Chapter 4 Benign Conditions Of Specific Reproductive Organs

Chapter 4: Benign Conditions Of Specific Reproductive Organs 1. Benign diseases of the vulva 2. Benign diseases of the vagina 3. Benign diseases of the cervix 4. Benign diseases of the uterus 5. Benign diseases of the ovary 6. The breast in gynecological practice

BENIGN DISEASES OF THE VULVA

SWELLINGS OF THE VULVA
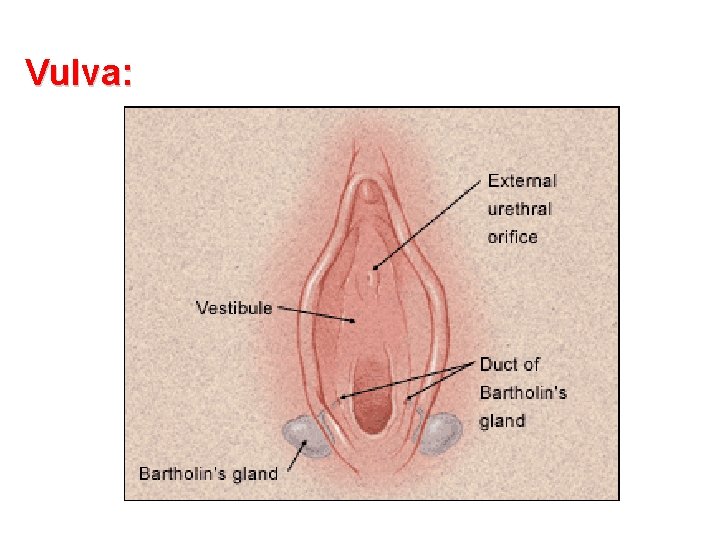
Vulva:
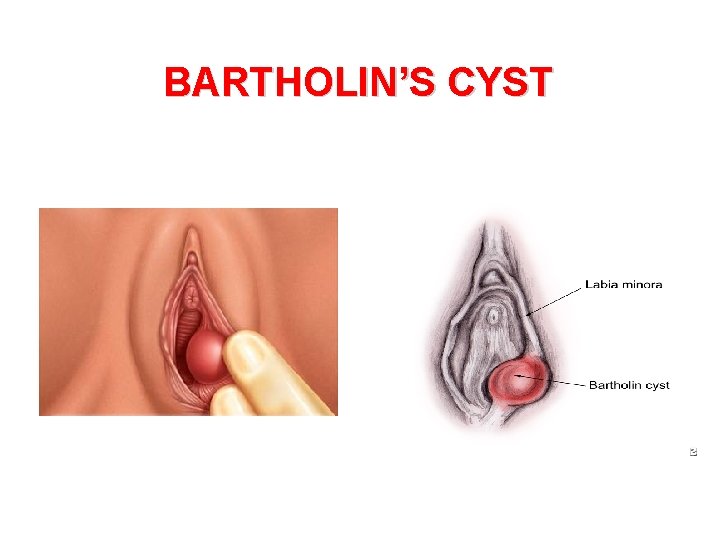
BARTHOLIN’S CYST
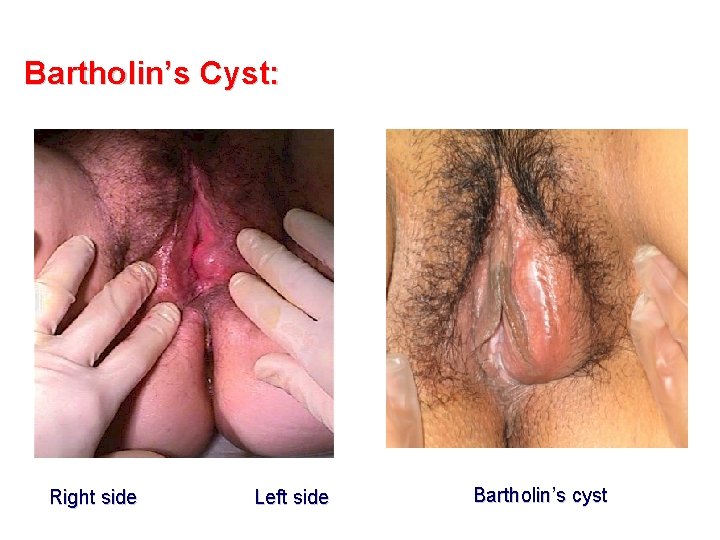
Bartholin’s Cyst: Right side Left side Bartholin’s cyst
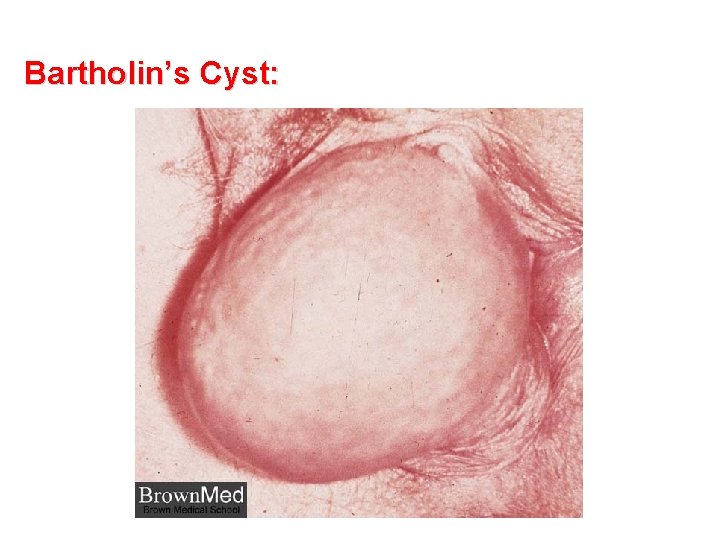
Bartholin’s Cyst:
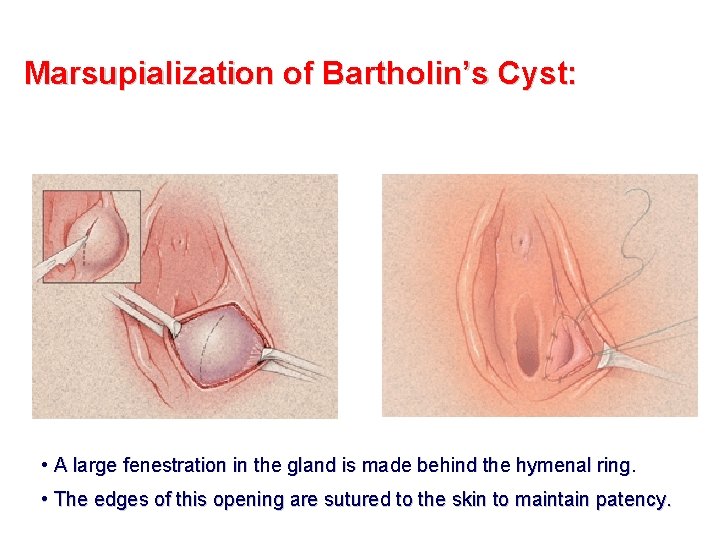
Marsupialization of Bartholin’s Cyst: • A large fenestration in the gland is made behind the hymenal ring. • The edges of this opening are sutured to the skin to maintain patency.
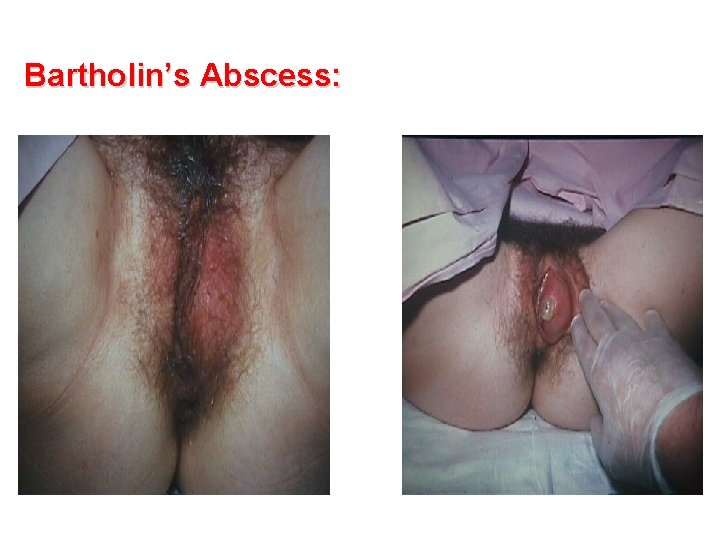
Bartholin’s Abscess:
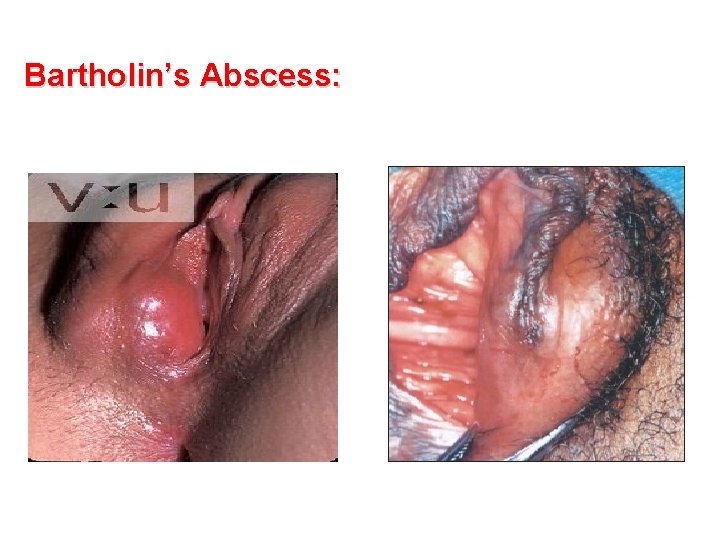
Bartholin’s Abscess:
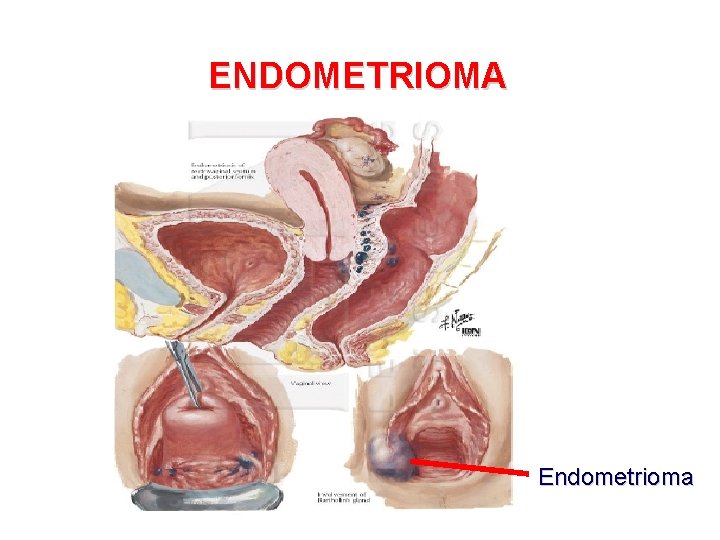
ENDOMETRIOMA Endometrioma
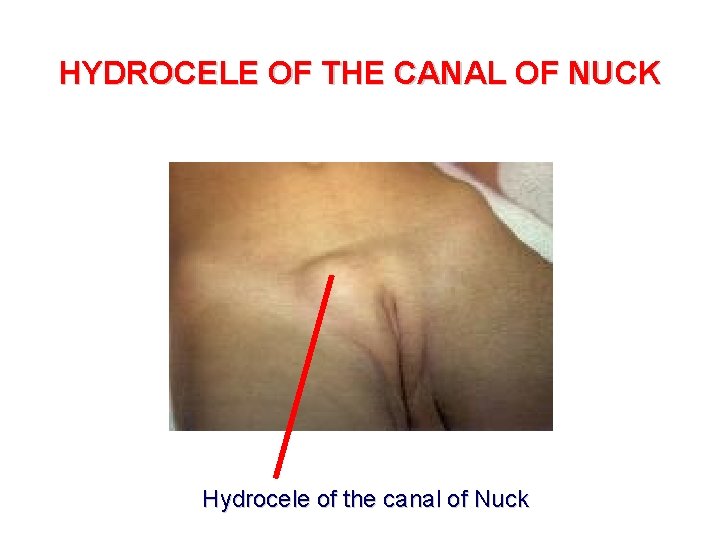
HYDROCELE OF THE CANAL OF NUCK Hydrocele of the canal of Nuck
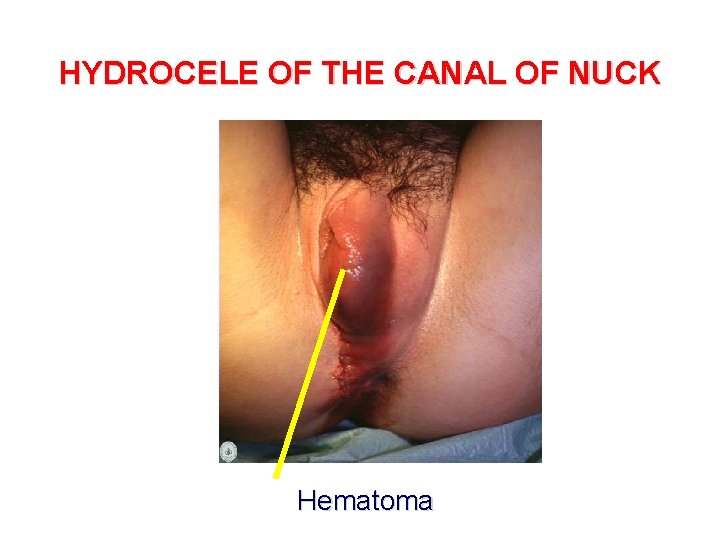
HYDROCELE OF THE CANAL OF NUCK Hematoma
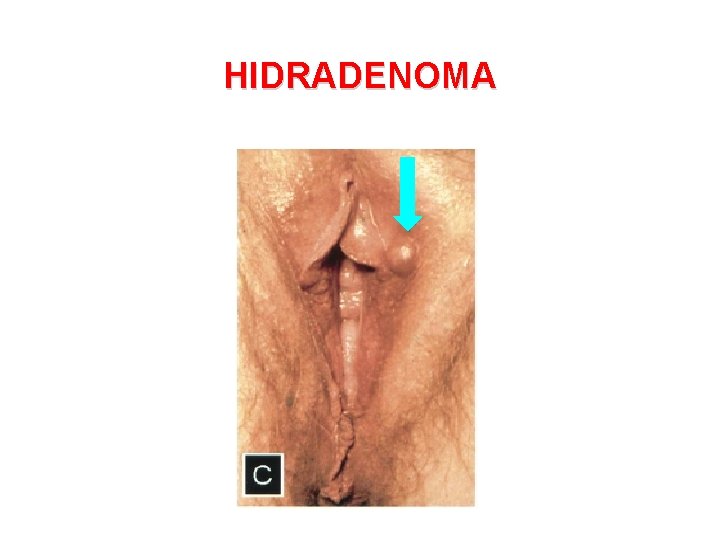
HIDRADENOMA
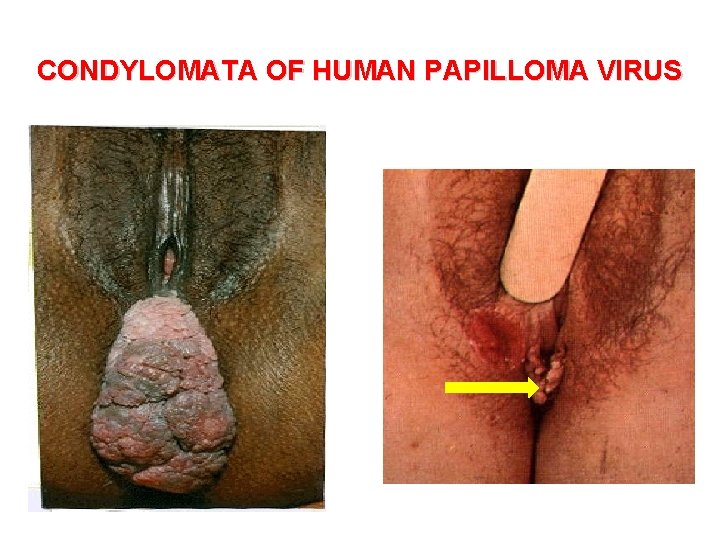
CONDYLOMATA OF HUMAN PAPILLOMA VIRUS
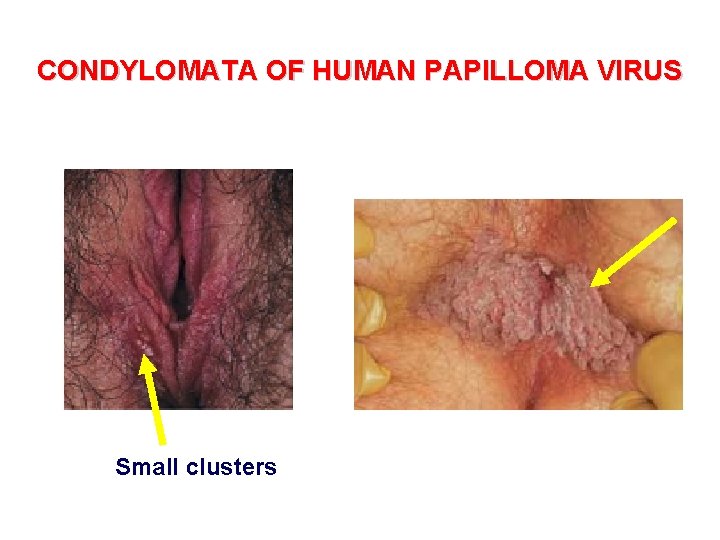
CONDYLOMATA OF HUMAN PAPILLOMA VIRUS Small clusters

ULCERS OF THE VULVA
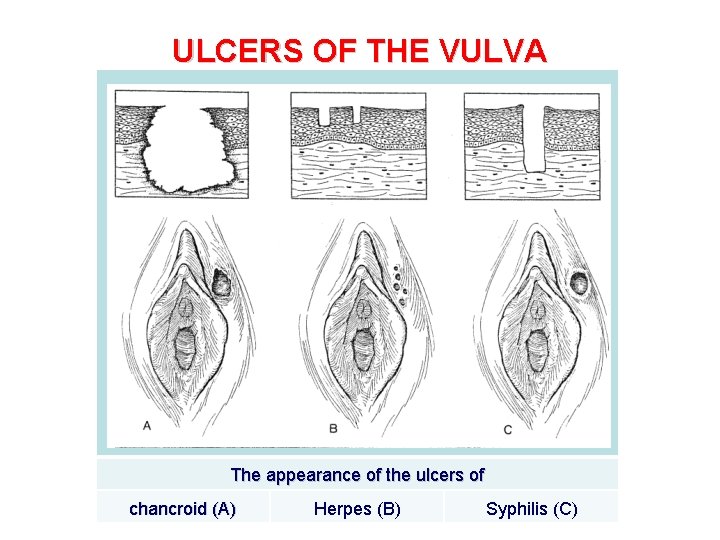
ULCERS OF THE VULVA The appearance of the ulcers of chancroid (A) Herpes (B) Syphilis (C)
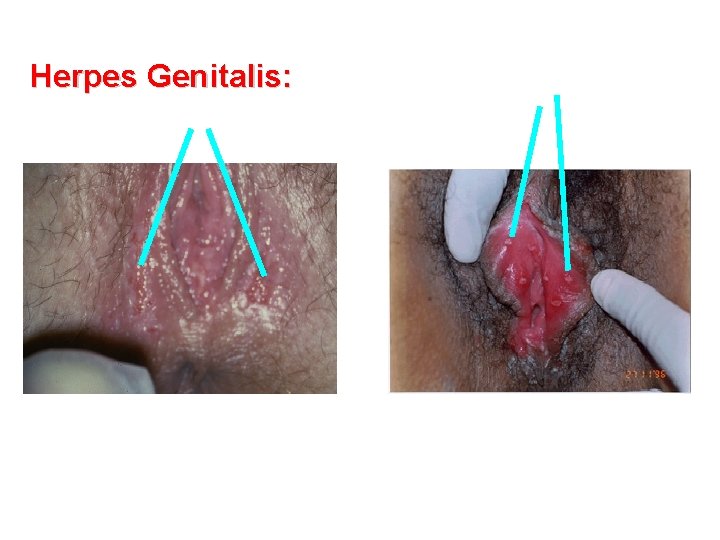
Herpes Genitalis:

EPITHELIAL DISORDERS OF THE VULVA
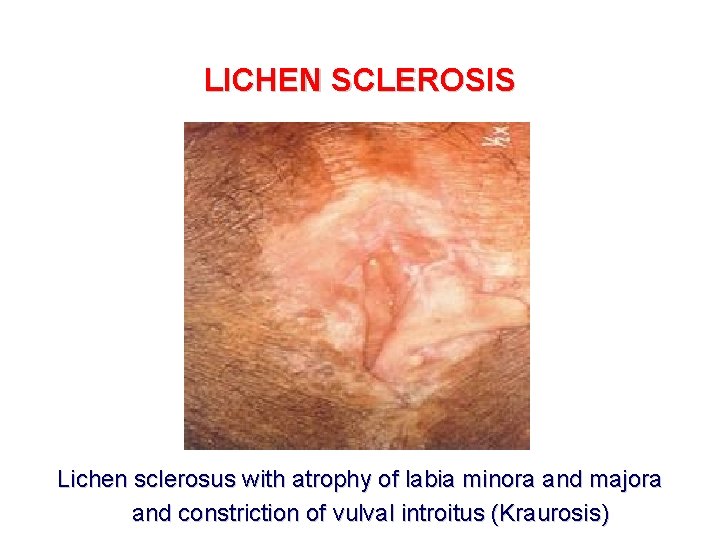
LICHEN SCLEROSIS Lichen sclerosus with atrophy of labia minora and majora and constriction of vulval introitus (Kraurosis)
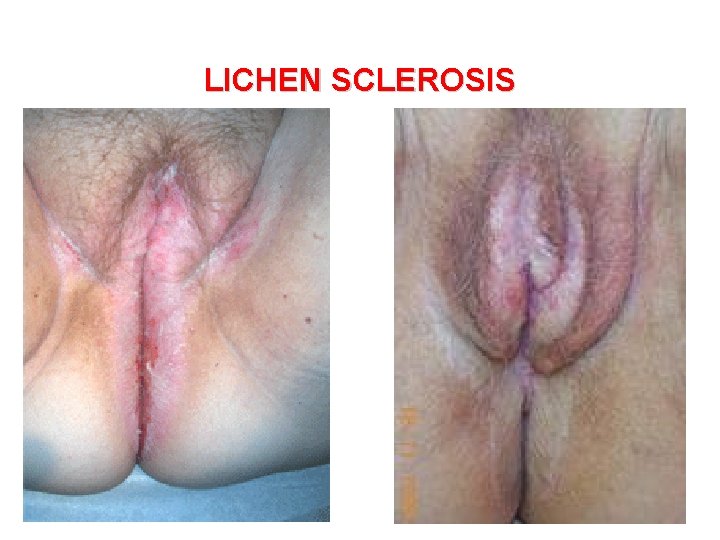
LICHEN SCLEROSIS
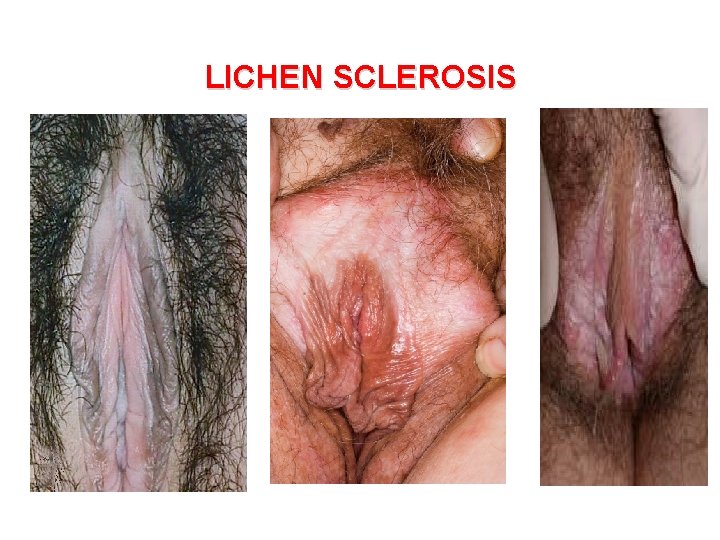
LICHEN SCLEROSIS
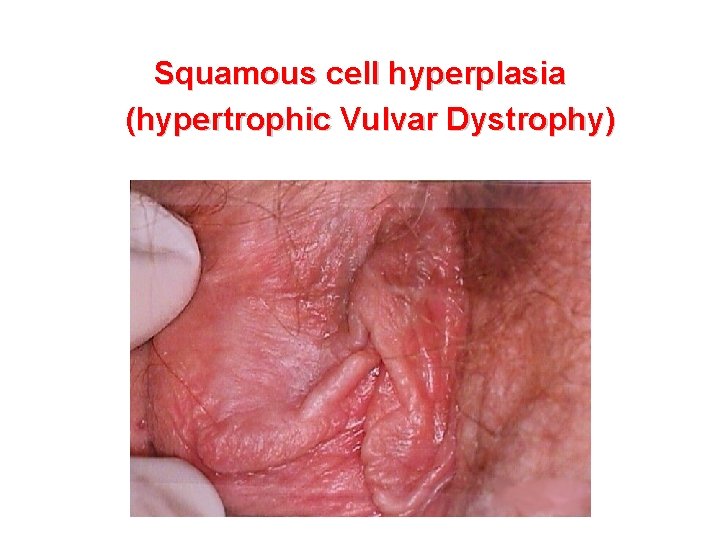
Squamous cell hyperplasia (hypertrophic Vulvar Dystrophy)
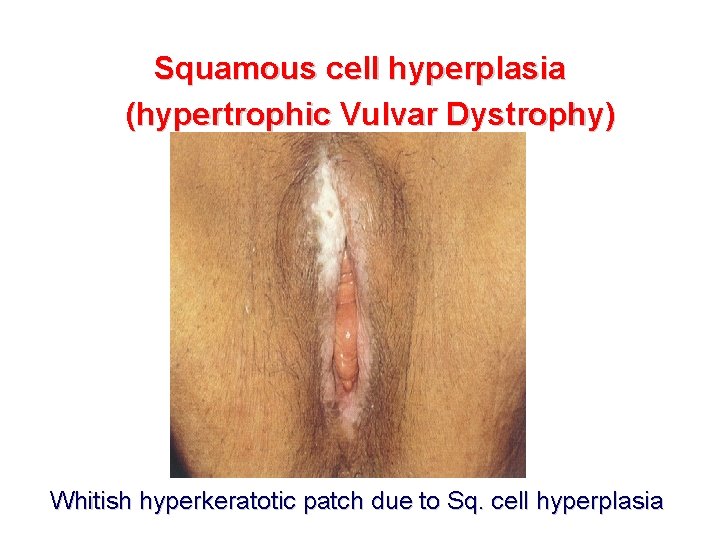
Squamous cell hyperplasia (hypertrophic Vulvar Dystrophy) Whitish hyperkeratotic patch due to Sq. cell hyperplasia
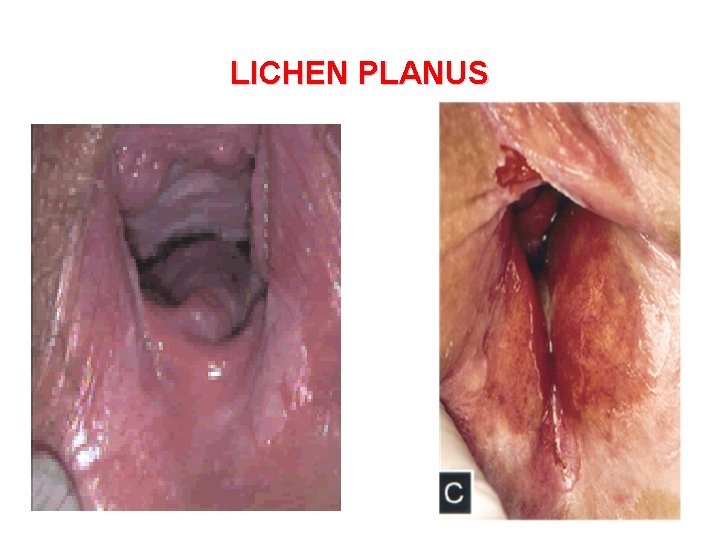
LICHEN PLANUS
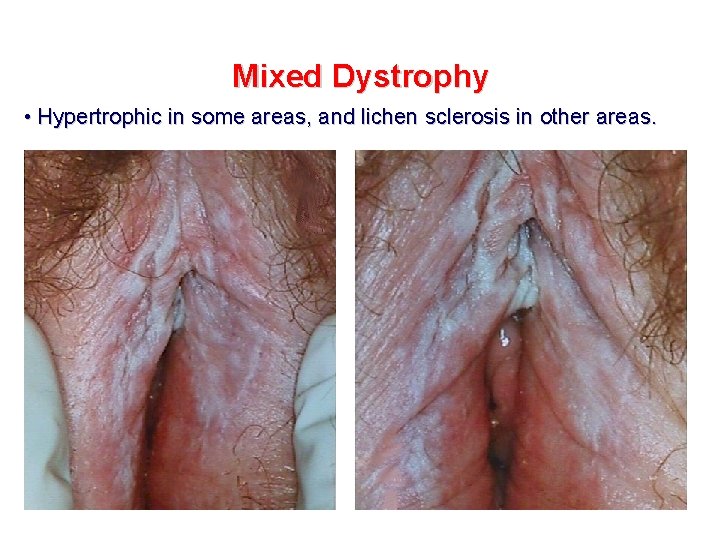
Mixed Dystrophy • Hypertrophic in some areas, and lichen sclerosis in other areas.

BENIGN DISEASES OF THE VAGINA

SWELLINGS OF THE VAGINA
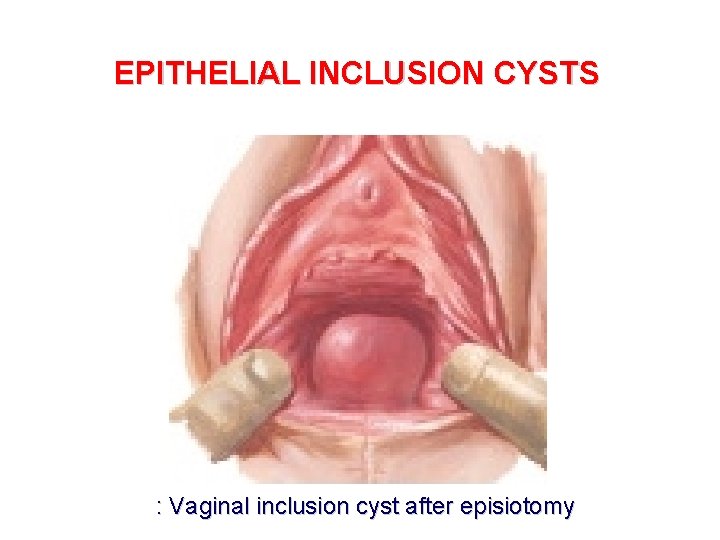
EPITHELIAL INCLUSION CYSTS : Vaginal inclusion cyst after episiotomy
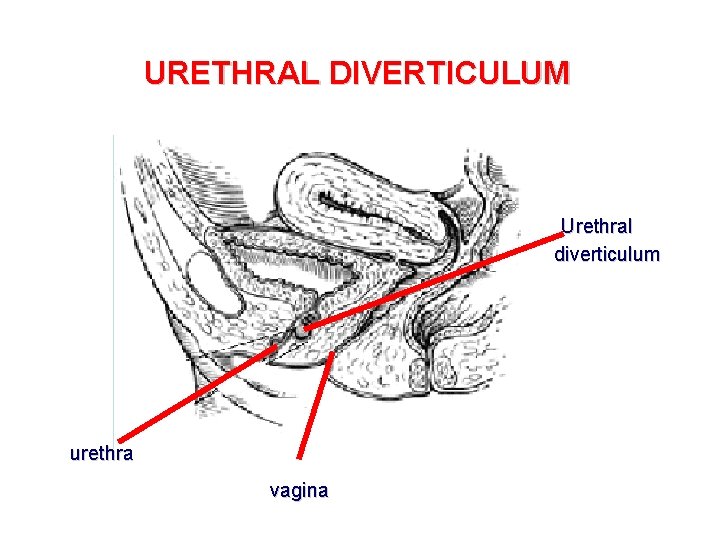
URETHRAL DIVERTICULUM Urethral diverticulum urethra vagina
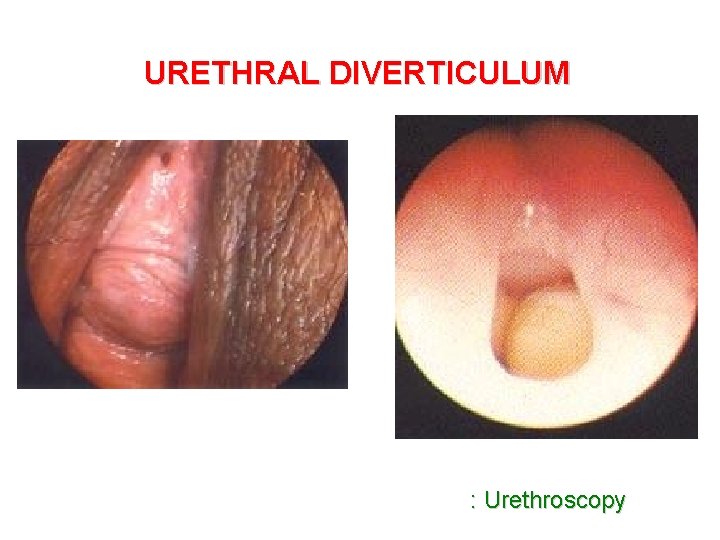
URETHRAL DIVERTICULUM : Urethroscopy

VAGINAL ADENOSIS
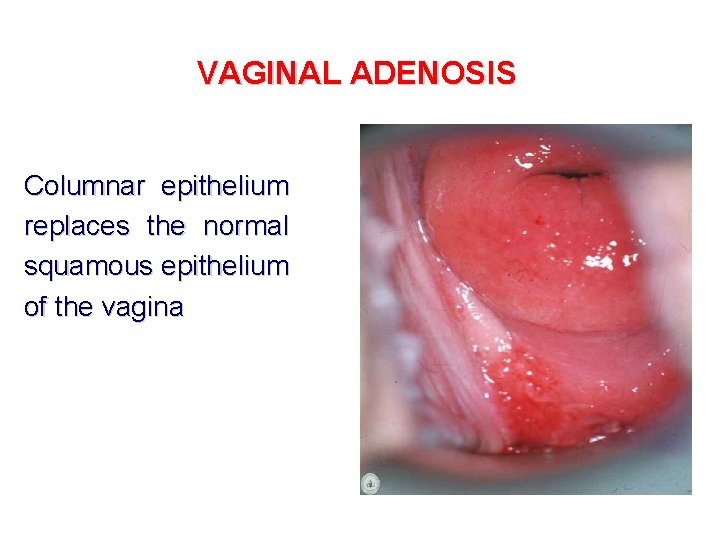
VAGINAL ADENOSIS Columnar epithelium replaces the normal squamous epithelium of the vagina

BENIGN DISEASES OF THE CERVIX

CERVICAL EROSION (ECTOPY)
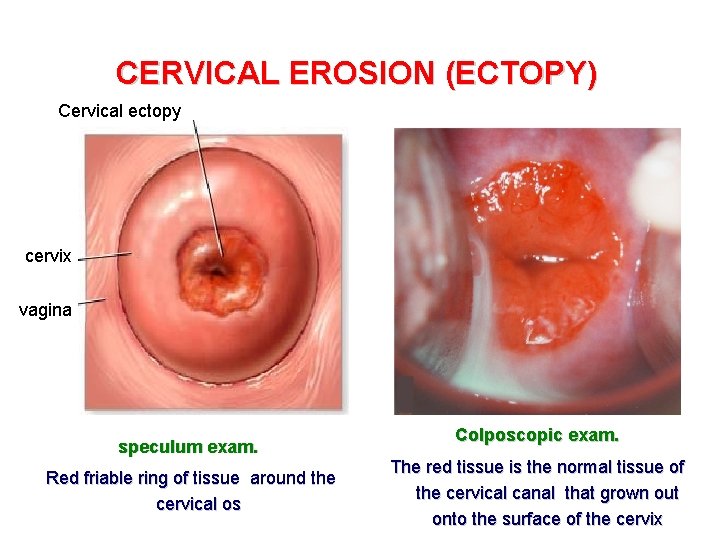
CERVICAL EROSION (ECTOPY) Cervical ectopy cervix vagina speculum exam. Red friable ring of tissue around the cervical os Colposcopic exam. The red tissue is the normal tissue of the cervical canal that grown out onto the surface of the cervix
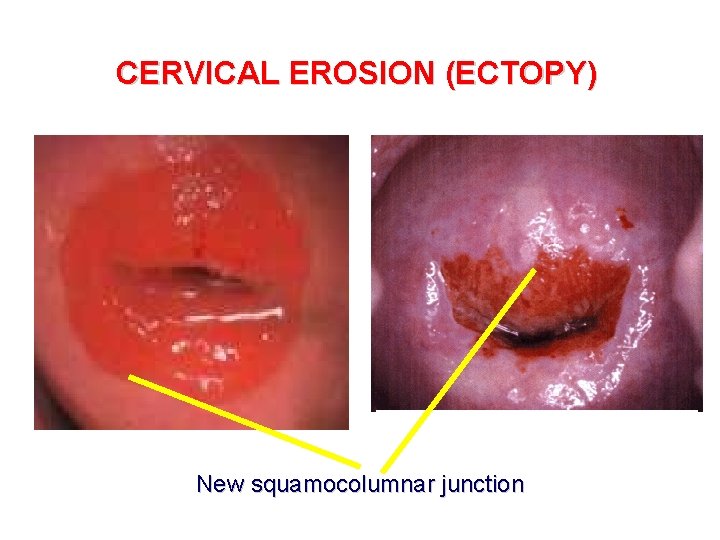
CERVICAL EROSION (ECTOPY) New squamocolumnar junction

CERVICAL POLYPS
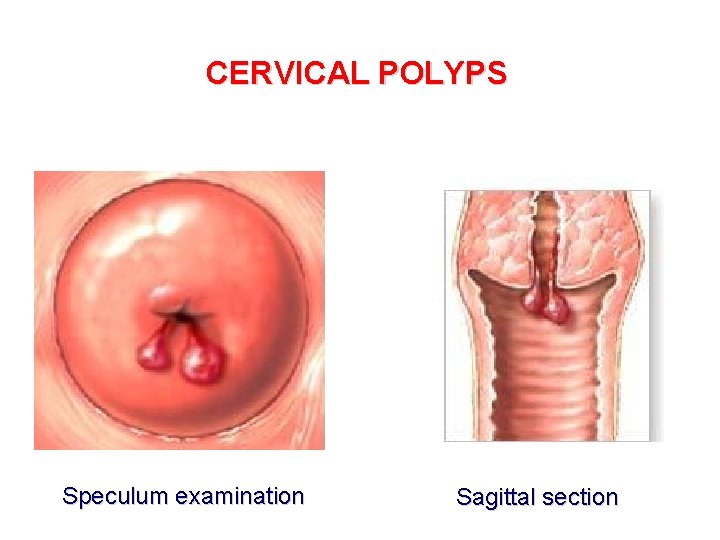
CERVICAL POLYPS Speculum examination Sagittal section

BENIGN DISEASES OF THE UTERUS

ENDOMETRIAL POLYPS
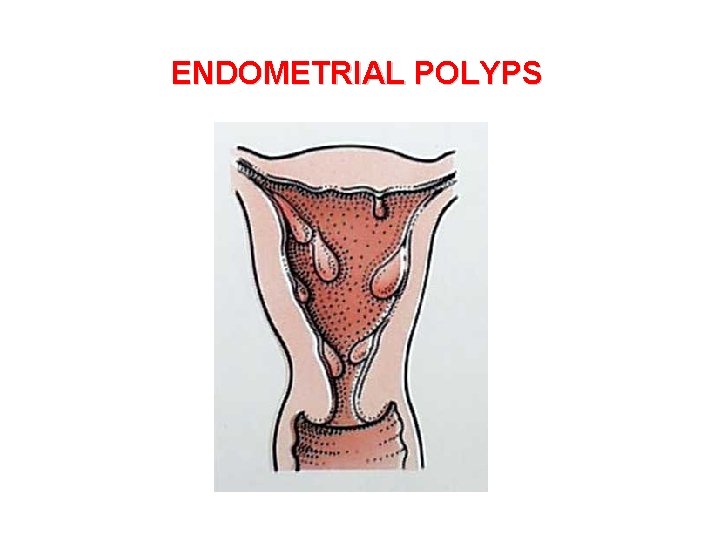
ENDOMETRIAL POLYPS
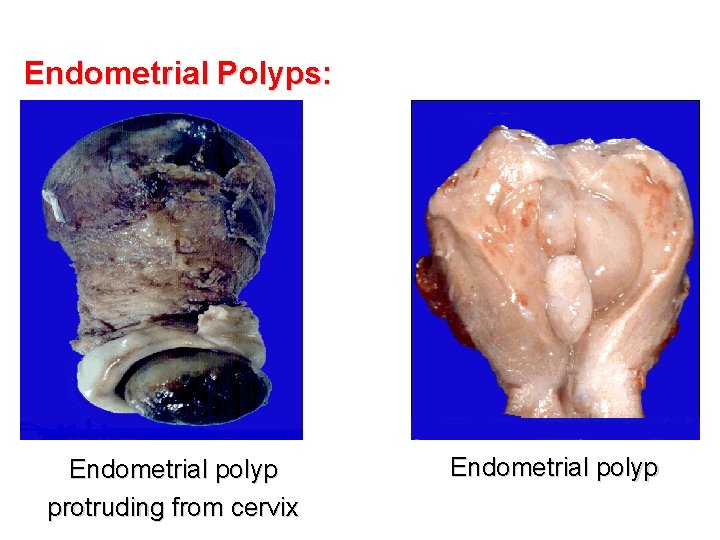
Endometrial Polyps: Endometrial polyp protruding from cervix Endometrial polyp
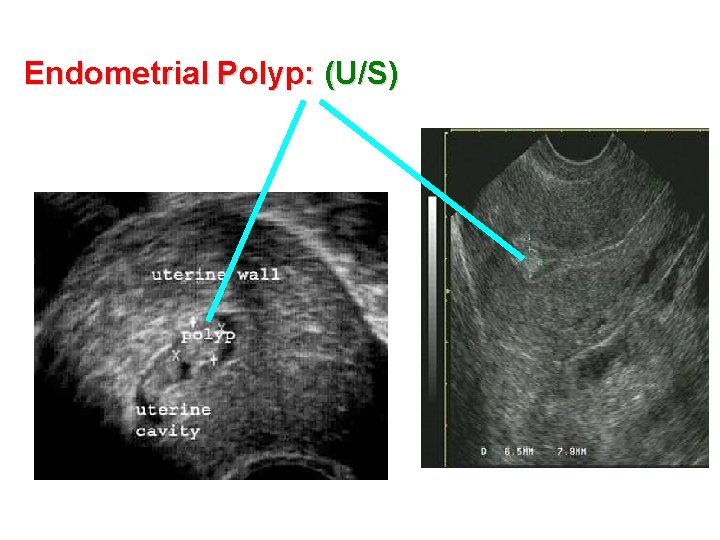
Endometrial Polyp: (U/S)
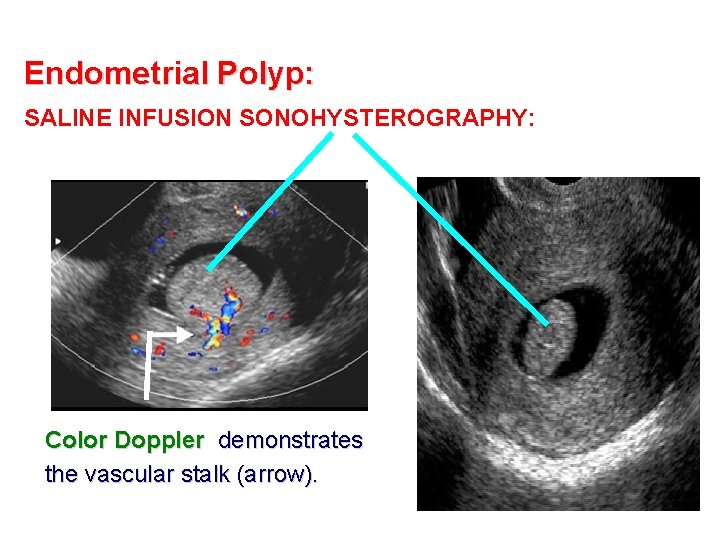
Endometrial Polyp: SALINE INFUSION SONOHYSTEROGRAPHY: Color Doppler demonstrates the vascular stalk (arrow).
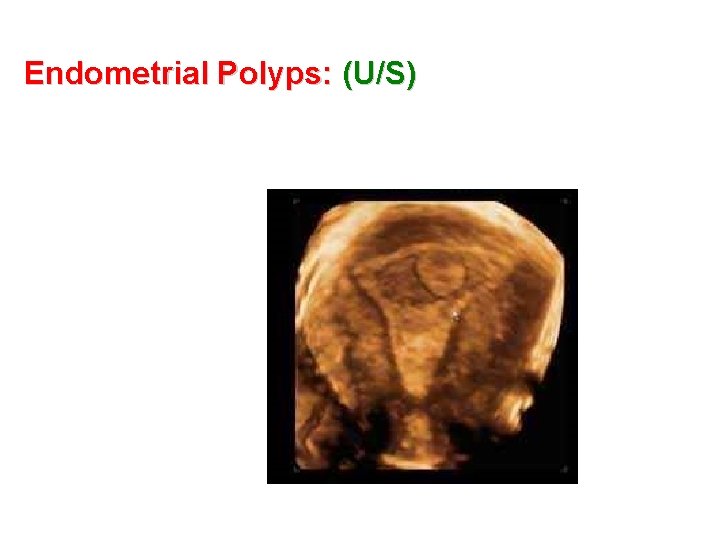
Endometrial Polyps: (U/S)
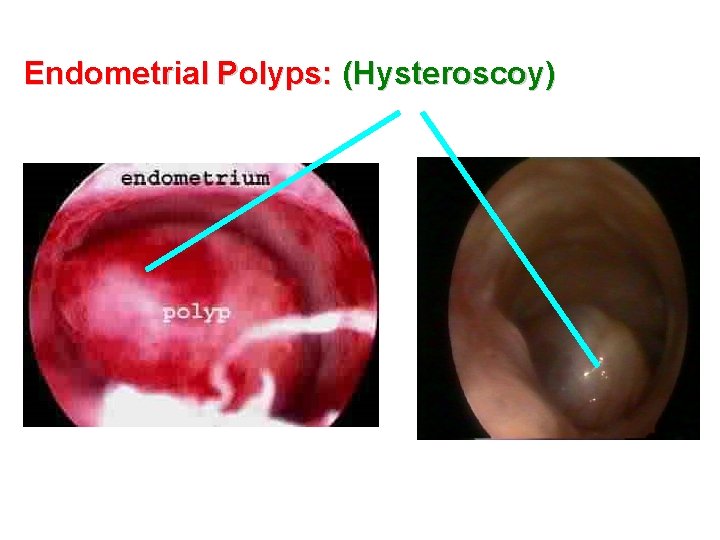
Endometrial Polyps: (Hysteroscoy)
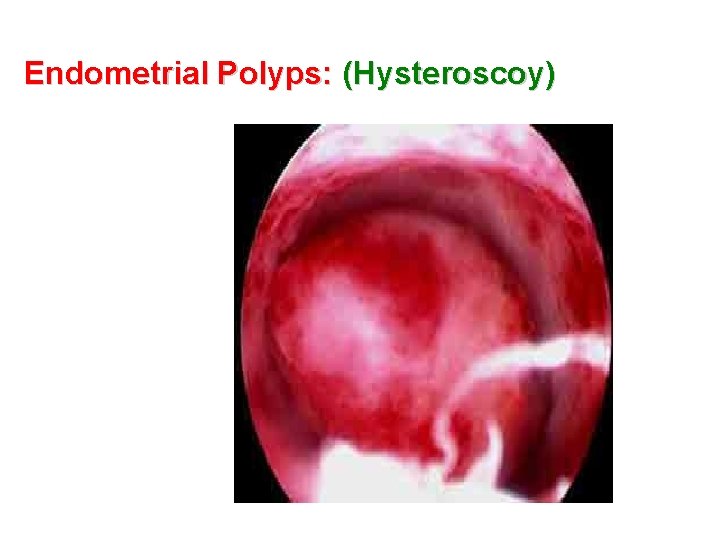
Endometrial Polyps: (Hysteroscoy)

ENDOMETRIAL HYPERPLASIA
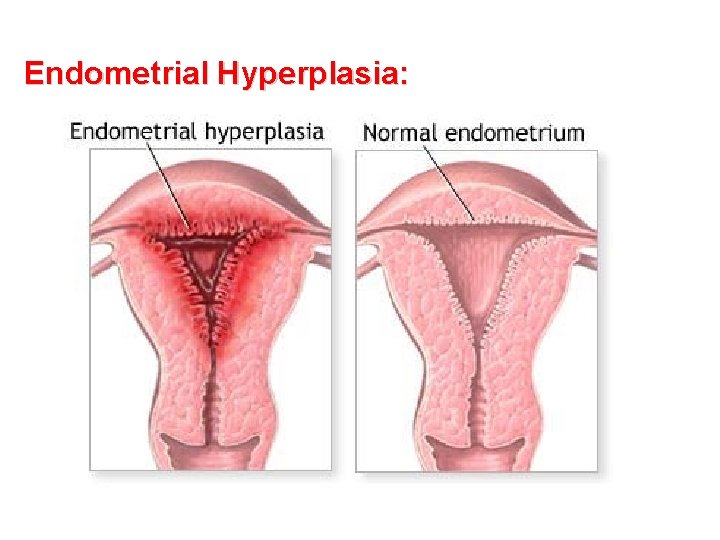
Endometrial Hyperplasia:
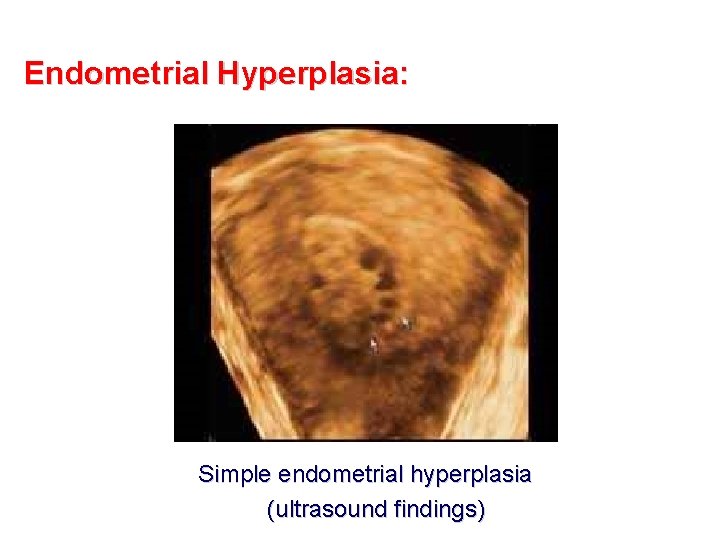
Endometrial Hyperplasia: Simple endometrial hyperplasia (ultrasound findings)
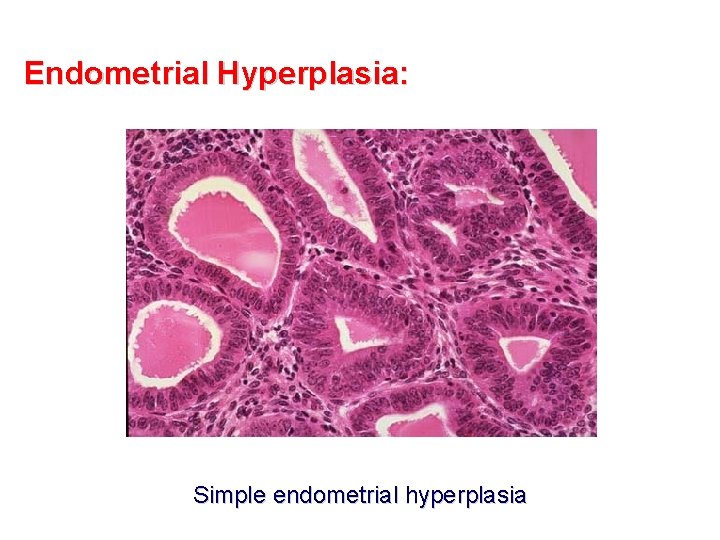
Endometrial Hyperplasia: Simple endometrial hyperplasia
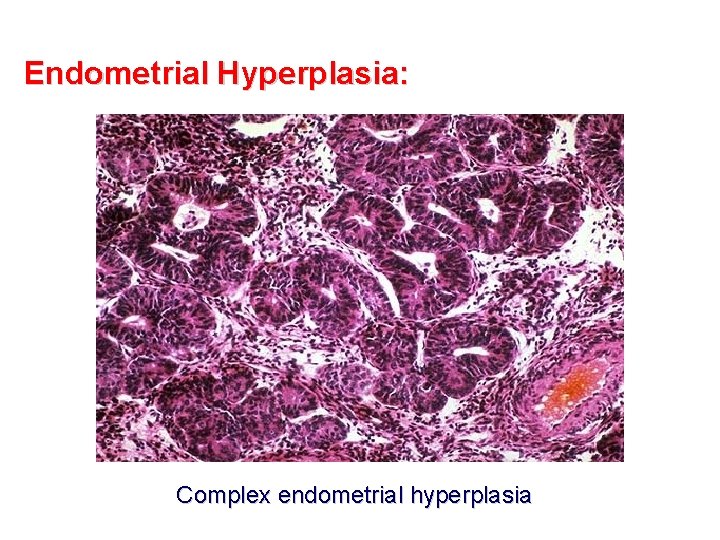
Endometrial Hyperplasia: Complex endometrial hyperplasia
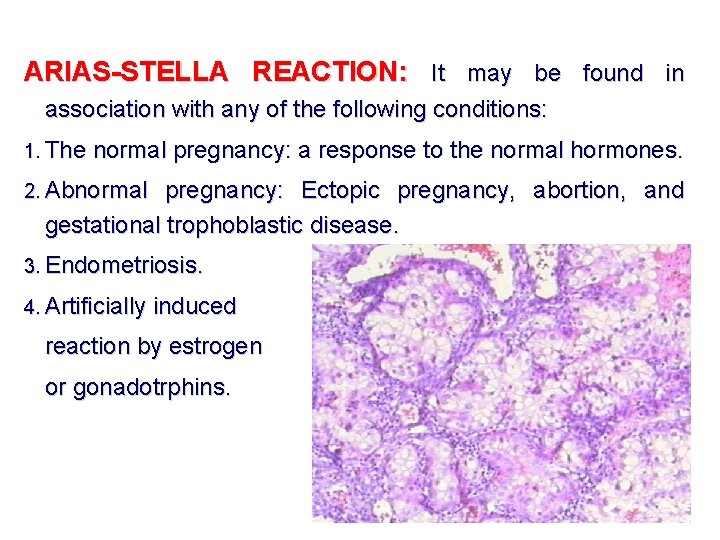
ARIAS-STELLA REACTION: It may be found in association with any of the following conditions: 1. The normal pregnancy: a response to the normal hormones. 2. Abnormal pregnancy: Ectopic pregnancy, abortion, and gestational trophoblastic disease. 3. Endometriosis. 4. Artificially induced reaction by estrogen or gonadotrphins.

INTRAUTERINE ADHESIONS (ASHERMAN’S SYNDROME)
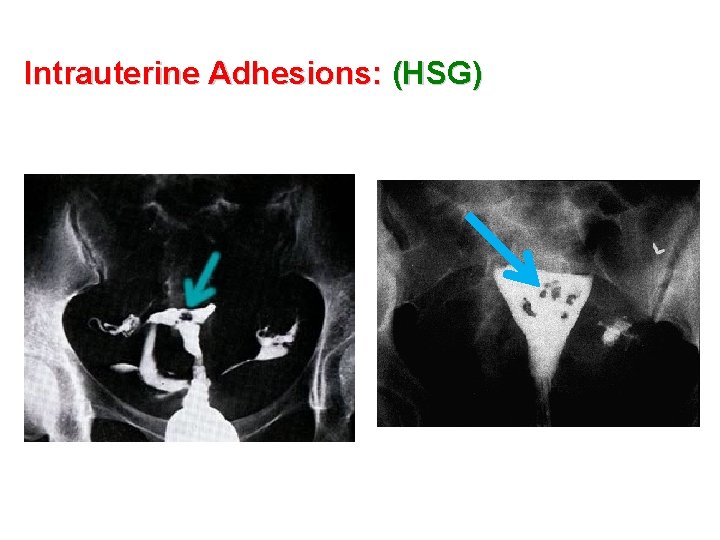
Intrauterine Adhesions: (HSG)
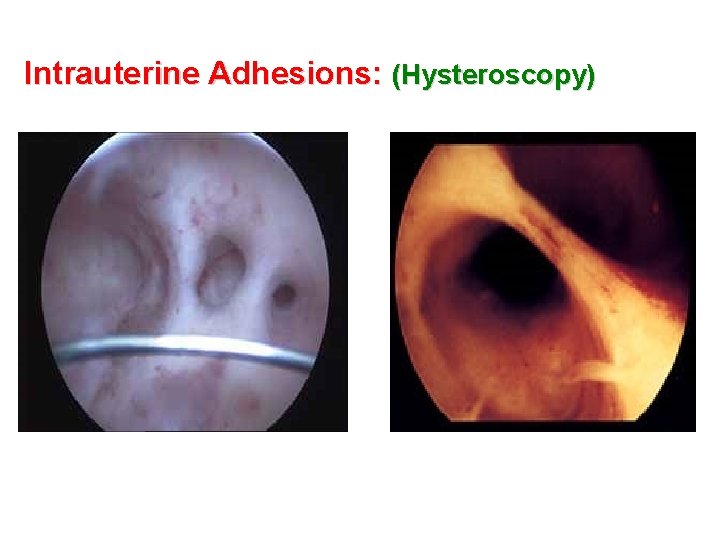
Intrauterine Adhesions: (Hysteroscopy)

UTERINE FIBROIDS
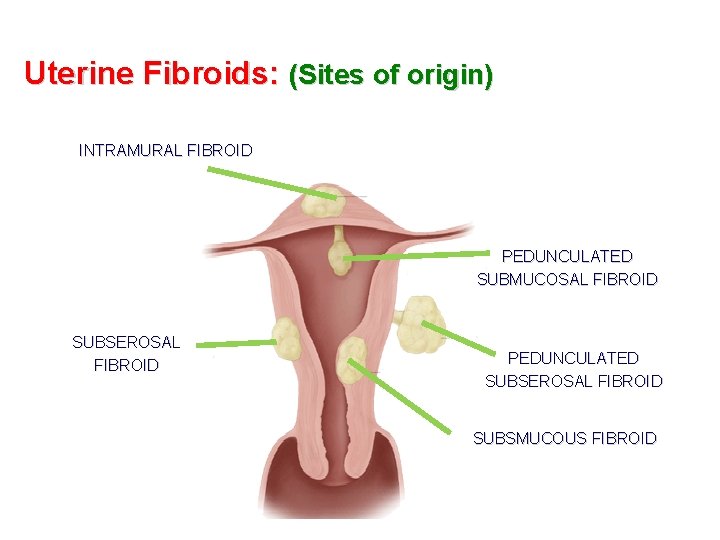
Uterine Fibroids: (Sites of origin) INTRAMURAL FIBROID PEDUNCULATED SUBMUCOSAL FIBROID SUBSEROSAL FIBROID PEDUNCULATED SUBSEROSAL FIBROID SUBSMUCOUS FIBROID
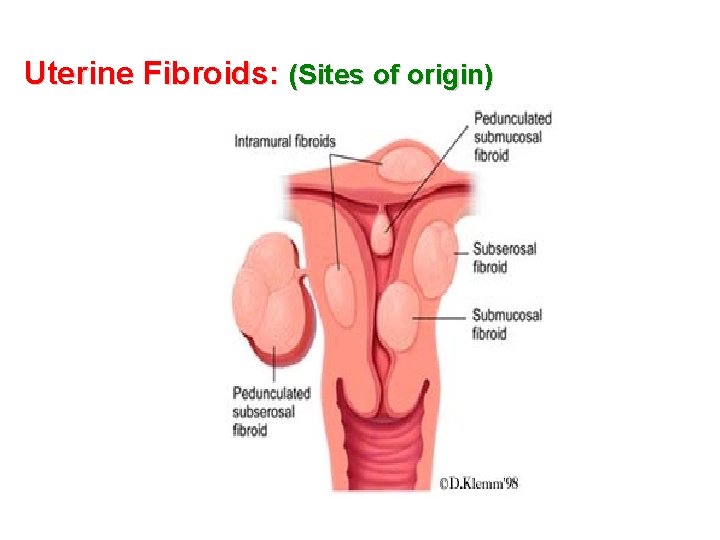
Uterine Fibroids: (Sites of origin)
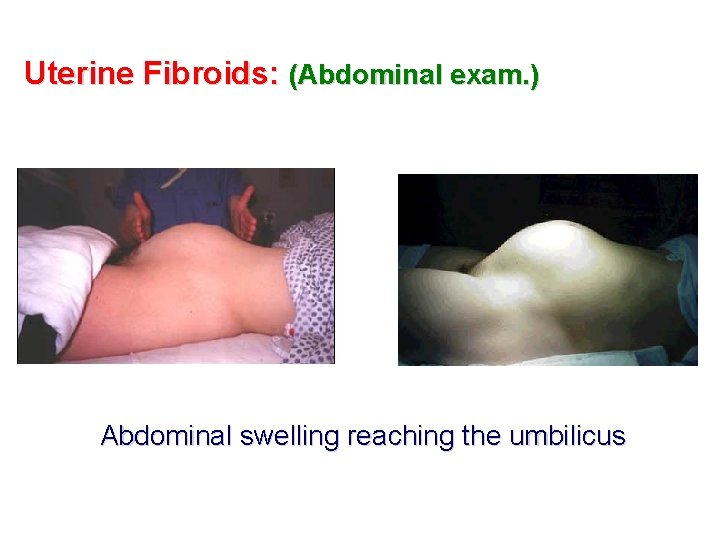
Uterine Fibroids: (Abdominal exam. ) Abdominal swelling reaching the umbilicus
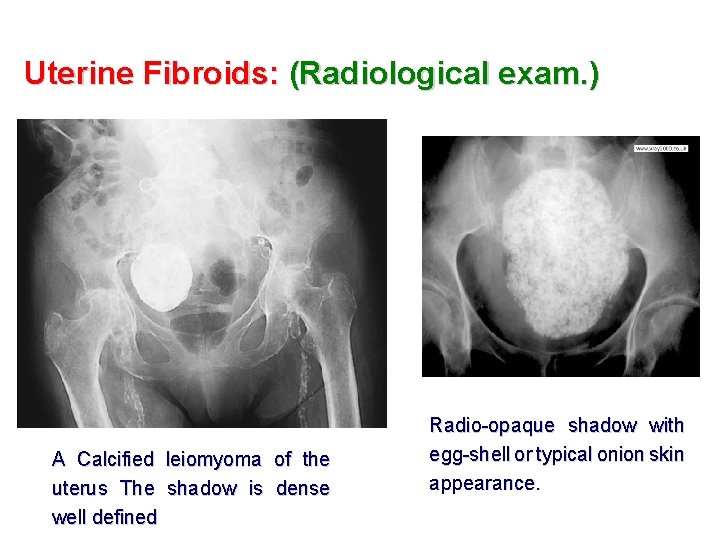
Uterine Fibroids: (Radiological exam. ) A Calcified leiomyoma of the uterus The shadow is dense well defined Radio-opaque shadow with egg-shell or typical onion skin appearance.
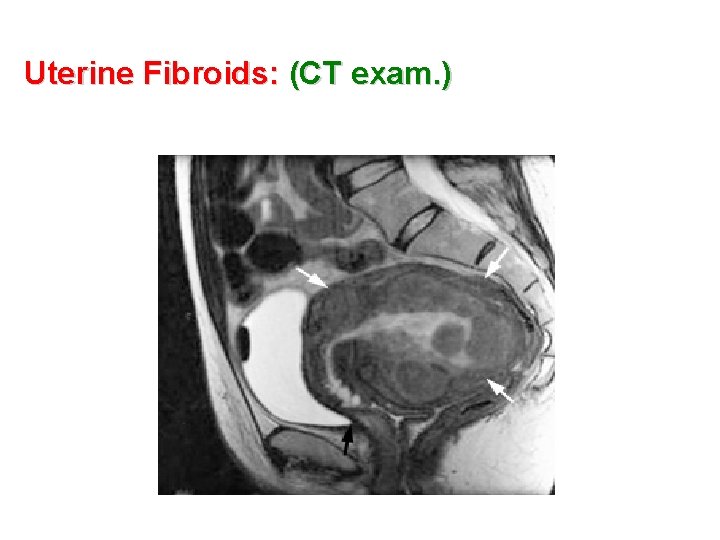
Uterine Fibroids: (CT exam. )
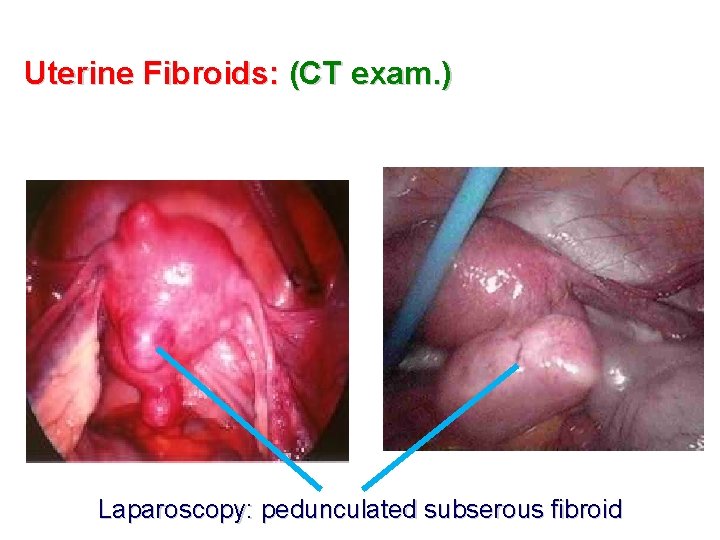
Uterine Fibroids: (CT exam. ) Laparoscopy: pedunculated subserous fibroid
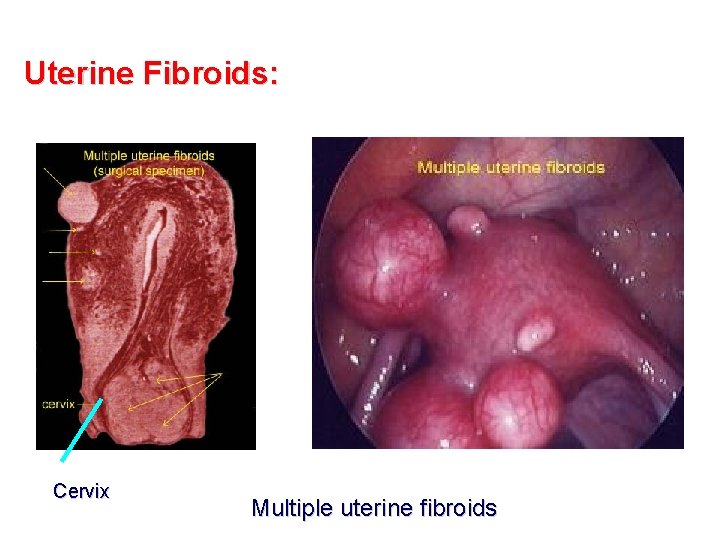
Uterine Fibroids: Cervix Multiple uterine fibroids
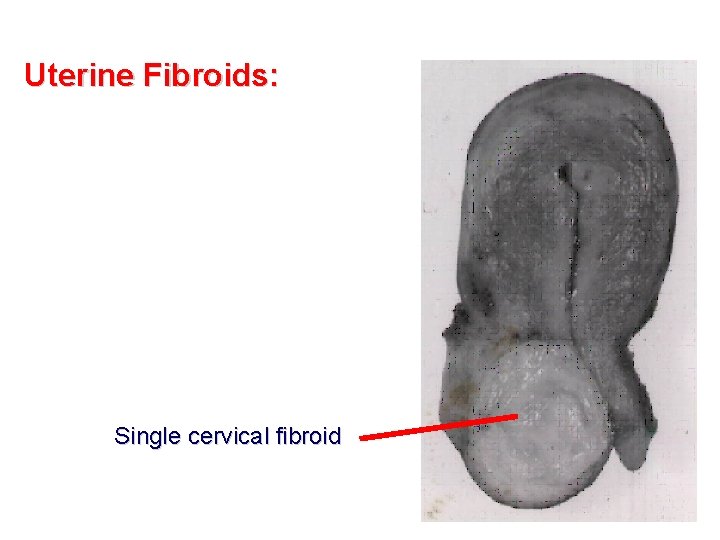
Uterine Fibroids: Single cervical fibroid
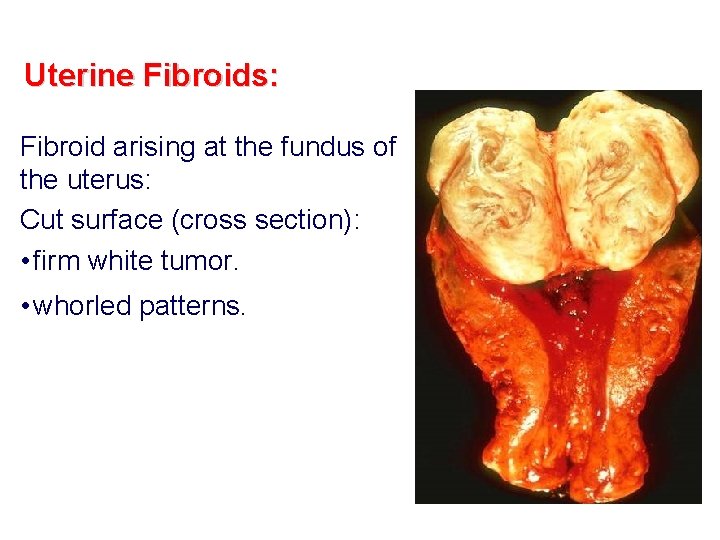
Uterine Fibroids: Fibroid arising at the fundus of the uterus: Cut surface (cross section): • firm white tumor. • whorled patterns.
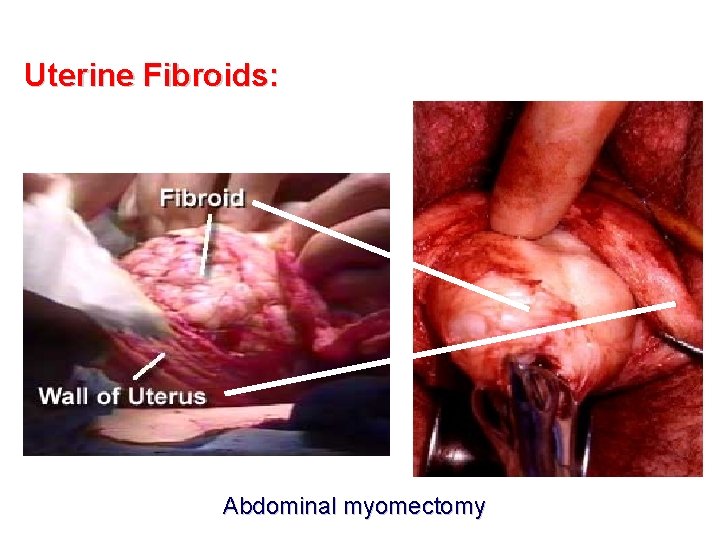
Uterine Fibroids: Abdominal myomectomy
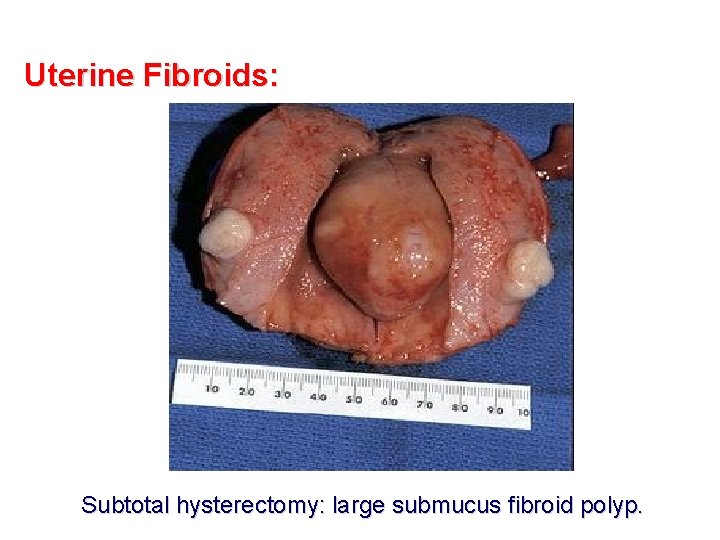
Uterine Fibroids: Subtotal hysterectomy: large submucus fibroid polyp.
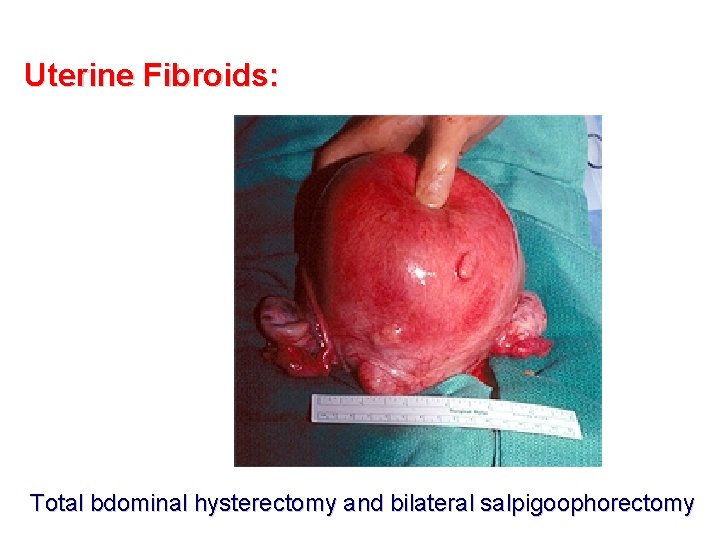
Uterine Fibroids: Total bdominal hysterectomy and bilateral salpigoophorectomy
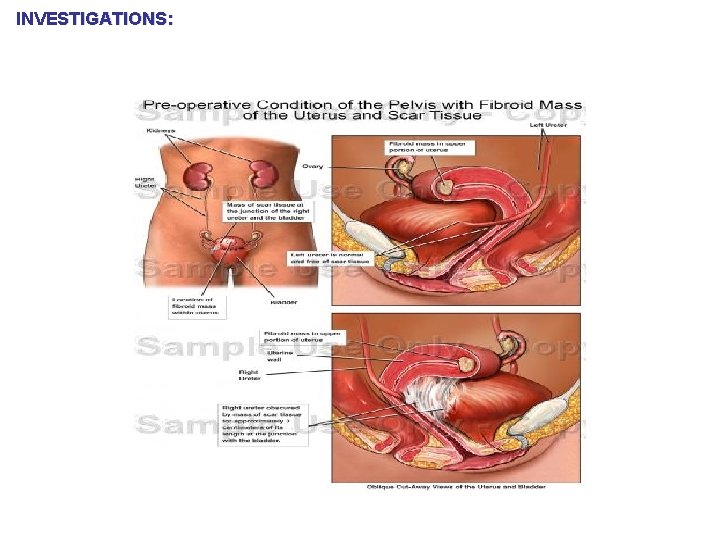
INVESTIGATIONS:

BENIGN DISEASES OF THE OVARY

NON-NEOPLASTIC OVARIAN ENLARGEMENTS
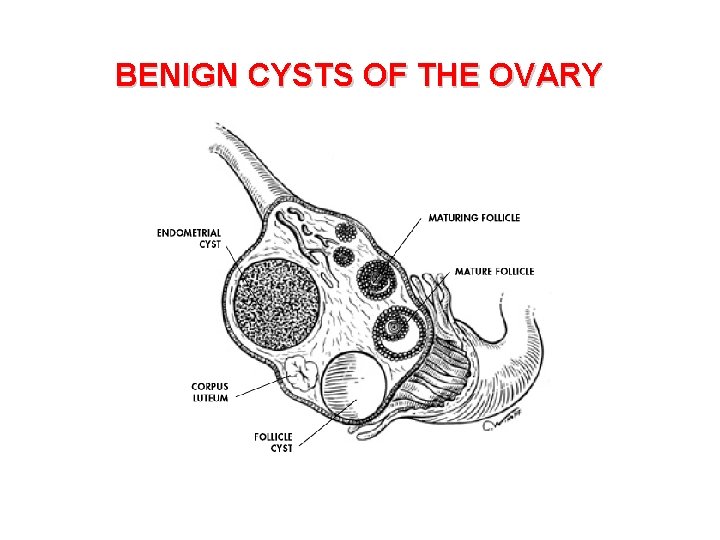
BENIGN CYSTS OF THE OVARY
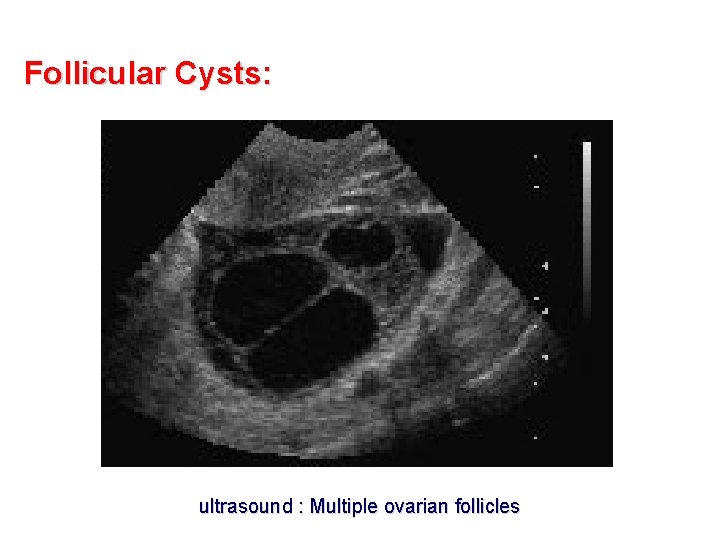
Follicular Cysts: ultrasound : Multiple ovarian follicles
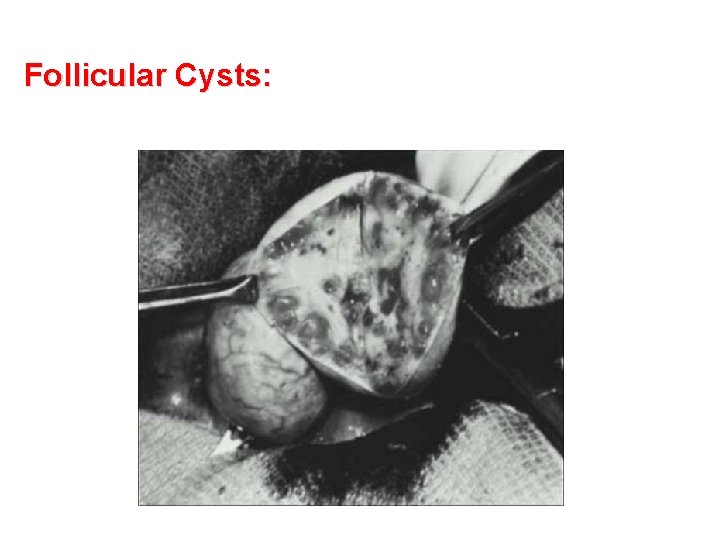
Follicular Cysts:
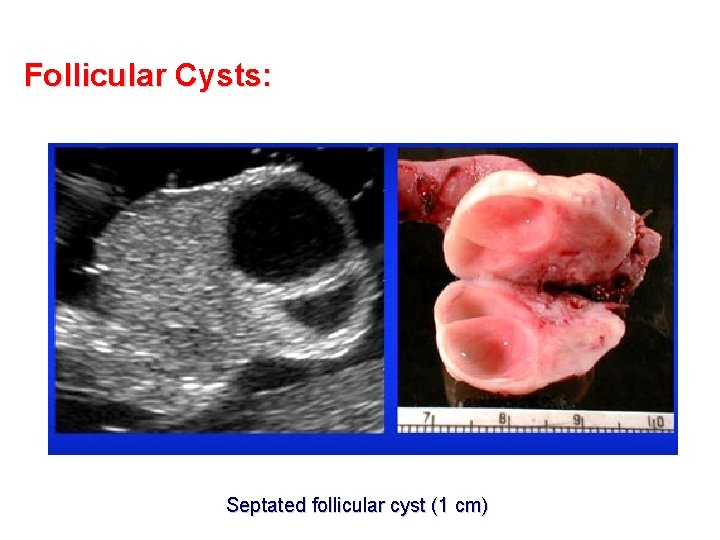
Follicular Cysts: Septated follicular cyst (1 cm)
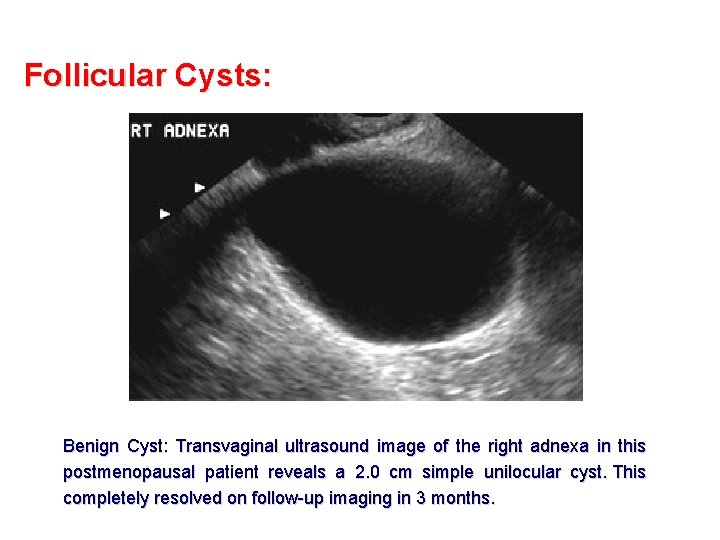
Follicular Cysts: Benign Cyst: Transvaginal ultrasound image of the right adnexa in this postmenopausal patient reveals a 2. 0 cm simple unilocular cyst. This completely resolved on follow-up imaging in 3 months.

Follicular Cysts:
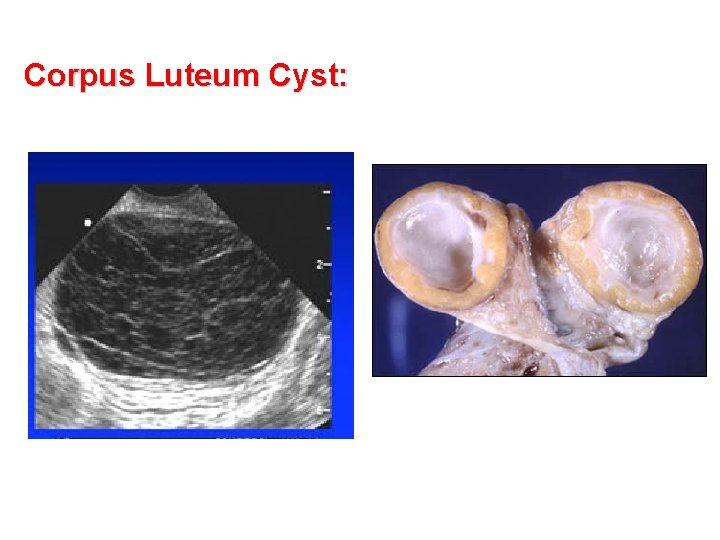
Corpus Luteum Cyst:
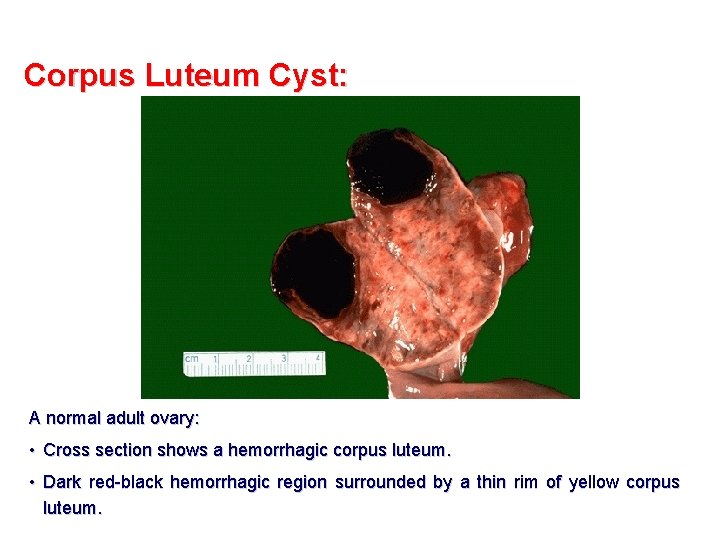
Corpus Luteum Cyst: A normal adult ovary: • Cross section shows a hemorrhagic corpus luteum. • Dark red-black hemorrhagic region surrounded by a thin rim of yellow corpus luteum.

BENIGN NEOPLASTIC OVARIAN ENLARGEMENTS

1 - EPITHELIAL OVARIAN TUMORS
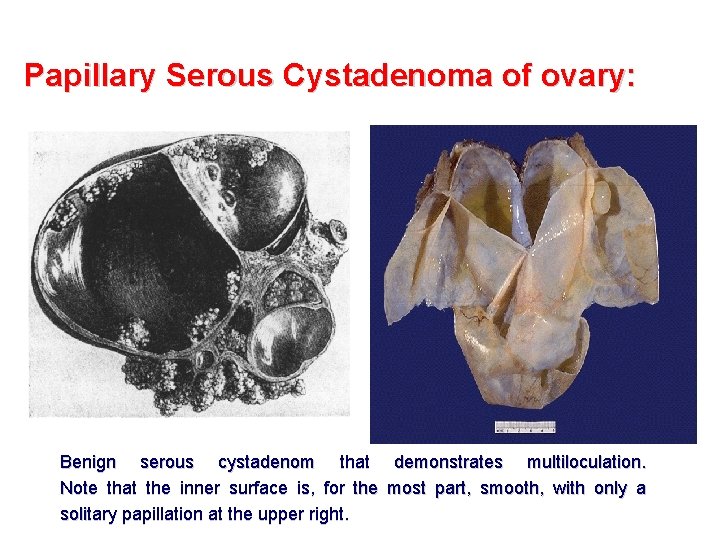
Papillary Serous Cystadenoma of ovary: Benign serous cystadenom that demonstrates multiloculation. Note that the inner surface is, for the most part, smooth, with only a solitary papillation at the upper right.
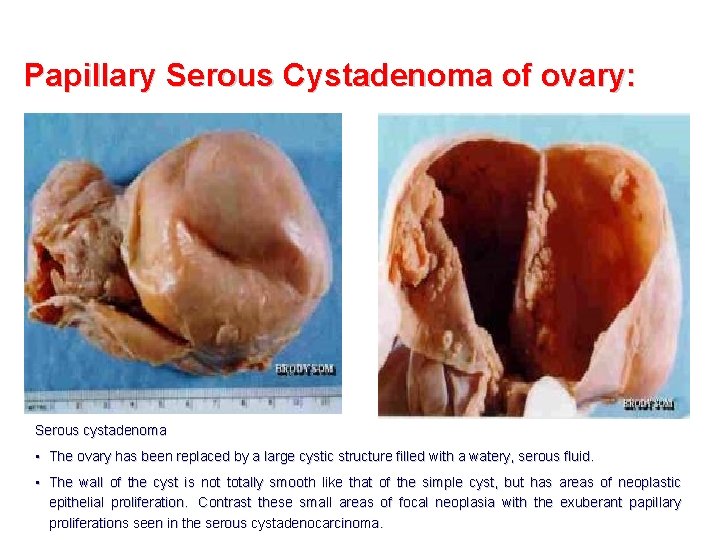
Papillary Serous Cystadenoma of ovary: Serous cystadenoma • The ovary has been replaced by a large cystic structure filled with a watery, serous fluid. • The wall of the cyst is not totally smooth like that of the simple cyst, but has areas of neoplastic epithelial proliferation. Contrast these small areas of focal neoplasia with the exuberant papillary proliferations seen in the serous cystadenocarcinoma.
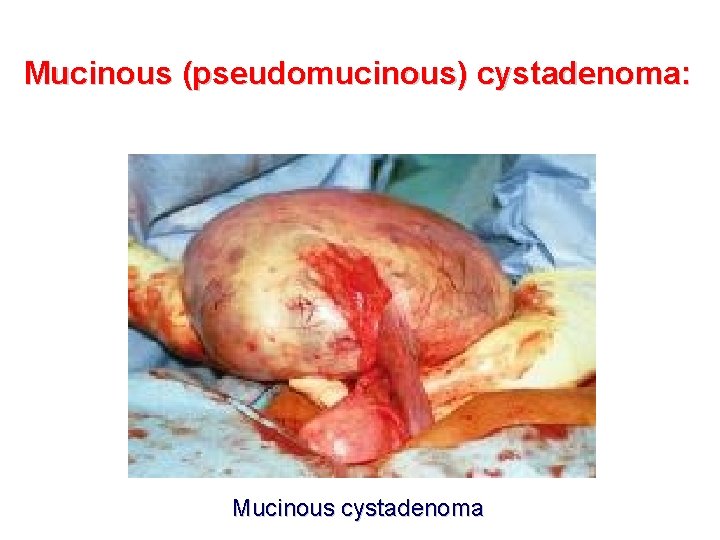
Mucinous (pseudomucinous) cystadenoma: Mucinous cystadenoma
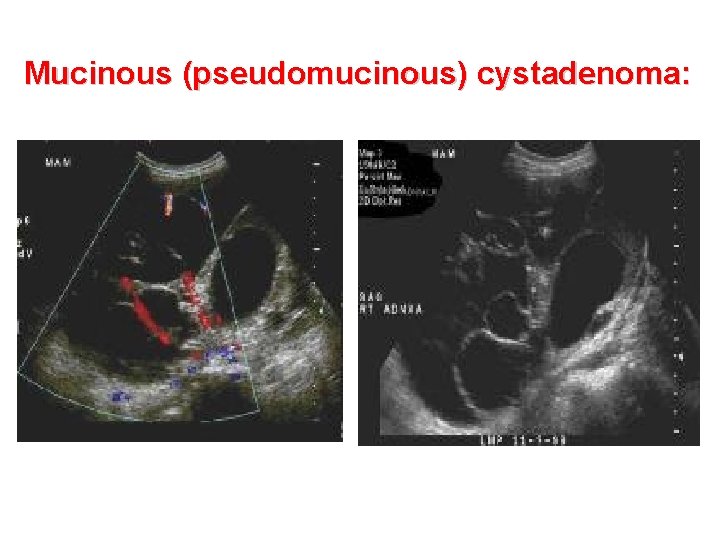
Mucinous (pseudomucinous) cystadenoma:

2 - GERM CELL OVARIAN TUMORS
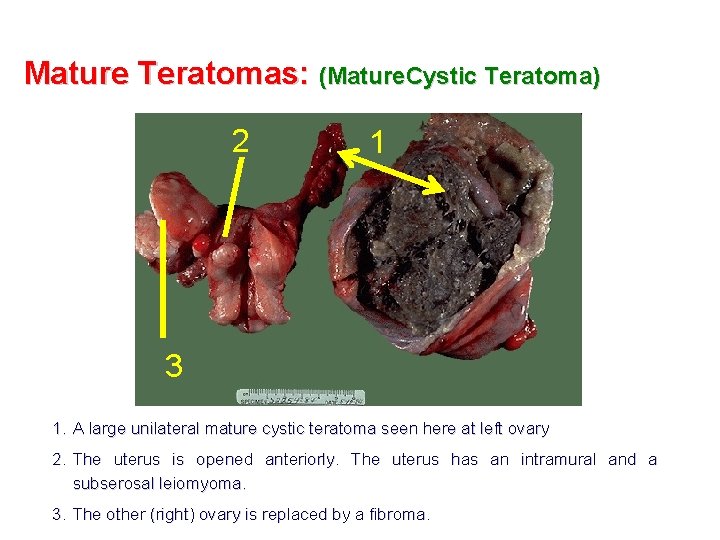
Mature Teratomas: (Mature. Cystic Teratoma) 2 1 3 1. A large unilateral mature cystic teratoma seen here at left ovary 2. The uterus is opened anteriorly. The uterus has an intramural and a subserosal leiomyoma. 3. The other (right) ovary is replaced by a fibroma.
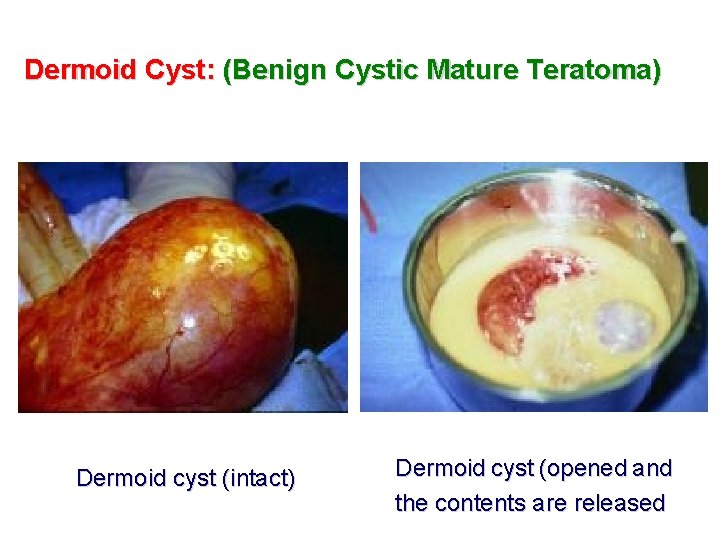
Dermoid Cyst: (Benign Cystic Mature Teratoma) Dermoid cyst (intact) Dermoid cyst (opened and the contents are released
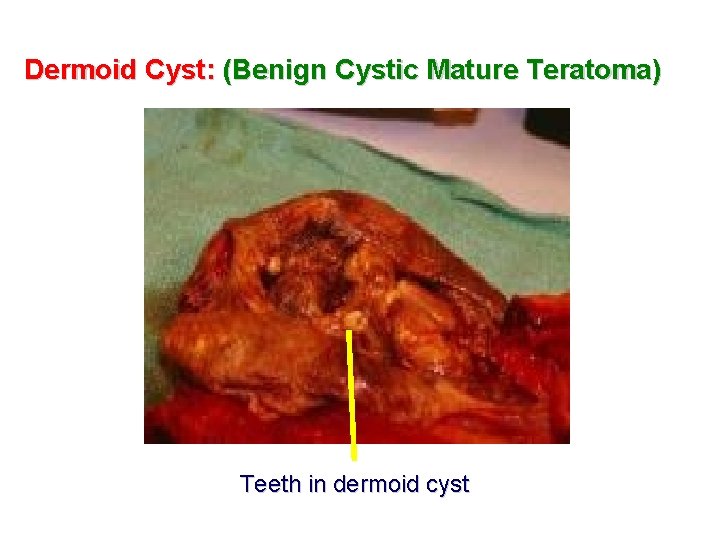
Dermoid Cyst: (Benign Cystic Mature Teratoma) Teeth in dermoid cyst
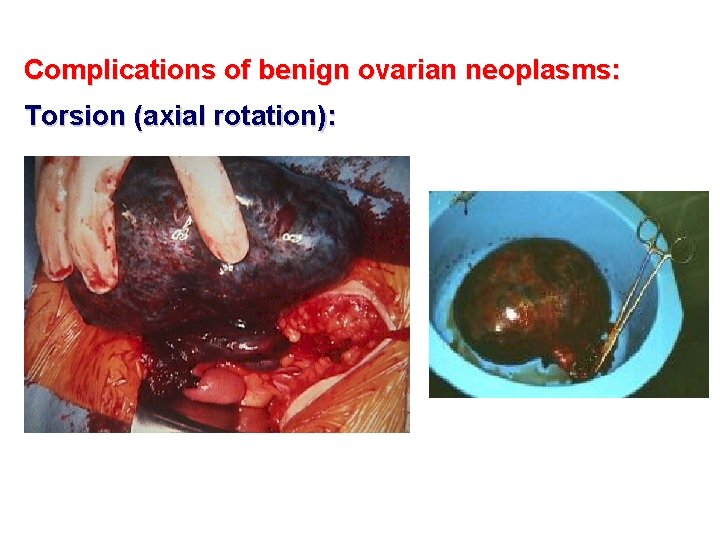
Complications of benign ovarian neoplasms: Torsion (axial rotation):

THE BREAST IN GYNECOLOGICAL PRACTICE

EVALUATION AND SCREENING METHODS

BREAST SELF EXANINATION (BSE) • Advise BSE every month to all women after age 20 years. • BSE is best during the first 10 days after menstruation when the hormonal influence is least. • The aim is detection of small masses.

Procedure of BSE: • utilize different positions to detect small masses deep in the fatty tissues. 1. Standing in front of a mirror 2. Lie in the supine position and breast is symmetrically flattened against the chest wall
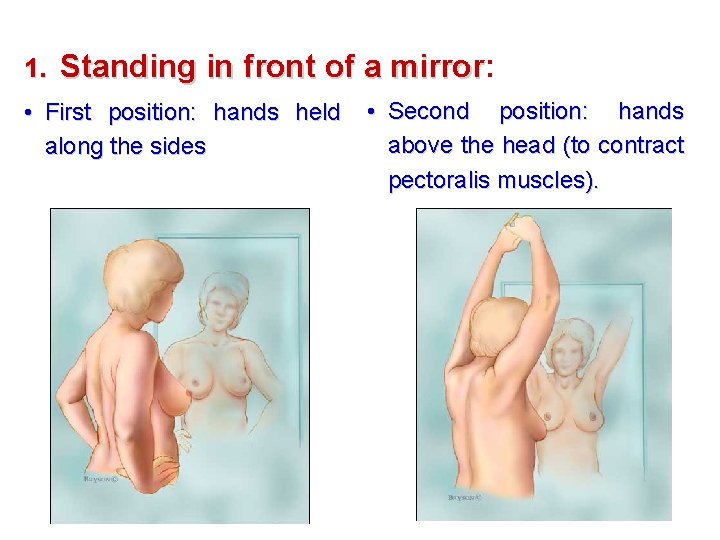
1. Standing in front of a mirror: mirror • First position: hands held along the sides • Second position: hands above the head (to contract pectoralis muscles).

1. Standing in front of a mirror: mirror a. Woman is looking for any abnormality especially the following: the breast contour, asymmetry, skin changes, nipple alterations, or discharge. b. Woman palpates supraclavicular and axillary locations looking for masses or nodes.
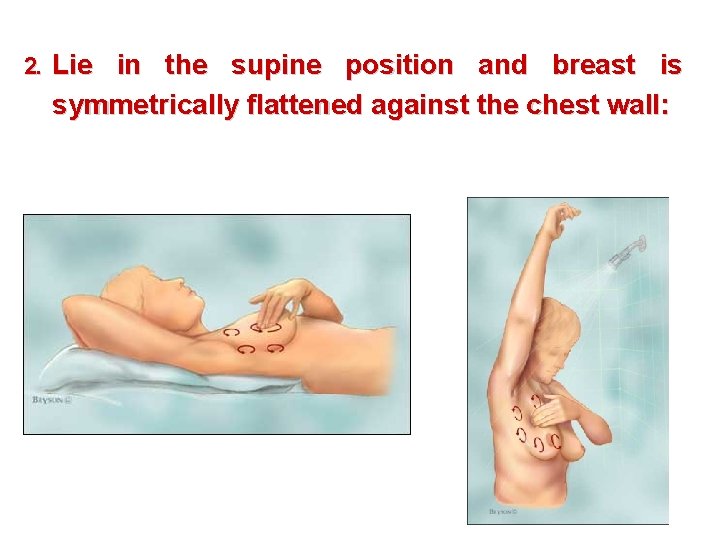
2. Lie in the supine position and breast is symmetrically flattened against the chest wall:

2. Lie in the supine position and breast is symmetrically flattened against the chest wall: a. The patient should then systematically palpate her breast. b. The breasts are pressed for evidence of discharge.
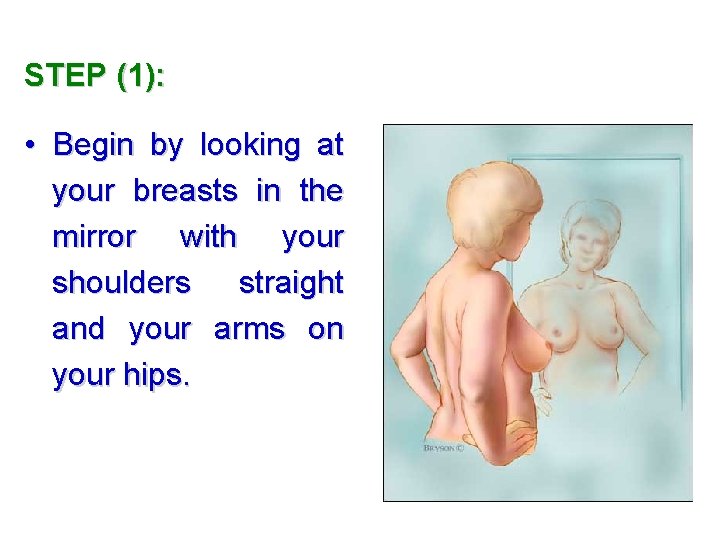
STEP (1): • Begin by looking at your breasts in the mirror with your shoulders straight and your arms on your hips.

STEP (1): • Look for: - Breasts: the size, shape, and color. - Breasts that are evenly shaped without visible distortion or swelling. q If you see any of the following changes, bring them to your doctor's attention: • Dimpling. • puckering. • bulging of the skin.

STEP (1): • Look for: - Nipple: • changed position. • become inverted (pushed inward instead of sticking out). - skin: Redness, soreness, rash, or swelling.

STEP (2): • Raise your arms and look for the same changes.
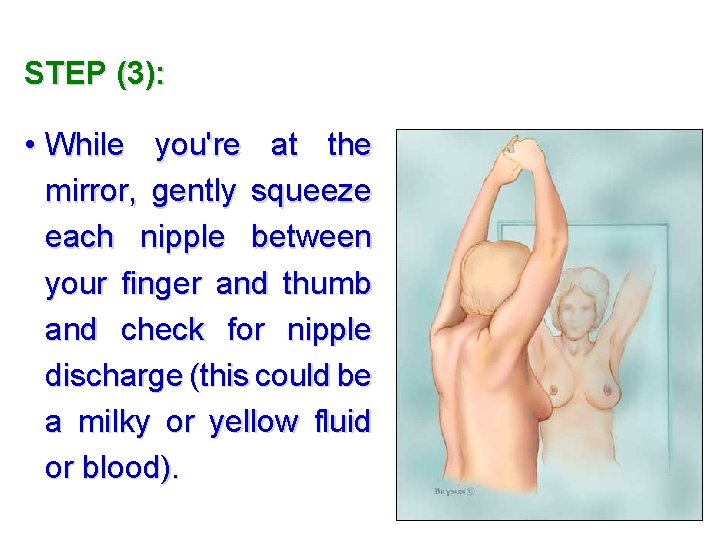
STEP (3): • While you're at the mirror, gently squeeze each nipple between your finger and thumb and check for nipple discharge (this could be a milky or yellow fluid or blood).
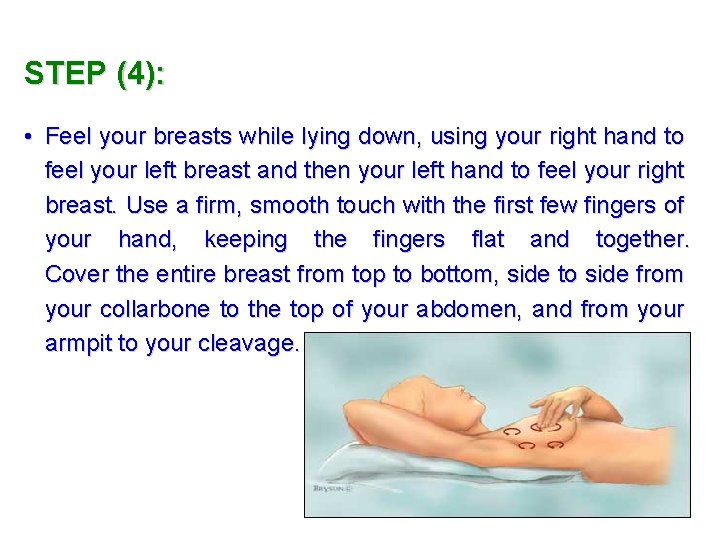
STEP (4): • Feel your breasts while lying down, using your right hand to feel your left breast and then your left hand to feel your right breast. Use a firm, smooth touch with the first few fingers of your hand, keeping the fingers flat and together. Cover the entire breast from top to bottom, side to side from your collarbone to the top of your abdomen, and from your armpit to your cleavage.
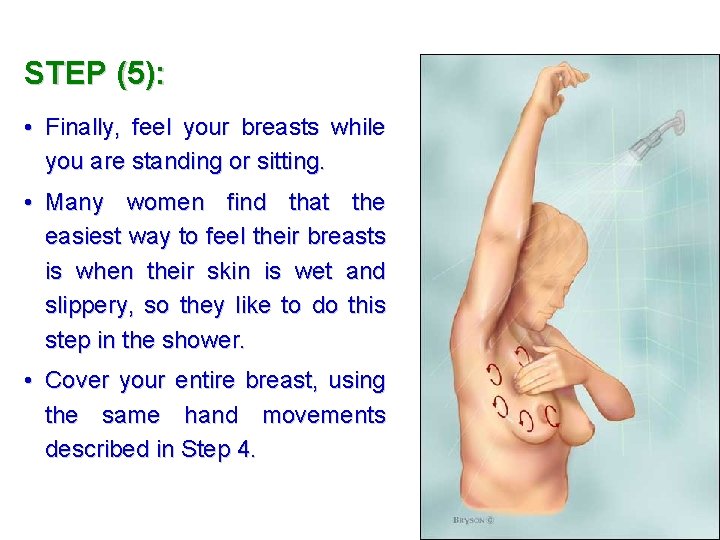
STEP (5): • Finally, feel your breasts while you are standing or sitting. • Many women find that the easiest way to feel their breasts is when their skin is wet and slippery, so they like to do this step in the shower. • Cover your entire breast, using the same hand movements described in Step 4.
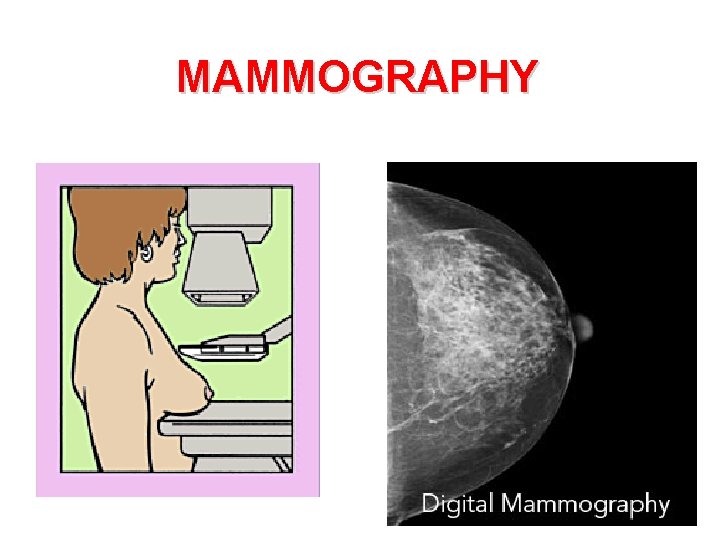
MAMMOGRAPHY

MALIGNANT BREAST DISEASES
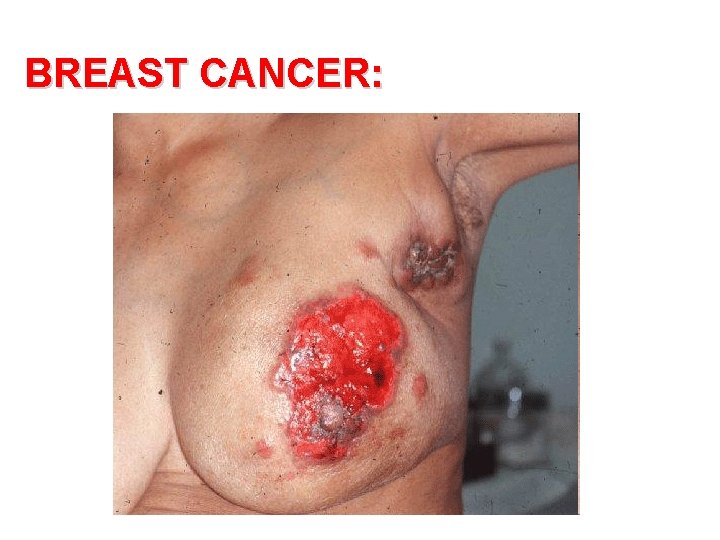
BREAST CANCER:
- Slides: 111