Chapter 47 Bowel Elimination Copyright 2017 Elsevier Inc

Chapter 47 Bowel Elimination Copyright © 2017, Elsevier Inc. All Rights Reserved.
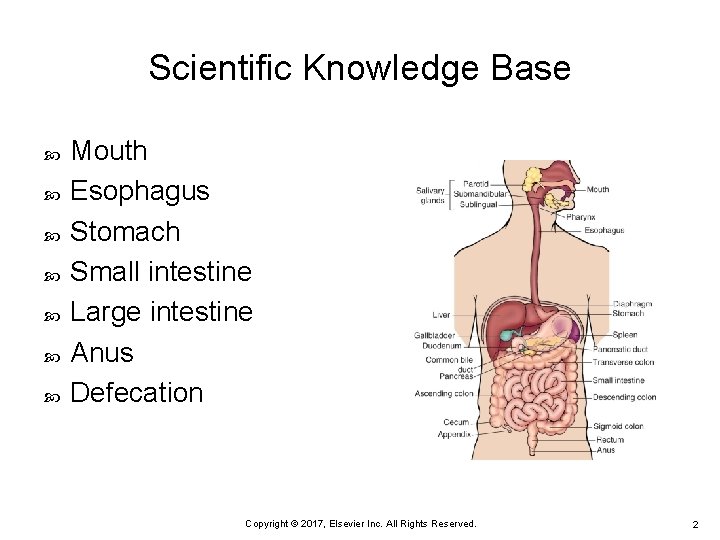
Scientific Knowledge Base Mouth Esophagus Stomach Small intestine Large intestine Anus Defecation Copyright © 2017, Elsevier Inc. All Rights Reserved. 2

Case Study Mr. Gutierrez resides in an assisted-living apartment of a long-term care center. He keeps busy in his small garden plot and enjoys other activities of the center, such as nightly card games and outings to baseball games. He is 82 years old and widowed and has lived in the area for longer than 3 years. His family, with whom he is quite close, is scattered across the country. He has one niece, who lives in the same town. Mr. Gutierrez feels he is in good health; as long as he eats green chili peppers every day, he believes he will remain healthy. Copyright © 2017, Elsevier Inc. All Rights Reserved. 3

Case Study (Cont. ) Because Mr. Gutierrez has a small kitchen in his apartment, he is able to make some of his favorite foods. His diet consists of flour and corn tortillas, beans, and rice. He likes most meats, but he prefers chicken and asado (made with pork). For breakfast, he usually has huevos rancheros. He has been hospitalized only twice —once for the flu and once for placement of a pacemaker. He presently takes three medications: digoxin, Zestril, and Metamucil. Copyright © 2017, Elsevier Inc. All Rights Reserved. 4

Nursing Knowledge Base: Factors Affecting Bowel Elimination Age Diet Fluid intake Physical activity Psychological factors Personal habits Position during defecation Pain Pregnancy Surgery and anesthesia Medications Diagnostic tests Copyright © 2017, Elsevier Inc. All Rights Reserved. 5

Common Bowel Elimination Problems Constipation Impaction A symptom, not a disease; infrequent stool and/or hard, dry, small stools that are difficult to eliminate Results from unrelieved constipation; a collection of hardened feces wedged in the rectum that a person cannot expel Diarrhea Incontinence An increase in the number of stools and the passage of liquid, unformed feces Inability to control passage of feces and gas to the anus Flatulence Hemorrhoids Accumulation of gas in the intestines causing the walls to stretch Dilated, engorged veins in the lining of the rectum Copyright © 2017, Elsevier Inc. All Rights Reserved. 6

Case Study (Cont. ) This afternoon Mr. Gutierrez has telephoned his niece for the fourth time. He reports, “My bowels are locked up and haven’t moved in the last 2 days. ” He ate a big meal the previous evening and now reports feeling “all gassed up. ” His niece tried to explain about eating foods containing fiber and more vegetables. She reminded Mr. Gutierrez that the nursing student was coming later this afternoon, and he could talk to the student about his problem. Copyright © 2017, Elsevier Inc. All Rights Reserved. 7
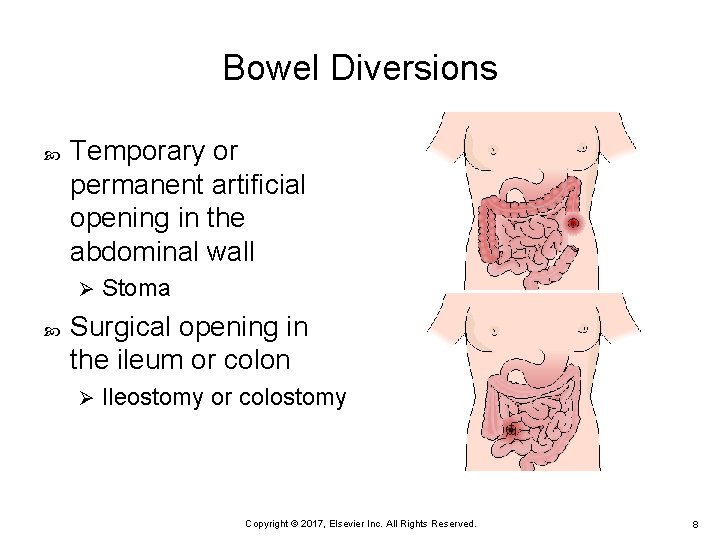
Bowel Diversions Temporary or permanent artificial opening in the abdominal wall Ø Stoma Surgical opening in the ileum or colon Ø Ileostomy or colostomy Copyright © 2017, Elsevier Inc. All Rights Reserved. 8

Bowel Diversions (Cont. ) Ostomies Sigmoid colostomy Ø Transverse colostomy Ø Ileostomy Ø Loop colostomy Ø End colostomy Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 9

Case Study (Cont. ) Vickie is the nursing student assigned to Mr. Gutierrez. She has been seeing him once a week for 5 weeks as part of a home health care clinical experience. They have developed a good rapport. Mr. Gutierrez’ self-identified problems with his bowels are a frequent topic of conversation. As Vickie prepares to assess Mr. Gutierrez, she reflects on experiences with other home care patients. She recalls one patient who had elimination problems resulting from a diet consisting mainly of high-fat and high-carbohydrate foods. She believes her involvement with that patient may help in Mr. Gutierrez’ care. Copyright © 2017, Elsevier Inc. All Rights Reserved. 10
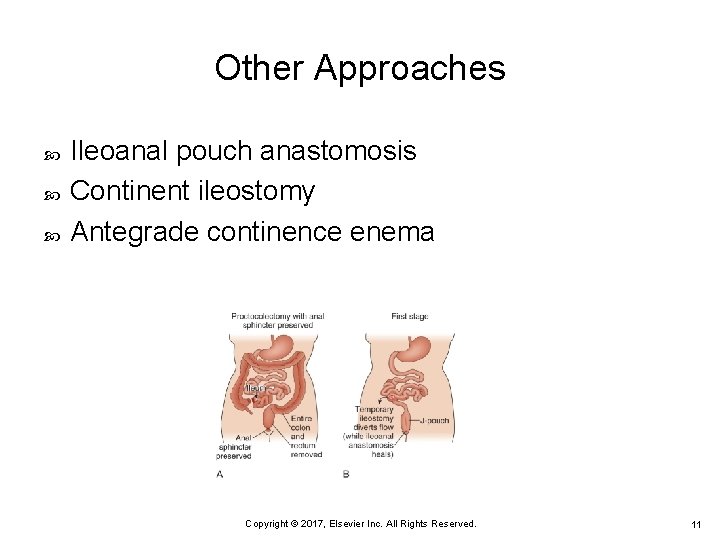
Other Approaches Ileoanal pouch anastomosis Continent ileostomy Antegrade continence enema Copyright © 2017, Elsevier Inc. All Rights Reserved. 11

Critical Thinking Integrate the knowledge from nursing and other disciplines to understand the patient’s response to bowel elimination alterations. Experience in caring for patients with elimination alterations helps you provide an appropriate plan of care. Use critical thinking attitudes such as fairness, confidence, and discipline. Apply relevant standards of practice when selecting nursing measures. Copyright © 2017, Elsevier Inc. All Rights Reserved. 12

Case Study (Cont. ) Vickie reviews her class notes on the anatomy and physiology of the GI system. Vickie reviews the physiological changes that aging produces within the GI system: loss of teeth, taste bud atrophy, decreased secretion of gastric acid, and a slight decrease in small intestine motility. Vickie will thoroughly assess Mr. Gutierrez’ dietary intake with a 24 -hour diet recall. Being familiar with his Hispanic heritage, Vickie anticipates certain food preferences. She knows he does not like the food served at the center and frequently requests “home-cooked” tortillas and green chili peppers from his niece. Copyright © 2017, Elsevier Inc. All Rights Reserved. 13

Quick Quiz! 1. A newly admitted patient states that he has recently had a change in medications and reports that stools are now dry and hard to pass. This type of bowel pattern is consistent with: A. abnormal defecation. B. constipation. C. fecal impaction. D. fecal incontinence. Copyright © 2017, Elsevier Inc. All Rights Reserved. 14

Case Study (Cont. ) From their last visit, Vickie and Mr. Gutierrez have been able to communicate without difficulty. Mr. Gutierrez complains of feeling “full of gas” but has not “passed any wind” in the past 2 days. His stove has not been working well, and he has been unable to prepare rice and beans. Based on the nursing history, Vickie estimates that Mr. Gutierrez normally drinks about 1200 m. L of fluid daily. Copyright © 2017, Elsevier Inc. All Rights Reserved. 15

Nursing Process: Assessment Through the patient’s eyes Nursing history What a patient describes as normal or abnormal is often different from factors and conditions that tend to promote normal elimination. Ø Identifying normal and abnormal patterns, habits, and the patient’s perception of normal and abnormal with regard to bowel elimination allows you to accurately determine a patient’s problems. Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 16
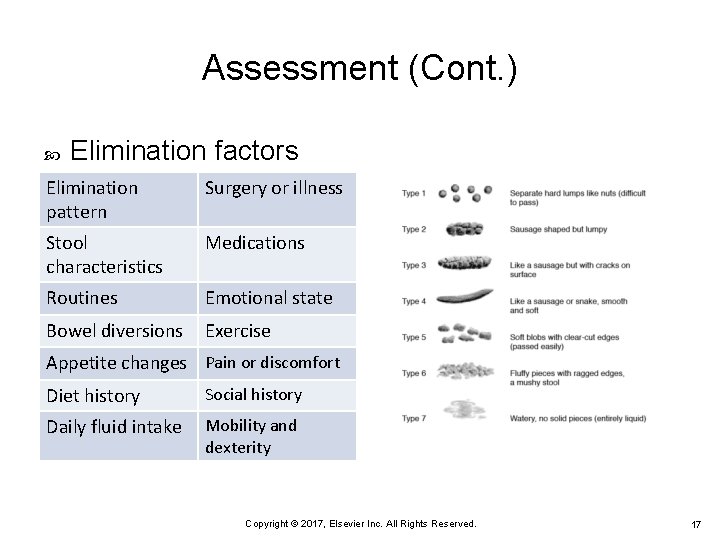
Assessment (Cont. ) Elimination factors Elimination pattern Surgery or illness Stool characteristics Medications Routines Emotional state Bowel diversions Exercise Appetite changes Pain or discomfort Diet history Social history Daily fluid intake Mobility and dexterity Copyright © 2017, Elsevier Inc. All Rights Reserved. 17

Assessment (Cont. ) Physical assessment Ø Laboratory tests Ø Mouth, abdomen, and rectum Fecal specimens Diagnostic examinations Direct visualization Ø Indirect visualization Ø Bowel preparation Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 18

Case Study (Cont. ) Determine when Mr. Gutierrez had his last bowel movement. He had his last bowel movement 2 days ago. The stool was brown and hard. “I took a laxative last night, and I think I need an enema. ” Determine Mr. Gutierrez’ medication history. A medication history shows that Mr. Gutierrez frequently resorts to taking laxatives. Establish Mr. Gutierrez’ dietary habits. Mr. Gutierrez eats a high intake of corn tortillas and cheese and a low intake of fruits. He states, “I really haven’t felt like eating today and have not eaten much for the last 4 days. ” Assess Mr. Gutierrez’ abdomen. Hypoactive bowel sounds in all four quadrants. Abdomen is soft but slightly distended. Copyright © 2017, Elsevier Inc. All Rights Reserved. 19

Nursing Diagnosis Some diagnoses that apply to patients with elimination problems include: Disturbed body image Ø Bowel incontinence Ø Constipation Ø Perceived constipation Ø Risk for constipation Ø Diarrhea Ø Nausea Ø Deficit knowledge (nutrition) Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 20

Planning Goals and outcomes Incorporate elimination habits or routines Ø Reinforce routines that promote health Ø Consider preexisting concerns Ø Setting priorities Ø Patients often have multiple diagnoses Teamwork and collaboration Copyright © 2017, Elsevier Inc. All Rights Reserved. 21

Case Study (Cont. ) Nursing diagnosis: Constipation related to lessthan-adequate fluid and dietary intake and chronic laxative use Goals: Mr. Gutierrez will establish and maintain a normal defecation pattern within 1 month. Ø Mr. Gutierrez will identify practices that reduce the risk for or prevent constipation within 2 weeks. Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 22

Implementation: Health Promotion Routine Colorectal cancer Promotion of normal defecation Sitting position Ø Privacy Ø Positioning on bedpan Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 23
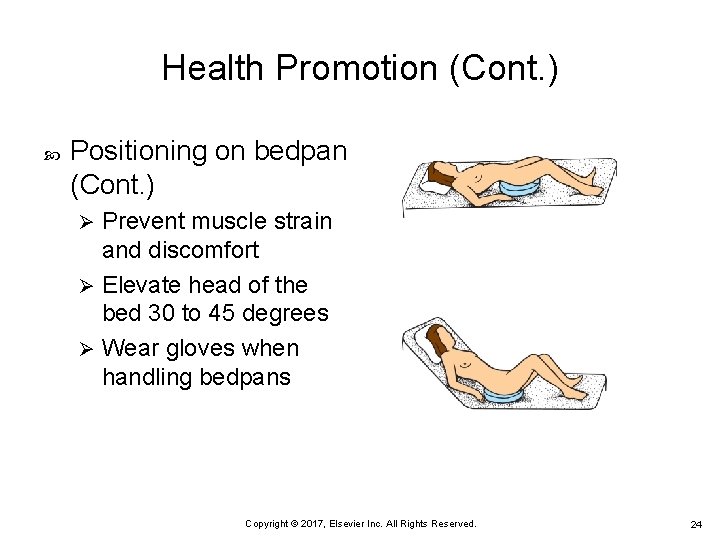
Health Promotion (Cont. ) Positioning on bedpan (Cont. ) Prevent muscle strain and discomfort Ø Elevate head of the bed 30 to 45 degrees Ø Wear gloves when handling bedpans Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 24
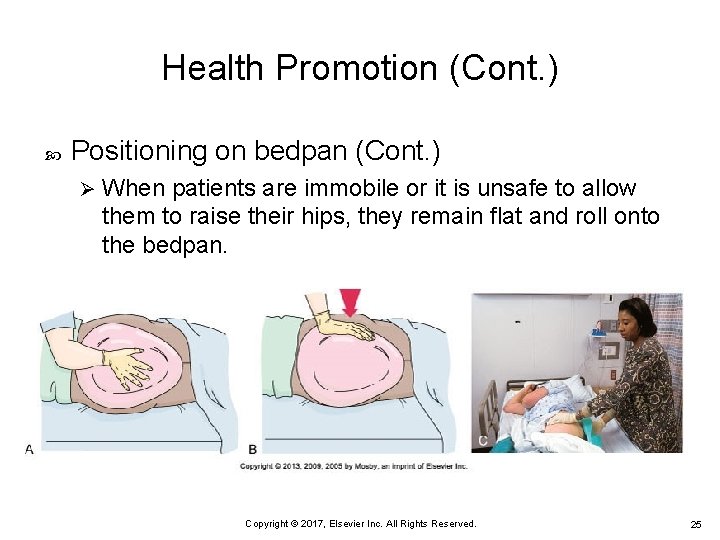
Health Promotion (Cont. ) Positioning on bedpan (Cont. ) Ø When patients are immobile or it is unsafe to allow them to raise their hips, they remain flat and roll onto the bedpan. Copyright © 2017, Elsevier Inc. All Rights Reserved. 25

Case Study (Cont. ) Instruct Mr. Gutierrez in a weekly menu plan, including foods high in fiber: brown rice, beans and rice, tomatoes, and wheat tortillas. Add bran flakes, bran, or fiber supplement to Mr. Gutierrez’ diet. Consult with Mr. Gutierrez’ niece and long-term care center to have the patient’s stove repaired. Educate Mr. Gutierrez about the use of liquids to promote softening of stool and defecation; have him drink a decaffeinated beverage of choice. Encourage Mr. Gutierrez to try to establish a routine time for defecation, for example, after a meal. Copyright © 2017, Elsevier Inc. All Rights Reserved. 26

Acute Care Environment Cathartics and laxatives Cathartics have a stronger and more rapid effect on the intestines than laxatives Ø Suppositories may act more quickly than oral medications Ø Antidiarrheal agents Ø Opiates used with caution Copyright © 2017, Elsevier Inc. All Rights Reserved. 27
Acute Care (Cont. ) Enemas Ø Cleansing enemas • • Tap water Normal saline Hypertonic solutions Soapsuds Oil retention Ø Others types of enemas Ø • Carminative and Kayexalate Copyright © 2017, Elsevier Inc. All Rights Reserved. 28

Acute Care (Cont. ) Enema administration Sterile technique is unnecessary. Ø Wear gloves. Ø Explain the procedure, positioning, precautions to avoid discomfort, and length of time necessary to retain the solution before defecation. Ø Digital removal of stool Use if enemas fail to remove an impaction. Ø Last resort in managing severe constipation. Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 29

Acute Care (Cont. ) Inserting and Maintaining a Nasogastric Tube Ø Purposes • Decompression, enteral feeding, compression, and lavage Ø Categories of nasogastric (NG) tubes • Fine- or small-bore for medication administration and enteral feedings • Large-bore (12 -French and above) for gastric decompression or removal of gastric secretions Clean technique Ø Maintaining patency Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 30

Quick Quiz! 2. To maintain normal elimination patterns in the hospitalized patient, you should instruct the patient to defecate 1 hour after meals because: A. the presence of food stimulates peristalsis. B. mass colonic peristalsis occurs at this time. C. irregularity helps to develop a habitual pattern. D. neglecting the urge to defecate can cause diarrhea. Copyright © 2017, Elsevier Inc. All Rights Reserved. 31
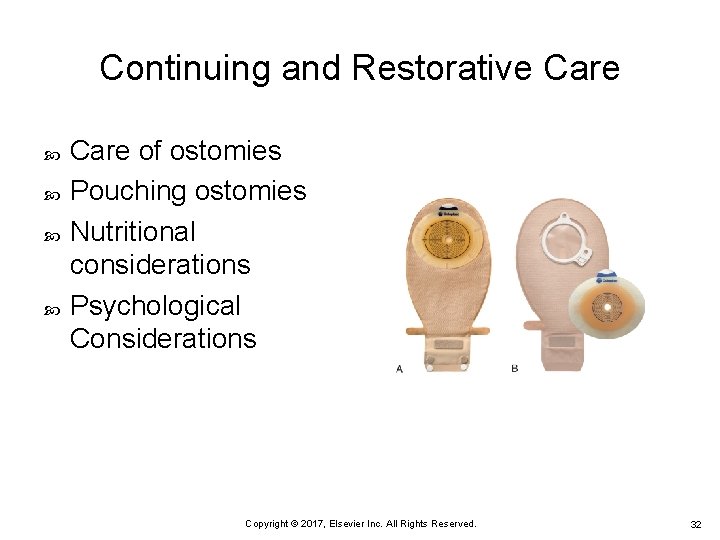
Continuing and Restorative Care of ostomies Pouching ostomies Nutritional considerations Psychological Considerations Copyright © 2017, Elsevier Inc. All Rights Reserved. 32

Continuing and Restorative Care (Cont. ) Bowel training Maintenance of proper fluid and food intake Promotion of regular exercise Management of the patient with fecal incontinence or diarrhea Maintenance of skin integrity Copyright © 2017, Elsevier Inc. All Rights Reserved. 33

Case Study (Cont. ) Review Mr. Gutierrez’ diary of foods, and ask him about his intake as well. Mr. Gutierrez describes likes and dislikes but admits to eating high-fat foods and few fruits and vegetables. Fluid intake averaged 1400 m. L daily for a week. Ask Mr. Gutierrez about Mr. Gutierrez says, “I still go about the his pattern of elimination same” but states that he thinks he now goes about every 2 days. Mr. Gutierrez over the past 2 weeks has not used any laxatives for a week. and laxative use. During follow-up visit, examine patient’s abdomen and observe stool (if possible). Patient reports that stool is formed but is “not hard like before. ” Bowel sounds are normal. Abdomen is soft and nontender with no distention. Copyright © 2017, Elsevier Inc. All Rights Reserved. 34

Evaluation Through the patient’s eyes Ø The patient or caregiver determines which therapies were the most effective Patient outcomes Develop a therapeutic relationship Ø Evaluate a patient’s level of knowledge Ø Determine the extent to which the patient accomplishes normal defecation Ø Ask the patient to describe changes in diet, fluid intake, and activity to promote bowel health Ø Copyright © 2017, Elsevier Inc. All Rights Reserved. 35

Case Study (Cont. ) Vickie returns to see Mr. Gutierrez 2 weeks later. Vickie is eager to determine whether patient has made changes in his diet, and if his problems with bowel elimination have been progressing. Vickie is also eager to learn if his stove has been repaired. Mr. Gutierrez tells Vickie that he has been eating bran cereal in the morning, has been eating rice and/or beans for dinner, and has added one fruit each day to his diet. He has been walking twice a day through the long-term care center. Although he does not have a bowel movement each day, his stools are much softer and easier to pass, and he says he is less concerned. He has not taken a laxative for a stool since last talking with Vickie. Copyright © 2017, Elsevier Inc. All Rights Reserved. 36

Safety Guidelines For Nursing Skills Instruct patients who self-administer enemas to use the side-lying position. If a patient has cardiac disease or is taking cardiac or hypertensive medication, obtain a pulse rate, because manipulation of rectal tissue stimulates the vagus nerve and sometimes causes a sudden decline in pulse rate. Copyright © 2017, Elsevier Inc. All Rights Reserved. 37
- Slides: 37