Chapter 57 Nursing Management Acute Intracranial Problems Factors

Chapter 57 Nursing Management Acute Intracranial Problems

Factors That Affect ICP • • • Arterial pressure Venous pressure Intraabdominal and intrathoracic pressure Posture Temperature Blood gases-CO 2 levels
Intracranial Pressure • Regulation and maintenance of intracranial pressure – Normal intracranial pressure-total pressure exerted by the brain, blood, and CSF – Normal compensatory adaptations • Changes in CSF volume by altering absorption or production and displacement of CSF into spinal subarachnoid space • Alteration of blood volume • Tissue brain volume changes by distention of dura or compression of brain tissue – Measuring ICP- 0 -15 mm HG
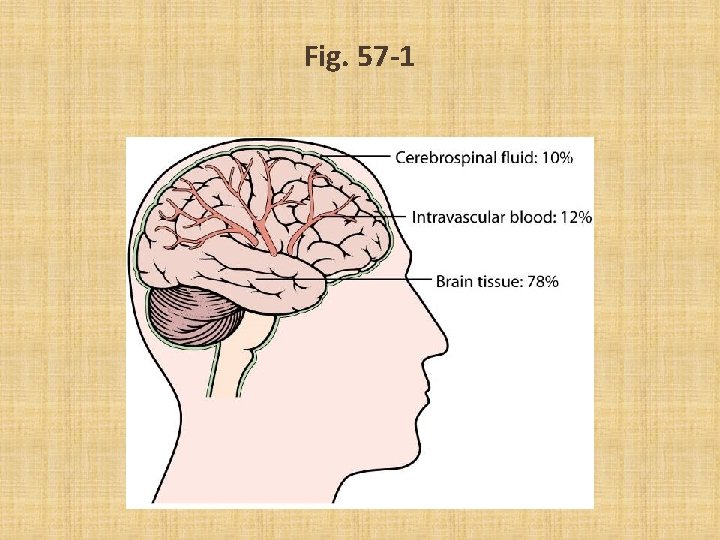
Fig. 57 -1
Intracranial Pressure (cont’d) • Cerebral blood flow – Autoregulation of cerebral blood flow • CPP- cerebral perfusion pressure (CPP= MAP-ICP) – Pressure changes • Compliance= volume/pressure – Factors affecting cerebral blood flow • carbon dioxide- ↑ in Pa. Co 2 relaxes smooth muscle, dilates cerebral vessels, ↓ cerebrovascular resistance, and ↑CBF • ↓ O 2→ cerebrovascular dilation • Hydrogen ion- if O 2 not ↑ → ↑ lactic acid→acidosis→dilation

Increased Intracranial Pressure • Cerebral edema – Vasogenic cerebral edema-most common (white matter)-leakage of macromolecules→osmotic gradient →edema – Cytotoxic cerebral edema-gray matter)destructive lesions or trauma→fliud and proteins shift from extracellular into cells – Interstitial cerebral edemahydrocephalus or water excess →fluid moves into cell
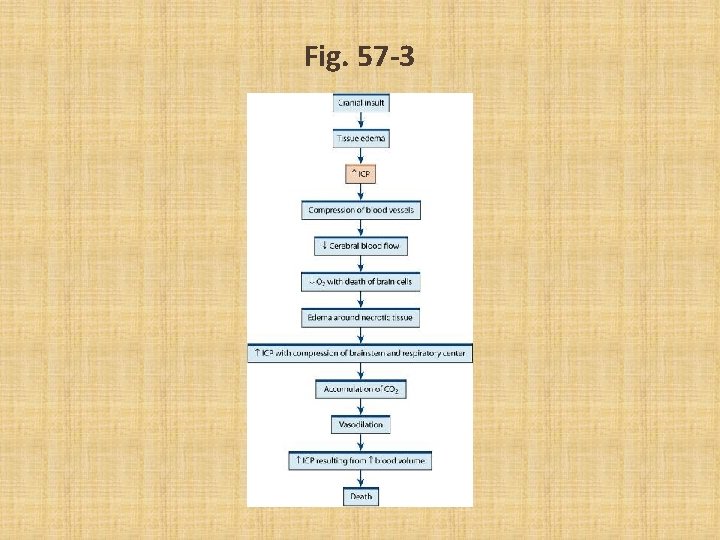
Fig. 57 -3

Increased Intracranial Pressure (cont’d) • Clinical manifestations – – – Change in level of consciousness Changes in vital signs Ocular signs Decrease in motor function Headache Vomiting
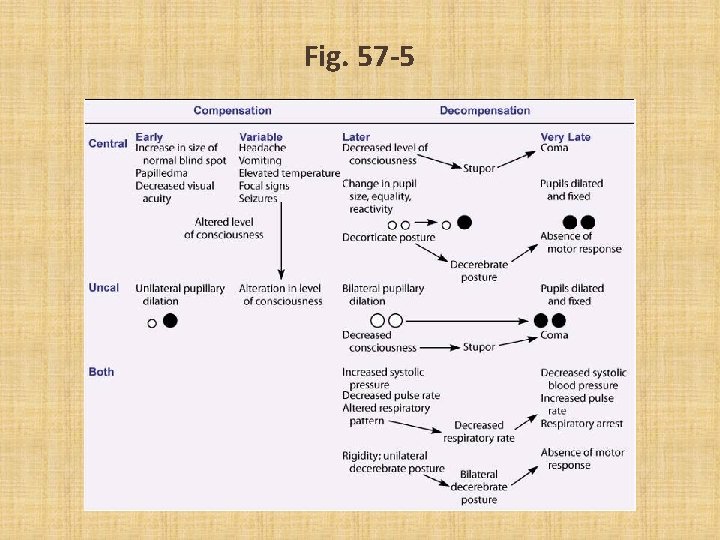
Fig. 57 -5
Increased Intracranial Pressure (cont’d) • Complications-inadequate cerebral perfusion and herniation • Diagnostic studies – see Table 57 -3 • Measurement of ICP – Indications for ICP monitoring -Glascow Coma Scale<8, abnormal CT or MRI – Methods of measuring ICP- gold standardbetween ventricles – LICOX brain tissue oxygenation catheter and jugular venous bulb catheter – CSF drainage-removing fluid to ↓ pressure
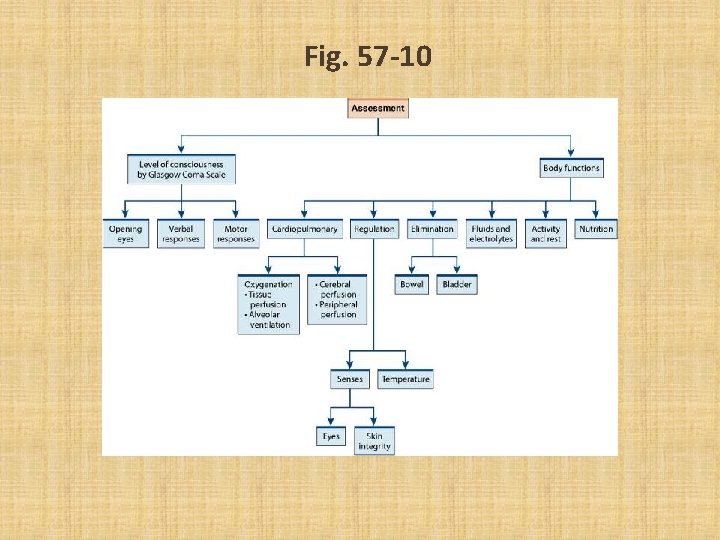
Fig. 57 -10
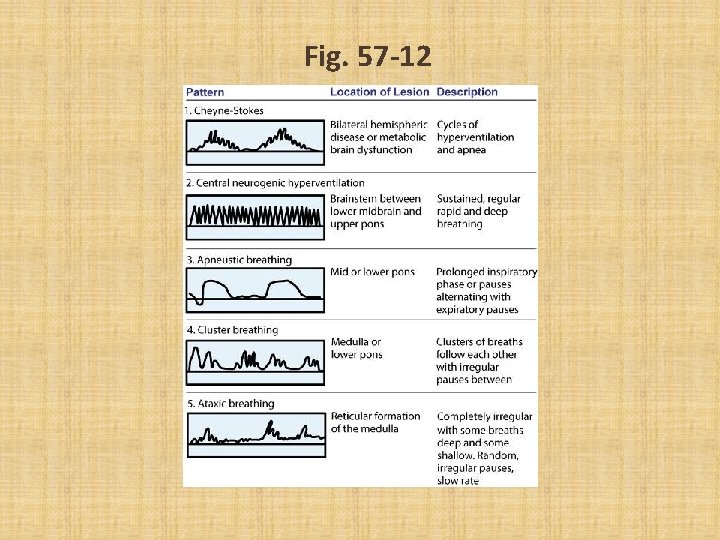
Fig. 57 -12

Head Injury • Types of head injuries – Scalp lacerations – Skull fractures- see Table 57 -7 – Minor head trauma-concussion – Major head trauma • Pathophysiology-axonal injury leads to changes in function and disconnection (12 -24 hrs)

Head Injuries • Epidural – bleeding between the dura and the inner surface of the skull- emergency-initial period of LOC→↓LOC, HA, vomiting • Subdural-bleeding between dura matter and arachnoid layer of meninges- venous • Intracerebral-bleeding within the parenchymafrontal and temperal lobes

Brain Tumors • Types – Primary – secondary • Clinical manifestations- headache , seizures, cognitive dysfunction, memory problems, vomiting, muscle weakness • Complications • Diagnostic studies • Collaborative care – Surgical therapy – Radiation therapy and radiosurgery – Chemotherapy
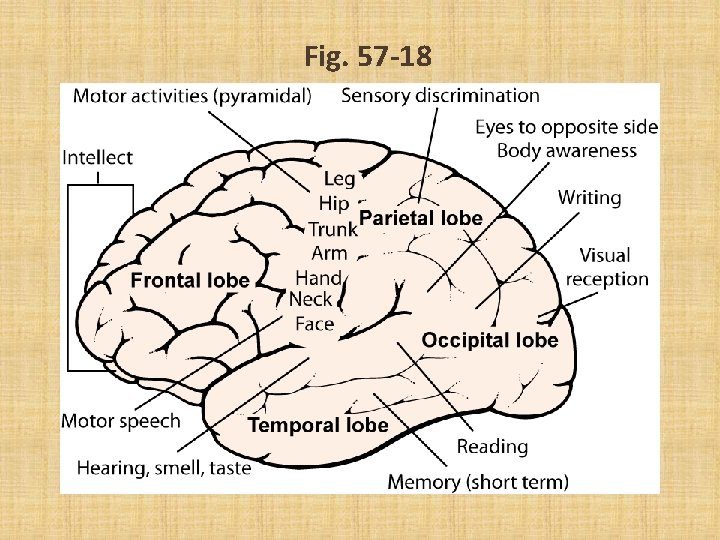
Fig. 57 -18

Inflammatory Conditions of the Brain

Bacterial Meningitis • Etiology and pathophysiology- medical emergency- inflammation of meninges • Clinical manifestations • Complications-↑ ICP, residual neurological dysfunction • Diagnostic studies- LP- ↑protein, ↓glucose, purulent

Viral Meningitis CSF-↑protein, normal glucose, clear or purulent, lymphotycytosis

Encephalitis • Etiology and pathophysiologyinflammation of brain caused by a virus • Clinical manifestations and diagnostic studies-fever, HA, nausea and vomiting – See Table 57 -16

Rabies • Etiology and pathophysiology-RNA virus from saliva from bite of an infected animal • Clinical manifestations- flu like symptoms • Diagnostic studies – blood and CSF • Nursing and collaborative management: Rabies
- Slides: 21