Chapter 41 Fluid Electrolyte and AcidBase Balance Characteristics

Chapter 41 Fluid, Electrolyte, and Acid-Base Balance

Characteristics of Body Fluids Fluid = Water that contains dissolved or suspended substances such as glucose, mineral salts, and proteins. Fluid amount = Volume. Fluid concentration = Osmolality. Fluid composition (electrolyte concentration) Degree of acidity = p. H
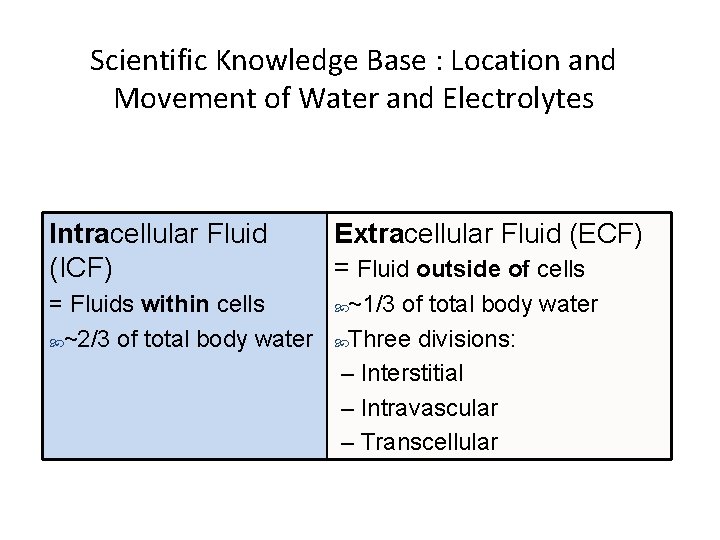

Scientific Knowledge Base : Location and Movement of Water and Electrolytes Intracellular Fluid (ICF) = Fluids within cells ~2/3 of total body water Extracellular Fluid (ECF) = Fluid outside of cells ~1/3 of total body water Three divisions: – Interstitial – Intravascular – Transcellular
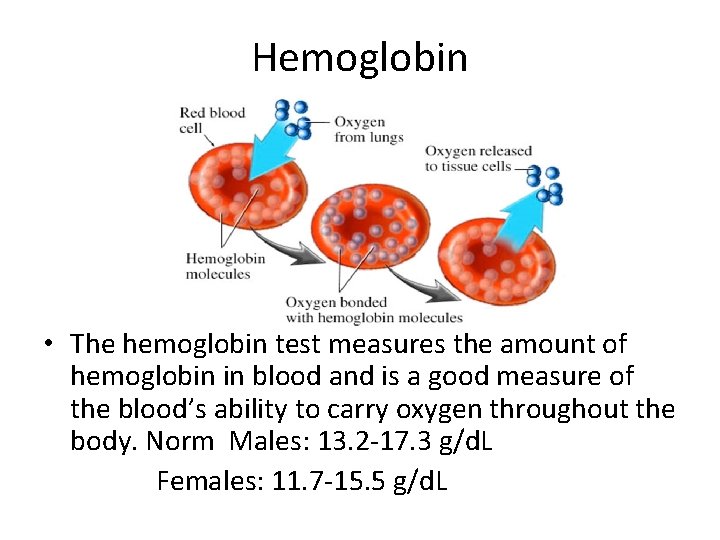
Hemoglobin • The hemoglobin test measures the amount of hemoglobin in blood and is a good measure of the blood’s ability to carry oxygen throughout the body. Norm Males: 13. 2 -17. 3 g/d. L Females: 11. 7 -15. 5 g/d. L

Hematocrit This test measures the amount of space (volume) red bloods cells take up in the blood. The value is given as a % of RBCs in a volume of blood. For example, a hematocrit of 38 means that 38% of the blood’s volume is made of RBCs. Norm: Male: 39%-50% Females: 35%-47%
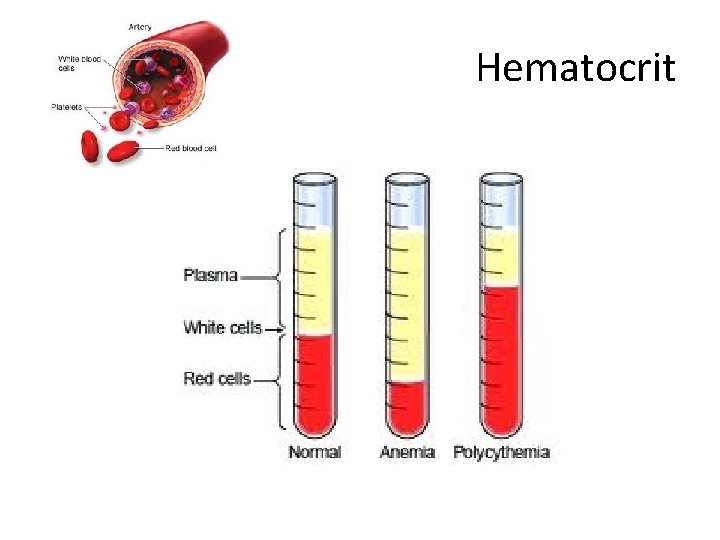
Hematocrit
ECF Volume deficit Hypovolemia �Causes �Abnormal fluid loss �Diarrhea �Fistula drainage �Hemorrhage �Polyuria �Fever (↑ perspiration) �Inadequate intake �Osmotic diuresis 7

ECF Volume deficit Hypovolemia: Sign and Symptoms Cardiovascular Changes �Mild to moderate Respiratory Changes �↑ respiratory rate �↑ HR (due to SNS) �Peripheral pulses are weak, difficult to find �Change in position may cause ↑ HR or ↓ BP �Dizziness and lightheadedness �Severe fluid volume �↓ BP in lying position �Pulse: weak, thready �Flattened neck veins 8

ECF Volume deficit Hypovolemia: Sign and Symptoms Renal Changes �UO below 500 m. L/day Neurologic changes �Alteration in Mental Status �Restlessness �Drowsiness �Lethargy �Confusion (more common in the elderly; may be first indicator of fluid balance problem) �Seizures, coma 9

ECF Volume deficit Hypovolemia: Sign and Symptoms �Skin turgor is diminished �Skin may be warm and dry with mild deficit �Skin may be cool and moist with severe deficit �Skin may appear dry and wrinkled �Oral mucous membranes will be dry, sticky, pastelike coating and the tongue may be furrowed �Patient C/O thirst �Eyes: soft, sunken �Lab data: �↑ H & H; BUN; 10

Nursing Care Plan Therapeutic Interventions �Restore fluid and electrolyte balance �IVs and blood products as ordered; small, frequent drinks by mouth �Daily weights to monitor progress of fluid replacement �Loss or gain of 2. 2 lbs is equal to 1 L of fluid �I & O, hourly outputs �Two most important assessments: HR & Output �Avoid hypertonic solutions �Promote comfort �Frequent skin care �Position: change q hr to relieve pressure �meds as ordered: antiemetics, antidiarrheal 11

Nursing Care Plan Therapeutic Interventions �Prevent physical injury �Risk for falls due to orthostatic hypotension, dysrhythmia, muscle weakness, gait stability and level of alertness. �Frequent mouth care �Dry mucous membrane due to dehydration �Monitor IV flow rate �Observe for circulatory overload (↑ pulse, ↑ HR) �Pulmonary edema (SOB) �Monitor vital signs �BP should be rising, ↑ LOC: more alert 12

ECF Volume excess Hypervolemia • Causes – Excessive intake of fluids – Abnormal retention of fluids • Heart failure • Renal failure – Long-term corticosteroid therapy 13
ECF Volume excess Hypervolemia: Signs and symptoms Cardiovascular Changes �↑ Pulse: full and bounding �Full peripheral pulses �Distended neck veins �↑ BP Other Changes -Urine; polyuria, nocturia -Lab data ↓ Hematocrit, BUN Respiratory Changes �↑ respiratory rate �Shallow respirations �↑ dyspnea with exertion or in the supine position �Pulmonary congestion and pulmonary edema �SOB �Irritative cough �Moist crackles 14
ECF Volume excess Hypervolemia: Signs and symptoms Neurologic changes �Altered LOC �Visual disturbances �Skeletal muscle weakness �Paresthesias �Cerebral edema �Headache �Confusion �Lethargy �Diminished reflexes �Seizures, coma �Skin �Edematous may feel cool �Skin may feel taut and hard �Edema-eyelids, facial, dependent (sacrum), pitting, peripheral extremities �GI Changes �Increased motility �Enlarged liver 15

Nursing Care Plan Therapeutic Interventions �Maintain oxygen to all cells �Position: sim-Fowler’s or Fowler’s to facilitate improved gas exchange. �Vital signs; q 4 hrs and PRN �Tachycardia �↑ BP (overload) and ↓ BP (fluid deficit) �Fluid restriction: I & O �Promote excretion of excess fluid �Meds as ordered: diuretics �Monitor electrolytes, esp. Mg and K 16

Nursing Care Plan Therapeutic Interventions �Obtain/maintain fluid balance �Wt gain is the best indicator of fluid retention and overload �Weight daily; 2. 2 lbs = 1 Liter (1000 ml) �Measure: all edematous parts, abdominal girth, �I & O: fluid restriction �Limit fluids by mouth, IVs per doctors orders �Strict monitoring of IV fluids �Prevent tissue injury �Skin and mouth care as needed �Evaluate feet for edema and discoloration when client is OOB �Observe suture line on surgical clients (Potential for evisceration due to excess fluid retention) 17

Functions of Sodium • Regulates osmolality – ICF: 14 mmol/L & ECF: 135 -145 mmol/L • Helps maintain blood pressure by balancing the volume of water in the body • Works with other electrolytes to promote nerves, muscles and other body tissues to work properly. 18

Hypernatremia Water loss: Causes �Inadequate water intake �Unconscious or cognitively impaired individuals �NPO status �Excessive water loss �↑ insensible water loss � High fever �Diuretic therapy �Watery diarrhea �Disease states �Uncontrolled diabetes mellitus Water loss: Signs and Symptoms • Restlessness, agitation, twitching, confusion • Seizures*, Coma • Intense thirst • Dry, swollen tongue • Sticky mucous membranes • Weight loss • Weakness, lethargy • Postural hypotension 19

Hypernatremia Na gain: Causes Na gain: Signs and Symptoms �Na intake • Restlessness, agitation, twitching • Seizures, Coma • Intense thirst • Flushed skin • Weight gain • Peripheral and pulmonary edema • ↑ BP �IV fluids: hypertonic Na. Cl, excessive isotonic Na. Cl �Hypertonic tube feeding with out water supplement �Use of Na containing drugs �corticosteroids �Diseases � Renal failure 20

Hyponatremia • Dilutional (↑ ECF Volume) Causes – Use of hypotonic irrigation solution – Tap water enemas – Excessive water gain • Excessive hypotonic IV fluid �Dilutional (↑ ECF Volume) Signs and Symptoms �Headache, apathy, confusion �Nausea, vomiting, anorexia � Lethargy � Weakness �Muscle spasms, seizures, coma �Diarrhea, Abdominal cramps �Weight gain �↑ BP 21

Hyponatremia �Na Loss: Causes �GI �Vomiting �Diarrhea �NG suctioning �NPO Status �Kidney �Diuretic �Skin � • Burns • Wounds • Excessive diaphoresis �Na Loss: Signs and Symptoms �Irritability, apprehension, confusion �Dizziness �Personality changes � Tremors, seizures, coma � Dry mucous membranes � Postural hypotension �Tachycardia, thread pulse � Cold & clammy skin 22

Functions of Potassium • Maintains fluid balance in the cells – Contributes to intracellular osmotic pressure • Direct effect on excitability of nerves and muscles – Skeletal, cardiac, and smooth muscle contraction • Regulates glucose use and storage 23

Hyperkalemia Causes • Most cases of hyperkalemia occur in hospitalized patients and in those undergoing medical treatment. • Those at greatest risk for hyperkalemia are – Chronically ill patients – Debilitated patients – Older adult 24

Hyperkalemia Causes Actual hyperkalemia • Excess potassium Intake – Excessive or rapid parenteral administration Relative hyperkalemia • Shift of potassium Out of Cells – Acidosis – Crushing injury – Tissue catabolism (fever, sepsis, burns) 25

Hyperkalemia Causes • Failure to Eliminate Potassium – Renal disease – Potassium-sparing diuretics – ACE inhibitors 26

Hyperkalemia Signs and Symptoms Clinical Manifestations �Irritability �Abdominal cramping, diarrhea �Weakness of lower extremities �Irregular pulse �Cardiac arrest if hyperkalemia sudden or severe Electrocardiogram Changes • Ventricular fibrillation • Ventricular standstill 27

Hypokalemia Causes • Potassium Loss – GI losses: diarrhea, vomiting, fistulas, NG suction, NPO status – Renal losses: diuretics, – Skin losses: diaphoresis – Dialysis • Shift of Potassium into Cells – Alkalosis 28

Hypokalemia Causes • Lack of Potassium Intake – Starvation – Diet low in K – Failure to include K in parenteral fluids if NPO – TPN 29

Hypokalemia Signs and Symptoms Clinical Manifestations �Fatigue �Muscle weakness, leg cramps �Nausea, vomiting, paralytic ileus �Soft, flabby muscles �Paresthesias, decreased reflexes �Weak, irregular pulse Electrocardiogram Changes • Ventricular dysrhythmias (e. g. , PVCs) • Bradycardia 30

Hypokalemia Medical Management �Administration of KCl supplements �K may be given orally (K chloride, K gluconate, K citrate) or IV �KCl should be administered IV at a rate of 10 to 20 m. Eq/L over an hour. Rapid infusion could cause cardiac arrest �IV K solutions irritate veins and cause phlebitis. Check IV site q 2 hrs. Discontinue IV if infiltrate to prevent necrotic and slough of tissue 31

Functions of Calcium • Helps maintain muscle tone • Contributes to regulation of blood pressure by maintaining cardiac contractility • Necessary for nerve transmission and contraction of skeletal and cardiac muscle 32

Hypercalcemia Causes �Increased Total Calcium �Prolonged immobilization �Thiazide diuretics �Dehydration �Renal failure 33

Hypercalcemia Signs and Symptoms Clinical Manifestations �Lethargy, weakness �Depressed reflexes (DTR) �Decreased memory �Confusion, personality changes, psychosis �Anorexia, nausea, vomiting, constipation �Bone pain, fractures Electrocardiogram Changes • Ventricular dysrhythmias • Hypertension 34

Hypocalcemia Causes �Decreased Total Calcium �Chronic renal failure �Loop diuretics (e. g. , furosemide [Lasix]) �Chronic alcoholism �Diarrhea �Decreased Ionized Calcium �Excess administration of citrated blood 35

Hypocalcemia Signs and Symptoms Clinical Manifestations �Easy fatigability �Depression, anxiety, confusion �Numbness and tingling in extremities and region around mouth • Hyperreflexia, muscle cramps • Chvostek’s sign & Trousseau’s sign • Laryngeal spasm • Tetany, seizures Electrocardiogram Changes • Ventricular tachycardia 36

Functions of Magnesium • Cofactor in clotting cascade • muscular irritability and contractions • Maintains strong and healthy bones 37

Hypermagnesemia Causes �Renal failure �Diabetes Mellitus �Clients who ingest large amounts of Mgcontaining antacids such as Tums, Maalox, Mylanta, or laxatives such as MOM are also in ↑ risk for developing hypermagnesemia 38

Hypermagnesemia Signs and Symptoms – Bradycardia and hypotension – Severe hypermagnesemia: cardiac arrest – Drowsy or lethargic – Coma – Deep tendon reflexes are reduced or absent – Skeletal muscle contractions become progressively weaker and finally stop 39

Hypomagnesaemia Causes • Malabsorption disorders – Inflammatory bowel disease (IBD) – Bowel resection – Bariatric population who undergoes gastric bypass surgery • Alcoholism • Prolonged diarrhea • Draining GI fistulas • Diuretics 40

Hypomagnesaemia Signs and Symptoms • Confusion • Hyperactive deep tendon reflexes • Tremors • Seizures • Neuromuscular changes – Hyperactive deep tendon reflexes – Numbness and tingling – Painful muscle contractions – Monitor for positive Chvostek’s and Trousseau’s signs (hypocalemia may 41

Case Study • Susan Reynolds, a 42 -year-old married accountant, has just been admitted to the acute care unit with a history of nausea, loss of appetite, and vomiting and diarrhea for 7 days. She feels her symptoms are related to “bad food” she had on her recent business trip. Past medical history includes hypertension controlled by furosemide (Lasix) 40 mg by mouth once a day and a no -salt-added diet.

Discussion • What is Mrs. Reynolds at risk for? • What will you assess? • How does Lasix factor into this situation? – What lab should be monitored when administering this medication? 43

• Mrs. Reynolds’ electrolytes are out of balance due to the vomiting and diarrhea. Lasix therapy compounds this issue because Lasix is a diuretic that causes fluid loss. • Reference: Pg. 887 44

Case Study (cont’d) • Mrs. Reynolds’ physician has admitted her for observation and has obtained a blood sample for electrolyte levels, CBC, and an ECG. Orders include nothing by mouth, an IV infusion of 0. 9% saline at 125 m. L/hr, intake and output (I&O) recordings, and vital signs every 4 hours, in addition to daily weights. • What assessment activities do you anticipate Robert will perform?

What should Robert Assess? • Ask Mrs. Reynolds to describe her nausea and what accompanying signs and symptoms she is experiencing. • Conduct an examination of GI and urinary function. • Assess Mrs. Reynolds’ vital signs. • Assess Mrs. Reynolds’ skin and mucous membranes for indicators of dehydration. • Evaluate Mrs. Reynolds’ laboratory values and ECG results. • Reference: Pg. 895 46

Nursing Knowledge Base • Use the scientific knowledge base in clinical decision making to provide safe, optimal fluid therapy. • Apply knowledge of risk factors for fluid imbalances and physiology of normal aging when assessing older adults, knowing that this age group is at high risk for fluid imbalances. • Ask questions to elicit risk factors for fluid, electrolyte, and acid-base imbalances. • Perform clinical assessments for signs and symptoms of these imbalances.
Nursing Process: Assessment • Nursing history – Age: very young and old at risk – Environment: excessively hot? – Dietary intake: fluids, salt, foods rich in potassium, calcium, and magnesium – Lifestyle: alcohol intake history – Medications: include over-the-counter (OTC) and herbal, in addition to prescription medications

Nursing Process: Assessment (cont’d) • Medical history – Recent surgery (physiological stress) – Gastrointestinal output – Acute illness or trauma • Respiratory disorders • Burns • Trauma – Chronic illness • Cancer • Heart failure • Oliguric renal disease

Physical Assessment • Daily weights – Indicator of fluid status – Use same conditions. • Fluid intake and output (I&O) – 24 -hour I&O: compare intake versus output – Intake includes all liquids eaten, drunk, or received through IV. – Output = Urine, diarrhea, vomitus, gastric suction, wound drainage • Laboratory studies

Case Study (cont’d) • Mrs. Reynolds states that she has no appetite, is nauseous, and has been vomiting and has had diarrhea for 7 days. • Bowel sounds are hyperactive in all four quadrants. The patient has had only two loose stools since midnight. She voids with difficulty, with dark yellow urine. Her 24 -hour intake was 1850 m. L; her output was 2200 m. L (of which urine was only 1000 m. L). • Temperature 99. 6° F; pulse 100 bpm; BP 110/60 mm Hg with no changes when standing

What’s wrong? • The assessment findings indicate that Mrs. Reynolds is dehydrated. • Reference: Pg. 895 52

Case Study (cont’d) • Mrs. Reynolds’ laboratory results: – Hematocrit 44% (suggesting hypovolemia) – Potassium 3. 6 m. Eq/L and sodium 138 m. Eq/L (both low normal because of prolonged vomiting and diarrhea) – Electrocardiogram (ECG) showed normal sinus rhythm.

Nursing Diagnosis ? ? ? ? ?

Possible nursing diagnoses for Mrs. Reynolds include: 1. Risk for electrolyte imbalance 2. Fluid volume deficit 3. Impaired oral mucous membrane 4. Deficient fluid volume related to excessive diarrhea, vomiting, and use of potassiumwasting diuretic Reference: Pg. 900 55

Case Study (cont’d) • Nursing diagnosis: Deficient fluid volume related to excessive diarrhea, vomiting, and use of potassium-wasting diuretic

GOALS – Mrs. Reynolds’ fluid volume will return to normal by time of discharge. – Mrs. Reynolds will achieve normal electrolyte balance by discharge. – What are 3 other goals? • 1. • 2. • 3. 57

Planning • Goals and outcomes • Setting priorities • Collaborative care

Expected Outcomes ? ? ? ? 59

Case Study (cont’d) • Fluid balance – – Urine output will equal intake of ~1500 m. L in 2 days. Mucous membranes will be moist in 24 hours. Skin turgor will return to normal within 24 hours. Daily weights will not vary by more than 2 lbs over the next 2 days. • Electrolyte and acid-base balance – Serum electrolyte and blood counts will be within normal limits within 48 hours. – Mrs. Reynolds will not have any nausea or vomiting in 24 hours.

Nursing Interventions • Interventions for electrolyte imbalances – Support prescribed medical therapies – Aim to reverse the existing acid-base imbalance – Provide for patient safety

Interventions & Rationales ? ? ? ? ? 62

Interventions • Administer IV fluids (0. 9% normal saline) at 125 m. L/hr. – 1. Replacement of body fluid restores blood volume and normal serum electrolyte levels; an isotonic solution expands the body’s intravascular fluid volume without causing a fluid shift from one compartment to another. • Provide patient with an additional 480 m. L of noncaffeinated oral fluids every 8 hours. – 2. Pepto-Bismol is an antidiarrheal to inhibit GI secretions, stimulate absorption of fluid and electrolytes, inhibit intestinal inflammation, and suppress the growth of Helicobacter pylori.

Interventions and Rationales 1. Maintain accurate I&O measurements. a. I&O documents hydration and fluid balance for directing therapy. 2. Weigh Mrs. Reynolds daily; monitor trends. a. Daily weights provide reliable data of fluid balance. 3. Teach Mrs. Reynolds and family about specific dietary modification (potassium-rich foods). a. Furosemide (Lasix) is a potassium-wasting diuretic. The body does not store potassium, thus requiring dietary supplements rich in potassium. Reference: Pg. 903 64

Implementation • Health promotion – Fluid replacement education – Teach patients with chronic conditions about risk factors and signs and symptoms of imbalances. • Acute care – Enteral replacement of fluids – Restriction of fluids – Parenteral replacement of fluids and electrolytes • Total parenteral nutrition • Crystalloids (electrolytes) • Colloids (blood and blood components)

Implementation • Restorative care – Home intravenous therapy – Nutrition support – Medication safety • Medications • OTC drugs • Herbal preparations

Case Study (cont’d) • Nursing actions: – Monitor electrolyte levels and daily weights. – Inspect oral mucous membranes; assess skin turgor. – Evaluate I&O trends during next 48 hours. • Findings – Serum electrolyte levels: potassium 4. 0 m. Eq/L and sodium 140 m. Eq/L – Mucous membranes remain dry; skin turgor normal – Mrs. Reynolds’ 24 -hour intake is 2800 m. L, and output is 2200 m. L with 1800 m. L urine. Urine specific gravity is 1. 025, and weight has returned to 143 lb.

Evaluation 1. Are the goals met? 2. How do we know?

Evaluation • Robert is encouraged by Mrs. Reynolds’ progress. He discusses sources of potassium in the diet and writes this documentation note: • “Denies nausea and reports feeling better. No diarrheal stool since yesterday afternoon around 3 p. m. On inspection, oral mucosa remains dry, without lesions or inflammation. Skin turgor is normal. Bowel sounds are normal in all four quadrants, abdomen soft to palpation. IV of 0. 9% normal saline is infusing in left cephalic vein in forearm at 40 m. L/hr per MD order. No tenderness or inflammation at IV site. Is able to identify five food sources for potassium to include in diet. Is resting comfortably, out of bed in a chair, ate all of breakfast. Will continue to monitor. ” • Reference: Pg. 914 69
- Slides: 69