Chapter 45 Hormones and the Endocrine System Essential




































- Slides: 65

Chapter 45 Hormones and the Endocrine System Essential Idea: Hormones are used when signals need to be widely distributed. travismulthaupt. com

Internal Communication Ø Animals have 2 systems of internal communication to regulate and maintain homeostasis: Ø 1. The nervous system. Ø 2. The endocrine system.

1. The Nervous System Ø The nervous system is the pathway of communication involving high speed electrical signals. Ø There are two portions to it: Ø CNS Ø PNS

2. The Endocrine System Ø The endocrine system is all of the animal’s hormone secreting cells. Ø The endocrine system coordinates a slow, long-lasting response.

Endocrine Glands Ø Endocrine glands are hormone secreting organs. Ø They are ductless glands. Ø Their product is secreted into extracellular fluid which then diffuses into circulation.

Positive and Negative Feedback Ø Positive and negative feedback mechanisms control hormonal responses. Ø Recall, Ø Positive feedback acts to reinforce the stimulus. It leads to a greater response. Ø Negative feedback acts to reduce the response of the stimulus.

Molecules Functioning as Hormones Ø There are 3 major classes of molecules that function as hormones: Ø 1. Proteins/peptides-water soluble. ØGlucagon, insulin, leptin Ø 2. Amines-water soluble. ØThyroxin, melatonin Ø 3. Steroids-not water soluble. ØTestosterone, estrogen, progesterone

Key Events Ø There are 3 key events involved in signaling: Ø 1. Reception-is when the signal binds to the receptor protein in or on the target cell. Ø Receptors can be inside or outside the cell. Ø 2. Signal transduction-a signal binds to and triggers events within the cell (cascade events). Ø 3. Response-changes a cell’s behavior.

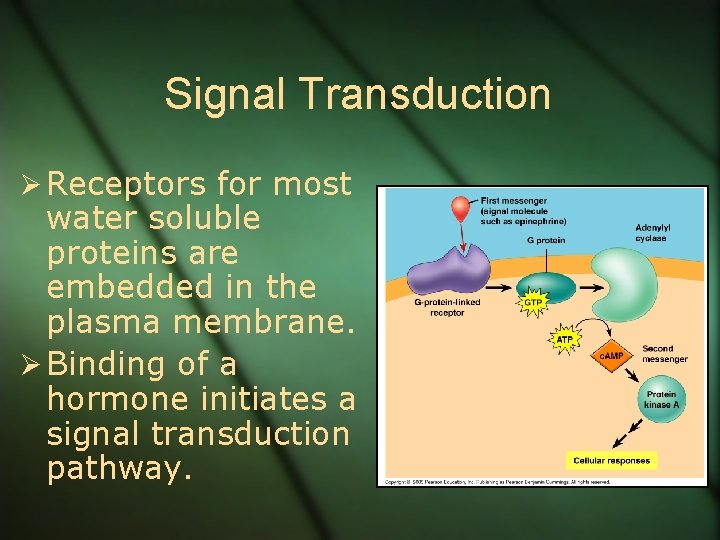
Signal Transduction Ø Receptors for most water soluble proteins are embedded in the plasma membrane. Ø Binding of a hormone initiates a signal transduction pathway.

Signal Transduction Ø A signal transduction pathway is a series of changes where cellular proteins convert an extracellular chemical signal into an intracellular response. Ø Examples: Ø Activation of an enzyme Ø Uptake or secretion of a specific molecule Ø Rearrangement of a cytoskeleton

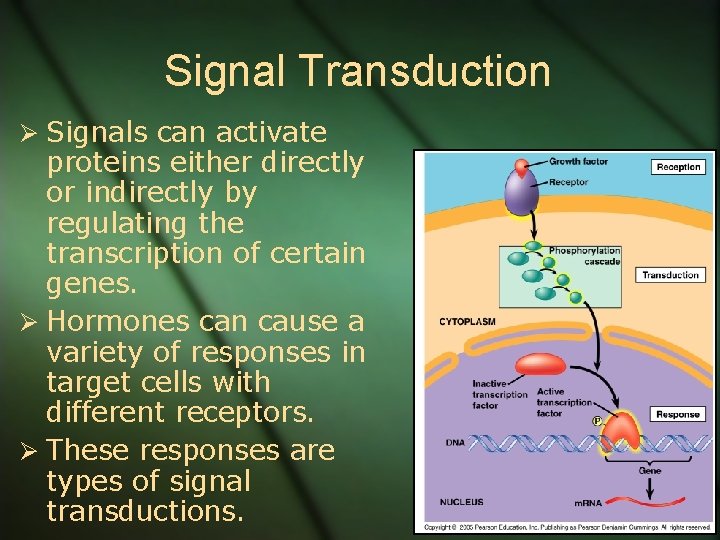
Signal Transduction Ø Signals can activate proteins either directly or indirectly by regulating the transcription of certain genes. Ø Hormones can cause a variety of responses in target cells with different receptors. Ø These responses are types of signal transductions.


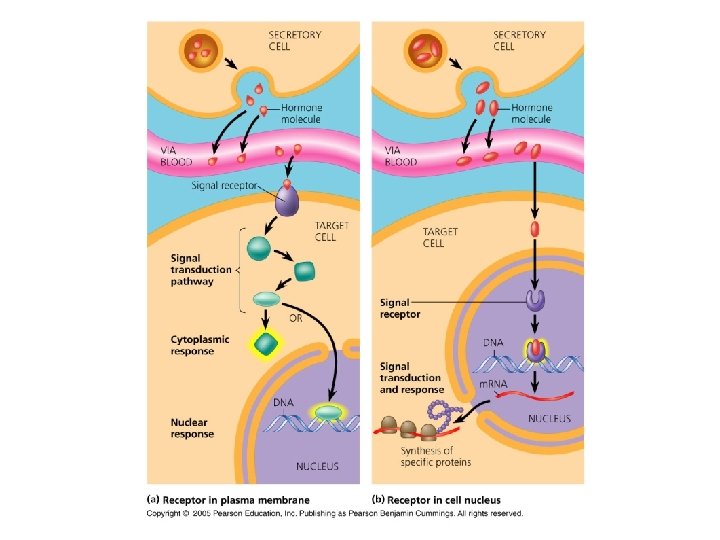
Water Soluble Hormones Ø Most water soluble hormones have receptors embedded in the membrane. Ø Surface receptor proteins activate proteins in the cytoplasm which then move into the nucleus and regulate transcription.

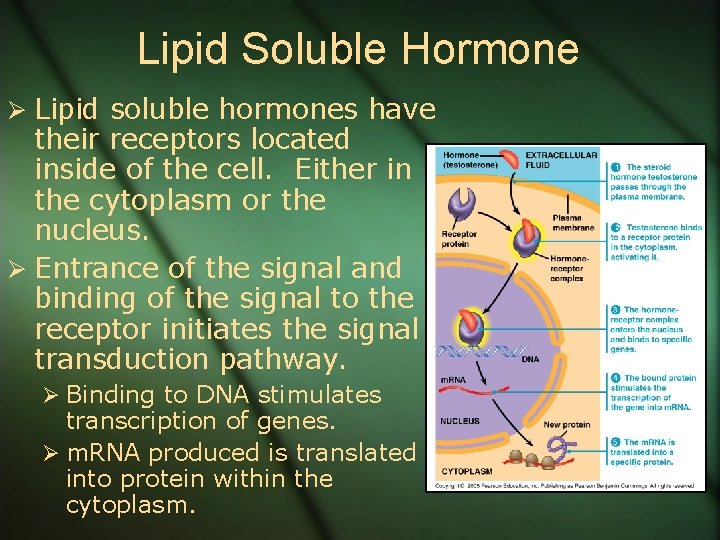
Lipid Soluble Hormone Ø Lipid soluble hormones have their receptors located inside of the cell. Either in the cytoplasm or the nucleus. Ø Entrance of the signal and binding of the signal to the receptor initiates the signal transduction pathway. Ø Binding to DNA stimulates transcription of genes. Ø m. RNA produced is translated into protein within the cytoplasm.

The Thyroid Gland Ø The thyroid produces 2 hormones. Ø Triiodothyroxine (T 3) Ø Thyroxin (T 4) Ø In mammals, T 4 is converted to T 3 by target cells. Ø T 3 is mostly responsible for the cellular response.

Thyroxin Ø Thyroxin is secreted by the thyroid gland has a variety of effects on the body. Ø It helps to regulate the metabolic rate. Ø It assists in controlling body temperature. Ø It plays a role in the metabolism of carbohydrates, fats, proteins. Ø It aids the immune system.

Pancreas Ø The pancreas is both an endocrine and a exocrine gland. Ø Exocrine-releases secretions into ducts. Ø Endocrine-secretions diffuse into bloodstream. Ø Islets of Langerhans are scattered throughout the exocrine portion of the pancreas.

Pancreas Ø Each islet contains α-cells and β-cells. α-cells produce glucagon. Ø β-cells produce insulin. Ø Insulin and glucagon oppose each other and regulate the concentration of glucose in the blood. Ø

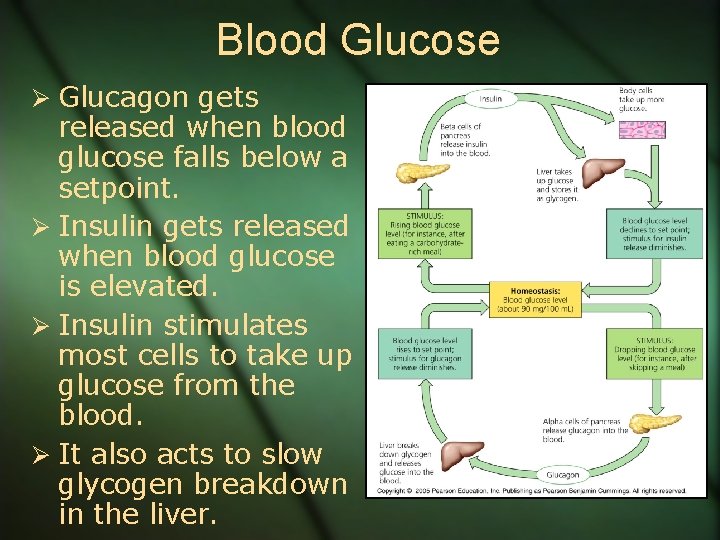
Blood Glucose Ø Glucagon gets released when blood glucose falls below a setpoint. Ø Insulin gets released when blood glucose is elevated. Ø Insulin stimulates most cells to take up glucose from the blood. Ø It also acts to slow glycogen breakdown in the liver.

Diabetes Mellitus Ø Diabetes is an endocrine disorder caused by a deficiency in insulin or decreased response to insulin. Ø There are 2 types: ØType I-insulin dependent. ØType II-non-insulin dependent.

Type I Diabetes Ø Insulin dependent. It’s an autoimmune disease resulting in the destruction of the body’s βcells. Ø The pancreas can’t produce insulin and the person requires insulin injections.

Type II Diabetes Ø Non-insulin dependent. Ø It is caused by a reduced responsiveness of the cells to insulin. Ø Treat with diet and exercise. Ø Medicine, if necessary.

Adipose Tissue Ø Leptin is a hormone secreted by cells in adipose tissue. Ø It acts on the hypothalamus in the brain to inhibit appetite and regulate energy metabolism. Ø It is often called the “satiety hormone”.

Pineal Gland Ø During the hours of darkness, the pineal gland secretes melatonin. Ø Melatonin is involved in controlling circadian rhythms. Ø It regulates sleep/wake cycles, mood, puberty.

Sex Determination and the Y Chromosome Ø The Y chromosome contains the SRY gene which codes for proteins that induce the gonads to form testes. Ø In the absence of this protein, the gonads form ovaries.

Prenatal Gonad Development: Male Ø During the first 6 weeks of development, male and female human embryos are indistinguishable from one another. Ø They have a pair of unisex gonads and two sets of primitive tubing called the Wollfian and Mullerian duct systems.

Prenatal Gonad Development: Male Ø During the 7 th week of gestation, the SRY gene is switched on for a few hours. Ø The SRY protein then acts on many other genes on several different chromosomes tripping a succession of genetic relays to stimulate the development of the testes.

Prenatal Gonad Development: Male Ø The testes produce two different hormones: AMH and testosterone. Ø AMH destroys the Mullerian duct system, while testosterone protects the Wolffian system from destruction. Ø The Wollfian ducts grow and form the internal components of the male reproductive system: prostate gland, seminal vesicles and the vas deferens.

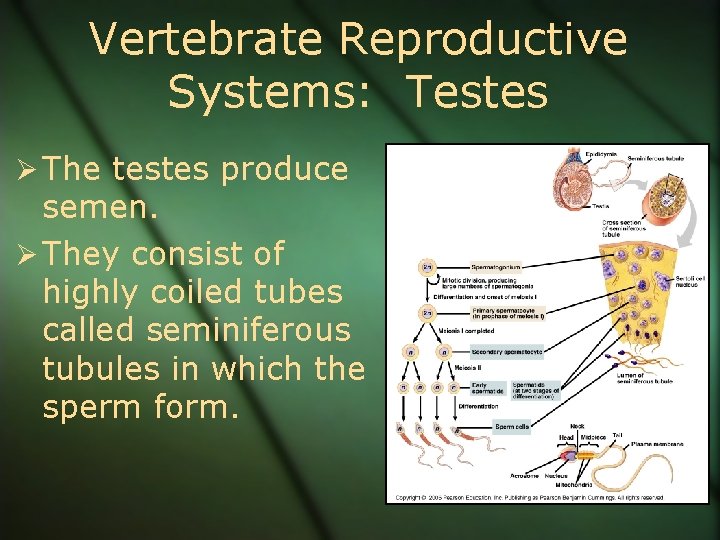
Vertebrate Reproductive Systems: Testes Ø The testes produce semen. Ø They consist of highly coiled tubes called seminiferous tubules in which the sperm form.

Vertebrate Reproductive Systems: Testes Ø These tubules also produce a sugary solution to feed the sperm during their journey. Ø The epididymus is where mature sperm are stored. Ø The prostate gland provides an alkaline solution to offset the female’s acidic reproductive system.

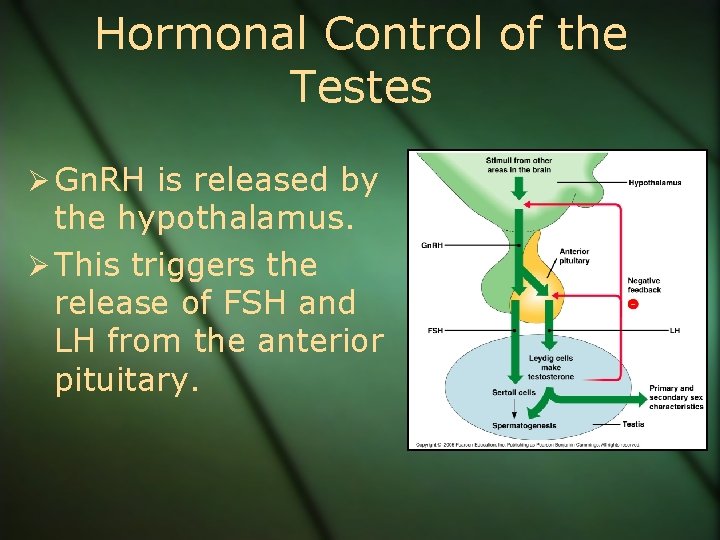
Hormonal Control of the Testes Ø Gn. RH is released by the hypothalamus. Ø This triggers the release of FSH and LH from the anterior pituitary.

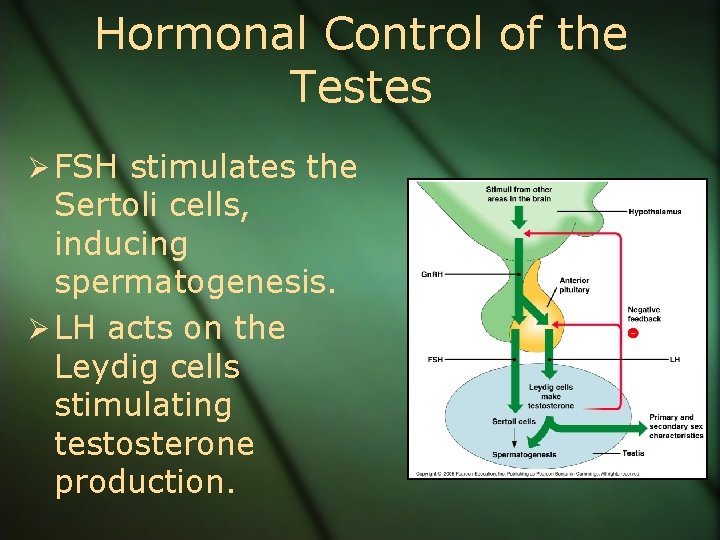
Hormonal Control of the Testes Ø FSH stimulates the Sertoli cells, inducing spermatogenesis. Ø LH acts on the Leydig cells stimulating testosterone production.

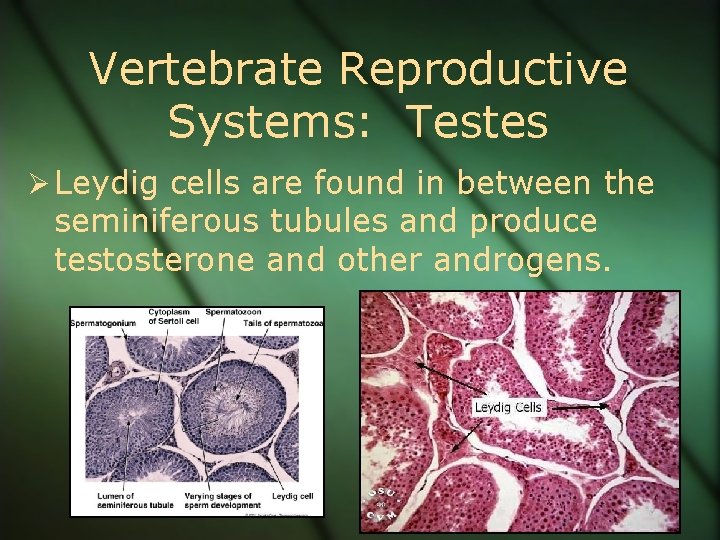
Vertebrate Reproductive Systems: Testes Ø Leydig cells are found in between the seminiferous tubules and produce testosterone and other androgens.

Roles of Testosterone Ø 1. Testosterone promotes differentiation of spermatogonia into mature sperm. Ø 2. It also stimulates the development of the prenatal genitalia. Ø 3. Promotes the development of male secondary sexual characteristics. Ø 4. Maintains sex drive.

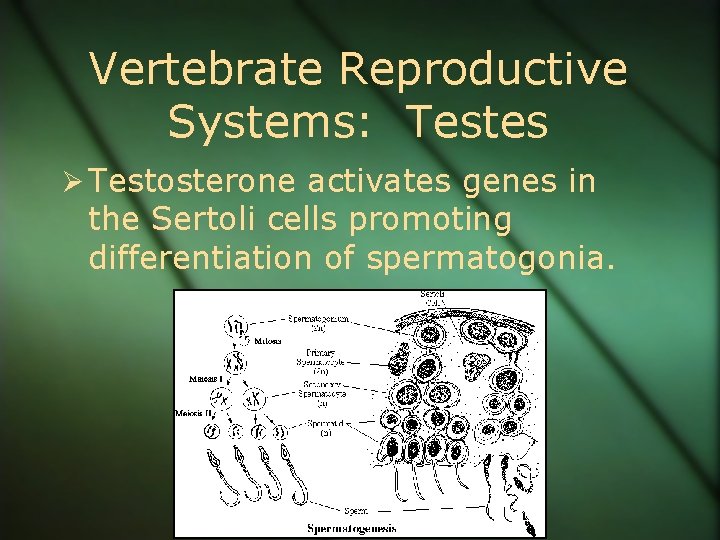
Vertebrate Reproductive Systems: Testes Ø Testosterone activates genes in the Sertoli cells promoting differentiation of spermatogonia.

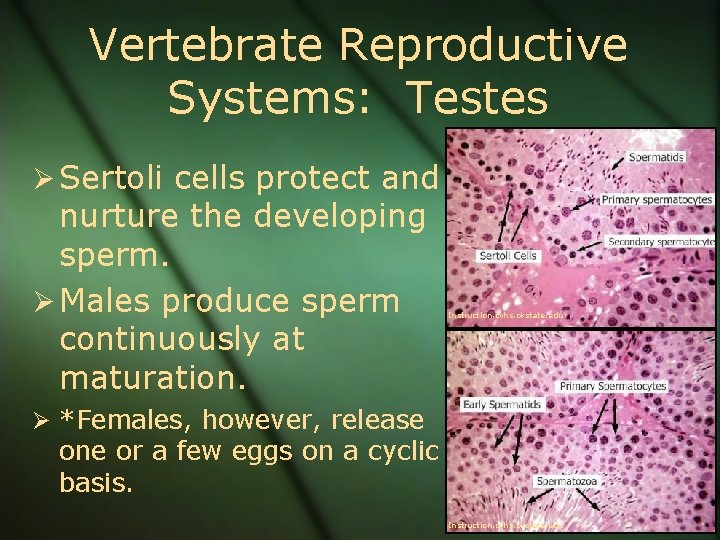
Vertebrate Reproductive Systems: Testes Ø Sertoli cells protect and nurture the developing sperm. Ø Males produce sperm continuously at maturation. Instruction. cvhs. okstate. edu Ø *Females, however, release one or a few eggs on a cyclic basis. Instruction. cvhs. okstate. edu

Embryonic Development of Sperm Ø During embryonic development, primordial germ cells of embryonic testes differentiate into spermatogonia which, at puberty will give rise to sperm.

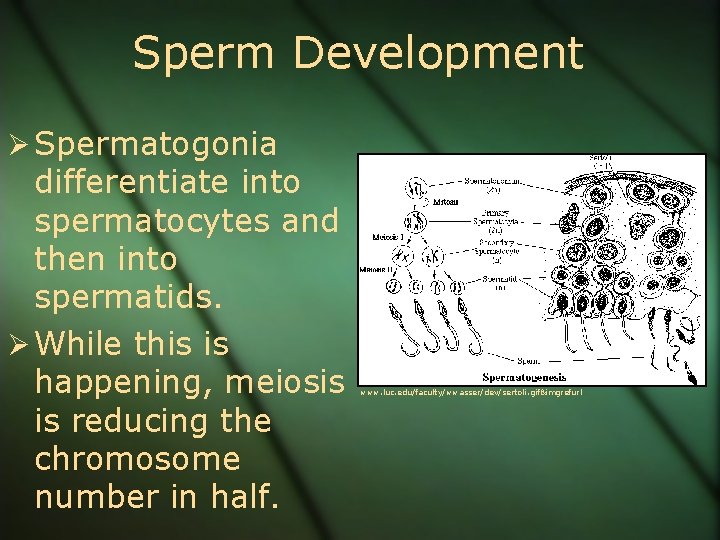
Sperm Development Ø Spermatogonia differentiate into spermatocytes and then into spermatids. Ø While this is happening, meiosis is reducing the chromosome number in half. www. luc. edu/faculty/wwasser/dev/sertoli. gif&imgrefurl

Sperm Ø Most species have sperm with a head that contains the nucleus and a tip called an acrosome that has enzymes which assist the entry of the sperm into the egg. Copyright © 2005 Pearson Education, Inc. Publishing as Pearson Benjamin Cummings. All rights reserved.

Prenatal Gonad Development: Female Ø In females, during the 12 th week of gestation, the unisex gonads begin to transform into ovaries. Ø There is no SRY protein, no AMH, and very little testosterone. Thus, the Wolffian ducts begin to disintegrate.

Prenatal Gonad Development: Female Ø The estrogen stimulates the formation of the female duct system (Fallopian tubes, uterus and vagina) and the obvious differences in the external female anatomy.

Roles of Estrogen Ø 1. Works with progesterone to promote preparation and maintenance of uterine lining for pregnancy. Ø 2. Induces release of LH then triggers ovulation. Ø 3. Promotes female secondary sexual characteristics. Ø 4. Maintains sexual drive.

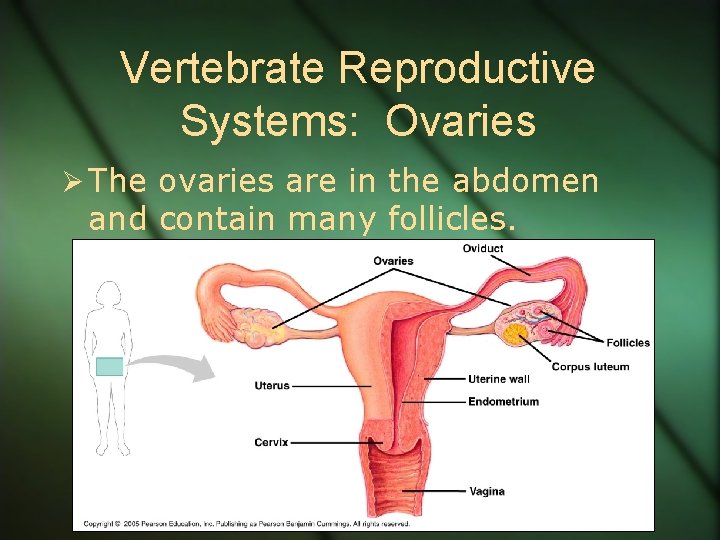
Vertebrate Reproductive Systems: Ovaries Ø The ovaries are in the abdomen and contain many follicles.

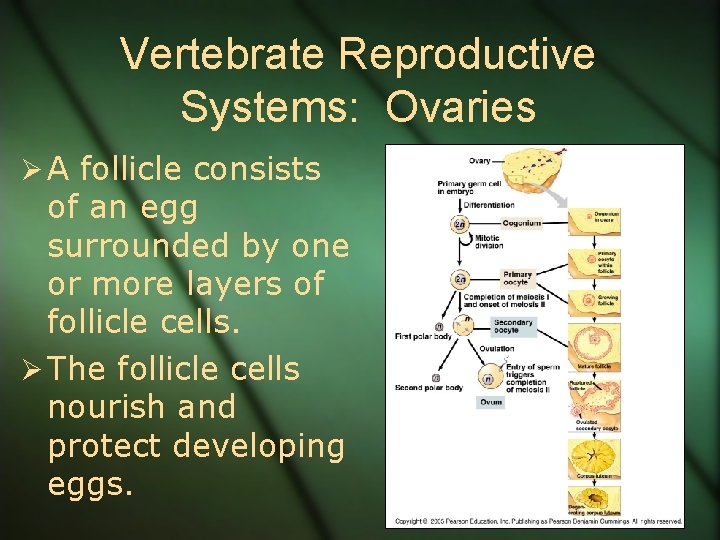
Vertebrate Reproductive Systems: Ovaries Ø A follicle consists of an egg surrounded by one or more layers of follicle cells. Ø The follicle cells nourish and protect developing eggs.

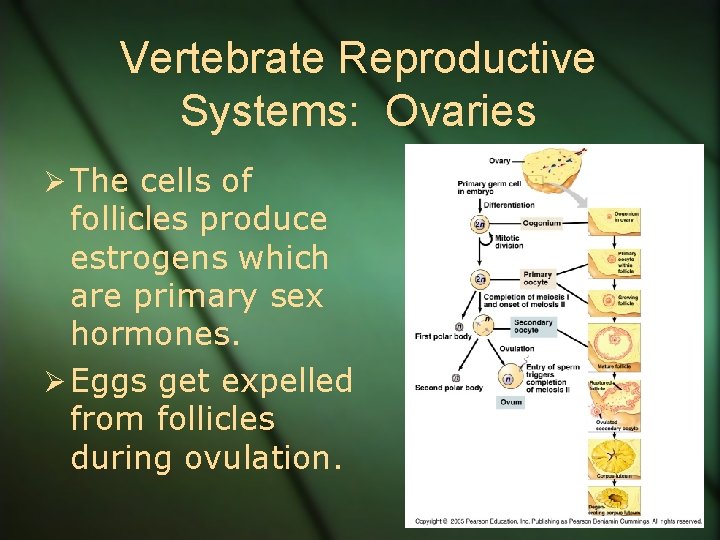
Vertebrate Reproductive Systems: Ovaries Ø The cells of follicles produce estrogens which are primary sex hormones. Ø Eggs get expelled from follicles during ovulation.

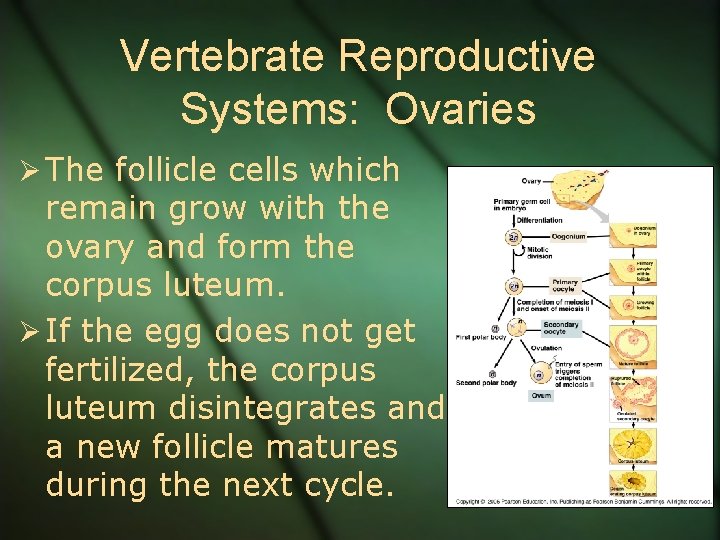
Vertebrate Reproductive Systems: Ovaries Ø The follicle cells which remain grow with the ovary and form the corpus luteum. Ø If the egg does not get fertilized, the corpus luteum disintegrates and a new follicle matures during the next cycle.

Vertebrate Reproductive Systems: Ovaries Ø The egg cell is released into the abdominal cavity near the opening of the oviduct (fallopian tube). Ø There is a funnel-like opening to the oviduct with cilia that help to draw fluid (and eggs) into them. Ø The cilia also beat and move the egg down to the uterus.

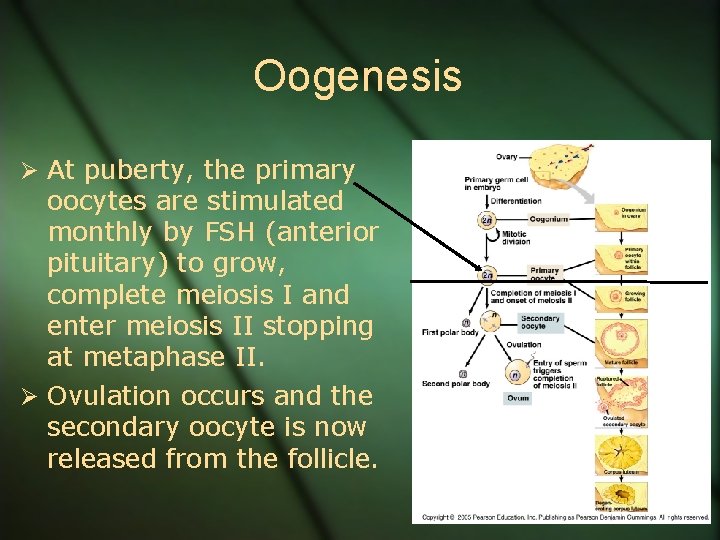
Oogenesis Ø Oogenesis begins in the female embryo when primordial germ cells differentiate into oogonia-ovary specific stem cells. Ø An oogonia multiplies by mitosis and then undergoes meiosis and stops at prophase I. Ø They are now called primary oocytes.

Oogenesis Ø At puberty, the primary oocytes are stimulated monthly by FSH (anterior pituitary) to grow, complete meiosis I and enter meiosis II stopping at metaphase II. Ø Ovulation occurs and the secondary oocyte is now released from the follicle.

3 Main Differences Between Spermatogenesis and Oogenesis Ø 1. Meiotic divisions of oogenesis are unequal. A single daughter cell becomes a secondary oocyte and the other products of cell division are called polar bodies and they degenerate.

3 Main Differences Between Spermatogenesis and Oogenesis Ø 2. Most cells from which eggs arise are not thought to be from cells which continuously arise. Ø 3. Oogenesis has long resting periods. By contrast, sperm are produced continuously.

Human Female Reproductive Cycle Ø The human female reproductive cycle is sometimes called the menstrual cycle and can be broken into 2 phases: Ø The ovarian cycle Ø The uterine cycle

Vertebrate Reproductive Systems: Ovaries Ø The corpus luteum’s main job is to secrete additional progesterone and estrogen that help to maintain the uterine lining during pregnancy. Ø The female reproductive system is not completely closed.

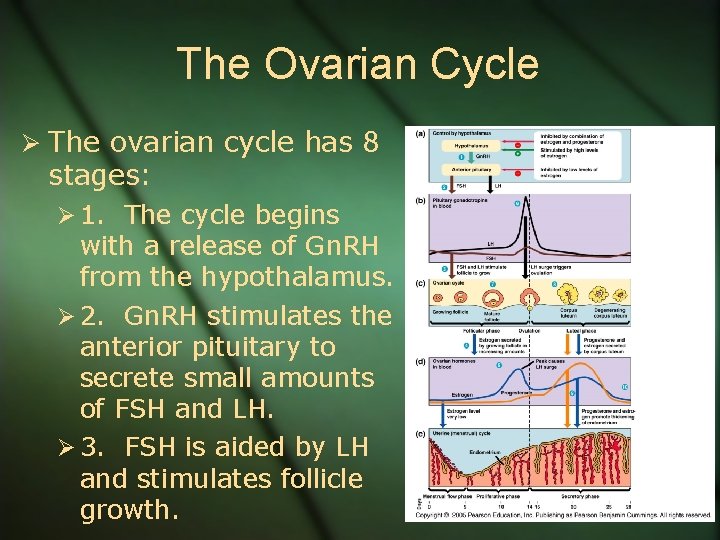
The Ovarian Cycle Ø The ovarian cycle has 8 stages: Ø 1. The cycle begins with a release of Gn. RH from the hypothalamus. Ø 2. Gn. RH stimulates the anterior pituitary to secrete small amounts of FSH and LH. Ø 3. FSH is aided by LH and stimulates follicle growth.

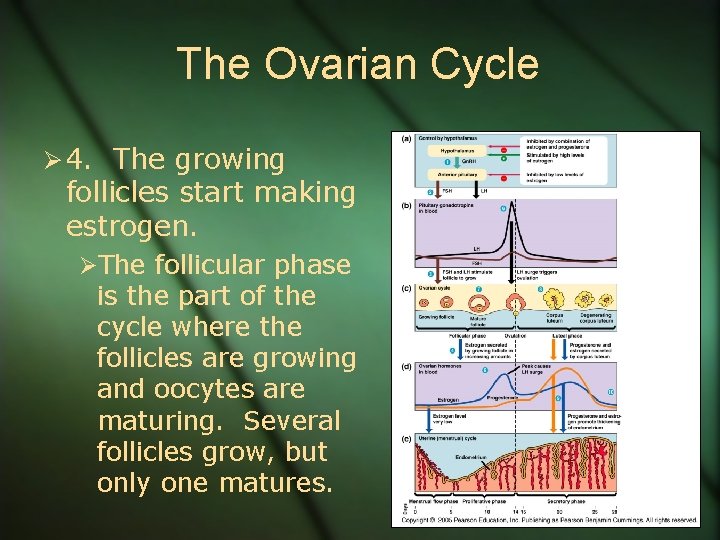
The Ovarian Cycle Ø 4. The growing follicles start making estrogen. ØThe follicular phase is the part of the cycle where the follicles are growing and oocytes are maturing. Several follicles grow, but only one matures.

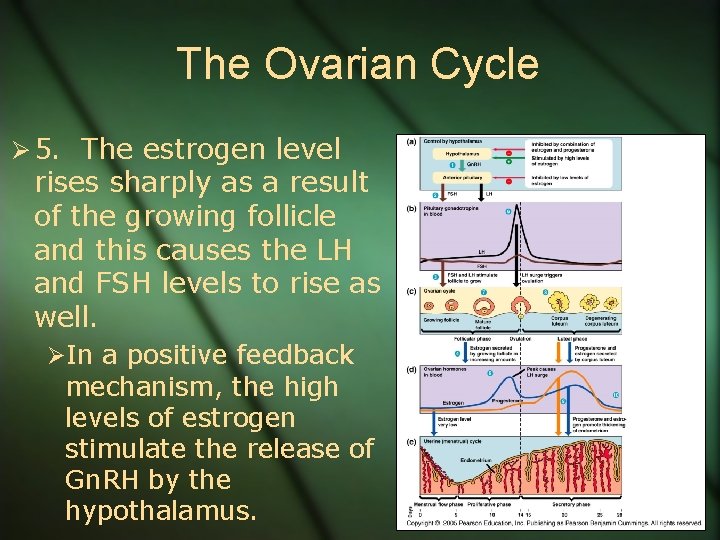
The Ovarian Cycle Ø 5. The estrogen level rises sharply as a result of the growing follicle and this causes the LH and FSH levels to rise as well. ØIn a positive feedback mechanism, the high levels of estrogen stimulate the release of Gn. RH by the hypothalamus.

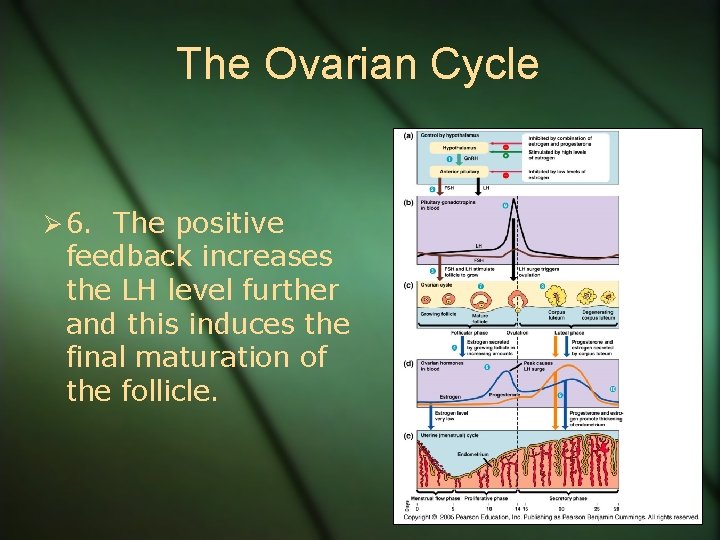
The Ovarian Cycle Ø 6. The positive feedback increases the LH level further and this induces the final maturation of the follicle.

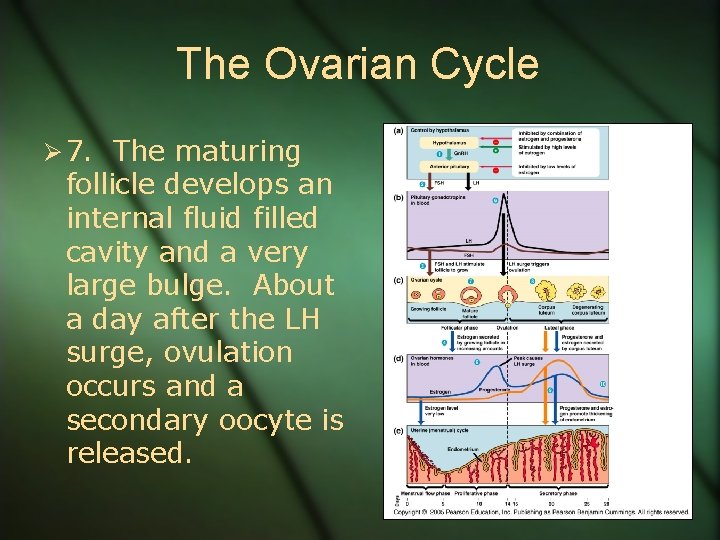
The Ovarian Cycle Ø 7. The maturing follicle develops an internal fluid filled cavity and a very large bulge. About a day after the LH surge, ovulation occurs and a secondary oocyte is released.

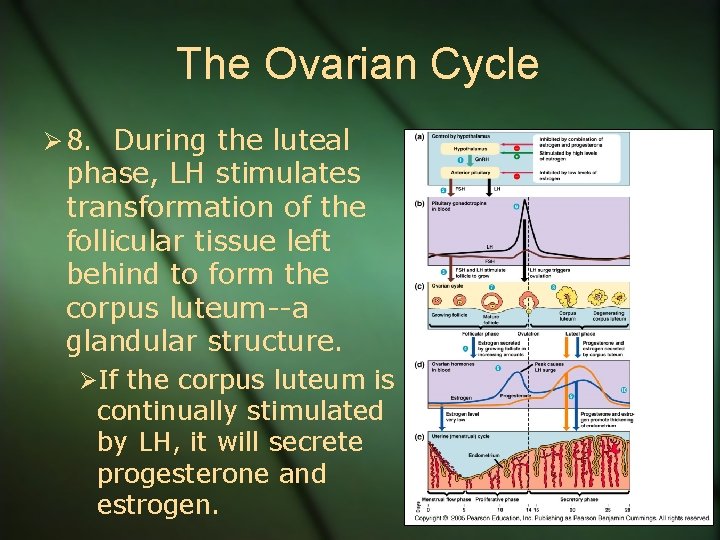
The Ovarian Cycle Ø 8. During the luteal phase, LH stimulates transformation of the follicular tissue left behind to form the corpus luteum--a glandular structure. ØIf the corpus luteum is continually stimulated by LH, it will secrete progesterone and estrogen.

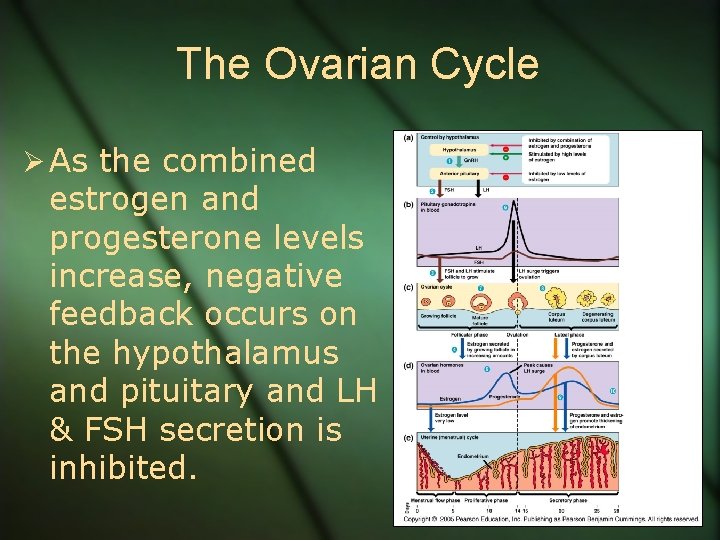
The Ovarian Cycle Ø As the combined estrogen and progesterone levels increase, negative feedback occurs on the hypothalamus and pituitary and LH & FSH secretion is inhibited.

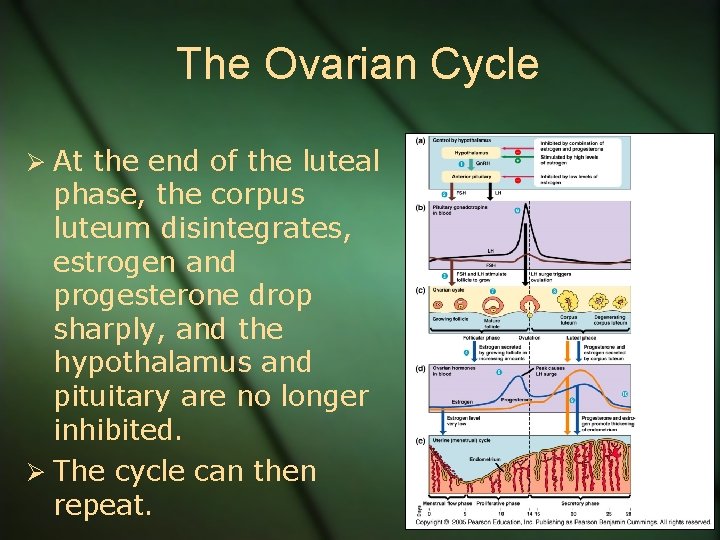
The Ovarian Cycle Ø At the end of the luteal phase, the corpus luteum disintegrates, estrogen and progesterone drop sharply, and the hypothalamus and pituitary are no longer inhibited. Ø The cycle can then repeat.

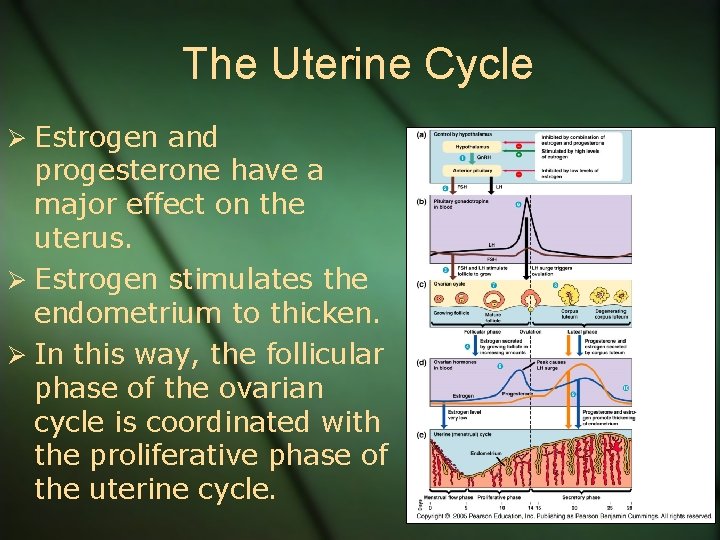
The Uterine Cycle Ø Estrogen and progesterone have a major effect on the uterus. Ø Estrogen stimulates the endometrium to thicken. Ø In this way, the follicular phase of the ovarian cycle is coordinated with the proliferative phase of the uterine cycle.

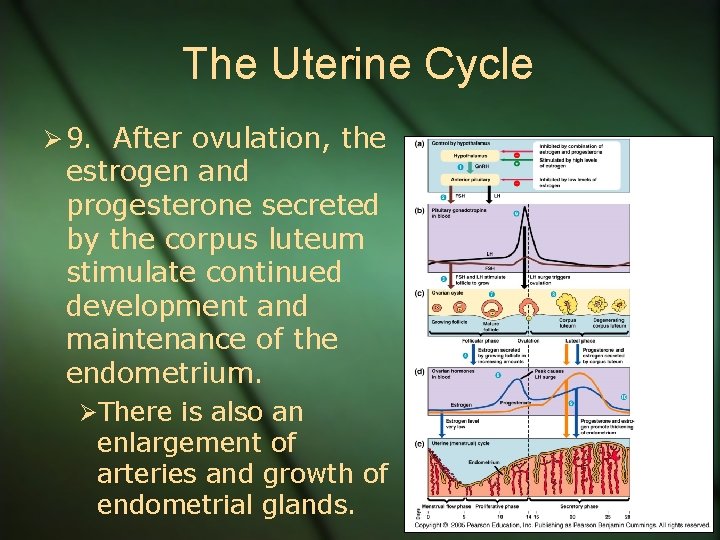
The Uterine Cycle Ø 9. After ovulation, the estrogen and progesterone secreted by the corpus luteum stimulate continued development and maintenance of the endometrium. ØThere is also an enlargement of arteries and growth of endometrial glands.

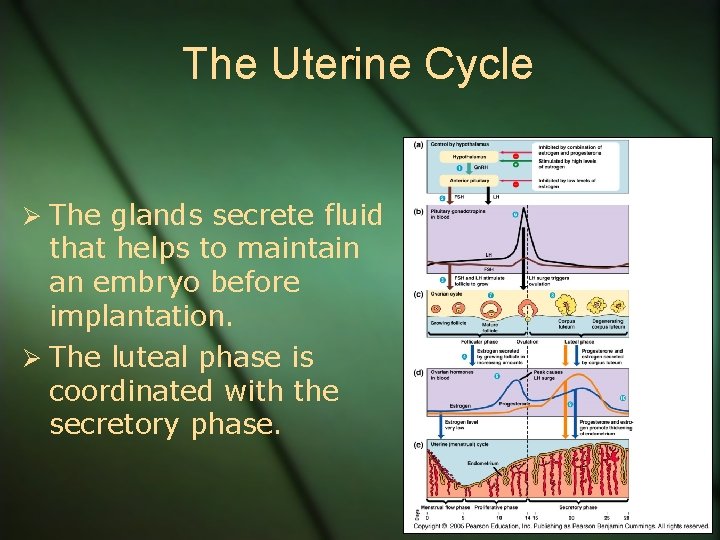
The Uterine Cycle Ø The glands secrete fluid that helps to maintain an embryo before implantation. Ø The luteal phase is coordinated with the secretory phase.

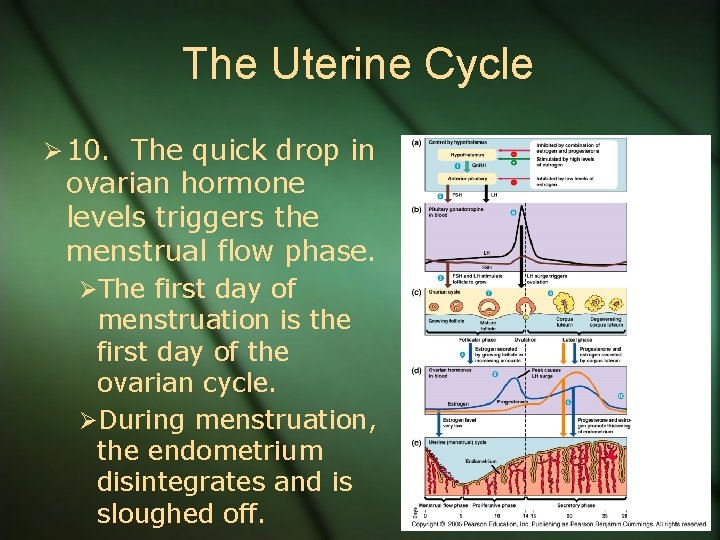
The Uterine Cycle Ø 10. The quick drop in ovarian hormone levels triggers the menstrual flow phase. ØThe first day of menstruation is the first day of the ovarian cycle. ØDuring menstruation, the endometrium disintegrates and is sloughed off.