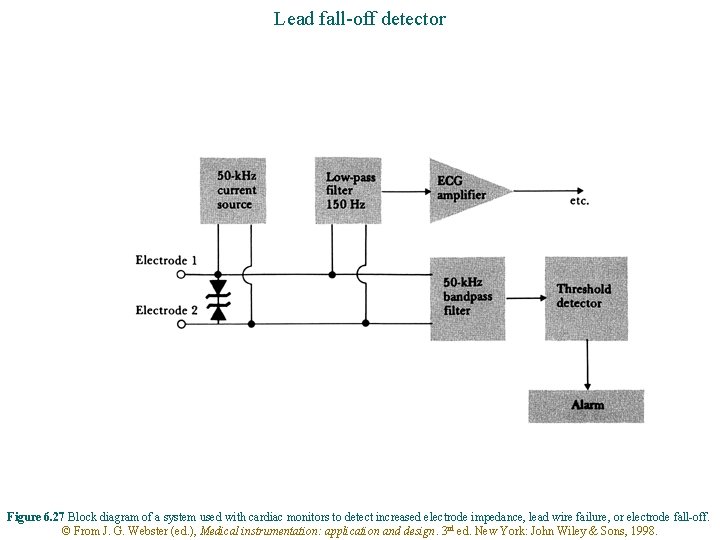
Lead fall-off detector Figure 6. 27 Block diagram of a system used with cardiac monitors to detect increased electrode impedance, lead wire failure, or electrode fall-off. © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
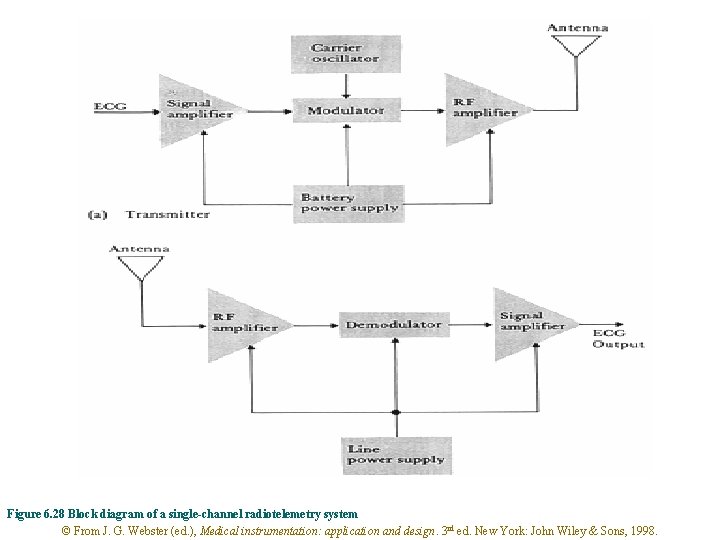
Figure 6. 28 Block diagram of a single-channel radiotelemetry system © From J. G. Webster (ed. ), Medical instrumentation: application and design. 3 rd ed. New York: John Wiley & Sons, 1998.
- Slides: 51