Chapter 3 Carbohydrates 2009 CengageWadsworth Carbohydrates play a

Chapter 3 Carbohydrates � 2009 Cengage-Wadsworth

• Carbohydrates play a major role in human diets, comprising some 40 -75% of energy intake. • Their most important nutritional property is digestibility in the small intestine. • In terms of their physiological or nutritional role, they are often classified as available and unavailable carbohydrates.

• Available carbohydrates are those that are hydrolyzed by enzymes of the human gastrointestinal system to monosaccharides that are absorbed in the small intestine and enter the pathways of carbohydrate metabolism. • Unavailable carbohydrates are not hydrolyzed by endogenous human enzymes, although they may be fermented in the large intestine to varying extents.

• Carbohydrates are further classified according to their degree of polymerization (DP) as: • sugars (mono- and disaccharides), • oligosaccharides (contain three to nine monosaccharide units), and • polysaccharides (contain ten or more monosaccharide units)

Structural Features • Simple carbohydrates – Monosaccharides – Disaccharides • Complex carbohydrates – Oligosaccharides – Polysaccharides � 2009 Cengage-Wadsworth

Some biologically important monosaccharide 1. Ribose a pentose present in RNA 2. Deoxyribose a pentose present in DNA. 3. Glucose or grape sugar is the main sugar of the blood. 4. Fructose is the sugar of the fruits. 5. Galactose present in milk sugar lactose. 6. Mannose enter in the composition of mucopolysaccharide.

Simple Carbohydrates • Disaccharides – Maltose – Lactose – Sucrose � 2009 Cengage-Wadsworth

Disaccharides • Condensation of 2 monosaccharides forms a disaccharide. • The bond between them is called glycosidic bond. • A disaccharide is reducing when it has free anomeric carbon Disaccharide structure bond Reducing Examples ofsource disaccharides: property Sucrose cane sugar beat sugar table sugar α-D-glucose + β-D-Fructose α-1, 2 glycosidic bond. not reducing sugar Lactose milk sugar β-D-galactose + α-Dglucose β-1, 4 glycosidic bond Reducing sugar Maltose Malt sugar 2 molecules of α-D-glucose α-1, 4 glycosidic bond. Reducing sugar

B. The disaccharidases include: 1. Lactase (β-galactosidase) which hydrolyses lactose into two molecules of glucose and galactose: Lactase Lactose Glucose + Galactose 2. Maltase ( α-glucosidase), which hydrolyses maltose into two molecules of glucose: Maltase Maltose Glucose + Glucose 3. Sucrose (α-fructofuranosidase), which hydrolyses sucrose into two molecules of glucose and fructose: Sucrose Glucose + Fructose 4. α - dextrinase (oligo-1, 6 glucosidase) which hydrolyze (1 , 6) linkage of isomaltose. Dextrinase Isomaltose Glucose + Glucose

Complex Carbohydrates • Oligosaccharides – Raffinose – Stachyoses – Verbascose • Polysaccharides – Starch – Glycogen – Cellulose � 2009 Cengage-Wadsworth

Digestion • Polysaccharides – Salivary -amylase - mouth – Pacreatic -amylase - small intestine – Resistant starches • Digestion of disaccharides – Disaccharidases - active in microvilli of enterocytes � 2009 Cengage-Wadsworth

Absorption • Absorption is the movement of molecules across the gastrointestinal (GI) tract into the circulatory system. • Most of the end-products of digestion, along with vitamins , minerals, and water, are absorbed in the small intestinal lumen by four mechanisms for absorption: (1) active transport, (2) passive diffusion, (3) endocytosis, and (4) facilitative diffusion. • Active transport requires energy

Absorption, Transport, & Distribution • Absorption of glucose & galactose – Into cell: active transport - SGLT 1 – Into blood: diffusion, GLUT 2 • Absorption of fructose – Into cell: facilitated transport - GLUT 5 – Into blood: GLUT 2 – Limited in 60% of adults � 2009 Cengage-Wadsworth

Absorption, Transport, & Distribution • Monosaccharide transport & cellular uptake • Glucose transporters – GLUT isoforms • Integral proteins • Each has specific combining site • Undergoes a conformational change upon binding the molecule • Can reverse this change when unbound � 2009 Cengage-Wadsworth

Absorption, Transport, & Distribution – Specificity of GLUTs • GLUT 1 - basic supply of glucose to cells • GLUT 2 - low infinity transporter; glucose from enterocyte to blood • GLUT 3 - high-affinity for brain & other glucosedependent tissues • GLUT 4 - insulin sensitive, in muscle & adipose tissues • GLUT 5 - for fructose � 2009 Cengage-Wadsworth

Absorption, Transport, & Distribution • Insulin – Role in cellular glucose absorption • Binds to membrane receptor • Stimulates GLUT 4 to move to membrane • Maintenance of blood glucose levels � 2009 Cengage-Wadsworth

Glycemic Response to Carbohydrates • Glycemic index – Increase in blood glucose during 2 -hour period after consumption of a certain amount of CHO compared with equal CHO from reference food • Glycemic load – GI x g of CHO in 1 serving of food � 2009 Cengage-Wadsworth

Introduction to Carbohydrate Metabolism • It is mainly Glucose metabolism which has many anabolic and catabolic pathways: • Major pathway for Glucose oxidation: – Glycolysis – Citric Acid Cycle • Minor Pathways for Glucose oxidation: – HMP (Hexose Monophosphate Pathway) shunt • Glycogenesis • Gluconeogenesis • Conversion to other monosaccharides � 2009 Cengage-Wadsworth
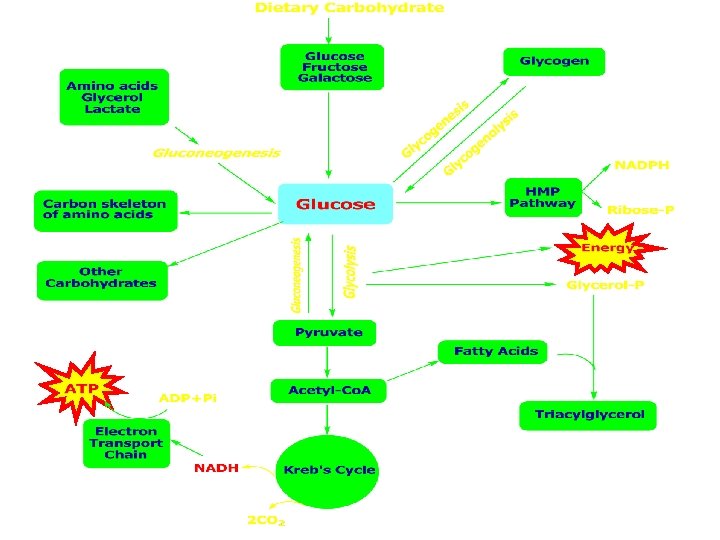

Major Pathway of Glucose Oxidation • Definition: – Conversion of Glucose to 2 pyruvate(or lactate), then to 6 CO 2 & producing ATPs + reduced nucleotides • Site: – Glycolysis in all cells – Krebs’ Cycle in all cells containing mitochondria
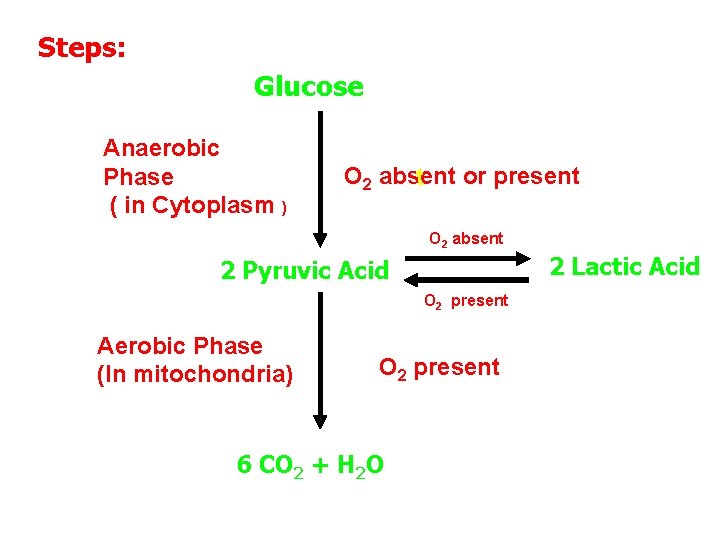
Steps: Glucose Anaerobic Phase ( in Cytoplasm ) O 2 absent or present t O 2 absent 2 Lactic Acid 2 Pyruvic Acid O 2 present Aerobic Phase (In mitochondria) O 2 present 6 CO 2 + H 2 O
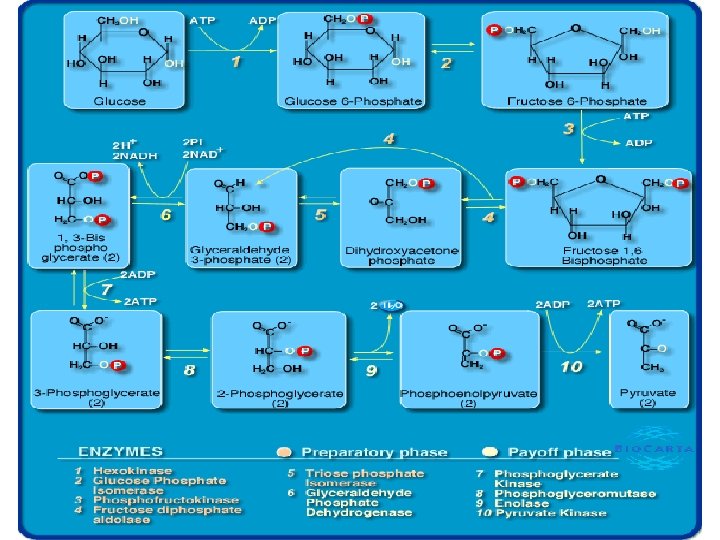

I. Glycolysis (Embden Meyerhof Pathway): A. Definition: 1. Glycolysis means oxidation of glucose to give pyruvate (in the presence of oxygen) or lactate (in the absence of oxygen). B. Site: cytoplasm of all tissue cells, but it is of physiological importance in: 1. Tissues with no mitochondria: mature RBCs, cornea and lens. 2. Tissues with few mitochondria: Testis, leucocytes, medulla of the kidney, retina, skin and gastrointestinal tract. 3. Tissues undergo frequent oxygen lack: skeletal muscles especially during exercise.

C. Steps: Stages of glycolysis 1. Stage one (the energy requiring stage): a) One molecule of glucose is converted into two molecules of glycerosldhyde-3 -phosphate. b) These steps requires 2 molecules of ATP (energy loss) 2. Stage two (the energy producing stage): a) The 2 molecules of glyceroaldehyde-3 -phosphate are converted into pyruvate (aerobic glycolysis) or lactate (anaerobic glycolysis(. b) These steps produce ATP molecules (energy production). D. Energy (ATP) production of glycolysis: ATP production = ATP produced - ATP utilized
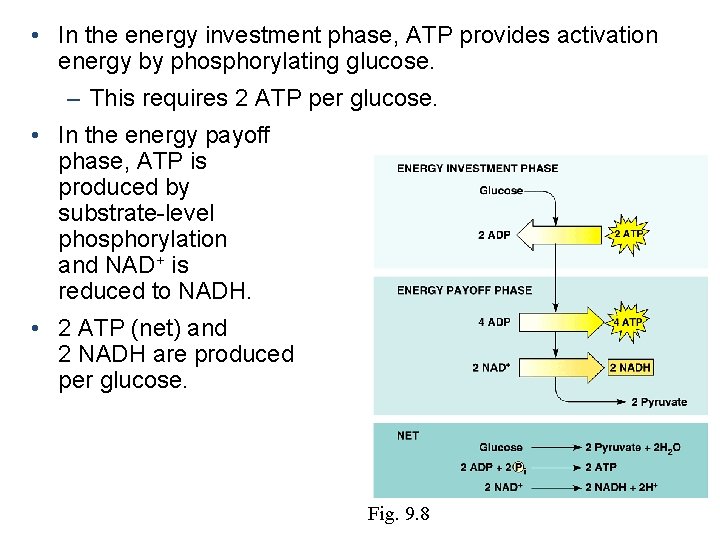
• In the energy investment phase, ATP provides activation energy by phosphorylating glucose. – This requires 2 ATP per glucose. • In the energy payoff phase, ATP is produced by substrate-level phosphorylation and NAD+ is reduced to NADH. • 2 ATP (net) and 2 NADH are produced per glucose. Fig. 9. 8
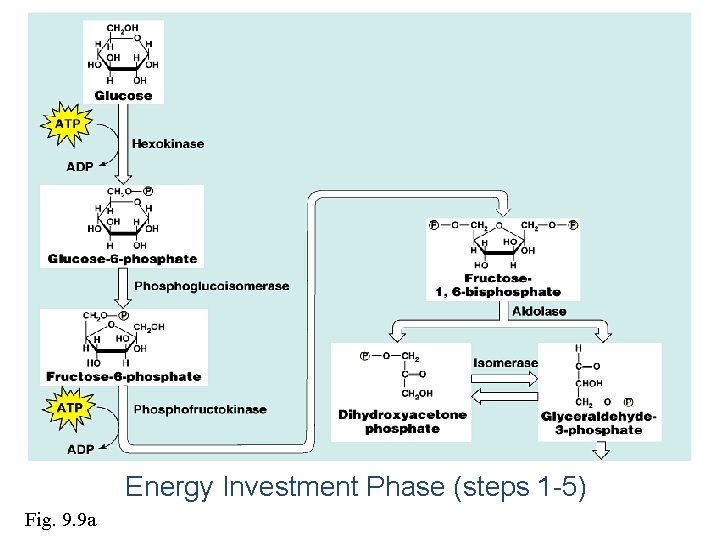
Energy Investment Phase (steps 1 -5) Fig. 9. 9 a
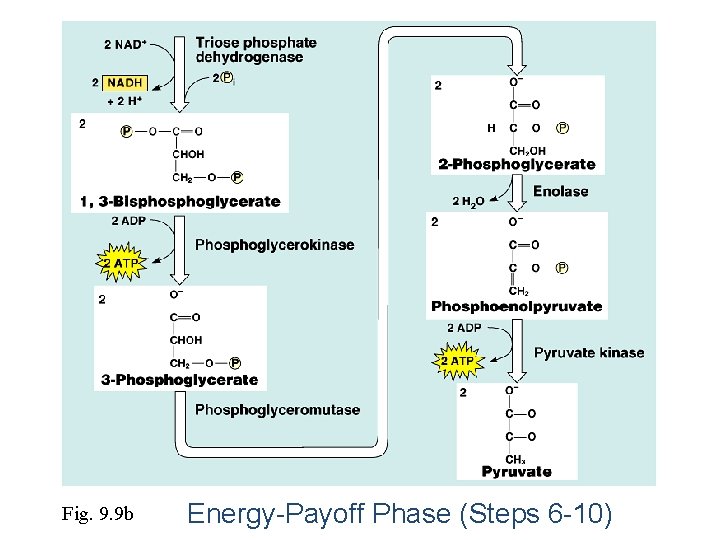
Fig. 9. 9 b Energy-Payoff Phase (Steps 6 -10)
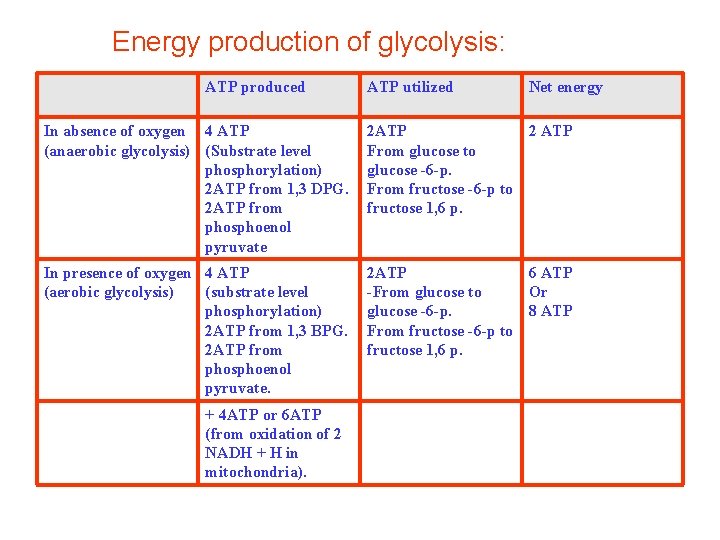
Energy production of glycolysis: ATP produced ATP utilized Net energy In absence of oxygen 4 ATP (anaerobic glycolysis) (Substrate level phosphorylation) 2 ATP from 1, 3 DPG. 2 ATP from phosphoenol pyruvate 2 ATP 2 ATP From glucose to glucose -6 -p. From fructose -6 -p to fructose 1, 6 p. In presence of oxygen 4 ATP (aerobic glycolysis) (substrate level phosphorylation) 2 ATP from 1, 3 BPG. 2 ATP from phosphoenol pyruvate. 2 ATP 6 ATP -From glucose to Or glucose -6 -p. 8 ATP From fructose -6 -p to fructose 1, 6 p. + 4 ATP or 6 ATP (from oxidation of 2 NADH + H in mitochondria).
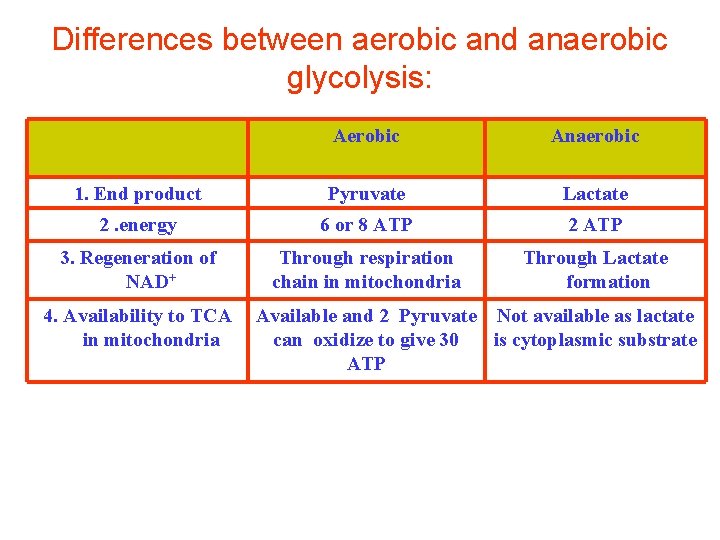

Differences between aerobic and anaerobic glycolysis: Aerobic Anaerobic 1. End product Pyruvate Lactate 2. energy 6 or 8 ATP 2 ATP 3. Regeneration of NAD+ Through respiration chain in mitochondria Through Lactate formation 4. Availability to TCA in mitochondria Available and 2 Pyruvate Not available as lactate can oxidize to give 30 is cytoplasmic substrate ATP

Biological importance (functions) of glycolysis: 1. Energy production: a) anaerobic glycolysis gives 2 ATP. b) aerobic glycolysis gives 8 ATP. 2. Oxygenation of tissues: Through formation of 2, 3 bisphoglycerate, which decreases the affinity of Hemoglobin to O 2. 3. Provides important intermediates: a) Dihydroxyacetone phosphate: can give glycerol-3 phosphate, which is used for synthesis of triacylglycerols and phospholipids (lipogenesis). b) 3 Phosphoglycerate: which can be used for synthesis of amino acid serine. c) Pyruvate: which can be used in synthesis of amino acid alanine. 4. Aerobic glycolysis provides the mitochondria with pyruvate, which gives acetyl Co. A Krebs' cycle.

Comparison between glucokinase and hexokinase enzymes: Glucokinaase Hexokinase 1. Site Liver only All tissue cells 2. Affinity to glucose Low affinity (high km) i. e. it acts only in the presence of high blood glucose concentration. High affinity (low km) i. e. it acts even in the presence of low blood glucose concentration. 3. Substrate Glucose only Glucose, galactose and fructose 4. Effect of insulin Induces synthesis of glucokinase. No effect 5. Effect of glucose-6 -p No effect Allosterically inhibits hexokinase 6. Function Acts in liver after meals. It removes glucose coming in portal circulation, converting it into glucose -6 -phosphate. It phosphorylates glucose inside the body cells. This makes glucose concentration more in blood than inside the cells. This leads to continuous supply of glucose for the tissues even in the presence of low blood glucose concentration.

Importance of lactate production in anerobic glycolysis: 1. In absence of oxygen, lactate is the end product of glycolysis: Glucose Pyruvate Lactate 2. In absence of oxygen, NADH + H+ is not oxidized by the respiratory chain. 3. The conversion of pyruvate to lactate is the mechanism for regeneration of NAD+. 4. This helps continuity of glycolysis, as the generated NAD+ will be used once more for oxidation of another glucose molecule.
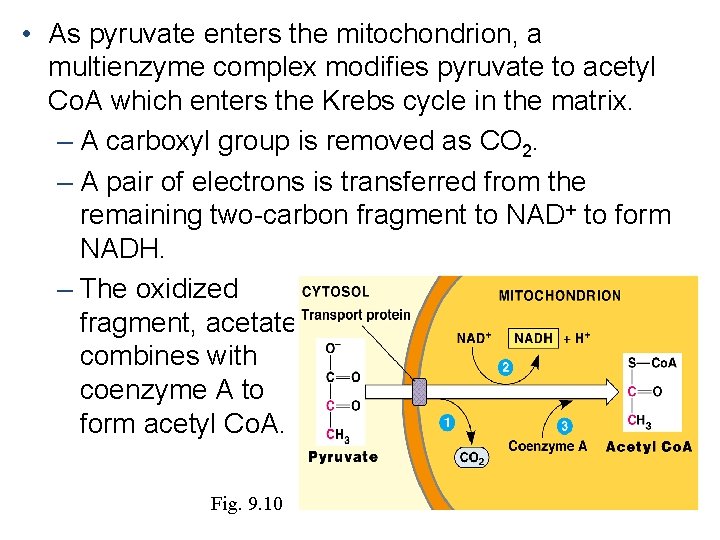
• As pyruvate enters the mitochondrion, a multienzyme complex modifies pyruvate to acetyl Co. A which enters the Krebs cycle in the matrix. – A carboxyl group is removed as CO 2. – A pair of electrons is transferred from the remaining two-carbon fragment to NAD+ to form NADH. – The oxidized fragment, acetate, combines with coenzyme A to form acetyl Co. A. Fig. 9. 10

Citric acid Cycle (Tricarboxylic Acid Cycle) (Kreb’s Cycle)

Definition: Complete oxidation of acetyl Co. A to 2 molecules of CO 2 and generating energy either directly as ATP or in the form of reducing equivalents (NADH or FADH 2). Location: All cells that contain mitochondria (i. e. not in RBCs) Site: All enzymes are found free in mitochondria matrix except succinate dehydrogenase which is found on the inner border of the inner mitochondrial membrane.

The Krebs Cycle • Occurs in the matrix of the mitochondrion • Aerobic phase (requires oxygen) • 2 -carbon acetyl Co. A joins with a 4 -carbon compound to form a 6 - carbon compound called Citric acid

• Citric acid (6 C) is gradually converted back to the 4 carbon compound -ready to start the cycle once more • The carbons removed are released as CO 2 -enzymes controlling this process called decarboxylases • The hydrogens, which are removed, join with NAD to form NADH 2 -enzymes controlling the release of hydrogen are called dehydrogenases
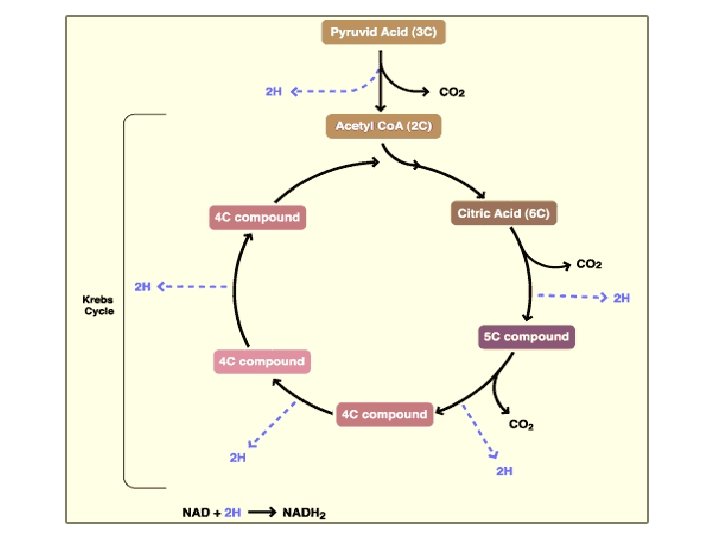

Functions of Citric Acid Cycle Amphibolic Function I- Energy production II- Catabolic for glucose, fat &proteins III- Anabolic Function
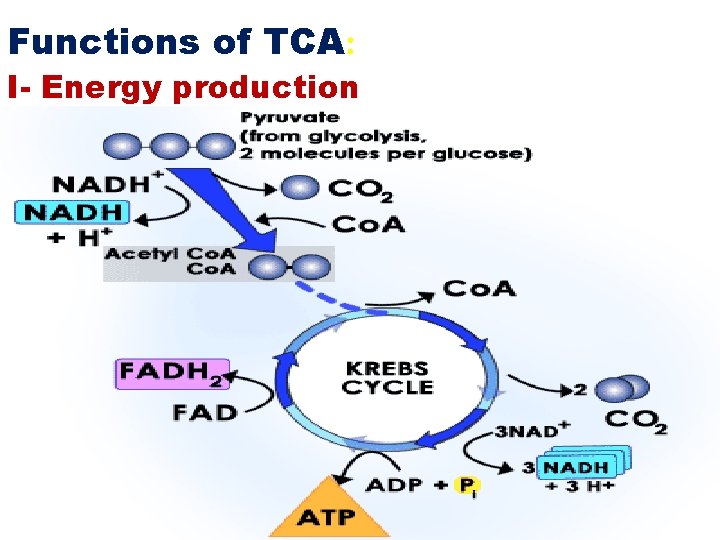
Functions of TCA: I- Energy production
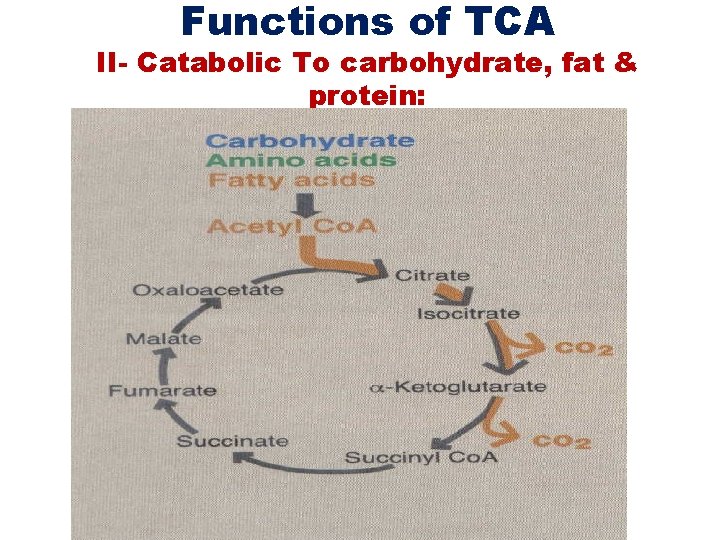
Functions of TCA II- Catabolic To carbohydrate, fat & protein:
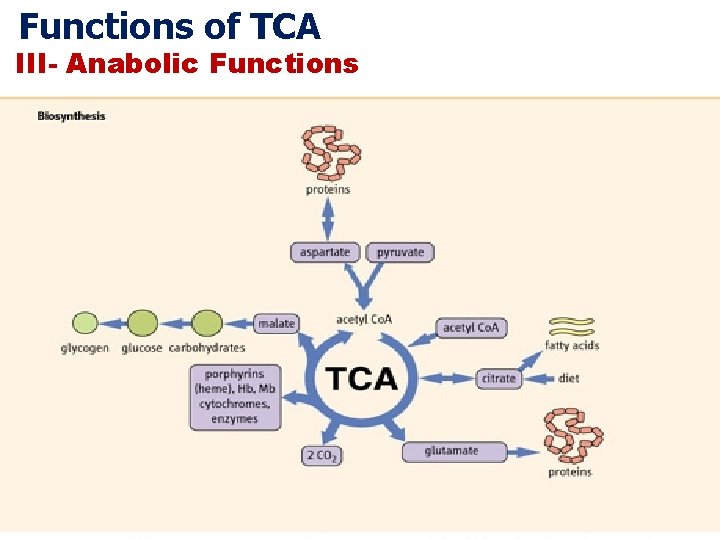
Functions of TCA III- Anabolic Functions
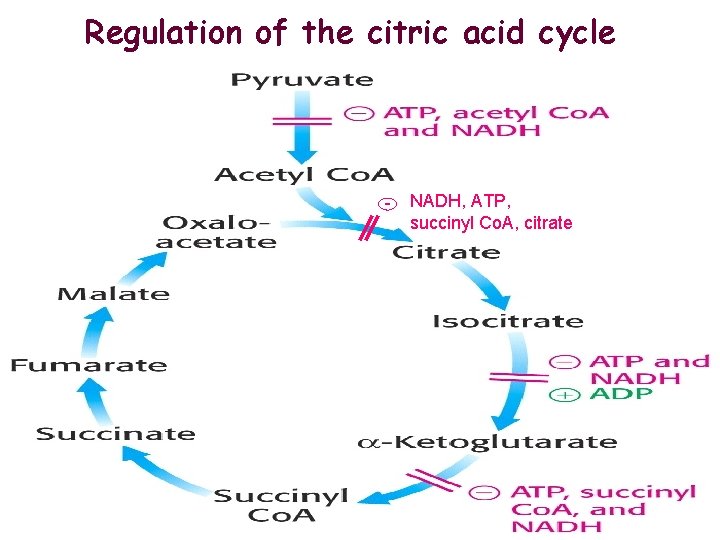
Regulation of the citric acid cycle - NADH, ATP, succinyl Co. A, citrate
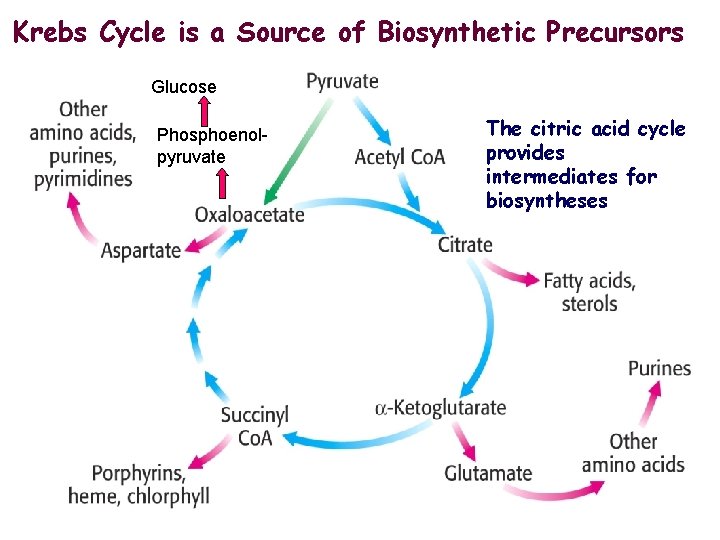
Krebs Cycle is a Source of Biosynthetic Precursors Glucose Phosphoenolpyruvate The citric acid cycle provides intermediates for biosyntheses

Summary for Complete oxidation of Glucose Complete aerobic oxidation of glucose in glycolysis, citric acid cycle and ETC produces 6 molecules of CO 2 + 38 molecules of ATP (38 moles of ATP / one mole of glucose) N. B: Complete oxidation of one glucose molecule in RBC gives 2 ATP + 2 lactate molecules

Key Concepts The TCA cycle accounts for more than two thirds of the ATP generated from fuel oxidation. All of the enzymes required for the TCA cycle are in the mitochondria. Acetyl Co. A, generated from fuel oxidation, is the substrate for the TCA cycle. Acetyl Co. A, when oxidized via the cycle, generates CO 2, reduced electron carriers, and GTP. The reduced electron carriers [NADH, FADH 2} donate electrons to O 2 via the electron transport chain, which leads to ATP generation from oxidative phosphorylation.

The cycle requires a number of cofactors to function properly, some of which are derived from vitamins. These include thiamin pyrophosphate (derived from vitamin B 1, thiamin), FAD (derived from vitamin B 2, riboflavin), and coenzyme A (derived from pantothenic acid) and NAD (from niacin). Intermediates of the TCA cycle are used for many biosynthetic reactions and are replaced by anaplerotic (refilling) reactions within the cell. The cycle is carefully regulated within the mitochondria by energy and the levels of reduced electron carriers. As energy levels decrease, the rate of the cycle increases. Impaired functioning of the TCA cycle leads to an inability to generate ATP from fuel oxidation and an accumulation of TCA cycle precursors.

Minor Pathway for oxidation of glucose • The hexosemonophosphate shunt (pentose phosphate pathway)=pentose shunt=HMP. � 2009 Cengage-Wadsworth

Pentose Phosphate Pathway Definition: It is a pathway by which pentose phosphate is produced from glucose (with production of two molecules of NADPH), or from other monosaccharides. No ATP is directly consumed or produced in the cycle. Location: Mainly in liver, lactating mammary glands, adipose tissue, adrenal cortex, gonads and RBCs. Site: Cytoplasm

Steps: The pentose phosphate pathway occurs in two phases oxidative and non oxidative �I Oxidative Phase This phase is irreversible; glucose 6 phosphate is converted to ribulose 5 phosphate with production of two molecules of NADPH. �II Non oxidative Phase This phase is reversible. It catalyzes the conversion of pentoses produced in phase one into 2 molecules of Glyceraldehyde 3 Phosphate and Fructose 6 Phosphate (By the enzymes transketolase and transaldolase), which continue in the glycolytic pathway.

Regulation of HMP The regulated step is glucose 6 P dehydrogenase (G 6 PD), which is strongly inhibited by NADPH (its product).

Importance of Pentose Phosphate Pathway I- It is the ONLY source of ribose-5 -phosphate Ribose 5 phosphate forms phospho ribosyl pyrophosphate (PRPP) for synthesis of nucleotides and nucleic acids. In tissues (e. g. muscles) which lack the dehydrogenases of the oxidative phase and in cases of deficiency of G 6 PD, pentoses are formed by reversal of the non oxidative phase, starting from fructose 6 P and glyceradehyde 3 P.

ll- It is the main source of NADPH required for the reaction of many reductases, hydroxylases and NADPH oxidase. lll – It provides a way for utilizing dietary C 4 -, C 5 -, and C 7 sugars

Regulation of Metabolism • 4 mechanisms: – Negative or positive modulation of allosteric enzymes – Hormonal activation by covalent modification/induction – Directional shifts in reactions – Translocation of enzymes within cells � 2009 Cengage-Wadsworth

Anabolic Pathway Glycogenesis and glycogenolysis

Glycogenesis • Glycogen is a highly branched glucose polymer used for carbohydrate storage in animals • Glycogen stores are used to keep the blood sugar level steady between meals • Glycogenesis is the synthesis of glycogen from glucose-6 phosphate - it occurs when high levels of glucose-6 -phosphate are formed in the first reaction of glycolysis - it does not operate when glycogen stores are full, which means that additional glucose is converted to body fat
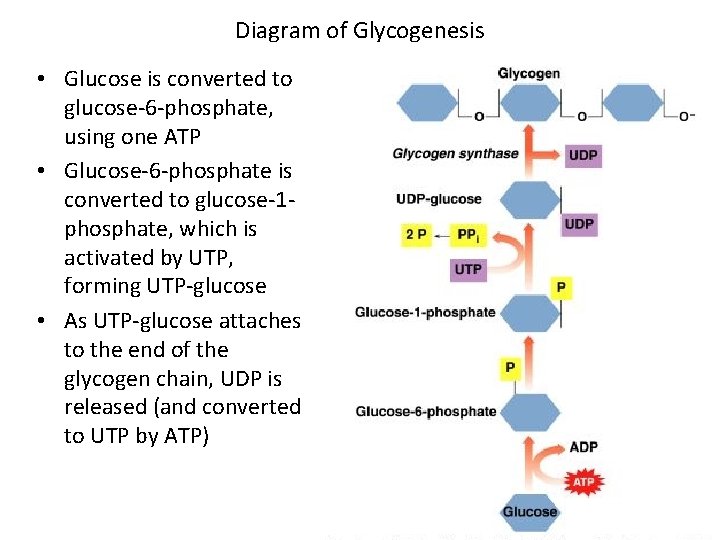
Diagram of Glycogenesis • Glucose is converted to glucose-6 -phosphate, using one ATP • Glucose-6 -phosphate is converted to glucose-1 phosphate, which is activated by UTP, forming UTP-glucose • As UTP-glucose attaches to the end of the glycogen chain, UDP is released (and converted to UTP by ATP)
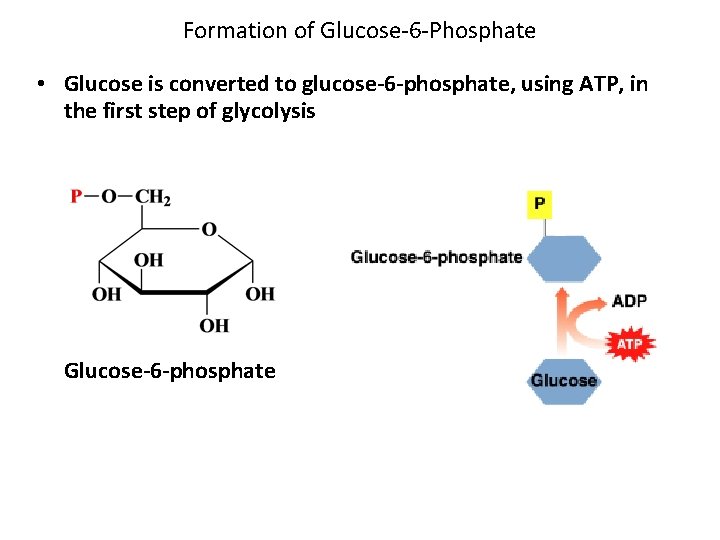
Formation of Glucose-6 -Phosphate • Glucose is converted to glucose-6 -phosphate, using ATP, in the first step of glycolysis Glucose-6 -phosphate
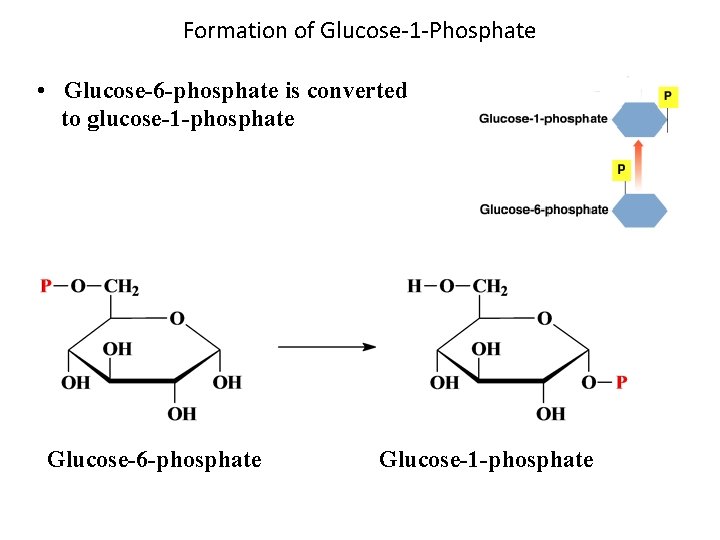
Formation of Glucose-1 -Phosphate • Glucose-6 -phosphate is converted to glucose-1 -phosphate Glucose-6 -phosphate Glucose-1 -phosphate
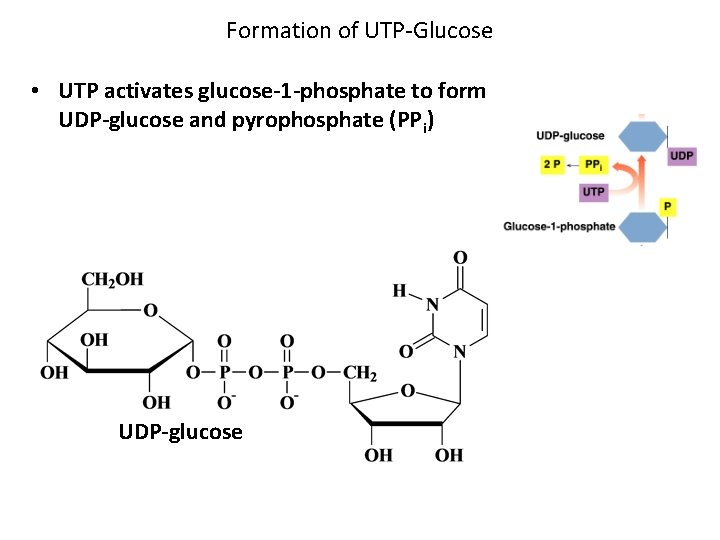
Formation of UTP-Glucose • UTP activates glucose-1 -phosphate to form UDP-glucose and pyrophosphate (PPi) UDP-glucose

Glycogenolysis • Glycogenolysis is the breakdown of glycogen to glucose • The glucose is phosphorylated as it is cleaved from the glycogen to form glucose-1 -phosphate • Glucose-1 -phosphate can be converted to glucose-6 phosphate, which can enter glycolysis • Phosphorylated glucose can’t be absorbed into cells - in the liver and kidneys, glucose-6 -phosphate can be hydrolized to glucose • Glycogenolysis is activated by glucogon in the liver and epinephrine in muscles - these are produced when blood glucose levels are low • Glycogenolysis is inhibited by insulin - insulin is produced when blood glucose levels are high
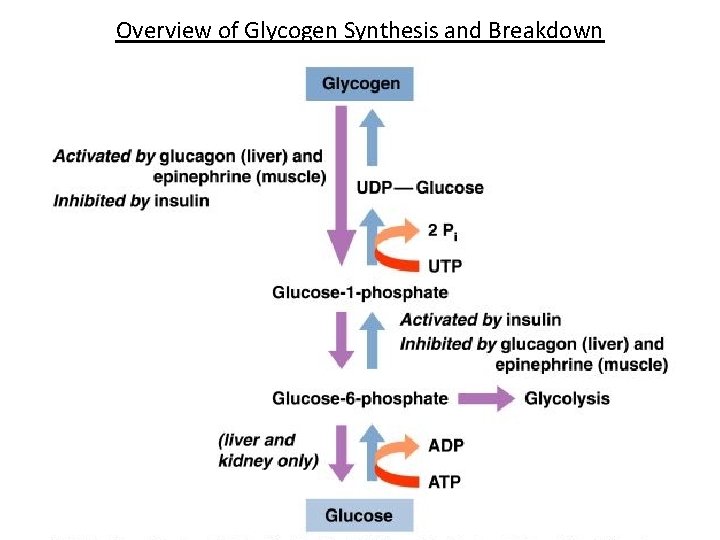
Overview of Glycogen Synthesis and Breakdown
Gluconeogenesis (Glucose Synthesis) • Glucose is the primary energy source for the brain, skeletal muscle, and red blood cells • Deficiency can impair the brain function • Gluconeogenesis is the synthesis of glucose from carbon atoms of noncarbohydrates - required when glycogen stores are depleted

GLUCONEOGENESIS

GLUCONEOGENESIS • Definition: – It is synthesis of glucose from non carbohydrate sources. Its main function is to supply blood glucose in case of carbohydrate deficiency (fasting more than 10 18 hours). • Location: – It occurs mainly in the liver cells and to lesser extent in kidneys • Site: – Cytoplasm except for the first step (carboxylation of pyruvate) occurs in the mitochondria.

Substrates for Gluconeogenesis (Gluconeogenic Precursors) � These are molecules that can be used to produce glucose. They give directly or indirectly pyruvate, oxaloacetate or any intermediates of glycolysis or citric acid cycle. � 1 Glucogenic Amino Acids � 2 Glycerol � 3 Lactate

Substrates for Gluconeogenesis (Gluconeogenic Precursors) • 1 Glucogenic Amino Acids These are amino acids which are convertible to glucose. They give pyruvate or oxaloacetate directly or indirectly by giving intermediates of citric acid cycle • 2 Glycerol released from hydrolysis of TAG in adipose tissue, go to the liver via blood. In the liver the following will occur: NB. Adipose tissue has NO glycerol kinase

Substrates for Gluconeogenesis (Gluconeogenic Precursors) • 3 Lactate It is produced by red blood cells and by contracting muscles, then passes to the liver where it is converted to glucose which is released back into the circulation. (Cori’s Cycle)
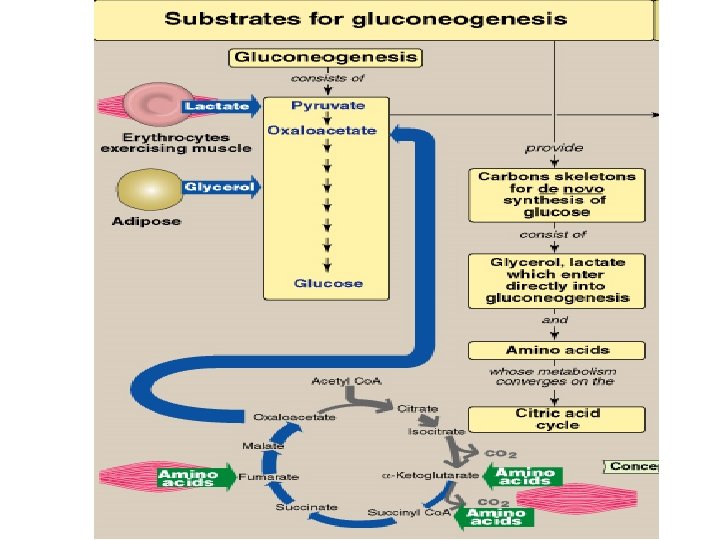

Importance of Gluconeogenesis � 1 Maintenance of blood glucose: The main function of gluconeogenesis is the maintenance of blood glucose when carbohydrates are not available in sufficient amounts e. g. fasting, starvation, stress, prolonged exercise and dietary carbohydrate deficiency for more than 10 – 18 hours. � 2 Removal of lactic acid produced by red cells and contracting muscles. � 3 Removal of glycerol produced by lipolysis in adipose tissues.

A common intermediate in the conversion of glycerol and lactate is which of the following? a. Pyruvate b. Oxaloacetate c. Malate d. Glucose 6 phosphate e. Phosphoenolpyruvate

Cori and Alanine Cycles Cori cycle prevents loss of lactate as waste product in urine, and prevent its accumulation in blood (acidosis) Both help to maintain blood glucose level specially to tissues that dependant on it as their primary source of energy. Both supply RBCs and contracting muscles with glucose for reutilization and ATP production. Both spare energy in red cells and contracting muscles.
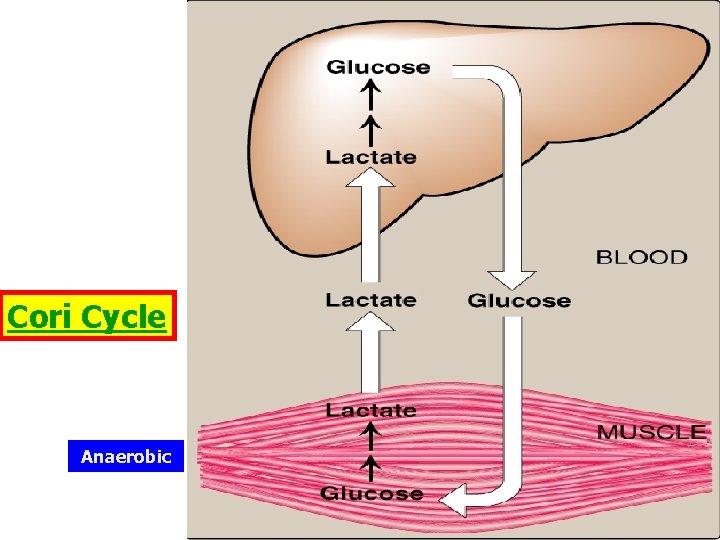
Cori Cycle Anaerobic
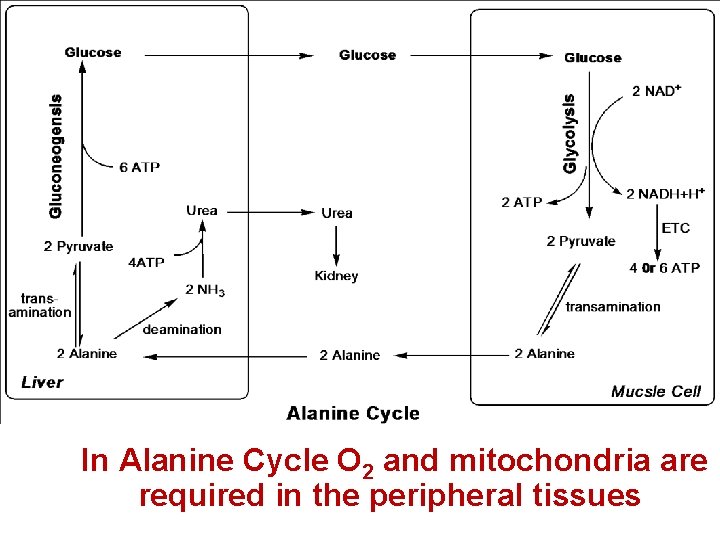
In Alanine Cycle O 2 and mitochondria are required in the peripheral tissues

REGULATION OF GLUCONEOGENESIS The gluconeogenic regulatory key enzymes are those which reverse the glycolytic key enzymes. • Glycolysis and gluconeogenesis are reciprocally controlled.

Factors which increase gluconeogenesis I- Availability of substrates: Availability of gluconeogenic substrates specially glucogenic amino acids provide increased amounts of oxaloacetic acid. � Excess ATP (from FA oxidation) produces allosteric inhibition of phosphofructokinase 1 and pyruvate kinase (glycolysis) and activate F 1, 6 BPase (gluconeogenesis). � Excess acetyl Co. A, (from FA oxidation), allosterically stimulates pyruvate carboxylase enzyme and inhibits pyruvate dehydrogenase, thus directs pyruvate to gluconeogenesis.

Cori Cycle • When anaerobic conditions occur in active muscle, glycolysis produces lactate • The lactate moves through the blood stream to the liver, where it is oxidized back to pyruvate. • Gluconeogenesis converts pyruvate to glucose, which is carried back to the muscles • The Cori cycle is the flow of lactate and glucose between the muscles and the liver
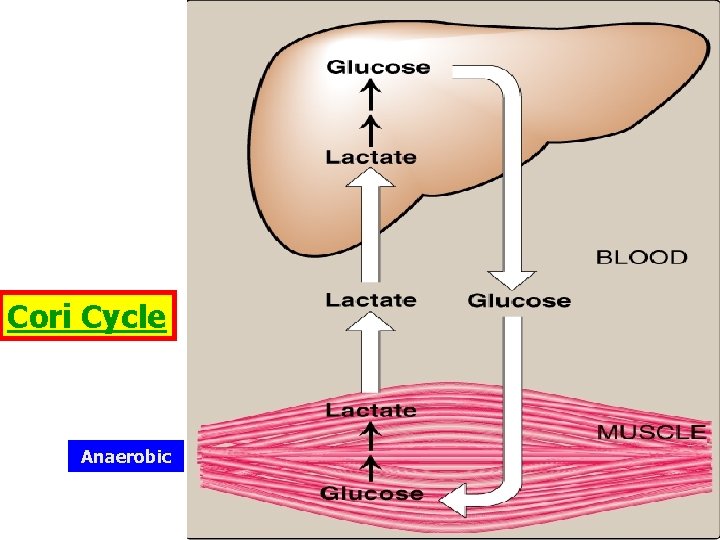
Cori Cycle Anaerobic

Cori and Alanine Cycles Cori cycle prevents loss of lactate as waste product in urine, and prevent its accumulation in blood (acidosis) Both help to maintain blood glucose level specially to tissues that dependant on it as their primary source of energy. Both supply RBCs and contracting muscles with glucose for reutilization and ATP production. Both spare energy in red cells and contracting muscles.
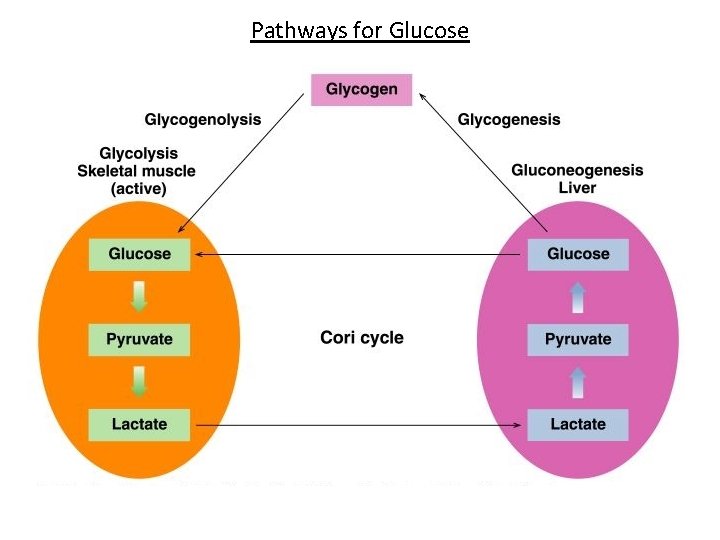
Pathways for Glucose
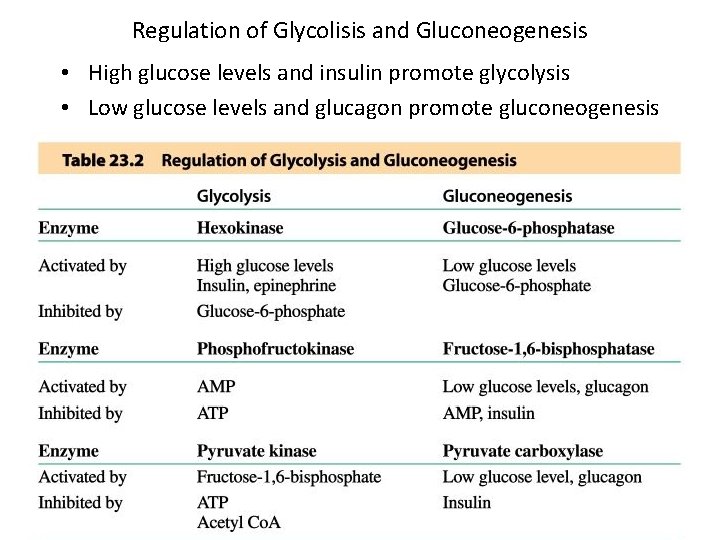
Regulation of Glycolisis and Gluconeogenesis • High glucose levels and insulin promote glycolysis • Low glucose levels and glucagon promote gluconeogenesis

Hypoglycemia • Preprandial vs. postprandial serum glucose levels • Types: – Fasting hypoglycemia • Usually caused by insulin, sulfonylureas – Fed (reactive) hypoglycemia • Impaired glucose tolerance, idiopathic postprandial syndrome � 2009 Cengage-Wadsworth
- Slides: 82