Chapter 30 Promoting Bowel Elimination Copyright 2018 2014

Chapter 30 Promoting Bowel Elimination Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Lesson 30. 1 Overview of Bowel Elimination Theory 1) Describe the process of normal bowel elimination. 2) Identify abnormal characteristics of stool. 3) Summarize the physiologic effects of hypoactive bowel, as well as nursing interventions to assist patients with constipation. 4) Analyze safety considerations related to giving a patient an enema. Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 2

Lesson 30. 1 Overview of Bowel Elimination Clinical Practice 1) Summarize nursing measures to promote regular bowel elimination in patients. 2) Collect a stool specimen. 3) Perform a focused assessment of bowel function. 4) Write a nursing care plan for a patient with bowel problems. 5) Prepare to administer an enema. Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 3

Structures Involved in Waste Elimination Small intestine Duodenum Ø Jejunum Ø Ileum Ø Carries chyme from the stomach to the large intestine Ileocecal valve Ø Controls flow of chyme into the large intestine Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 4

Structures Involved in Waste Elimination (cont’d) Large intestine Ascending colon Ø Transverse colon Ø Descending colon Ø Sigmoid colon Ø Rectum Ø Anus Ø Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 5

Figure 30 -1: The intestinal system Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 6

Structures Involved in Waste Elimination (cont’d) Walls of the intestine have four layers Mucosa Ø Submucosa Ø Muscular layer Ø Serous layer (serosa) Ø Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 7

Functions of the Intestines Small intestine Processes chyme into a more liquid state Adds bile from the liver to help break down fats Ø Villi on the small intestine walls absorb nutrients Ø Large intestine Absorbs water, sodium, chlorides Waste material stored until expelled Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 8

Functions of the Intestines (cont’d) Peristalsis moves chyme and gas through the intestines (causing bowel sounds) Normal transit time in intestine is 18 to 72 hours Feces is stored in the sigmoid colon until the gastrocolic reflex initiates defecation Defecation is under voluntary control and uses the Valsalva maneuver Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 9

Effects of Aging on the Intestinal Tract Atrophy of the villi Decreased absorption of fats, vitamin B 12 Decrease in motility Bowel habits should not change in the normal healthy individual Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 10

Normal Stool Color: light to dark brown Consistency: soft-formed in children and adults; consists of ¼ solids and ¾ water Appearance: affected by diet and metabolism Composition: solid materials consist of 70% undigested roughage from carbohydrates, fat, protein, and inorganic matter, and 30% dead bacteria Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 11

Abnormal Stool Blood in the stool: most serious abnormality Fresh red blood: bleeding in colon Ø Occult: upper GI bleed (black stool called melena) Ø Pale white or light gray stool: absence of bile in the intestine Large amounts of mucus, fat, pus, or parasites Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 12

Hypoactive Bowel and Constipation Indicates a decrease in peristalsis Usually results in constipation Causes Immobility Ø Injury to the bowel Ø Drugs Ø Surgery Ø A patient restricted to bed at risk for constipation Flatus (gas) accumulates in the intestinal tract when peristalsis reduced or absent Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 13

Drugs That May Contribute to Constipation Narcotic analgesics Ø Codeine, morphine, meperidine General anesthetics Diuretics Sedatives Anticholinergics Calcium channel blockers Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 14

Drugs Used for Constipation Stool softeners Ø Bulk-forming laxatives Ø Fibercon, Metamucil, Citrucel Irritant/stimulant laxatives Ø Colace, Surfak, Dialose Dulcolax, Neolid, Ex-Lax, Correctol, Senokot Saline laxatives Ø Citrate of magnesia, milk of magnesia, phosoda Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 15

Hyperactive Bowel and Diarrhea Increase in peristalsis Usually results in diarrhea May be self-limiting Causes Inflammation of GI tract, infectious diseases, diseases such as: Diverticulitis Ø Ulcerative colitis Ø Crohn’s disease Ø Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 16

Hyperactive Bowel (cont’d) Drugs Many antibiotics kill normal bowel bacteria, resulting in diarrhea Patients who experience diarrhea from antibiotics should replace normal flora by: Eating yogurt Ø Drinking buttermilk Ø Taking acidophilus (available OTC) Ø Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 17

Medications Used to Control Diarrhea Camphorated tincture of opium (paregoric) Diphenoxylate hydrochloride with atropine sulfate (Lomotil) Loperamide hydrochloride (Imodium) Difenoxin hydrochloride with atropine sulfate (Motofen) Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 18

Fecal Incontinence Lack of voluntary control of fecal evacuation; inability to retain feces Causes Illness Ø Cerebrovascular accident Ø Traumatic injury Ø Neurogenic dysfunction Ø Distressing condition that causes a loss of dignity Feelings of being less of a person Ø Loss of self-respect Ø Embarrassed Ø Anxiety or fear of losing control Ø Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 19

Initial Assessment Does patient have a bowel problem? Usual bowel pattern Any measures used to promote defecation? Use of enemas or laxatives Usual eating habits and exercise Foods that produce diarrhea or constipation Disorders that contribute to constipation or diarrhea Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 20

Initial Assessment (cont’d) Physical assessment Shape of the abdomen with the patient supine Ø Flat, distended Auscultate for bowel sounds in all four quadrants Percuss for presence of excessive air/gas in the abdomen Palpate for masses or tenderness Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 21

Nursing Diagnoses Constipation related to hypoactive bowel Diarrhea related to food intolerance Bowel incontinence related to loss of anal sphincter control Pain related to abdominal distention Self-care deficit, toileting related to traction Disturbed body image related to bowel incontinence Deficient knowledge related to factors that contribute to constipation Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 22

Question 1 The most serious abnormality in the stool is: 1) 2) 3) 4) mucus. pale white appearance. parasites. blood. Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 23

Question 2 Which patient is at the greatest risk for constipation? 1) 2) 3) 4) A 70 -year-old active male An 80 -year-old active female A 3 -year-old child An 18 -year-old female patient with a fractured pelvis Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 24

Question 3 Which two groups may become dehydrated very quickly if diarrhea persists? 1) 2) 3) 4) Infant, school-age children School-age children, adults Infant, elderly School-age and elderly Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 25

Lesson 30. 2 Ostomy, Stoma, and Peristoma Care Theory 4) Analyze safety considerations related to giving a patient an enema. (continued) 5) Analyze the psychosocial implications for a patient who has an ostomy. 6) Discuss the stoma and peristoma assessment and skin care. 7) Describe three types of intestinal diversions. Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 26

Lesson 30. 2 Ostomy, Stoma, and Peristoma Care Clinical Practice 6) Assist and teach a patient with a bowel retraining program for incontinence. 7) Evaluate the performance of a patient who is self-catheterizing a continent diversion. 8) Provide ostomy care, including irrigation and changing the ostomy appliance. Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 27

Rectal Suppositories Used to promote bowel movements Glycerin and bisacodyl suppositories Promote bowel evacuation Stimulate the inner surface of the rectum and increasing the urge to defecate Ø Form gas that expands the rectum Ø Melt into a lubricating material to coat the stool for easier passage through the anal sphincter Ø Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 28

Enemas Fluid introduced into rectum by means of a tube Stimulate peristalsis or wash out waste products Often given before a colonoscopy or an x-ray Volume of typical cleansing enema Infants: 20 to 150 m. L Ø Ages 3 to 5 years: 200 to 300 m. L Ø School-age: 300 to 500 m. L Ø Adults: 500 to 1000 m. L Ø Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 29
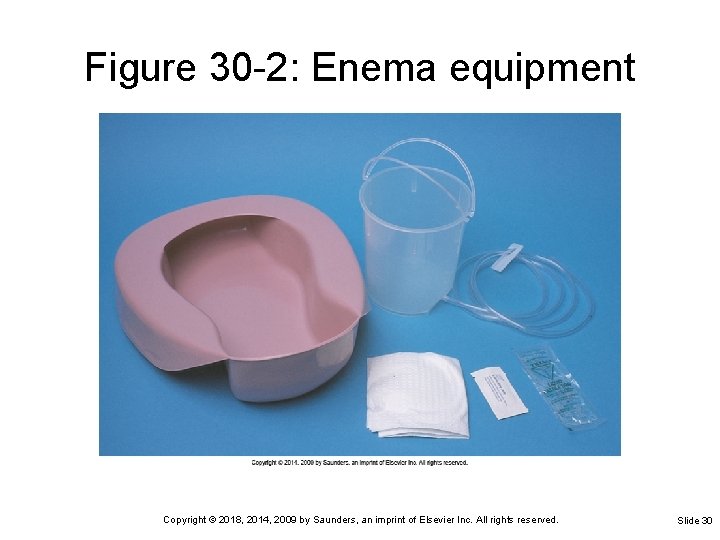
Figure 30 -2: Enema equipment Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 30
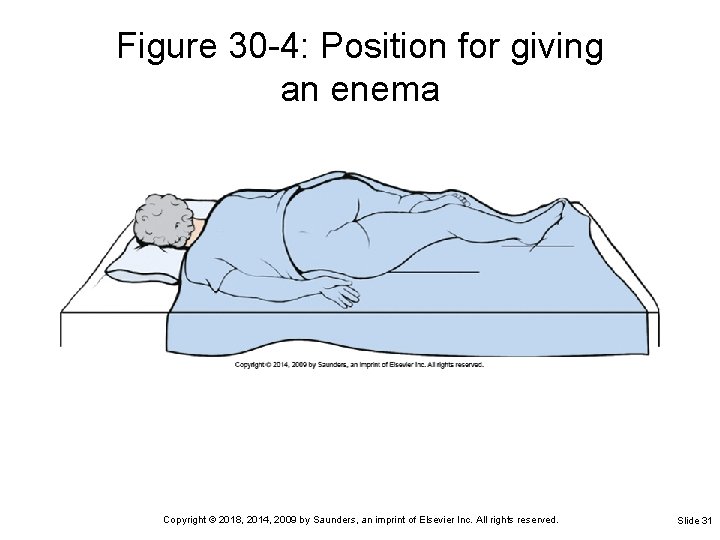
Figure 30 -4: Position for giving an enema Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 31

Types of Enemas Retention enema Ø Cleansing enema Ø Relieves discomfort from flatus causing distention Medicated enema Ø Stimulates peristalsis through distention and irritation of colon and rectum Distention reduction enema Ø Softens stool as oil is absorbed Solution with drugs to reduce bacteria or remove potassium Disposable enema (small volume) Ø Stimulates peristalsis by acting as irritant Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 32

Amount and Temperature of Solution Disposable enema units Contain about 240 m. L of solution Ø May be given at room temperature, but work best when slightly warmed Ø Cleansing enema Ø Adults is between 500 and 1000 m. L; smaller amounts are used for children Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 33

Fecal Impaction Means that the rectum and sigmoid colon become filled with hardened fecal material Most obvious sign is the absence of (or only a small amount of) bowel movement for more than 3 days in a patient who usually has a bowel movement more frequently Occurs in patients who are very ill, are on bed rest, or are confused Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 34

Bowel Training for Incontinence Principles for establishing regular bowel elimination Adequate diet Ø Sufficient fluids Ø Adequate exercise Ø Sufficient rest Ø Regular time for evacuation should be established All efforts must be made to provide patient with environment that is conducive to evacuation May require digital stimulation to relax the anal sphincter Suppositories, stool softeners, and bulk laxatives used to assist in establishing a normal, regular bowel pattern Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 35

Bowel Ostomy A diversion of intestinal contents from their normal path Results in formation of an external opening called a stoma May be an internal tissue pouch with a valve opening Special procedures aid in effective, controlled elimination through the stoma Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 36

Types of Ostomies Ileostomy Ø Diversion of the small bowel contents to a pouch or stoma; effluent is liquid Colostomy Diversion of the colon Ø Effluent may be liquid or solid depending on the site; may require irrigation Ø Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 37

Figure 30 -6: Sigmoid colostomy Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 38
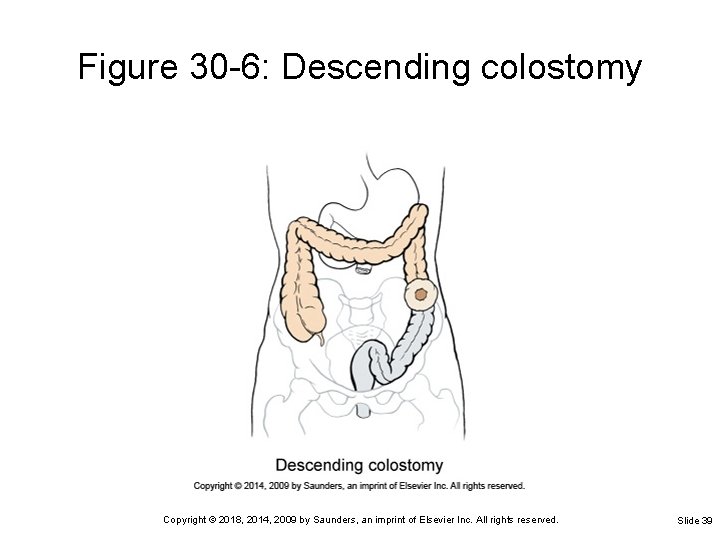
Figure 30 -6: Descending colostomy Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 39
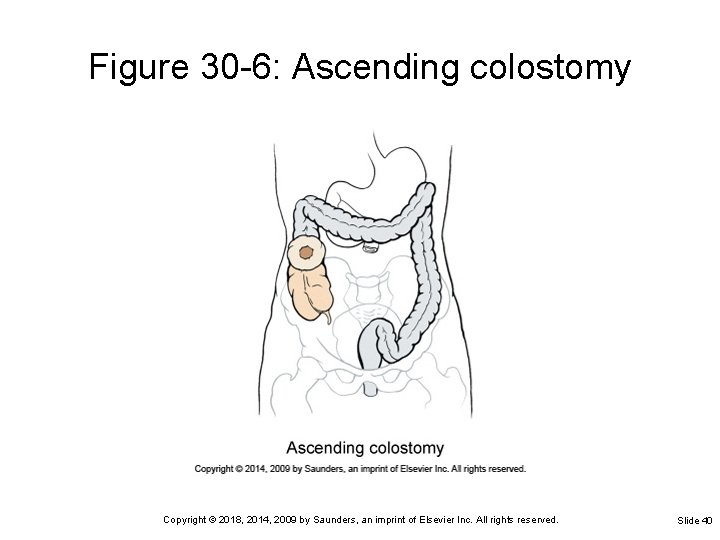
Figure 30 -6: Ascending colostomy Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 40
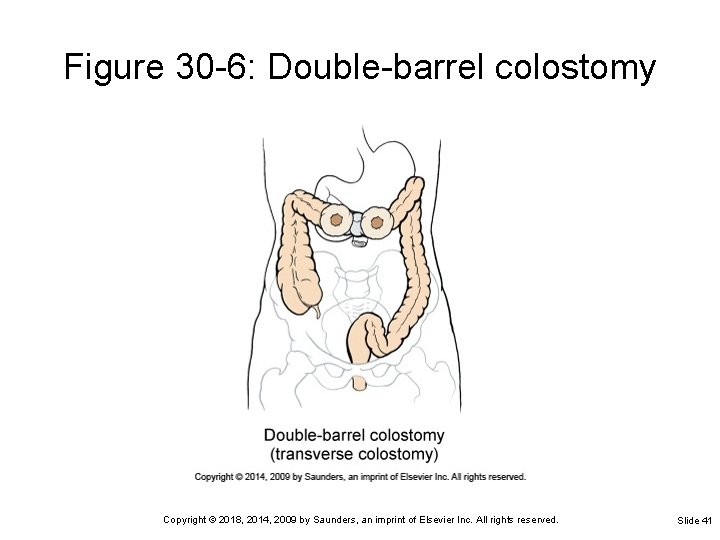
Figure 30 -6: Double-barrel colostomy Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 41
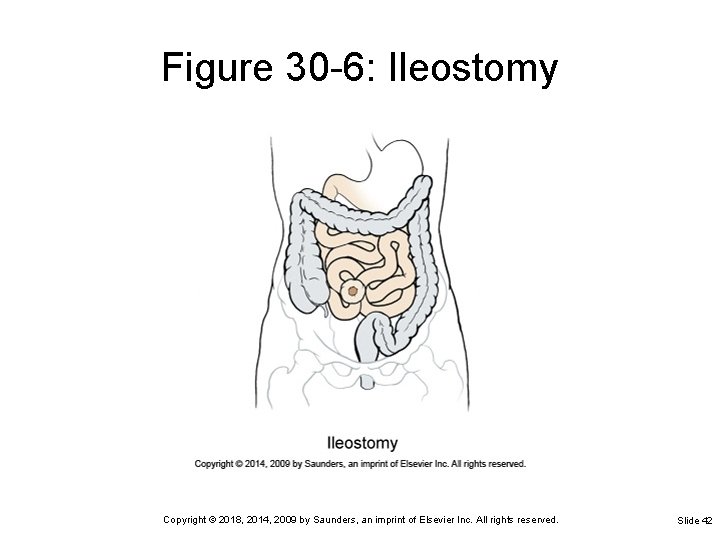
Figure 30 -6: Ileostomy Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 42
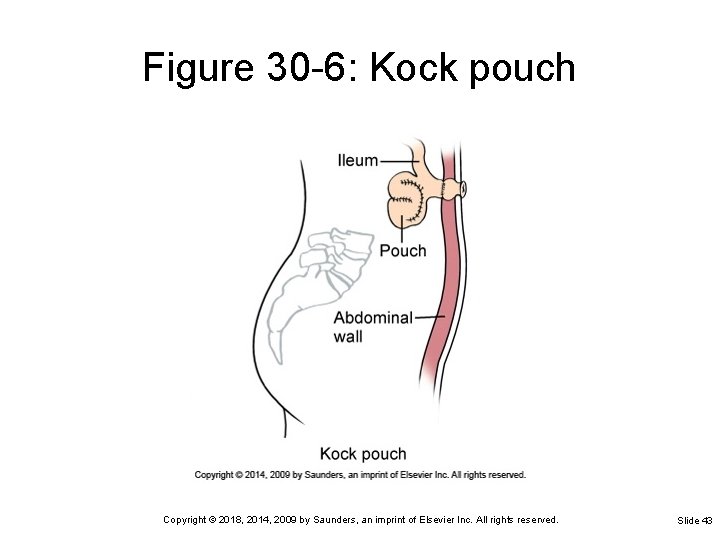
Figure 30 -6: Kock pouch Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 43

Ostomy Care Skin care Stoma and skin washed with mild soap and water and patted dry Ø Skin barrier paste is applied Ø Applying an ostomy appliance Ø Appliance is positioned with the stoma protruding through the opening in the center of the faceplate Irrigating a colostomy Ø A solution is instilled into the colon via the stoma Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 44

Question 4 Barbara’s patient is trying to understand the difference between an ileostomy and a colostomy. Barbara explains to her patient: 1) 2) 3) 4) an ileostomy is an opening into the colon and a colostomy is an opening into the ileum. an ileostomy has more effluent than a colostomy, which has more liquid fecal matter. an ileostomy has more liquid effluent and a colostomy has effluent that is more formed. diet will not adversely affect the ileostomy or colostomy patient. Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 45

Question 5 Stacy is working in a home health care situation and trying to establish bowel training with her patient. Her patient asks how long it usually takes to establish bowel training. Stacy’s correct response would be that a bowel training program can take: 1) 2) 3) 4) a couple of days or longer. a couple of weeks or longer. a couple of months or longer. years or may not even be successful. Copyright © 2018, 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Slide 46
- Slides: 46